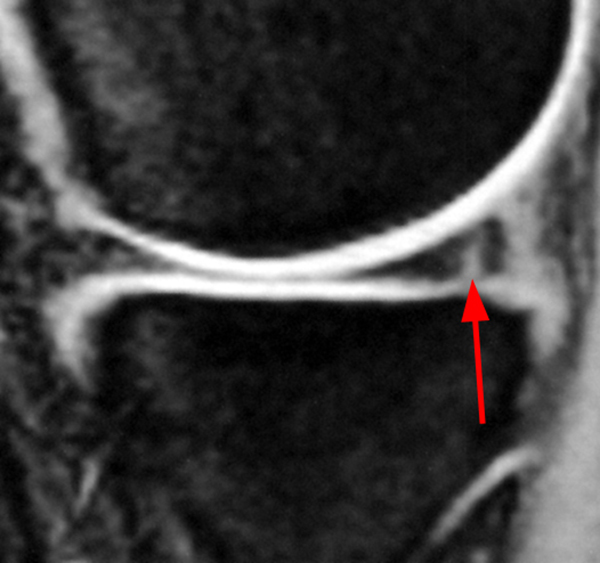
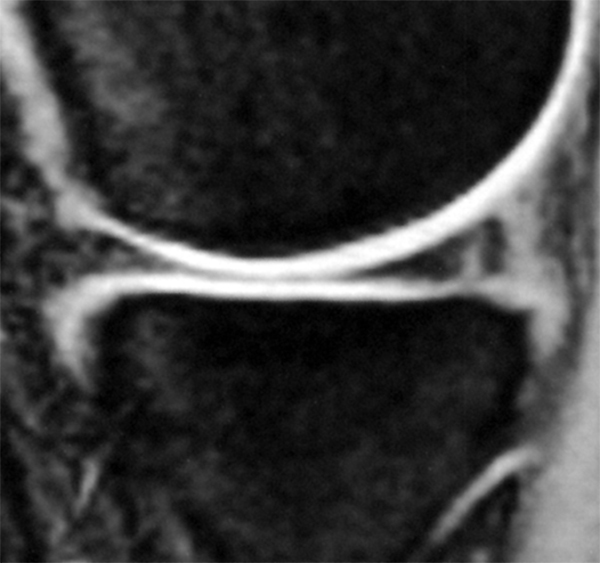
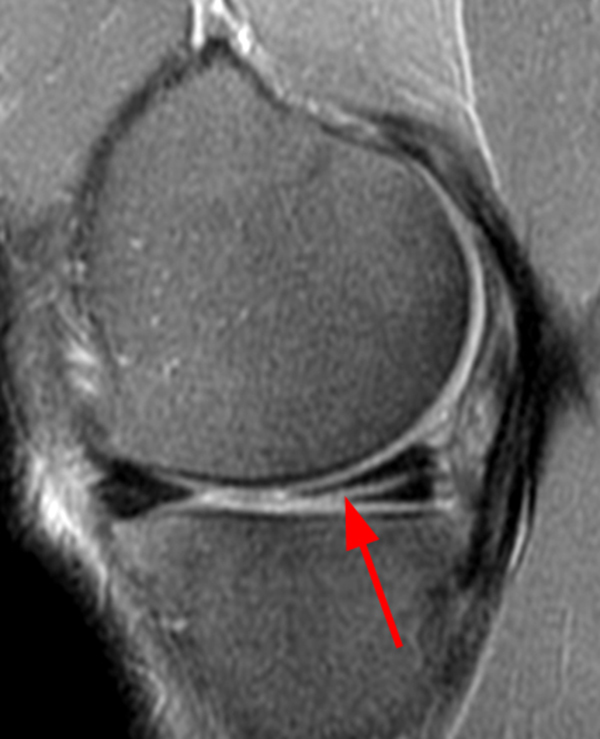
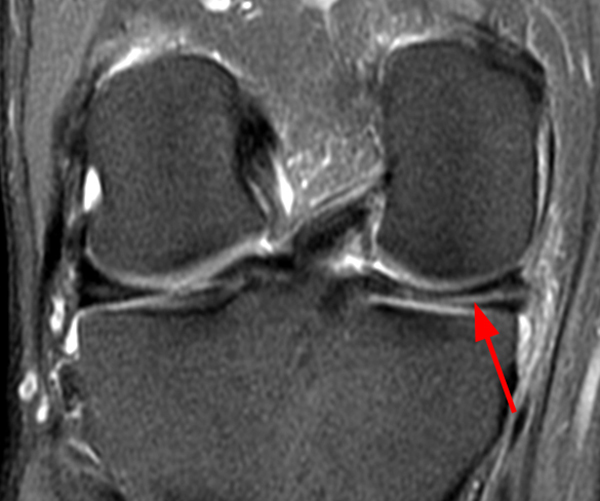
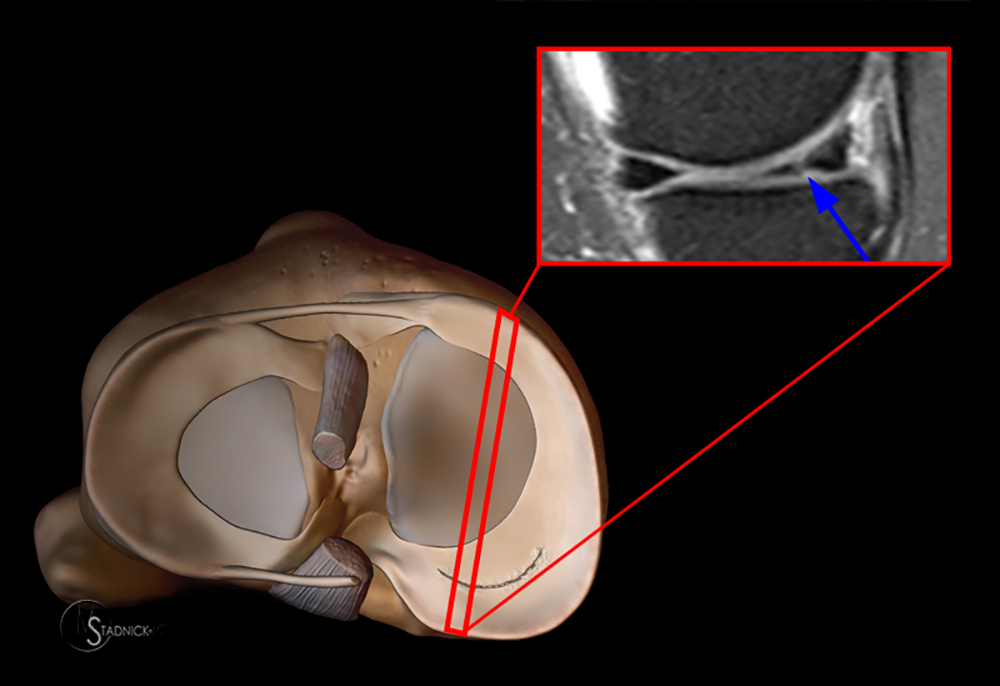
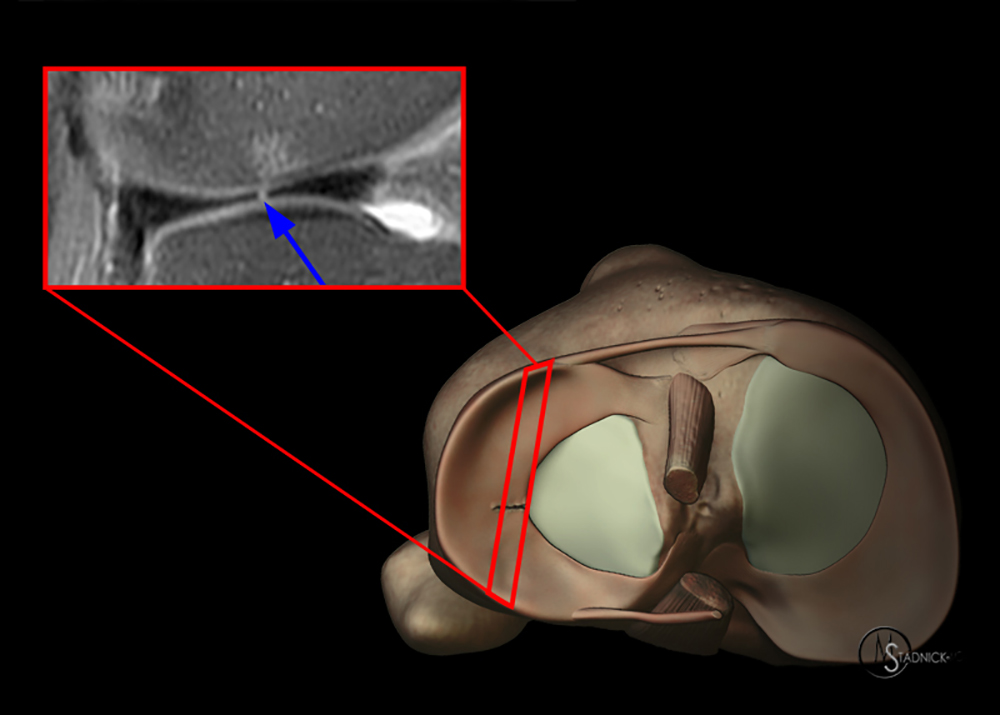
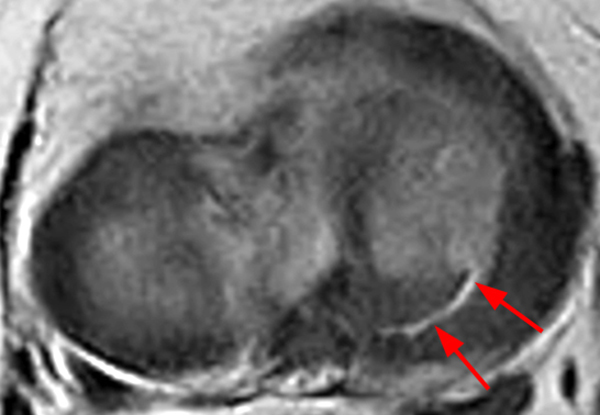
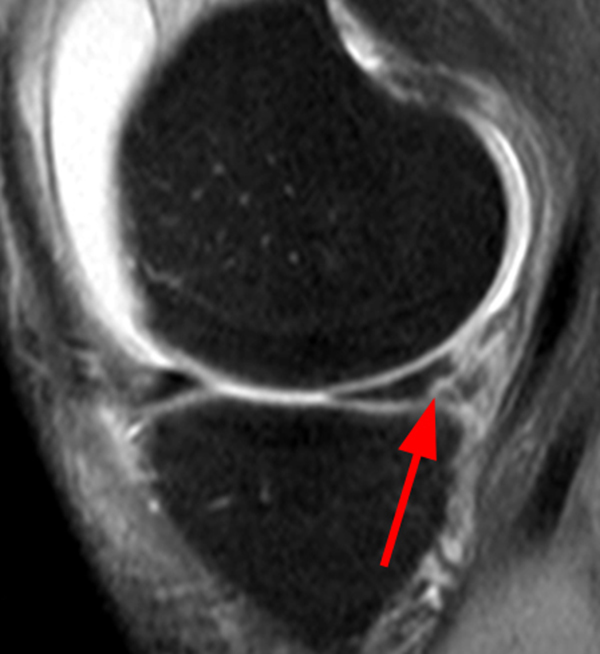
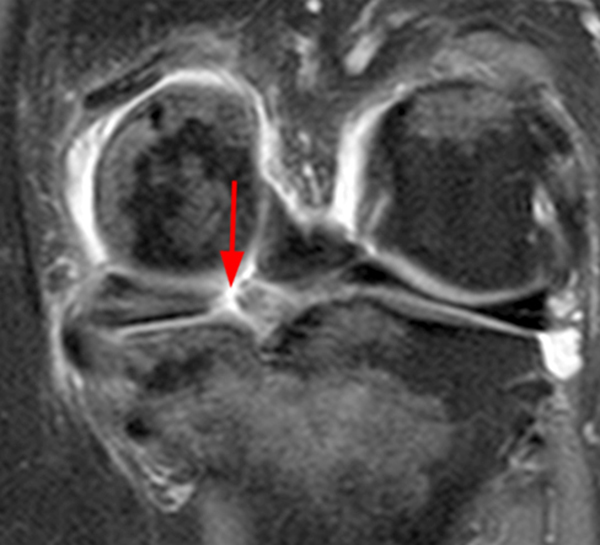
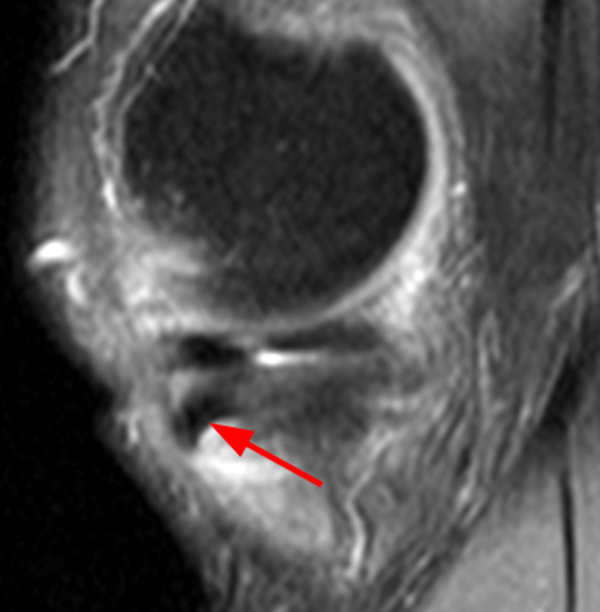
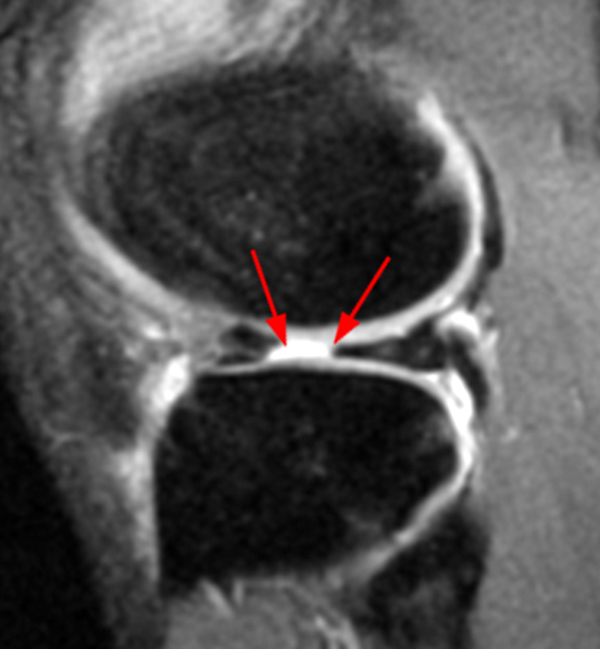
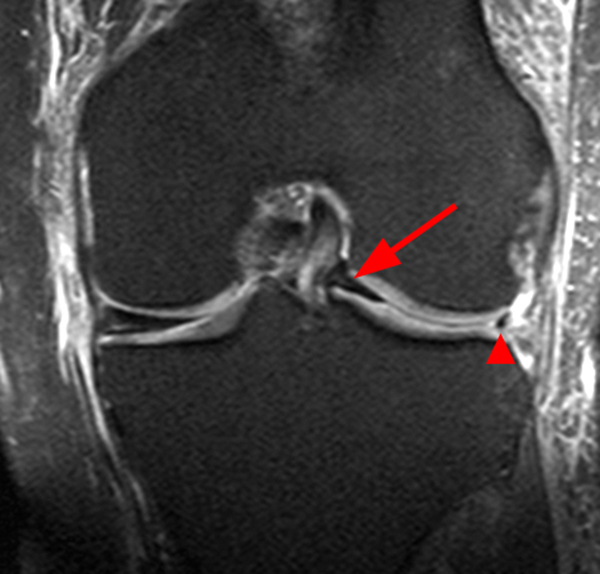
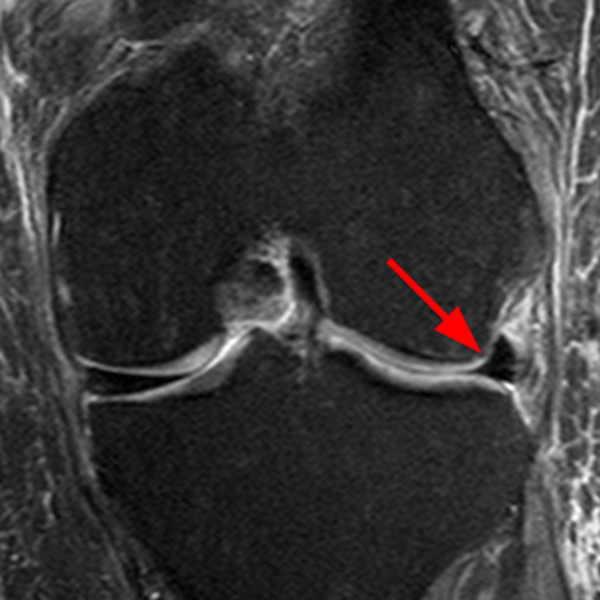
A gradient-echo T2*-weighted sagittal image demonstrates a tear within the posterior horn of the medial meniscus (arrow). The preferred nomenclature for this tear pattern is:
A. Radial Tear
B. Horizontal Tear
C. Vertical Tear
D. Longitudinal Tear
E. Oblique Tear
Answer
Although C, a vertical tear, is commonly used to describe such an appearance, the better answer is D, a longitudinal tear. Even better would be to describe a peripheral longitudinal tear extending to the tibial surface within the posterior horn of the medial meniscus!
Introduction
Long ago, the menisci were felt to be vestigial structures that served no useful purpose in humans.1 Of course, we now realize that the menisci are vital structures that play a key role in the normal biomechanical function of the knee. Because of their importance and the clinical impact of meniscal tears, assessment of the menisci has become the most common indication for MR of the knee. In the early days of MR, it was often felt that the role of MR was simply to identify whether a tear was present or not, and treatment of meniscal tears was largely composed of operative resection. With the realization that even partial meniscectomy leads to accelerated osteoarthritis,2 surgeons have increasingly turned to meniscal repair. Not all meniscal tear types, however, are amenable to repair, and thus an accurate description of meniscal tears on MR can have a dramatic impact on preoperative planning.
Meniscal Anatomy
The menisci are C-shaped fibrocartilages with concave upper surfaces and flat undersides that match their respective interfaces with the femoral condyles and tibial plateau. The lateral meniscus has a symmetrical C-shape, whereas the medial meniscus is more crescentic (3a), as the posterior horn of the medial meniscus is always larger than the anterior horn. The medial meniscus has a firmer capsular attachment than the lateral meniscus. This makes the medial meniscus less mobile and is one reason why the medial meniscus is more prone to injury.3 In adults, only the periphery of the meniscus remains vascularized. This region of the outer meniscus, sometimes referred to as the “red zone”, is thought to occupy approximately 15% of the peripheral meniscus.4 Tears that occur within the red zone of the meniscus are more likely to heal than those in the avascular, “white zone” of the meniscus. Tears that lie within or contact the red zone are also more likely to be amenable to meniscal repair. Currently, routine MR images do not reveal signal intensity differences between the red and white zones of the menisci.
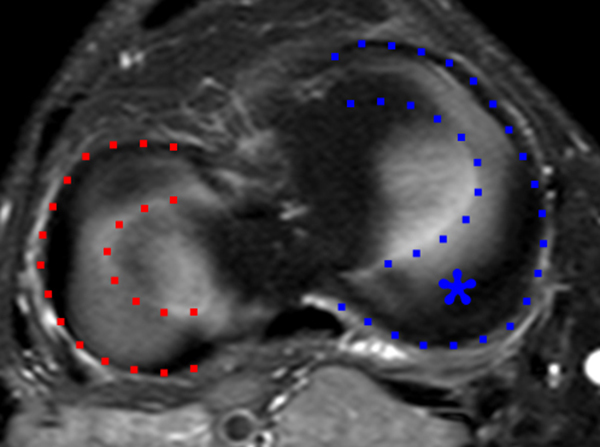
Figure 3:
(3a) A fat-suppressed proton density-weighted axial image through the knee joint demonstrates the C-shaped menisci. Not the symmetrical shape of the lateral meniscus (red outline) and the asymmetry of the medial meniscus (blue outline), where the posterior horn (asterisk) is significantly larger than the anterior horn.
Meniscal Tear Description
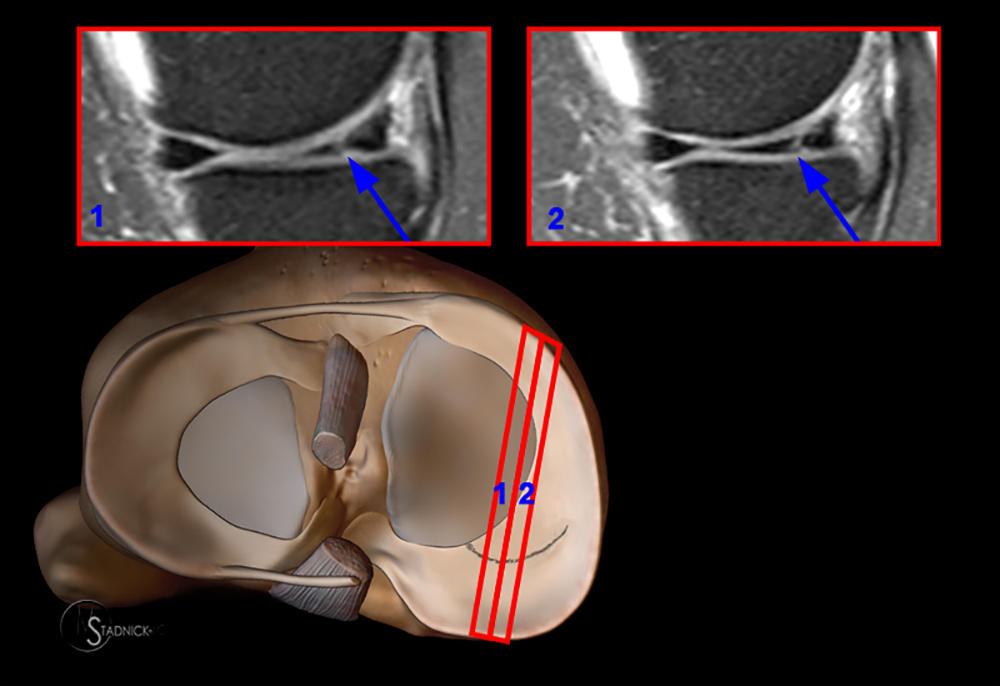
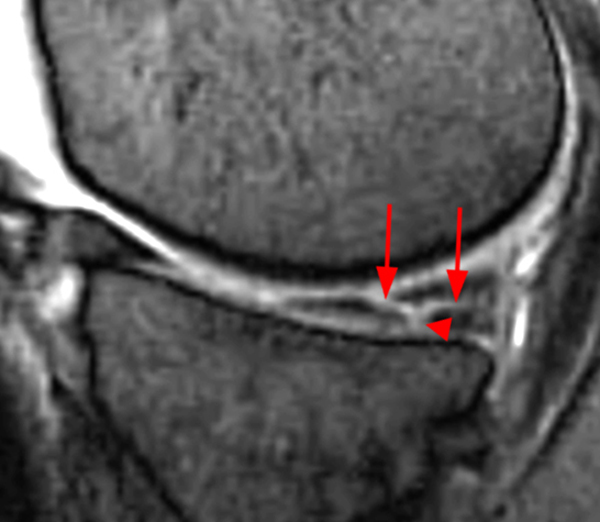
Meniscal tears may be categorized into five common configurations, including horizontal, longitudinal, radial, oblique (parrot-beak), and complex.5 Horizontal tears, the most common meniscal tear pattern, lie parallel to the tibial plateau and separate the meniscus into upper and lower parts (4a,4b). Both longitudinal and radial tears may appear vertical on MR images (5a,6a), but longitudinal tears extend parallel to the c-shaped circumference of the meniscus, whereas radial tears lie perpendicular to the meniscal circumference. Because these two tear patterns differ greatly in prognosis and treatment approach, vertical is therefore not the preferred descriptor for such meniscal tears, unless paired with the proper category, such as “vertical longitudinal”. An oblique tear (7a,8a) is often referred to as a parrot-beak tear, as the tear shape resembles a parrot’s beak. Oblique tears combine features of radial and longitudinal tears in that they lie perpendicular to the free edge of the meniscus but then curve such that a portion of it lies parallel to the c-shaped fibers of the meniscus.
Figure 8:
(8a) The curvilinear course of oblique tears often results in abnormal vertical signal (arrows) that progresses towards or away from the free edge of the meniscus on consecutive images, as seen in these sequential images of an oblique tear (arrows) of the posterior horn of the medial meniscus.
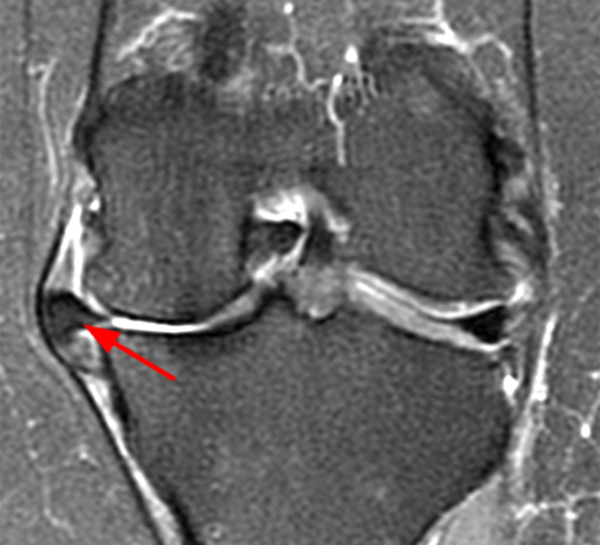
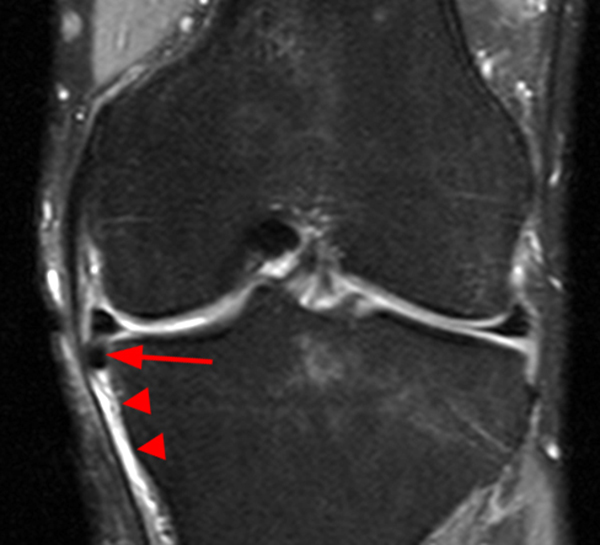
In addition to categorizing meniscal tears based on morphology, care should be taken to describe the exact location of meniscal tears. When appropriate, tears that appear to involve the periphery, or red zone of the meniscus, should be described as such (9a), thereby alerting the surgeon to the fact that the tear is more amenable to repair.
MR is also able to assess the stability of meniscal tears,6 an important factor, as unstable tears require operative treatment for symptom relief. Of course, if a displaced meniscal fragment is identified, the tear is by definition unstable. When displacement is not evident on MR images, additional criteria that suggest tear instability include the presence of fluid signal intensity within the tear on T2-weighted images, a tear that is greater than 10mm in length, and tears with complex patterns (10a).
Additional Meniscal Tear Types
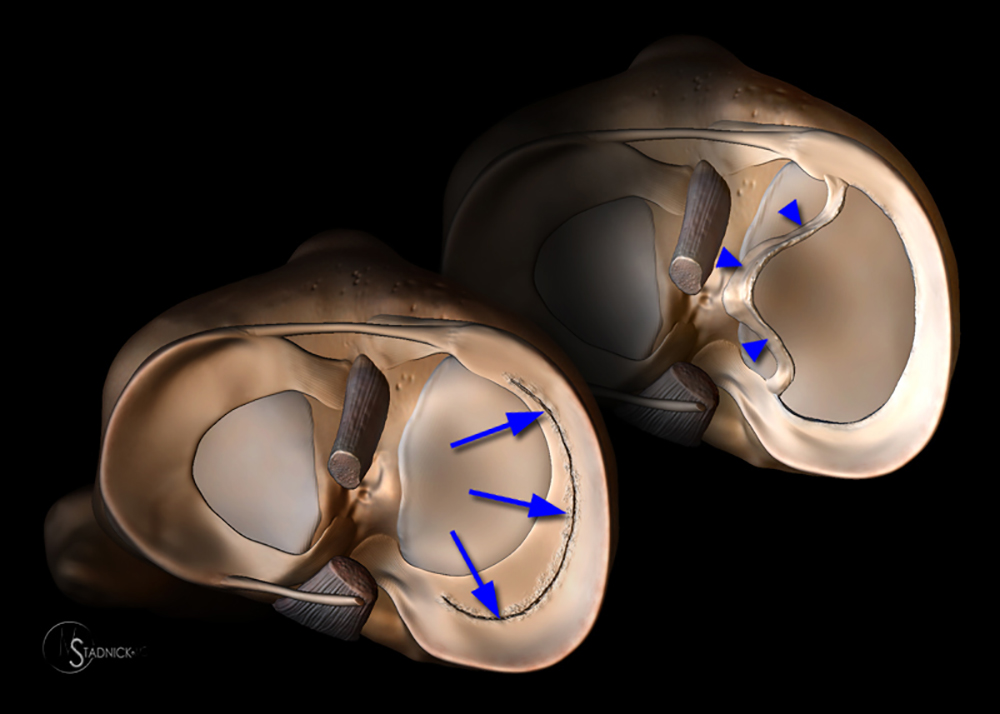
Several variations in meniscal tear patterns have been granted specific names that recognize the unique characteristics of the tear. Perhaps the best know of these is the bucket-handle tear. Bucket-handle tears are actually a form of longitudinal tear in which subsequent displacement of the inner rim of the tear results in a configuration that resembles the handle of a bucket (11a). These tears often occur in association with ACL tears, but even if found in isolation, are highly likely to be clinically relevant, as the displaced meniscal fragment frequently results in knee locking.
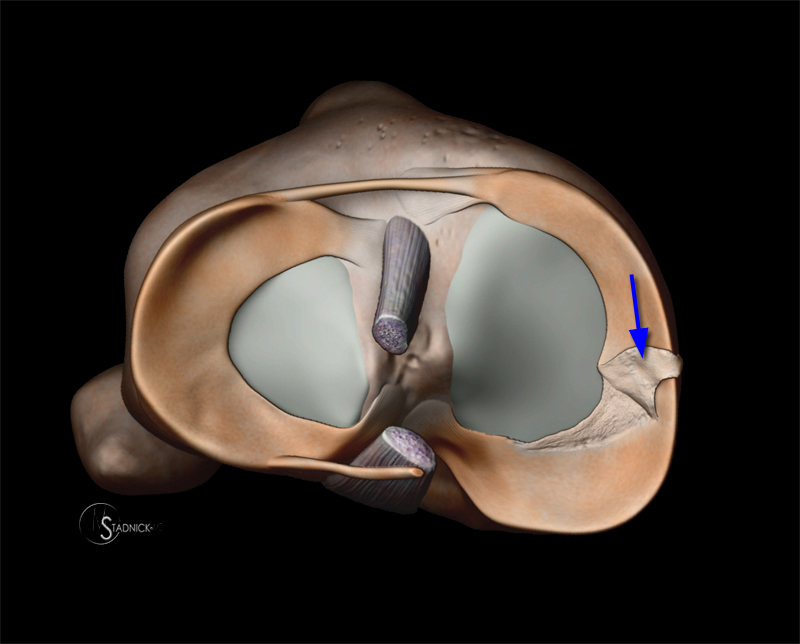
Figure 11:
(11a) A 3D illustration of a bucket handle tear demonstrates that these tears actually are longitudinal in nature (arrows), coursing parallel to the c-shaped fibers of the meniscus. Displacement of the inner rim of the tear (arrowheads) results in the classic "bucket-handle" configuration.
Meniscal root tears are a form of radial tear that involves the central attachment of the meniscus (12a). They are most frequently seen at the posterior horn of the medial meniscus. Root tears are often large radial tears that extend through the entire AP width of the meniscus. The loss of the central attachment of the posterior horn may allow extrusion of the body of the meniscus relative to the joint (13a). Additionally, the large radial tear dramatically undermines the ability of the meniscus to distribute hoop stress. Both of these factors increase contact forces across the joint, leading to accelerated osteoarthritis and predisposing the patient to the development of subchondral insufficiency fractures.7
A flap tear is a descriptive term that refers to a situation where the meniscus tears within its midsubstance, usually in a predominantly horizontal pattern, and then the upper or lower component of the torn meniscus becomes displaced from its site of origin (14a).8 These tears are most common at the medial meniscal body, and when displaced, the flap component may migrate into the superior or inferior meniscal gutter (15a,15b). These tears can be challenging to recognize on MRI,9 but are important to diagnose since they are often highly symptomatic due to a reactive synovitis. Arthroscopic treatment is typically required for adequate symptom relief in patients with displaced meniscal flap tears.
Figure 15:
Fat suppressed proton density-weighted (15a) coronal and (15b) sagittal images reveal a tibial sided flap tear of the body of the medial meniscus, with displacement of the undersurface component (arrows) into the inferior gutter. Reactive synovitis and edema (arrowheads) are readily apparent deep to the tibial collateral ligament on the coronal view.
Surgical Implications of Meniscal Tear Patterns
As recognition of the critical function of the menisci in normal biomechanical function of the knee has grown, attempts at preserving meniscal tissue via repair as opposed to partial meniscectomy have also gained favor. The operative equipment needs and post-operative rehabilitation process markedly differ between meniscal repair and partial meniscectomy. With meniscal repair, weight bearing may be severely limited for up to six weeks following surgery, and protection from heavy stress to the knee extends for up to six months. Meniscal repair is a more difficult surgical technique and requires a motivated, diligent patient in order to be successful. It is therefore quite important in treatment planning for the pre-operative MR to provide information that can be used to determine whether meniscal repair rather than partial meniscectomy is to be performed.
Although some reports have described successful repair of the avascular portion of the meniscus,11 it is generally accepted that meniscal repair is more likely to be successful if it involves or at least communicates with the meniscal red zone, lying within three to four millimeters of the capsular rim.12 A basic principle of meniscal repair is to rasp the tear edges and the parameniscal synovium above and below the meniscus, which is thought to enhance the vascular healing process. If a repair is attempted within meniscal tissue that is questionably vascular or non-vascular, healing enhancement techniques such as the use of fibrin clot and the creation of channels that communicate with the vascular zone may be utilized.10
With regard to tear morphology, the classic ideal candidate for meniscal repair is the peripheral longitudinal tear. Longitudinal tears do not disrupt the circumferential architecture of the meniscus, and thus repair of longitudinal tears leads to a meniscus with relatively normal biomechanical function. The tear should be eight millimeters or more in length, as shorter peripheral longitudinal tears are less likely to be symptomatic and may heal spontaneously. Radial tears, because they are oriented perpendicular to the c-shaped fibers of the meniscus, have a devastating effect upon meniscal function. Those that extend through the entire width of the meniscus are particularly harmful (16a,16b), and even if such tears appear stable following repair, they are unlikely to regain the ability to provide hoop stress to the meniscus.13 Radial tears have therefore classically been treated with partial meniscectomy, though evolving surgical techniques have led to successful reports of the repair of radial tears that communicate with the meniscal periphery.11 A recent report has even described the successful repair of radial tears of the medial meniscal root,14 utilizing a tibial tunnel through which sutures are placed in the avulsed meniscus, a technique similar to that used in patients undergoing meniscal transplantation.
Horizontal cleavage, oblique, and complex meniscal tear patterns have traditionally been poor candidates for meniscal repair. When small, conservative therapy or simply rasping the meniscus may result in healing of these tear types. Larger, unstable tears of this type often cause mechanical symptoms, however, and therefore warrant operative treatment, usually via partial meniscectomy. Repair is sometimes attempted even with these tear types, particularly when the patient is young and substantial loss of meniscal tissue would lead to an unacceptable risk of future arthritis.11 Repair of these challenging tear types should only be attempted when the meniscal tissue is of good quality and a stable result is achievable. Adjunctive measures to promote vascularity and healing at the repair sites are also recommended.
Meniscal repairs are more likely to be successful when performed near the time of injury. If an ACL tear is also present, meniscal repairs are more successful if the ACL is also repaired, likely due to the protection afforded by knee stability. Patients with ACL tears are also thought to be better candidates for meniscal repair because of the presence of serum-derived growth factors within the hemarthrosis that accompanies ACL tears.15
Displaced meniscal tears are by definition unstable, and should be repaired relatively quickly, as displaced meniscal fragments may fibrose and distort, making delayed repair difficult or impossible. The “best known” displaced tear that is amenable to repair is the bucket-handle tear. Although all bucket handle tears are repair candidates,16 the bucket handle tear is an example of when the more severe appearing tear is actually better for the patient. In other words, when the majority of the meniscus forms the “handle”, that requires tear formation near the meniscal periphery, resulting in a vascular site for operative repair. Repair of such lesions can result in dramatic clinical as well as MR imaging results (17a,17b).
Figure 17:
Fat-suppressed coronal images demonstrate before and after images following repair of a bucket handle tear. In (17a), the preoperative study, a large displaced "handle" (arrow) from the body of the lateral meniscus is seen near the intercondylar notch. Only a small peripheral rim of meniscal tissue (arrowhead) is present at the native site of the lateral meniscus. Two months later, the post-operative image (17b) reveals a repaired, normal appearing lateral meniscal body (arrow), with resolution of the previously seen displaced fragment.
Conclusion
The skilled interpreter of MR of the knee must do more than simply identify the presence of a meniscal tear. Tears should be characterized with regard to morphology, size, location, and stability, all of which are important factors that may influence the choice of operative treatment. As orthopaedic surgeons increasingly consider meniscal repair, accurate pre-operative assessment with MR becomes more important, allowing proper planning on the part of both the surgeon and the patient.
We’re America’s trusted radiologists and hospital PACS software company. Download our web clinic below!
References
1 Sutton JB. Ligaments: their nature and morphology. 2nd ed. London;1897.
2 Jaureguito JW, Elliot JS, Lietner T. The effects of arthroscopic partial lateral meniscectomy in an otherwise normal knee: a retrospective review of functional, clinical, and radiographic results. Arthroscopy. Feb 1995;11(1):29-36.
3 Thornton DD, Rubin DA. Magnetic resonance imaging of the knee menisci. Semin Roentgenol. Jul 2000;35(3):217-30.
4 Hauger O, Frank LR, Boutin RD, et al. Characterization of the “red zone” of knee meniscus: MR imaging and histologic correlation. Radiology 2000; 217:193-200.
5 Jee WH, McCauley TR, Kim JM, et al. Meniscal tear configurations: categorization with MR imaging. AJR 2003; 180:93-97.
6 Vande Berg BC, Poilvache P, Duchateau F. Lesions of the menisci of the knee: value of MR imaging criteria for recognition of unstable lesions. AJR 2001; 176:771-776.
7 Yao L, Stanczak J, Boutin RD. Presumptive subarticular stress reactions of the knee: MRI detection and association with meniscal tear patterns. Skeletal Radiology 2004; 33:260-264.
8 Ruff C, Weingardt J, Russ P, Kilcoyne R. MR imaging patterns of displaced meniscus injuries of the knee. AJR 1998;170:63-67.
9 Lecase LK, Helms CA, Kosarek FJ, Garret WE. Inferiorly displaced flap tears of the medial meniscus: MR appearance and clinical significance. AJR 2000; 174:161-164.
10 DeHaven KE. Meniscus Repair. AJSM 1999; 27:242-250.
11 Noyes FR, Barber-Westin SD. Arthroscopic repair of meniscal tears extending into the avascular zone in patients younger than twenty years of age. AJSM 2002; 30:589-600.
12 McGinty JB, Burkhart SS, Jackson RW, et al. Operative Arthroscopy, 3rd Edition, 2002, Lippincott Williams and Wilkins.
13 Newman AP, Daniels AU, Burks RT. Principles and decision making in meniscal surgery. Arthroscopy. 1993;9(1):33-51.
14 Marzo JM, Kumar BA. Primary repair of medial meniscal avulsions: 2 case studies. AJSM 2007; 35:1380-1383.
15 Koski JA, Ibarra C, Rodeo SA. Meniscal injury and repair: clinical status. Orthop Clin North Am. Jul 2000;31(3):419-36.
16 O’Shea JJ, Shelbourne KD. Repair of locked bucket-handle meniscal tears in knees with chronic anterior cruciate ligament deficiency. AJSM 2003; 31:216-220.