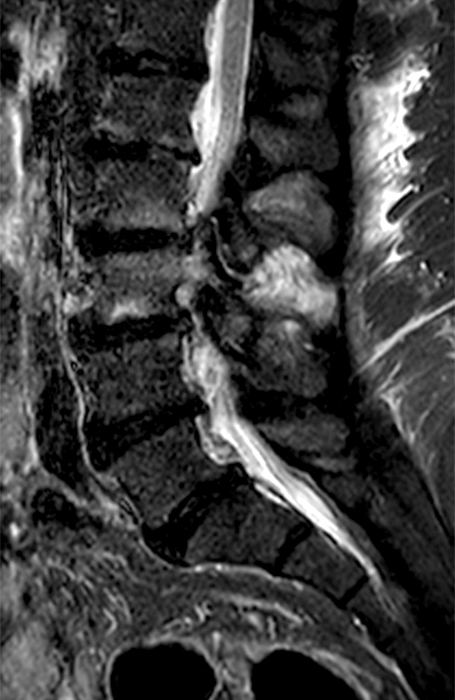
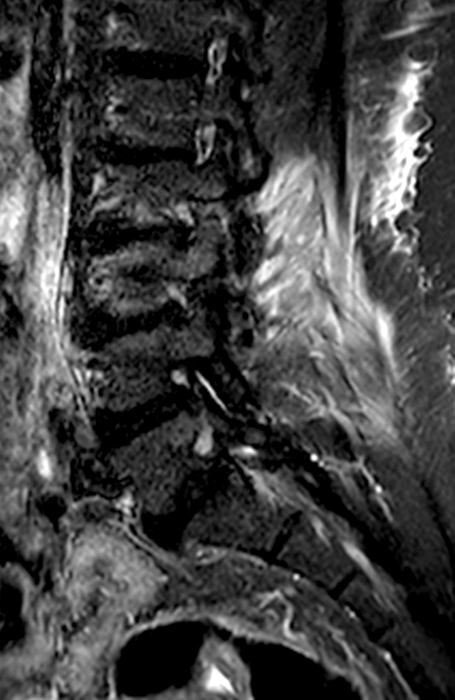
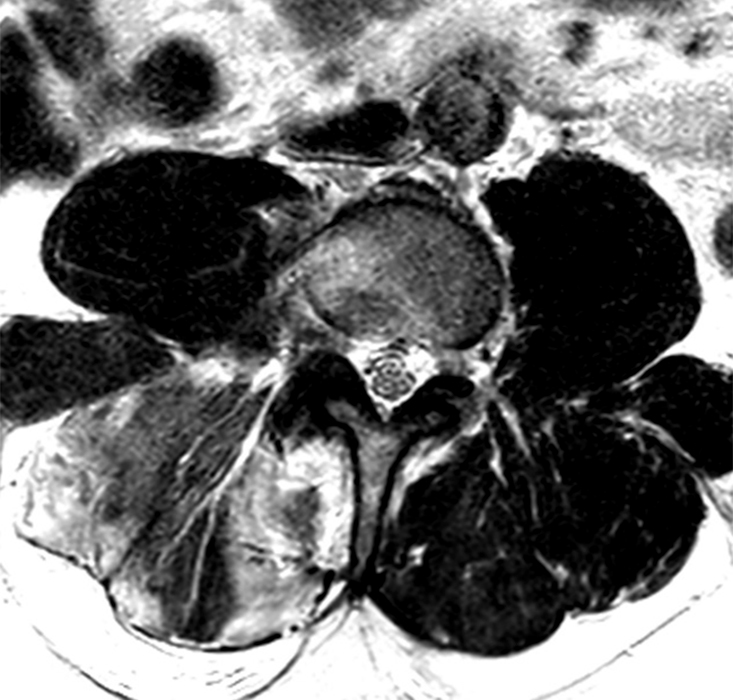
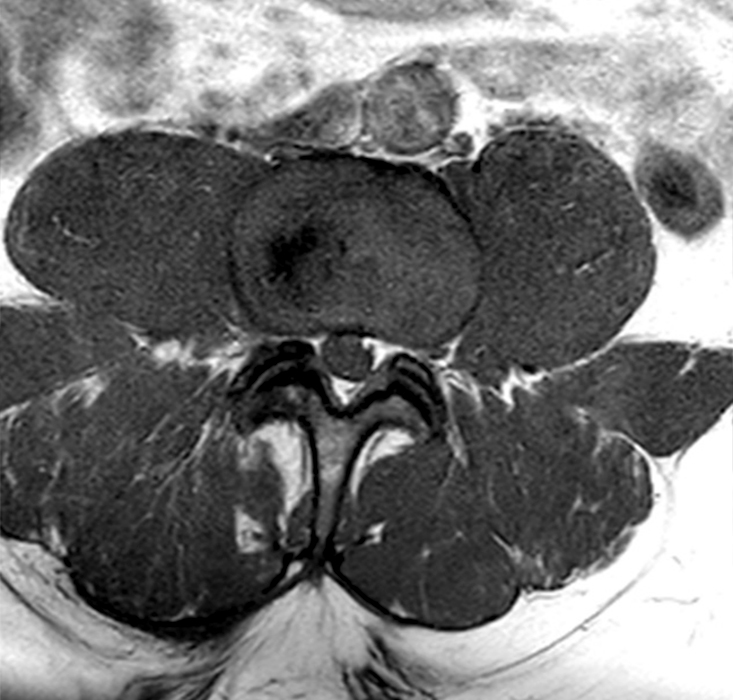
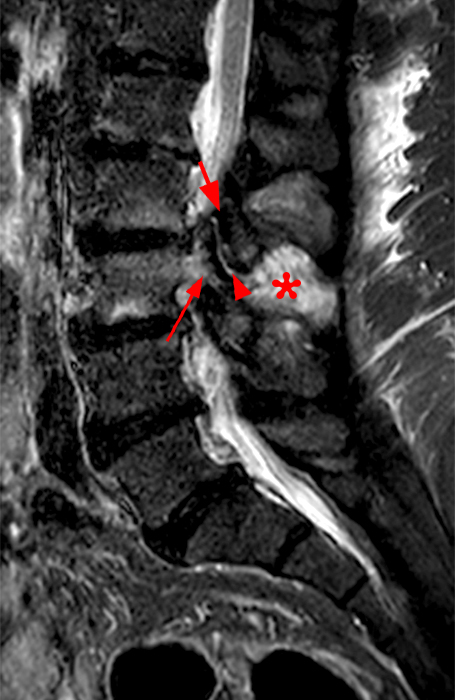
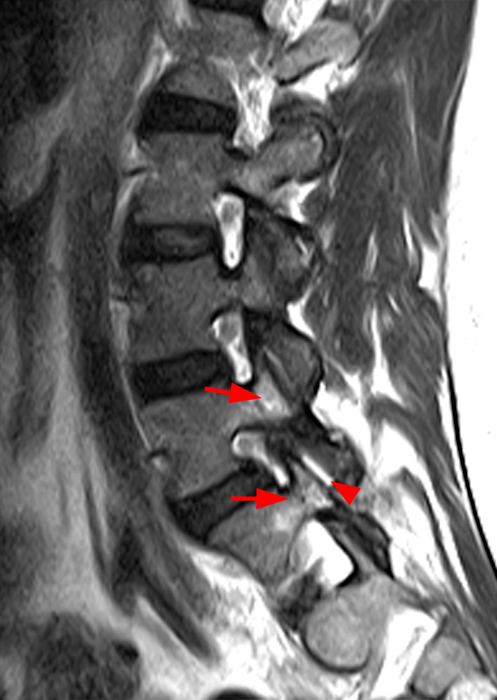
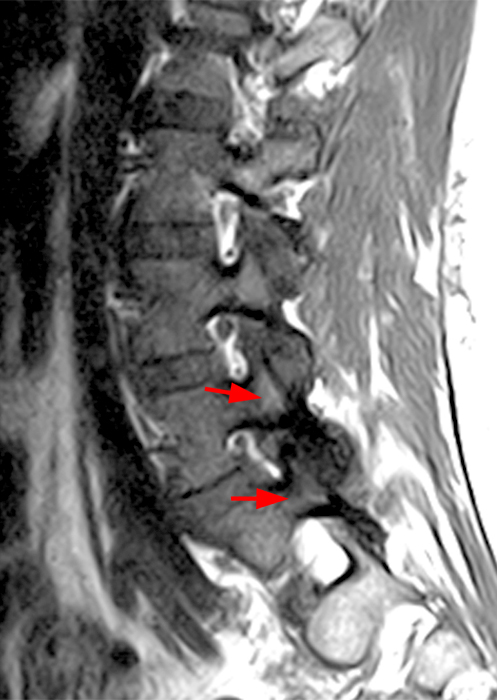
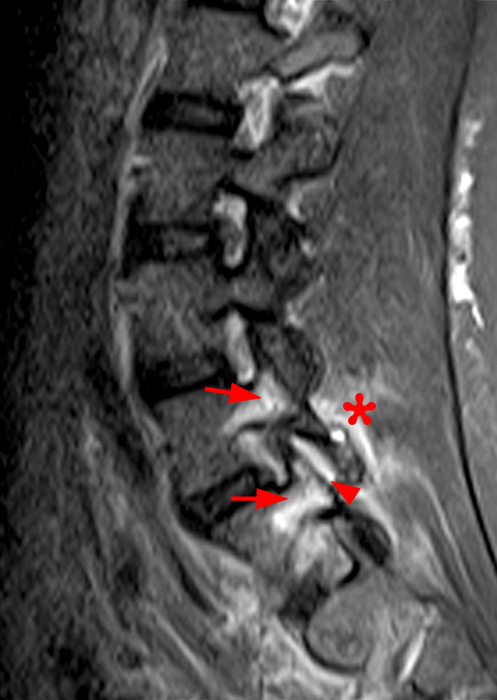
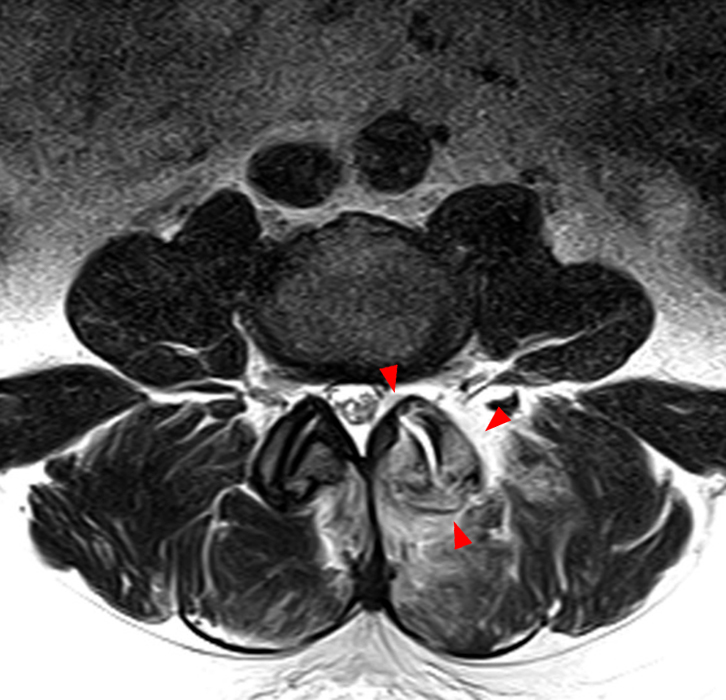
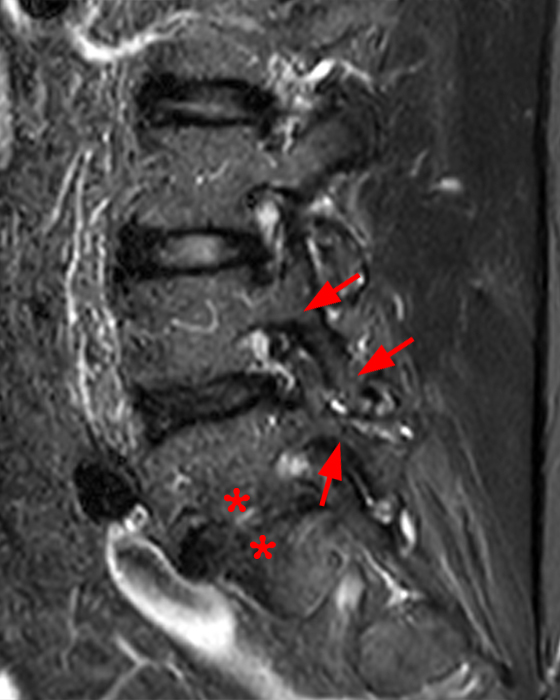
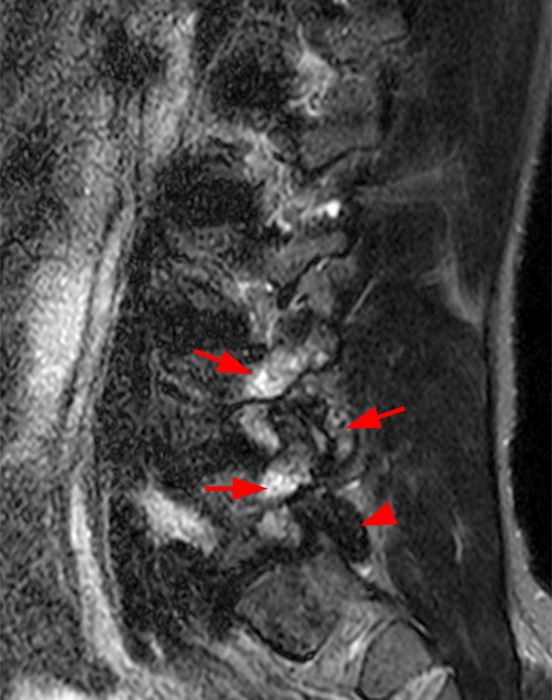
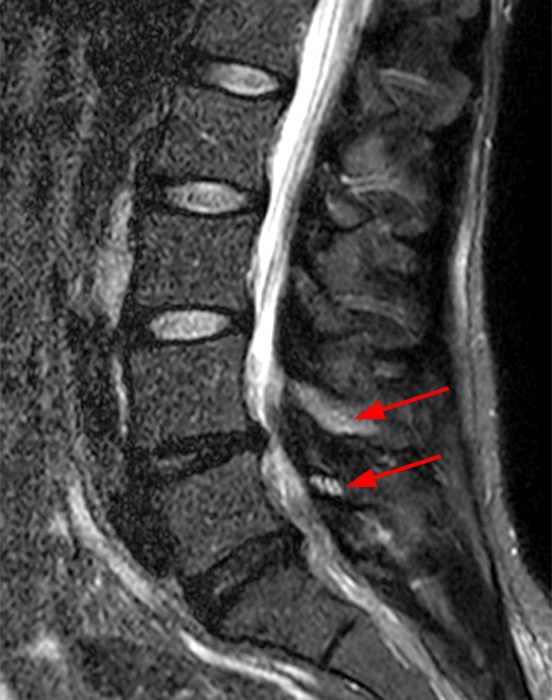
Clinical History: A 69-year-old female presents with low back pain, bilateral buttock, and posterior right thigh pain, aggravated when moving from seated to standing position. The patient denies radicular type symptoms. On exam, the patient demonstrates increased pain with hyperextension and lateral movements in hyperextension. There is point tenderness over the paraspinal lower lumbar levels greater on the left. Sagittal STIR (1a and 1b) and axial T2-weighted (1c) and T1-weighted (1d) images are provided. What are your findings? What is your diagnosis?
Findings
Figure 2:
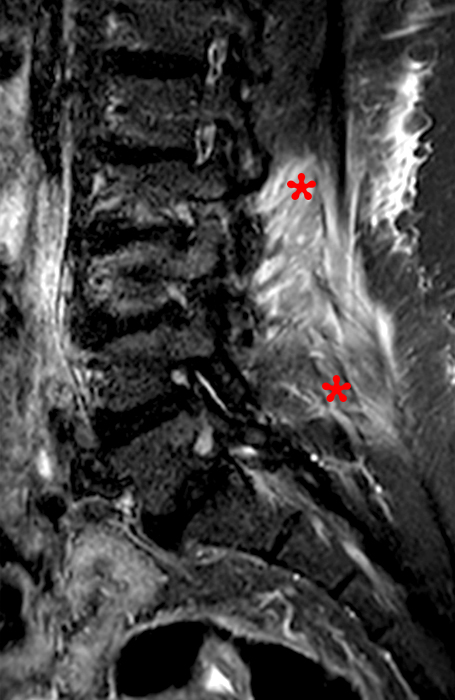
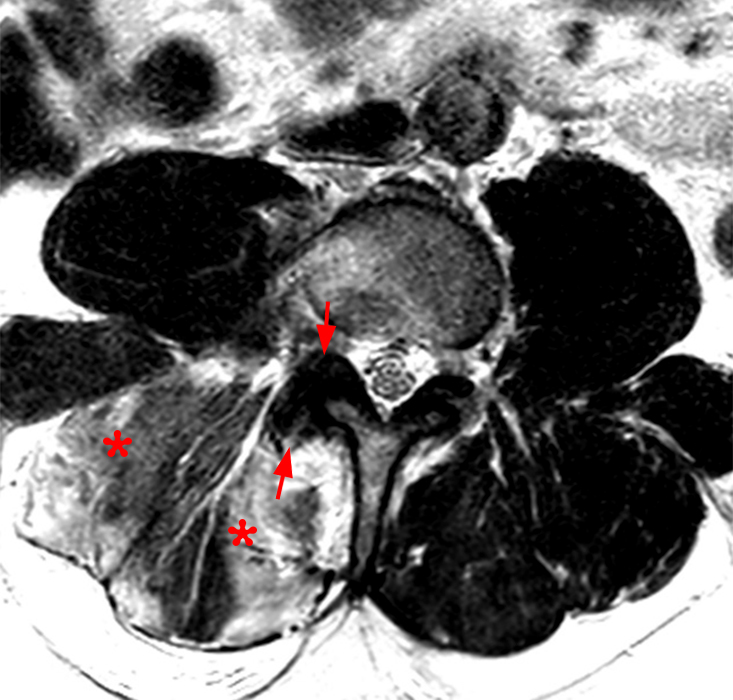
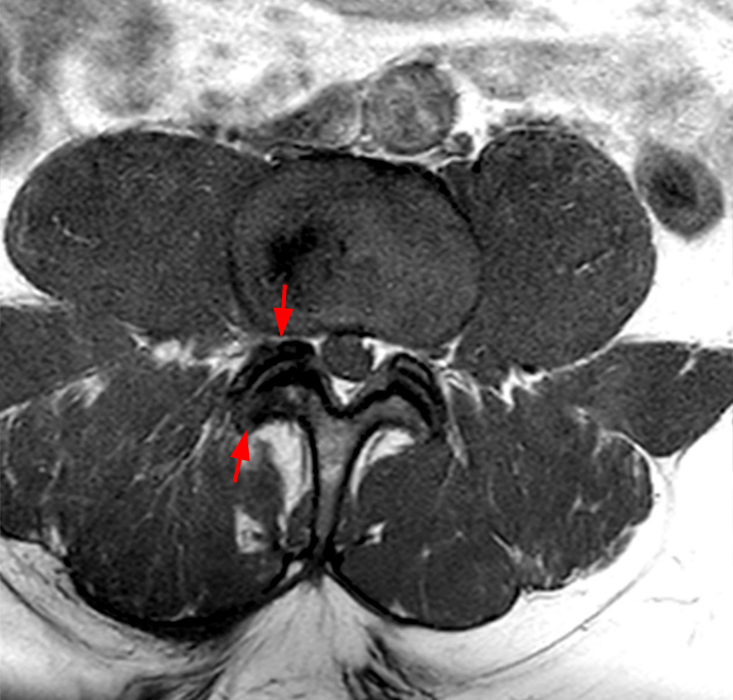
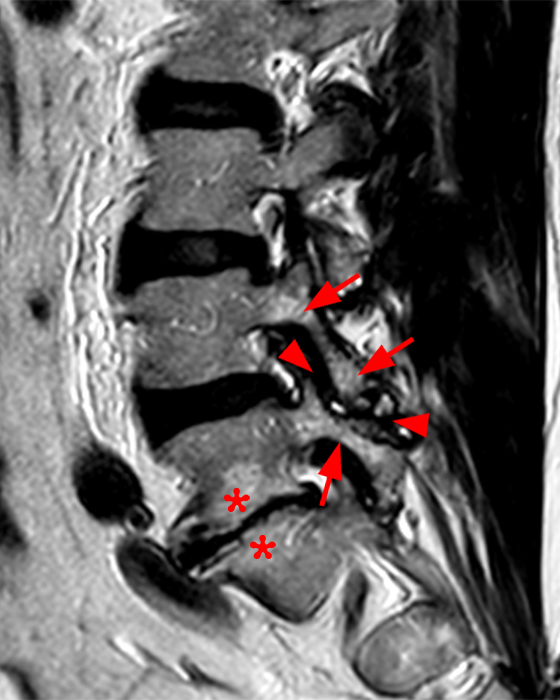
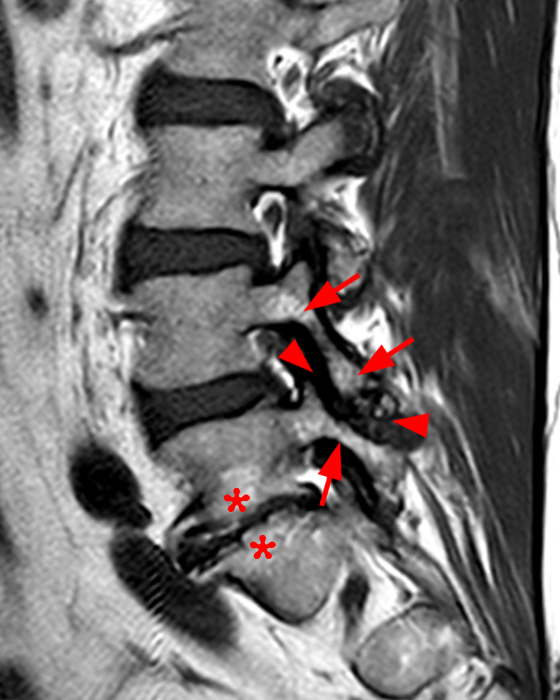
The STIR sagittal image through the right L3-4 facet (2a) demonstrates L3 pedicle and inferior articulating process edema (arrow), a small facet effusion (arrowhead), and subarticular sclerotic changes (short arrow) with periarticular soft tissue edema (asterisk). The extent of cranial and caudal periarticular edema is seen on the more lateral image (2b) (asterisks), and edema is evident within the multifidus and erector spinae muscles (asterisks) on the axial T2-weighted image (2c). Facet hypertrophy and articular sclerosis (short arrows) are seen on the axial T2-weighted (2c) and T1-weighted images (2d).
Diagnosis
Osteoarthritis and synovitis of the right L2-3 facet with marrow and periarticular soft tissue inflammatory edema.
Introduction
The facet joints account for significant lumbar, thoracic, and cervical pain. Facet arthropathy is present in 50 percent of the population by age 30 and virtually all over age 60.1 The paired facet joints and the intervertebral disc form a three joint stabilizing unit at each intervertebral level with disc or facet joint degeneration most often occurring in conjunction with each other but also occurring independently.
The facet (zygapophyseal) joint is a diarthrodial joint with two articular surfaces lined with cartilage, surrounded by a fibrous capsule, and containing synovial fluid. Chronic flexion, rotational and axial loading stresses result in degenerative facet arthropathy with cartilage breakdown, hypertrophic osteophytic bone overgrowth, and synovial hypertrophy with increase joint fluid.
Unlike focal neuronal impingement caused by a facet osteophyte or facet cyst involving the central canal or neural foramen, facet origin pain arises from the rich nociceptive innervation of inflamed synovium of the facet and sympathetic efferent nerve fibers within subchondral bone, resulting in pain, often clinically difficult to distinguish from other sources of back pain.2
Clinical Presentation
Typically, facetogenic origin pain is localized in the back over the involved zygapophyseal joints, with facet arthropathy most commonly affecting the lumbar spine. Referred pain commonly extends to the buttocks and posterior thighs. Pain is often aggravated with standing after long periods of sitting with patients having difficulty extending to a full erect position. Symptoms are reproduced clinically with hyperextension of the spine and lateral movements during hyperextension. This constellation of findings is often referred to clinically as ”axial pain”. Clinically isolating a facet as a sole source of axial pain remains difficult but several small studies found that asymmetrically prominent synovitis on imaging shows high correlation with corresponding ipsilateral symptoms.3
MR Imaging
Radiographs and CT demonstrate bony changes of joint sclerosis, hypertrophy, and spondylolisthesis but are less able than MRI to show associated edema and inflammatory changes associated with facet synovitis. MRI’s multiple sequences, particularly with the addition of T2-weighted fat-suppressed techniques , most commonly STIR (short tau inversion recovery), can demonstrate the joint fluid, inflammatory facet articulating process marrow and soft tissue perifacet/periarticular edema changes. STIR sequences prove better than T1- and T2-weighted images alone at demonstrating the inflammatory edema within bone and perifacet soft tissues (Fig 3).
Figure 3:
34-year-old female with right-sided back pain at the lumbosacral junction. Sagittal T2-weighted (3a) image demonstrates increased signal in the right pedicle and articular processes of L4 and L5 (short arrows), and the sagittal T1-weighted (3b) image demonstrates decreased signal relative to adjacent marrow in the same locations (short arrows), consistent with marrow edema. Osseous (short arrows) and periarticular soft tissue edema (asterisk) is more conspicuous on the STIR image (3c).
Gadolinium enhancement typically mirrors the edematous signal changes seen on STIR images, not typically adding additional diagnostic information. Czervionke et al. found in a small series, 100% correlation of ipsilateral pain if periarticular inflammatory changes involved 50% or more of the perimeter of the joint (Fig 4).3
Figure 4:
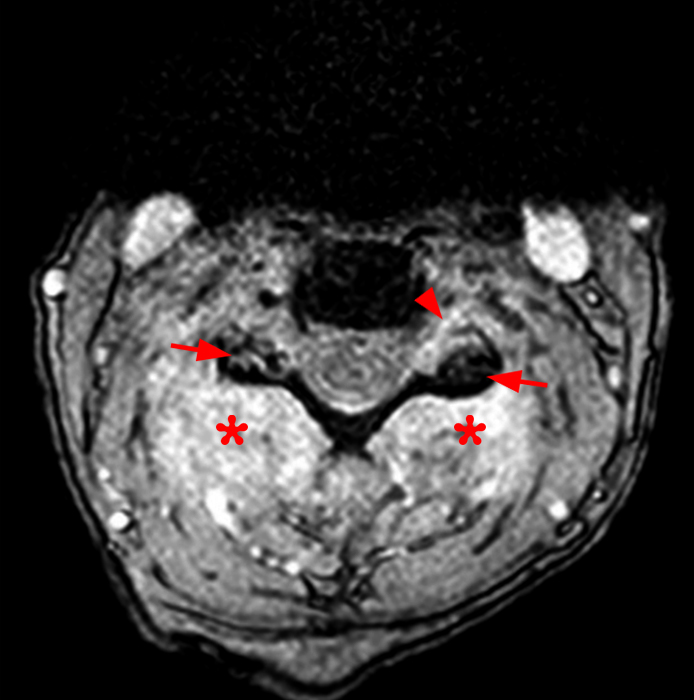
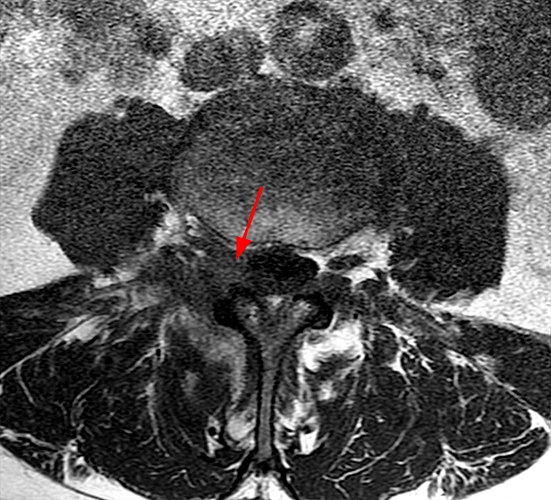
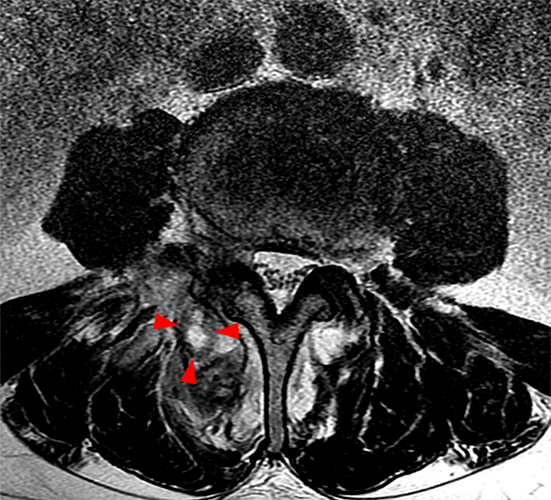
56 year-old male with left-sided low back pain with occasional radiculitis in the left lateral thigh. Axial T2-weighted image at L3-4 demonstrates a left facet joint effusion, marrow edema and periarticular facet edema that extends beyond 50% of the perimeter of the joint with probable foraminal involvement (arrowheads) and no bone destruction.
Differential
Osteoarthritic degeneration of the joint is by far the most common etiology for a facet synovitis but when bilateral and multiple joints are involved a crystal deposition arthropathy such as gout or calcium pyrophosphate deposition disease and non-osteoarthritic seronegative arthropathies should be considered (Fig 5).
Figure 5:
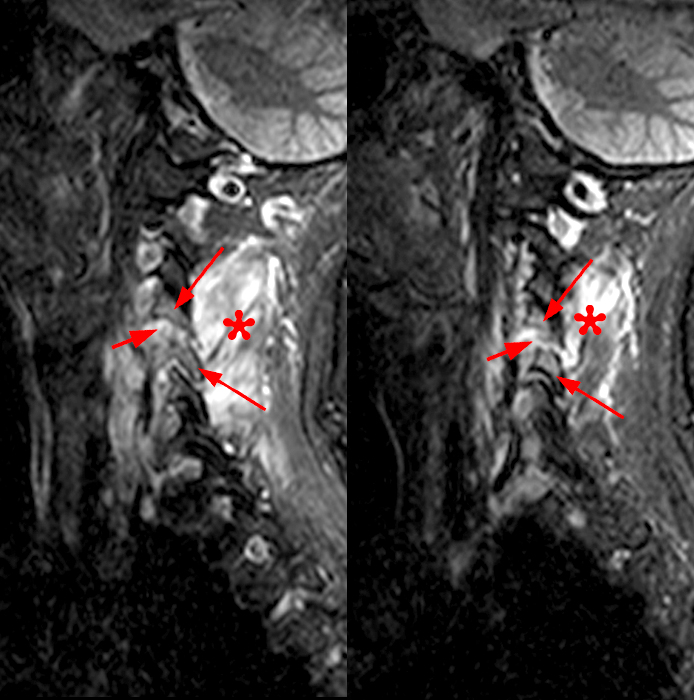
63-year-old female with stiff neck, muscle spasm, and right shoulder pain for 3 months with presumptive diagnosis of crystal deposition disease. Left parasagittal (left) and right parasagittal (right) STIR images (5a) demonstrate bilateral multiple facet joint involvement at C4-5 and C5-6, most severe at C4-5 with facet effusions (short arrows), articulating process edema (arrows) and soft tissue periarticular edema (asterisks). Axial T2* gradient-echo image at the C3-4 level demonstrates articular cartilage destruction (short arrows) and prominent periarticular edema (asterisks) with left foraminal extension of edema (arrowhead).
Although rare, septic arthritis or direct inoculation from prior procedure should be considered if unilateral soft tissue inflammatory changes, an extra-articular fluid collection and erosive bone changes are present (Fig 6).
Figure 6:
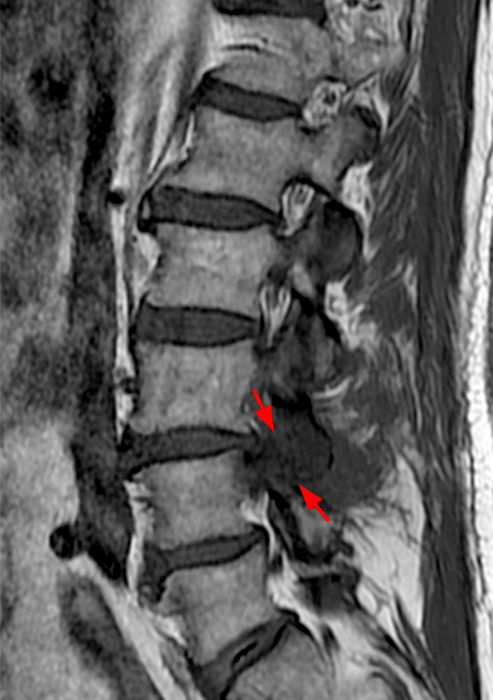
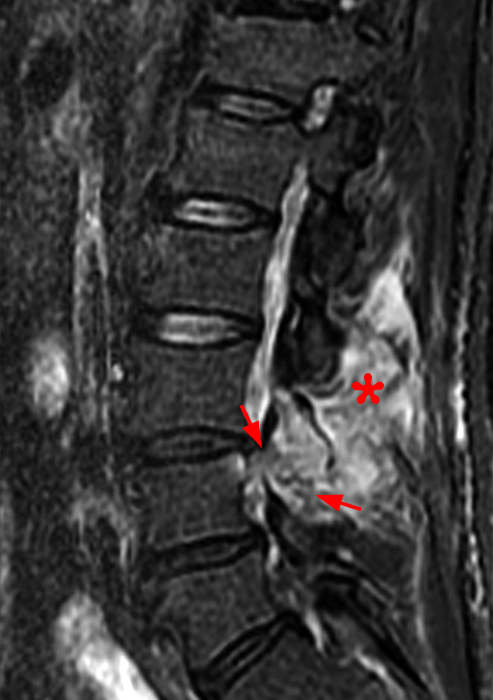
56-year-old male with low back pain and occasional radiculitis to the left leg. Right parasagittal T1-weighted (6a) and STIR (6b) and axial T1-weighted (6c) and T2-weighted (6d) images demonstrate findings of septic facet arthritis. Single level severe facet articulating process edema, periarticular edema with foraminal extension (arrow) and articular bone erosion at the L3-4 level (short arrows). Prominent edema is seen within the periarticular soft tissues (asterisks) as well as a periarticular abscess collection (arrowheads).
Within the differential but more mass-like in presentation are rare primary bone lesions including the benign osteoid osteoma and osteochondroma and tumors such as plasmacytoma and tenosynovial giant cell tumor.
Like the vertebral endplates the facet joint subchondral bone and articulating processes can demonstrate acute edema as well as sclerosis and fatty changes of chronic degeneration (Fig 7). Both T2- and T1-weighted images demonstrate increased signal intensity with fatty changes. Marrow edema results in increased signal on T2-weighted images while the T1-weighted images demonstrate reduced signal intensity in the same area. STIR imaging can help in differentiating edema and fatty changes by increasing the conspicuity of edema and suppressing the signal of areas of fat (Fig 3). Articulating process sclerosis can be so severe that marrow edema originating from facet inflammation may only be seen in the pedicle or adjacent vertebral body marrow, lamina, or spinous process. (Fig 8).
Figure 7:
80-year-old female with chronic low back pain. T2-weighted right parasagittal image (7a) demonstrates facet joint arthritis (arrowheads) with increased signal relative to the adjacent marrow in the articular processes and pedicles at L4 and L5 (short arrows). These same areas (short arrows) are increased in signal relative to the adjacent marrow on the T1-weighted image (7b) confirming degenerative fatty change. The sagittal STIR series (7c) confirms a lack of edema in these areas (short arrows). A similar pattern of marrow signal changes bordering the L5-S1 disc indicates Modic type II fatty degenerative changes.
Figure 8:
Right parasagittal STIR (8a) image demonstrates edema of the L4 and L5 pedicles and inferior articular process of L4 bordering degenerative L4-5 and L5-S1 facets. The inferior articular process of L5 demonstrates low signal corresponding to marked sclerosis without edema. Midline sagittal STIR image (8b). Marrow edema associated with facet arthritis extends into the L4 and L5 spinous processes (arrows) on the midline sagittal STIR image.
Conclusion
Differentiating facet origin pain from discogenic and radicular causes remains clinically difficult. Hypertrophy, sclerosis and facet effusions can persist long after facet inflammation has resolved, contributing to the diagnostic challenge of facet disease. Facet synovitis/inflammation, effusions, marrow edema and periarticular edema are findings that have been shown to correlate significantly with clinical symptoms. MRI reliably identifies these abnormalities, allowing appropriate initiation of facet-oriented therapy.
References
- Eubanks D, Lee J et al. Prevalence of lumbar facet arthrosis and relationship to age, sex, and race: and anatomic study of cadaveric specimens. Spine 2007 Sep 1;32(19):2058-62. ↩
- Ashton IK, Ashton BA et al. Morphological basis for back pain: The demonstration of nerve fiber and neuropeptides in the facet joint capsule but not in ligamentum flavum. J Orthop Res 1992; 10:72-8 ↩
- Czervionke L, Fenton D. Fat-Saturation MR Imaging in the Detection of Inflammatory Facet Arthropathy (Facet Synovitis) in the Lumbar Spine. Pain Medicine, Volume 9, Issue 4, May 2008, 400-406. ↩