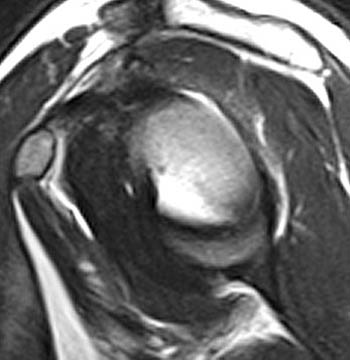
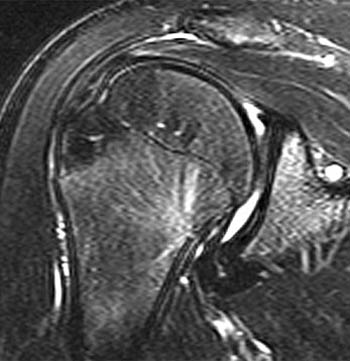
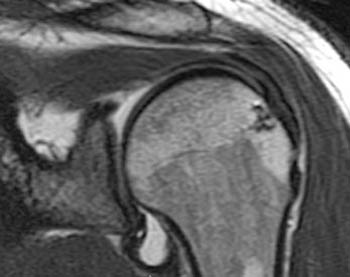
Clinical History: 54-year-old female with decreased range of motion and right shoulder pain increasing over the last 2 months. (1a) Sagittal T2-weighted and (1b) Coronal fat-suppressed T2-weighted images of the right shoulder are provided. What are the findings? What is your diagnosis?
Findings
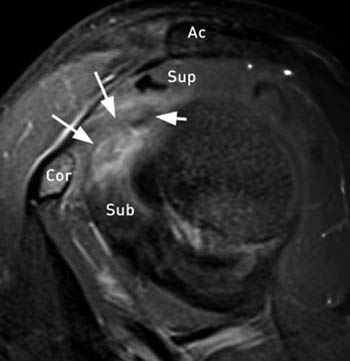
Figure 2:
(2a) The sagittal T2-weighted image demonstrates a thickened coracohumeral ligament (arrow) and soft tissue thickening in the rotator interval (arrowheads). The short arrow indicates the adjacent long head of the biceps tendon.
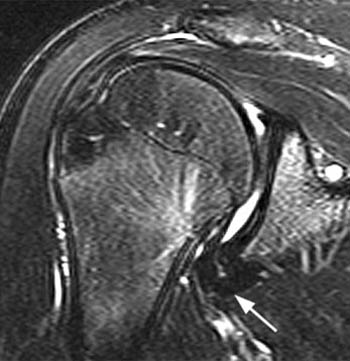
(2b) The coronal T2-weighted fat-suppressed image demonstrates an abnormally thickened inferior glenohumeral ligament (arrow).
Diagnosis
Adhesive Capsulitis
Discussion
Adhesive capsulitis or “frozen shoulder” is an inflammatory condition of the glenohumeral joint synovium and capsule leading to a restricted range of motion. It is most commonly encountered in female patients who are 40 to 60 years of age. Primary or idiopathic adhesive capsulitis is encountered in the absence of preceding trauma. Secondary adhesive capsulitis or post-traumatic arthritis results from antecedent injury, low-level repetitive trauma, surgery, or rheumatologic conditions. Although poorly understood, adhesive capsulitis is felt to begin as an inflammatory hypervascular synovitis, which prompts a progressive fibroblastic response in the adjacent capsule. Capsular thickening and contraction ensue.1 At arthroscopy, synovial inflammation or capsular thickening may be seen. The abnormalities most commonly involve the rotator interval capsule, the biceps tendon root, and the inferior and posterior capsule.
The clinical diagnosis of idiopathic adhesive capsulitis relies on the detection of a global decreased range of motion at the glenohumeral joint, absence of previous major trauma, and a normal joint space on plain radiographs.2 However, these diagnostic criteria are nonspecific, as the clinical features of rotator cuff pathology and impingement often mimic those of adhesive capsulitis.
MRI effectively demonstrates the rotator interval and the axillary recess, which are sites commonly affected by adhesive capsulitis. The rotator interval lies between the supraspinatus muscle and tendon posterosuperiorly and the subscapularis muscle and tendon anteroinferiorly. The rotator interval capsule is composed of the coracohumeral ligament and the superior glenohumeral ligament. The coracohumeral ligament is readily identified on sagittal and coronal T1-weighted or T2-weighted FSE images as a curvilinear low-signal structure surrounded by fat, lateral to the coracoid process (3a and 4a). The thickness of the capsule of the axillary recess is best demonstrated on coronal images at the mid glenoid level (5a).
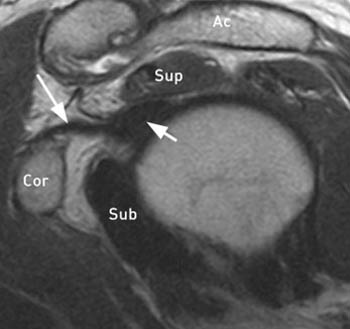
Figure 3:
(3a) A sagittal T2-weighted image of the shoulder demonstrates the normal rotator interval. The coracohumeral ligament (arrow), which along with the superior glenohumeral ligament forms the rotator interval capsule, is normally surrounded by fat. The supraspinatus muscle (Sup), subscapularis muscle (Sub), coracoid process (Cor), acromion (Ac) and long head of the biceps (short arrow) are indicated.
Figure 4:
(4a) A coronal T1-weighted image through the anterior shoulder demonstrates the normal coracohumeral ligament (arrow) arising from the coracoid process (Cor) and extending laterally toward its insertion on the greater and lesser tuberosities of the humerus. The distal clavicle (Cl) is indicated.
The MRI findings that suggest adhesive capsulitis include soft tissue thickening in the rotator interval, which may encase the coracohumeral and superior glenohumeral ligaments, and soft tissue thickening adjacent to the biceps anchor (2a, 6a). A thickened inferior glenohumeral ligament greater than 4 mm is often seen in the axillary pouch (2b). Loss of definition of the inferior capsule secondary to edema and synovitis may also be demonstrated. IV gadolinium enhancement increases the specificity of the diagnosis by demonstrating enhancement of the rotator interval capsule (7a) and enhancement of the capsuloligamentous structures in the axillary recess.3,4 MR Arthrography has also been utilized as a means of making the diagnosis of adhesive capsulitis. However, this procedure is relatively invasive and offers no specific or reproducible signs of adhesive capsulitis.5
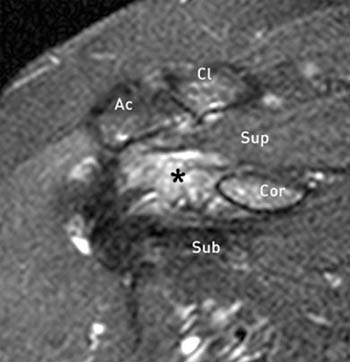
Figure 6:
(6a) A coronal T2-weighted fat suppressed image through the anterior aspect of the shoulder demonstrates increased signal intensity (asterisk) in the rotator interval region, obscuring the normal fat, suspicious for adhesive capsulitis. The supraspinatus muscle (Sup), subscapularis muscle (Sub), clavicle (Cl), Acromion (Ac) are also indicated.
Figure 7:
(7a) Post IV gadolinium enhanced sagittal T1-weighted image with fat-suppression demonstrates enhancement in the rotator interval region (arrows), confirming the diagnosis of adhesive capsulitis. The long biceps tendon (short arrow), supraspinatus muscle (Sup), subscapularis (Sub), and Coracoid (Cor) are indicated.
The natural history of idiopathic or secondary forms of adhesive capsulitis is quite variable with residual pain and stiffness persisting in some studies up to 7 years.6 Treatment regimens vary greatly, reflecting the complexity of this condition. Supportive treatment, oral and injected medications, physical therapy, the brisement procedure, manipulative therapy, and surgical release are all used in addressing this disorder, depending on the severity and duration of symptoms.
Conclusion
The MRI changes of adhesive capsulitis are most often observed at the rotator interval and the inferior glenohumeral ligament. Recent evidence indicates that IV gadolinium enhanced MR provides even greater specificity in diagnosing adhesive capsulitis. MRI is therefore an invaluable tool in differentiating adhesive capsulitis from other conditions that may have a similar clinical presentation.
References
1 Hannafin JA, DiCarlo ED, Wickiewicz TL, and Warren RF: Adhesive capsulitis: capsular fibroplasias of the Glenohumeral joint. J Shoulder Elbow Surg 3(S):5, 1994.
2 Kessel L: Disorders of the Shoulder. New York: Churchill Livingstone, 1982, p82.
3 Carillon Y, Noel E, Fantino O, Perrin-Faylle O, Tran-Minh VA: Magnetic resonance imaging findings in idiopathic adhesive capsulitis of the shoulder. Rev Rhum Engl Ed. 1999 Apr;66(4):201-6.
4 Connell D, Padmanabhan R, Buchbinder R. Adhesive capsulitis: role of MR imaging in differential diagnosis. European Radiology. 2002 Aug;12(8):2100-6.
5 Manton GL, Schweitzer ME, Weishaupt D, Karasick D. Utility of MR arthrography in the diagnosis of adhesive capsulitis. Skeletal Radiol 2001;30:326-30.
6 Shaffer B, Tibone JE, Kerlan RK: Frozen shoulder: A long-term follow-up. J Bone Joint Surg 74A:738-746, 1992.