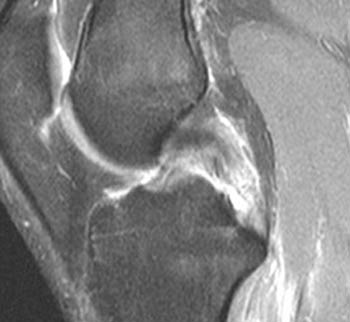
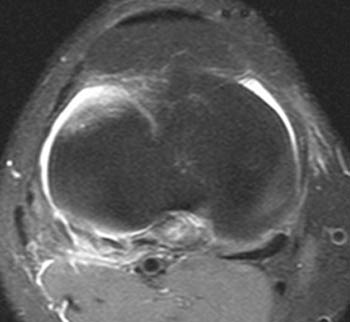
Clinical History: A 17 year-old female presents after falling on her knee while playing soccer. Sagittal (1a) and axial (1b) proton-density weighted fat-suppressed images are provided. What are the findings” What is your diagnosis?
Findings
Figure 2:
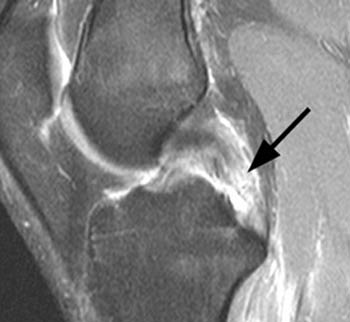
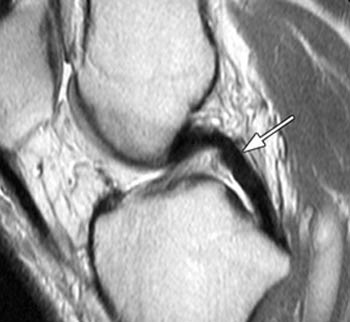
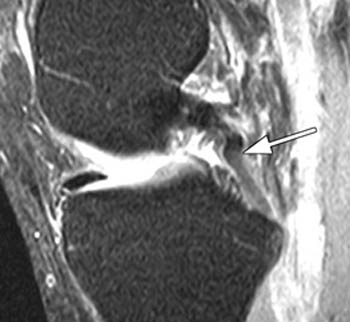
In (2a), a fat-suppressed proton-density sagittal image, the mid-substance posterior cruciate ligament fibers are ill-defined and discontinuous (arrow).
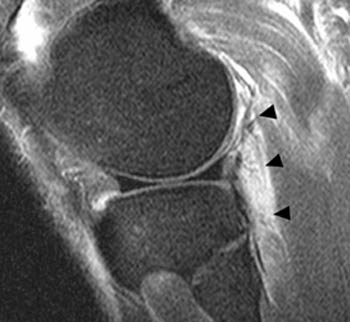
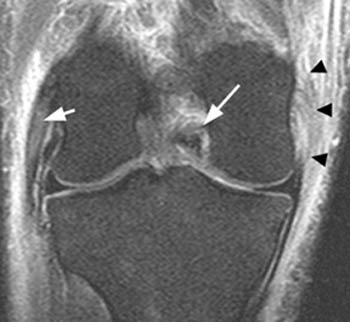
(2b) A fat-suppressed proton-density axial image demonstrates edema within the popliteus muscle (arrowhead). The posterior cruciate ligament is ill-defined and edematous (arrow).
Diagnosis
Mid-substance posterior cruciate ligament rupture and popliteus muscle partial tear.
Introduction
Posterior cruciate ligament (PCL) injuries account for up to 23% of all knee ligament injuries in the general population and are most commonly seen as a result of motor vehicle accidents and sports-related injuries. The anatomic and biomechanical roles of the PCL have been less investigated and are less well understood than those of the anterior cruciate ligament (ACL). Not surprisingly, the clinical outcomes of PCL injuries treated either conservatively or by surgery are poorer than those for the ACL. The appropriate surgical treatment of PCL injuries is controversial. Isolated injuries have traditionally been treated nonoperatively.1 However studies have shown an increased incidence of instability and arthritis in such patients due to altered biomechanics.2,3 Unfortunately, the outcome of surgery for isolated PCL injuries has been relatively disappointing, with a high number of patients experiencing residual knee laxity and a suboptimal long-term prognosis. Recent advancements in the understanding of PCL function and the improved detection of PCL and coexisting injuries afforded by MRI have improved the orthopaedic surgeon’s ability to address the biomechanical deficits resulting from PCL injuries.4
Anatomy
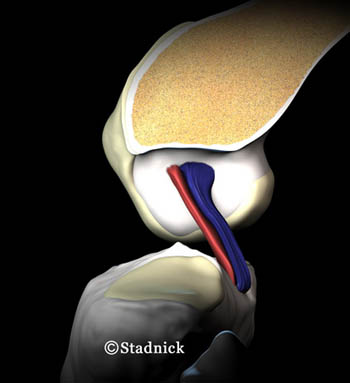
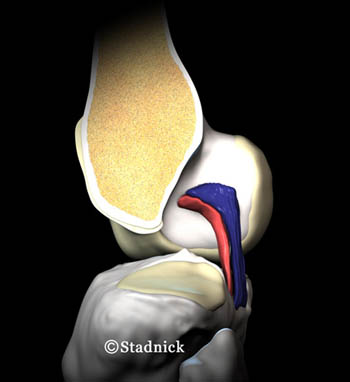
The PCL extends from the lateral surface of the medial femoral condyle to the posterior aspect of the tibia. It is an intraarticular but extrasynovial structure. The PCL is covered along its anterior, medial and lateral aspects by a sheath of synovium that is reflected from the posterior capsule, and its posterior aspect blends with the posterior capsule. The PCL is composed of two major components, most often referred to as the anterolateral (AL) and posteromedial (PM) bundles. The AL bundle is taut in passive flexion and the PM is taut in passive extension (3a,4a).5 The meniscofemoral ligaments (Humphrey and Wrisberg) are considered a part of the PCL complex. While the posterolateral corner structures are not considered part of the PCL complex, they work closely with the PCL to provide posterior knee stability (MRI Web Clinic 2003).
Biomechanics
The PCL is almost twice as strong as the ACL. The AL bundle is larger and stronger than the PM bundle. The primary function of the PCL is to restrain posterior tibial translation. The PCL and posterolateral corner act synergistically to prevent posterior tibial translation and to restrain external rotation of the tibia and varus angulation of the knee. The PCL provides more restraint to posterior tibial translation with the knee in flexion and the posterolateral corner more restraint with the knee in extension.
Mechanism of Injury
PCL injuries are most often combined with other ligamentous injuries. The most commonly associated injury is to the posterolateral corner, occurring in up to 60% of PCL injuries.6 Isolated injuries appear to be more common in sports-related injuries. Three mechanisms of PCL tear have been identified:
- A direct blow to the proximal anterior tibia in a flexed knee with forceful posterior displacement of the tibia usually results in a midsubstance tear, often with disruption of the posterior capsule. Dashboard injuries and falls on a hyperflexed knee are common examples of this mechanism of injury. Bone bruises occur at the site of impact between the anterior tibial plateau and the posterior femoral condyle.7 Because of the high-energy forces associated with motor vehicle accidents, dashboard injuries are usually combined with ligamentous, osteochondral, or meniscal injuries.
- Hyperextension injuries typically result in avulsion of the tibial attachment. Associated ACL rupture is common in this mechanism and when present should alert the clinician to the possibility of a transient knee dislocation and prompt a careful assessment of the popliteal neurovascular structures. Bone bruises are seen in the anterior portion of the tibial articular surface and in the anterior femoral condyles.7
- Severe abduction or adduction associated with rotational forces may rupture the cruciate ligaments after collateral ligament disruption.7
Physical and Arthroscopic Diagnosis
The detection of PCL tears by physical exam relies upon the examiner’s ability to identify abnormal posterior translation of the tibia relative to the femur by various maneuvers. The most sensitive and specific test to detect injury to the PCL is the posterior drawer test. However, physical examination is often inconclusive as to the presence of a PCL tear,8 as the findings may be limited by pain or quadriceps and hamstring spasm, particularly in the acute setting and with combined ligamentous injuries. Because PCL tears often accompany ACL tears, tibial laxity on physical exam may not be correctly attributed to a PCL tear. Importantly, arthroscopic detection of PCL tears may be difficult through an anterior approach, especially with an intact ACL.9 An intact meniscofemoral ligament of Humphrey can simulate an intact PCL at arthroscopy even with rupture of the PCL.10
MRI
The normal PCL is homogenously low in signal on T1 and T2-weighted sequences and demonstrates a smooth convex posterior curve (5a,6a,7a). The meniscofemoral ligaments of Humphrey and Wrisberg, when present, may be seen anterior and posterior to the PCL, respectively. MRI readily differentiates partial and complete PCL tears. Partial tears or degenerative changes of the PCL usually involve the central fibers of the PCL without loss of PCL continuity (8a). Complete PCL tears demonstrate focal interruption of the ligament fibers and alterations in PCL contour (2a,2b). In complete midsubstance tears with an intact synovial sheath, the PCL may maintain its shape with diffusely increased signal intensity. The location of the tear and the presence of avulsed bony fragment can be identified (9a). Because progressive functional instability and arthritis often occur due to unrecognized posterolateral, posteromedial, or anterior instability, the structures in these regions should be carefully scrutinized for injury (10a,11a,12a).
Figure 6:
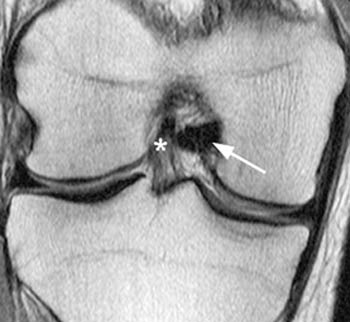
(6a) A coronal proton-density weighted image through the posterior intercondylar region demonstrates the posteromedial bundle attachment of the PCL (arrow) to the medial femoral condyle. The ligament of Wrisberg is also seen just superior to the PCL (small arrow). The ACL origin is depicted (asterisk).
Figure 9:
(9a) A sagittal T2 weighted image demonstrates a tibial avulsion fracture (arrow) at the PCL attachment. The tibial fracture fragment (arrowhead) is mildly elevated. Although mildly lax, the PCL demonstrates normal signal with no evidence for ligamentous injury. Hemarthrosis is demonstrated by layered blood in the anterior joint space (small arrows).
Figure 10:
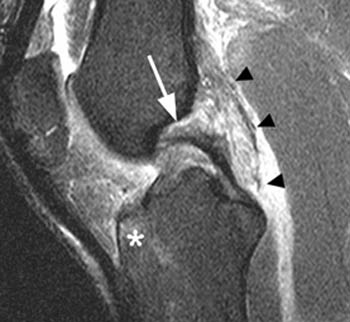
(10a) A sagittal fat-suppressed proton-density weighted image demonstrates a proximal tear of the PCL near the femoral attachment (arrow). Hemorrhage and edema associated with a posteriorly disrupted capsule (arrowheads) are demonstrated deep to the medial gastronemius muscle. An anterior tibial bone bruise is also depicted (asterisk).
Figure 12:
(12a) A coronal fat-suppressed proton-density weighted image of the same patient in (10a) and (11a) demonstrates abnormal hyperintensity at the PCL-bone interface (arrow). Edema within the fibular collateral ligament (short arrow) is compatible with a ligament sprain. Hemorrhage and edema are present along the posteromedial capsule and posterior oblique ligaments (arrowheads). The findings in (10a-12a) indicate a combined PCL injury with associated injury of the posterolateral corner.
MRI readily delineates injuries of bone, other ligaments, menisci, cartilage, capsule, tendons, and vascular structures. Indirect signs of PCL injury include bone bruises of the anterior tibia and posterior femoral condyles, indicating forced posterior displacement of the tibia with the knee flexed. Anterior tibial articular surface and anterior femoral condyle bone bruises are often seen with a hyperextension mechanism of injury. In chronic PCL tears, the PCL typically remains in continuity between the tibia and femur but the ligament caliber is attenuated or the contour is buckled (13a). A buckled or J-shaped PCL may also be seen with a normal PCL accompanying an ACL tear or in a hyperextended knee with normal ligaments.
Treatment
In the past the significance of PCL injuries has been understated, though studies have shown an increased incidence of arthritis in this patient population. Medial compartment and patellofemoral joint pressures increase significantly with PCL deficiency and are magnified with a coexisting posterolateral corner injury. Unfortunately previous PCL reconstruction techniques have been largely ineffective in restoring PCL function.2,3,4 Most authors agree with a conservative approach to isolated PCL injuries with less than 10mm posterior tibial translation at 90 degrees of flexion, or for asymptomatic chronic isolated PCL injuries. Close follow-up is recommended to identify unrecognized posterolateral instability and worsening functional instability. Surgical treatment is recommended for acute PCL injuries with insertional avulsions or PCL tears with greater than 10 mm of posterior tibial displacement, associated multiple ligament injuries, or associated meniscal or chondral injuries. Combined ACL-PCL injuries are assumed to be the result of a knee dislocation and neurovascular assessment is required. In patients with PCL and posterolateral corner injuries, surgical repair is indicated for both structures. Failure to correct the posterolateral corner instability results in an increased likelihood of PCL graft failure and a universally poor outcome.11 Surgical treatment is also recommended in chronic isolated PCL tears when the tear becomes symptomatic.
Single bundle tibial tunnel PCL reconstructions attempt to recreate the function of the AL bundle, however the results of this technique have been generally poor.3,4 As with the ACL, a better understanding of the anatomy and biomechanics of the PCL may allow better reconstruction techniques and functional outcomes. Tibial inlay graft techniques have the advantage of improved long-term stability over tibial tunnel techniques, by eliminating the stresses and attritional changes of the graft that commonly occur at the tibial tunnel.12 Double bundle PCL graft reconstructions have been shown to more closely restore normal knee motion patterns compared to single band (anterolateral band) reconstructions.13,14 However, the clinical advantages of this technique have not yet been documented with well-controlled prospective studies.
Conclusion
The approach to PCL injuries is complex and challenging. Following PCL disruption, both physical examination and arthroscopy have diagnostic limitations, and thus MRI plays a pivotal role in the assessment of PCL integrity. Historically, treatment of PCL tears was often conservative, though surgical reconstruction has gained in popularity as the understanding of the importance of the PCL in knee stability and the effects of PCL deficiency upon the development of osteoarthritis have grown. MRI frequently guides treatment decisions, as the identification of coexisting injuries to other ligaments and the posterolateral corner increases the likelihood of PCL reconstruction.
References
1 Shelbourne KD, Davis TJ, Patel DV. The Natural History of Acute, Isolated, Nonoperatively Treated Posterior Cruciate Ligament Injuries: A Prospective Study.
Am. J. Sports Med., May 1, 1999; 27(3): 276 – 283.
2 Logan M, Williams A, Lavelle J, Gedroyc W, Freeman M. The Effect of Posterior Cruciate Ligament Deficiency on Knee Kinematics. Am. J. Sports Med., December 1, 2004; 32(8): 1915 – 1922.
3 Gill TJ, DeFrate LE, Wang C, Carey CT, Zayontz S, Zarins B, Li G. The Effect of Posterior Cruciate Ligament Reconstruction on Patellofemoral Contact Pressures in the Knee Joint Under Simulated Muscle Loads. Am. J. Sports Med., January 1, 2004; 32(1): 109 – 115.
4 Gill TJ, DeFrate LE, Wang C, Carey CT, Zayontz S, Zarins B, Li G. The Biomechanical Effect of Posterior Cruciate Ligament Reconstruction on Knee Joint Function: Kinematic Response to Simulated Muscle Loads. Am. J. Sports Med., July 1, 2003; 31(4): 530 – 536.
5 Girgis FG, Marshall JL, Al Monajem ARS. The cruciate ligaments of the knee joint: anatomical, functional and experimental analysis. Clin Orthop 1975;106:216-231.
6 Fanelli GC, Edson CJ. Posterior cruciate ligament injuries in trauma patients: part II. Arthroscopy 1995;11:526-529.
7 Sonin AH, et al. Posterior Cruciate Ligament Injury: MR Imaging Diagnosis and Patterns of Injury. Radiology 1994;190:455-458.
8 Grover JS, Bassett LW, Gross ML, Seeger LL, Finerman CAM. Posterior cruciate ligament: MR imaging. Radiology 1990; 174:527-530.
9 Lysholm J, Gillquist J. Arthroscopic examination of the posterior cruciate ligament. J Bone Joint Surg [Am] 1981; 63:363-366.
10 Dehaven KE. Arthroscopy in the cruciate injured knee. In: Feagin JA Jr. ed. The crucial ligaments. New York, NY: Churchill, 1988; 334.
11 Fanelli GC. Arthroscopically Assisted Posterior Cruciate Ligament Reconstruction: Transtibial Tunnel Technique. In: Fanelli GC, ed. Posterior cruciate ligament injuries a practical guide to management. New York: Springer,2001:141-156.
12 Parker RD, et al. Arthroscopically Assisted Posterior Cruciate Ligament Reconstruction: Tibial Inlay Technique. In: Fanelli GC, ed. Posterior cruciate ligament injuries a practical guide to management. New York: Springer,2001:157-173.
13 Sekiya JK, Haemmerle MJ, Stabile KJ, Vogrin TM, Harner CD. Biomechanical Analysis of a Combined Double-Bundle Posterior Cruciate Ligament and Posterolateral Corner Reconstruction. Am. J. Sports Med., March 1, 2005; 33(3): 360 – 369.
14 Harner CD, et al. Biomechanical Analysis of a Double-Bundle Posterior Cruciate Ligament Reconstruction. Am. J. Sports Med., March 1, 2000; 28(2): 144 – 151.