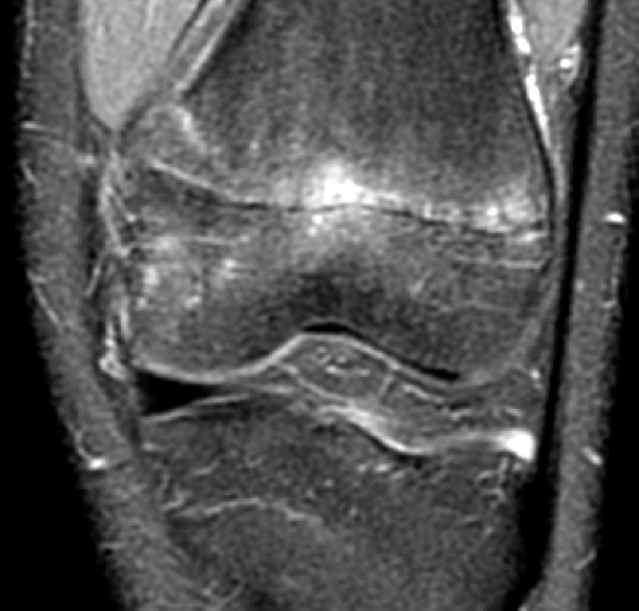
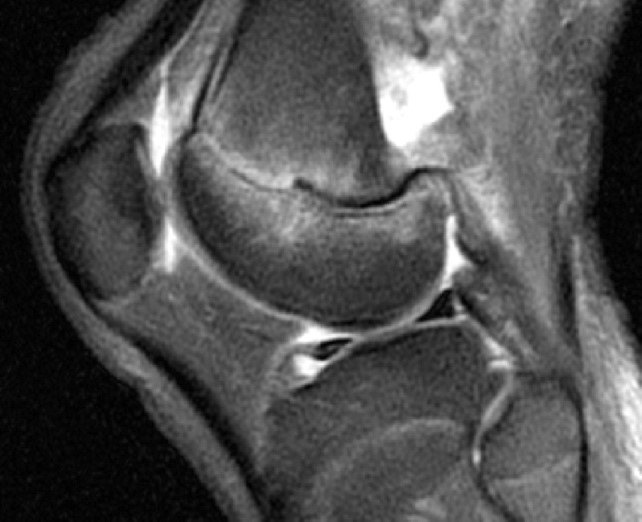
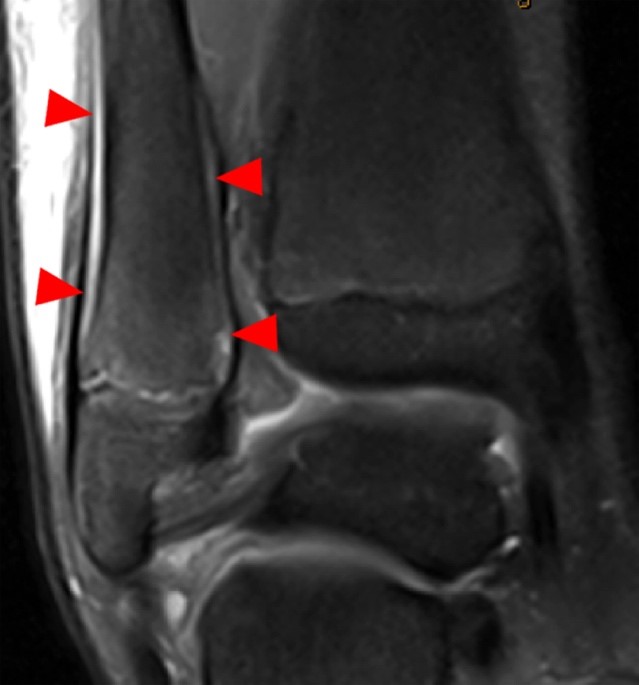
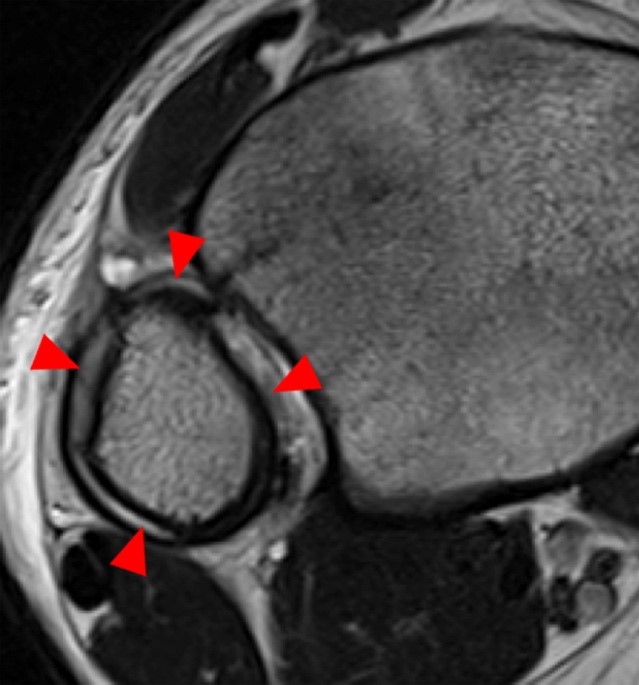
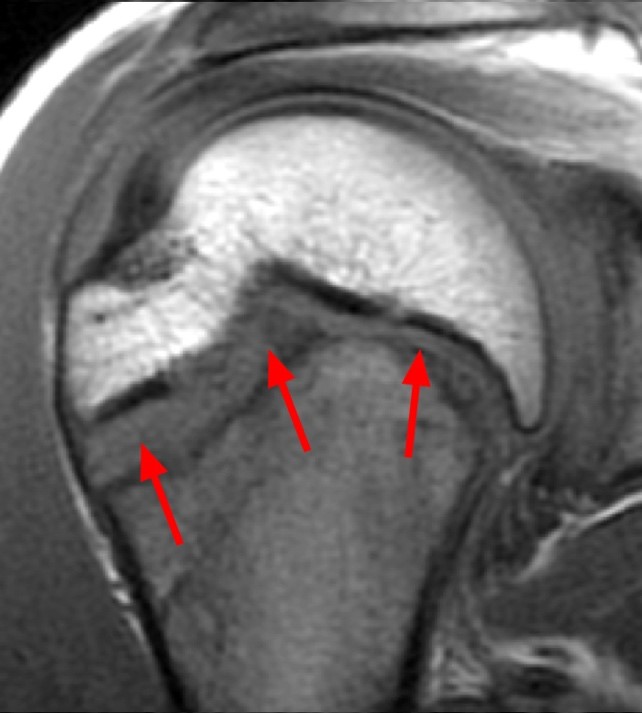
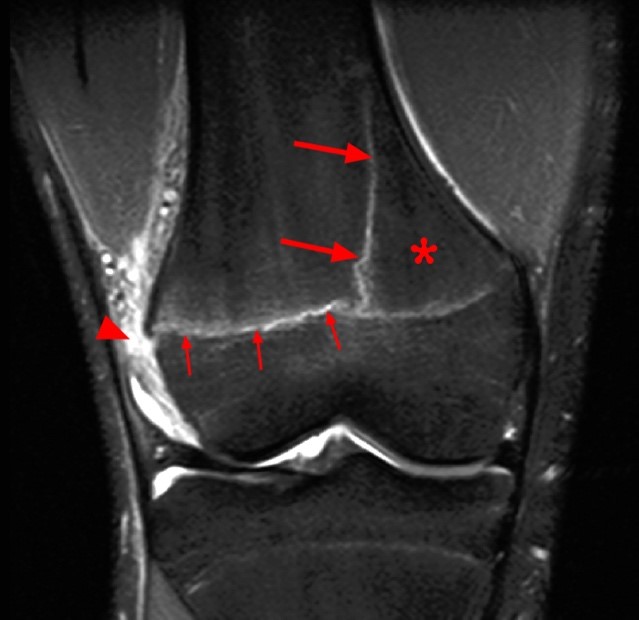
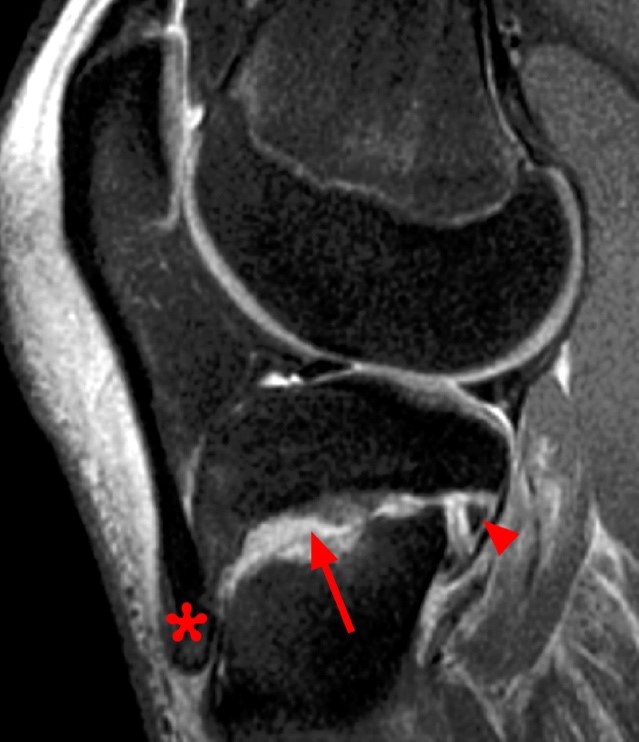
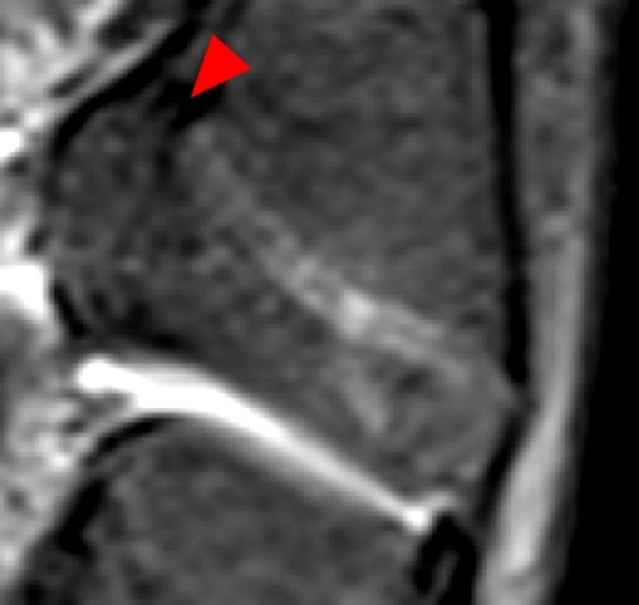
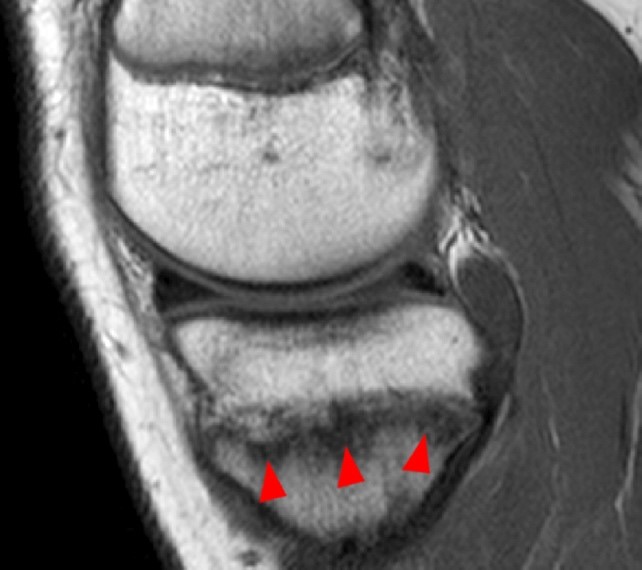
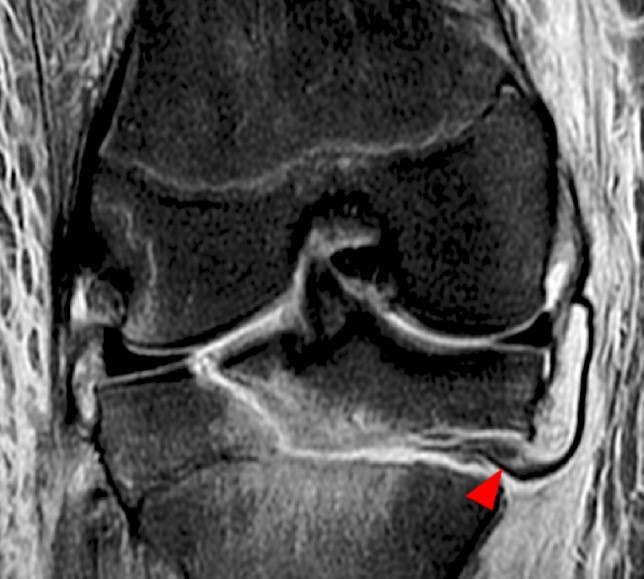
Clinical History: A 15 year-old male was injured 11 days ago performing a long jump. Coronal (1A) and sagittal (1B) fat-suppressed proton density-weighted images are provided. What are the findings? What is your diagnosis?
Findings
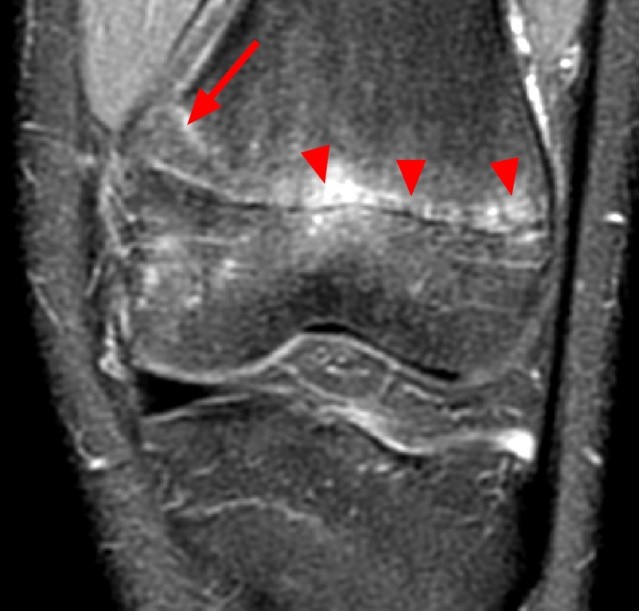
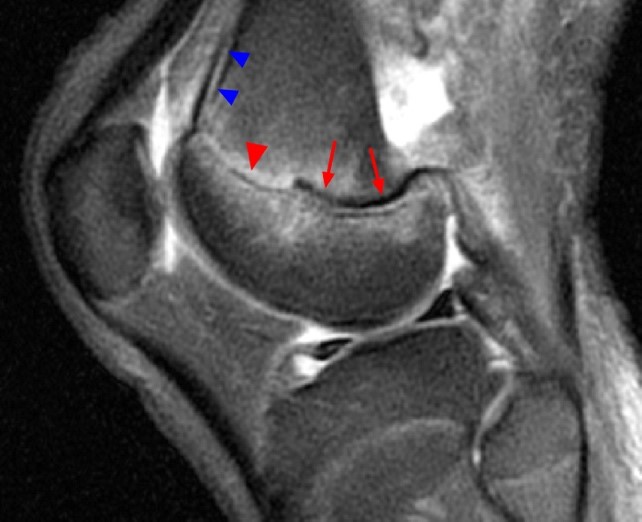
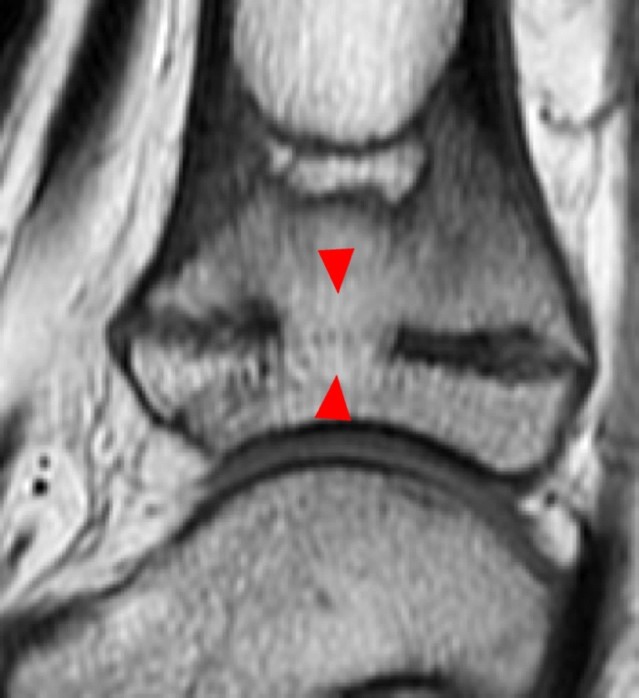
Figure 2:
Coronal (2A) and sagittal (2B) fat-suppressed proton density-weighted images of the knee reveal high signal intensity at the mid to lateral growth plate (arrowheads) with a triangular fracture of the medial metaphysis (arrow), indicating a Salter-Harris type 2 fracture. The periosteum has been stripped from the metaphysis of the lateral femur (blue arrowheads). Posteriorly the periosteum is torn and displaced into the fracture at the growth plate (small arrows).
Diagnosis
Salter-Harris 2 fracture of the distal femur with trapped periosteum.
Introduction
Injuries to the extremities of children frequently involve the physis, partially because the ligaments and joint capsule can be 5 times stronger than the growth plate.1 About 15% of fractures of children involve the growth plate. These physeal injuries were first described by a French surgeon named Foucher in 1860. Multiple classification systems followed, leading to the Salter and Harris system in 1963 which was based on radiographic appearance and the prognosis for growth disturbance.2,3
The Salter-Harris system was expanded and modified by Ogden in 1981 to account for more complicated combination injuries as well as injury to other growth mechanisms including the metaphysis, diaphysis, periosteum, zone of Ranvier and epiphyseal perichondrium.3 The mechanism of injury is shearing or avulsive in about 80% of cases and splitting or compressive in the rest.1 The growth plate is made of several layers. The layer closest to the epiphysis is the resting/germinal layer which is responsible for bone lengthening. The next layer is the proliferative layer, followed by the hyperplasia and degenerative layer, which is the weakest. This is followed by the vascular invasion and calcifying layers.1
Type 1 (figs 3-5):
The Salter-Harris 1 (SH 1) fracture extends through the growth plate, leaving the resting and dividing cell layers attached to the epiphysis. The fracture is not always perfectly transverse but can undulate so that microscopic involvement of the metaphysis can occur. This is more common as the child ages. A larger ossification center increases the likelihood of metaphyseal involvement. Displacement is frequently prevented by an intact periosteal attachment into the zone of Ranvier, the region responsible for peripheral growth of the physis.3 Type 1 injuries are more common in patients under the age of 5 with the exception of the proximal humerus where the peak age is 10-12 (little league shoulder)(fig 5). Apophyseal injuries are a form of Type 1 injury.1 Subclass 1B occurs in children with systemic disorders affecting endochondral ossification in the metaphysis (myeloproliferative, thalassemia or neuromuscular sensory disorders) so that the fracture passes through the zones of degenerating cartilage and primary spongiosa.
Subsequent growth is generally normal in types 1A and B, as the germinal layer responsible for epiphyseal growth remain intact. An exception can occur in the proximal femur if the major blood supply to the epiphysis is disrupted which can lead to osteonecrosis, premature physeal closure and severe growth deformity.
Subclass 1C has associated injury to the germinal portion of the physis and is most likely at birth or in early infancy. This can cause formation of an osseous bridge after growth of the secondary center reaches the damaged area.3
Salter-Harris Type 2: (figures 6 and 7):
Type 2 is the most common variety of Salter-Harris fractures. It is frequent from ages 3-7 and is the most common type over the age of 10. It is similar to the type 1 but with a variably sized metaphyseal fragment. There is a compressive and a distractive side. The compressive forces redirect from the horizontal into the metaphysis, creating the metaphyseal fracture fragment (Thurston Holland fragment). The periosteum usually remains intact on the compressive side but is disrupted on the tension side. Periosteal tears occur at the metaphyseal attachment where it is more loosely attached. This torn periosteum can invaginate in the physeal gap and prevent healing.3 This may be due to the periosteum’s propensity to produce bone rather than cartilage.4
Growth is otherwise usually not disturbed because the germinal layers remain attached to the epiphysis and circulation is maintained. Undulation of the physis can cause focal areas of more severe injury.3 Subclass 2B adds a free metaphyseal fragment on the tensile side, opposite the usual compressive side fragment and may require open reduction. Subclass 2C has a thin layer of metaphysis involved rather than the typical triangular fragment. This subclass is more common in slower growing sites such as the phalanges.3
Localized compression of the metaphysis into the physis can occur, especially in the distal femur and tibia, and can cause angular deformity.3 SH 2 fractures of the distal femur are associated with a high ( nearly 50%) risk of complications, particularly premature fusion. Entrapped periosteum is one cause. Other risk factors for premature fusion are high energy trauma, undulating growth plates and greater degrees of displacement. About 40% of the length of the lower extremity is due to growth at the distal femur.4
Salter Harris Type 3:
The SH type 3 fracture is essentially a type 1 fracture with an additional epiphyseal fracture. This frequently occurs at a time of partial fusion of the growth plate and is common in the distal tibia (Tillaux fracture).1,3 (figures 8 and 9)
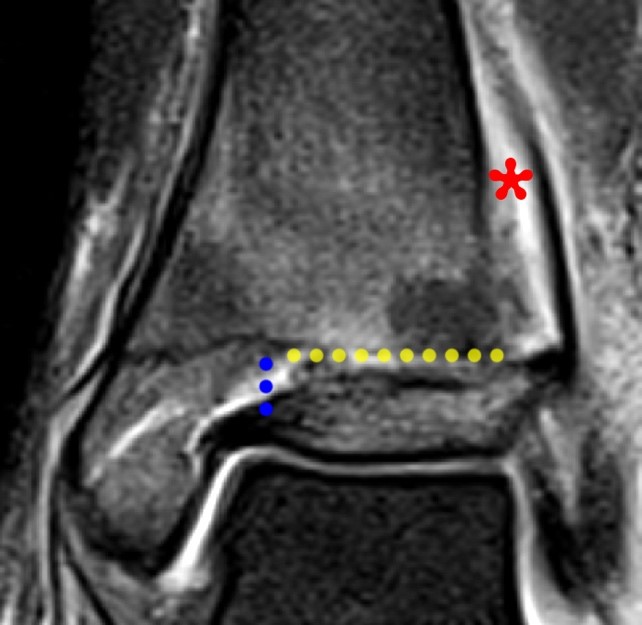
Figure 8:
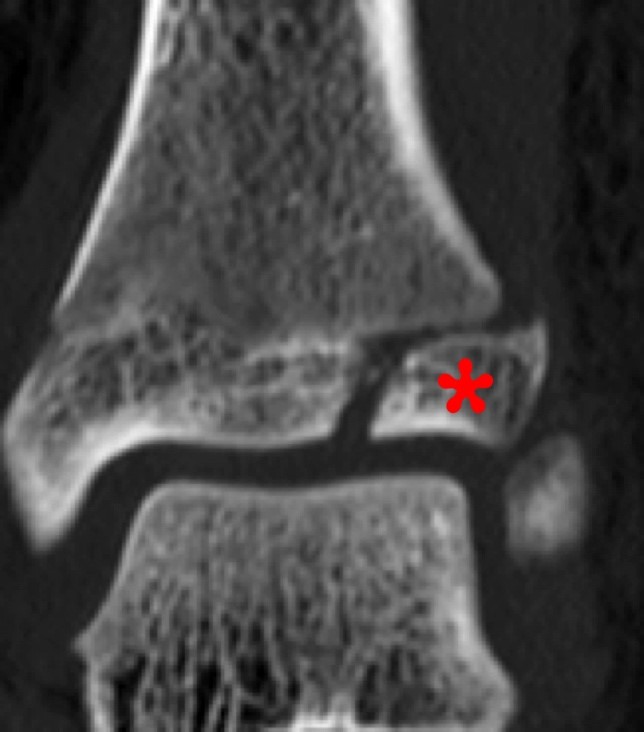
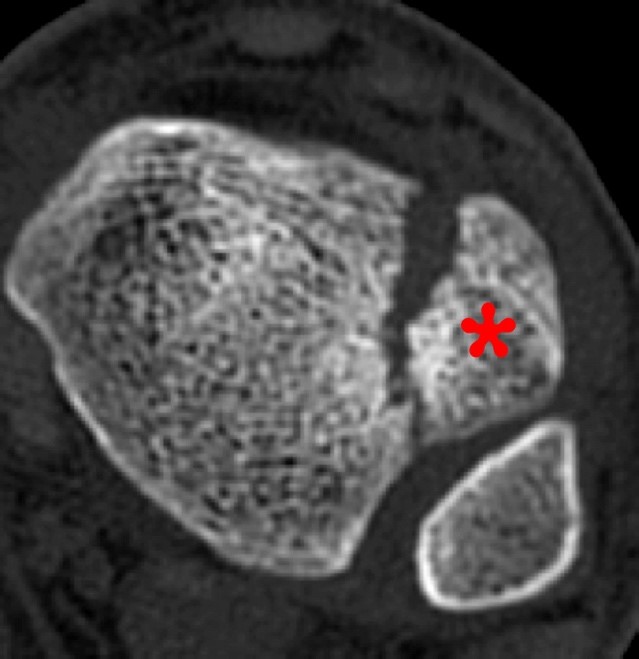
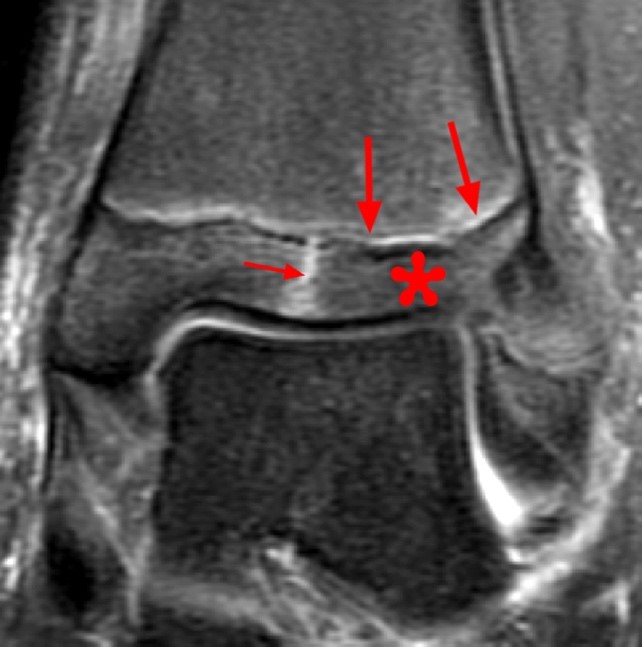
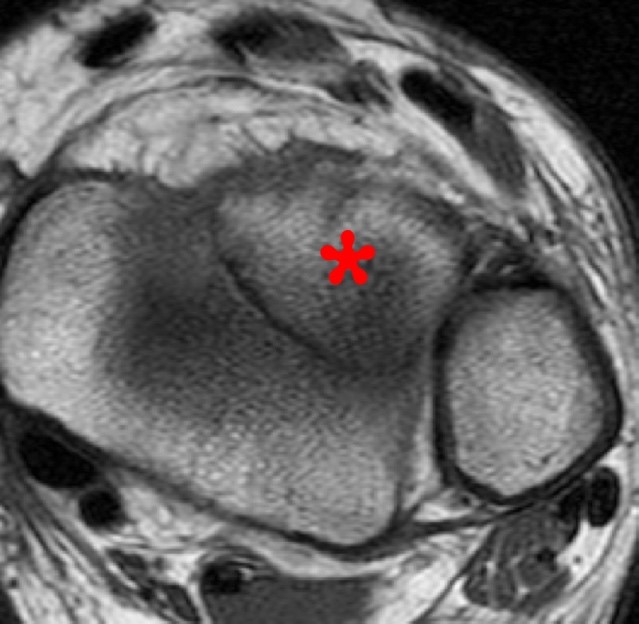
Coronal and axial CT and MR images of the ankle (different patients) demonstrate a Tillaux fracture with a sagittally oriented fracture through the epiphysis of the distal tibia (small arrow) and the axial fracture through the growth plate (large arrows). The displaced epiphyseal component (asterisk) is readily apparent. The coronal CT image demonstrates the fusing growth plate which is typical for this fracture.
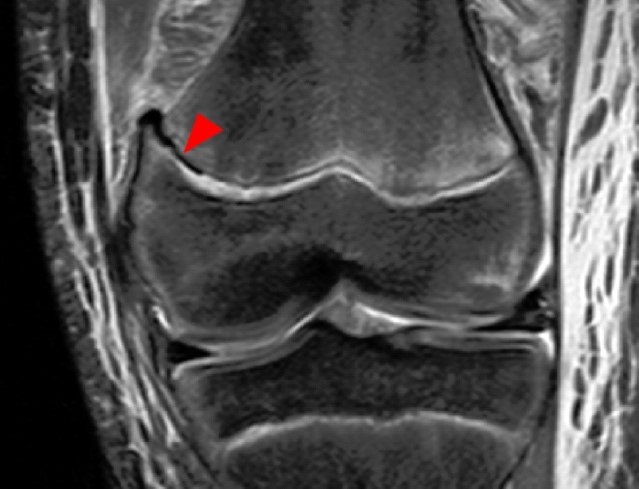
Figure 9:
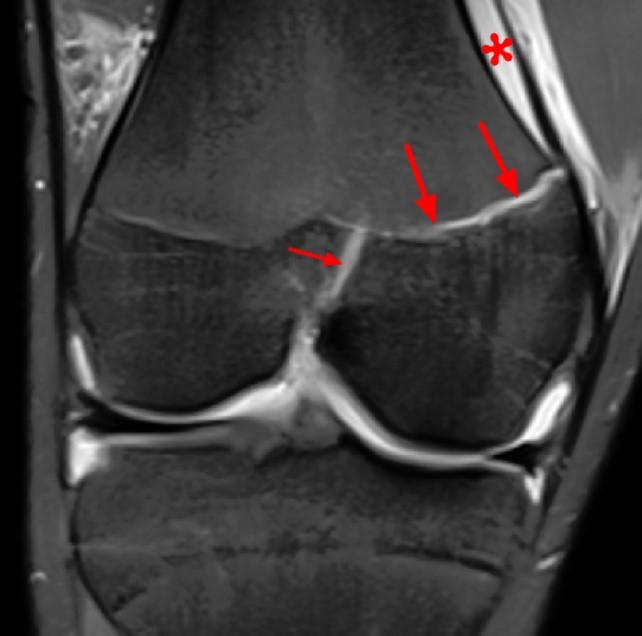
Coronal fluid-sensitive MR image of the knee shows a SH 3 fracture with a sagittal fracture of the epiphysis (small arrow) and axial fracture of the growth plate (larger arrows). Mild angulation results in incongruity of the articular surface. The periosteum is elevated by hematoma (red asterisk).
Salter-Harris Type 4:
SH 4 is a longitudinal fracture extending through the epiphysis, physis and metaphysis. It is commonly seen in the medial and lateral condyles and epicondyles of the distal humerus and in the medial malleolus. Displacement can be caused by the original injury and by muscle pull. Local physeal fusion can occur despite anatomic reduction due to compression injury to the growth plate.3
The triplane fracture of the distal tibia is an example of a SH 4 injury. (figure 10)
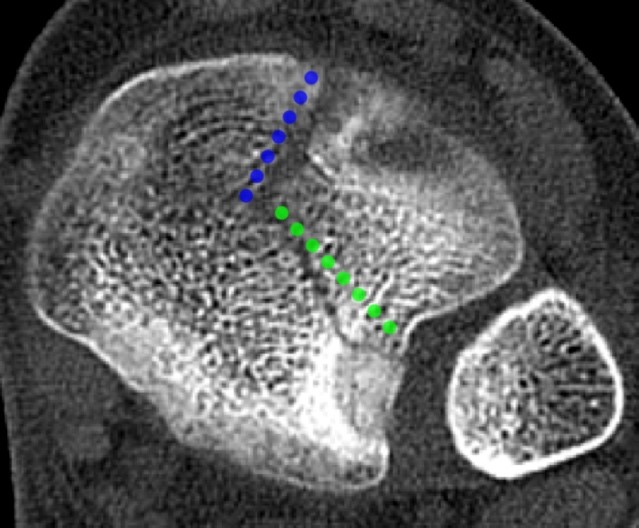
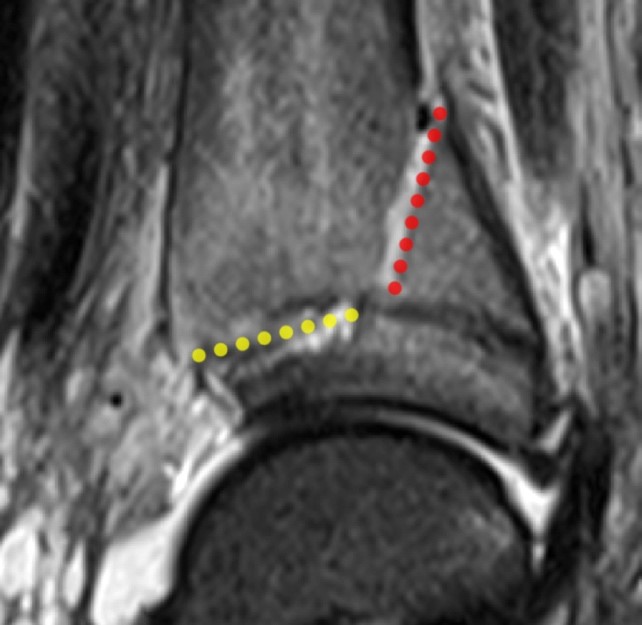
Figure 10:
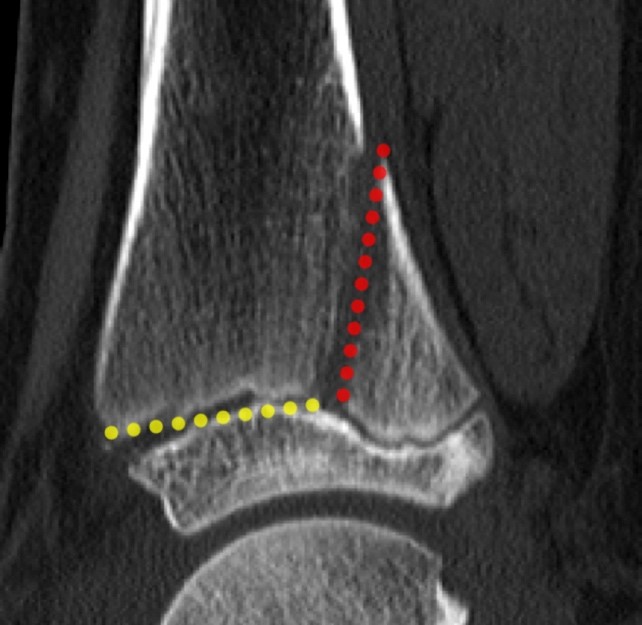
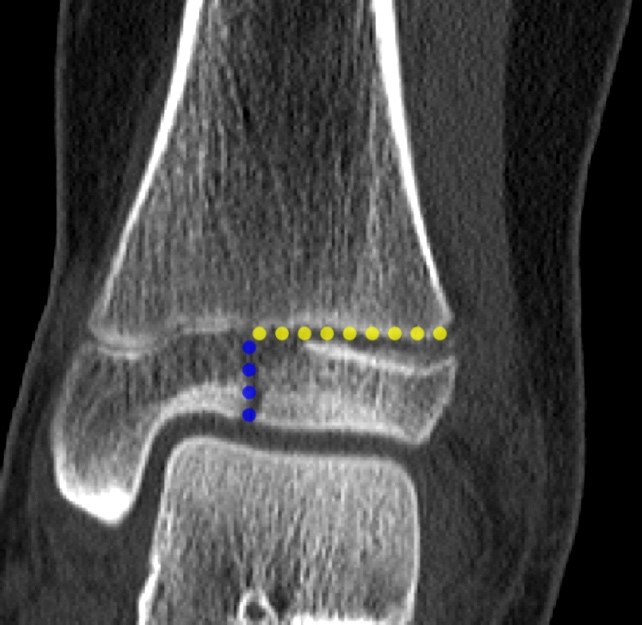
Sagittal, coronal and axial CT (10 A, B and C) and coronal and sagittal MR (10 D and E) images of the ankle demonstrate a SH 4 fracture of the triplane type. A coronal fracture extends through the posterior metaphysis of the distal tibia (red line) with a horizontal fracture through the lateral growth plate (yellow line) and a sagittal fracture through the epiphysis (blue line). Subperiosteal hemorrhage is present (red asterisk).
Subclass 4B has an additional fracture across the physis and is more common near skeletal maturity. Subclass 4C is in a non-articular location such as the femoral neck. Subclass 4D has multiple fragments.3
Additional Salter-Harris Fractures:
Type 5 is a pure compression injury and is rare. The prognosis is poor and there is almost always premature fusion which can occur several years after the initial injury. In addition to physical trauma, these occur with thermal, frostbite, electrical and radiation trauma.1,3
Type 6 injuries are very rare and involve the peripheral growth plate in the zone of Ranvier, usually from focal contusion or avulsion. Peripheral osseous bridging frequently occurs, resulting in an angular deformity.1,3 This may also be a mechanism for osteochondroma formation.3
Type 7 is a completely intraepiphyseal fracture without involvement of the growth plate, such as osteochondritis dissecans.3
Type 8 is an injury to the blood supply of the metaphysis.3
Type 9 is a selective injury to the diaphyseal periosteum which affects the ability of the bone to remodel and grow circumferentially.3
Utility of MRI
MRI provides the most sensitive detection of radiographically occult fractures and proper diagnosis can alter staging and management.5,6 This is particularly true in the pediatric elbow which is difficult to evaluate radiographically man H and Eustace S. MRI of pediatric growth plate injury: correlation with plain film radiographs and clinical outcome. Skeletal Rbecause of the multiple ossification centers, many of which do not ossify until 11-12 years of age. The elbow is the site of the most frequent epiphyseal fractures after the distal radius and distal tibia. These fractures tend to be unstable and frequently require surgical fixation.6
Complications of growth plate injuries mainly involve growth disturbance. (figures 11, 12 and 13) Growth abnormalities are more associated with vertical interruptions of the growth plate than horizontal fractures.7
Treatment
Treatment options for growth arrest include physeal bar resection, epiphysiodesis, chondrodiastasis and limb lengthening and deformity correction.
Physeal bar resection is indicated if at least 2 years of growth is remaining and 25-40% of physis is affected, as patient prognosis is good if less that 10% of the physis is involved and poor if greater than 25% is involved.8 The bar must be completely resected and material interposed (cement, cartilage or fat). A fibrous bridge across the physis can only be seen on MRI but is difficult to differentiate from a bony bridge. Either may need to be resected, however.7
Epiphysiodesis is used for a bony bar affecting greater than 50% of the physis.
Chondrodiastasis or physeal distraction uses external fixation and progressive lengthening after breaking the physeal bar and is controversial.8
Failure of healing can be caused by entrapment of adjacent soft tissues. This can be the periosteum, tendons, ligaments, muscles or neurovascular bundles.9 (fig 14 and 15)
Conclusion
Childhood fractures can frequently involve growth centers and are thus at risk for growth disturbances. Such fractures are commonly described using the Salter-Harris classification system. Most of the fractures will heal without complications but surgery may be needed to restore articular surface congruency or remove interposed soft tissue structures which could delay healing or cause premature fusion. In cases, where growth plate disturbances arise, MR provides critical guidance in the detection of disturbances and in the evaluation of the severity of growth arrest.

References
- Ozonoff MB. Pediatric orthopaedic Radiology 2nd edition. W.B. Saunders Company. ↩
- Salter RB, Harris WR. Injuries involving the epiphyseal plate. JBJS 1963; 45: 587-622. ↩
- Ogden JA. Injury to the growth mechanisms of the immature skeleton. Skeletal Radiology 1981; 6, 237-253. ↩
- Chen J, Abel MF, Fox MG. Imaging appearance of entrapped periosteum within a distal femoral Salter-Harris II fracture. Skeltal Radiology 2015; 44: 1547-1551. ↩
- Carey J, Spence L, Blickadiology 1998; 27, 250-255. ↩
- Beltran J, Rosenberg ZS, Kawelblum M, Montes L, Bergman AG, Strongwater A. Pediatric elbow fractures: MRI evaluation. Skeletal Radiology 1994; 23: 277-281. ↩
- Jaramillo D, Hoffer FA, Shapiro F and Rand F. MR imaging of fractures of the growth plate. AJR Dec 1990; 155: 1261-1265. Growth arrest occurs in 5-10% of physeal fractures. ↩
- Dabash S, Prabhakar G, Potter E, Thabet AM, Abdelgawad A, Heinrich S. Management of growth arrest: Current practice and future directions. Journal of Clinical Orthopaedics and Trauma 20178; https://doi.org/10.1016/j.jcot.2018.01.001 ↩
- Whan A, Breidahl W and Janes G. MRI of trapped periosteum in a proximal tibial physeal injury of a pediatric patient. AJR Nov 2003; 181: 1397-1399. ↩