Clinical History:
A 51-year-old male with chronic wrist pain felt a sudden pop and acute pain exacerbation while lifting a heavy object. Axial and coronal fat-suppressed proton density-weighted and two sagittal T2-weighted MR images are provided. What are the findings? What is your diagnosis?
Findings
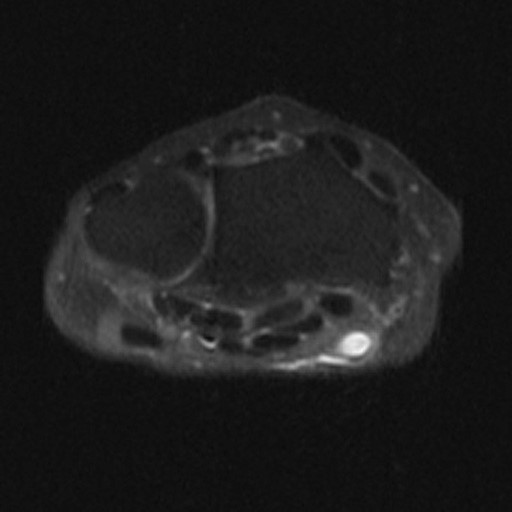
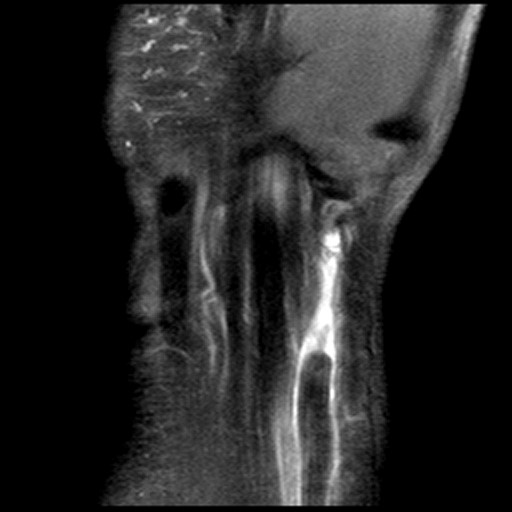
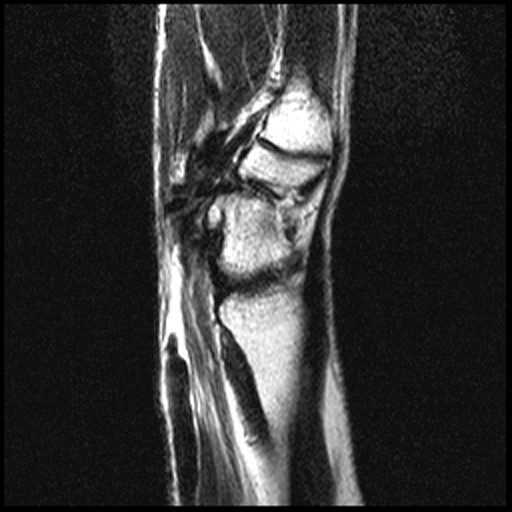
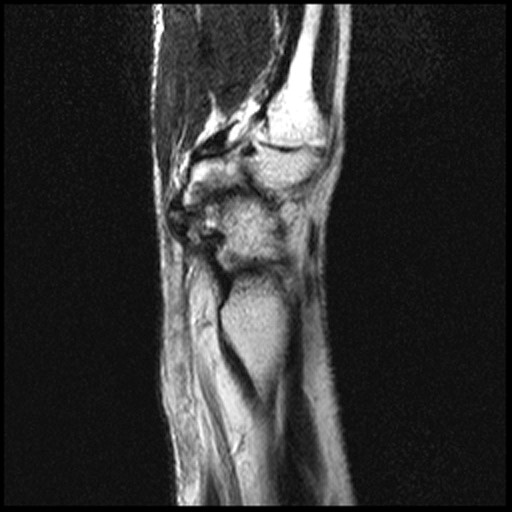
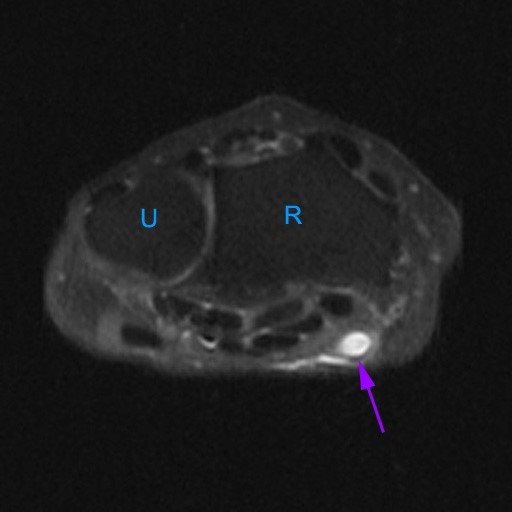
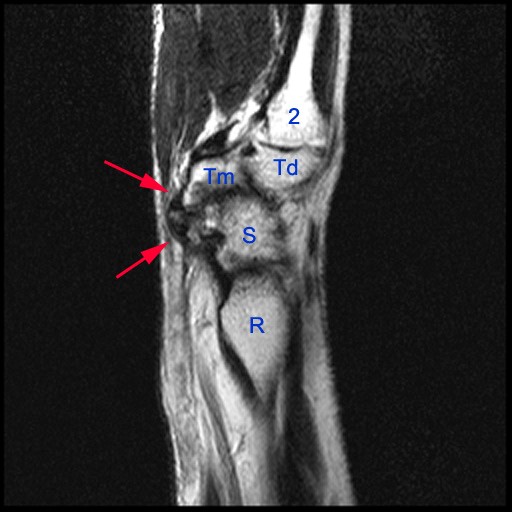
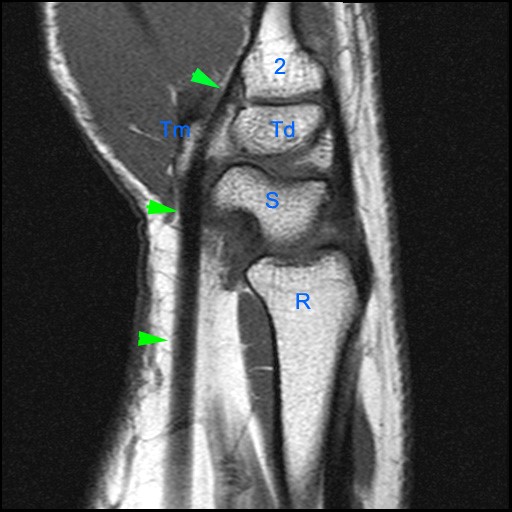
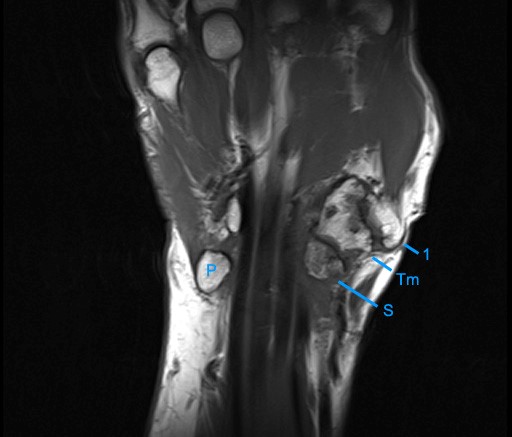
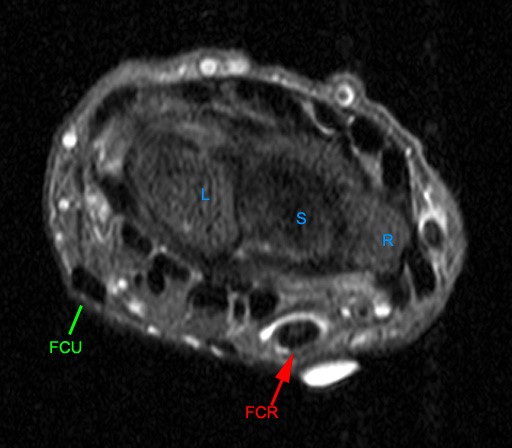
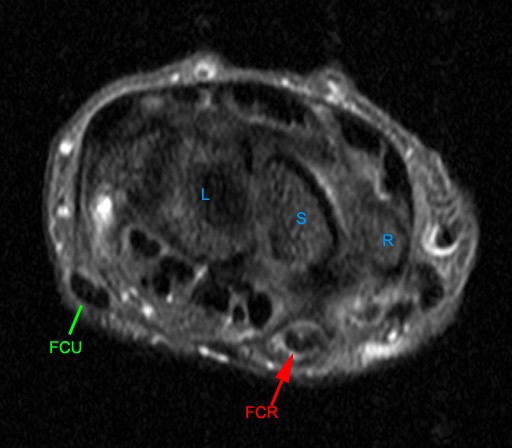
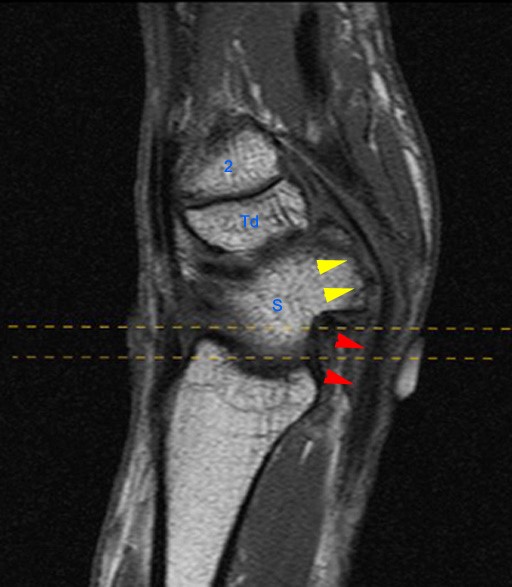
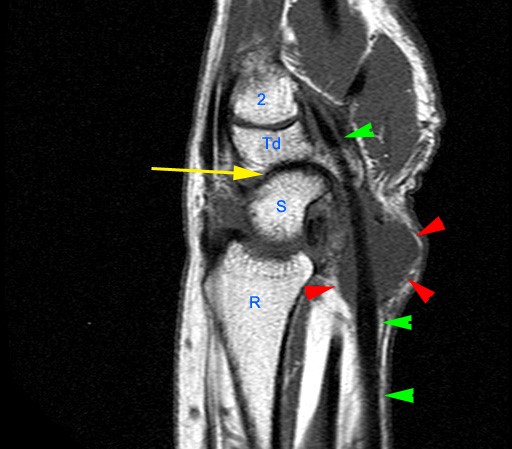
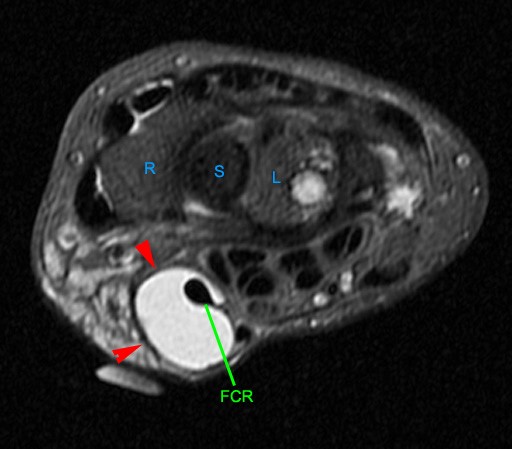
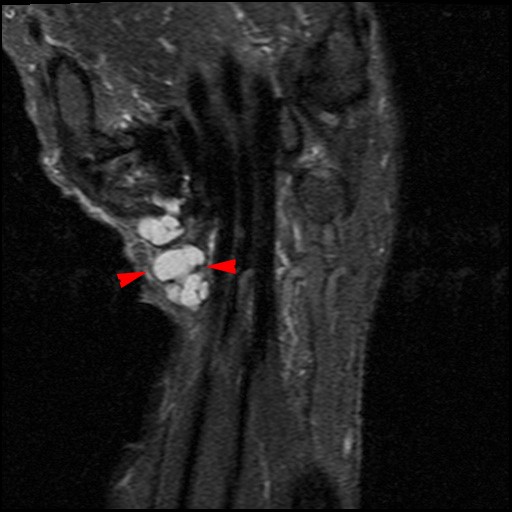
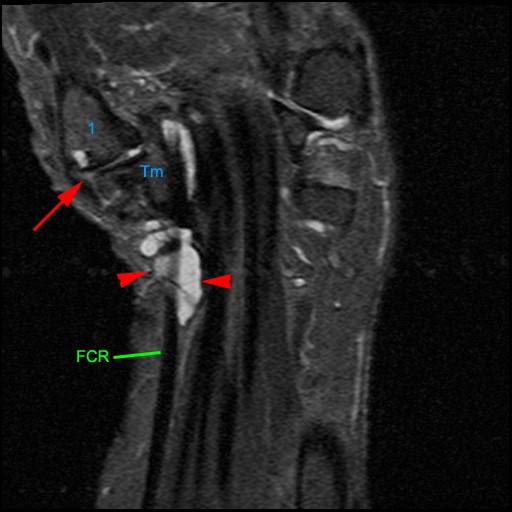
Figure 2:
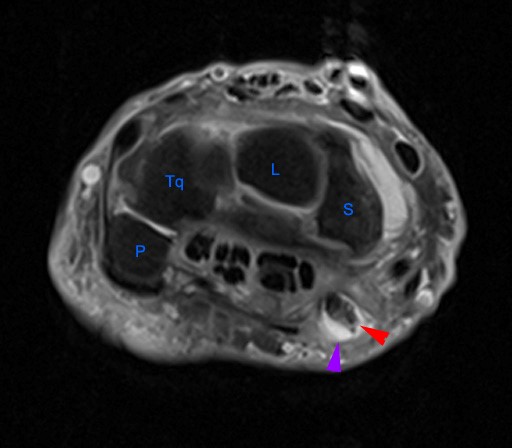
The axial image (2a) demonstrates a small rounded fluid collection (purple arrows) in the expected position of the flexor carpi radialis (FCR) tendon. The coronal (2b) and sagittal (2c) images reveal a completely torn FCR tendon (red arrowheads) retracted to the level of the distal radius. An intact segment of FCR tendon is visible more distally (green arrowheads) The second sagittal image (2d) reveals severe osteoarthritis involving the scaphotrapezial joint with irregular volarly projecting osteophytes (red arrows). U=ulna, R=radius, S=scaphoid, Td=trapezoid, 2=index metacarpal, Tm=trapezium.
Diagnosis
- Complete tear of the flexor carpi radialis tendon with proximal retraction.
- Severe osteoarthritis of the triscaphe joint.
Introduction
The flexor carpi radialis (FCR) muscle functions to flex and radially deviate the wrist. FCR tendinopathy is a relatively frequent cause of volar radial wrist pain, but is often unrecognized since it is usually overshadowed by pain from adjacent osteoarthritis with which it is commonly associated. This web clinic will review the anatomy, pathophysiology, and MRI diagnosis of FCR tendinopathy.
Anatomy
The FCR muscle originates at the medial epicondyle together with the flexor-pronator muscle mass. The muscle has a single tendon which courses in the volar radial portion of the distal forearm adjacent to the palmaris longus tendon. These two superficial tendons are visible on clinical exam just proximal to the wrist crease during resisted wrist flexion. At the wrist, the FCR tendon passes over the scaphoid and the scaphotrapeziotrapezoid (STT) joint (aka triscaphe joint) before entering its own fibro-osseous tunnel. The FCR tunnel is bounded volarly and laterally by the trapezial groove and dorsally by the trapezial tubercle (aka trapezial ridge). Medially, a retinacular septum separates the FCR tunnel from the carpal tunnel. Distal to the FCR tunnel the tendon angles deeply to reach its insertions. The primary insertion of the FCR tendon (80%) is onto the base of the second metacarpal. A secondary insertion (20%) is onto the base of the third metacarpal and a few fibers additionally insert on the trapezial tubercle. The FCR tendon is surrounded by a sheath from the level of the distal radius to the tendon insertion.
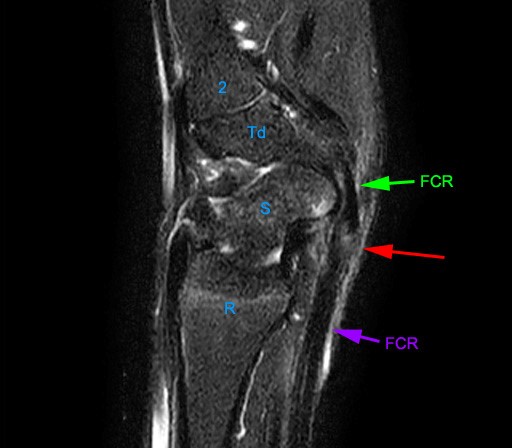
Figure 4:
Normal FCR tendon. Sagittal T1-weighted image. The FCR tendon (green arrowheads) enters the wrist and passes just volar to the distal pole of the scaphoid (S) before entering the FCR tunnel at the level of the trapezium (Tm). In the FCR tunnel it angles toward its primary insertion onto the base of the 2nd metacarpal (2). Td=trapezoid, R=radius.
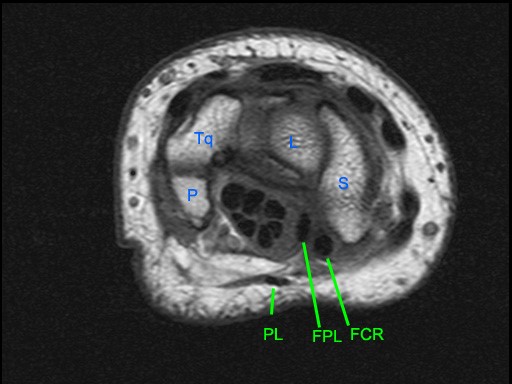
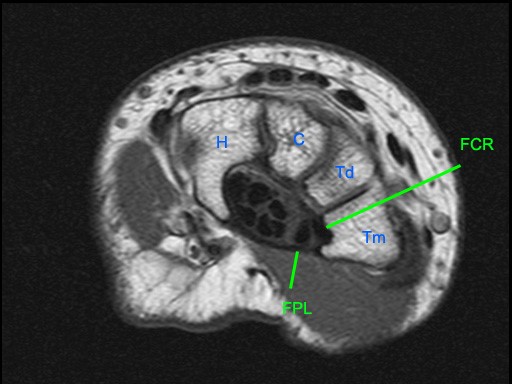
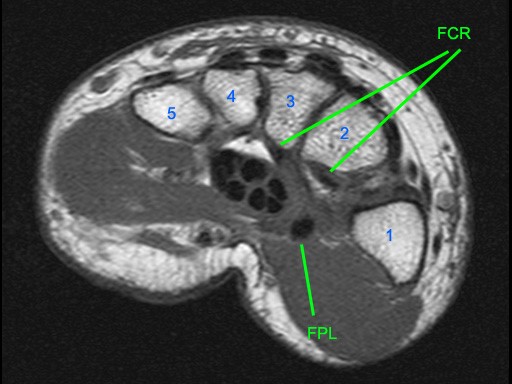
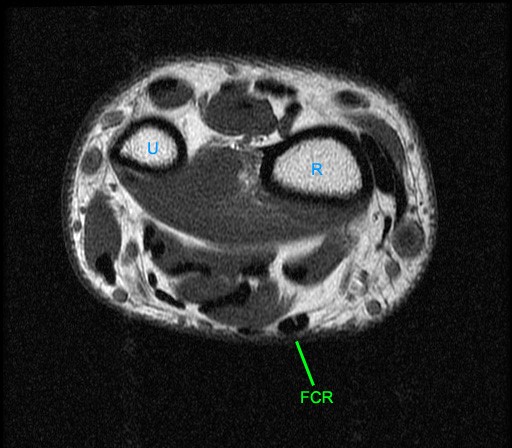
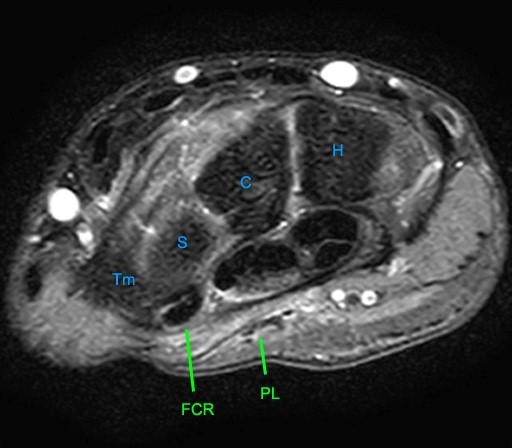
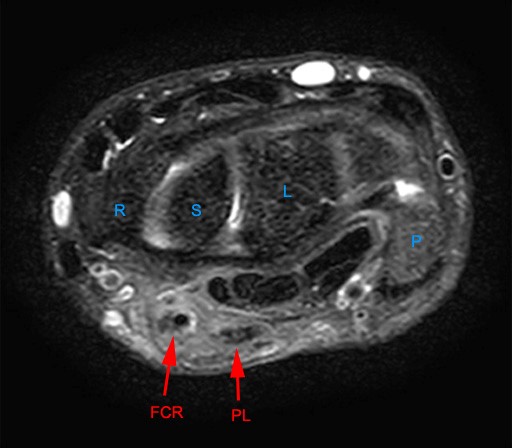
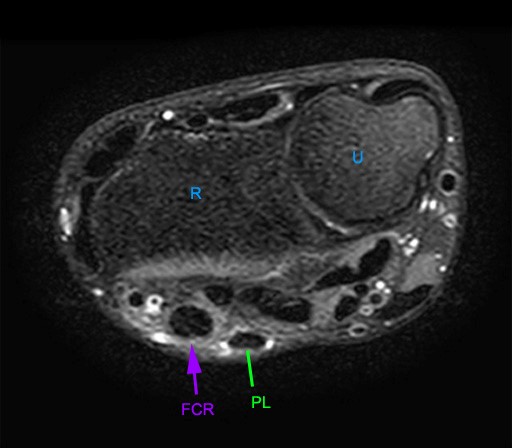
Figure 5:
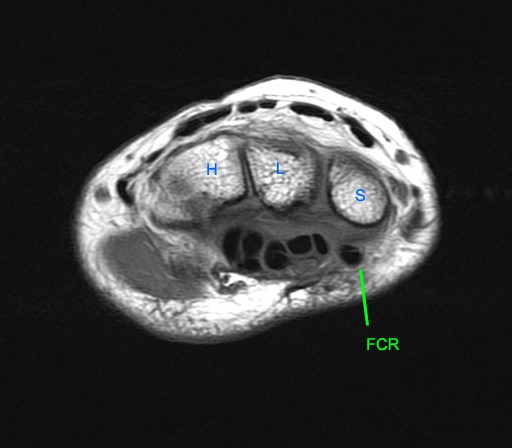
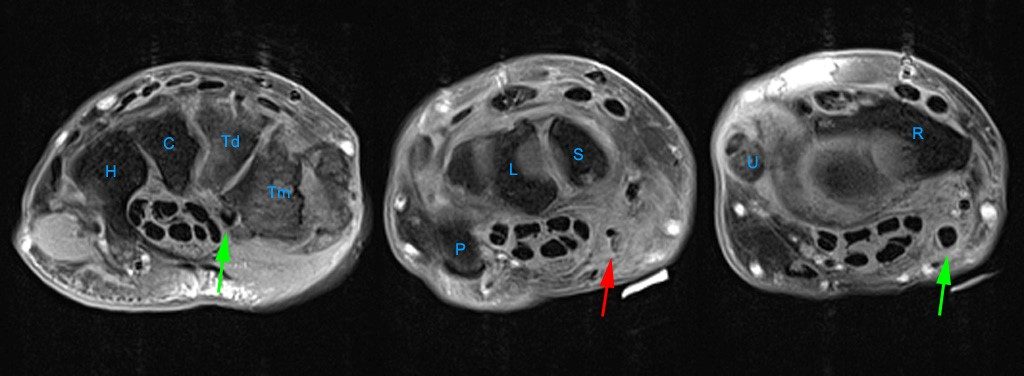
Axial images at the levels of the proximal carpal tunnel and pisiform (5a), mid carpal tunnel and scaphoid (5b), distal carpal tunnel and trapezoid (5c), and bases of the metacarpals (5d). Note the central group of FDP and FDS tendons and the peripheral locations of the FCR, FCU, and PL tendons. The FCU inserts onto the pisiform on the most proximal image. Note the close relations of the FCR with the FPL with which it may be confused. Note the FCR tendon passing along the volar margin of the scaphoid and within the FCR tunnel which is primarily comprised of the groove of the trapezium (Tm). A thin intermediate signal septum separates the FCR tunnel from the carpal tunnel and FPL. Distally the FCR tendon inserts primarily on the base of the 2nd metacarpal and to a smaller degree onto the base of the 3rd metacarpal. P=pisiform, Tq=triquetrum, L=lunate, S=scaphoid, H=hamate, C=capitate, Td=trapezoid, Tm=trapezium, 1-5=metacarpals.
The most frequent developmental anatomic variations of the FCR tendon are differing proportions at the tendon insertions, including partial to total attachment to the trapezium, or partial insertion onto other adjacent structures. The flexor carpi radialis brevis (FCRB) is an accessory muscle with a prevalence of 2.6% to 7.5%.1 The muscle origin is along the volar aspect of the distal radius and the insertion is on the base of the 2nd metacarpal. It is usually an asymptomatic incidental finding. Two reports have described pain from FCRB tenosynovitis.2,3 Another FCRB muscle presented as a painful forearm mass.4
Figure 6:
Flexor carpi radialis brevis – a normal anatomic variant. The intermediate signal intensity FCRB muscle is located deep to the position of the FCR tendon. On the sagittal image a thin low signal line separates the FCRB from the underlying lateral margin of the pronator quadratus (PQ) muscle. The axial image is at a position just distal to the pronator quadratus muscle. RNB=radial neurovascular bundle, R=radius, S=scaphoid, U=ulna.
Another potentially confusing normal variant appearance is a thin line of high signal occasionally seen within the proximal portions of the tendon on axial T1-weighted images. This is a normal finding that should not be misconstrued as a tear, especially in the absence of tenosynovitis or other abnormal findings. A similar appearance is often found in the extensor carpi ulnaris (ECU) tendon which has been shown to be normal fibrovascular tissue at histology.5 Isolated tendon signal changes without associated morphologic changes or tenosynovitis may be normal or from mild tendinosis and should be not be overestimated as a cause of symptoms.6
Pathophysiology
Tendon pathology most often develops from chronic overuse, especially in areas exposed to rough surfaces. Since the FCR tendon passes immediately adjacent to the trapezium and the STT joint, it is vulnerable to injury by cortical irregularities of these structures. These may develop in the event of fracture malunion7 or more often from joint degeneration.8,9
While the thumb carpometacarpal (CMC) joint (aka basal joint) is the most common site of osteoarthritis (OA) in the upper extremity, osteoarthritis also very common at the scaphotrapeziotrapezoid (STT) joint. Over time, the tendon may develop surface fraying, degeneration (tendinosis), and tearing. Pain is typically chronic in this area from the underlying arthritis. With progressive tendinopathy, patients may develop worsening of pain or a snapping sensation. Clinical exam may reveal point tenderness along the FCR tendon at the level of the wrist crease, especially with resisted flexion and radial deviation. Diagnosis can be confirmed by relief of symptoms following injection of lidocaine into the tendon sheath.
Figure 8:
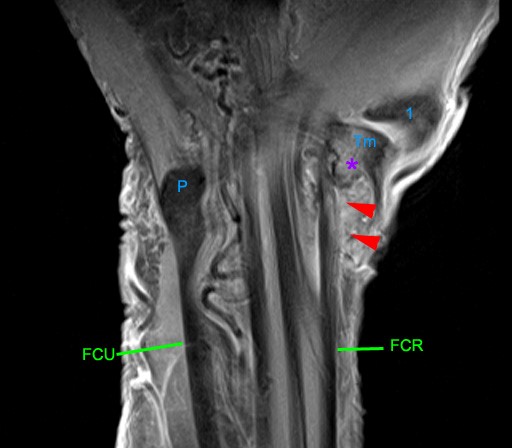
Tendinosis & tenosynovitis, surface fraying, early partial tearing of the FCR tendon. 81-year-old with persistent volar radial wrist pain over 9 months, exacerbated by lifting. Two prior cortisone injections. Surface irregularity, signal changes and caliber change involve the FCR tendon (red arrowheads). Fluid distends the surrounding tendon sheath from associated tenosynovitis (purple arrowhead). The trapezium (Tm) demonstrates reactive marrow edema (asterisk) and degenerative cortical irregularity. P=pisiform, Tq=triquetrum, L=lunate, S=scaphoid, Tm=trapezium, 1=thumb metacarpal.
Figure 9:
High grade partial tear of the FCR tendon. 67-year-old with chronic volar radial wrist pain and swelling. A markedly reduced caliber partially torn and irregular FCR tendon (red arrow) is found at the site of clinical symptoms as indicated by a marker on the skin surface. The FCR tendon (green arrows) is normal in caliber at the level of the trapezium (Tm) and at the distal radius (R). The coronal image demonstrates severe osteoarthritis at both the thumb CMC and the STT joints. S=scaphoid, Tm=trapezium, 1=thumb metacarpal.
FCR tendinopathy rarely occurs in isolation, but can be caused by repetitive wrist flexion or overstretching, as with sports such as golf, racquet sports, volleyball or water polo,10 or with occupations involving repeated wrist flexion. Overuse injury may be exacerbated by constriction in the FCR tunnel, although most often the underlying mechanism of injury is irritation from STT osteophytes.
Synovial processes such as rheumatoid arthritis11 or PVNS involving the STT joint may involve the adjacent FCR tendon sheath. A tendon chronically weakened by mechanical attrition or rheumatoid arthritis can spontaneously rupture during a relatively minor strain such as while lifting an object.12 Tendon rupture is even more frequent among patients who have received corticosteroid injections at the site.13,14,15 After rupture, the retracted tendon and muscle may form a palpable forearm lump. Partially regenerated “pseudotendon” or “neotendon” can form in or adjacent to the tear site. This has relatively disorganized collagen and is weaker than native tendon. It is also often symptomatic, with pain thought to be secondary to tethering.15,16
Figure 10:
Partial FCR tendon tear and tenosynovitis. 71-year-old tennis player with volar radial wrist pain for 6 months. A marker overlies the site of pain and swelling. Increased signal is seen on the axial images at the deep aspect of the tendon from tendinosis and partial tearing (red arrows). Surrounding fluid from associated tenosynovitis. Relatively little chondral loss is visible at the STT joint, but cortical irregularity (yellow arrowheads) is present along the volar cortex of the distal pole of the scaphoid (S), impinging on the overlying FCR tendon (red arrowheads).
Mild to moderate tenosynovitis often accompanies tendinopathy, but may be present in isolation. Ganglion cysts may also develop.
Figure 11:
Severe tenosynovitis with underlying STT OA. 64-year-old with wrist pain and palpable lump. The FCR tendon sheath is profoundly distended (red arrowheads) proximal to the FCR tunnel. STT osteoarthritis is present with full-thickness cartilage loss and subchondral sclerosis (yellow arrow). Marginal osteophytes were also present on other image slices.
Figure 12:
Ganglion cyst. 81-year-old with painful mass and pain in the palm and base of the thumb. A large lobulated ganglion cyst (red arrowheads) arises from the FCR tendon sheath and partially surrounds the tendon. Severe osteoarthritis involves the thumb CMC joint (red arrow). Mild osteoarthritis was present at the STT joint (not shown). (Tm=trapezium, 1=thumb metacarpal)
The FCR tendon can be a site of hydroxyapatite deposition disease (HADD) although deposition in the adjacent STT joint capsule appears to be more common in our experience. As with other wrist tendons, acute injuries may also occur from laceration or strain.
Figure 13:
Tendon lacerations. 17-year-old with pain since a fall onto glass one month ago. The FCR tendon is irregularly diminished in caliber at the level of the proximal carpal row from high-grade partial laceration. High-grade partial laceration also involves the adjacent palmaris longus (PL) at the same level. Focal laceration of the FCR tendon is also visible on the sagittal image (red arrow). The FCR tendon is normal distal to the laceration site (green arrow). Proximal to the laceration site the tendon appears thickened (purple arrow), possibly related to partial regeneration or “pseudotendon” formation.
Treatment
Initial treatment of FCR tendinopathy is typically conservative and may include splint immobilization, activity modification, and/or NSAIDs. Steroid injection into the tendon sheath is effective for many patients, particularly those with primary tenosynovitis. However, it is less effective for tendinopathy secondary to osteoarthritis and may further weaken the tendon and predispose it to rupture.
FCR tunnel release (tenolysis) is effective for cases related to constriction in the tunnel, but less so for patients with underlying osteoarthritis. The retinacular septum is opened, taking special care to not injure the adjacent median nerve branch to the thumb.17 In refractory cases, tenotomy may be performed, suturing the tendon stump side to side to the adjacent palmaris longus tendon.
Some patients with complete rupture have spontaneous pain resolution over time, with minor residual deficits after splinting and physiotherapy18 Others have disabling pain, postulated to be from the tethering effect of pseudotendon formation after tendon stump retraction. Excision of the pseudotendon and stump in 6 patients achieved full pain relief.15 Debridement of the reactive synovitis at the tendon ends has also been reported to be effective.
Other flexor tendon injuries
Digital flexor tendon injuries were discussed in detail in a previous MRI web clinic. These are most frequently open injuries from lacerations, which are most often located at the level of the proximal phalanx (zone II). Among closed flexor tendon injuries, the most common is acute traumatic avulsion of the flexor digitorum profundus (FDP) tendon at its insertion on the distal phalanx, i.e. “jersey finger.” More proximal injuries include closed rupture of the flexor pollicis longus (FPL) tendon at the level of the carpal tunnel (Mannerfelt Syndrome), with an underlying attritional mechanism similar to that of FCR tendon injuries. Also, closed proximal (palm or wrist level) ruptures of the FDP have been described following nonunion of hamate hook fractures or from irritation by a rough surface on the radial side of the hamate hook19 Other significant underlying factors predisposing to midtendon ruptures include rheumatoid arthritis and gout.
The flexor carpi ulnaris (FCU) tendon can be injured by laceration or strain such as in a fall. Symptomatic degenerative tendinosis can develop from chronic overuse, especially at the palmar aspect of the tendon insertion onto the pisiform.20 FCU tendinopathy that does not respond to conservative treatment has been successfully treated with debridement.21
Conclusion
FCR tendinopathy is an underrecognized cause of volar radial wrist pain. It is most frequently secondary to underlying STT osteoarthritis, which may also confound the clinical diagnosis. MRI is effective for diagnosis of this entity and underlying conditions, especially when clinical signs are inconclusive.
References
- Nakahashi T, Izumi R. Anomalous interconnection between flexor and extensor carpi radialis brevis tendons. Anat Rec. 1987;218(1):94–97. https://www.ncbi.nlm.nih.gov/pubmed/3605665 ↩
- Kosiyatrakul A, Luenam S, Prachaporn S. Symptomatic flexor carpi radialis brevis: case report. J Hand Surg Am. 2010 Apr;35(4):633-5. doi: 10.1016/j.jhsa.2009.12.028. Epub 2010 Feb 24. ↩
- Smith J, Kakar S. Combined flexor carpi radialis tear and flexor carpi radialis brevis tendinopathy identified by ultrasound: a case report. 2014 Oct;6(10):956-9. doi: 10.1016/j.pmrj.2014.04.005. Epub 2014 Apr 18. https://www.ncbi.nlm.nih.gov/pubmed/24751680 ↩
- Peers SC, Kaplan FT. Flexor carpi radialis brevis muscle presenting as a painful forearm mass: case report. J Hand Surg Am. 2008; 33(10):1878–1881. https://www.ncbi.nlm.nih.gov/pubmed/19084194 ↩
- Pfirrmann C, Zanetti M. Variants, pitfalls, and asymptomatic findings in wrist and hand imaging. Eur J Radiol. 2005;56:286–95. doi: 10.1016/j.ejrad.2005.03.010. https://www.ncbi.nlm.nih.gov/pubmed/16298674 ↩
- Stoop N, van der Gronde BATD, Janssen SJ, Kuntz MT, Ring D, Chen NC. Incidental Flexor Carpi Radialis Tendinopathy on Magnetic Resonance Imaging. Hand (N Y). 2018 Feb 1:1558944718760033. doi: 10.1177/1558944718760033. http://journals.sagepub.com/doi/abs/10.1177/1558944718760033 ↩
- Soejima O, Iida H, Naito M. Flexor carpi radialis tendinitis caused by malunited trapezial ridge fracture in a professional baseball player. J Orthop Sci. 2002, 7: 151–3. https://www.ncbi.nlm.nih.gov/pubmed/11819149 ↩
- Luong DH, Smith J, Bianchi S. Flexor carpi radialis tendon ultrasound pictorial essay. Skeletal Radiol. 2014 Jun;43(6):745-60. https://www.ncbi.nlm.nih.gov/pubmed/24658615 ↩
- Parellada AJ, Morrison WB, Reiter SB, et al. Flexor carpi radialis tendinopathy: spectrum of imaging findings and association with triscaphe arthritis. Skelet Radiol. 2006;35:572–578. doi: 10.1007/s00256-006-0116-2. https://www.ncbi.nlm.nih.gov/pubmed/16570175 ↩
- Avery DM, Rodner CM, Edgar CM. Sports-related wrist and hand injuries: a review. J Orthop Surg Res. 2016; 11: 99. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5025579/ ↩
- Moore JR, Weiland AJ, Valdata L. Tendon ruptures in the rheumatoid hand: Analysis of treatment and functional results in 60 patients. J Hand Surg Am. 1987, 12: 9–4. https://www.nbi.nlm.nih.gov/pubmed/3805649 ↩
- Verellen K, Dauwe D, Demuynck M, et al. Spontaneous ruptures of the flexor carpi radialis tendon secondary to STT osteoarthritis. Acta Orthop Belg. 1992;58(4):474-476. https://www.ncbi.nlm.nih.gov/pubmed/1485518 ↩
- Yamada K, Masuko T, Iwasaki N. Rupture of the flexor digitorum profundus tendon after injections of insoluble steroid for a trigger finger. J Hand Surg Eu. 2011, 36:77-78. http://journals.sagepub.com/doi/abs/10.1177/1753193410382377 ↩
- Tonkin MA, Stern HS. Spontaneous rupture of the flexor carpi radialis tendon. J Hand Surg Br. 1991 Feb;16(1):72-4. https://www.ncbi.nlm.nih.gov/pubmed/2007820 ↩
- Henry M. Pseudotendon formation causing painful tethering of ruptured flexor carpi radialis tendons. J Hand Microsurgery. 2013, 5: 1–3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3650158/ ↩
- Van Demark RE, Helsper E, Hayes M, Hayes M, Smith V. Painful Pseudotendon of the Flexor Carpi Radialis Tendon: A Literature Review and Case Report. Hand (N Y). 2017 Sep;12(5):NP78-NP83. doi: 10.1177/1558944716672196. Epub 2016 Oct 3. https://www.ncbi.nlm.nih.gov/pubmed/28832214 ↩
- Brink PR, Franssen BB, Disseldorp DJ. A simple blind tenolysis for flexor carpi radialis tendinopathy. Hand (NY) 2015;10(2):323–7. doi: 10.1007/s11552-014-9631-0. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4447664/ ↩
- Kanevsky J, Zammit D, Brutus JP. Rupture of the flexor carpi radialis tendon secondary to trauma: case report and literature review. Plast Aesthet Res 2015;2:138-9. http://parjournal.net/article/view/488 ↩
- Kim YJ, Baek JH, Park JS, Lee JH. Interposition Tendon Graft and Tension in the Repair of Closed Rupture of the Flexor Digitorum Profundus in Zone III or IV. Ann Plast Surg. 2018 Mar;80(3):238-241. doi: 10.1097/SAP.0000000000001240. https://www.ncbi.nlm.nih.gov/pubmed/29095192 ↩
- Kofman KE, Schuurman AH, Mulder MC, Verlinde SAMW, Gierman LM, van Diest PJ, and Bleys RLAW. The Pisotriquetral Joint: Osteoarthritis and Enthesopathy. J Hand Microsurg. 2014 Jun; 6(1): 18–25. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4037443/ ↩
- Budoff JE, Kraushaar BS, Ayala G. Flexor carpi ulnaris tendinopathy. J Hand Surg (Am) 2005;30(1):125–129. doi: 10.1016/j.jhsa.2004.07.018. [https://www.ncbi.nlm.nih.gov/pubmed/15680567 ↩