Clinical History: Images from four different upper extremity sports injuries are presented. Match each patient with the associated sport.
A) Boxing
B) Gymnastics
C) Golf
D) Bowling
Case 1:
Case 2:
Case 3:
Case 4:
Findings
Case 1:
Figure 5:
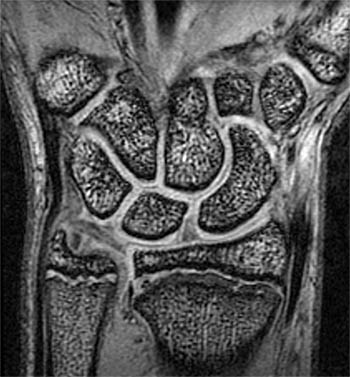
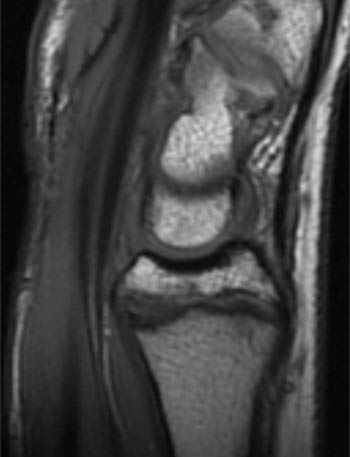
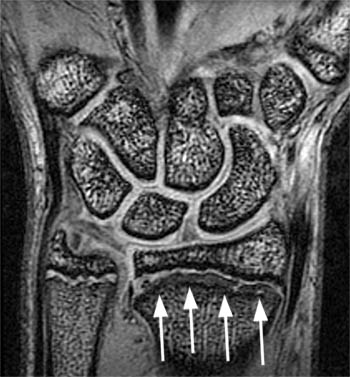
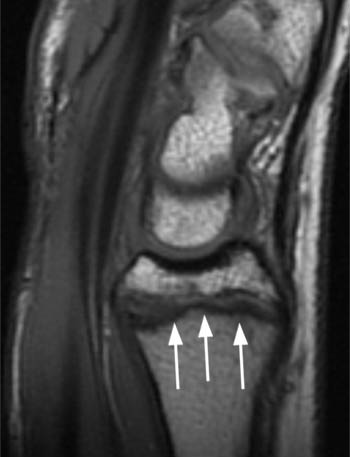
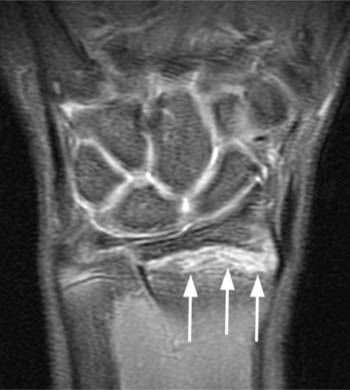
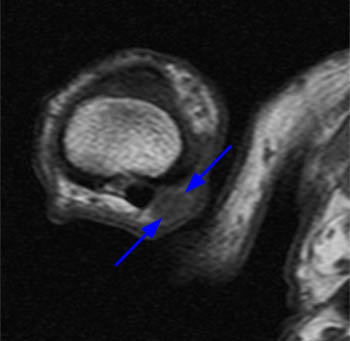
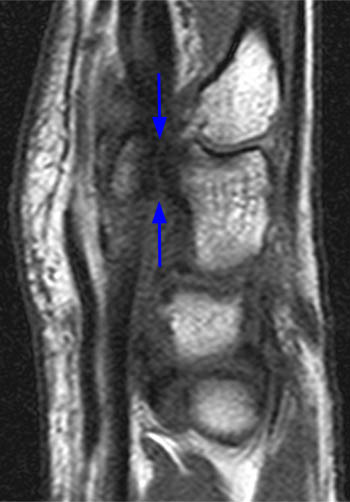
(5a) The coronal gradient echo image demonstrates a widened distal radial physis with mild irregularity of the distal radial metaphysis (white arrows). (5b) The sagittal T1 weighted image demonstrates that the distal radial physeal irregularity is somewhat more prominent at the volar aspect of the radius. The physis is mildly widened throughout (arrows).
Case 2:
Figure 6:
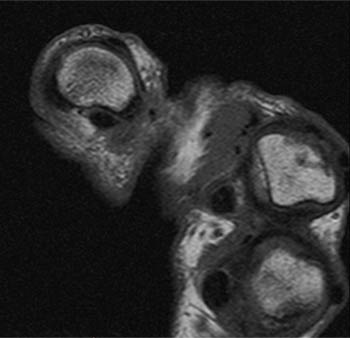
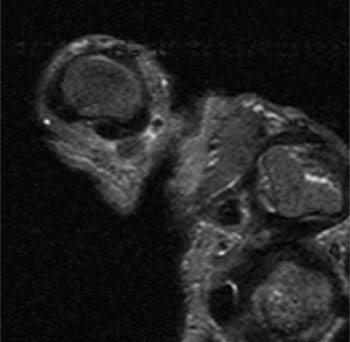
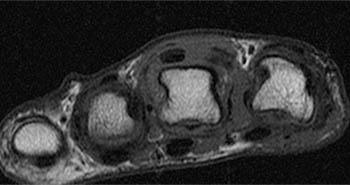
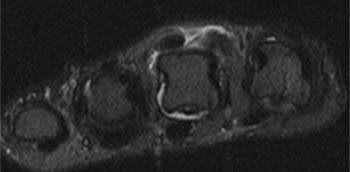
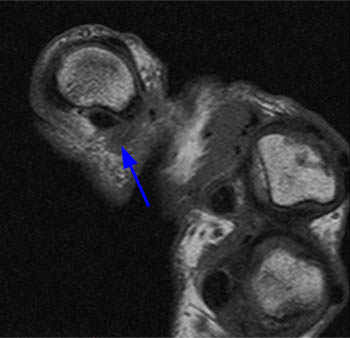
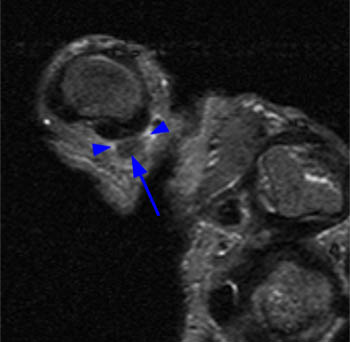
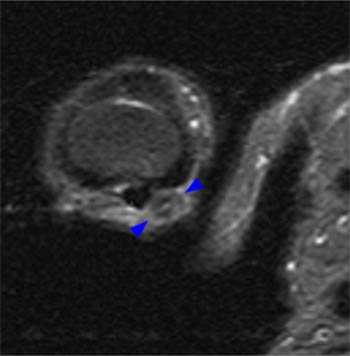
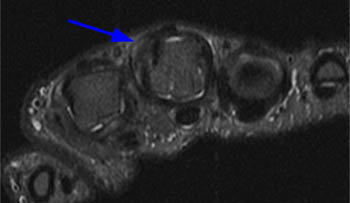
(6a) An axial T1 weighted image of the thumb obtained at the level of the proximal phalangeal base demonstrates diffuse thickening of the ulnar digital nerve ( arrow) with irregular margins reflecting adjacent soft tissue edema. (6b) An axial inversion recovery image at the same level as 6a. The enlarged ulnar digital nerve ( arrow) is surrounded by a thin margin of high signal edema (arrowheads).
Case 3:
Figure 7:
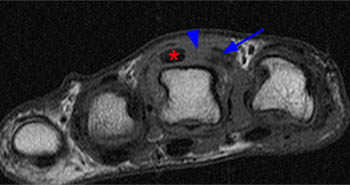
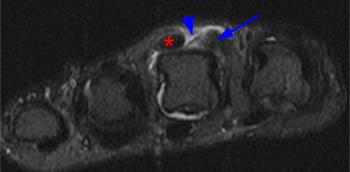
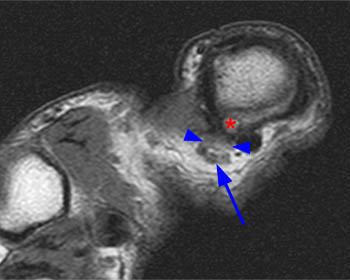
(7a) An axial T1 weighted image at the level of the metacarpal heads. The extensor tendon (asterisk) is ulnarly subluxed. The radial sagittal band (arrow) is thickened and is displaced radially. A defect (arrowhead) lies at the site of disruption of the sagittal band. (7b) An axial inversion recovery image obtained at the same level as figure 7a. Ulnar subluxation of the extensor tendon (asterisk) is seen with a large defect in the extensor mechanism dorsally (arrowhead). The thickened and radially displaced sagittal band (arrow) is surrounded by mild edema.
Case 4:
Figure 8:
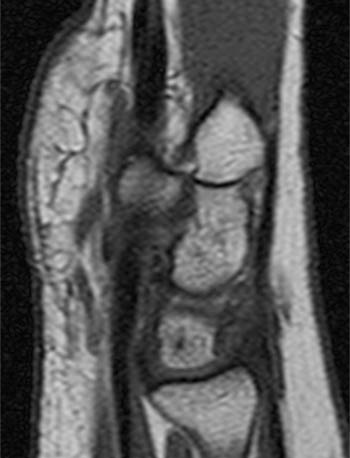
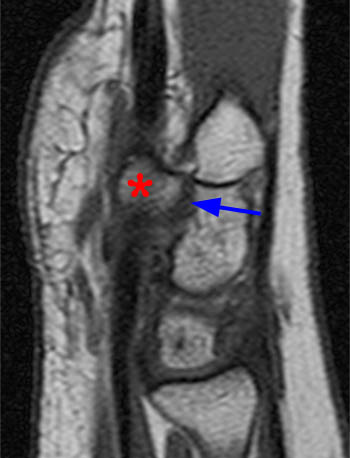
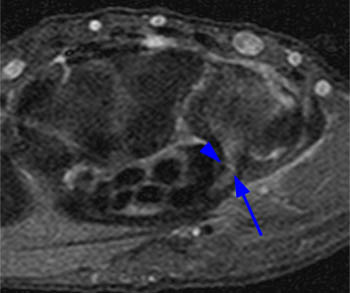
(8a) Axial T1 weighted image of the wrist. A transverse fracture (arrow) extends across the base of the hamulus. (8b) Sagittal T1 weighted image through the hamate bone. The hamulus is indicated by the asterisk. A coronal plane fracture (arrow) at the base of the hamulus is mildly displaced.
Diagnoses
A) Boxing – Case 3
B) Gymnastics – Case 1
C) Golf – Case 4
D) Bowling – Case 2
Discussion
Case 1 – Gymnast’s Wrist
Along with acute physeal injuries in children, the physician caring for young athletes must be aware of chronic stress injuries that can cause physeal damage. As children participate in rigorous training programs at younger ages, the incidence of these injuries is likely to increase. Repetitive stress, including a sudden increase in training, can lead to physeal injury with no history of direct trauma.
Because the ligamentous structures and joint capsule of the adolescent wrist are two to five times stronger than the open growth plate, the open growth plate is the site most susceptible to injury in young athletes1. Compressive loading and shearing forces are thought to cause Salter-Harris type I microfractures within the growth plate at the level of the zone of hypertrophying cells, which lies just above the zone of provisional calcification2. This layer is the weakest within the growth plate, because it has the least amount of collagen matrix and no reinforcing calcification3.
The repetitive forces also may cause temporary ischemia in the zone of provisional calcification, which receives its vascular supply from end capillary loops that arise in the marrow of the shaft and enter through the metaphysis2,3. This ischemia inhibits normal calcification of the growth plate, resulting in the radiographic findings of physeal widening and metaphyseal irregularity.
One of the more common physeal stress injuries occurs in the distal radial physis in gymnasts. Roy and colleagues1 reported on 21 elite gymnasts with wrist pain. Radiographs showed widening of the physis, cystic changes involving the metaphyseal side of the growth plate, and a beaked effect at the distal aspect of the epiphysis. They felt these findings represented stress changes and possible stress fracture of the distal radial physis. Carter and Aldridge2 reported similar findings in 21 gymnasts and also noted that the skeletal age of their patients was delayed, increasing the length of time the physis was at risk.
Liebling and colleagues4 reported on the MR imaging appearance of a patient with gymnast’s wrist. They described physeal widening with a thin, irregular line of high signal located just proximal to the normal high signal region of the physis (9a). This linear region of increased signal was thought to represent persistent chondrocytes and cartilaginous matrix in the primary spongiosa of the metaphysis4. This appearance is analogous to that seen in other physeal stress injuries such as Little League shoulder (10a).
Young athletes involved in strenuous training programs who develop pain at the end of a long bone should undergo radiographic evaluation of the adjacent physes. Any evidence of widening or other abnormality should lead the physician to recommend avoidance of the offending activity for up to 3 months. With cessation of the causative stress, the pain will subside and the abnormalities seen on radiographs will resolve without apparent impairment of normal growth1,2,4. Roy et al.1 found that the time required for clinical resolution was proportional to the extent of the changes seen on the radiographs obtained at the time gymnast’s wrist was detected. Therefore, the more subtle the changes recognized at the time of diagnosis, the better the prognosis for rapid recovery.
Figure 9:
A 12 year-old male gymnast with dorsal wrist pain. This coronal fat suppressed proton-density weighted image demonstrates widening and irregularity of the distal radial physis with a proximal line of increased signal intensity (arrows). This is thought to represent persistent chondrocytes and cartilaginous matrix within the distal metaphysis.
Figure 10:
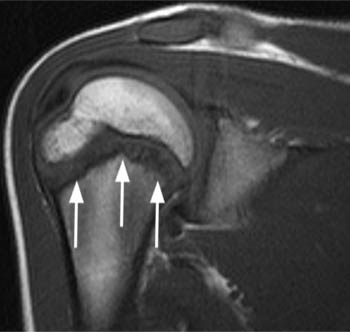
Little League Shoulder. Coronal T1 weighted image through the proximal humerus of a 12 year old baseball player who had pain with throwing. The proximal humeral physis is widened and irregular (arrows). This is another example of a chronic overuse injury to the growing skeleton and is analogous to the injury seen within the distal radius of gymnasts.
Case 2 – Bowler’s Thumb
Over 95 million people enjoy bowling worldwide with nearly 3 million certified league bowlers in the United States. While the incidence of Bowler’s thumb is unknown, the symptoms can be severe enough to prevent further sport participation5. Bowlers thumb affects bowlers who impart spin on the ball by keeping their thumb in the thumb-hole until the moment of release. The clinical presentation involves paresthesias, hyperesthesias, possible changes in sensation, and a thickened digital nerve on palpation.
This condition occurs almost exclusively in bowlers and represents a proliferation of perineural fibrous elements which surround and separate the nerve fascicles, which are eventually strangulated by the fibrous tissue and undergo atrophy6. This fibrous proliferation also extends into the adjacent fascial and subcutaneous structures. The cause of this entity appears to be repeated friction between the thumb and the edge of the thumb hole in the bowling ball. The digital nerve on the ulnar side of the thumb is particularly vulnerable during bowling because it lies superficial to the sesamoid bone within a thin layer of subcutaneous tissue. Although normally the nerve is mobile, it is easily trapped, since it is partly tethered by its branches to local skin areas. As scarring in the area increases, the nerve becomes more fixed and less likely to be displaced sufficiently to escape irritating pressures.
Two different appearances have been described on MR imaging evaluation7. In some cases, the ulnar digital nerve appears enlarged and somewhat nodular (11a,12a). The nerve may be of increased signal intensity on T2 weighted images and is often surrounded by edema-like signal. The abnormal nerve has been reported to enhance following administration of Gadolinium based contrast material7. In other instances, the soft tissues surrounding the nerve are more severely affected, with prominent perineural fibrosis and edema demonstrated (13a). In either case, the underlying pathology is the same – extensive proliferation of fibrous tissue which surrounds, separates, and engulfs nerve fascicles6.
Early recognition and treatment of this condition is important, because permanent disability may result if the lesion is allowed to persist. Non-operative treatment may include technical solutions such as changing the size and weight of the ball, the spacing between holes, the fitting of thumb to ball, and the slope and size of thumb holes. Protective guards may be tried, but athlete compliance is poor due to the bulk of the devices typically used.
It is not yet clear how many patients require surgery, but the percentage is likely to be low. The outcome from surgery may be good when the digital nerve is severely compressed by a perineural mass. However, surgery is unlikely to completely restore the thumb to normal. Surgery consisting of neurolysis of the extraneural and epineural scar from the involved nerve may be beneficial if the symptoms are severe5,6. Swanson et al recently reported an operative technique involving transposition of the nerve beneath the adductor pollicis muscle, which must be incised and repaired5. The surgical outcome for active bowlers remains unclear and postoperative protection from the repetitive trauma of throwing is therefore important.
It is important that both bowlers and clinicians are sufficiently aware of bowler’s thumb to allow early diagnosis and treatment of this lesion.
Figure 13:
An axial T1 weighted image obtained through the thumb of a 36yo bowler who complained of pain at the interphalangeal joint. The ulnar digital nerve (arrow) is mildly enlarged with prominent subcutaneous edema and fibrosis located deep to the nerve (arrowheads). The ulnar sesamoid bone is indicated by the asterisk. The location of the sesamoid bone deep to the nerve has been postulated as a contributing factor to the development of the fibrosis.
Case 3 – Boxer’s Knuckle
The unique function of the boxer’s hand requires persistent, forceful punching in a constantly clenched fist posture, therefore, the metacarpophalangeal joints are continually exposed to blunt trauma and are highly vulnerable to injury. The term boxer’s fracture is a well-known eponym describing a typically transverse, minimally comminuted fracture of the small finger metacarpal with angulation of the distal fragment. Boxer’s knuckle is a less-well-known eponym used in the sports medicine literature to describe one of the most severe and frequent types of this injury: damage to the sagittal bands of the extensor mechanism8,9. The sagittal bands are transversely oriented ligaments that help stabilize the extensor tendon during joint motion10(14a).
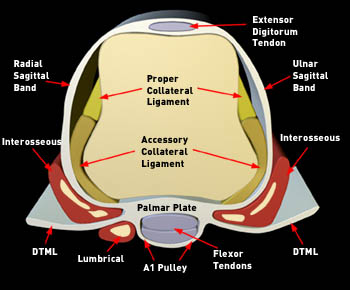
Figure 14:
Diagrammatic representation of an axial view through the metacarpal head of the middle finger depicts the surrounding supporting structures. The sagittal bands extend from the extensor digitorum tendon to the palmar plate. Additional structures depicted include the proper and accessory collateral ligaments, flexor digitorum profundus and superficialis tendons (Flexor Tendons), A1 pulley, interosseous muscles and tendons (Interosseous), lumbrical muscle and tendon (Lumbrical), and the deep transverse metacarpal ligaments (DTML).
Complete metacarpophalangeal joint extensor mechanism disruption is usually caused by blunt trauma10, and typical symptoms are pain, metacarpophalangeal joint swelling, loss of full joint extension, central tendon dislocation or subluxation, and a palpable defect at the site of the disruption11. Although any of the fingers can be affected, the most commonly injured finger is the long finger8. Its anatomic predisposition and prominence when a fist is made make it particularly susceptible to injury. Additionally, the metacarpophalangeal joints are forced into acute flexion during a punch, and the overlying extensor mechanism and joint capsule are maximally stretched over the prominent metacarpal head. Depending on the degree of initial trauma and its repetitiveness, a spectrum of injuries to the extensor mechanism may be encountered. These include tears in the sagittal bands, either on the ulnar or radial side of the central tendon, and tears longitudinally in the central tendon. If an excessive force causes extreme flexion and ulnar deviation of the joint, a complete tear of the radial sagittal band with ulnar dislocation of the central tendon can be expected8,11. This may or may not be associated with an underlying capsular tear.
The clinical manifestation and findings at physical examination are usually sufficient to establish a diagnosis of traumatic subluxation of the extensor tendon due to injury of the sagittal band. Difficulties in diagnosis may arise, however, when the tendon position cannot be confidently palpated because of overlying soft-tissue swelling or when the clinical manifestation is atypical. In such cases, MR imaging can play an important diagnostic role (15a,16a). Recently, the use of dynamic ultrasound has also been shown to be of diagnostic utility9.
Controversy surrounds the question of what method is best for treatment of extensor mechanism disruption at the MP joint. Several authors have advocated that nonoperative treatment should be attempted before operative intervention, particularly in cases of acute extensor mechanism injury12. However, there is very little evidence of successful nonoperative treatment in the literature. Direct surgical repair with realignment of the central tendon is usually adequate and highly successful. Augmentation with local tendon slips is rarely indicated. However, if there is extensive tissue loss, it can be a viable alternative8, 11.
The goal of the athlete, trainer, and team physician is to prevent hand injuries during practice and competition. To do so, safety measures, including proper training, adequate wrapping and gloving of the hand, custom protective devices, and adequate medical supervision, must be employed. If an injury is sustained, prompt recognition and treatment will relieve symptoms and allow a return to athletic activity.
Figure 15:
An axial T1 weighted image at the level of the MCP joints in a 45 year old male who complained of pain and swelling at the long MCP joint after using a punching bag. In this case, the radial sagittal band is thickened and edematous, however it is not disrupted (arrow). The central extensor tendon (asterisk) is not subluxed or dislocated.
Case 4 – Golfer’s Wrist
Golf has historically been viewed as a refined sport with a low injury rate. Despite the perceived safety of golf, golfers do injure their wrists. A study of 703 amateur and professional golfers showed a 14% incidence of wrist and hand injuries13. One such injury involves a fracture of the hamulus, or hook, of the hamate bone.
Numerous reports have linked fractures of the hamulus to participation in sports that require gripping a racquet, bat, or club14,15. Stark et al.16 have shown that when a baseball bat, golf club, or racquet is grasped, the end of the handle is located over the distal and ulnar surfaces of the hook. If there is a slight relaxation of grasp at the conclusion of a swing or at the time of meeting a sudden resistance, the centrifugal force of the swing results in direct trauma upon the hook. Fractures may also occur when a golf club strikes the ground, or with repeated shots from deep rough. Hamulus fractures have also been reported to follow forceful muscular contractions without direct trauma14.
Hamulus fractures should be suspected in athletes participating in racquet sports, golf, or baseball who are seen with ulnar sided wrist pain. Physical examination reveals tenderness over the hook of the hamate, which lies on a line between the pisiform and index metacarpal head. However, the hook of the hamate can be difficult to palpate due to the overlying hypothenar musculature. Plain radiographs often do not reveal the fracture; carpal tunnel and supinated oblique views can be obtained, however patient discomfort often precludes optimal positioning. In such cases, the diagnosis can be confirmed with CT or MR imaging17 (17a,18a).
Treatment of hook of the hamate fractures in athletes varies from casting to open reduction and internal fixation to excision. Nonoperative treatment consists of immobilizing the hand and wrist in a short arm cast for 6 to 8 weeks14. However, this form of treatment carries a high non-union rate because of the distracting forces exerted on the hamulus by the hypothenar musculature and the pisohamate ligament. In the case of a painful nonunion of the fracture, operative intervention is often necessary to alleviate the disabling symptoms14,15. This has led many authors to consider early surgical intervention with excision of the hamulus to be the prudent approach to this problem14,15,16. Every report of excision of the hook, early or late, reveals that all patients have had good to excellent results, with no further pain, full wrist motion, normal grip strength, and a return to the previous level of activity within 6 to 8 weeks after surgery14. A fast recovery is often of importance since these fractures frequently occur in high performance or professional athletes. Early excision also eliminates potential ulnar or median nerve palsy, ulnar artery compromise, tendinitis, or rupture of the small, ring, or long finger flexor tendons.
Fractures of the hook of the hamate are difficult to diagnose clinically and may result in chronic pain, disability, and significant delayed complications. These fractures may occur without blunt trauma in professional or amateur athletes participating in sports which involve swinging of grasped objects. Considering the rapid increase in the popularity of recreational sports, fractures of the hamulus may become a more frequent cause of chronic wrist pain and disability. A high index of clinical suspicion and proper radiographic evaluation will allow early diagnosis and treatment of these fractures, thus preventing significant late complications.
Figure 17:
A sagittal T1 weighted image through the hamate bone in a 34yo male. He heard a 'pop' while golfing and complained of persistent ulnar sided wrist pain. A region of low signal intensity (arrows) extends through the mid portion of the hamulus with cortical disruption and no significant fracture displacement.
Conclusion
MR’s high resolution and soft tissue contrast make it ideally suited for the evaluation of the musculoskeletal system, and athletic injuries are no exception. Although the pattern of injury associated with a particular sport can be characteristic, physical examination and routine radiographs are often equivocal in the evaluation of the injured athlete. In many such cases, the astute interpreter of MR is able to recognize and properly characterize the findings that account for the patient’s symptoms, providing valuable guidance that allows proper treatment to be provided.
References
1 Roy S, Caine D, Singer KM. Stress changes of the distal radial epiphysis in young gymnasts: A report of twenty-one cases and a review of the literature. Am J Sports Med 1985;13:301-308.
2 Carter SR, Aldridge MJ, Fitzgerald R, Davies AM. Stress changes of the wrist in adolescent gymnasts. Br J Radiol 1988:61:109-112.
3 Salter RB, Harris WR. Injuries involving the epiphyseal plate. J Bone Joint Surg[Am] 1963;45-A:587-622.
4 Lieblinig MS, Berdon WE, Ruzal-Shapiro C, Levin TL, Roye D Jr, Wilkinson R. Gymnast’s Wrist (Pseudorickets Growth Plate Abnormality) in Adolescent Athletes: findings on Plain Films and MR Imaging. AJR 1995; 164:157-159.
5 Swanson S, Macias LH, Smith AA. Treatment of Bowler’s Neuroma with Digital Nerve Translocation. Hand 2009;4:323-326.
6 Dobbs JH, O’Brien ET, Linsheid RL, Farrow GM. Bowler’s Thumb: Diagnosis and Treatment: A Review of Seventeen Cases. J Bone Joint Surg Am. 1972;54:751-755.
7 Muramatsu K, Yoshida K, Taguchi T. Two Different Types of Bowler’s Thumb. orthopaedics 2009; 32:525.
8 Hame SL, Melone CP. Boxer’s Knuckle in the Professional Athlete. Am J Sports Med 2000; 28:879-882.
9 Lopez-Ben R, Lee DH, Nicolodi DJ. Boxer Knuckle (Injury of the Extensor Hood with Extensor Tendon Subluxation): Diagnosis with Dynamic US-Report of Three Cases. Radiology 2003;228:642-646.
10 Clavero JA, Golano P, Farinas O, Alomar X, Monill JM, Esplugas M. Extensor Mechanism of the Fingers: MR Imaging-Anatomic Correlation. RadioGraphics 2003; 23:593-611.
11 Posner MA, Ambrose L. Boxer’s Knuckle-Dorsal Capsular Rupture of the Metacarpophalangeal Joint of a Finger. J Hand Surg 1989;14A: 229-236.
12 Ritts GD, Wood MB, Engber WD. Nonoperative treatment of traumatic dislocations of the extensor digitorum tendons in patients without rheumatoid disorders. J Hand Surg 1985; 10A: 714-716.
13 Gosheger G, Liem D, Ludwig K, Greshake O, Winkelmann W. Injuries and Overuse Syndromes in Golf. Am J Sports Med 2003; 31: 438-443.
14 Parker RD, Berkowitz MS, Brahms MA, Bohl WR. Hook of the hamate fractures in athletes. Am J Sports Med 1986; 14: 517-523.
15 David TS, Zemel NP, Matthews PV. Symptomatic, Partial Union of the Hook of the Hamate Fractures in Athletes. Am J Sports Med 2003; 31:106-111.
16 Stark HH, Jobe FW, Boyes JH, Ashworth CA. Fracture of the hook of the hamate in athletes. J Bone Joint Surg [Am]1977; 59:575-582.
17 Murray WT, Meuller PR, Rosenthal DI, Jauernek RR. Fracture of the Hook of the Hamate. AJR 1979; 133:899-903.