Clinical History: A 73-year-old female presents with chronic low back pain with recent worsening in severity. Sagittal (1a) T1 and T2-weighted images are provided. What are the findings? Which of the findings is the most likely cause of her worsening pain?
Findings
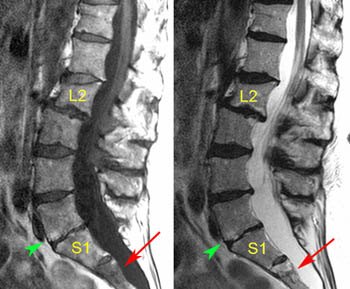
Figure 2:
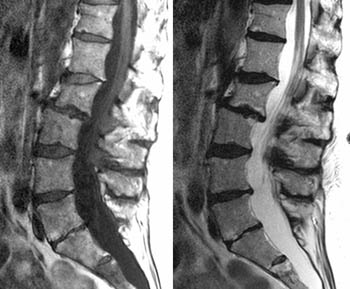
Sagittal (2a) T1- and T2-weighted images of the lumbar spine show the L2 vertebral body to be chronically deformed by a wedge compression fracture. The marrow signal matches that of other vertebrae, demonstrating no edema to suggest that the fracture is recent. No retropulsed bone or significant canal stenosis is present. The L2 vertebral body is mildly displaced posteriorly relative to L3, degenerative in nature. The intervertebral discs are degenerated, particularly at L5-S1, where Type III (fatty, chronic) marrow reactive endplate changes (green arrowhead) are present. At the S2 sacral segment, a horizontal fracture line is identified (red arrow), with surrounding marrow edema. The edema is more conspicuous on the T1-weighted image (abnormally low signal) while the underlying fracture line is better seen on the T2-weighted image.
Diagnosis
1 Sacral insufficiency fracture with a horizontal component through S2.
2 Chronic non-neoplastic wedge compression fracture of L2.
3 Mild L2 retrolisthesis.
4 L5-S1 disc degeneration with disc height loss and type III endplate degenerative changes.
Introduction
Of the multiple abnormalities present, the sacral insufficiency fracture is perhaps the most difficult to identify, but also the most important. Unlike the chronic compression fracture at L2, this fracture has marrow edema, indicating that it is an active process and the most likely cause of this patient’s severe pain.
Finding a specific cause for a patient’s back pain can be elusive, particularly in older patients that have multiple abnormalities on MRI. Degeneration may involve the spine at the discs and the facet joints, scoliosis may be present, various forms and degrees of disc herniation or spinal stenosis may be seen, and compression fractures of various ages may be found. When there are multiple abnormalities on the MRI, or one finding that is conspicuous, a relatively subtle additional finding is more likely to be overlooked. A sacral insufficiency fracture may occur in such a setting, and is an important and not rare finding, particularly in elderly women.
An insufficiency fracture is a subtype of stress fracture that occurs in bones with underlying structural weakness, most commonly due to osteoporosis. Common sites of insufficiency fracture include the sacrum and the pubic bone. Fatigue fracture is the other major subtype of stress fracture, occurring in healthy bone that is subjected to a repetitive load, such that the rate of osseous breakdown exceeds the rate of repair. Typical examples include tibial stress fractures in runners, metatarsal stress fractures in military recruits, and olecranon stress fractures in baseball pitchers. Recent literature describes sacral stress fractures in long distance runners, particularly women.3-5 One of the postulated reasons for the female gender predilection, even in young athletes, is mild underlying osteopenia, such that the distinction between insufficiency and fatigue fracture is sometimes blurred.
Sacral stress fractures typically develop a characteristic H-shaped pattern, with vertical fractures (in the sagittal plane) through both sacral ala, and a horizontal fracture line through the mid sacrum at the S2 or S3 level. This H pattern is well known on nuclear scans as the “Honda sign” for its resemblance to the auto maker’s insignia.
Pubic stress fractures (parasymphyseal or pubic rami) are commonly associated with sacral stress fractures2, and are likely caused by increased stresses in this area following failure of the pelvic ring at the sacrum. While the pain of a sacral fracture may be nonspecific and lead to exams centered on the lumbar spine, the pain produced by pubic fractures may lead to an MRI of the hip or pelvis and concomitant identification of both pubic and sacral insufficiency fractures may thus be possible.
MR Diagnosis
MRI is highly sensitive and specific for the diagnosis of sacral stress fractures. Often it is the edema which is most conspicuous, exhibiting low signal intensity on T1-weighted images. The fracture lines themselves, whether sclerotic or fluid-filled, may be obscured by the background of low signal intensity edema on T1-weighted sequences. Stress fractures, with their usual associated sclerosis, are typically best seen on T2-weighted sequences, appearing as dark lines within a relatively bright signal edema background. Care must be taken to not mistake these lines for the sacroiliac joints, which they parallel in position.
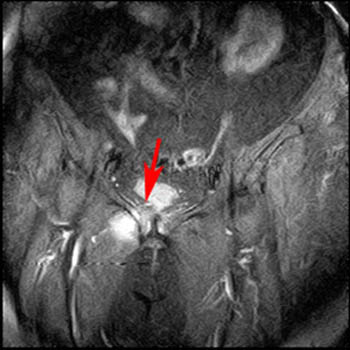
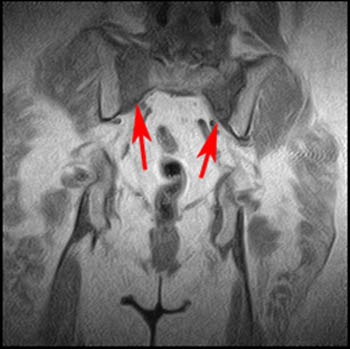
Figure 5:
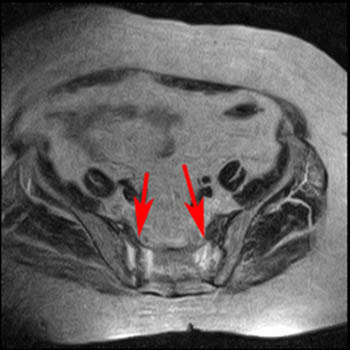
Sacral insufficiency fractures on (5a) T1-weighted coronal and (5b) T2-weighted axial images from a study of the pelvis (Same patient as in Figure 4). The images show vertical fractures and associated edema in both sacral alae. The edema and vertical orientation are best seen on the T1-weighted sequence. The dark fracture lines are best seen on the T2-weighted sequence.
The vertically oriented abnormalities in the sacral alae are conspicuous on MRIs that include the entire sacrum. However, since patients often present with pain that is nonspecific or in the lower back, it is more common to encounter sacral stress fractures on studies of the lumbar spine.
The diagnosis of sacral insufficiency fractures on MRI of the lumbar spine requires a consistent and thorough search pattern with attention to detail. Axial images acquired on a lumbar exam often include only the upper sacrum. A keen MR reader must be alert to the possibility of this diagnosis, particularly in elderly patients or in patients with other evidence of underlying osteoporosis, such as the presence of a compression fracture.
The full H pattern of sacral insufficiency fractures is not always seen. If the horizontal fracture component is not present, identification on lumbar MRI may be more challenging since the vertical component may be the only fracture visible, and only on the most peripheral images. This emphasizes the importance of not only paying attention to midline images on a lumbar spine study, but also carefully inspecting the far lateral sagittal views.
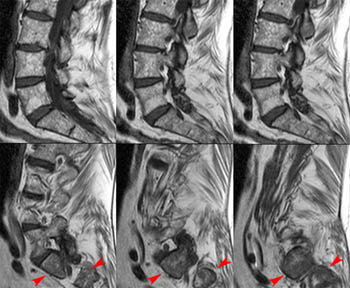
Figure 6:
(6a) Vertical sacral fracture on sagittal images, without a horizontal fracture component. This series of sequential sagittal T1-weighted images through the lumbar spine shows a relatively normal appearance near midline (with patchy low signal red marrow elements). On the more laterally positioned images, low T1 signal is apparent in the sacrum, representing marrow edema (arrowheads). This can be distinguished from the low signal of the sacroiliac joint by noting the low signal on several sequential images and by correlating wtih axial images, if they extend low enough to include this area. Typically at least one axial image will include the upper margin of the sacrum and demonstrate the edema as being distinct from the sacroiliac joint or from other pathology.
Differential Diagnosis
Other causes of signal abnormalities on MRI of the sacrum include neoplasm and sacroiliitis. Sagittal images are more likely to present a diagnostic challenge, since the orientation of slices along the vertical stress fracture line may mask the fracture. One should not mistake the edema from fracture for one of these other diagnoses. Correlation with axial images usually allows identification of fracture lines. In cases where the fracture line is not discretely visible, the edema pattern is still characteristic to the point that a confident diagnosis can be made. Sacral insufficiency fractures are usually bilateral and relatively symmetric at presentation, but can be unilateral or asymmetric. Neoplasm is typically asymmetric, better defined, and geographic in shape, compared with the diffuse pattern of edema associated with fractures.
In cases of sacroiliitis, edema is most prominent immediately adjacent to the sacroiliac joints, which will also typically exhibit a distinctly abnormal joint space. The edema of insufficiency fractures is generally farther removed, at the mid sacral ala or along the sacral foramina.
Although MRI is diagnostic in the presence of a sacral stress fracture, if any doubt remains, thin-section CT or radionuclide bone scan can be used for confirmation. If a CT is performed, coronal and/or sagittal CT reconstructions may be helpful for the detection of a horizontal fracture component.
Clinical Presentation
Sacral stress fractures are most commonly seen in elderly postmenopausal women with osteoporosis. They can also be found in patients that have undergone pelvic radiation therapy. As mentioned above, sacral stress fractures may also present in younger patients, particularly female long-distance runners. These fractures are likely underdiagnosed as a cause of back pain in long-distance running athletes.3
Symptoms are often nonspecific, with low back, buttock, or hip pain, exacerbated with weight bearing, occasionally rendering the patient unable to walk. The pain may be of gradual onset or may develop acutely following minor trauma.
The consequences of sacral stress fractures include chronic pain and disability, as well as development of additional fractures of the pelvic ring, particularly pubic. Neurologic complications of sacral stress fractures are very rare7, in contrast to sacral fractures of acute traumatic origin.
Treatment
Treatment of sacral stress fractures usually consists of conservative measures, including pain control, limited weight-bearing, and gradual physical rehabilitation. Healing is typically achieved within four months. A new more aggressive approach that offers a significant reduction in recovery time is the percutaneous sacroplasty, although the merits and consequences of this procedure remain under evaluation.8
Conclusion
Chronic back pain poses a significant diagnostic and therapeutic challenge, particularly in elderly patients with multiple spinal abnormalities. MRI is an effective tool for the identification of most of the underlying causes. Of these causes, sacral insufficiency fractures are an occasionally subtle but important diagnosis, and one that can be reliably made on lumbar examinations by the careful MRI reader.
References and Additional Reading
1 Stroebel RJ, Ginzburg WW, McLeod RA. Sacral insufficiency fractures: an often unsuspected cause of low back pain. J Rheumatol 1991;18: 117-119.
2 De Smet AA, Neff JR. Pubic and sacral insufficiency fractures: clinical course and radiologic findings. AJR1985; 145:601 -606.
3 Major NM, Helms CA. Sacral stress fractures in long-distance runners. AJR Am J Roentgenol. 2000;174:727-729.
4 Johnson AW, Weiss CB Jr, Stento K, Wheeler DL. Stress fractures of the sacrum. An atypical cause of low back pain in the female athlete. Am J Sports Med. 2001;29:498-508.
5 Fredericson M, Salamancha L, Beaulieu C. Sacral stress fractures: tracking down nonspecific pain in distance runners. Physician Sportsmed. 2003;31:31-42.
6 Diel J, Ortiz O, Losada RA, Price DB, Hayt MW, Katz DS. The sacrum: pathologic spectrum, multimodality imaging, and subspecialty approach. RadioGraphics 2001;21:83-104.
7 Jacquot JM, Finiels H, Fardjad S, Belhassen S, Leroux JL, Plessier J. Neurological complications in insufficiency fractures of the sacrum. Three case reports. Rev Rhum (Engl Ed) 1999;66:109-14.
8 Whitlow CT, Mussat-Whitlow BJ, Mattern CWT, Baker MD, and Morris PP. Sacroplasty versus Vertebroplasty: Comparable Clinical Outcomes for the Treatment of Fracture-Related Pain. AJNR Am. J. Neuroradiol., August 1, 2007; 28(7): 1266 – 1270.