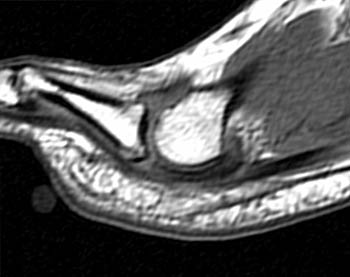
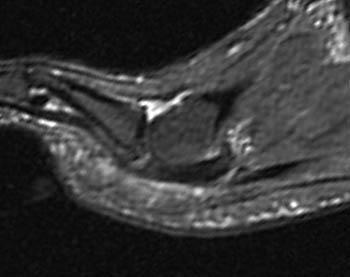
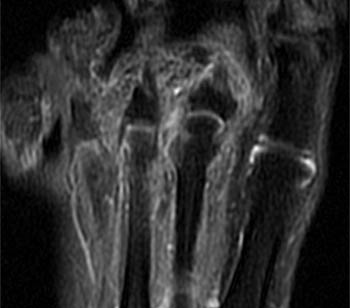
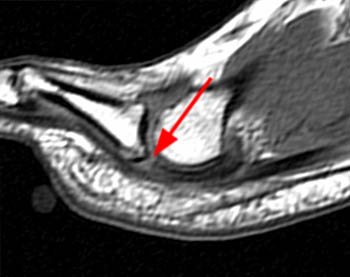
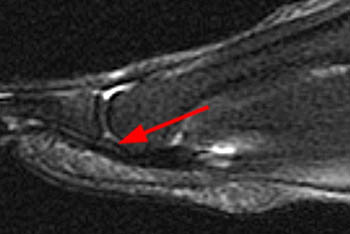
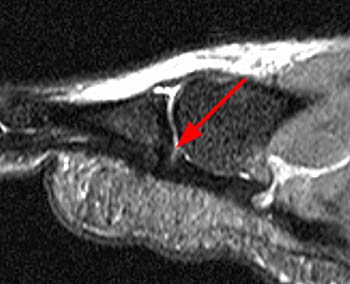
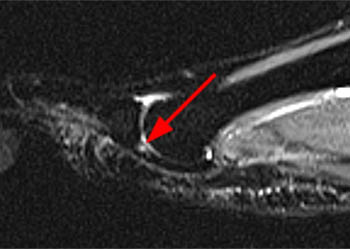
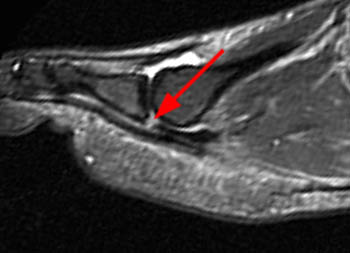
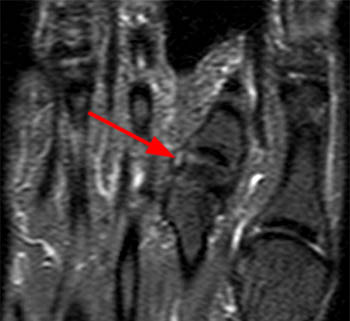
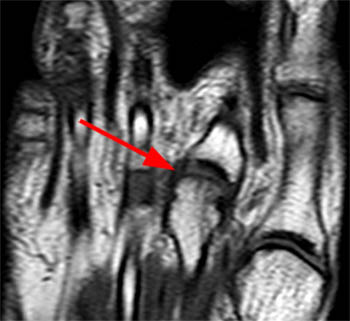
Clinical History: A 56 year-old female presents with gradual onset of right forefoot pain over 4 months. Physical examination reveals point tenderness over the plantar second metatarsophalangeal joint. MRI of the right forefoot was obtained with (1a) sagittal T1-weighted and (1b) fat-suppressed T2-weighted images, (1c) axial fat-suppressed proton density-weighted images, and (1d) coronal fat-suppressed T2-weighted images. What are the findings? What is your diagnosis?
Findings
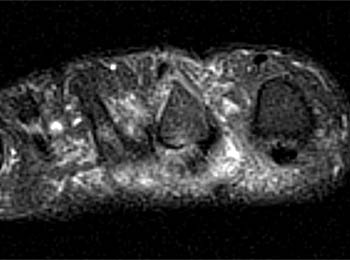
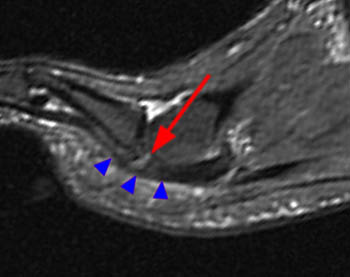
Figure 5:
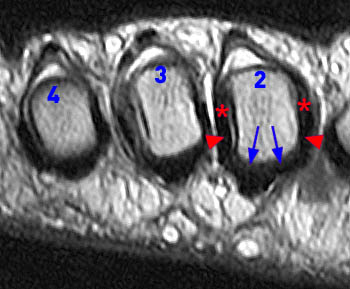
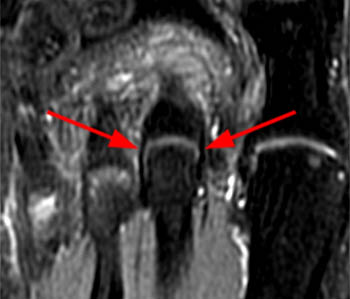
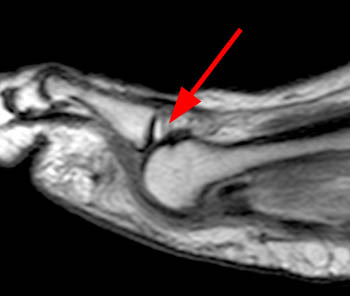
The coronal fat-suppressed T2-weighted image reveals abnormal hyperintense signal in the usual location of the plantar plate (arrow), extending laterally into the lateral accessory collateral ligament (red arrowheads). Note intact medial accessory and proper collateral ligaments (blue arrowhead).
Diagnosis
Instability of the second metatarsophalangeal joint with tears of the plantar plate, lateral accessory collateral ligament and lateral proper collateral ligament.
Introduction
Lesser metatarsophalangeal joint instability is thought to be due to repetitive stress causing irritation and synovitis in the MTP joint, with subsequent degeneration and tearing of the plantar plate. The disease process may progress to tears of the collateral ligament complex, with associated joint deformity.1
Women over the age of 50 are the most frequently affected demographic group, with female patients comprising 86% in one recent series.15 Predisposing anatomic factors include a congenitally long metatarsal (usually of the second ray), hallux valgus, and joint hypermobility. Wearing shoes with high heels and/or a restrictive, narrow toe-box is also associated.2 Athletes may suffer direct injury to the joint and present with acute onset of symptoms.3
The second MTP joint is most frequently involved, possibly due to the length of the second metatarsal, which is usually the longest metatarsal.4 Physiologic stress on the MTP joints also tends to decrease from medial to lateral, making third to fifth MTP joint instability significantly less common.5
Anatomy
Alignment of the second through fifth metatarsophalangeal joints is maintained by both static and dynamic stabilizers. Static stabilizing structures include the plantar plate, the collateral ligament complexes, and the joint capsule. Dynamic stabilizers include the flexor and extensor muscles and tendons, and generally require an intact plantar plate to function.6 Imaging of the lesser MTP joints is focused on assessing the integrity of the static stabilizing structures, because of their functional importance (6a).
The most important static stabilizer is the plantar plate, a fibrocartilaginous bandlike structure extending from the plantar surface of the distal metatarsal to the plantar base of the proximal phalanx (6a,7a,8a). The plantar plate measures approximately 20 mm in length, 8 to 13 mm in width and 2 to 5 mm in thickness. The distal longitudinal bands of the plantar aponeurosis insert on the plantar plate. The deep transverse intermetatarsal ligament blends into the deep fibers of the plantar plate along its medial and lateral margins.7
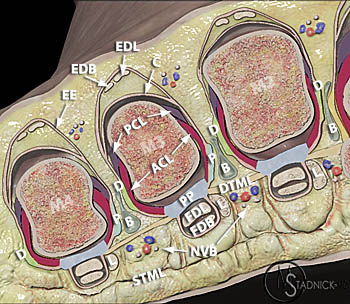
Figure 6:
3D representation of the anatomic structures at the 2nd - 4th metatarsophalangeal joints depict the static stabilizing structures which include the plantar plate (PP), proper collateral ligament (PCL), accessory collateral ligament (ACL), fibrous capsule (C), and deep transverse metatarsal ligament (DTML). Additional structures depicted include the intermetatarsal bursae (B), dorsal interosseous tendon (D), extensor digitorum brevis (EDB), extensor digitorum longus (EDL), extensor expansion (EE), Flexor digitorum brevis (FDB), flexor digitorum longus (FDL), neurovascular bundle (NVB), lumbrical tendon (L), plantar interosseous tendon (P), superficial transverse metatarsal ligament (STML).
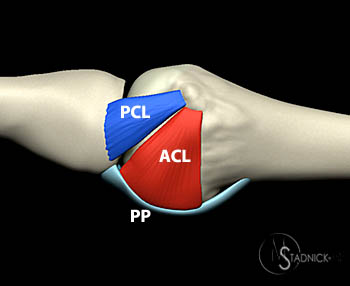
On either side of the plantar plate are the medial and lateral collateral ligament complexes (6a,7a,9a,10a). Each collateral ligament complex can be separated anatomically into two main components, both originating from the dorsal tubercle of the metatarsal head. The dorsal component inserts on the base of the proximal phalanx, and is commonly called the proper collateral ligament, frequently abbreviated as the PCL. (Synonyms include main collateral ligament [MCL], phalangeal collateral ligament, metatarsophalangeal collateral ligament, or collateral ligament.) The plantar component is a thin, broader structure which courses obliquely to insert on the peripheral margin of the plantar plate. This is commonly termed the accessory collateral ligament, frequently abbreviated as the ACL. (Synonyms include suspensory ligament or metatarsoglenoid ligament.)8,9
Although the ACL can be dissected from the PCL in 68% of anatomic specimens9, it is generally not possible to delineate the ACL from the PCL on MR images as they are both hypointense structures which are contiguous and blend together. Some authors therefore prefer not to label them separately, but describe both structures together as the collateral ligament complex (CLC).10
When reporting tears of the collateral ligaments on MRI, it is often possible to infer which ligament is torn based on location.11 A ligamentous tear adjacent to the plantar plate can be described as an ACL tear, and disruption of the far lateral and more dorsal ligament fibers indicates PCL tear. However, it may be difficult to determine whether a tear is confined to a single component or involves both the ACL and the PCL, since their margins are not distinct.
On MRI, the plantar plate is best seen in the sagittal plane as a hypointense band-like structure. The proper collateral ligaments are visualized in the axial plane on either side of the joint. The accessory collateral ligaments are often best visualized in cross section on the coronal sequences as curvilinear hypointense structures at the medial and lateral aspects of the plantar plate, blending into the plantar plate centrally and the PCL laterally.
On coronal images, the intact plantar plate, medial and lateral CLCs form a continuous U-shaped hypointense band across the plantar aspect of the MTP joint. The plantar plate may occasionally be seen as a biconvex area of thickening in coronal section.10
Imaging
Radiographs may demonstrate osteoarthritis of the MTP joint or toe malalignment, but are relatively insensitive.12 Ultrasound visualizes the normal plantar plate as a homogeneous hyperechoic band arching over the metatarsal head, which becomes discontinuous or heterogeneously hypoechoic when torn.13
MRI is often helpful in diagnosis. The intact plantar plate is hypointense on all pulse sequences, and uniform in morphology. The plantar plate recess (11a) of the MTP joint is a normal variant which may slightly undercut the phalangeal insertion of the plantar plate, and can be accentuated by fluid in the joint. This recess was present in up to 47% of cadaveric specimens in one series, although only 6% displayed a large recess.10 Articular cartilage may normally undercut the phalangeal insertion of the plantar plate, resulting in mild uniform hyperintense signal at the distal insertion.13 This should be contiguous with the hyaline articular cartilage layer of the phalanx, and usually does not produce diagnostic difficulty. Mild increased intrasubstance signal in the distal plantar plate without discontinuity may indicate degenerative change (12a), particularly on longer TE sequences.10
Figure 11:
Normal plantar plate recess. A post-contrast fat-suppressed T1-weighted sagittal image demonstrates a tiny focus of enhancing fluid signal intensity (arrow) at the plantar plate insertion on the proximal phalanx. This is contiguous with the joint and penetrates less than half the thickness of the plantar plate.
Thinning and partial discontinuity of the plantar plate indicates more severe disease, which may progress to complete tear and retraction. Plantar plate tears most commonly occur at the distal phalangeal insertion (13a,14a).14
As instability progresses, the collateral ligament complexes may become attenuated and torn, usually on the lateral side (15a,15b).11 Lateral collateral ligament complex tears may result in dorsal and medial deviation of the toe, causing a “crossover deformity” with the second toe deviated dorsally over the great toe.15 Associated medial subluxation of the flexor digitorum tendons may also be present.13
Finally, the ligaments and plantar joint capsule may become completely disrupted, allowing dorsal dislocation of the toe with respect to the metatarsal (16a).16
Clinical diagnosis and management
In patients with plantar plate injuries of the lesser toes, the insidious onset of ill-defined forefoot pain is the most common presentation, although sudden onset after athletic injury can also occur. Physical examination may reveal point tenderness over the MTP joint.12 Dorsal stress on the toe may elicit pain at the plantar side of the MTP joint, and possibly dorsal subluxation of the toe (the “drawer sign”, considered positive if the toe can be displaced by 2 mm with reproduction of symptoms).6 More advanced disease may present with crossover deformity, hammertoe, or complete dorsal dislocation of the toe.16
Conservative treatment prior to onset of deformity may include stabilization by taping and/or use of a metatarsal pad. Altering the patient’s physical activity regimen may help reduce symptoms.17 For persistent pain or more advanced cases, surgical treatment may be indicated to restore neutral alignment of the joint. Capsular reefing may be sufficient in mild cases. Flexor tendon transfer and extensor digitorum longus tendon lengthening can be performed in more advanced cases.1 For complete dislocation, osteotomy may be necessary.18
Conclusion
Lesser metatarsophalangeal joint instability is a treatable cause of forefoot pain. Other causes of metatarsalgia such as stress fractures, flexor tendinitis, plantar keratosis, interdigital neuroma and adventitial bursitis may mimic or coexist with metatarsal joint instability. Clinical diagnosis in such patients may be difficult or equivocal, particularly in mild cases without joint deformity. MRI is a useful noninvasive method to evaluate for MTP joint instability and other forefoot pathology, allowing accurate diagnosis and appropriate treatment.
References
1 Haddad SL, Sabbagh RC, Resch S, Myerson B, Myerson MS: “Results of Flexor-to-Extensor and Extensor Brevis Tendon Transfer for Correction of the Crossover Second Toe Deformity”, Foot Ankle Int 20:781-788, 1999
2 Gregg J, Silberstein M, Clark C, Schneider T: “Plantar plate repair and Weil osteotomy for metatarsophalangeal joint instability”, Foot and Ankle Surgery, 13:116-121, 2007
3 Coughlin MJ: “Second metatarsophalangeal joint instability in the athlete”, Foot Ankle 14(6): 309-19, 1993
4 Coughlin MJ: “Lesser-Toe Abnormalities”, The Journal of Bone and Joint Surgery (American), 84:1446-1469, 2002
5 Stainsby GD: “Pathological anatomy and dynamic effect of the displaced plantar plate and the importance of the integrity of the plantar plate-deep transverse metatarsal ligament tie-bar”, Ann R Coll Surg Engl; 79(1):58-68, 1997
6 Yu GV, Judge MS, Hudson JR, Seidelmann FE: “Predislocation syndrome: progressive subluxation / dislocation of the lesser MPJ”, J Am Podiatr Med Assoc 92 (4): 182-199, 2002
7 Deland JT, Lee KT, Sobel M, DeCarlo EF: “Anatomy of the Plantar Plate and its Attachments in the Lesser Metatarsophalangeal Joint”, Foot and Ankle International 16(8): 480-486, 1995
8 Sarrafian SK: Anatomy of the foot and ankle, Lippincott, Philadelphia PA, p. 189, 1983
9 Loretz L, Gerbert J, Moss K: “Significance of the suspensory and collateral ligaments in lesser metatarsal neck surgery”, J Foot Surg 23: 123-128, 1984
10 Mohana-Borges AVR, Theumann NH, Pfirrmann CWA, Chung CB, Resnick DL, Trudell DJ: Lesser Metatarsophalangeal Joints: Standard MR Imaging, MR Arthrography and MR Bursography ? Initial Results in 48 Cadaveric Joints, Radiology 227 (1), 175-182, 2003
11 Stoller, DA: Magnetic Resonance Imaging in Orthopaedics and Sports Medicine, 3rd edition, Lippincott Williams & Wilkins, Baltimore, Chapter 5, 965-969, 2007
12 Porter DA, Schon LC: Baxter’s The Foot and Ankle in Sport, 2nd edition, Mosby, Chapter 17, 2007
13 Gregg JM, Schneider T, Marks P: “MR Imaging and Ultrasound of Metatarsalgia ? The Lesser Metatarsals”, Radiol Clin N Am (46) 1061-1078, 2008
14 Umans HR, Elsinger E: “The plantar plate of the lesser metatarsophalangeal joints: potential for injury and role of MR imaging”, Magn Reson Imaging Clin N Am. 9(3):659-669, 2001
15 Kaz AJ, Coughlin MJ: “Crossover second toe: demographics, etiology and radiographic assessment”, presented at the American Orthopaedic Foot and Ankle Society 23rd Annual Summer Meeting, Toronto, July 13-15, 2007
16 Coughlin MJ: “Subluxation and dislocation of the second metatarsophalangeal joint”, Orthop Clin North Am; 20(4):535-551, 1989
17 Mizel MS, Yodlowski ML: “Disorders of the Lesser Metatarsophalangeal joints”, J Am Acad Orthop Surg, 3:166-173, 1995
18 O’Kane C, Kilmartin TE: “The surgical management of central metatarsalgia”, Foot Ankle Int. 23(5):415-9, May 2002