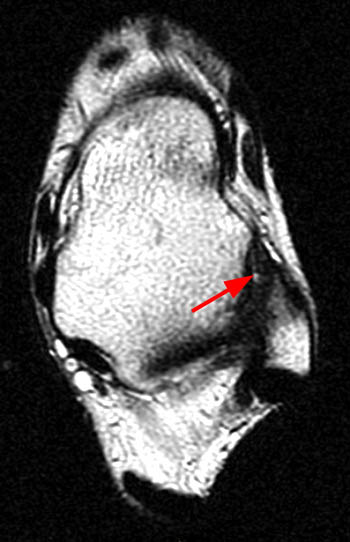
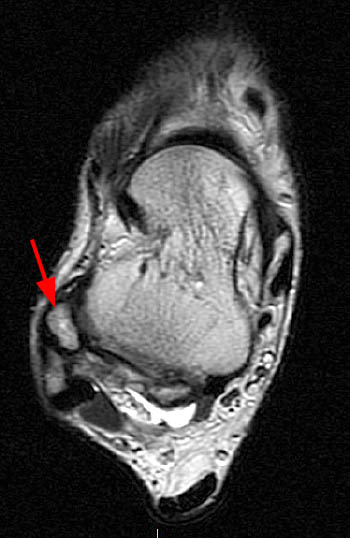
Clinical History: A 16 year-old female presents with chronic anterolateral ankle pain and a history of injury one year prior. Oblique axial proton density-weighted (1A) and coronal (1B) and sagittal (1C) T2-weighted fat-suppressed images are provided. What are the findings? What is your diagnosis?
Figure 1:
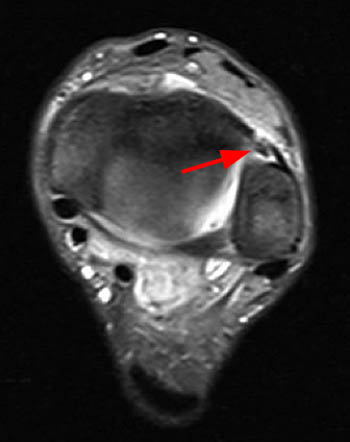
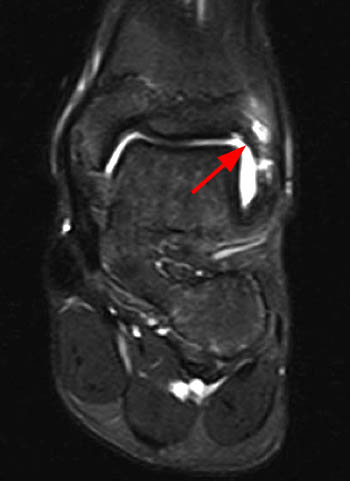
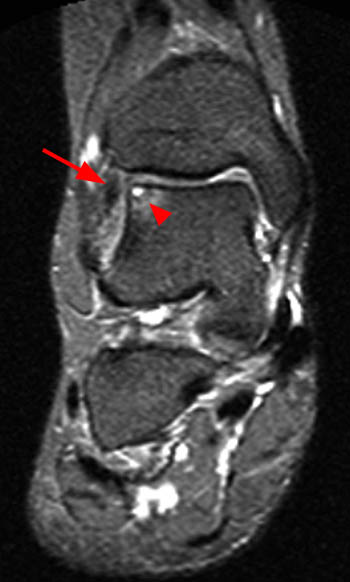
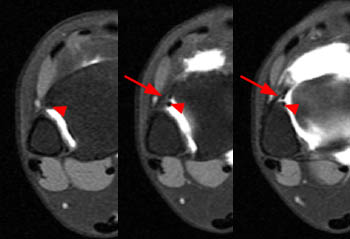
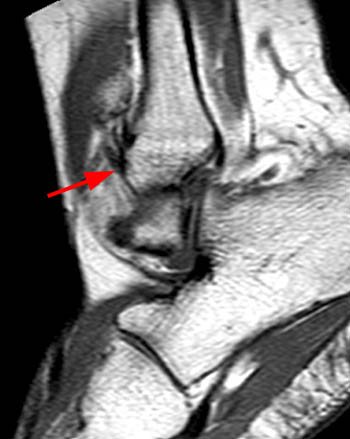
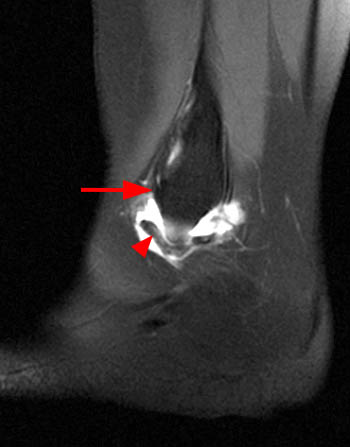
Oblique axial proton density-weighted (1A) and coronal (1B) and sagittal (1C) T2-weighted fat-suppressed images demonstrate an abnormally thickened accessory anterior inferior tibiofibular (Bassett's) ligament (arrows), surrounded by prominent fluid and/or synovitis within the anterolateral ankle gutter.
Diagnosis
Thickened accessory anterior inferior tibiofibular (Bassett’s) ligament, contributing to anterolateral impingement.
Introduction
Anterolateral ankle impingement is a common cause of chronic ankle pain, typically following inversion injury1, 2, 3. Multiple factors may contribute to pain from anterolateral impingement, including synovitis, hyalinized scar tissue, and chondral injury of the talar dome3. A lesser known contributing factor to anterolateral impingement is a thickened accessory anterior inferior tibiofibular ligament1, 4. This accessory ligament is an anatomical variant present in the most ankles1, 4, 5, which may become sprained and pathologically thickened in the setting of inversion injury, resulting in impingement and mild residual anterior instability1, 3.
Anatomy
The distal tibiofibular joint is composed of a ligamentous complex including the anterior inferior tibiofibular ligament (AITFL), the posterior inferior tibiofibular ligament (PITFL), and the interosseous ligament. Posteriorly, a transverse ligament is also present, which coalesces with the PITFL to form the so called tibial slip or intermalleolar ligament6.
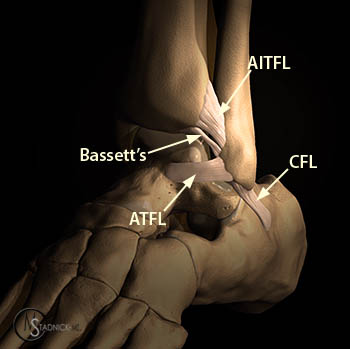
The AITFL is a flat band typically attaching to the distal tibia approximately 5 mm above the articular surface, anterior to the interosseous ligament, descending obliquely, attaching to the anterior aspect of the lateral malleolus4,3 (Figure 2). The length ranges from 12-22 mm, thickness from 1.5-3 mm, and width from 9-22 mm (at the tibial attachment) to 7-12 mm (at the fibular attachment)4.
A distal separate ligament or fascicle of the AITFL has been described, located just distal to the AITFL, the accessory anterior inferior tibiofibular ligament. The structure was originally described by Nikolopoulos in a Greek 1982 thesis but never published in the English literature7, 4. Basset et al. first described the structure in the English literature, and also first described an associated impingement upon the talar dome, , found at both arthroscopy and cadaveric dissections. Bassett described the structure as an accessory fascicle to the AITFL, present in most human ankles (found in 10/11 cadavers). Nikolopoulos later performed additional cadaveric studies concluding the structure was a distinct separate ligament from the AITFL due to the presence of an intervening fibrofatty septum4, 3.
The accessory anterior inferior tibiofibular ligament (also published in the radiology literature as “Bassett’s ligament”)8 runs parallel and distal to the AITFL, also attaching to the tibia and fibula (Figure 3). The distal attachment of Bassett’s ligament approximates the fibular attachment of the anterior talofibular ligament (ATFL)9, 3. The length ranges from 17-22 mm, thickness from 1-2 mm, and width from 3-5 mm9, 3.
Figure 3:
Cadaveric specimen shown in the lateral orientation demonstrates the relationships of the AITFL (black arrow), Bassett's ligament (white arrow), and the ATFL (blue arrow) and their sites of attachment on the lateral malleolus (asterisk). Photograph courtesy of Emily N. Vinson, MD, Duke University Medical Center.
Pathology
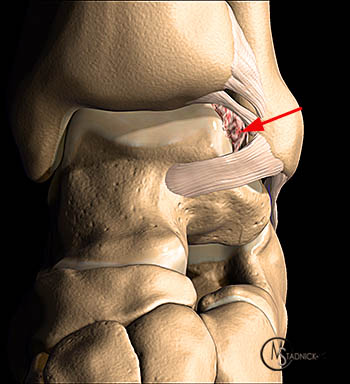
Repetitive microtrauma may result in hypertrophied synovial tissue and fibrosis within the anterolateral gutter, contributing to pain and anterolateral impingement10, 11, 12. In advanced cases, the mechanical impingement may mold tissue into a hyalinized “meniscoid lesion”, originally described by Wolin et al13, 4 (Figure 4).
Basset et al. postulated that post-traumatic anterolateral hyperlaxity, due to an injured ATFL, results in anterior extrusion of the talar dome with dorsiflexion, contacting the accessory inferior fascicle of the AITFL, with more pressure and friction1, 3. This results in thickening of the accessory AITFL, contributing to anterolateral impingement (Figure 5). Of note, the AITFL may still be normal in the presence of a pathologic accessory AITFL1, 8.
Akseki et al. postulated that variations in the width, length, and obliquity of the accessory AITFL fascicle may result in pathology5. Wider and longer fascicles are potentially at greater risk. A fibular attachment point far from the joint level was also thought to result in greater risk.
Several authors report the association of talar dome chondral abrasion with the presence of a pathologic accessory AITFL. Anterior and anterolateral talar dome articular cartilage abrasion has been reported to be present in 82.9%9, 17%5, and 71%1 of cases of an abnormal accessory AITFL. Presumably the abnormally thickened accessory AITFL contacts the superolateral talar dome, resulting in the cartilage abrasion3 (Figure 6).
Imaging
Subhas et al. reported Bassett’s ligament to be visible in all three standard MR imaging planes, seen most commonly (89%) with sequential axial images8. Due to the anatomic orientation of Bassett’s ligament, coronal imaging is often easiest to visualize the low signal fibers paralleling the course of the AITFL, and separated by a band of higher signal (Figure 7). Axial images are useful to identify the fibular attachment located inferior and slightly medial to the AITFL fibular attachment (Figure 8). Sagittal images again demonstrate Bassett’s ligament inferior to the fibular attachment of the AITFL, at or below the apex of the anterior fibular contour (Figure 9). The tibial attachment of Bassett’s ligament may be less conspicuous due to blending of fibers with the AITFL.
Figure 9:
Sagittal T1 (Figure 9) and fat-suppressed proton density-weighted (Figure 9b) images in two different patients demonstrating the fibular attachment of Basset's ligament, located inferior to that of the AITFL, located at or inferior to the to the apex of the fibular contour (arrow). Figure 10 also demonstrates an abnormally thickened ATFL (arrowhead).
Due to the small size of Bassett’s ligament, determining normal from pathologic thickening can be difficult, with greater degrees of thickening having greater chances of being pathologic. In the study of Subhas et al., a Bassett’s ligament thickness of greater than 3 mm was 89% specific for subsequent arthroscopic pathology8.
Irregular or nodular low signal tissue between the AITFL and ATFL has a high correlation with anterolateral scarring and/or synovitis11. The absence of a fluid filled recess between the anterolateral soft tissues and the anterior surface of the fibula has also been described as a sign of scarring and/or synovitis10, 11 (Figure 10). If present, osseous fragments or spurs may also contribute to anterolateral impingement (Figure 11).
Figure 11:
Osseous contributions to anterolateral impingement. An axial T2-weighted image (Figure 11a) demonstrates an ununited avulsion ossification in the anterolateral gutter (arrow). An axial T1-weighted image (Figure 11b) in a different patient demonstrates prominent osseous spurs along the anterior joint (arrows).
Management
If conservative treatment fails, arthroscopic debridement is considered a safe and effective method to confirm and treat anterolateral impingement[14 Urgüden M, Söyüncü Y, Ozdemir H, Sekban H, Akyildiz FF, Aydin AT. Arthroscopic treatment of anterolateral soft tissue impingement of the ankle: evaluation of factors affecting outcome. Arthroscopy. 2005 Mar;21(3):317-22.]. Diagnostic ankle arthroscopy is first performed in a systematic fashion, evaluating for synovitis, scar tissue, a thickened Bassett’s ligament, and chondromalacia of the talar dome2. Debridement of hypertrophic scar tissue is performed. If present, an abnormally thickened Bassett’s ligament is excised1, 14. Loose bodies may be removed. Chondroplasty is also performed, as necessary2. Postoperatively, the patient is placed in a soft dressing for a few days. Early physical therapy is begun shortly after, involving gentle movement, muscle strengthening, proprioceptive balancing exercises, and weight-bearing as tolerated15. Factors that negatively affect outcome include chondral lesions of the talar dome, associated syndesmotic lesions, and new inversion injuries after surgery15.
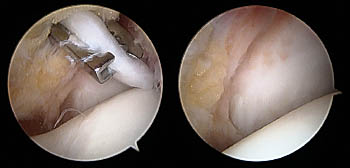
Figure 12:
Intraoperative images demonstrate arthroscopic removal of a thickened Bassett's ligament (same patient as the Figure 1 MRI). The left image demonstrates a thickened Bassett's ligament (white band of tissue) surrounded by a surgical "biter". The image on the right is post-resection. The smooth surface on the bottom of the images represents the talar dome. The white surface behind Bassett's ligament is the lateral malleolus. Images courtesy of Shay Tenenbaum, MD, Chris Royer, MD, and James Brodsky (Baylor University Medical Center, Dallas TX).
Conclusion
An accessory anterior inferior tibiofibular (Bassett’s) ligament is an anatomical variant within most ankles. An injured Bassett’s ligament may result in pain due to mild anterior instability (allowing slight anterior translation of the talus) and anterolateral impingement. A pathologically thickened Bassett’s ligament and other causes of anterolateral impingement can be demonstrated with preoperative MRI. Awareness of an abnormal Bassett’s ligament, scar tissue, and associated talar dome chondral lesions can be useful in pre-operative planning.
Acknowledgments
Thanks to:
- Shay Tenenbaum, MD, Chris Royer, MD, James Brodsky, MD (Baylor University Medical Center, Dallas TX)
- Jeffrey Willers, MD, Lauren Erickson, PA-C, Rick Willard (Elite Orthopaedic, Nashville, TN)
- Emily Vinson, MD (Duke University Medical Center, Durham NC)
for assistance with images and support with this web clinic.
- Bassett FH, Gates HS, Billys JB, Morris HB, Nikolaou PK. Talar impingement by the anteroinferior tibiofibular ligament. A cause of chronic pain in the ankle after inversion sprain. J Bone Joint Surg Am. 1990 Jan;72(1):55-9. ↩
- Ferkel RD, Karzel RP, Del Pizzo W, Friedman MJ, Fischer SP. Arthroscopic treatment of anterolateral impingement of the ankle. Am J Sports Med. 1991 Sep-Oct;19(5):440-6. ↩
- van den Bekerom MPJ, Raven, EEJ. The distal fascicle of the anterior inferior tibiofibular ligament as a cause of tibiotalar impingement syndrome: a current concepts review. Knee Surg Sports Traumatol Arthrosc. 2007 Apr;15(4):465-71. ↩
- Nikolopoulos CE, Tsirikos AI, Sourmelis S, Papachristou G. The accessory anteroinferior tibiofibular ligament as a cause of talar impingement: a cadaveric study. Am J Sports Med. 2004 Mar;32(2):389-95. ↩
- Akseki D1, Pinar H, Yaldiz K, Akseki NG, Arman C. The anterior inferior tibiofibular ligament and talar impingement: a cadaveric study. Knee Surg Sports Traumatol Arthrosc. 2002 Sep;10(5):321-6. Epub 2002 Jun 4. ↩
- Hermans JJ, Beumer A, de Jong TA, Kleinrensink GJ. Anatomy of the distal tibiofibular syndesmosis in adults: a pictorial essay with a multimodality approach. J Anat. 2010 Dec;217(6):633-45. ↩
- Nikolopoulos CE. Anterolateral instability of the ankle joint: an anatomical, experimental and clinical study. 1982 Thesis, University of Athens, Athens, Greece. ↩
- Subhas N, Vinson EN, Cothran RL, Santangelo JR, Nunley JA, Helms CA. MRI appearance of surgically proven abnormal accessory anterior-inferior tibiofibular ligament (Bassett’s ligament). Skeletal Radiol. 2008 Jan;37(1):27-33. ↩
- Ray RG, Kriz BM. Anterior inferior tibiofibular ligament. Variations and relationship to the talus. J Am Podiatr Med Assoc. 1991 Sep;81(9):479-85. ↩
- Robinson P, White LM, Salonen DC, Daniels TR, Ogilvie-Harris D. Anterolateral ankle impingement: MR arthrographic assessment of the anterolateral recess. Radiology. 2001 Oct;221(1):186-90. ↩
- Robinson P, White LM. Soft-tissue and osseous impingement syndromes of the ankle: role of imaging in diagnosis and management. Radiographics. 2002 Nov-Dec;22(6):1457-69; discussion 1470-1. ↩
- Cerezal L, Abascal F, Canga A, Pereda T, García-Valtuille R, Pérez-Carro L, Cruz A. MR imaging of ankle impingement syndromes. Am J Roentgenol. 2003 Aug;181(2):551-9. ↩
- Wolin I, Glassman F, Sideman S, Levinthal DH. Internal derangement of the talofibular component of the ankle. Surg Gynecol Obstet. 1950 Aug;91(2):193-200. ↩
- Kim SH, Ha KI. Arthroscopic treatment for impingement of the anterolateral soft tissues of the ankle. J Bone Joint Surg Br. 2000 Sep;82(7):1019-21. ↩
- Moustafa El-Sayed AM. Arthroscopic treatment of anterolateral impingement of the ankle. J Foot Ankle Surg. 2010 May-Jun;49(3):219-23. ↩