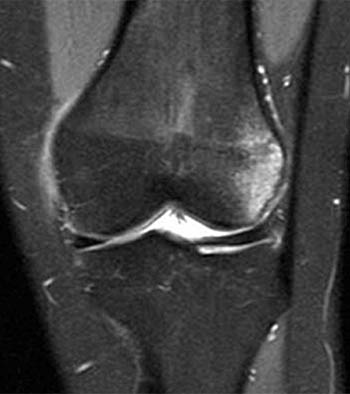
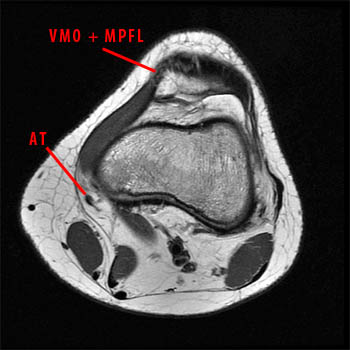
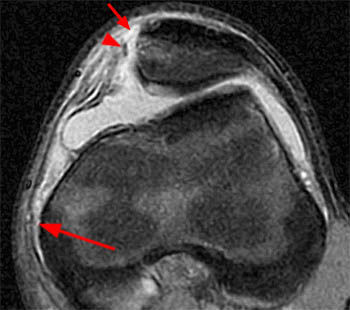
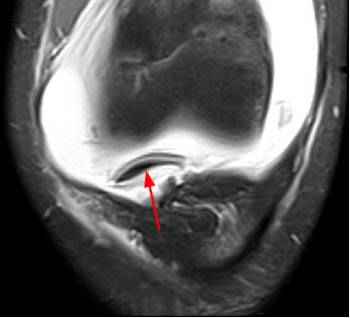
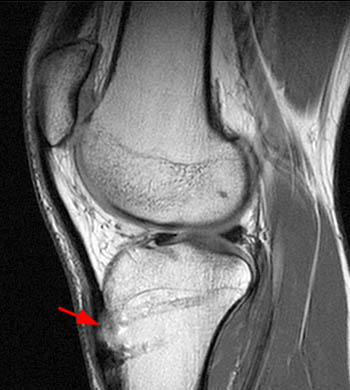
Clinical History: A 23 year-old female presents with medial knee pain following a twisting injury. (1a) A single fat-suppressed proton density-weighted coronal image is provided. What is the diagnosis?
Findings
Diagnosis
Transient lateral patellar dislocation.
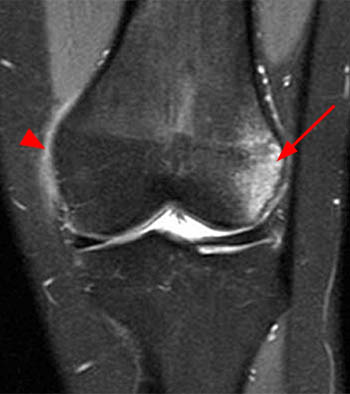
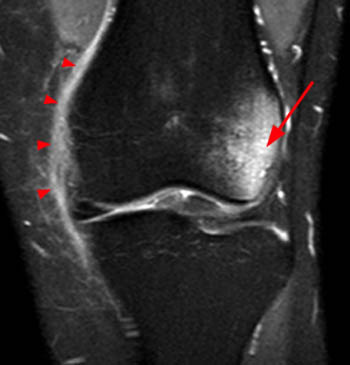
Although you may feel that being asked to make the specific diagnosis of lateral patellar dislocation from a single image is unrealistic, the coronal view in fact reveals a classic and highly characteristic appearance, allowing the diagnosis to be made with confidence.
The marrow edema and medial patellofemoral ligament (MPFL) injury pattern above are virtually pathognomonic of a transient lateral patellar dislocation, as little else will cause such an appearance. Given the lack of history of direct trauma, a reliable diagnosis can be made.
Introduction
The pattern of bone bruising seen in a transient lateral patellar dislocation is easy to understand if one considers the mechanism of injury. The injury typically occurs from a twisting event with the knee in mild flexion (less than 30°). The patella becomes unstable and undergoes a transient, violent lateral displacement. During this dislocation phase of injury, shearing forces can damage the articular surfaces of either the patella or the lateral femoral condyle. With knee extension and subsequent reduction, the patella bounces back into position and in doing so, the medial patella impacts against the non-weightbearing anterolateral aspect of the lateral femoral condyle, resulting in the characteristic marrow edema pattern.
The convex articular surface of the patella places it at risk for chondral injury in either the dislocation or the reduction phases of injury. Femoral condylar chondral injuries occur during the dislocation phase due to impaction shearing forces of the patella upon the flexed femur, typically occurring at the weightbearing surface. Because as noted above, the femoral bone bruise occurs as the patella moves forward during reduction, bone bruises at the lateral femoral condyle always course anteriorly from the site of any femoral chondral injury that may be present. The trochlea, due to its large surface area and concave contour, is rarely subject to chondral injury in patellar dislocation.
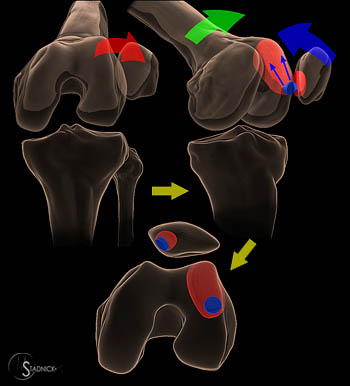
Figure 3:
(3a) Graphical depictions of the mechanism of patellar dislocation: With the knee in flexion, the patella dislocated laterally. Because the knee is flexed in dislocation, the patella impacts upon the weightbearing surface of the lateral femoral condyle. A bone bruise occurs anterior to this site of impaction as the patella reduces with knee extension. Medial patellar chondral injuries may occur during either the dislocation or reduction phases of injury.
The above video demonstrates the mechanism of injury in patellar dislocation. Courtesy of Daniel Bodor, MD, Radsource.
Because of the transient and brief nature of lateral patellar dislocations, the diagnosis is frequently unrecognized by both patients and clinicians.1 Pain is often described as medial because of soft tissue injuries that occur to the medial retinaculum and/or MPFL. Evaluation of both of these soft tissue structures is critical when one examines a MRI following lateral patellar dislocation, as the extent of soft-tissue injury influences the use of operative repair. Trauma itself rarely causes patellofemoral dislocations without predisposing factors such as trochlear dysplasia, patella alta and lateralization of the tibial tuberosity. MRI plays a crucial role in quantification and characterization of these predisposing anatomic variations which are key to addressing the patient?s patellar instability operatively. Nearly 50% of all first-time dislocators will sustain further dislocations. Recurrent dislocations and chronic patellofemoral joint instability will lead to significant cartilage damage and severe arthritis if left untreated. The primary aim of surgery is to repair the knee damage and to correct the anomalies that are predisposing to chronic instability.
Anatomy and Function
The most important soft tissue passive stabilizers involved in patellofemoral dislocation injuries have traditionally been referred to as the MPFL and the medial retinaculum. Despite the presence of numerous detailed anatomical dissection and MRI based studies of the anatomy2,3, there is much variability in the description of these structures within the literature. Most, however, agree regarding the importance of the MPFL and its role as the strongest restraint to lateral patellar displacement. The MPFL is composed of a stronger transverse band and a more variable and weaker oblique decussation. The transverse band attaches to the upper pole of the patella, and this component originates on a bony groove that lies between the adductor tubercle and the medial epicondyle, slightly posterior to the epicondyle. The oblique decussation of the MPFL blends with fibers of the superficial MCL. Other structures that blend in this region include the medial patellotibial ligament, the medial patellomeniscal ligament, the investing fascia, and the medial joint capsule. In effect all three medial layers of the knee thus comprise the medial retinaculum, which is by itself not a discrete, single structure. Anatomically, the transverse band of the MPFL is also a component of the medial retinaculum, but for purposes of MRI interpretation, the general convention is to describe abnormalities of the transverse band as being MPFL injuries, whereas more distal injuries which involve multiple layers are generally referred to as abnormalities of the medial retinaculum.
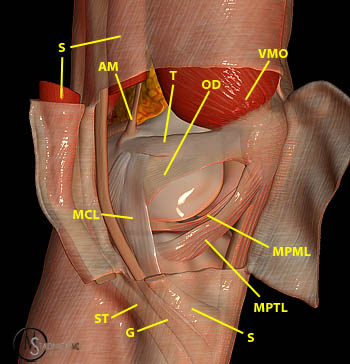
Figure 4:
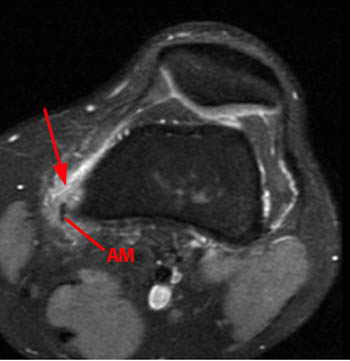
(4a) This 3D graphic view of the medial knee with the crural fascia and sartorius (S) muscle incised and reflected demonstrates the main medial contributors to patellar stability. The medial patellofemoral ligament is composed of a transverse (T) component arising between the adductor tubercle and medial epicondyle and an oblique decussation that originates from the medial collateral ligament (MCL). Additional passive stabilizers include the medial patellotibial ligament (MPTL) and the medial patellomeniscal ligament (MPML). The vastus medialis oblique (VMO) provides active stability of the patella. Other indicated structures: gracilis (G), semitendinosus (ST), and adductor magnus (AM) tendons.
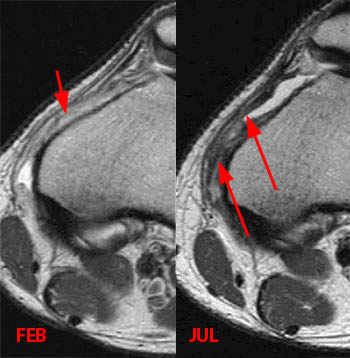
As with the anatomy, there is considerable variability in both the surgical and radiology literature regarding the location of soft tissue injuries in patients following patellar dislocation. There is agreement, however, that the MPFL is almost always injured with lateral patellar dislocations4. In our experience, injuries to the transverse band most often involve the femoral attachment, whereas injuries to the oblique decussation and associated medial retinacular structures are more common at the patellar attachment. The femoral attachment of the transverse band of the MPFL is not always discretely visible, and therefore secondary signs on MRI such as fluid, edema, and soft tissue thickening at the attachment indicate MPFL injury.
The most important active stabilizer of the patella is the vastus medialis oblique (VMO). The VMO blends distally with the MPFL to attach to the medial border of the patella along its upper two thirds. The VMO is active, not only in full extension but also at 30 degrees and up to 100 degrees of flexion. It acts as a powerful extensor of the knee. VMO dysplasia may play a role in patellofemoral instability. Fluid extending into the VMO myotendinous junction is generally seen in the setting of coexisting MPFL/retinacular tears.
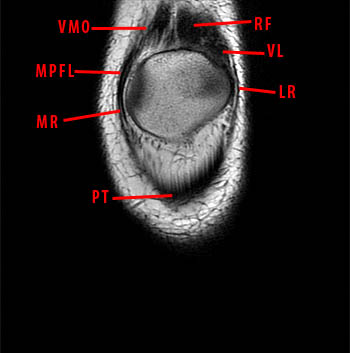
Figure 7:
(7a) A coronal T1-weighted image at the level of the patella demonstrates blending of fibers of the VMO with the MPFL superiorly. Inferiorly, components of the medial retinaculum blend with the patellar tendon. The rectus femoris (RF), vastus lateralis (VL), and lateral retinaculum (LR) are also indicated.
The osteocartilaginous anatomy of the patellofemoral joint provides additional static stabilization to the joint. Trochlear geometry, including slope of the lateral wall and depth, is an important factor. Predisposing factors to patellofemoral dislocation include patella alta, excessive lateral distance between the tibial tubercle and trochlear groove and a congenitally shallow trochlear groove5, any of which significantly increase a patient’s likelihood for dislocation. Less common predisposing factors to be aware of include laterally tilted patella, VMO dysplasia and generalized joint laxity.
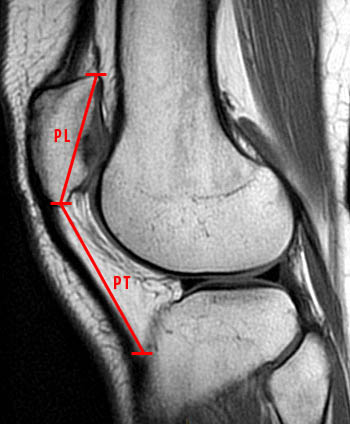
Patella alta is considered an important factor in patellar instability. The decreased patellar contact area decreases stability particularly in shallow degrees of flexion and thus predisposes to lateral patellar subluxation. There are several different techniques described in the literature to assess patella alta and many of these are reviewed in detail in the MRI Web Clinic, August 20106. The Insall-Salvati index is the most widely accepted measurement and is easily performed on radiographs and MRI examinations.
Excessive lateralization of the tibial tuberosity allows the patella to be pulled laterally in flexion and is considered to be a risk factor for instability. The distance from the tibial tubercle to the trochlear groove (TT-TG) provides a quantitative evaluation of excessive lateralization of the tibial tuberosity.7
Figure 10:
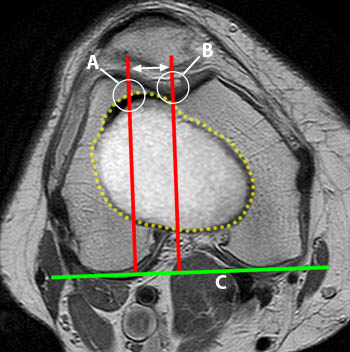
(10a) Axial image of the knee with superimposition of the tibial tubercle from another slice (yellow outline). The distance (double-headed arrow) from the deepest point of the trochlea (line B) to the middle of the tibial tubercle (line A) is measured, again by using the posterior plane of the condyles as the reference line (line C). A distance between the tibial tubercle and the trochlear groove of less than 15 mm is considered normal. Distances between 15 and 20 mm are borderline, and distances of more than 20 mm indicate significant lateralization of the tuberosity.5
The normal trochlea is concave with medial and lateral facets articulating with the patellar facets. Flattening or developmental dysplasia of the trochlea leads to loss of normal patellar tracking and can predispose to lateral patellar dislocation with flexion. Techniques for quantifying trochlear dysplasia with MRI have been standardized and shown to be accurate and reproducible in assessing lateral trochlear inclination, facet asymmetry, and trochlear depth8,9. The discrimination between low-grade and high-grade dysplasia is important because prognosis and treatment may depend upon the severity of trochlear dysplasia. These measurements are not routinely recorded in the MRI report, but in select situations may be helpful in quantifying low-grade versus high-grade dysplasia.
Figure 11:
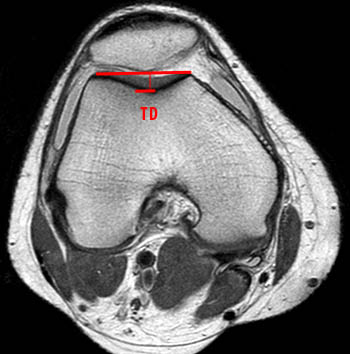
(11a) The depth of the trochlear groove is measured by drawing a line from the most anterior position of the medial trochlea to the lateral trochlear anterior cortex. A perpendicular line is measured to the most posterior cortex of the central trochlea. This distance is the trochlear sulcus depth (TD). Normal TD > 5.2mm. A trochlear depth of < 3mm indicates dysplasia.
Trochlear depth of less than 3 mm on MRI has a sensitivity of 100% and a specificity of 96% for trochlear dysplasia.10
Figure 12:
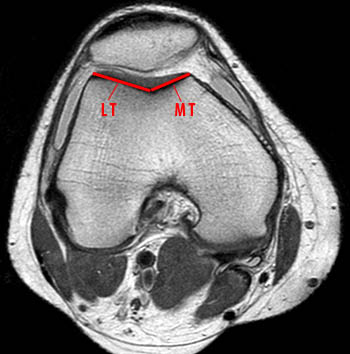
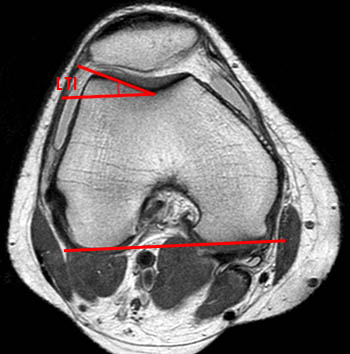
(12a) At an axial image 3 cm proximal to the femoral-tibial joint space, the lengths of the medial and lateral trochlear facets are obtained. The ratio of the medial to the lateral facet length defines trochlear facet asymmetry (MT/LT) *100%. A facet ratio of < 40% indicates dysplasia.
Figure 13:
(13a) A line is drawn between the cortex of the lateral trochlear facet on the most superior axial image showing cartilage. A second line is drawn parallel to a line along the posterior femoral condyles. The angle between the two lines is the lateral trochlear inclination (LTI). LTI < 11 degrees indicates dysplasia.
MRI Findings in Transient Patellofemoral Dislocation
Bone bruises at the anterolateral aspect of the lateral femoral condyle and at the inferomedial patella are the most constant findings in patients who have sustained a recent patellar dislocation. Osteochondral injuries of the inferomedial patella are seen in up to 70% of patellofemoral dislocations. Osteochondral injuries to the inferomedial patella may be the result of impaction during dislocation or shearing with reduction. Femoral osteochondral injuries, when present, typically involve the lateral weightbearing surface. In either case, careful search for possible displaced osteochondral fragments is necessary, as surgery is often indicated in such patients.
Abnormalities of the medial retinaculum and MPFL are seen in 82-100% of MRI examinations following patellar dislocation. Characterization of the type of medial restraint injury is crucial for surgical planning. Tears of the medial retinaculum and the MPFL are commonly present at both the patellar and femoral attachments, though tears of the transverse band of the MPFL are more likely at the femoral attachment. Femoral avulsion of the MPFL is a predictor of chronic instability and may be a surgical indication in some patients with acute injury. Persistent abnormalities of patellar alignment and abnormalities of trochlear morphology are also common, and should be carefully described.
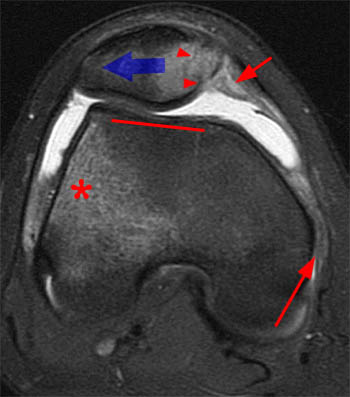
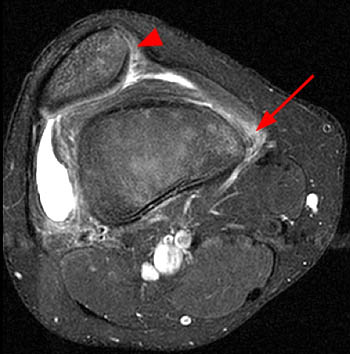
Figure 16:
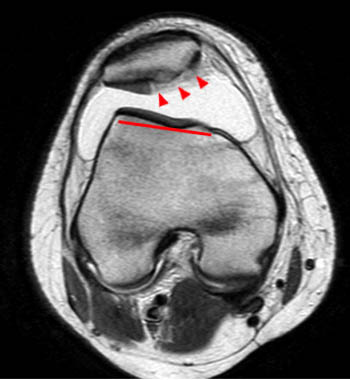
(16a) An axial fat-suppressed T2-weighted image reveals numerous typical findings of recent lateral patellar dislocation. The patella remains laterally shifted (blue arrow) and an osteochondral injury of the medial patella (arrowheads) is apparent. Edema and thickening compatible with tears of the MPFL and medial retinaculum (red arrows) are apparent both anteriorly and posteriorly. A bone bruise of the lateral femoral condyle (asterisk) and an abnormally shallow trochlear groove (red line) are also indicated.
Figure 18:
(18a) A 13-year-old female following acute patellar dislocation. The axial proton density-weighted image reveals a large osteochondral shearing injury involving the mid to medial patella (arrowheads). The patella remains laterally subluxed and tilted, and the patient has an abnormally shallow trochlear groove (line).
Figure 20:
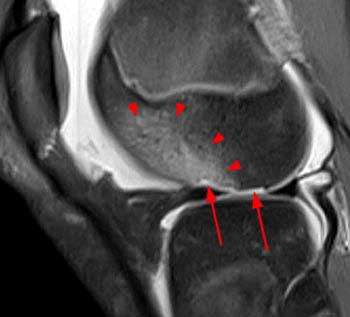
(20a) A fat-suppressed proton density-weighted sagittal image in a patient following patellar dislocation reveals an osteochondral injury with a chondral defect (arrows) at the lateral weightbearing surface of the lateral femoral condyle, a finding seen in only 5% of patients. As is typical, a bone bruise extends anteriorly (arrowheads) from the site of the chondral defect.
Figure 22:
(22a) In this patient with an acute first time patellar dislocation injury, typical bone bruises were not apparent. However, subtle sprains are seen at the anterior medial retinaculum (arrowhead) and posterior MPFL (arrow) along with a large joint effusion. A patient with acute first-time transient patellar dislocation without osteochondral lesions and severe risk factors for redislocation is generally treated conservatively.
MRI findings of Chronic Patellofemoral Instability and Recurrent Dislocations
Patients who experience multiple patellar dislocations are more likely to have anatomical variants of the trochlea, patellar alta, or tibial tubercle lateralization. Of course, if medial soft tissue restraints are disrupted at the first dislocation, the loss of such restraints makes future dislocations more likely. Areas of scarring and osteochondral lesions become more common as the frequency of patellar dislocation increases.
Figure 23:
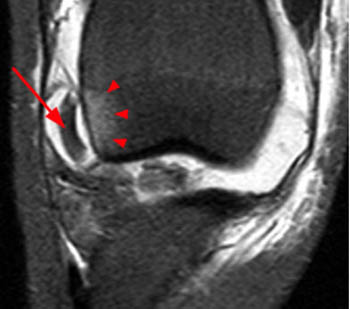
(23a) In this patient with recurrent patellofemoral dislocations, there are findings of subchondral degeneration (arrow) from recurrent impaction and chondral shearing injuries to the inferolateral femoral condyle. A sliver of fluid undermines a moderately thickened and scarred MPFL at the medial femoral condyle attachment consistent with a chronic partial stripping tear (arrowheads).
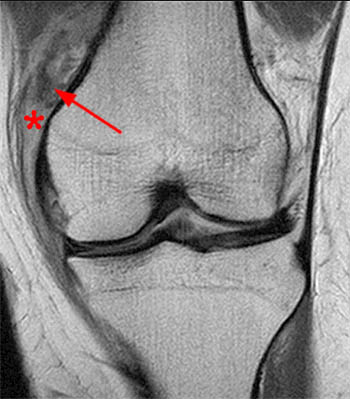
Figure 24:
(24a) Scarring of the medial stabilizers (asterisk) often leads to healing in a more superior and lateral location (long arrow) leading to persistent medial instability, laxity and malalignment even after the patella has been repositioned. Laxity of the medial stabilizers will lead to increasing instability over time.
Figure 26:
(26a) An axial proton density-weighted image reveals trochlear dysplasia (line, indicating facet asymmetry and a shallow trochlear groove), ossification in the medial retinaculum and MPFL attachment anteriorly (short arrow) and diffuse scarring of the medial retinaculum (arrowheads)--these findings indicate chronic patellofemoral instability.
Surgical Indications and Repair Techniques
Nonoperative treatment is generally recommended in first time dislocators unless there are MRI findings of severe predisposing dysplasia and the presence of a chondral or osteochondral body. Such patients are generally treated with immobilization for 3 to 6 weeks. Physical therapy is directed to increasing range of motion and to strengthening the VMO and quadriceps muscles. The patients are then J-braced for 3 to 6 months for all sports activities.
Surgical indications following patellar dislocation include the presence of a chondral or osteochondral body, significant rupture of the medial stabilizers most importantly the MPFL, a persistent laterally subluxed patella, or a second dislocation injury in a patient with malalignment or dysplasia. It is reported in surgical literature that 50-75% of recurrent dislocators, have some form of dysplasia, malalignment or generalized joint laxity.
Surgical repair is most commonly directed to MPFL reconstruction and to distal realignment in the subset of patients who have significant osseous malalignment. The latter distinction is important to recognize among both radiologists and surgeons. In patients without osseous malalignment, MPFL reconstruction and plication of the medial restraints is reported to decrease re-dislocation rates to 5%. However, in the setting of osseous malalignment, MPFL reconstruction alone leads to higher rates of recurrent instability. In general realignment surgery such as tibial tubercle transfer should be strongly considered in patients with TT-TG > 15mm (borderline) and typically should be performed in patients with TT-TG > 20mm. It is therefore recommended that radiologists include measurement of TT-TG in reports on patients who undergo MRI for patellar instability.
There are numerous techniques reported in literature and commonly used to reconstruct the medial sided soft tissue constraints. One of the more common MPFL reconstruction procedures uses a single hamstring tendon graft passed through the medial intermuscular septum at the adductor magnus insertion fixed by an anchor in the femoral condyle and sutured or anchored to the superomedial pole of the patella11. MRI can provide valuable information regarding the status of such repairs in patients who experience recurrent dislocation following surgery.
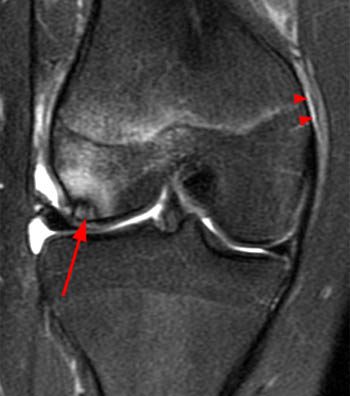
Figure 27:
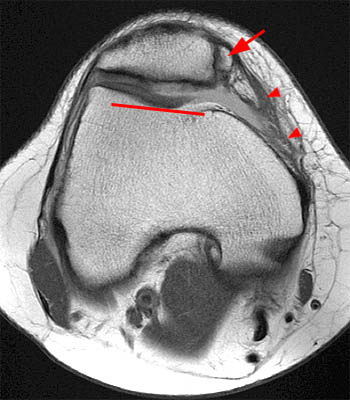
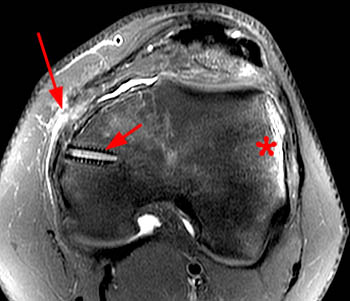
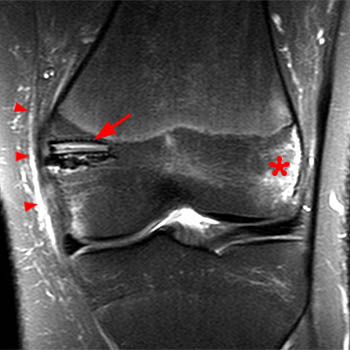
(27a) Axial and (27b) coronal fat suppressed proton density-weighted images in a patient who experienced recurrent patellar dislocation following surgery. A tear of the reconstructed MPFL is indicated by fluid interrupting the fibers (27a, long arrow) (27b, arrowheads). A typical bone bruise is seen within the anterolateral aspect of the lateral femoral condyle (asterisk).
Surgical realignment procedures include medialization of the tibial tubercle particularly in patients with a TT-TG distance greater than 20mm. Patients with patella alta may also benefit from tibial tuberosity advancement.
Trochleoplasty is rarely performed in this country and is reserved for significant dysplasias or when other surgical options have been insufficient in restoring patellofemoral stability. The most common trochleoplasty procedure described is a combination of lateral trochlear osteotomy and bone graft to heighten the lateral trochlea.
Recent literature does not encourage the use of lateral release, since this can increase patellar instability. The lateral retinaculum provides significant additive support to the medial stabilizers. Long term follow up studies in patients who have undergone a lateral release have shown an increased incidence of patellofemoral arthritis.
Conclusion
Lateral patellar dislocation is a common clinical entity with a characteristic MR appearance. Because the diagnosis of lateral patellar dislocation is often unsuspected, MR provides valuable diagnostic information in such cases. Additionally, MR’s ability to delineate the extent of injury and predisposing factors is important in patient care and surgical planning.
References
1 Lance E, Deutsch AL, Mink JH. Prior lateral patellar dislocation: MR imaging findings. Radiology 1993; 189:905-907.
2 Baldwin JL. The anatomy of the medial patellofemoral ligament. Am J Sports Med 2009 37: 2355-2362.
3 Dirim B, Haghighi P, Trudell D et al. Medial patellofemoral ligament: cadaveric investigation of anatomy with MRI, MR arthrography, and histologic correlation. AJR 2008: 191:490-498.
4 Sanders TG, Morrison WB, Singleton BA, Miller MD, Cornum KG. Medial patellofemoral ligament injury following acute transient dislocation of the patella: MR findings with surgical correlation in 14 patients. J Comput Assist Tomogr 2001; 25:957-962.
5 Carrillon Y, Abidi H, Dejour D, et al. Patellar instability: Assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology 2000; 216: 582-585.
6 Cone R. Patella Alta and Baja. MRI Web Clinic, August 2010. https://radsource.us/patella-alta-and-baja/.
7 Balcarek P, Jung K, Frosch KH, Sturmer KM. Value of the tibial tuberosity-trochlear groove distance in patellar instability in the young athlete. Am J Sports Med. 2011;39(8):1756-1761.
8 Lippacher S, Dejour S, Elsharkawi M, et al. Observer Agreement on the Dejour Trochlear Dysplasia Classification: A comparison of true lateral radiographs and axial magnetic resonance images. Am J Sports Med. 2012;40(4):837-844.
9 Lippacher S, Dejour S, Elsharkawi M, et al. Observer Agreement on the Dejour Trochlear Dysplasia Classification: A comparison of true lateral radiographs and axial magnetic resonance images. Am J Sports Med. 2012;40(4):837-844.
10 Diederichs G, Issever Ahi S, Scheffler S. MR Imaging of Patellar Instability: Injury Patterns and Assessment of Risk Factors. RadioGraphics 2010; 30: 961-981.
11 Lind M, Jakobsen B, Lund B, et al. Reconstruction of the medial patellofemoral ligament for treatment of patellar instability. Division of Sports Trauma, Department of Orthopaedics, Aarhus University Hospital, Aarhus, Denmark. Correspondence ML: [email protected] Submitted 07-19-2011.