Clinical History: A 67 year old man presents with a history of chronic low back pain radiating into both buttocks, the back of both legs, and into the calves. He also complains of paresthesias manifested as a “pins and needles” sensation in a non-dermatomal pattern. There is no history of neoplasm, back surgery, spine intervention or myelography. A physical exam reveals mild bilateral weakness in hip internal rotation and great toe extension. Patellar and ankle reflexes were mildly depressed.
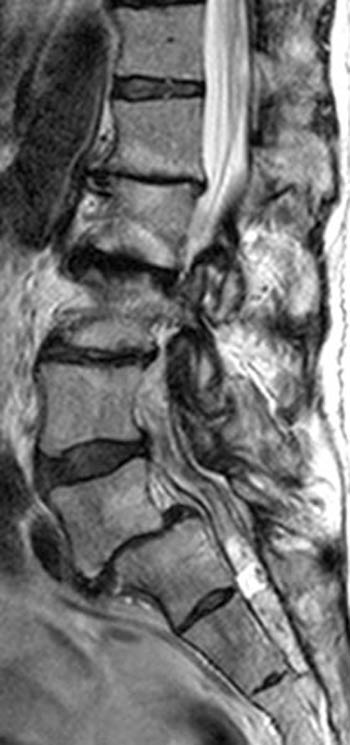
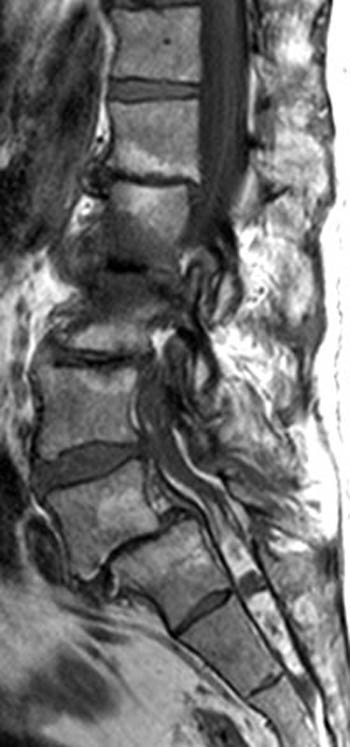
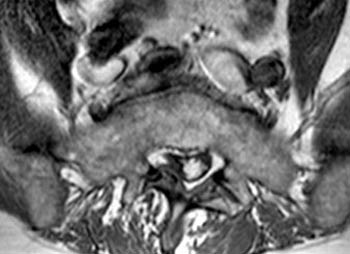
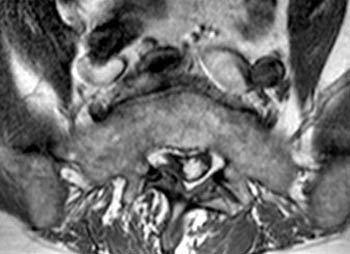
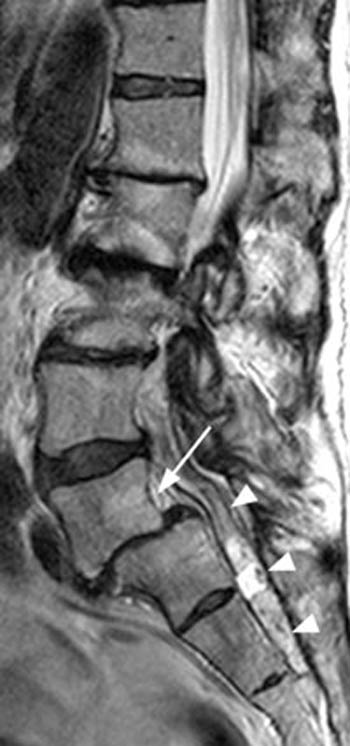
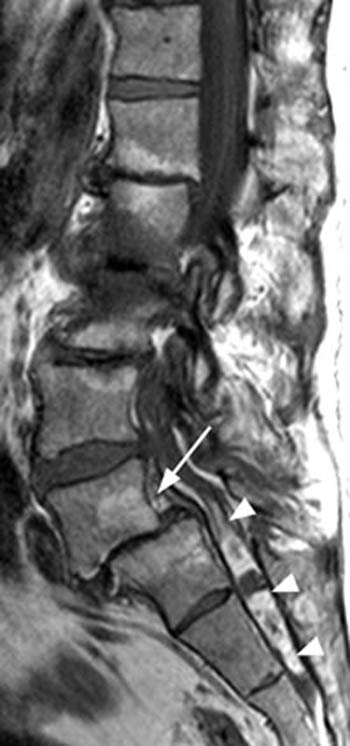
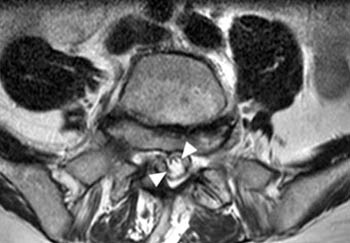
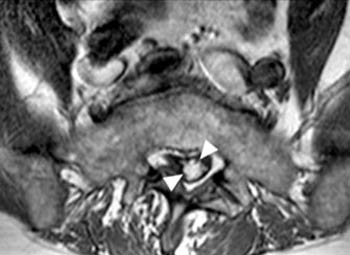
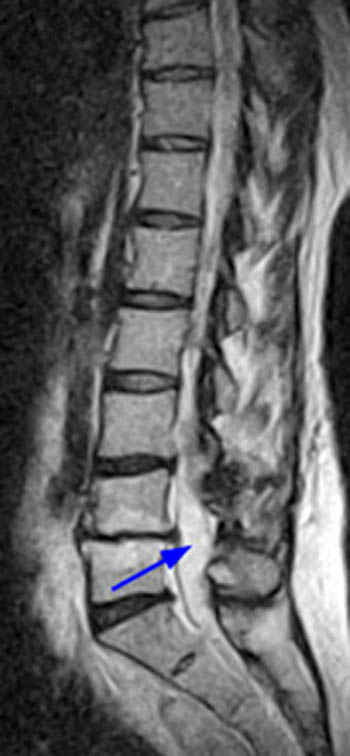
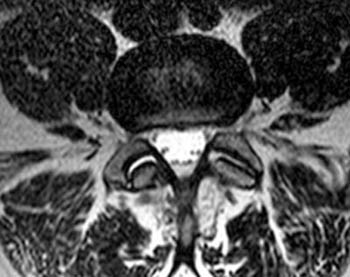
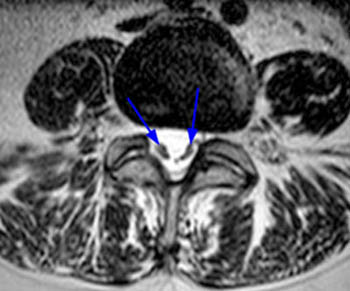
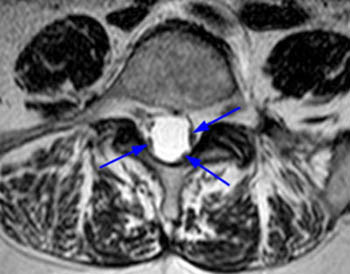
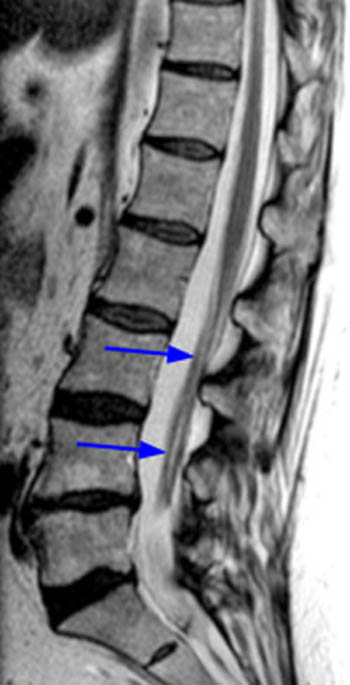
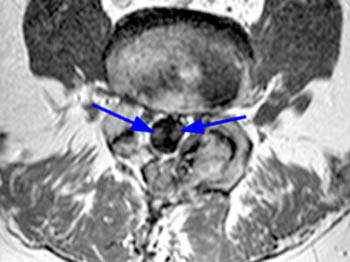
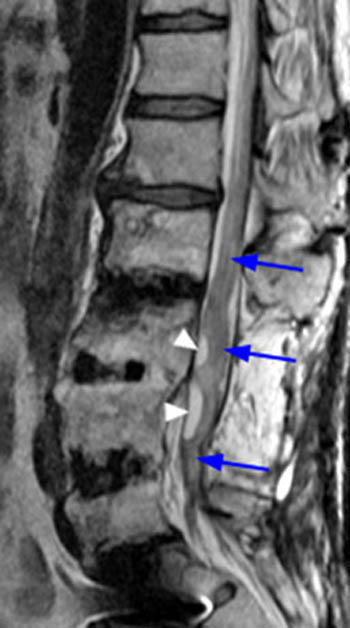
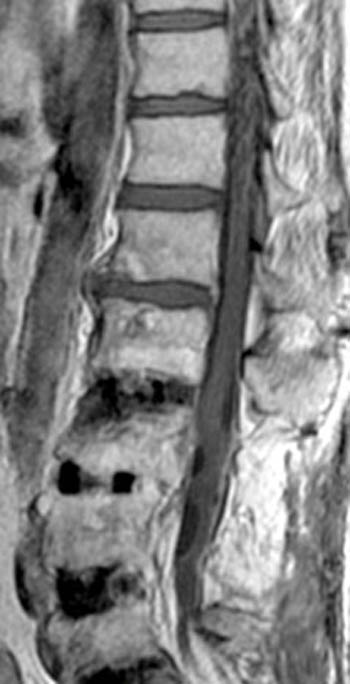
Fast spin echo T2-weighted and T1-weighted (1a,1b) sagittal and (1c,1d) axial images of the lumbar spine are provided. What are the findings” What is your diagnosis?
Findings
Figure 2:
(2a,2b) Sagittal images reveal a Grade II spondylolisthesis at L5-S1 (arrows) and a long tubular intrathecal mass (arrowheads) extending from L5-S1 through S1-S2. This mass has complex signal, but is substantially bright on T1 and T2-weighted sequences. The central high signal intensity intrathecal mass (arrowheads) is confirmed on (2c,2d) the axial images. A CT scan (not shown) demonstrated high density within the mass compatible with calcification/ossification.
Diagnosis
Arachnoiditis Ossificans.
Discussion
Chronic adhesive arachnoiditis is a form of leptomeningeal and neural inflammation within the spinal canal. It develops after an acute form of arachnoiditis or nerve root “radiculitis”, beginning with an inflammatory exudative reaction and progressing into fibrin deposition along nerve root sheaths and pial/arachnoid surfaces. Collagenous strands then develop, adhering nerve roots and septating the subarachnoid space.
The inciting injury may be related to intradural surgery or dural tears, meningitis, trauma, subarachnoid hemorrhage, myelography, injection of intraspinal anesthetic agents, or injection of epidural steroids (as most of these agents contain preservatives which are neurotoxic). Myelography with oil-based agents such as Pantopaque, especially after a subarachnoid hemorrhage, carries higher risk than the use of non-ionic water soluble agents. Pyogenic or granulomatous meningitis carries greater risk than viral infection. Many cases of arachnoiditis, however, are idiopathic.
Patients commonly present with chronic low back pain with or without radicular symptoms, which may simulate spinal stenosis and polyneuropathy. Paraesthesia and hypoesthesia are common. Gait disturbance, incontinence and myelopathic symptoms dominate in a minority of patients. No gender or race predisposition is apparent. Treatment choices are limited and include intrathecal steroid injection and spinal cord stimulation for pain management. Surgical lysis of adhesions and arachnoid septations is usually not indicated or successful. The severity of symptoms may not correlate with the degree of imaging findings, though the imaging appearance does correlate with pathological findings.
Mild cases of arachnoiditis are manifested as clumping of nerve roots, usually more obvious at the L3 and L4 levels. Imaging clues include the loss of normal “fanning” (3a) of the nerve roots in the thecal sac on sagittal images.
The lack of normal “fanning” on sagittal views (4a) indicates an abnormal position of nerve roots within the sac due to segmental nerve root adherence. Slight thickening of nerve roots (5a), adherence of one or more roots to the periphery of the thecal sac, and blunting of nerve root sheaths are all signs of mild disease. The latter finding is more obvious or more confidently visualized on myelography. The thickened nerve roots do not substantially enhance. If significant enhancement is present, another diagnosis such as CSF metastases, Guillan-Barre syndrome, active granulomatous infection or breakdown of the “blood “brain barrier” along nerves after conus infarct should be considered. Overall, mild arachnoiditis is probably underreported on imaging due to the subtly of appearance and the serious nature of the diagnosis.
Moderate arachnoiditis is diagnosed when multiple nerve roots are adherent to the margins of the thecal sac (empty sac sign) or are clumped together across multiple segments (7a, pseudotethering). Strands of scar can loculate the CSF, creating intradural cysts or a bizarre appearance to the sac.
Severe arachnoiditis (11a,12a,13a) is manifested as intradural soft tissue masses and a bizarre constricted appearance of the thecal sac with stenosis. Disturbed CSF flow resulting from loculations and scar may lead to syrinx formation. Arachnoiditis Ossificans is a form of severe arachnoiditis where scar is ossified. Proposed mechanisms for this appearance include ossification after intradural hemorrhage and osseous metaplasia following chronic inflammation. The MR appearance of this process is complex, as scar can be bright or dark on T2, and bone in certain forms of mineralization may be bright on T1. The appearance may be further complicated by the coexistence of hemorrhage. In addition, any bright focus in the caudal aspect of the thecal sac needs to be differentiated from retained Pantopaque, which is bright on T1, dark on T2, and suppresses with fat-suppression techniques.
Conclusion
Chronic adhesive arachnoiditis is a sometimes debilitating condition that is not uncommon in routine clinical practice. The clinical presentation of arachnoiditis may be confusing, and though the MR appearance varies widely, certain findings are characteristic, allowing the proper diagnosis and assessment to be performed in these patients.
References
1 Frizzel B, Kaplan P, Dussault R, Sevick R . Arachnoiditis Ossificans: MR Imaging Features in Five Patients: AJR 2001; 177:461-464
2 Henkelman RM, Watts JF, Kucharczyk W. High signal intensity in MR images of calcified brain tissue. Radiology 1991; 179:199 -206
3 Jaspan T, Preston BJ, Mulholland RC, Webb JK. The CT appearances of arachnoiditis ossificans. Spine 1990; 15: 148 -151
4 Johnson CE and G Sze G. Benign lumbar Arachnoiditis: MR Imaging with Gadopentetate Dimeglumine. AJNR 1990; 11: 763-770
5 Ross JS, Masaryk TJ, Modic MT, et al. MR Imaging of Arachnoiditis. AJR 1987: 1025-1032.
6 Ross JS. Magnetic Resonance Imaging of the Postoperative Spine. Semin Musculoskelet Radiol: 2000; 4:281-291.
7 Sharma A, Goyal M, Mishra M, et al. MR Imaging of Tubercular Spinal Arachnoiditis: AJR 1997; 186: 807-812.