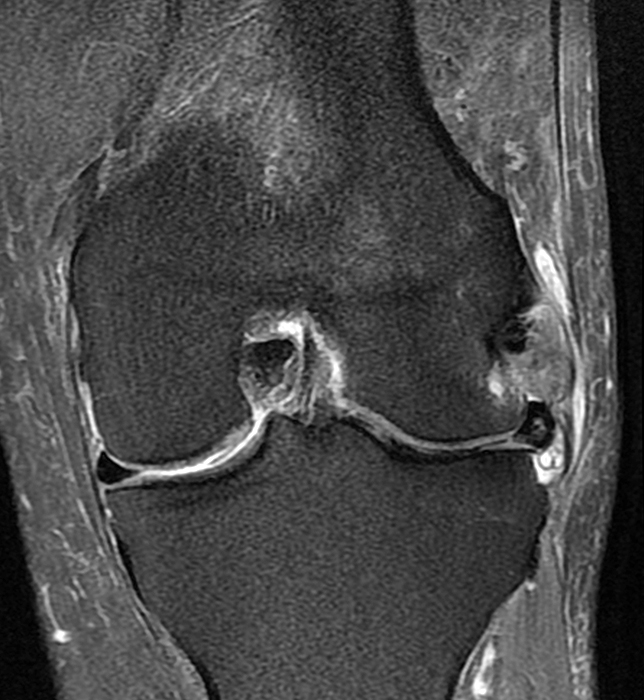
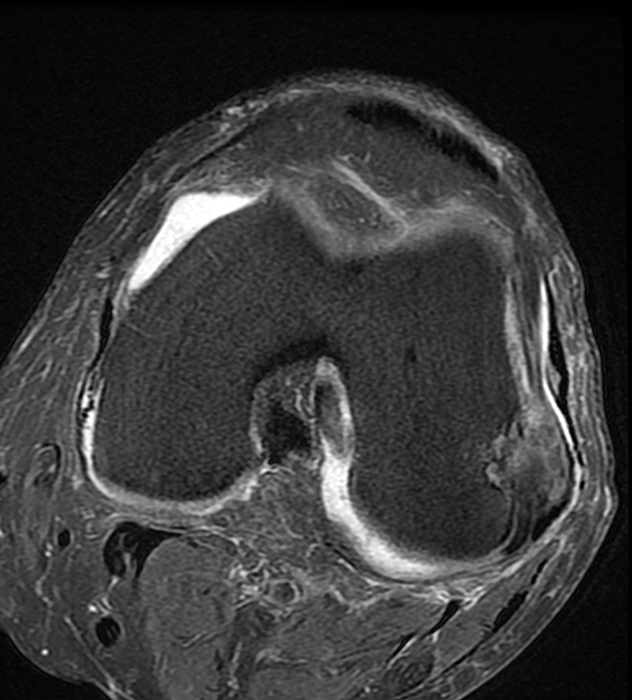
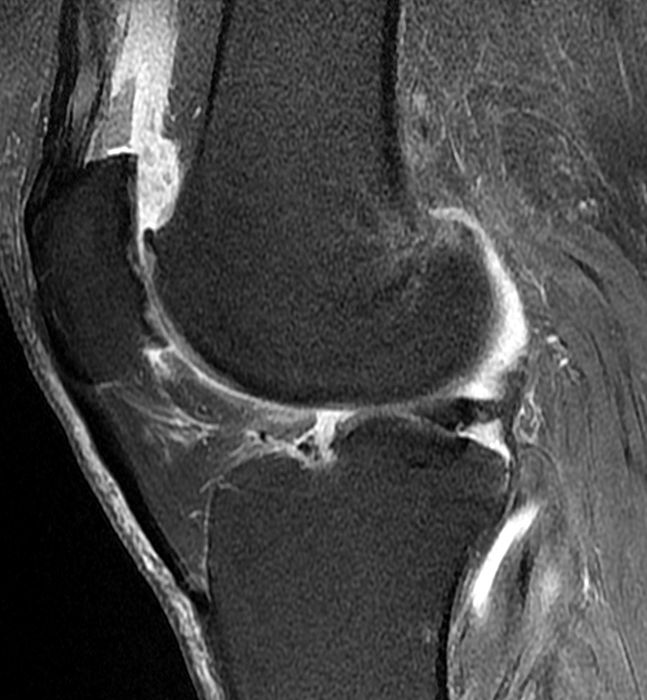
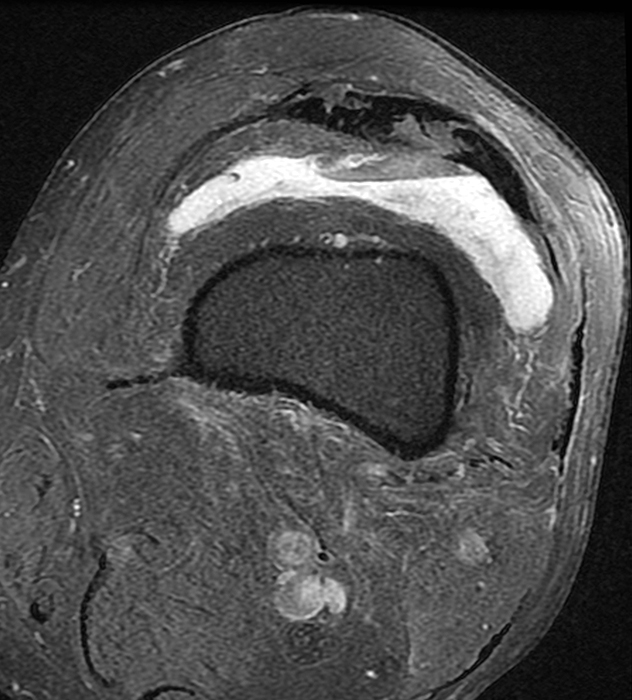
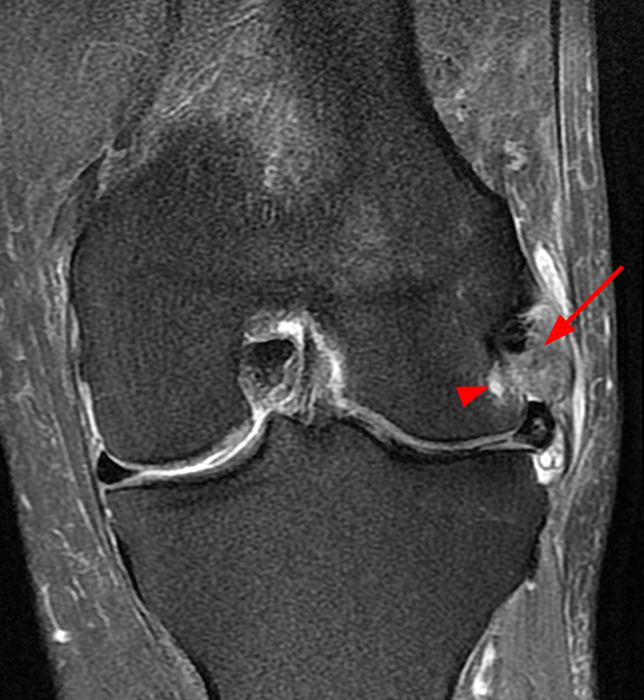
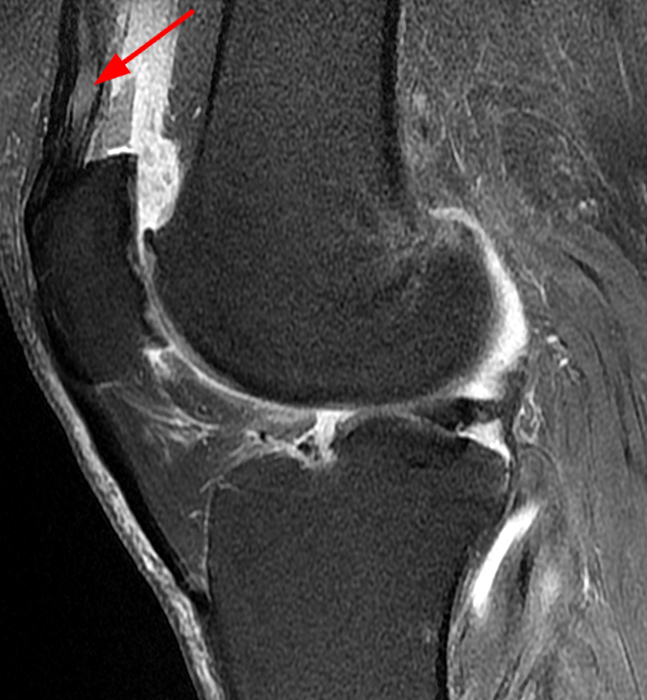
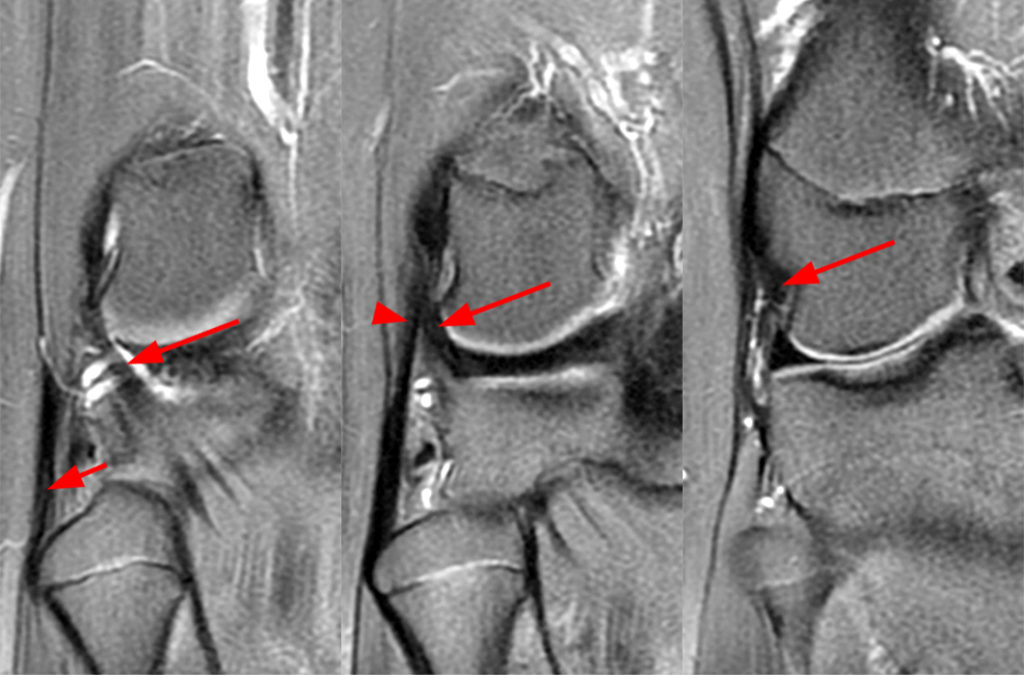
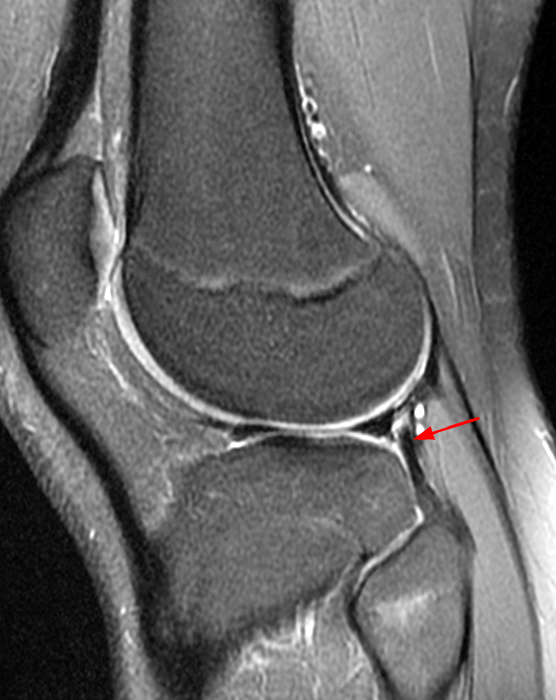
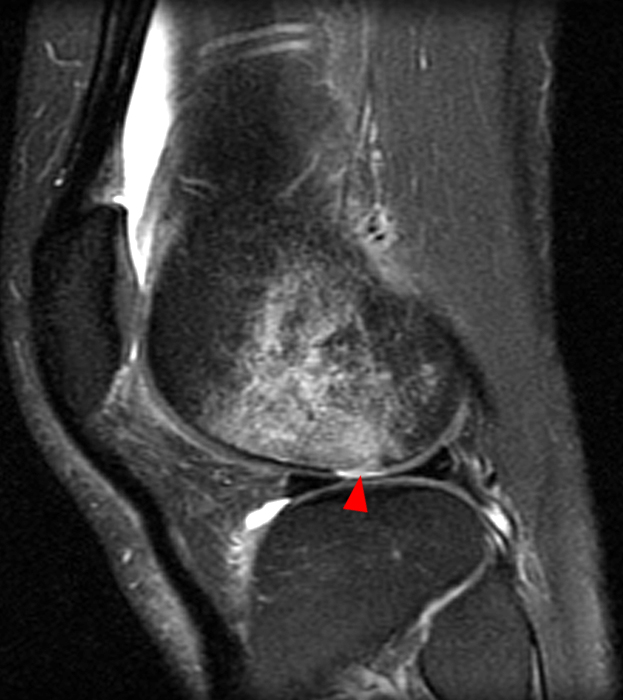
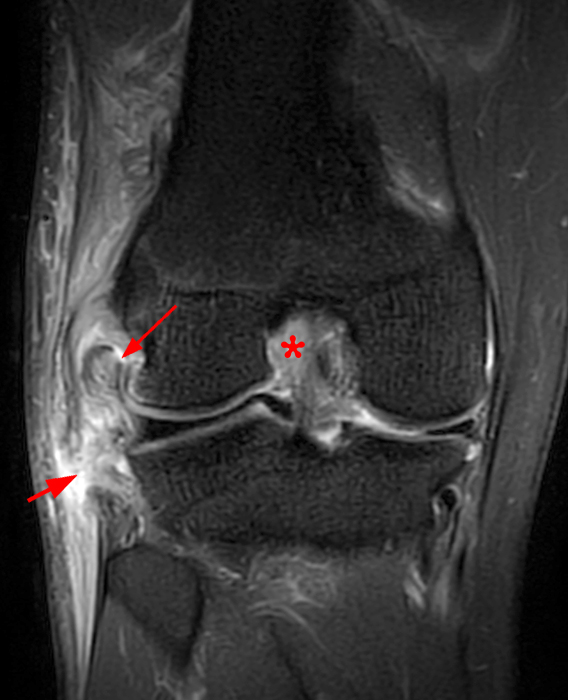
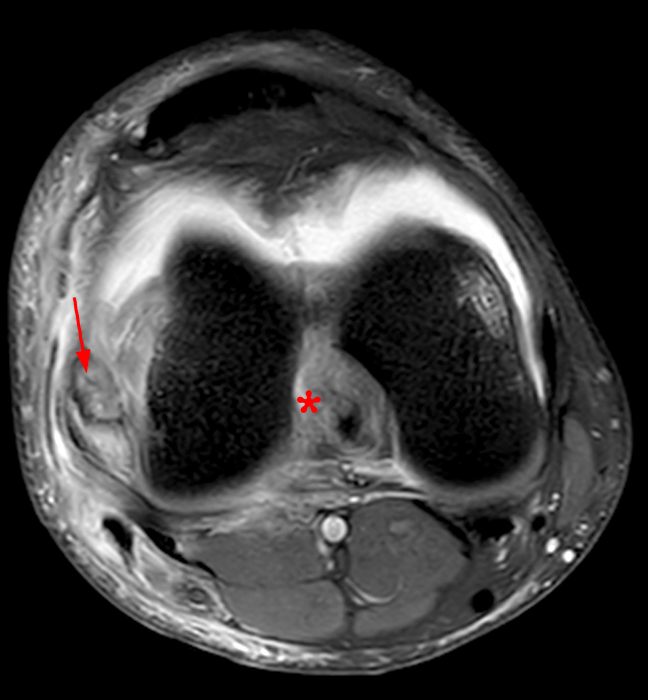
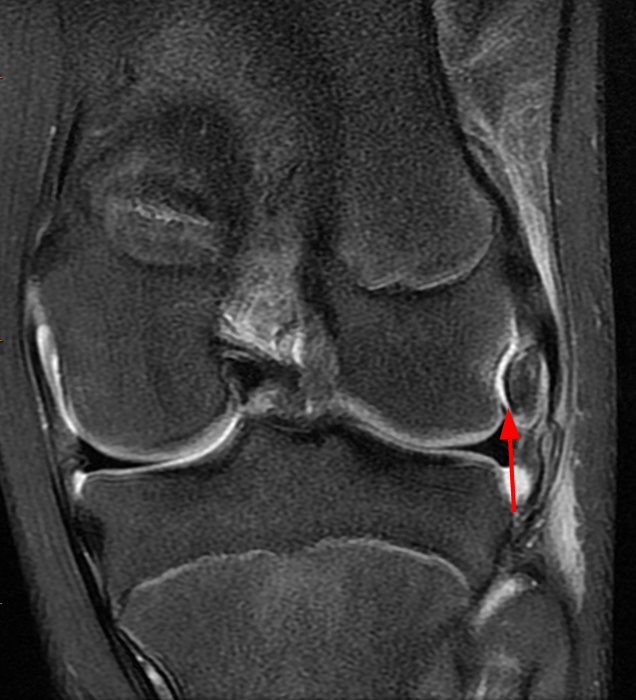
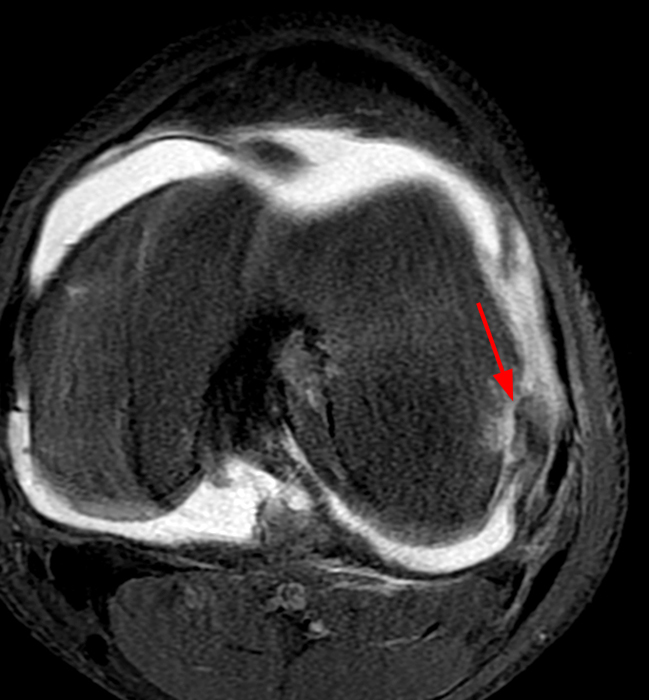
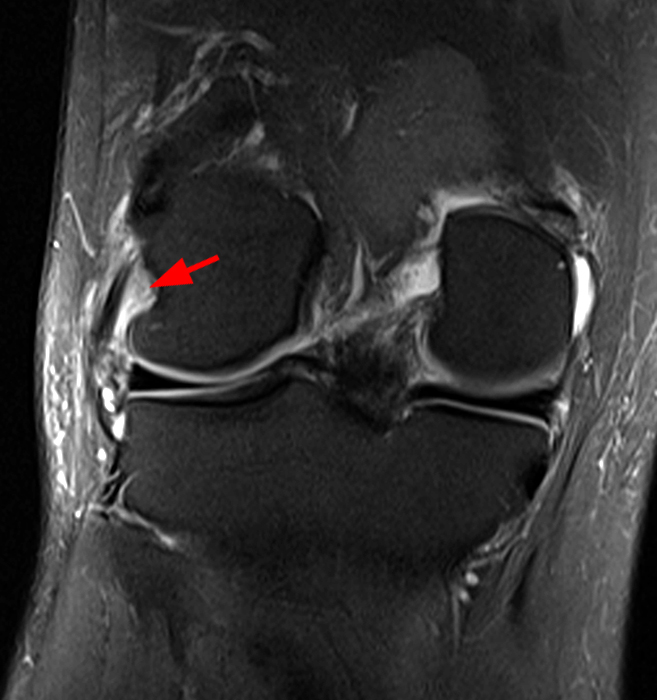
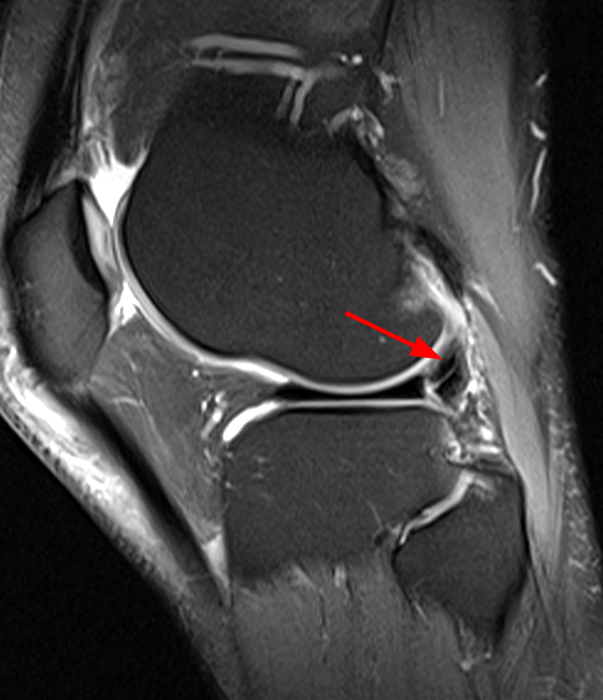
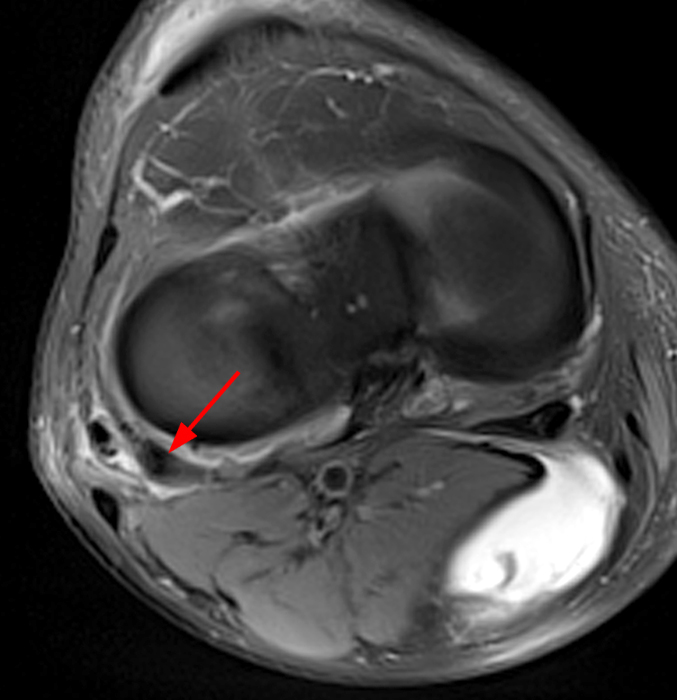
Clinical History: An 84-year-old male presents with lateral knee pain and swelling. Coronal (1A), axial (1B, 1D), and sagittal (1C) fat-suppressed proton-density-weighted images of the knee are provided. What are the findings? What is your diagnosis?
Findings
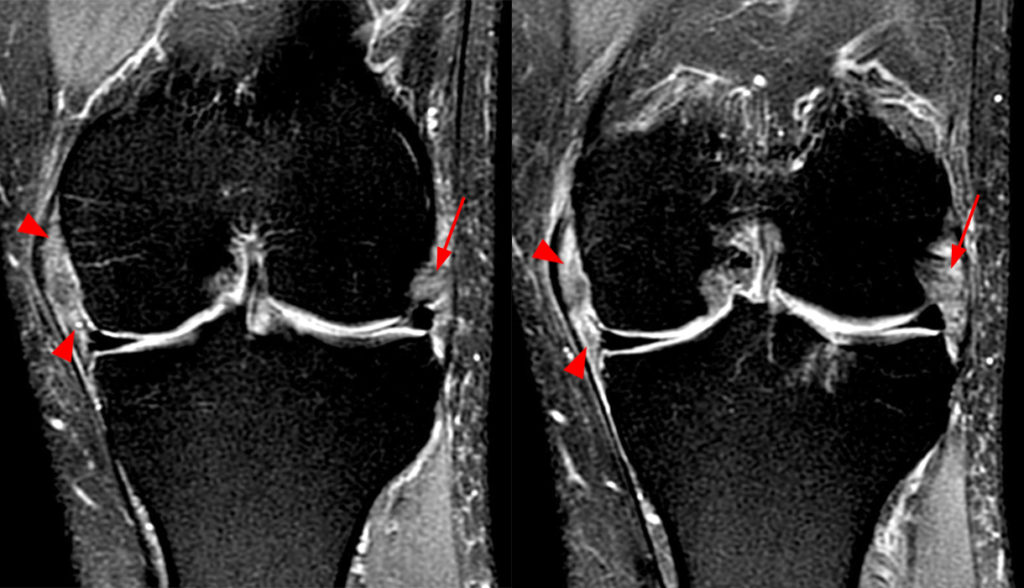
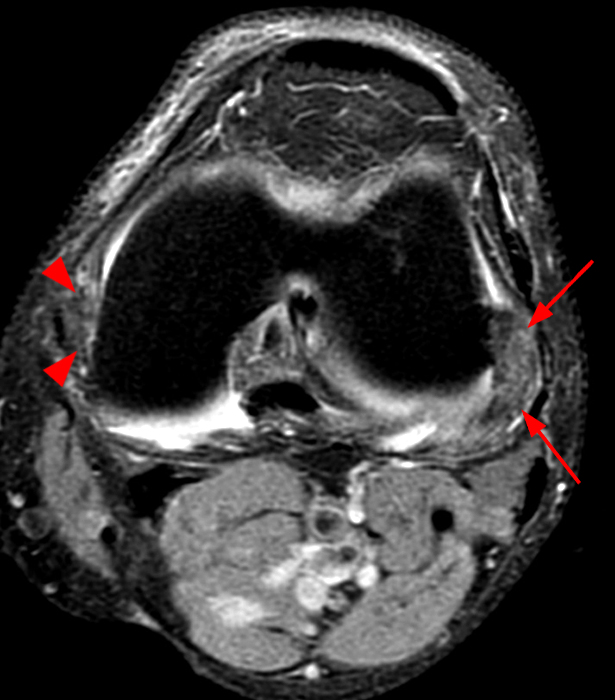
Figure 2:
Coronal (2A) and axial fat-suppressed proton density-weighted (2B) images of the knee demonstrate a diffusely thickened, intermediate signal intensity infiltrative appearance of the intra-articular popliteus tendon (arrows) with subjacent mild erosions (arrowheads) at the popliteal sulcus. Overlying bursitis is additionally apparent. Sagittal (2C) and axial (2D) fat-suppressed proton density-weighted images of the knee demonstrate an infiltrative appearance of the distal quadriceps tendon (arrows), similar to the process involving the popliteus tendon.
Diagnosis
Gout with involvement of the intra-articular popliteus as well as distal quadriceps tendons.
Introduction
Although the popliteus tendon is an integral component of the posterolateral corner of the knee as well as a site of chronic and insidious pathology, this long and strong tendon with its unique anatomy is oftentimes overlooked. Acute injuries to the popliteus tendon typically occur in conjunction with other injuries to the posterolateral corner structures of the knee, the cruciate ligaments and menisci and, rarely, in isolation. Chronic pathology of the popliteus tendon, which may be underappreciated, includes tendinosis, crystalline deposition diseases and pigmented villonodular synovitis. This Web Clinic will delve into the anatomy and function of the popliteus tendon with case examples of both traumatic and chronic disease.
Anatomy, Function and Normal MRI Appearance
The relatively small, triangular and obliquely oriented popliteus muscle ascends superolaterally from a broad attachment at the posteromedial tibia just above the soleal line, continues as a tendon deep to the lateral collateral ligament and biceps femoris tendon through the popliteal hiatus, and inserts at the popliteal sulcus of the lateral femoral condyle. The tendon is intra-capsular but extra-synovial and extra-articular.1 The popliteus musculotendinous complex, composed of the musculotendinous unit and popliteofibular ligament, provides static and dynamic resistance to external rotation and acts as a secondary restraint to posterior translation (Figure 3).1,2 The tendon and muscle are typically best evaluated on axial and coronal images (Figure 4).
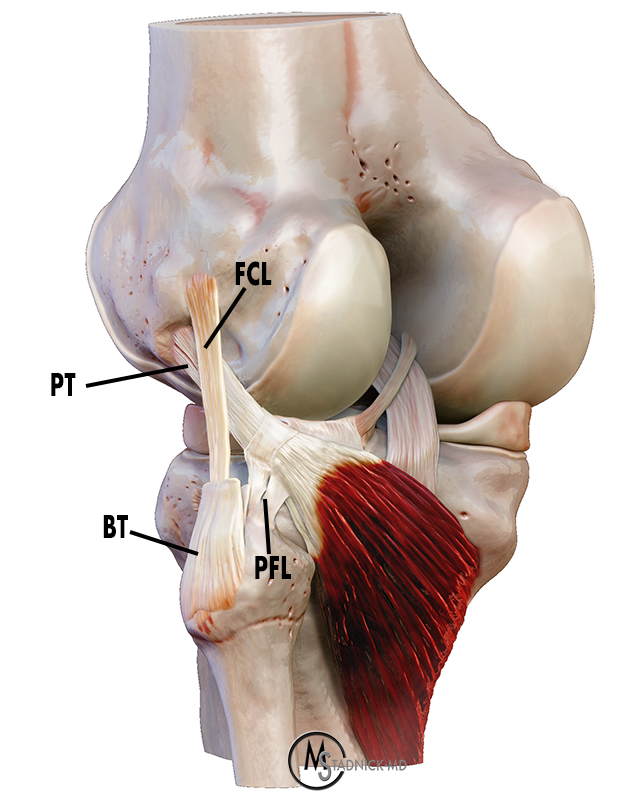
Figure 3:
3D render of the popliteus musculotendinous complex with the biceps femoris tendon (BT) partially removed demonstrates the popliteus tendon (PT) passing deep to the fibular collateral ligament (FCL) and inserting at the popliteal sulcus of the lateral femoral condyle. The popliteofibular ligament (PFL) extends from the fibular styloid process to the popliteus tendon.
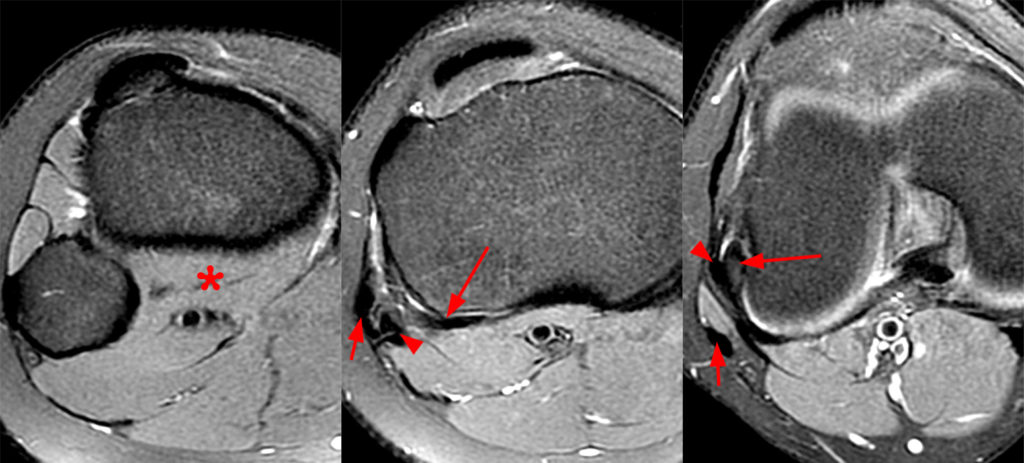
Figure 4:
Normal anatomy and MRI appearance of the popliteus tendon. Multiple fat-suppressed axial (4A) and coronal (4B) proton-density-weighted images of the knee from inferior to superior and posterior to anterior, respectively, demonstrate the superolateral ascension of the popliteus muscle (asterisk) and extra-articular and intra-articular tendon (arrow), deep to the fibular collateral ligament (arrowhead) and biceps femoris tendon (short arrow), to the attachment at the popliteal sulcus. The popliteal hiatus is best evaluated in the sagittal plane (4C), as in this fat-suppressed proton-density-weighted image.
Abnormalities of the Popliteal Hiatus
Assessment of the popliteal hiatus on sagittal images is important as pathology such as meniscal flaps and loose bodies occasionally extend into this area (Figure 5). Of note, the popliteus bursa is a normal fluid-filled and synovial-lined structure along the extra-articular tendon and musculotendinous junction which, on occasion, contains pathology and should not be confused for a musculotendinous injury (Figure 6).
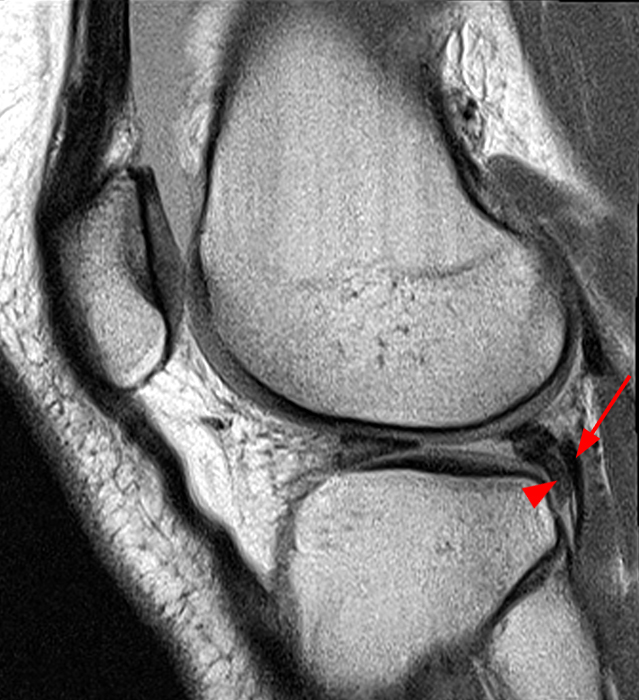
Figure 5:
Displaced meniscal flap extending into the popliteal hiatus. A sagittal proton density-weighted image demonstrates a flap tear of the posterior horn of the lateral meniscus with a displaced meniscal flap (arrowhead) extending into the popliteal hiatus anterior to the popliteus tendon (arrow).
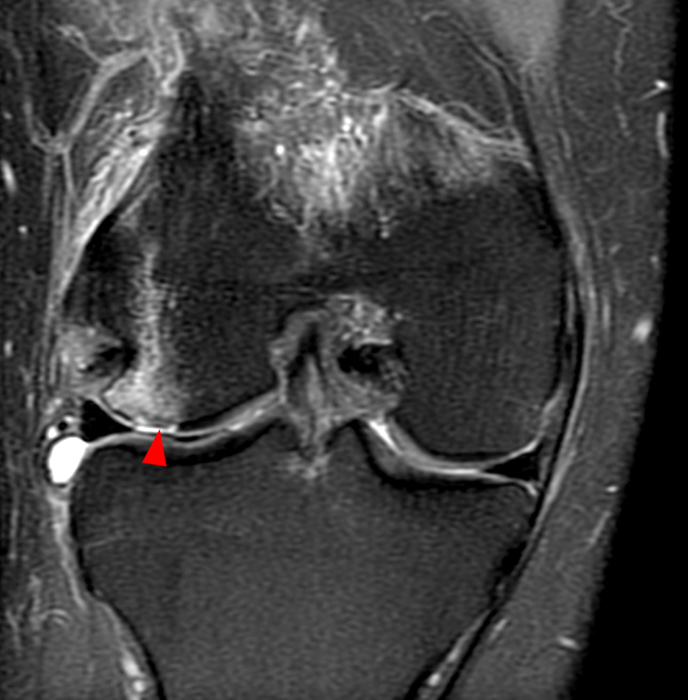
Figure 6:
Chondral body displaced into the popliteal bursa status post recent transient lateral patellar dislocation. Fat-suppressed axial (6A), coronal (6B), and sagittal (6C) proton-density-weighted images of the knee demonstrate a displaced chondral body (arrow) within the popliteal bursa. The chondral defect from which the body arose is identified at the lateral weight-bearing lateral femoral condyle (arrowheads). A typical bone bruise for patellar dislocations is present above and anterior to the defect.
Traumatic Popliteus Injuries
Acute popliteus tendon tears typically occur in the setting of multi-ligament and meniscal tears and, as such, careful attention should be paid to the adjacent posterolateral corner structures as well as the cruciate ligaments and menisci1-3 (Figure 7). Tears of the popliteus tendon should be characterized as partial or complete, intra-articular or extra-articular, and with regards to the proximity to the popliteal sulcus and the extent of retraction. Partial tears may be treated conservatively whereas complete tears retracted beyond the popliteal hiatus require an open or combined approach. The presence of an avulsed osseous fragment should also be noted as these can be fixated back into place (Figure 8). Rarely, isolated tendinous avulsions of the popliteus may occur (Figure 9).1
Figure 7:
Popliteus tendon avulsion in the setting of multi-ligament tears. Fat-suppressed coronal (7A), axial (7B), and sagittal (7C) proton-density-weighted images of the knee demonstrate a significant posterolateral corner knee injury with a tendon avulsion at the femoral attachment of the popliteus (arrow), a complete tear of the mid-substance fibular collateral ligament (short arrow) and tearing of the posterolateral joint capsule (arrowhead). The ACL was also torn (asterisk).
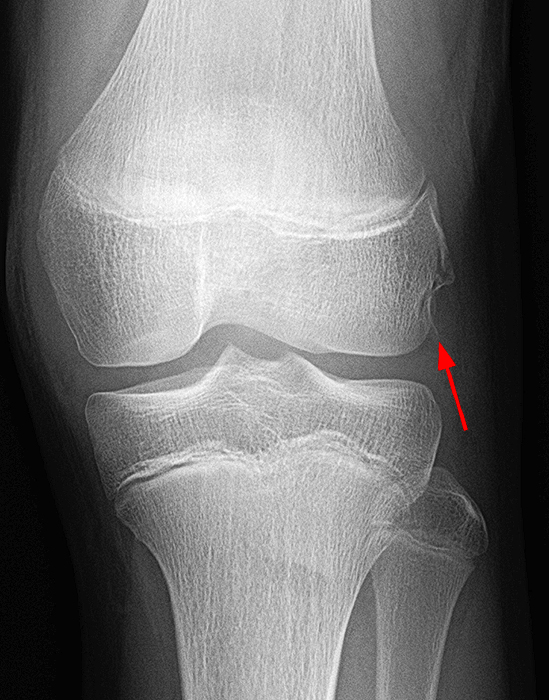
Figure 8:
Cortical avulsion at the femoral attachment of the popliteus tendon. Fat-suppressed coronal and axial proton-density-weighted images of the knee demonstrate a minimally displaced cortical avulsion (arrow) at the femoral attachment of the popliteus. The tendon itself demonstrates no intrinsic tear. Although subtle, a corresponding curvilinear fracture (arrow) is apparent on a frontal radiograph obtained a few days before the MRI.
Figure 9:
Isolated popliteus tendon avulsion. Fat-suppressed coronal (9A), sagittal (9B), and axial (9C) proton-density-weighted images of the knee demonstrate a tendon avulsion of the femoral attachment of the popliteus. In this case, the popliteal sulcus is “empty” (short arrow) and the torn, redundant and retracted tendon (arrow) remains intra-articular and sits folded over itself posterior to the posterior horn lateral meniscus. This intra-articular tear is amenable to arthroscopic repair. The remainder of the posterolateral structures, cruciate ligaments, medial collateral ligament and menisci are intact in this patient.
Tendinosis
Popliteus tendinosis results from chronic repetitive stress, may be seen with downhill runners and is characterized by tendon enlargement and intrasubstance intermediate signal. It is not uncommon to see interstitial splitting and partial tearing superimposed upon tendinosis (Figure 10).
Crystalline Deposition Disease
The popliteus tendon is a common intra-articular location for gout in the knee. The tendon appears enlarged, diffusely infiltrated and intermediate in signal and erosive or cystic change may be present at the popliteal sulcus as in the initial case. Correlation with radiographs to assess for associated calcifications may be helpful. Rarely, hydroxyapatite deposition occurs at the popliteus tendon.4 Radiographs demonstrate a calcification or calcifications in the expected location of the popliteus tendon and if an MRI is obtained, associated edema and fluid should be noted.
Pigmented Villonodular Synovitis
Synovial proliferative diseases such as pigmented villonodular synovitis also may extend along the popliteus tendon (Figure 11).
Figure 11:
Pigmented villonodular synovitis along the popliteus tendon. Contiguous fat-suppressed coronal (11A) and axial (11B) proton density-weighted images of the knee demonstrate thickening and intermediate signal infiltration of the popliteus tendon (arrows) and, to a lesser extent, similar-appearing nodular intermediate signal foci deep to the proximal tibial collateral ligament (arrowheads). The constellation of findings is typical for pigmented villonodular synovitis. Deep chondral fissuring and associated subchondral reactive marrow change are additionally present at the lateral tibial plateau.
Conclusion
The popliteus musculotendinous complex is a critical stabilizer of the posterolateral corner of the knee and resists both external rotation and posterior translation. The popliteus tendon is a strong but often underappreciated tendon and an important site for traumatic and chronic pathology. Routine assessment of the tendon and its hiatus in all imaging planes should be performed to ensure that relevant pathology is not overlooked.
References
- Jadhav S, More S et al. Comprehensive Review of the Anatomy, Function, and Imaging of the Popliteus and Associated Pathologic Conditions. RadioGraphics 2014;34:496-513. ↩
- Rosas H. Unraveling the Posterolateral Corner of the Knee. RadioGraphics 2016;36:1776-1791. ↩
- Vinson E, Major N et al. The Posterolateral Corner of the Knee. American Journal of Roentgenology 2008 Feb;190(2):449-58. ↩
- Doucet C, Gotra A et al. Acute Calcific Tendinopathy of the Popliteus Tendon: A Rare Case Diagnosed Using a Multimodality Approach and Treated Conservatively. Skeletal Radiol. 2017;46)7):1003-6. ↩