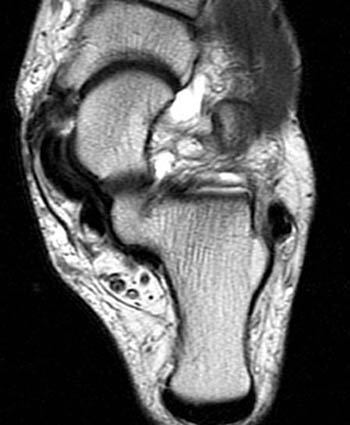
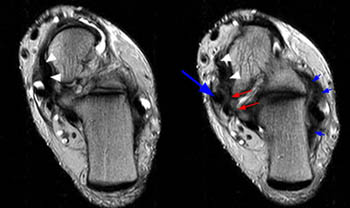
Clinical History: A 59 year-old male with a 3 year history of medial ankle pain is referred for MR imaging. (1a) Fat-suppressed proton density-weighted coronal and (1b) T2-weighted axial oblique images are provided. What are the findings” What is your diagnosis?
Findings
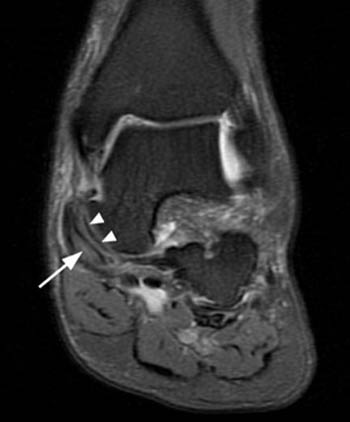
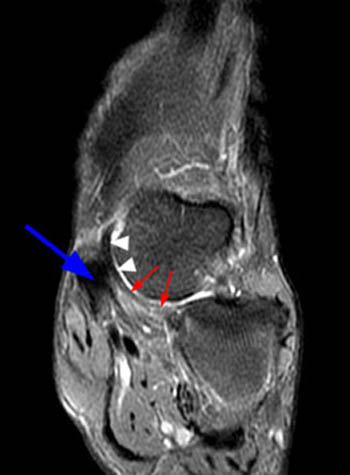
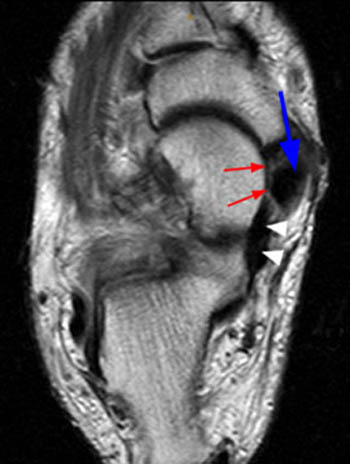
Figure 2:
(2a) The fat-suppressed proton density-weighted coronal image demonstrates abnormal thickening and increased signal intensity of the distal posterior tibial tendon (arrow). The superomedial portion of the calcaneonavicular (spring) ligament is diffusely thinned and attenuated (arrowheads).
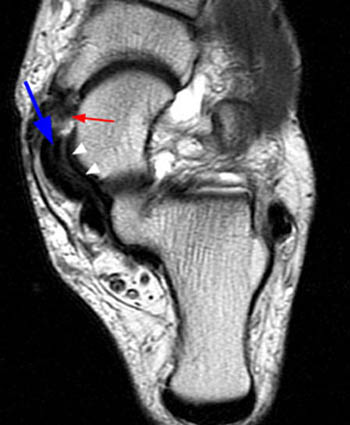
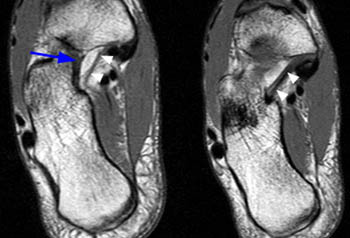
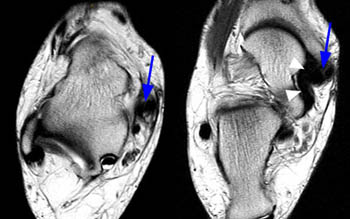
Figure 3:
(3a) The T2-weighted axial oblique image through the ankle demonstrates a thickened posterior tibial tendon with partial tear along the deep surface (arrow). The superomedial portion of the calcaneonavicular (spring) ligament is diffusely thinned (arrowheads) and torn distally at the navicular insertion (small arrow).
Diagnosis
Partial tear of the posterior tibial tendon with a distal tear of the superomedial calcaneonavicular (spring) ligament.
Introduction
The posterior tibial tendon is the most commonly injured tendon at the foot and ankle. Insufficiency of the posterior tibial tendon has been recognized as the primary cause of acquired flatfoot deformity in adults.1 More recently, the importance of the static stabilizers of the foot in maintaining the medial longitudinal arch has been emphasized. The calcaneonavicular ligament (spring ligament) complex is a key static stabilizer of the arch and is frequently injured in association with posterior tibial tendon insufficiency. In patients with acquired flatfoot deformity, an isolated repair of the posterior tibial tendon may result in a poor long-term functional outcome, if coexistent abnormalities of the spring ligament are not addressed.2,3
Anatomy and Function
The medial longitudinal arch of the foot is maintained by static and dynamic stabilizers of the calcaneus, talus, navicular, and medial cuneiforms. The posterior tibial tendon is the most important dynamic stabilizer, serving to invert the hindfoot and lock the transverse tarsal joint through the middle and late phase of gait. With failure of posterior tibial tendon function, the contracting gastrocnemius soleus muscle complex generates forces which act abnormally across the talonavicular joint rather than the metatarsal heads.3 This places an abnormal load on the static stabilizers of the arch, most significantly affecting the calcaneonavicular (spring) ligament complex.4
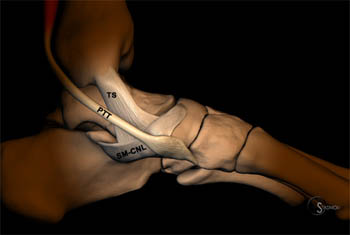
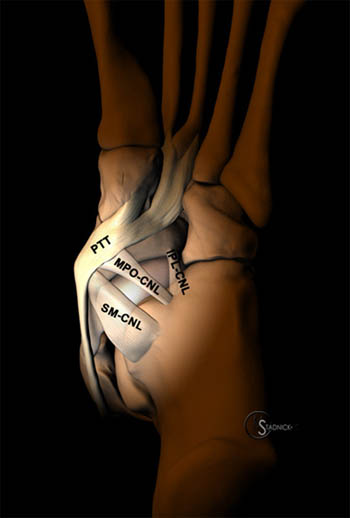
Figure 4:
Medial and plantar 3D representations of the midfoot demonstrate the 3 major components of the spring ligament complex, the superomedial (SM-CNL), medioplantar oblique (MPO-CNL), and inferoplantar longitudinal (IPL-CNL) calcaneonavicular ligaments. The posterior tibial tendon (PTT) and tibiospring ligament (TS)are also demonstrated.
The spring ligament complex forms the medial and plantar margins of the articular cavity of the head of the talus and has 3 components. The superomedial calcaneonavicular ligament (SM-CNL) is the strongest component of the spring ligament complex and extends from the sustentaculum tali to the dorsal aspect of the medial navicular. The posterior tibial tendon (PTT) lies immediately superficial to the SM-CNL and is separated by a layer of loose connective tissue. Histologically, fibrocartilage elements are present along the deep portion of the SM-CNL, which articulates with the head of the talus. A gliding zone is present between the PTT and the SM-CNL composed of fibrocartilage elements in both the deep layer of the PTT and the superficial layers of the SM-CNL. A thin synovial layer is present along both surfaces. The SM-CNL is usually seen on routine axial (5a) and coronal MR images (6a). Axial oblique images of the ankle are also helpful in visualizing the SM-CNL. Differentiation of the SM-CNL and PTT is often difficult at their point of contact; however the SM-CNL is readily differentiated proximal to this level. The tibiospring ligament is the anterior, superficial portion of the deltoid ligament complex and fuses with the superior margin of the SM-CNL (7a).
The inferoplantar longitudinal calcaneonavicular ligament (IPL-CNL) is seen along the plantar aspect of the anterior talus and extends from the coronoid fossa of the calcaneus just anterior to the sustentaculum tali and inserts on the lateral plantar aspect of the navicular, at the the inferior beak of the navicular.1 This ligament may be seen on sagittal, coronal, and axial or axial oblique images (8a). The medioplantar oblique calcaneonavicular ligament (MPO-CNL) is the third component of the spring ligament complex. Previously the MPO-CNL and IPL-CNL were considered a single plantar calcaneonavicular ligament. However, recent anatomic dissections have identified the MPO-CNL as a separate ligament.5 The MPO-CNL originates at the coronoid fossa of the calcaneus just anterior to the IPL-CNL and has a medial oblique course attaching at the medioplantar navicular, just plantar to the navicular tuberosity (8a).
Figure 6:
(6a) A fat-suppressed proton-density weighted coronal image of the ankle demonstrates the normal appearance of the superomedial portion of the spring ligament (arrowheads), which is seen deep to the posterior tibial tendon (arrow). The inferior portion of the spring ligament complex, consisting of the inferoplantar and medioplantar oblique components, demonstrates greater heterogeneity of signal because of interposed fat between the ligament bundles (small arrows).
Figure 7:
(7a) A more posterior fat-suppressed proton density-weighted coronal image demonstrates the tibiospring portion of the deltoid ligament complex (arrow) fusing with the superior margin of the superomedial spring ligament (arrowheads). The posterior tibial tendon (arrow) is clearly discernible as separate from the superomedial spring ligament at this level.
Clinical Presentation
Spring ligament injuries have a high association with posterior tibial tendon tears.1 Spring ligament tears, like posterior tibial tendon tears, are most commonly seen in middle-aged women and are most often the result of chronic degeneration.6 Disruption of the spring ligament destabilizes the longitudinal arch, allowing plantar and medial rotation of the head of the talus and valgus alignment of the calcaneus (pes planovalgus). The clinical result is an acquired flatfoot deformity.
Clinical symptoms are similar to those of posterior tibial dysfunction. Early in the disease process the patient may complain of vague, activity-related pain at the medial ankle and foot or difficulty with balance and walking on uneven ground. Later, as the pes planovalgus deformity progresses, the patient often complains of activity related pain in the sinus tarsi and lateral malleolus, presumably because of impingement of lateral structures. With the development of subtalar and transverse tarsal osteoarthritis, the patient presents with pain, stiffness, and swelling.7
Acute injuries of the spring ligament are rare but have been described. Isolated tears of the spring ligament without associated PTT tear are extremely rare and can present as an acquired flatfoot deformity.8
MRI Appearance of Tears
The SM-CNL is the most important spring ligament component for providing functional stability of the arch and is also the most frequently injured spring ligament component.9 Efforts at evaluating the integrity of the spring ligament complex should focus on the SM-CNL.4 Published reports give a mean thickness for the SM-CNL ranging from 2.5 mm to 4.7mm, suggesting significant interobserver variability and possible inconsistent methods of assessing thickness.5,10 In pathologic states the SM-CNL frequently thickens. A measurement of 4 mm has been suggested as the threshold beyond which the spring ligament is abnormal.1 Our experience suggests this value may be frequently exceeded in the normal population. We prefer to utilize a threshold value of 5 mm or greater in addition to abnormal ligament contour and signal characteristics, and the presence of associated posterior tibial tendon pathology.9 Atretic ligament tears are also frequently seen and demonstrate an abnormally thinned SM-CNL (<2mm) usually accompanied by discontinuity of the ligament and surrounding edema. In almost all instances of spring ligament tears or laxity, accompanying posterior tibial tendon abnormalities are present.
As in the test case (1a,1b), tears of the SM-CNL may be seen as abnormal thinning of the ligament. More often, the SM-CNL is abnormally thickened with intrinsic signal heterogeneity on T1 and T2 weighted images (9a).4 This appearance is the least specific for identifying a spring ligament tear, but is considered abnormal and should prompt a careful search for additional signs of ligament insufficiency.
Laxity of the spring ligament is frequently observed in association with stretching of fibers or a full-thickness ligamentous defect (10a). The most specific finding of a ligament tear is a fluid-signal filled discontinuity of the ligament on T2-weighted sequences, representing a tear through the full thickness of the spring ligament. Tears most commonly occur at the distal or proximal attachment sites of the SM-CNL (10a,11a).
Figure 10:
(10a) Sequential T2-weighted axial images in a patient with a partial tear of the distal posterior tibial tendon (arrow), demonstrate an abnormally lax and thickened SM-CNL along its anterior fibers (arrowheads). The posterior fibers of the SM-CNL are torn near the sustentaculum (small arrows). Also noted is abnormal thickening of the anterior talofibular and calcaneofibular ligaments (short arrows) indicating scarring secondary to prior ligament sprains.
Signal heterogeneity due to fat interposed between the IPL-CNL and MPO-CNL components is normal and should not be confused with a ligament tear (6a,8a). The IPL-CNL and MPO-CNL components of the spring ligament complex are less frequently torn. Of the two, the MPO-CNL is more susceptible to injury due to its close proximity to the SM-CNL.
MRI Operative Repair
Current repair options for an acquired flatfoot vary depending on the severity of the flatfoot deformity, and center around repair of the PTT. Transfers of the flexor digitorum longus tendon are commonly performed in conjunction with a medial calcaneal slide osteotomy to correct mild deformity. With more severe flatfoot deformities, lateral column lengthening procedures or fusions are being incorporated. In many instances the patient is left with a stiff foot and is prone to developing arthritis. As a result, orthopaedic surgeons have more recently focused efforts on evaluating and correcting associated spring ligament complex injuries, resulting in a more anatomic repair. Reconstruction or augmentation methods for spring ligament tears or laxity include the use of anterior deltoid, peroneal tendon graft, split thickness tibialis anterior tendon graft, posterior tibial tendon stump, or suture repair.3
Conclusion
Posterior tibial tendon tears are a frequent cause of flatfoot deformity. In many cases, an associated tear of the spring ligament is present. Spring ligament tears usually involve the superomedial calcaneonavicular ligament portion of the ligament, which is the most important static stabilizer of the longitudinal arch. MRI provides optimal visualization of the spring ligament, but abnormalities of this complex structure are frequently overlooked by those who interpret MRI. Proper knowledge of anatomy and pathology of the spring ligament complex enables the careful MR reader to diagnose spring ligament tears. This in turn allows the surgeon to provide a more complete and functional repair of the longitudinal arch.
References
1 Mengiardi B, Zanetti M, Schottle PB, Vienne P, Bode B, Hodler J, Pfirrmann CWA. Spring Ligament Complex: MR Imaging-Anatomic Correlation and Findings in Asymptomatic Subjects. Radiology 2005; 237:242-249.
2 Michelson J, Conti S, Jahss MH. Survivorship analysis of tendon transfer surgery for posterior tibial tendon rupture. Orthop Trans 1992; 16:30.
3 Gazdag AR, Cracchiolo A 3rd. Rupture of the posterior tibial tendon: evaluation of injury of the spring ligament and clinical assessment of tendon transfer and ligament repair. J Bone Joint Surg Am 1997;79:675-681.
4 Balen PF, Helms CA. Association of Posterior Tibial Tendon Injury with Spring Ligament Injury, Sinus Tarsi Abnormality, and Plantar Fasciitis on MR Imaging. AJR 2001;176:1137-1143.
5 Taniguchi A, Tanaka Y, Takakura Y, Kadono K, Maeda M, Yamamoto H. Anatomy of the spring ligament. J Bone Joint Surg Am 2003;85-A:2174-2178.
6 Holmes GB, Mann RA. Possible epidemiological factors associated with rupture of the posterior tibial tendon. Foot and ankle 1992;13:70-79.
7 Pomeroy GC, Pike RH, Beals TC, Maoli A 2nd. Acquired Flatfoot in Adults Due to Dysfunction of the Posterior Tibial Tendon. J Bone Joint Surg Am 1999;81-A:1173-1182.
8 Borton D, Saxby T. Tear of the plantar calcaneonavicular (spring) ligament causing flatfoot. J Bone Joint Surg Br 1997;79B:641-643.
9 Toye LR, Helms CA, Hoffman BD, Easley M, Nunley JA. MRI of Spring Ligament Tears. AJR 2005;184:1475-1480.
10 Yao L, Gentili A, Cracchiolo A. MR imaging findings in spring ligament insufficiency. Skeletal Radiol 1997;26:310-312.