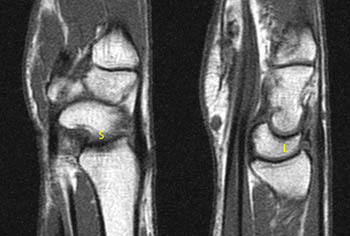
Clinical History: Each of two patients presents with wrist pain. What are the findings in relation to the scapholunate ligament? Which patient has the more significant abnormality?
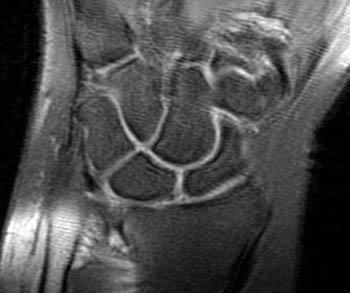
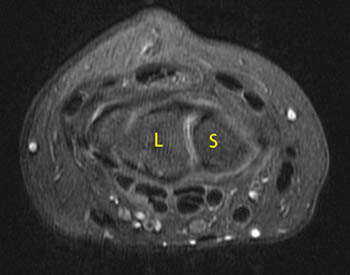
Patient 1.
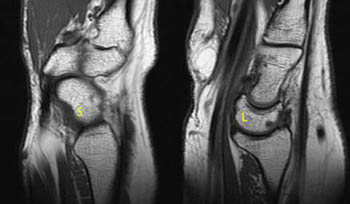
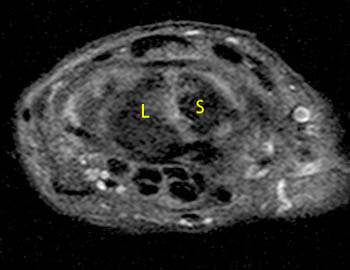
Patient 2.
Findings
Patient 1.
1. Incomplete tear of the scapholunate ligament (SLL) sparing the dorsal component.
2. Essentially normal carpal alignment.
Patient 2.
1. Tear of the scapholunate ligament involving central and dorsal components.
2. DISI deformity.
The involvement of the dorsal component of the SLL and associated instability pattern in patient 2 indicates a more significant injury.
Discussion
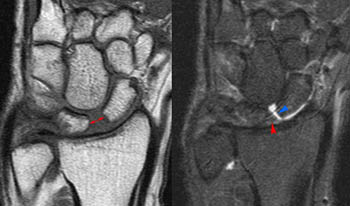
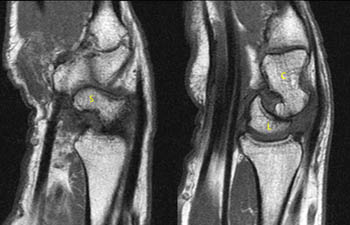
Each of the patients presented has a tear in the central portion of the scapholunate ligament visible on the coronal images, without diastasis (3a,3b).
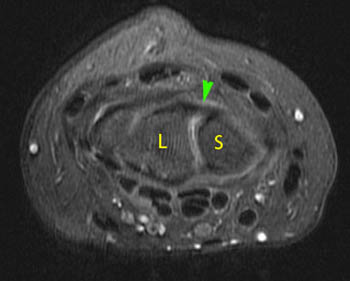
Patient 1 has an intact dorsal component, well seen on the axial image. Patient 2 has indistinct intermediate signal in the expected position of the dorsal component of the scapholunate ligament (4a,5a).
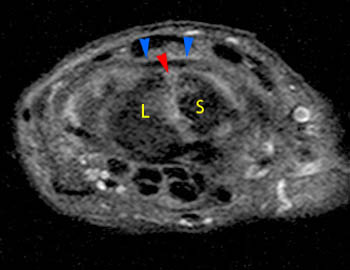
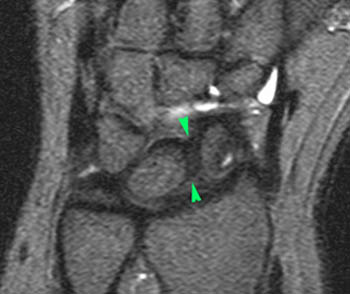
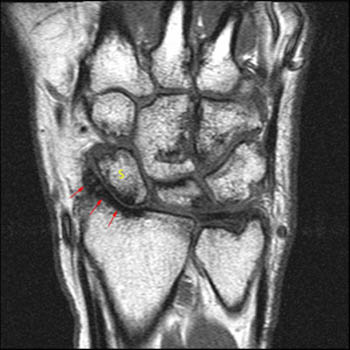
Figure 5:
Patient 2. The dorsal component of scapholunate ligament is not visible at its expected position (red arrowhead) and is either torn or degenerated. Dorsal to this site, an extrinsic capsular ligament, the dorsal intercarpal ligament (blue arrowheads) should not be mistaken for the scapholunate ligament.
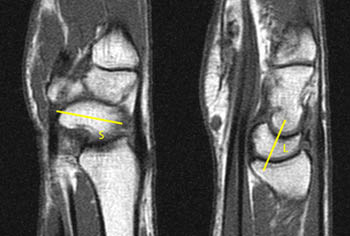
Both patients have mild dorsal tilt of the lunate. However, Patient 1 has accompanying mild dorsal tilt of the scaphoid relative to its normal position, keeping an essentially normal position relative to the lunate. This appearance is often seen with mild ulnar deviated positioning of the wrist. Patient 2 has a volar scaphoid tilt away from the tilt of the lunate. This indicates scapholunate dissociation, DISI deformity, and a functionally significant underlying scapholunate ligament injury (6a,7a).
Anatomy and MRI Assessment of the Scapholunate Ligament
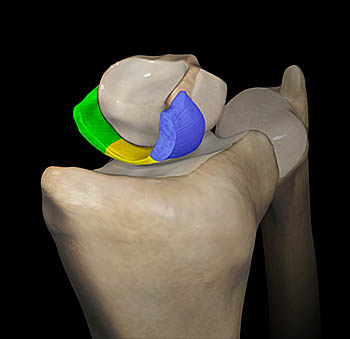
The scapholunate ligament (SLL) is an intrinsic intercarpal ligament that is U-shaped in the sagittal plane. It has three distinct components, dorsal, volar, and proximal1. These form the back and front walls and the floor of an “open box” configuration (8a).
Tears of the ligament may be complete (extending through all three components of the ligament) or incomplete (sparing at least one component, sometimes referred to as partial). They may also be full-thickness or extend only partially through the ligament. The proximal component (also known as central or membranous) is mainly comprised of fibrocartilage, with a few overlying longitudinally oriented collagen fibers. It usually has a triangular appearance on coronal images, extending distally into the joint space similar to a knee meniscus. Incomplete tears or degenerative perforations limited to the proximal component are frequently asymptomatic and are common, reaching nearly 50% prevalence by the 8th decade of life2,3. Degenerative tears involve the weaker scaphoid end of the proximal component. Traumatic tears also usually begin at this site4. The weak volar component of the SLL is comprised of thin obliquely oriented fibers. The dorsal component of the SLL is thickest and most functionally important. Tears of the SLL that involve the dorsal component more closely correlate with symptoms and are typically traumatic rather than degenerative in nature4. This is most often from a fall on the outstretched hand, with the thenar eminence striking the ground first.
The most obvious sign of a significant SLL tear is found on radiographs as a widened scapholunate interval (Terry-Thomas sign). This is also obvious on MRI (9a).
Figure 9:
Scapholunate diastasis on MRI (equivalent to the radiographic Terry-Thomas sign). The osseous diastasis (red double arrow) is more apparent on the T1 sequence. Low signal intensity marrow and some motion artifact on the fat-suppressed sequence limit discrimination between the bone and the adjacent ligament (red arrowhead). The SLL is torn at the scaphoid attachment and fluid (blue arrow) is well seen on the fat-suppressed image in the gap created by the diastasis. This patient's sagittal images demonstrated DISI deformity as well (not shown).
Studies have shown that for diastasis to occur, extrinsic ligament injury must be present in addition to a functionally complete SLL tear5. The corollary to this is that significant SLL tears can be present without extrinsic ligament injury or diastasis. Studies have confirmed the role of the scapholunate ligament (SLL) as the primary stabilizer of the scaphoid and lunate, with the surrounding volar and dorsal extrinsic wrist ligaments playing secondary roles6,7.
When evaluating the SLL on MRI, it is important to recognize that the most obvious component is not the most functionally significant. On coronal imaging sequences, the proximal component of the SLL is visible on multiple adjacent images due to its anatomic orientation perpendicular to the image slices. Meanwhile, the in-plane orientation of the functionally more important dorsal component usually makes it visible on only a single coronal image slice near the dorsal margin of the bones (10a).
As demonstrated earlier in our case example, a normal dorsal SLL component can be well seen on axial images (4a). A normal dorsal component identified in either plane assures us that a clinically significant tear is unlikely. If an intact dorsal component is not clearly identified on either axial or coronal images, it may be disrupted or it may be altered in signal from degeneration. Assessment of carpal instability patterns is particularly important in this situation.
Wrist Dynamics and Instability
As indirect signs of significant injury, instability patterns are very helpful in detecting or confirming clinically significant ligamentous injuries.
The proximal carpal row is considered an “intercalated segment” because it is positioned between the radius and the distal carpal row and no tendons attach to it. The lunate is positioned centrally in the proximal carpal row between the scaphoid and the triquetrum, which each have opposing volarflexion and dorsiflexion tendencies. If the lunate’s connection to the scaphoid is functionally disrupted, the bones become dissociated. The unopposed scaphoid follows its natural tendency to volarflex (rotatory subluxation), and the triquetrum pulls the lunate into dorsiflexion. This is the DISI (Dorsal Intercalated Segmental Instability) pattern (11a). A tear of the lunotriquetral ligament produces the opposite pattern, VISI (Volar Intercalated Segmental Instability), since the lunate is freed from the triquetrum and pulled volar by the scaphoid.
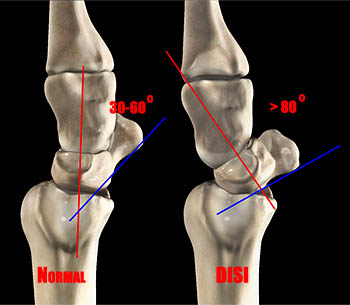
DISI may be recognized by assessment of sagittal MR images, but needs to be distinguished from the normal dorsal tilt of the lunate that can occur with normal ulnar deviated or hyperextended wrist positions. In a normal wrist, the lateral scapholunate angle is between 30o and 60o. A measurement over 80o indicates definite dorsiflexion instability. This angle can be calculated on MRI by adding the dorsal tilt angle of the lunate and the volar tilt angle of the scaphoid relative to vertical.
While DISI is an indicator of a significant SLL tear, DISI may develop with a completely intact SLL in the case of an unstable scaphoid waist fracture. The fracture may disrupt the normal dynamic linkage of the proximal carpal row by allowing the distal pole of the scaphoid to displace proximal and volar while the proximal pole remains attached and tilting dorsally with the lunate (Fig. 12a).
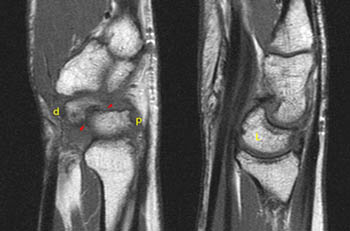
Figure 12:
Unstable fracture of the scaphoid causing DISI. Sagittal images show the scaphoid waist fracture (red arrows) with volar and proximal displacement of the distal pole (d), with the proximal pole (p) remaining normal or mildly dorsally tilted. Dorsal tilt of the lunate (L) is seen on the second image.
If DISI is long standing, it may progress to osteoarthritis of the radioscaphoid joint and a pattern known as SLAC (Scapholunate Advanced Collapse). The degenerative changes begin at the radial styloid, progress throughout the entire scaphoid fossa, and are followed by degenerative changes of the capitolunate joint (13a,13b) and proximal migration of the capitate. The radiolunate joint remains uninvolved until late in the process. If DISI is from scaphoid fracture nonunion, this may lead to SNAC (Scaphoid Nonunion Advanced Collapse), with similar features. Secondary problems such as carpal tunnel syndrome may develop.
Figure 13:
SLAC wrist. Degenerative changes including subchondral sclerosis and remodeling involve the entire radioscaphoid articulation (red arrows). Degenerative changes and subluxation at the capitolunate joint indicate an advanced stage. DISI deformity is evident on the sagittal images with dorsal tilt of the lunate and volar rotary subluxation of the scaphoid.
Treatment
Acute or subacute tears of the scapholunate ligament may be repaired surgically with suture anchors and temporary K-wire fixation. If the dorsal capsule attachment to the ligament is torn or the dorsal radiocarpal ligament is detached from the lunate, these are reattached.
Asymptomatic or mildly symptomatic SLAC with good grip strength may be treated nonoperatively with splinting, activity modification, NSAIDs, and/or steroid injections. More symptomatic cases may be treated surgically, involving carpal fusion with radial styloid resection, proximal row carpectomy, or scaphoid excision with four-corner arthrodesis.
Conclusion
A defect in the SLL may be small and insignificant or a lesion that causes significant instability, pain, and chronic disability. MRI is well suited in the assessment of scapholunate ligament tears, allowing sensitive detection and detailed assessment. Knowledge of the anatomy, dynamic function, and instability patterns is central to evaluating these lesions. Accurate assessment of these injuries is important for determining the best conservative or surgical approach to the injured patient.
References
1 Berger RA. The gross and histologic anatomy of the scapholunate interosseous ligament. J Hand Surg [Am]. 1996 Mar;21(2):170-8.
2 Lee DH, Dickson KF, Bradley EL. The incidence of wrist interosseous ligament and triangular fibrocartilage articular disc disruptions: a cadaveric study. J Hand Surg [Am]. 2004 Jul;29(4):676-84.
3 Wright TW, Del Charco M, Wheeler D. Incidence of ligament lesions and associated degenerative changes in the elderly wrist. J Hand Surg [Am]. 1994 Mar;19(2):313-8.
4 Linkous MD, Pierce SD, Gilula LA. Scapholunate Ligamentous Communicating Defects in Symptomatic and Asymptomatic Wrists: Characteristics. Radiology. 2000 Sep;216(3):846-50.
5 Elsaidi GA, Ruch DS, Kuzma GR, and Smith BP. Dorsal wrist ligament insertions stabilize the scapholunate interval: cadaver study. Clinical Orthopaedics and Related Research(425):152-7, 2004 Aug.
6 Short WH, Werner FW, Green JK, Masaoka S. Biomechanical evaluation of the ligamentous stabilizers of the scaphoid and lunate: Part II. J Hand Surg [Am]. 2005 Jan;30(1):24-34.
7 Short WH, Werner FW, Green JK, Masaoka S. Biomechanical evaluation of the ligamentous stabilizers of the scaphoid and lunate: Part III. J Hand Surg [Am]. 2007 Mar;32(3):297-309.
8 Green DP, Hotchkiss RN, Pederson WC, Wolfe SW, eds. Green’s operative hand surgery, 5th ed. Philadelphia, PA: Churchill Livingstone, 2005.
9 Kuo CE, Wolfe SW. Scapholunate instability: current concepts in diagnosis and management. J Hand Surg [Am]. 2008 Jul-Aug;33(6):998-1013.