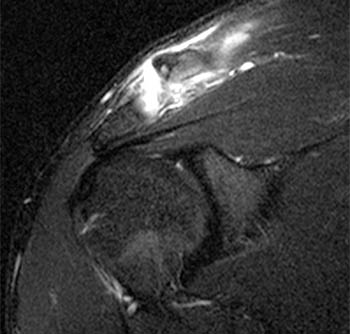
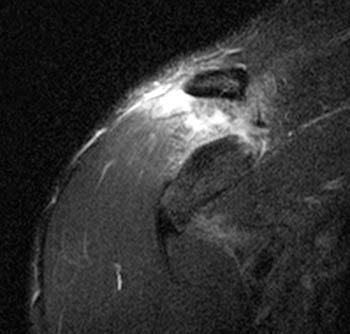
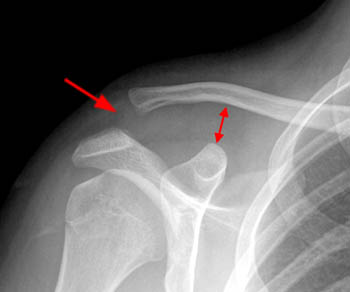
Clinical History: A 28 year-old male complains of shoulder pain after falling while playing ultimate Frisbee. A (1a) fat-suppressed T2-weighted coronal oblique image through the plane of the acromioclavicular joint and a (1b) fat-suppressed T2-weighted coronal oblique anterior to the plane of the acromioclavicular joint (ACJ) are provided. What are the findings? What is your diagnosis?
Findings
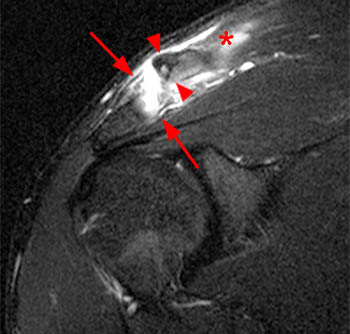
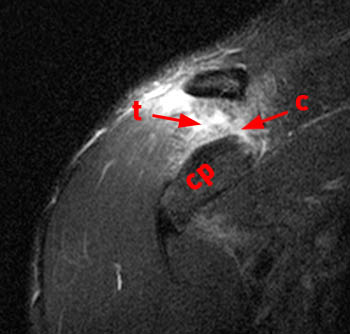
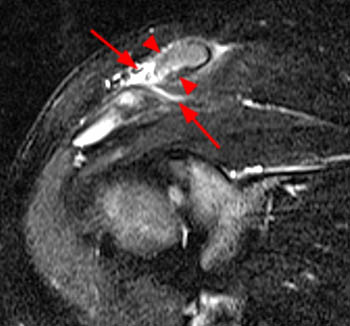
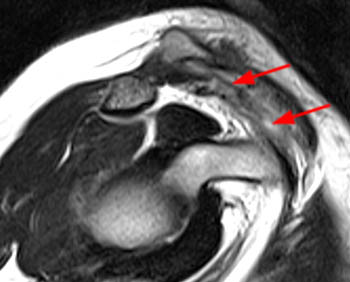
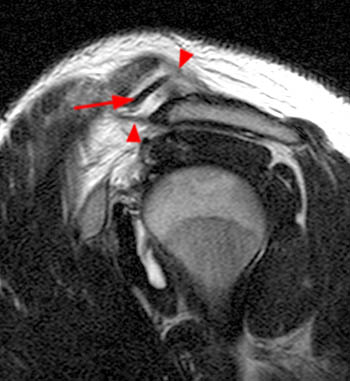
Figure 2:
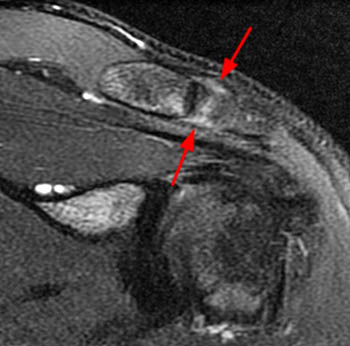
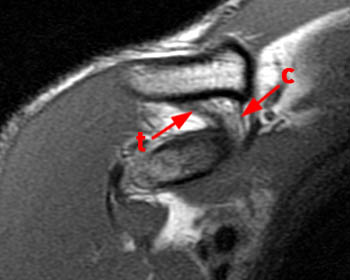
(2a) The fat-suppressed T2-weighted coronal image demonstrates an acute injury of the ACJ with disruption of the superior and inferior acromioclavicular ligaments (arrows), widening of the ACJ and superior displacement of the clavicle (arrowheads) relative to the acromion. The trapezius muscle (asterisk) is partially torn. (2b) The corresponding fat-suppressed T2-weighted coronal image anterior to the plane of the ACJ demonstrates tears of the conoid (c) and trapezoid (t) ligaments which comprise the coracoclavicular ligamentous complex. cp: coracoid process.
Diagnosis
Grade 3 acromioclavicular joint (ACJ) injury.
Injuries of the acromioclavicular joint (ACJ) are common, particularly in males involved in contact sports. The prototypical mechanism of injury to the ACJ involves a direct force produced when a patient falls on the shoulder with the arm adducted to the side. Although ACJ injuries occur with any contact sport, participants of hockey, rugby, and football are particularly vulnerable to ACJ injuries1. ACJ injuries account for approximately 10% of all shoulder injuries, occur five times more frequently in males, and occur most commonly in the second decade2.
Relevant Anatomy
The ACJ is a diarthrodial joint between the lateral surface of the clavicle and the medial surface of the acromion. Within the joint is a wedge-shaped fibrocartilaginous disk that projects into the joint from superior and inferior. The disk is not commonly visualized with routine MR imaging of the shoulder. The ACJ capsule is considered relatively weak with the strongest component at the superoposterior aspect, which is at the attachment site of the trapezius muscle3. The superior and inferior components of the acromioclavicular ligament complex reinforce the joint at small degrees of distraction4. With routine MR imaging, the ACJ capsule cannot be differentiated from the acromioclavicular ligaments, which insert into the capsule (3a). The trapezius and deltoid muscles are dynamic stabilizers and are particularly important when the ligamentous structures are torn. The trapezius has insertions sites at the superior aspects of the spine of the scapula and acromion. The deltoid muscle has sites of origin from the inferolateral spine of the scapula and acromion5. The superior acromioclavicular ligament blends into the aponeuroses of the deltoid and trapezius muscles6.
The coracoclavicular ligament complex is the main stabilizer of the ACJ, particularly at large degrees of separation4. The coracoclavicular ligament complex main function is that of vertical stabilization, which prevents superior and inferior translation of the clavicle7. The coracoclavicular ligament complex has two components, the conoid and trapezoid ligaments. The two ligaments anatomically form a V-shape and are separated by fat or a bursa5. In some patients, the fat separating the ligaments is sparse and the two components are confluent with one another (4a and 5a). The normal coracoclavicular ligaments are best visualized with T1 or proton density weighted images without fat suppression and can be visualized in the coronal and sagittal oblique planes.
The more medial component is the conoid ligament and is named for its triangular shape. The inferior apex of the conoid ligament is attached to the coracoid process. The conoid ligament spirals vertically and attaches to the conoid tubercle of the clavicle, which is at the junction of the lateral and middle thirds of the clavicle5. The conoid ligament’s main function is to prevent anterior and superior displacement of the clavicle6.
The more lateral component of the coracoclavicular ligament complex is the trapezoid ligament, named for its quadrilateral shape. The inferior segment of the trapezoid ligament is attached to the coracoid process and the superior segment is attached to the inferior aspect of the clavicle. The trapezoid ligament stabilizes against posterior clavicular displacement as well as providing resistance against anterior, superior, and inferior forces5,6.
Mechanism of Injury
With a direct force on the shoulder, the shoulder girdle and scapula are driven downward relative to the clavicle. When this happens, one of two injuries can occur: ACJ injury or clavicular fracture (or a combination of the two). Depending on the mechanism of injury, other directions of force can occur such as force in the anterior to posterior direction. ACJ injuries represent a continuum of ligament injuries. The mildest injury is a mild sprain of the AC ligaments. The next level of injury involves the coracoclavicular ligaments. The most severe level of injury involves injuries of the deltoid and trapezius muscular attachments. With more severe levels of injury, the upper extremity drops downward relative the distal clavicle and in extreme cases the skin overlying the AC joint can also be disrupted. In the rare situations, a severe direct force on the superior aspect of the distal clavicle with the arm in abduction will displace the clavicle inferiorly, below the level of the acromion or the coracoid1.
Although less common than direct force trauma, indirect forces may also cause ACJ injuries. A significant force can be transmitted to the AC joint via the humeral head from impaction injuries to the elbow or an outstretched hand. The humeral head impacts on the acromion and these injuries typically cause isolated ACJ injury without involvement of the coracoclavicular ligaments. These patients are also at higher risk for either fracture of the acromion or rotator cuff tear8. Uncommonly, a downward force produced by a pull mechanism while carrying a heavy load may cause an ACJ injury1.
Clinical Evaluation
Depending on the severity of the injury and patient’s body habitus, deformities of the ACJ may be seen on visual inspection. Palpation of the ACJ is performed to evaluate for deformities and areas of tenderness. If no luxation of the ACJ is present, reduction can be attempted by supporting the ipsilateral arm and applying a downward force on the distal clavicle to establish the type of ACJ injury1. In some situations, an abrasion is present over the superior aspect of the shoulder and can be seen at the site of impact. With more severe ACJ injuries, superior and inferior translation can be detected and this finding is called the “positive piano key sign”9. A shoulder shrug can be used to help differentiate between Grade 3 and 5 injuries shoulders. In a Grade 5 injury, the ACJ displacement is exaggerated in degree with the shoulder shrug8. Closed manipulation of the joint can help differentiate between Grade 3 and 5 injuries. If the deformity can be reduced, the deltotrapezial fascia is intact (Grade 3). If the deformity cannot be reduced, it suggests the deltotrapezial fascia is disrupted and the distal clavicle has buttonholed through the tear, preventing anatomic reduction (Grade 5)8.
Radiographic Evaluation
A routine radiographic series should be obtained on all patients with suspected ACJ injuries. Routine AP radiographs of the ACJ taken using a horizontal-beam technique may lead to superimposition of the ACJ on the spine of the scapula. The Zanca view uses a 10° to 15° cephalad angulation to better isolate the ACJ from other structures. Axillary projections can be performed to evaluate for anterior or posterior displacement of the distal clavicle9. Stress views of the ACJ are obtained using 10- to 15-lb of weight passively suspended from the upper extremity. Stress views are used to differentiate between Grade 2 and 3 injuries. Some authors have suggested that the usefulness of stress views do not outweigh the added cost, discomfort, and time7. The most important evaluation is the side-to-side comparison with the uninvolved side. It has been reported that an increase in the coracoclavicular distance of the injured shoulder over the asymptomatic contralateral shoulder by 25-50% represents complete coracoclavicular ligament disruption10,11.
CT imaging has no role in the routine evaluation of ACJ injuries. In certain circumstances, CT may add additional information if a complex fracture injury is also present that is not adequately defined with routine radiography.
At this time, MR imaging does not have a proven role in the routine evaluation of ACJ injuries. There is, however, no imaging modality that offers as much information regarding injuries to soft tissue structures. No other modality can directly image the coracoclavicular and acromioclavicular ligaments and muscle attachment sites of the deltoid and trapezius muscles. Osseous injuries are well evaluated with MR because of the inherent high sensitivity to fractures and also because the multiplanar images can display osseous displacement in relationship to adjacent structures.
The accuracy of MR imaging in staging of ACJ injuries has not been evaluated with Level I or Level II studies. Small published studies suggest that MR will detect injuries not suspected with routine clinical and radiographic staging. In a series of 13 patients, MR imaging results upgraded 20% of Grade 2 injuries and 50% of Grade 1 injuries12. In another small study of four patients, MR imaging showed disruption of the conoid and trapezoid ligaments in three patients with clinical Grade 2 and Grade 3 injuries. In a patient with a Grade 5 injury, only the trapezoid ligament was disrupted. The authors concluded that the clinical Rockwood classification did not correlate with the MR findings13. One report has indicated that MR can detect tears of the acromioclavicular ligaments3 but other reports indicate that MR cannot reliably detect acromioclavicular ligament tears in Grade 1 ACJ injuries5,12.
The current orthopaedic literature is in general agreement that routine MR imaging for ACJ injuries is not indicated8,9,14. If the prevailing local practice is to treat Grade 3 injuries conservatively, then MR imaging would have a limited role in that community. If the prevailing local practice is to surgically treat Grade 3 injuries, then MR imaging could have a role in differentiating Grade 2 from Grade 3 injuries when radiographic and clinical findings are equivocal. The role of MR imaging is evolving and for the time being should be used in selective cases to guide appropriate therapy. Another advantage of MR imaging is the ability to evaluate adjacent structures that may be injured. For example, the rotator cuff complex, labral complex, humeral head and glenoid can all be examined for possible injuries.
Rockwood Classification of ACJ injuries
The Rockwood classification for ACJ injuries is widely used in clinical practice. The classification system is unfortunately, in some respects, non-intuitive and non-linear. For example, Grade 1 through Grade 3 and then Grade 5 injuries represent a linear continuum of progressively more severe injuries whereas Grade 4 and 6 represent injuries that do not fit neatly into progression of the injuries. Logically, the classification should have two major categories: nonoperative ACJ injuries and operative ACJ injuries. Having said that, the following discussion is a review of the categories as they now exist.
Grade 1 injuries represent a sprain of the acromioclavicular ligament only without a complete tear (6a). The AC joint remains stable, and the ligaments are intact. ACJ tenderness is minimal to moderate without a palpable deformity (1). Radiographs are normal with and without weight bearing. As discussed earlier, it has been stated that MR imaging will show tears of the superior component of the acromioclavicular ligament in Grade 1 injuries3. Others have disagreed with this finding stating that no specific MR findings are seen with Grade 1 injuries, particularly in adults who commonly have pre-existing chronic findings that are indistinguishable from mild acute trauma5.
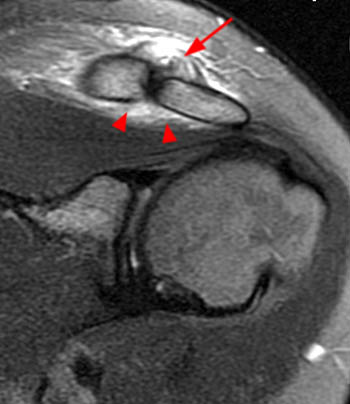
Figure 6:
A T2-weighted fat suppressed coronal oblique image demonstrates findings consistent with a Grade 1 ACJ injury. The superior acromioclavicular ligament is irregular and edematous with residual intact elements (arrow). The appearance is consistent with a partial tear. The inferior acromioclavicular ligament is not seen as a distinct structure but the presence of edema is consistent with a sprain injury (arrowheads).
Grade 2 injuries result in disruption of the ACJ capsule and ligaments. The distal end of the clavicle is unstable, but the coracoclavicular ligaments are intact (7a and 8a). The ACJ may be widened and if the coracoclavicular ligament is mildly stretched, downward displacement of the scapula may be present. Pain at the AC joint can be moderate to severe. The outer end of the clavicle may be slightly superior to the acromion1. Radiographs show a widened ACJ secondary to medial scapular rotation, slight elevation of the lateral end of the clavicle, and a normal or slightly increased coracoclavicular distance. MR imaging can demonstrate that the acromioclavicular ligaments are torn and the coracoclavicular ligaments are sprained or partially torn, as indicated by attenuation, edema, or hemorrhage of the ligament. The conoid component is most commonly involved in this injury. Bone marrow edema in the adjacent articular ends and soft-tissue swelling can occur during the acute phase3.
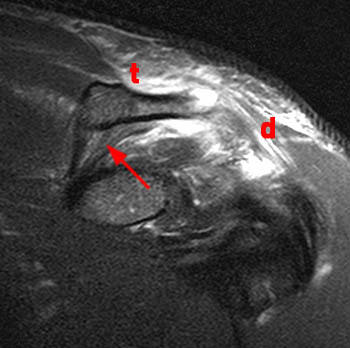
Grade 3 injuries involve complete tears of the acromioclavicular and coracoclavicular ligaments (9a,10a,11a). The injury may include tears of the deltoid and trapezius muscles3. The deltoid and trapezius muscles can be torn at the distal end of the clavicle, or the periosteal sleeve with muscle attachments can be stripped from the distal clavicle1. The ACJ is widened and the coracoclavicular distance is increased 25%-100%3. Grade 3 equivalent injuries occur with fractures of the coracoid process proximal to the conoid and trapezoid ligament attachments combined with acromioclavicular ligament disruption. Another Grade 3 variant occurs in children with type I or II Salter-Harris fractures of the distal clavicular growth plate. The distal clavicular metaphysis is displaced superiorly, the coracoclavicular ligaments are disrupted and the ACJ is intact3.
Grade 4 injuries are Grade 3 injuries that also have posterior displacement of the clavicle. This injury is a result of a force to the acromion that pushes the scapula posteriorly. The trapezius and deltoid muscles are torn from the clavicular insertions. A so-called “buttonholing” event can occur where the clavicle penetrates the trapezius3. Anterior dislocations of the sternoclavicular joint can also occur with Grade 4 injuries7.
A Grade 5 ACJ injury is a severe Grade 3 injury. The lateral trapezius and deltoid insertions, acromioclavicular and coracoclavicular ligaments are all torn. The unopposed pull of the sternocleidomastoid muscle results in an increase of the coracoclavicular distance of 100%-300%3. The clavicle may be displaced into the substance of the trapezius muscle5. On physical examination, the upper extremity droops inferiorly and the clavicle is notably prominent1.
Grade 6 ACJ injuries result from a superior blow to the clavicle and the distal clavicle luxates inferior to the acromion or coracoid. The acromioclavicular ligament and insertions of the deltoid and trapezius muscles are torn3. On physical examination, the shoulder has a flattened appearance, the acromion is prominent, and the superior surface of the coracoid process is palpable. Fractures of the clavicle and ribs and brachial plexus injuries are associated with Grade 6 injuries1.
Fractures of the distal clavicle or acromion can occur with any ACJ injury but particularly with Grade 3 and 4 injuries. Common fracture sites include the clavicular metaphysis or avulsion fractures involving the attachment sites of the acromioclavicular ligaments (12a). Posttraumatic osteolysis of the distal clavicle can occur after a single episode of trauma or with repetitive injuries or stresses3.
Treatment
The goals of ACJ injury treatment are normal pain-free range of motion of the shoulder, return of strength, and no limitations in activities. The type of treatment is decided by the type of injury, the patient’s occupation, the patient’s medical history, the acuity of the injury, patient expectations and physician preferences9.
Grade 1 and 2 ACJ injuries are treated nonoperatively and typically the joint retains some stability. Treatment consists of pain medications, ice, and a sling. Early active and passive motion and physiotherapy are recommended when the level of pain allows for it9.
The treatment of Grade 3 ACJ injury is controversial. Many published reports have shown that non-operative treatment for Grade 3 injuries provides satisfactory results for most patients. Nevertheless, the orthopaedic literature is replete with multiple articles describing different techniques, all of which, according to the authors, give excellent results9.
Grades 4-6 and open ACJ injuries are indications for surgical treatment but even these injuries can be treated non-operatively14. The different operative techniques are too numerous to list here, but involve the following fundamentals: primary fixation across the acromioclavicular joint, dynamic muscle transfer, fixation between the clavicle and the coracoid, and ligament reconstruction9.
Conclusion
ACJ injuries are common, particularly in males involved in contact sports. MR imaging does not have a role in routine imaging of ACJ injuries. MR imaging is, however, the most comprehensive imaging modality for the spectrum of soft tissue and osseous abnormalities that occur with ACJ injuries, and of course MR is able to detect numerous other internal derangements that may account for pain at the upper shoulder. MR imaging can differentiate Grade 2 from Grade 3 injuries, which aids in the selection of patients who may benefit from surgery.
References
1 Beim GM. Acromioclavicular Joint Injuries. J Athl Train 2000; 35:261-267.
2 Bucholz RW, Heckman JD. Acromio- clavicular joint injuries. In:Rockwood and Green?s fractures in adults. 5th ed. Philadelphia: Lippincott Williams & Wilkins, 2001; 1210 ?1244.
3 Alyas F, Curtis M, Speed C, Saifuddin A, Connell D. MR imaging appearances of acromioclavicular joint dislocation. Radiographics 2008; 28:463-479; quiz 619.
4 Lee KW, Debski RE, Chen CH, Woo SL, Fu FH. Functional evaluation of the ligaments at the acromioclavicular joint during anteroposterior and superoinferior translation. Am J Sports Med 1997; 25:858-862.
5 Antonio GE, Cho JH, Chung CB, Trudell DJ, Resnick D. Pictorial essay. MR imaging appearance and classification of acromioclavicular joint injury. AJR Am J Roentgenol 2003; 180:1103-1110.
6 Fukuda K, Craig EV, An KN, Cofield RH, Chao EY. Biomechanical study of the ligamentous system of the acromioclavicular joint. J Bone Joint Surg Am 1986; 68:434-440.
7 Provencher MT, Mazzocca AD, Romeo AA. Injuries to the Acromioclavicular Joint in Adults and Children. In: DeLee JC, David Drez D, Miller MD, eds. DeLee: DeLee and Drez’s Orthopaedic Sports Medicine, 3rd ed. 3rd ed. Philadelphia: Saunders, 2009.
8 Rios CG, Mazzocca AD. Acromioclavicular joint problems in athletes and new methods of management. Clin Sports Med 2008; 27:763-788.
9 Macdonald PB, Lapointe P. Acromioclavicular and sternoclavicular joint injuries. Orthop Clin North Am 2008; 39:535-545, viii.
10 Rockwood CAJ, Young DC. Disorders of the acromioclavicular joint. In: Rockwood CAJ, Matsen FAI, eds. The Shoulder. Philadelphia: WB Saunders, 1990; 413?476.
11 Bearden JM, Hughston JC, Whatley GS. Acromioclavicular dislocation: method of treatment. J Sports Med 1973; 1:5-17.
12 Schaefer FK, Schaefer PJ, Brossmann J, Hilgert RE, Heller M, Jahnke T. Experimental and clinical evaluation of acromioclavicular joint structures with new scan orientations in MRI. Eur Radiol 2006; 16:1488-1493.
13 Barnes CJ, Higgins LD, Major NM, Basamania CJ. Magnetic resonance imaging of the coracoclavicular ligaments: its role in defining pathoanatomy at the acromioclavicular joint. J Surg Orthop Adv 2004; 13:69-75.
14 Mazzocca AD, Arciero RA, Bicos J. Evaluation and treatment of acromioclavicular joint injuries. Am J Sports Med 2007; 35:316-329.