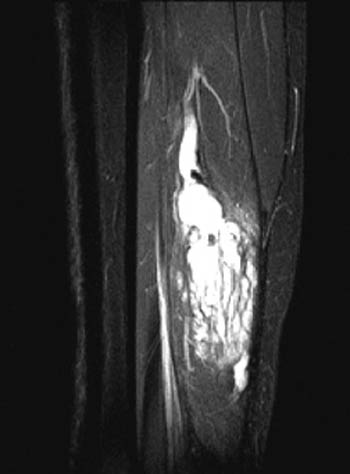
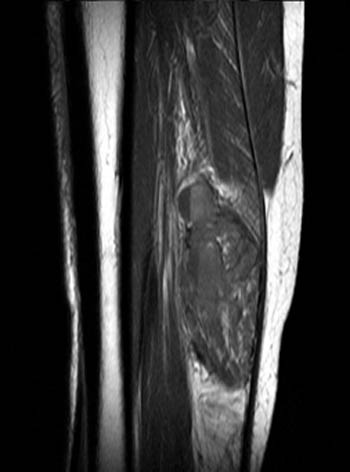
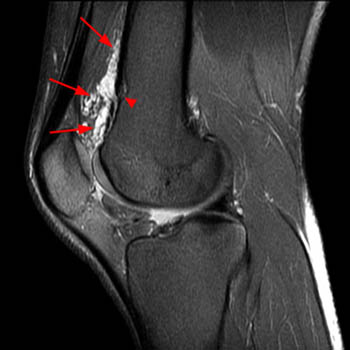
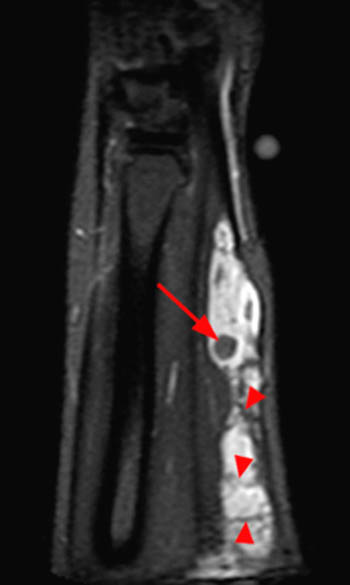
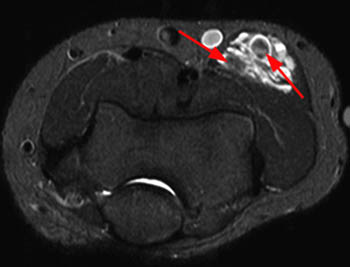
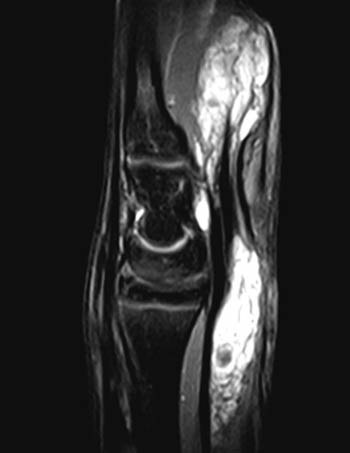
Clinical History: A 28 year-old female presents with calf swelling and pain. Sagittal (1a) T2-weighted and (1b) proton density-weighted images are provided. What are the findings? What is your diagnosis?
Findings
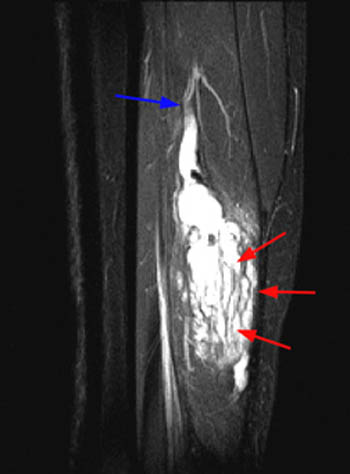
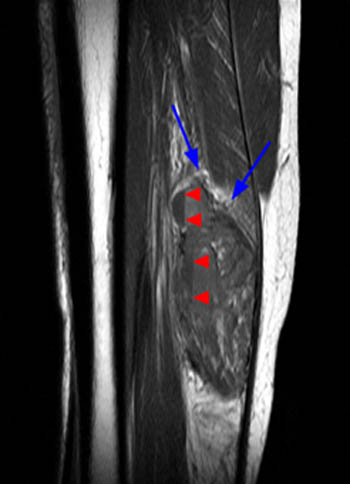
Figure 2:
(2a) The T2-weighted sagittal image shows a lesion of increased signal intensity in the soleus muscle. The lesion is composed of high signal intensity tubules (red arrows). An area of venous communication is seen along the cephalad portion of the lesion (blue arrow). (2b) The proton density-weighted sagittal image demonstrates fluid-fluid levels within the tubules of the lesion (arrowheads). Areas of fatty atrophy are seen along the periphery of the lesion (blue arrows).
Diagnosis
Venous malformation (formerly called hemangioma).
Discussion
Venous malformations, formerly referred to as hemangiomas, are the most common vascular soft tissue abnormality and comprise 7% of benign soft tissue tumors.1 The terminology for vascular anomalies in the medical literature is confusing and inconsistent. To address this confusion in terminology, a classification was developed by the International Society for the Study of Vascular Anomalies (ISSVA) and has subsequently been adopted internationally by the multi-disciplinary teams that treat vascular anomalies.2 The ISSVA classification is based on clinical, radiological, hemodynamic, and histological criteria. The ISSVA classification divides vascular anomalies into two major groups. The first group are vascular tumors that arise because of vascular proliferation, and are called hemangiomas. These hemangiomas are either infantile or congenital. The second group of lesions are called vascular malformations, and arise because of inborn errors in morphogenesis.
Vascular malformations are classified according to the dominant distorted vessel type. The simple types are capillary, lymphatic and venous malformations. Combined types include arteriovenous fistula and arteriovenous malformations, as well as combinations of capillary, lymphatic, arterial and venous components which include capillary venous, capillary lymphatic venous, lymphatic venous, capillary arterial venous and capillary lymphatic arterial venous malformations.3 Vascular malformations are also segmented into low flow and high flow groups, which has is particularly important when assigning the lesions to a treatment algorithm.
Hemangiomas, which occur in infancy, have rapid neonatal growth and slow involution. Vascular malformations are present at birth and grow with the child. According to ISSVA classification, the term hemangioma in adults is inaccurate and should be not be used.4 Although simple light microscopy can be used to differentiate hemangiomas from vascular malformations, special stains have also been used to differentiate the two groups. A recent report has indicated that hemangiomas stained positive for GLUT-1 antigen as opposed to vascular malformations, which did not stain positively.5 Another marker, S-100 immunostain, has been used to detect the nerve bundles that are consistently present in vascular malformations and absent in hemangiomas.6 Venous malformations never spontaneously resolve and the growth rate is variable and can exceed normal body growth. Venous malformations can occur anywhere in the body, and though the majority are solitary, many patients will have multiple lesions. Synovial venous malformations are rare and most involve the suprapatellar pouch of the knee joint, with patients presenting with pain, swelling, and joint effusion.4,C Venous malformations have variable presentation ranging from small, localized, superficial lesions to large, infiltrative lesions with poorly defined margins that cross soft tissue planes.4 Venous malformations can present with exertional and rest pain as well as swelling.7 The pain may is likely related to compression of adjacent structures, episodes of thrombosis and a steal phenomenon with resultant ischemia of adjacent structures.4,8
Imaging Findings
Routine radiography has a limited role in the evaluation of venous malformations and is used primarily to evaluate for osseous abnormalities rather than for diagnosis or staging. Venous malformations are associated with different types of bony abnormalities including bone hypoplasia and demineralization,9 bone overgrowth secondary to hyperemia8 and mixed sclerotic changes with periosteal reactions.4 Phleboliths are seen with some but not all venous malformations.4 CT scanning has a limited role in the evaluation of venous malformations and has been supplanted by MR imaging. Ultrasound can be useful as an adjunctive study to MR imaging in the evaluation of venous malformations. With sonography, venous malformations are compressible and have a heterogeneous echotexture, with the majority being hypoechoic relative to adjacent subcutaneous tissue.10 With Doppler interrogation, the majority of venous malformations will have monophasic flow.10
Conventional arteriography and venography usually have no role in the evaluation of venous malformations. Direct percutaneous phlebography (DPP), however, has an important role in characterizing venous malformations prior to treatment. Based on DPP appearances, venous malformations have been classified by the type of venous drainage. This has important implications regarding treatment and prognosis.11,12
- Type I: Isolated malformations without venous drainage.
- Type II: Drainage into normal veins.
- Type III: Drainage into dysplastic veins.
- Type IV: Lesions consist of venous ectasia.
- Type I and II venous malformations respond best to sclerotherapy, with higher cure rates and lower number of treatment sessions,12 while Types III and IV are associated with more complications related to systemic venous embolization and the sclerosants used in the procedures.11
MR imaging is the mainstay of imaging of venous malformations. MR imaging is the single best modality to detect, characterize and stage venous malformations. Most venous malformations have typical MR appearances, but the appearances can be variable and at times MR imaging alone is not diagnostic. The following is a summary of recognized MR features of venous malformations:
- Appearance on T2-weighted images: high signal-intensity lobules or tubules13 that have also been described as a bunch of grapes.14
- Heterogeneous mass on all sequences, though lesions measuring under 2 cm tend to be homogeneous.8
- Peripheral fat due to muscle atrophy secondary to chronic vascular insufficiency.8,Fig. 4a, Fig. 5a
- Gradient echo sequences reveal areas of low signal intensity corresponding to calcification or hemosiderin.12
- Low signal is observed in the areas containing fibrofatty septa, vascular channels, phleboliths, or thrombosis.12,Fig. 6a, Fig. 7a
- Homogeneously or heterogeneously enhance after gadolinium administration.4
- Fluid-fluid levels within cystic spaces.15
- Lace-like thin septa within or around the malformations.16
- Vascular spaces oriented along the long axis of the extremities follow a neurovascular bundle, and are sometimes multifocal.17,Fig. 8a
A MR grading system for venous malformations has been proposed, with the following criteria18:
- Grade I: Well defined and less than 5 cm.
- Grade II: Poorly defined or greater than 5 cm.
- Grade III: Poorly defined and greater than 5 cm.
The lower grade lesions are more responsive to treatment than the higher grade lesions.
Treatment
Percutaneous management of venous malformations in the form of sclerotherapy has become a common and effective treatment modality, though some lesions are better treated surgically or with combined surgery and sclerotherapy. The type of drainage is one the most important factors in determining the treatment of venous malformations. The decision to treat, surgically or percutaneously, should occur at a center with an experienced multidisciplinary team.4
Conclusion
Venous malformations, formerly called hemangiomas, are the most common vascular soft tissue abnormality. To address the confusion in terminology of vascular lesions, a new classification has been adopted that calls for dropping the use of hemangiomas in adults and substituting the term venous malformation. Venous malformations have characteristic features on MR imaging, and MR is the best imaging modality for the diagnosis and characterization of venous malformations. Findings on MR imaging allow staging of lesions, and prediction of the likely response to therapy.
References
1 Allen PW, Enzinger FM. Hemangioma of skeletal muscle. An analysis of 89 cases. Cancer 1972; 29:8-22.
2 Wassef M, Vanwijck R, Clapuyt P, Boon L, Magalon G. [Vascular tumours and malformations, classification, pathology and imaging]. Ann Chir Plast Esthet 2006; 51:263-281.
3 Enjolras O. Classification and management of the various superficial vascular anomalies: hemangiomas and vascular malformations. J Dermatol 1997; 24:701-710.
4 Legiehn GM, Heran MK. Classification, diagnosis, and interventional radiologic management of vascular malformations. Orthop Clin North Am 2006; 37:435-474, vii-viii.
5 North PE, Waner M, Mizeracki A, Mihm MC, Jr. GLUT1: a newly discovered immunohistochemical marker for juvenile hemangiomas. Hum Pathol 2000; 31:11-22.
6 Adegboyega PA, Qiu S. Hemangioma versus vascular malformation: presence of nerve bundle is a diagnostic clue for vascular malformation. Arch Pathol Lab Med 2005; 129:772-775.
7 Wild AT, Raab P, Krauspe R. Hemangioma of skeletal muscle. Arch Orthop Trauma Surg 2000; 120:139-143.
8 Olsen KI, Stacy GS, Montag A. Soft-tissue cavernous hemangioma. Radiographics 2004; 24:849-854.
9 Boyd JB, Mulliken JB, Kaban LB, Upton J, 3rd, Murray JE. Skeletal changes associated with vascular malformations. Plast Reconstr Surg 1984; 74:789-797.
10 Trop I, Dubois J, Guibaud L, et al. Soft-tissue venous malformations in pediatric and young adult patients: diagnosis with Doppler US. Radiology 1999; 212:841-845.
11 Puig S, Aref H, Chigot V, Bonin B, Brunelle F. Classification of venous malformations in children and implications for sclerotherapy. Pediatr Radiol 2003; 33:99-103.
12 Dubois JM, Sebag GH, De Prost Y, Teillac D, Chretien B, Brunelle FO. Soft-tissue venous malformations in children: percutaneous sclerotherapy with Ethibloc. Radiology 1991; 180:195-198.
13 Suh JS, Hwang G, Hahn SB. Soft tissue hemangiomas: MR manifestations in 23 patients. Skeletal Radiol 1994; 23:621-625.
14 Vilanova JC, Barcelo J, Smirniotopoulos JG, et al. Hemangioma from head to toe: MR imaging with pathologic correlation. Radiographics 2004; 24:367-385.
15 F. R. Tumors and tumorlike lesions of blood vessels. Berlin, Germany: Springer-Verlag, 2001.
16 Jenner G, Soderlund V, Bauer HF, Brosijo O. MR imaging of skeletal muscle hemangiomas. A report of 16 cases. Acta Radiol 1996; 37:140-144.
17 Rak KM, Yakes WF, Ray RL, et al. MR imaging of symptomatic peripheral vascular malformations. AJR Am J Roentgenol 1992; 159:107-112.
18 Goyal M, Causer PA, Armstrong D. Venous vascular malformations in pediatric patients: comparison of results of alcohol sclerotherapy with proposed MR imaging classification. Radiology 2002; 223:639-644.