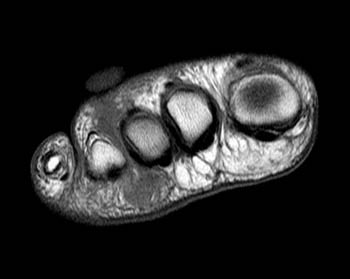
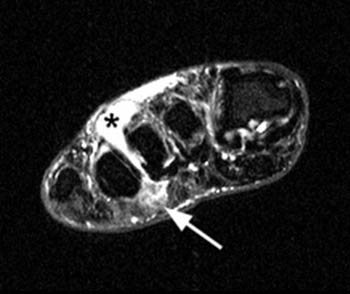
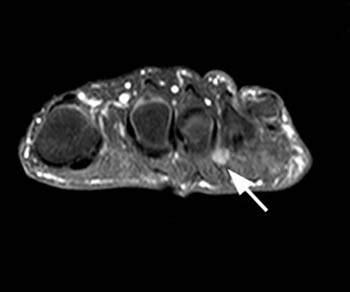
Clinical History: 45 year-old female with pain and swelling in the web space between the 3rd and 4th toes. (1a) T1-weighted coronal and (1b) T2-weighted fat-suppressed coronal images through the distal metatarsals are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Morton neuroma in the 3rd intermetatarsal space, with associated intermetatarsal bursitis.
Discussion
Morton neuroma was originally described in 1876 by Thomas Morton.1 Because this process was initially thought to be a neoplasm of the interdigital nerve, it was referred to as a neuroma. In actuality, Morton neuroma is non-neoplastic. A true neuroma represents a proliferation of nerve tissue, either as a primary neoplasm or in response to nerve amputation. With Morton neuroma, swelling of the common digital nerve and perineural fibrosis result in mass-like enlargement, but a true neoplasm is not present.
Morton neuroma is felt to most likely represent an entrapment syndrome. The common plantar digital nerve passes deep to the intermetatarsal ligament and into a relatively small space between the metatarsal heads (4a). Entrapment occurs when this confined space is further compromised on a repetitive basis. Morton neuroma most commonly occurs in the third intermetatarsal space, followed by the second intermetatarsal space.2 Anatomically, the second and third intermetatarsal spaces are smaller than the first or fourth intermetatarsal spaces. Young and middle-aged women are most commonly affected, which has been attributed to the belief that poorly fitting shoes in the toe region and high heels contribute to neuroma formation. Athletes who spend a significant portion of their activity on the ball of the foot, such as sprinters, are also at greater risk.
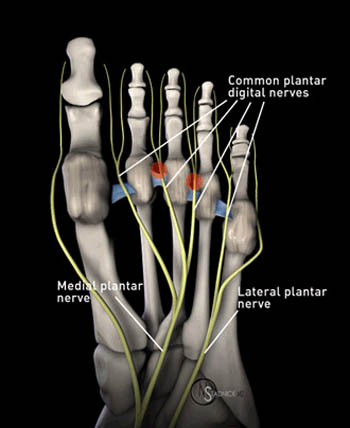
Figure 4:
(4a) A plantar view of the foot demonstrates the common plantar digital nerves passing plantar to the intermetatarsal ligaments (indicated in blue) in this 3D graphic representation. Morton neuromas arise from the common plantar digital nerves immediately distal to the intermetatarsal ligaments (indicated by red).
The typical clinical presentation for Morton neuroma is progressive pain, throbbing, and numbness radiating from the web space into the toes. There may be a sensation of walking on a marble. A palpable mass may be present, however, physical examination is frequently inconclusive. A wide range of clinical conditions may mimic Morton neuroma, including metatarsal stress fractures, Frieberg’s infraction, intermetatarsal bursitis, and synovial cysts. It should be noted that a significant percentage of Morton neuromas (up to 30%) are asymptomatic and demonstrate no gender predilection. These tend to be smaller lesions, whereas larger lesions are more commonly symptomatic.3
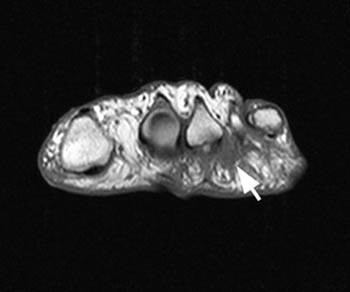
The MRI appearance of Morton neuroma is that of a tear-drop shaped soft tissue mass between the metatarsal heads, projecting inferiorly into the plantar subcutaneous fat and located on the plantar side of the intermetatarsal ligament (5a). The mass is typically intermediate in signal intensity on T1-weighted images. On T2-weighted images, fibrosis results in relatively low signal intensity. Fluid may be present in the intermetatarsal bursa secondary to associated inflammation (2a). Although intermetatarsal fluid is common in the asymptomatic population, larger collections (greater than 3mm in transverse dimension) are more likely to be associated with Morton neuroma.3 Gadolinium-enhanced MRI greatly improves the conspicuity of the neuroma (6a), which typically enhance.
The treatment of Morton neuroma begins with conservative measures. Modification of footware and steroid injections successfully treat most individuals.4 Surgery is reserved for those patients with a poor response to conservative measures. Surgical approaches include transection of the intermetatarsal ligament and nerve resection. Ironically, in a small percentage of patients, nerve resection may result in a stump neuroma that leads to dysesthesias of the innervated toes. Additional surgery may be required in this subset of patients.
Conclusion
Morton neuroma is a commonly encountered cause of pain in the forefoot. The MRI appearance is characteristic, enabling an accurate diagnosis of Morton neuroma and ready differentiation from other etiologies that have a similar clinical presentation.
References
1 Morton TG: Peculiar painful affection of fourth metatarsophalangeal articulation . Am J Med Sci 1876; 71: 37.
2 Alexander IJ, Johnson KA, Parr JW. Morton’s neuroma: a review of recent concepts. orthopaedics 1987;10:103-106.
3 Zanetti M, Strehle JK, Zollinger H, Hodler J. Morton neuroma and fluid in the intermetatarsal bursae on MR images of 70 asymptomatic volunteers. Radiology 1997;203:516-520.
4 Gaynor R, Hake D, Spinner SM, et al: A comparative analysis of conservative versus surgical treatment of Morton’s neuroma. J Am Podiatr Med Assoc 1989;79(1):27-30.