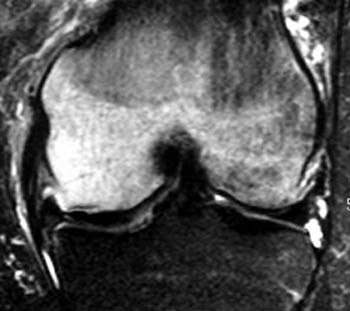
Clinical History: 78 year-old female with recent increase in right knee pain and no history of trauma. T1-weighted sagittal (1a) and fat-suppressed T2-weighted coronal (1b) images are provided. What are the findings? What is your diagnosis?
Findings
Figure 2:
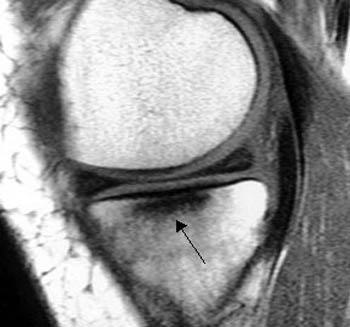
(2a) The T1-weighted sagittal image reveals an ill-defined degenerative tear (arrow) within the posterior horn of the medial meniscus. Abnormal subchondral low-signal intensity is apparent (arrowhead).
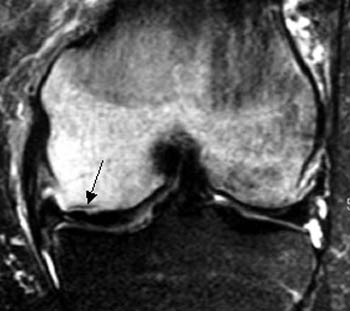
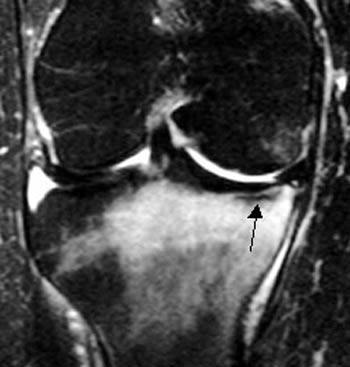
On (2b), the T2-weighted coronal image, striking bone marrow edema emanates from the medial femoral condyle. An intramedullary fracture line (arrow) is evident just above the articular surface.
Diagnosis
Subchondral insufficiency fracture along the weight-bearing surface of the medial femoral condyle.
Discussion
After reviewing the images from this case, some readers may have made the diagnosis of spontaneous osteonecrosis of the knee. This entity, first described in 1968,1 is characterized clinically by the sudden onset of severe knee pain in the absence of trauma or following minor trauma. The typical patient is an elderly female, and the medial femoral condyle is the most common site of involvement. Unlike secondary osteonecrosis, systemic risk factors such as corticosteroid use or alcoholism are not a factor in these patients. On MR images, the classic appearance of spontaneous osteonecrosis is a low signal intensity focus beneath the articular surface on T1 weighted images with striking marrow edema within the femoral condyle on fat-suppressed T2-weighted scans.2 The MR appearance in this case thus fulfills the classic diagnostic criteria. Why then, is the correct diagnosis in this case not spontaneous osteonecrosis” The preferred diagnosis of subchondral insufficiency fracture reflects relatively recent data that have increased our understanding of both the etiology and variability of outcomes in patients who were previously diagnosed with spontaneous osteonecrosis of the knee.
Radiologists and orthopaedists have long recognized that patients who develop spontaneous osteonecrosis are often elderly and osteoporotic. This osteoporotic bone is susceptible to microfracture, leading to accumulation of fluid within subchondral bone, seen as edema on MR images. In theory, the fluid leads to increased intraosseous pressure, compromising blood flow and ultimately resulting in osteonecrosis. However, osteonecrosis is not an inevitable outcome. Patients may recover completely with conservative treatment, and in these individuals MR marrow signal characteristics often return to normal. Studies have now confirmed that in many patients, the histopathologic abnormality underlying this process is a subchondral insufficiency fracture, without the presence of necrotic bone.3 Although some patients certainly do progress to osteonecrosis, the necrosis is felt to be consistently preceded by, and indeed caused by, an underlying subchondral insufficiency fracture. Interestingly, similar findings have been found in the hip, where it has been determined that many patients initially diagnosed with osteonecrosis in fact suffered from subchondral insufficiency fractures.4
Therefore, the diagnosis of spontaneous osteonecrosis should be made sparingly on MR. In late stages of disease, clearly necrotic foci may be noted, but the most common MR appearance is dominated by edema and subchondral architectural changes. With such an appearance, one can correctly make the diagnosis of subchondral insufficiency fracture, but whether or not osteonecrosis has occurred cannot be determined.
Subchondral insufficiency fractures are a relatively common cause of knee pain, particularly in older patients. Although the entity is most frequently encountered at the weightbearing surface of the medial femoral condyle, the lateral femoral condyle or the tibia may also be involved (3a,4a). Meniscal tears and osteoarthritis are often found in patients with subchondral insufficiency fractures, though the primary cause of the patient’s symptoms is almost always the fracture. MR therefore becomes quite important in the treatment algorithm, as conservative treatment of the insufficiency fracture, with limitation of weight bearing, often leads to symptom relief and fracture healing.
Conclusion
This month’s case of subchondral insufficiency fracture underscores the dynamic nature of MR imaging and orthopaedic disease classification. Even classic diagnoses such as spontaneous osteonecrosis of the knee are not immune from modification. Such changes are challenging but also exciting, as the greater understanding of the pathologic process can only improve our ability to diagnose and to treat this important cause of morbidity at the knee.
References
1 Ahlbuck S, Bauer GC, Bohne WH. Spontaneous osteonecrosis of the knee. Arthrit and Rheumat 11:705-733, 1968.
2 Resnick D. Osteonecrosis in bone and joint imaging. Ed. 2, pp. 955-958. Philadelphia, W.B. Saunders, 1996.
3 Yamamato T, Bullough PG. Spontaneous osteonecrosis of the knee: the result of subchondral insufficiency fracture. J Bone Joint Surg 82:858, 2000.
4 Yamamato T, Bullough PG. Spontaneous subchondral fracture of the femoral head. A newly recognized clinicopathologic entity. Mod Pathol 12:15A, 1999.