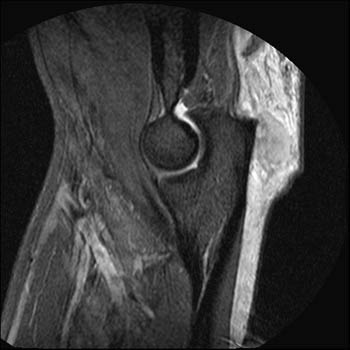
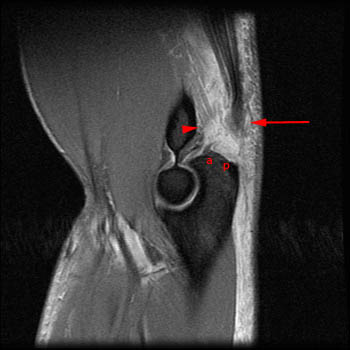
Clinical History: A 45 year old male complains of pain and swelling at the posterior elbow following a lifting injury three days ago. A sagittal inversion recovery image at the mid elbow is provided (1a). What are the findings? Is there a complete or an incomplete tear?
Findings
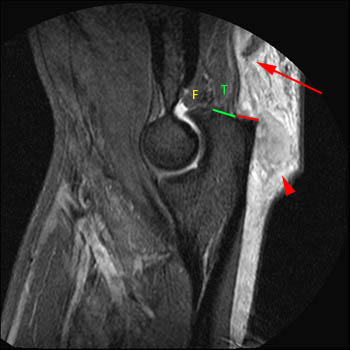
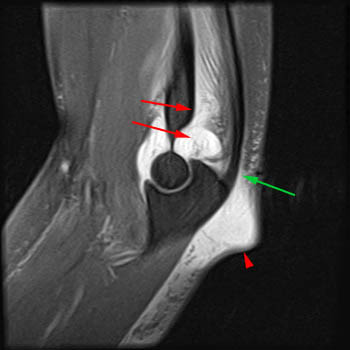
Figure 2:
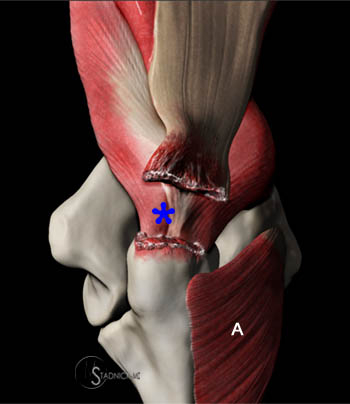
The posterior component of the distal triceps tendon (combined tendon of the lateral and long heads) is completely avulsed and retracted (red arrow). The anterior or deep component of the distal triceps (medial head) remains intact (T). Note the exposed surface of the olecranon from which the posterior component has been avulsed (red line) and the remaining intact attachment of the primarily muscular anterior component (green line). The posterior fat pad (F) is low in signal due to the fat-suppressed imaging technique. A localized hematoma (red arrowhead) is found posterior to the olecranon.
Diagnosis
Complete tear/avulsion of the posterior component of the triceps tendon (combined tendon of the lateral and long heads). Intact anterior component (medial head insertion).
Introduction
Tears of the triceps tendon are not common injuries, but are receiving increasing attention in the literature. It has been suggested that the modern athlete may be more predisposed to triceps injuries than his or her predecessors1. Among athletes, distal triceps injuries are more frequent in football linemen2 and weightlifters3. Other athletes with repetitive loading during elbow extension are also susceptible. Factors that weaken the tendon and increase the risk of tear include local corticosteroid injection, systemic steroids, and olecranon bursitis. Most cases remain in the non-athlete population, the vast majority of these involving falls on the outstretched hand, but also from lifting injuries or blunt trauma. Patients typically present with pain, swelling, and loss of extension strength.
Even in patients with higher grade injuries, the clinical diagnosis of a triceps tear can be difficult. In acute injuries edema and hemorrhage can limit range of motion and prevent palpation of a retracted tendon. Pain may limit assessment of strength. Radiographs may demonstrate a small avulsed bone fragment that some consider pathognomonic, but these are not always present. MRI is beneficial for confirming the diagnosis and evaluating the extent of injury.
Anatomy and Function
The triceps is the only major extensor of the elbow. It is a tripennate muscle with origins on the infraglenoid tubercle of the scapula (long head), the upper posterior humerus (lateral head), and lower posterior humerus (medial head). The distal insertion is primarily on the olecranon, with the exception being a lateral aponeurotic expansion that extends distally over the anconeus to the proximal forearm fascia (4a).
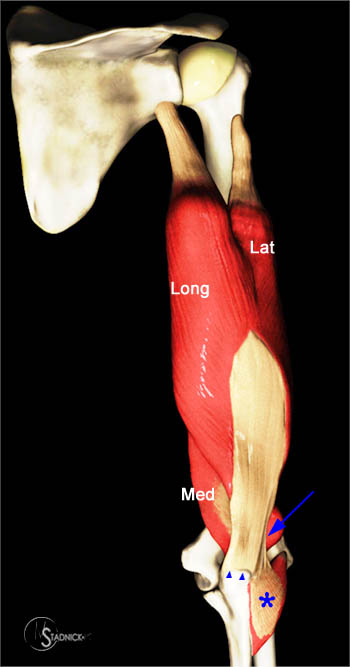
Figure 4:
A posterior 3D representation of the triceps demonstrates the long head (Long), the lateral head (Lat), and the medial head (Med). Distally the long head and lateral head insert at the olecranon as a common tendon (arrowheads). The lateral expansion (arrow) continues distally over the anconeus muscle (asterisk).
The distal triceps insertion has traditionally been considered to be one combined tendon unit. However, Madsen4 recently described a surgical observation and subsequent anatomic study confirming that the medial head of the triceps has a separate insertion that is positioned anterior/deep to the common tendon of the lateral and long heads. The result of this laminar anatomy is that the components may be injured separately, and the differing injuries may have a different clinical presentation and surgical approach. Although histologic assessments4,5,6 have shown a single confluent attachment to bone, the injury patterns do separate between the units Madsen described. Madsen also reported an uncommon case of isolated avulsion of the deep component. This manifested clinically by extension weakness with the elbow in full flexion. He therefore advocated adding to the clinical exam of patients with suspected triceps injuries an assessment of extension strength while in full flexion. Other authors have subsequently reported additional cases of isolated medial head avulsion and showed a separate insertion of the medial head in 53% and a combined insertion in 47% of specimen elbows7. In cases of a combined insertion the medial head tendon fibers were still shown to be positioned anterior to those of the combined lateral and long heads.
MRI Findings
Distal triceps tendon tears are nearly always avulsions at the tendon bone interface and have generally been characterized simply as complete or incomplete. Complete tears are reported to be more common. However, as in the test case presented above, MRI most frequently reveals a complete avulsion and retraction of the posterior component of the tendon (combined attachment of the long and lateral heads) with the anterior component (medial head) remaining intact. Of twenty cases of distal triceps injury sampled from our database, only one was a complete avulsion of both components (5a). Sixteen were complete avulsions of the posterior component alone, one was a partial tear of the posterior tendon insertion, two were partial tears at the myotendinous junction, and one was an isolated injury of the medial head attachment (6a).
Figure 5:
Complete avulsion of the distal triceps from a fall on ice. This includes anterior muscular (arrowhead) and posterior tendinous (arrow) components. The entire footprint is uncovered with the exception of a very small residual strand at the attachment site of the anterior/deep component (a) This was the only case out of a sample of twenty that demonstrated complete disruption of both components of the triceps.
Figure 6:
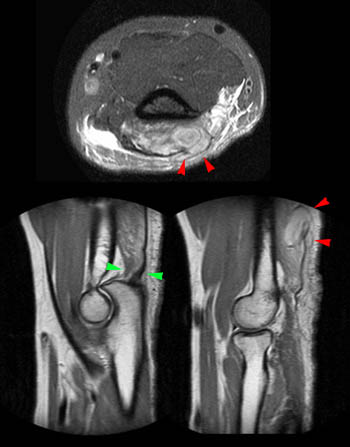
Isolated anterior component injury incurred while cutting tree limbs. The muscular anterior component of the distal triceps insertion (red arrows) is severely injured with little or no remaining attachment to the olecranon. Associated disruption of the posterior joint capsule has created continuity between the joint and the muscle gap. The posterior component (green arrow) remains intact. A fluid collection has accumulated posteriorly from hemorrhage and escape of joint fluid (red arrowhead).
Potential difficulties in MRI interpretation may arise from several factors. When avulsed, the posterior tendon component can retract several centimeters despite the anterior component remaining intact. A high position or irregularity of the retracted tendon margin may make it difficult to identify on sagittal images. Also, the intact tendinous portion of the anterior component may simulate a completely intact tendon. Clues to the correct diagnosis include posterior hemorrhage and edema as well as exposure of the footprint of the posterior component on the olecranon. Often the retracted tendon can be found high on the sagittal images and is definitively confirmed on correlation with the axial views (7a).
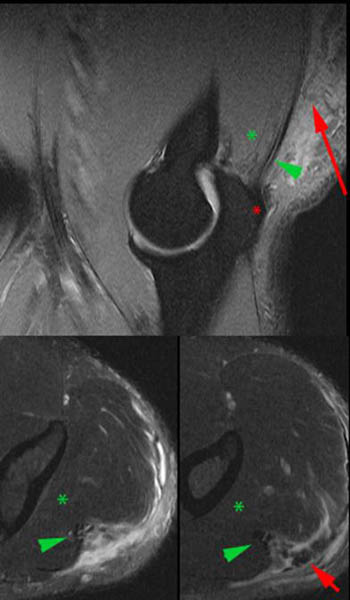
Figure 7:
Complete posterior component avulsion incurred while breaking up a fight. The completely avulsed end of the posterior triceps component (long and lateral head tendon) is irregular and retracted (red arrow). The anterior component (medial head) remains intact and is primarily muscular (green asterix). The tendinous portion of the anterior component (green arrowhead) may simulate an untorn tendon particularly if the posterior component is not well seen or is retracted above the imaged area. The uncovered footprint of the posterior component (red asterix) aids the diagnosis, as do serial axial images that demonstrate the retracted tendon above a fluid-filled gap. This injury pattern is the most common, and is similar to our test case above.
An additional potential difficulty in image interpretation may arise from our common use of fat suppressed imaging techniques. Fat suppression is very helpful in aiding diagnosis, but one must be aware of the the distinction between the posterior fat pad of the elbow and the anterior component of the distal triceps insertion. On fat-suppressed images, slightly higher signal and subtle linear striations help to distinguish the deep muscle from the adjacent posterior fat pad.
Bone fragments are often associated with triceps tendinopathy but may be difficult to identify on fat-suppressed images. Once again, these sequences that are so helpful to us in the delineation between torn and intact tissues make the fat in bone dark and difficult to distinguish from surrounding dark tissues such as tendon. In such cases, the T1-weighted sequences are more helpful than the fat-suppressed water-weighted ones. Osseous fragments may be due to avulsion fracture or from chronic tendinopathy with heterotopic ossification. The latter are typically more rounded, are circumferentially corticated, and are more often multiple (8a). Marrow edema is not typically present in either case and is therefore not a reliable differentiator.
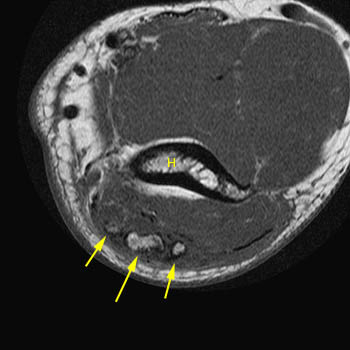
Figure 8:
A T1-weighted axial image reveals heterotopic ossifications in the distal triceps tendon of a patient with injury sustained in a fall on the elbow. The heterotopic ossifications (arrows) appear well-corticated with somewhat rounded margins and typically are not edematous. These indicate chronic underlying tendinopathy. In this patient the ossifications were displaced proximally together with the retracted posterior tendon component. The anterior component of the distal triceps remained intact. (H = humerus).
Although the majority of injuries occur as avulsions of the tendon insertion, the distal triceps may partially tear at the myotendinous junction (9a). The resultant hemorrhage and swelling may even simulate a mass.
Figure 9:
Partial tear of the triceps myotendinous junction from a fall. Axial STIR (above) and proton density weighted sagittal images are provided. The distal insertion remains intact (green arrowheads). On the more lateral sagittal image and on a proximally positioned axial image the myotendinous junction is partially torn and a hematoma simulates a small mass (red arrowheads). Tendon and muscle fibers are discontinuous at the site of injury.
Other Triceps Injuries
Injuries limited to the lateral triceps expansion are generally not considered to be surgically significant. Muscle strains occurring at the mid or proximal muscle bellies are probably underrepresented in MRI series since they are less likely to come to clinical attention. Proximal triceps avulsions are rare; one case of a proximal avulsion of the long head from the infraglenoid tubercle was recently reported in a surfer8.
Treatment Considerations
Primary repair of a torn triceps tendon is possible within the first 3 weeks after injury10. Delayed diagnosis may necessitate reconstruction, which is more complex and can have a longer recovery period. Unlike biceps tendon tears at the elbow, in which the brachialis still serves to flex the elbow, triceps tears result in a dramatic loss of function, as the triceps is the only extensor at the elbow. Surgery is therefore recommended for virtually all complete tears in active persons and for incomplete tears when there is concomitant loss of strength9. Since it is only relatively recently that Dr. Madsen described in the orthopaedic literature the separate attachment of the medial head, it is likely that the simple descriptions of complete versus incomplete tears actually were referring to the status of the posterior component alone. This is supported by the fact that some MR images depicting complete tears in previous literature1,2 show an intact anterior component in addition to the completely avulsed posterior tendon.
Conclusion
- MRI is adept at demonstrating the spectrum of distal triceps injuries and associated pathologies such as chronic tendinosis or bursitis.
- Distal triceps tears most commonly spare the anterior component (primarily muscular medial head insertion) and completely avulse the posterior component (combined tendon of the long and lateral head insertion). Retraction of the posterior component is common in these patients.
- If an injury sparing the anterior component is described in a report simply as an incomplete tear of the triceps tendon, this may inadvertently mislead the reader about the actual severity of injury, one that would otherwise have been termed and treated as complete. Both components of the distal triceps insertion are best described separately, with emphasis on the status of the posterior component.
References
1 Huber, FG. Arm: Tendon and Muscle Ruptures. In: DeLee JC, Drez D, Miller MD, eds. DeLee and Drez’s Orthopaedic Sports Medicine, 3rd ed. Philadelphia, Saunders, 2009.
2 Mair SD, Isbell WM, Gill TJ, Schlegel TF, Hawkins RJ. Triceps tendon ruptures in professional football players. Am J Sports Med. March 2004 vol. 32 no. 2 431-434.
3 Sollender JL, Rayan GM, and Barden GA, Triceps tendon rupture in weightlifters, J Shoulder Elbow Surg 7 (1998), pp. 151-153.
4 Madsen M, Marx RG, Millett PJ, Rodeo SA, Sperling JW, Warren RF. Surgical anatomy of the triceps brachii tendon: anatomical study and clinical correlation. Am J Sports Med. 2006 Nov;34(11):1839-43. Epub 2006 May 30.
5 Belentani C, Pastore D, Wangwinyuvirat M, Dirim B, Trudell DJ, Haghighi P, Resnick D. Triceps brachii tendon: anatomic-MR imaging study in cadavers with histologic correlation. Skeletal Radiol. 2009 Feb;38(2):171-5. Epub 2008 Nov 5.
6 Keener JD, Chafik D, Kim HM, Galatz LM, Yamaguchi K. Insertional anatomy of the triceps brachii tendon. Journal of Shoulder and Elbow Surgery. 2010 Jan.
7 Athwal GS, McGill RJ, Rispoli DM. Isolated Avulsion of the Medial Head of the Triceps Tendon: An Anatomic Study and Arthroscopic Repair in 2 Cases. Arthroscopy 2009 Sep; 25(9):983-988.
8 Clifford PD, Posada A, Hancock CR. Isolated long-head triceps brachii tendon avulsion in a surfer detected at MR imaging. Skeletal Radiol. 2009 Jan;38(1):77-80. Epub 2008 Sep 6.
9 Yeh PC, Dodds SD, Smart LR, Mazzocca AD, Sethi PM. Distal triceps rupture. J Am Acad Orthop Surg. 2010 Jan;18(1):31-40.
10 van Riet RP, Morrey BF, Ho E, O’Driscoll SW. Surgical treatment of distal triceps ruptures. J Bone Joint Surg Am 2003;85: 1961-7. 9.