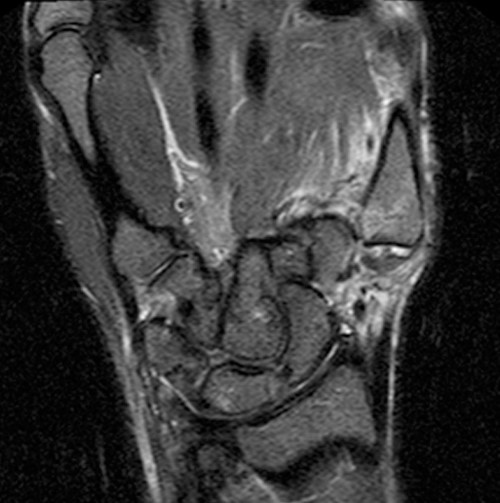
Clinical History: A 21 year-old male crashed his all-terrain vehicle 10 days ago and radiographs revealed dorsoradial dislocation of the thumb CMC joint. Coronal STIR images of the wrist/thumb are provided. What are the findings?
Findings
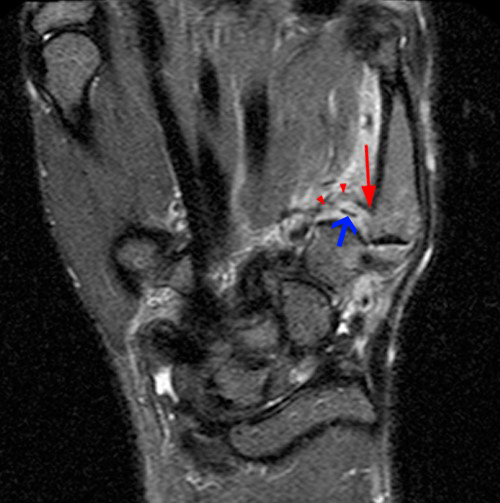
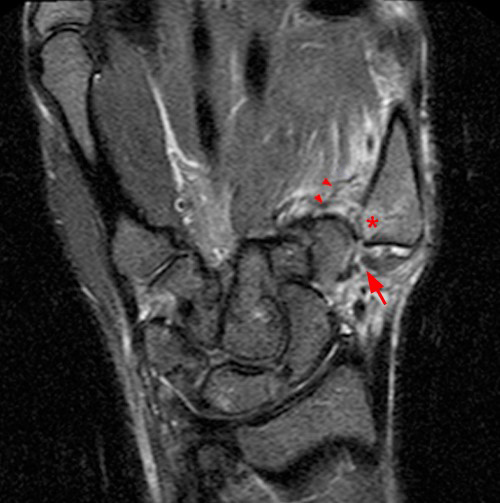
Figure 2:
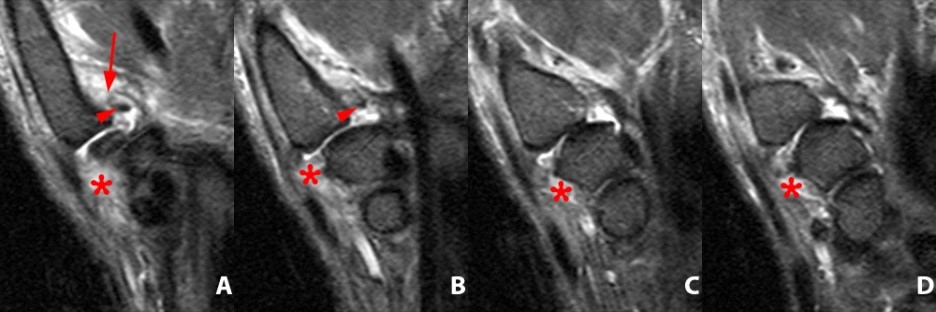
Coronal STIR images (A,B) reveal dorsoradial thumb CMC joint dislocation with laxity and edema of the anterior oblique ligament (AOL) (red arrowheads) and 5 mm distal stripping of the AOL attachment to the metacarpal base (arrow) with a small cortical avulsion fracture fragment (blue arrow) and a bone bruise in the metacarpal base (asterisk). An extensive partial tear of the trapezial aspect of the dorsal ligaments with focal trapezial avulsion is present (short arrow, B).
Diagnosis
Dorsoradial dislocation of the thumb CMC joint with a small cortical avulsion fracture and volar and dorsal ligament disruption.
Introduction
The thumb CMC (or trapeziometacarpal) joint is a semi-constrained, biconcave saddle joint between the distal surface of the trapezium and the base of the first metacarpal. It is composed of two perpendicular opposing saddles (Figure 3) which make possible a wide range of motion: flexion and extension in the plane of the palm of the hand, abduction and adduction in the plane at a right angle to the palm as well as circumduction, opposition (approximation of the thumb to the volar tip of the fifth finger) and apposition (contact between the volar tips of the thumb and the other fingers). This anatomy results in an opposable thumb with enhanced dexterity, grasp and pinch.1
The CMC joint of the thumb is one of the basal joints of the thumb and each is a trapezial articulation. The other three are the trapeziotrapezoid, scaphotrapezial and trapezium-index metacarpal joints. Of these, only the thumb CMC and scaphotrapezial joints are oriented along the longitudinal compression axis of the thumb and are therefore prone to trauma and degeneration. This web clinic is focused on the thumb CMC joint and will describe the normal anatomy and MR appearance of the principal ligaments supporting the thumb CMC joint, discuss post-traumatic and degenerative alterations that are observed with MRI and comment on the role of MRI in evaluating this joint and its ligaments.
Overview of Thumb CMC Joint Anatomy and Injury
The thumb metacarpal base is concave dorsal to volar and convex radial to ulnar, whereas the trapezial concave arc is radial to ulnar and the convex arc is dorsal to volar (Figure 3). The opposing articular surfaces have disparate radii of curvature that are congruent only at extremes of motion and incongruent in all other positions, including at rest. Due to the shallow concavity of each articular surface, there is little intrinsic skeletal stability.2,3,4
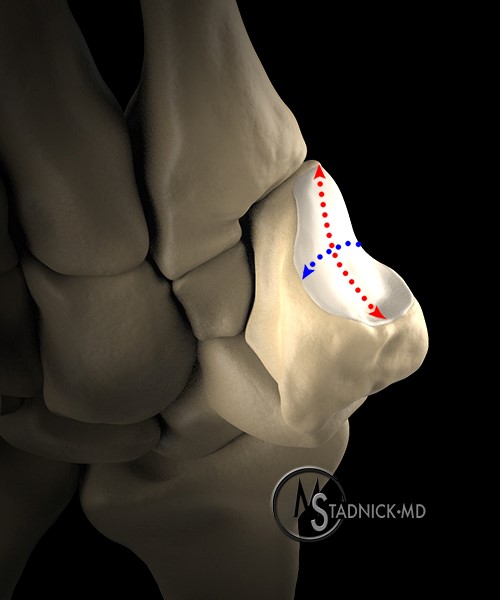
Figure 3:
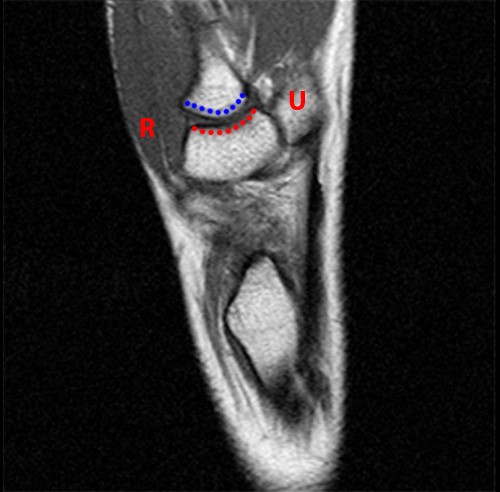
(3A) A three dimensional representation of the distal trapezial articular surface demonstrates a concave surface contour in the radial to ulnar direction (red dotted lines) and a convex surface contour in the dorsal to volar plane (blue dotted lines).
On a sagittal T1-weighted image of the wrist, coronal view of the thumb CMC joint (3B), the articular surface of the metacarpal base (blue dotted line) is convex and that of the trapezium (red dotted line) is concave in the radial - ulnar plane. R= radial, U= ulnar. On a coronal T2-weighted image of the wrist, sagittal view of the thumb CMC joint (3C), the articular surface of the metacarpal base is concave (blue dotted line) and that of the trapezium is convex (red dotted line), in the dorsal to volar plane. D = dorsal, V = volar.
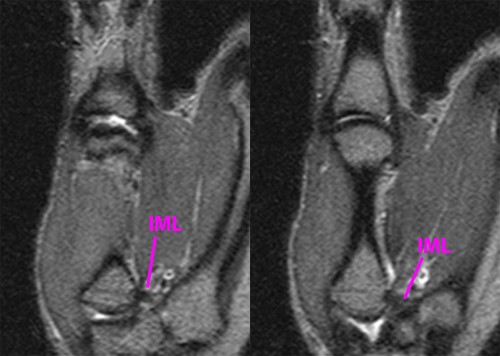
Stability at the thumb CMC joint is maintained by a capsuloligamentous complex which allows greater joint mobility and consists of five main components: the anterior oblique, or “beak”, ligament (AOL), the dorsoradial ligament (DRL), the dorsal central ligament (DCL), the posterior oblique ligament (POL) and the intermetacarpal ligament (IML) (Figure 4). Two other ligaments, at the ulnar aspect of the joint, the ulnar collateral ligament (UCL) and the first dorsal trapeziometacarpal ligament (DTM1), have less biomechanical significance. Dynamic stability of the thumb CMC joint is provided by nine muscles and tendons, of which the dorsal expansion of the abductor pollicis longus (APL) is the most important.5
Figure 4:
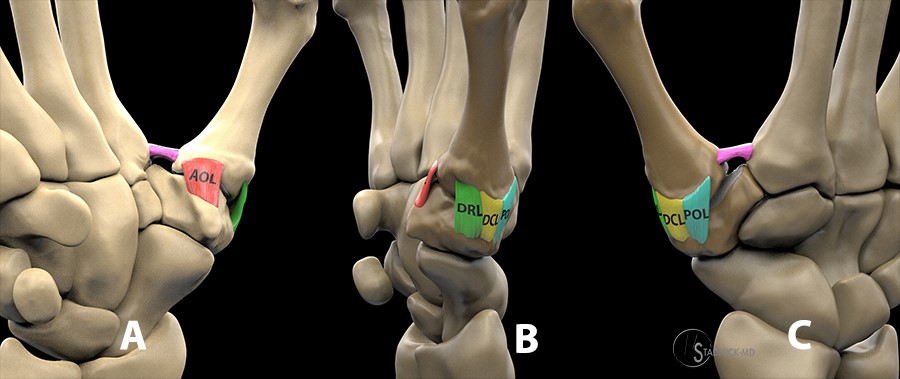
3-dimensional representations of the five principal supporting ligaments of the thumb CMC joint viewed from the volar perspective (A), the radial aspect of the joint (B) and from the dorsal perspective (C). AOL = anterior oblique ligament (red), DRL = dorsal radial ligament (green), DCL = dorsal central ligament (yellow), POL = posterior oblique ligament (blue). The intermetacarpal ligament is depicted in purple, bridging the thumb and index finger metacarpal bases. (Click on image for 3D interactive view. Click-drag to rotate, scroll to zoom.)
The most common injury of the thumb CMC joint is the Bennett fracture, which is an oblique, intra-articular fracture of the first metacarpal base associated with dorsal subluxation or dislocation of the metacarpal. This fracture usually occurs secondary to an axial blow on a partially flexed first metacarpal as occurs when punching an object with a clenched fist. It produces a variable-sized fragment of the volar lip of the metacarpal base that is anchored by the AOL. The remainder of the metacarpal is pulled proximally, radially and dorsally by the abductor pollicis longus tendon. The larger the volar fragment, the more likely the thumb CMC joint is unstable. Much less common is the Rolando fracture, classically a 3-part intra-articular fracture of the metacarpal base (but the term is also applied to comminuted intra-articular fractures) associated with dorsal subluxation. If the fracture cannot be anatomically reduced, open reduction and internal fixation are required. Isolated subluxation or dislocation of the thumb CMC joint is an uncommon injury. It is the result of ligament injury and, if not adequately treated, predisposes to joint instability with incongruent loading, progressive wear of articular cartilage and synovitis, hallmarks of osteoarthritis.
Thumb CMC Joint Ligaments
Volar Ligaments
Anterior Oblique (Beak) Ligament (AOL)
The AOL, also known as the beak ligament, has its origin at the volar tubercle of the trapezium and attaches to the volar beak of the first metacarpal base, at the ulnar-volar aspect of the joint.6,7,8,9 It has been described as consisting of a superficial, capsular layer and a deep, intracapsular layer.10,11 However, two distinct layers could not be distinguished in recent studies utilizing surgical dissection or arthroscopy12,13 or with ultrasound or conventional MRI.14,15 Alternatively, Cardoso et al. consistently identified the superficial and deep portions of the AOL in all 7 cadaveric specimens studied with MR-arthrography.15 At this time, most authors do not distinguish between these two layers.6-9 The volar joint capsule and AOL are intimately connected to the overlying thenar muscles which contribute to volar stability of the joint.16 In the previous century, the AOL was considered the most important stabilizing ligament of the thumb CMC joint, resisting dorsoradial and volar subluxation.11 More recent studies have increasingly stressed the importance of the dorsal ligaments and de-emphasized the AOL in ensuring joint stability.12,17,18
Ulnar Collateral Ligament (UCL)
The UCL is an extracapsular ligament that originates from the distal/ulnar margin of the flexor retinaculum insertion on the trapezial ridge, courses ulnar to the AOL and inserts on the volar ulnar tubercle of the first metacarpal base. It has intra-articular extensions that blend with the AOL.13 Recent studies have found that the UCL insertion on the first metacarpal is more volar and ulnar than previously described, suggesting it be renamed the “first volar trapeziometacarpal ligament” as its insertion is analogous to that of the first dorsal trapeziometacarpal ligament.12,13 It is a checkrein on extension and abduction.12
Dorsal Ligaments
Dorsal Deltoid Ligament
The dorsal deltoid ligament consists of three ligaments that are, from radial to ulnar, the dorsoradial ligament (DRL), the dorsal central ligament (DCL) and the posterior oblique ligament (POL).4 Each originates from the dorsal tubercle of the trapezium and, together, they form a broad insertion on the dorsal edge of the first metacarpal base. The DRL originates on the radial side of the dorsal trapezial tubercle and inserts on the radial-dorsal side of the metacarpal. The DCL and POL are purely dorsal structures, ulnar to the DRL. The DCL is the shortest and thickest and the POL is the longest of these ligaments.12 The DRL courses subjacent to and is reinforced by the abductor pollicis longus tendon. The DCL is directly beneath the extensor pollicis brevis (EPB) tendon.
The Intermetacarpal Ligament (IML)
The IML is an extracapsular ligament that runs obliquely from the dorsoradial aspect of the second metacarpal to the volar-ulnar tubercle of the first metacarpal base. It is just radial and volar to the extensor carpi radialis longus tendon insertion on the second metacarpal base. It inserts on the first metacarpal base adjacent to the UCL and POL insertions and its fibers are interspersed with UCL fibers at the metacarpal insertion. It is an extracapsular ligament and restricts radial translation of the first metacarpal.
Role of Thumb CMC Joint Ligaments in Joint Stability
As noted above, the dorsal ligaments are seen as having a critical role and the AOL a lesser function in conferring joint stability.19 On cadaveric dissection, the AOL is described as thin, membranous and diaphanous and, histologically, consisted of disorganized connective tissue with sparse collagen fibers and hypocellularity.12,13 A caveat is that the average age of the specimens was 69 and 76 years, respectively, in these two studies and the ligament appearance may represent degenerative change concomitant with aging. This is supported by a small study in which poor or lack of visualization of the AOL with high resolution ultrasound occurred in cadavers with advancing CMC joint degeneration.14 In contrast, in the dissection study, the dorsal ligaments were universally thick and stout with thick, organized collagen bundles.12 Biomechanical studies indicate that the dorsal ligaments are the chief restraints to posterior shear translation and dislocation and that the AOL provides support as a thin, complementary tension band.12,13,17 This is illustrated by a cadaveric study in which the AOL had to subperiosteally strip off the volar cortex of the metacarpal for dorsal dislocation to occur. An in vivo joint kinematic study concluded that the AOL is likely slack during most physiological positions, whereas the DRL appears taut and is, therefore, supporting the joint in positions of CMC joint abduction and flexion.19 The dorsal ligaments are innervated with sensory nerve endings, called mechanoreceptors, which monitor joint position and kinesthesia. They are most numerous about the metacarpal insertion and indicate that these ligaments are important for proprioception.4,16
MR Imaging Appearance of the CMC Joint Ligaments
Figure 5:
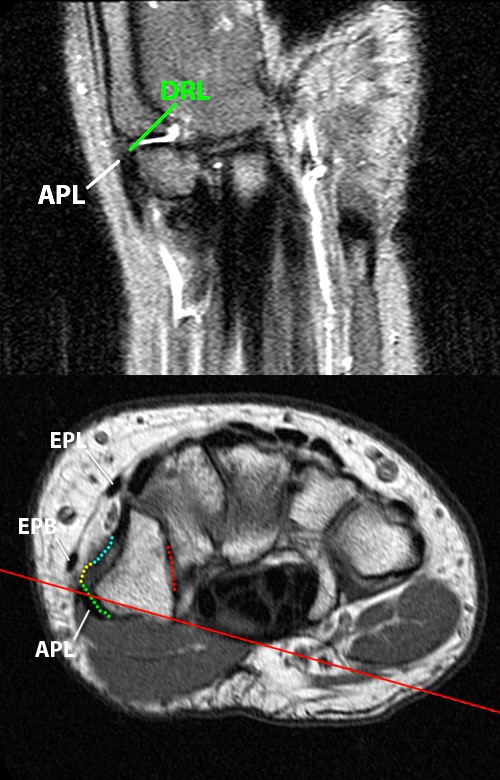
At the radial aspect of the thumb trapeziometacarpal joint (A), the dorsoradial ligament (DRL) and overlying abductor pollicis longus (APL) tendon cannot be distinguished from one another adjacent to the radial aspect of the dorsal tubercle of the trapezium.
In (B), just ulnar to the DRL ligament¬, the dorsal central ligament (DCL) lies directly beneath the extensor pollicis brevis tendon (EPB).
The next ulnar image in (C), is the junction of the DCL and posterior oblique ligament (POL). At the volar aspect, the anterior oblique ligament (AOL) attaches to the articular margin.
Nearing the ulnar aspect of the joint on the next image slice, the posterior oblique ligament (POL) and anterior oblique ligament (AOL) are both identified.
The normal MR imaging appearance of the thumb CMC joint ligaments is demonstrated in figures 5 and 6. The volar and dorsal ligaments of the thumb CMC joint are best seen on sagittal images and the IML is best seen in the coronal plane. The dorsal ligaments form a near continuous, deltoid-shaped ligament complex, best seen in the sagittal plane. Although it is not necessary to distinguish between the three dorsal ligaments on MRI, the DCL and the DRL are always found directly beneath the EPB and APL tendon, respectively. In most radiology practices, the CMC joint of the thumb is imaged in axial, sagittal oblique and coronal oblique planes as part of an MR exam of the wrist. The degree of obliquity can be determined by referring to annotated axial images. A sagittal oblique image is usually slanted across the first metacarpal such that the dorsoradial and ulnovolar surfaces are seen on the same image, rather than straight dorsal to volar. It has not been determined if scanning in the true coronal and sagittal planes of the joint would result in greater accuracy in interpretation. Optimal imaging of this small joint is best accomplished with a high field strength scanner (1.5 or 3 T), and a dedicated wrist coil, such as an MR-microscopy coil. Isotropic 3-dimensional imaging is a newer technique that eliminates slice gaps and partial volume averaging and allows reformatting images into any desired plane without loss of spatial resolution. It is a promising technique for imaging small joints.
The MR appearance of the principal supporting ligaments of the thumb CMC joint has been most thoroughly studied by Hirschmann et al., imaging 34 asymptomatic volunteers with a mean age of 33.9 years +/- 9.2 years. 20 Utilizing a 1.5 T scanner, the POL and IML were identified in all patients and the AOL and DRL were each visible in all but one patient. The DCL had not been described at the time this study was performed. The thin, extracapsular UCL could not be distinguished from the AOL, consistent with prior experience with MRI and ultrasound,14 and was not analyzed.
On intermediate-weighted fat-saturated images, the ligaments were described as structures of low signal intensity, increased signal intensity or striated (lamellar pattern of low and increased signal intensities). All four ligaments varied in signal intensity from patient to patient such that, among the 34 volunteers, each pattern of signal intensity was observed. The DRL and POL were predominantly increased in signal intensity, the IML was predominantly striated and the AOL appearance was spread nearly equally among low, increased and striated signal intensity.20 These results are at variance with previous studies that reported low signal intensity of these ligaments.15,21
It is uncertain whether this is due to ligament composition, magic angle effect or, for the AOL, the presence of two layers. For the IML, striation is likely due to ligament composition as it is oriented horizontal to the plane of the magnetic field, rendering magic angle moot.
The thickness of the ligaments varied considerably, with the mean thickness as follows: IML: 2.9 – 3.1 (+/-0.9) mm, POL: 1.9 – 2.3 (+/-0.6) mm, AOL: 1.4 – 1.6 (+/-0.6) mm and DRL: 1.2 – 1.4 (+/-0.5) mm. One may conclude that a confident diagnosis of ligament thickening requires a thickness of 3.0 mm for the POL (and probably, the DCL), 2.0 mm for the DRL and 2.4 mm for the AOL.
MR Imaging of Thumb CMC Joint Ligament Injuries
Ligamentous injury of the thumb CMC joint varies from low grade partial ligament tear (usually the AOL) to disruption of all five major ligaments with dislocation. The most common injury is a partial or complete tear of the AOL at its metacarpal insertion. The next most common ligament injury involves the dorsal ligaments at their trapezium attachment.21 Injury is typically caused by a longitudinally directed force on the CMC joint in full flexion. Extent and severity of injury will vary depending upon the rate and direction of the loading force.22 Less frequently, injury is due to a direct blow into the first web space of the thumb, such as may be produced by a motorcycle handlebar at impact.23
Following CMC joint ligament injury, radiographs usually provide limited information, demonstrating soft tissue swelling and, occasionally, a Bennett fracture at the metacarpal base. Stress views may show loss of anatomic alignment, indicating compromise of ligament function.21 Given the normal variation in thickness and signal intensity of the ligaments of the thumb CMC joint, the MR criteria for diagnosing injury to these ligaments are still evolving.
The largest study to assess MRI in evaluation of tear of these ligaments, by Connell et al., included only 14 injuries of which 4 had surgical confirmation.21 Partial or complete ligament discontinuity or ligament avulsion are the most reliable signs of injury. For the AOL, injury occurs at the metacarpal insertion where periosteal stripping of the metacarpal attachment is common with partial tears (Figure 7). Increased signal intensity of the ligament on fluid-sensitive images with peri-ligamentous edema suggests a ligament sprain but such edema may also be seen with chronic synovitis. Secondary signs of ligament tear that may be present include adjacent soft tissue hematoma and subcortical bone contusion on one or both sides of the CMC joint. Patients with chronic injury may reveal ligament laxity/redundancy, ligament thickening and/or a ganglion cyst arising from the AOL insertion on the thumb metacarpal. An AOL tear at the trapezial origin has not been reported. Other findings that MRI may demonstrate include chondral injury or thinning, bone contusion, occult fracture, avulsion fracture and intra-articular osseous fragments or interposed soft tissue.21
Figure 7:
A 44 year-old male with dorsoradial thumb CMC joint dislocation (following reduction) due to fall on the outstretched hand 6 days ago. Sequential coronal STIR images moving from radial (A) to ulnar (D) a reveal a high grade partial tear of the AOL with distal retraction of its attachment to metacarpal base (arrow, A) with periosteal stripping and with small avulsed cortical fragment (arrowheads in A and B). A severe partial tear of the trapezial aspect and attachment of the dorsal ligaments is present (asterisks) - DRL in (A), DRL/DCL in (B), DCL in (C), POL in (D).
In cases of dorsal ligament injury, the DRL, DCL and POL are often not clearly separable from one another and involvement of each is implied by knowledge of the anatomy. For each, injury typically entails avulsion or partial tearing at the trapezial attachment. In the study of Connell et al., the MR findings were validated in the four cases with surgical confirmation.21 Among the radiologist interpreters, there was good agreement on tear versus no tear but discrepancy was common in determining the degree of partial tearing as being mild, moderate or severe. MR-arthrography may have a role in evaluating these ligaments as it improved visualization of the IML, AOL and UCL and would be expected to increase conspicuity of cartilage abnormalities.15 Small field of view, high resolution imaging techniques would also be expected to enhance evaluation of these ligaments.24,25
Dorsoradial subluxation of the thumb CMC joint is a feature of both acute ligament injury and advancing osteoarthritis. Since the CMC joint is not congruent at rest, it may be difficult to recognize pathologic subluxation on radiographs or with MRI. A radiographic study of 69 healthy volunteers found radial subluxation to vary from 1.72 to 8.69 mm.26 The MRI study of 34 volunteers, discussed above, found a mean radial subluxation of 2.8 – 3.4 mm and dorsal subluxation of 1.8 to 2.0 mm.21
Treatment of Thumb CMC Joint Dislocation
Following thumb CMC joint dislocation, the goal of therapy is to restore joint stability. It has been documented that thumb CMC joint dislocation requires a complete or near-complete tear or proximal avulsion of the dorsal ligaments and varying degrees of stripping of the AOL from its metacarpal attachment23,27,28,29,30 Consensus on a uniform treatment approach has not yet been achieved but, in the last 20 years, there has been a trend toward conservative management or minimally invasive methods.31 If the joint is clinically stable after closed reduction, it is usually managed with plaster cast immobilization for 4 weeks. If the joint is unstable following reduction, some authors advocate K-wire fixation, plaster cast immobilization and radiographic/CT followup32 whereas others favor dorsal capsulorraphy and ligament reconstruction, especially in athletes with high upper extremity demand.28,30 Chronic dislocation requires open reduction, K-wire fixation, capsulorraphy and/or ligament reconstruction with plaster casting. A trial of splinting, non-steroidal anti-inflammatory drugs and intra-articular steroid injections is often used with a chronically unstable thumb CMC joint, however, if there is uncontrollable pain and loss of function, surgery is usually performed.32
CMC Joint Osteoarthritis (OA)
OA of the thumb CMC joint is a common disorder and 2 to 6 times more prevalent in women than in men. It increases with age and is usually due to trauma or overuse. For example, it may be produced by an occupation that requires manipulating a mouse with one hand and a microphone with the other for 8 to 12 hours a day and sometimes on weekends. One study reported a radiographic prevalence of 40% in women and 25% in men older than 75 years of age.33 It is likely even more prevalent, considering that radiographic staging may underestimate the extent of degeneration observed at surgery.34
It has been suggested that increased prevalence in women is due, at least in part, to increased concavity of the volar-dorsal aspect of the trapezial articular surface, creating a less congruent joint. 35 Recent CT-imaging based studies have found no difference in the shape of the articular facets of the CMC joint between men and women. The only difference in morphology was that the trapezium and first metacarpal are larger, on average, in men. It is hypothesized that a smaller volume of articular surface may be subject to increased biomechanical stress, thereby promoting development of osteoarthritis.36 Increased frequency of OA in this joint is also observed in females in the 5th and 6th decades and this has been attributed to increased ligament laxity and flexibility induced by the hormones estrogen and relaxin.30
Although the dorsal ligaments are the apparent primary restraint to traumatic dorsal subluxation, degeneration of the AOL has a primary role in development and progression of thumb CMC joint OA, indicating that this ligament is biomechanically important. Several studies have shown that degeneration of the AOL at its metacarpal attachment closely correlates with the presence and severity of degenerative arthrosis.6,10,37
With degeneration, the fibrocartilaginous insertion of the AOL retreats distally on the metacarpal and a volar synovial recess forms with variable osteophyte formation (Figures 8 and 9). As degeneration progresses, periosteal stripping of the AOL insertion ensues and this recess enlarges. Dorsal translation of the metacarpal increases and, at its end point, the ligament detaches. Progressive cartilage wear, initially primarily volar, spreads throughout the joint.10 Periarticular ganglion cysts are often seen as degeneration proceeds (Figure10).
Figure 8:
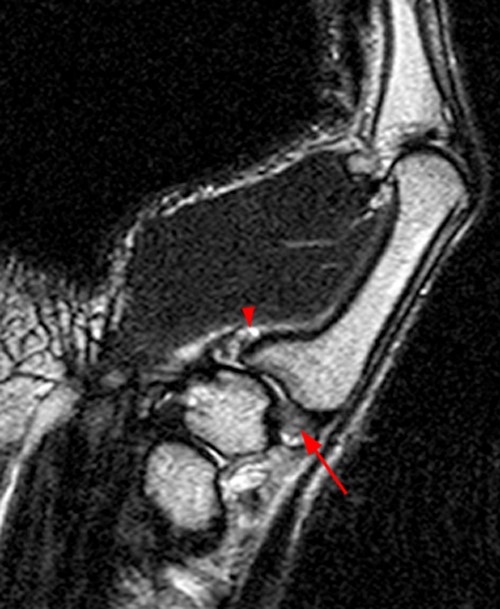
A 63 year-old female with CMC joint OA. Coronal T1-weighted (left) and STIR (right) images. Volar beak osteophyte of the metacarpal (arrowheads) with dorsal capsuloligamentous thickening (arrows). The AOL is attenuated with distal retraction of its metacarpal attachment (short arrow) distal to the osteophyte, best seen on the STIR image (right).
Figure 9:
A 50 year-old male with history of multiple dirt bike crashes in the past 6 months. A coronal T2-weighted image demonstrates CMC joint OA with a chronic distal tear of the AOL with retraction distally and a small ganglion cyst (arrowhead), thickened DCL (arrow), dorsal subluxation and severe cartilage loss.
Figure 10:
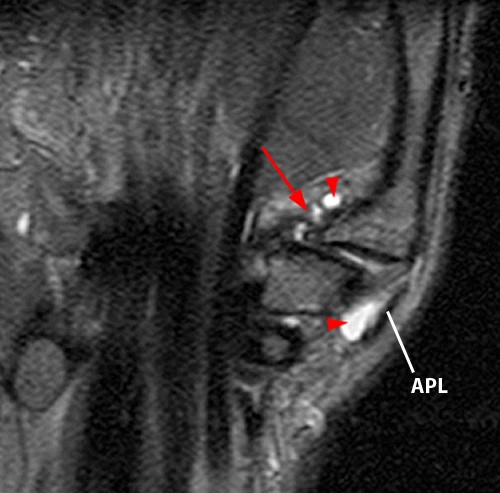
A 48 year-old female with severe wrist pain for 2 months. A coronal STIR image reveals attenuation and distal retraction of the AOL (arrow) with ganglion cysts (arrowheads) adjacent to the AOL and deep to the APL tendon, respectively, and dorsoradial subluxation. Mild increase in signal intensity of the DRL may be due to normal variation, recent sprain or chronic degeneration.
Affected patients present with localized pain, swelling, reduced motion, instability and weakness, with symptoms exacerbated by pinch or grasping. Alternative etiologies may be sought for pain at the thumb base, such as deQuervain’s tenosynovitis, scaphoid injury, flexor carpi radialis tendon pathology and carpal tunnel syndrome.38 Currently, diagnosis and treatment of thumb CMC joint OA rely on clinical history, physical examination and radiography. Instability is difficult to assess clinically due to the complex anatomy and biomechanics and if pain and swelling are present14. Surgery is indicated in patients with persistent pain, joint instability, decreased function and failed conservative therapy. The type of surgery depends on the stage of disease and options include beak ligament reconstruction with tendon interposition, implant arthroplasty and arthrodesis.5
Due to the limitations of radiography in evaluating instability and degeneration, it has been suggested that MRI may play a role in patients with CMC ligament laxity not responsive to conservative therapy.39 Since the AOL undergoes a predictable pattern of alteration at its metacarpal attachment as degeneration proceeds, this would be the imaging target. Studies have shown favorable outcomes when volar ligament reconstruction is used to treat painful, unstable, non-arthritic thumbs.39 Therefore, if a high resolution MRI demonstrated partial AOL detachment with or without a small volar synovial recess and relatively intact articular cartilage, this would indicate that the patient is a candidate for ligament reconstruction, with the goal of preventing or delaying development of progressive OA.39 If the ligament was intact, supportive therapy would be continued.
Conclusion
The most important joint of the thumb is the CMC joint and its unique anatomy facilitates a broad range of motion and makes possible prehension, which consists of grasping, pinching and manipulation of objects. Isolated dislocation of this joint is rare but instability and degeneration are common. Because of the small size of the joint and its supporting ligaments, it is best imaged with high resolution MR techniques. In particular, isotropic 3-dimensional MR imaging has great promise for imaging this joint.25 In order to provide an accurate assessment of this joint, the radiologist needs to know the anatomy and the reproducible patterns of injury, instability and degeneration. Evaluation of the ligaments may be challenging due to normal variation in signal intensity that has been observed on MRI. Confident diagnosis of dorsoradial subluxation may be difficult due to imaging in oblique planes, normal joint incongruity at rest and a normal broad range of motion. In patients with acute injury, MRI is useful for assessment of the ligaments and detection of pre-existing degenerative change. MR imaging may be useful in planning surgery in patients with mild or early instability, in whom reconstruction of the AOL may eliminate symptoms and halt or delay the degenerative process.
References
- Brown DP, Freeman ED, Cuccurullo S, Freeman TL. “Upper Extremities – Hand Region: Range of Motion of the Digits”. In Cuccurullo S: Physical Medicine and Rehabilitation Board Review, Demos Medical Publishing, 2004. ↩
- Edmunds JO. Traumatic dislocations and instability of the trapeziometacarpal joint of the thumb. Hand Clin 2006; 22:365-392. ↩
- Edmunds JO. Current concepts of the anatomy of the thumb trapeziometacarpal joint. J Hand Surg 2011; 36A:170-182. ↩
- Ladd AL, Weiss A-P C, Crisco JJ, Hagert E, Wolf JM, Glickel SZ, Yao J. The thumb carpometacarpal joint: anatomy, hormones and biomechanics. Instr Course Lect 2013; 62:165-179. ↩
- Khorashadi L, Ha AS, Chew FS. Radiologic guide to surgical treatment of first carpometacarpal joint osteoarthritis. AJR 2012; 198:1152-1160. ↩
- Pellegrini VD Jr. Osteoarthritis of the trapeziometacarpal joint: the pathophysiology of articular cartilage degeneration. I. Anatomy and pathology of the aging joint. J Hand Surg Am 1991; 16(6):967-974. ↩
- Imaeda T, An KN, Cooney WP, Linscheid R. Anatomy of trapeziometacarpal ligaments. J Hand Surg Am 1993; 18(2):226-231. ↩
- Pellegrini VD Jr, Olcott CW, Hollenberg G. Contact patterns in the trapeziometacarpal joint: the role of the palmar beak ligament. J Hand Surg Am 1993; 18(2)238-244. ↩
- Bettinger PC, Linscheid RL, Berger RA, Cooney WP III, An KN. An anatomic study of the stabilizing ligaments of the trapezium and trapeziometacarpal joint. J Hand Surg Am 1999; 24(4):786-798. ↩
- Doerschuk SH, Hicks DG, Chinchilli VM, Pellegrini VD Jr. Histopathology of the palmar beak ligament in trapeziometacarpal osteoarthritis. J Hand Surg Am 1999; 24:496-504. ↩
- Nanno M, Burford WL, Patterson RM, Andersen CR, Viegas SF. Three-dimensional analysis of the ligamentous attachments of the first carpometacarpal joint. J Hand Surg Am 2006; 31:1160-1170. ↩
- Ladd AL, Lee J, Hagert E. Macroscopic and microscopic analysis of the thumb carpometacarpal ligaments. A cadaveric study of ligament anatomy and histology. J Bone Joint Surg Am 2012; 94:1468-1477. ↩
- Zhang AY, Nortwick SV, Hagert E, Ladd AL. Thumb carpometacarpal ligaments inside and out: A comparative study of arthroscopic and gross anatomy from the Robert A. Chase Hand and Upper Limb Center at Stanford University. J Wrist Surg 2013; 2:55-62. ↩
- Gondim Teixeira PA, Omoumi P, Trudell DJ, Ward SR, Blum A, Resnick DL. High-resolution ultrasound evaluation of the trapeziometacarpal joint with emphasis on the anterior oblique ligament (beak ligament). Skeletal Radiol 2011; 40:897-904. ↩
- Cardoso FN, Kim H-J, Albertotti F, Botte MJ, Resnick DL, Chung CB. Imaging the ligaments of the trapeziometacarpal joint: MRI compared with MR arthrography in cadaveric specimens. AJR 2009; 192:W13-W19. ↩
- Mobargha N, Ludwig C, Ladd AL, Hagert E. Ultrastructure and innervation of thumb CMC ligaments in surgical patients with osteoarthritis. Clin Orthop Relat Res 2014; 472(4):1146-1154. ↩
- D’Agostino P, Kerkhof FD, Shahabpour M, Moermans JP, Stockmans F, Veereevke EE. Comparison of the anatomical dimensions and mechanical properties of the dorsoradial and anterior oblique ligaments of the trapeziometacarpal joint. J Hand Surg Am 2014; 39(6):1098-1107. ↩
- Gluck JS, Balutis EC, Glickel SZ. Thumb Ligament Injuries. J Hand Surg Am 2015; 40(4):835-842. ↩
- Halilaj E, Rainbow MJ, Moore DC, Laidlaw DH, Weis A-P C, Ladd AL, Crisco JJ. In vivo recruitment patterns in the anterior oblique and dorsoradial ligaments of the first carpometacarpal joint. J Biomech 2016 (in press). http://dx.doi.org/10.1016/j.jbiomech.2015.04.028 ↩
- Hirschmann A, Sutter R, Schweizer A, Pfirrmann CWA. The carpometacarpal joint of the thumb: MR appearance in asymptomatic volunteers. Skeletal Radiol 2013; 42:1105-1112. ↩
- Connell DA, Pike J, Koulouris G, Van Wettering N, Hoy G. MR imaging of thumb carpometacarpal joint ligament injuries. J Hand Surg Br 2004; 29(1):46-54. ↩
- Strauch RJ, Behrman MJ, Rosenwasser MP. Acute dislocation of the carpometacarpal joint of the thumb: an anatomic and cadaver study. J Hand Surg Am 1994; 19:93-98. ↩
- Uchida S, Sakai A, Okazaki Y, Okimoto N, Nakamura T. Closed reduction and immobilization for traumatic isolated dislocation of the carpometacarpal joint of the thumb in rugby football players. Two case reports. Am J Sports Med 2001; 29(2):242-244. ↩
- Kwok WE, You Z, Monu J, Seo G, Ritchlin C. High resolution uniform MR imaging of finger joints using a dedicated RF coil at 3 Tesla. J Magn Reson Imaging 2010; 31(1):240-247. ↩
- Johnson D, Stevens KJ, Riley G, Shapiro L, Yoshioka H, Gold GE. Approach to MR imaging of the elbow and wrist. Technical aspects and innovation. Magn Reson Imaging Clin N Am 2015; 23:355-366. ↩
- Wolf JM, Oren TW, Ferguson B, Williams A, Peterson B. The carpometacarpal stress view radiograph in the evaluation of trapeziometacarpal joint laxity. J Hand Surg Am 2009; 34(8):1402-1406. ↩
- Rettig AC. Athletic injuries of the wrist and hand. Part II: overuse injuries of the wrist and traumatic injuries to the hand. Am J Sports Med 2004; 32(1)262-273. ↩
- Shah J, Patel M. Dislocation of the carpometacarpal joint of the thumb. A report of four cases. Clin Ortop Relat Res 1983; 175:166-169. ↩
- Khan AM, Ryan MG, Teplitz GA. Bilateral carpometacarpal dislocations of the thumb. Am J Orthop 2003; 32:38-41. ↩
- Fotiadis E, Svarnas T, Lyrtzis C, Papadopoulos A, Akritopoulos P. Isolated thumb carpometacarpal joint dislocation: a case report and review of the literature. J Orthop Surg Res 2010; 5:16-22. ↩
- Neumann DA, Bielefeld T. The carpometacarpal joint of the thumb: stability, deformity and therapeutic intervention. J Orthop Sports Phys Ther 2003; 33:386-399. ↩
- Bosmans B, Verhofstad MHJ, Gosens T. Traumatic thumb carpometacarpal joint dislocations. J Hand Surg Am 2008; 33:438-441. ↩
- Armstrong AL, Hunter JB, Davis TR. The prevalence of degenerative arthritis of the base of the thumb in post-menopausal women. J Hand Surg Br 1994; 19:340-341. ↩
- Wajon A, Ada L, Edmunds I. Surgery for thumb (trapeziometacarpal joint) osteoarthritis. Cochrane Database Syst Rev 2005; 4:CD004631. ↩
- Ateshian GA, Rosenwasser MP, Mow VC. Curvature characteristics and congruence of the thumb carpometacarpal joint: differences between female and male joints. J Biomech 1992; 25:591-607. ↩
- Schneider MTY, Zhang J, Crisco, Weiss APC, Ladd AL, Nielsen P, Besier T. Men and women have similarly shaped carpometacarpal joint bones. J Biomech 2016 (in press). http://dx.doi.org/10.1016/j.jbiomech.2015.05.031. ↩
- Pellegrini VD Jr. Osteoarthritis and injury at the base of the human thumb: survival of the fittest? Clin Orthop Relat Res 2005; 438:266-276. ↩
- Melville DM, Taljanovic MS, Scalcione LR, Eble JM, Gimber LH, DeSilva GL, Sheppard JE. Imaging and management of thumb carpometacarpal joint osteoarthritis. Skeletal Radiol 2015; 44:165-177. ↩
- Collins E. Magnetic resonance imaging technology in evaluating the presence and integrity of the anterior oblique ligament of the thumb. orthopaedic Reviews 2012; 4:e23. ↩