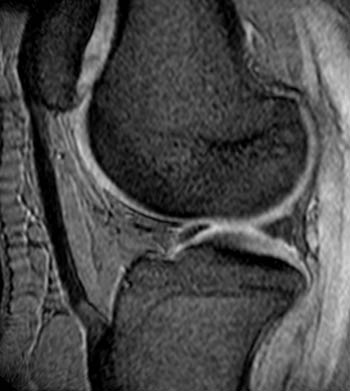
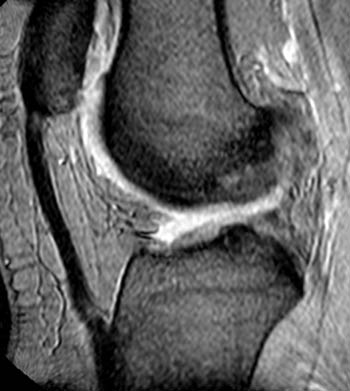
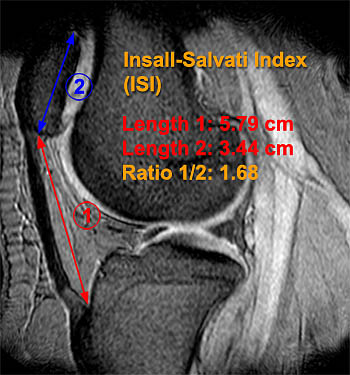
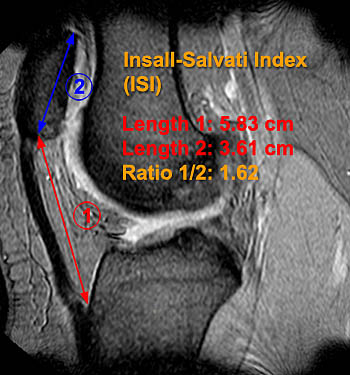
Clinical History: A 20 year-old woman is referred for MRI of the knee with complaints of chronic bilateral anterior knee pain and instability. Sagittal 2D gradient echo MRI sequences of the left (1a) and right (1b) knees are provided. What are the findings and what is the likely etiology for the patient’s symptoms?
Findings
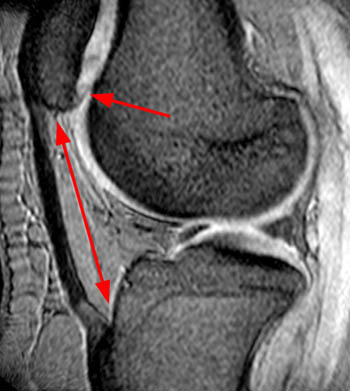
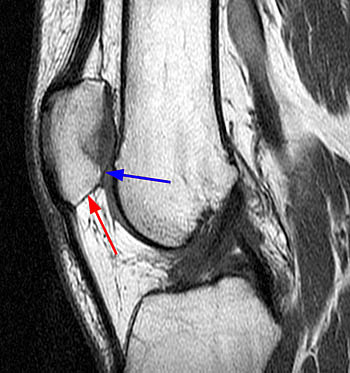
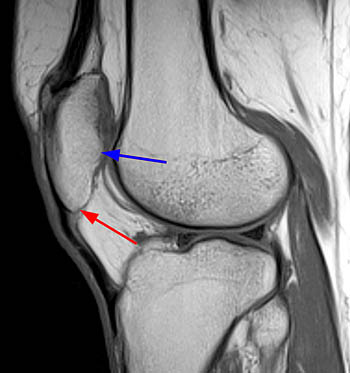
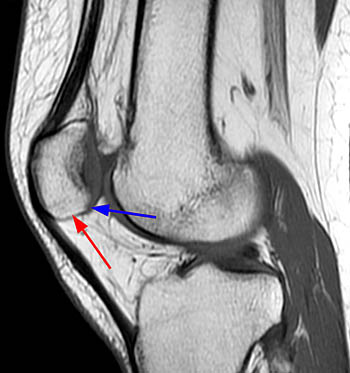
Figure 2:
The patellar tendons are elongated (double arrows) and there is almost no overlap between the patellar articular facets and the femoral trochlea (arrows). The findings are diagnostic for patella alta and may be confirmed using the Insall-Salvatti index or one of several other patellar height indices.
Discussion
The patella serves as an anchor point for the various soft tissue components of the extensor apparatus, which allows balance of the opposing forces at the knee. By shifting the plane of the extensors anterior to the central axis of flexion and extension of the knee, extension is facilitated and the force of extension is increased. The hyaline cartilage of the patellofemoral articulation also functions to minimize friction during the transmission of the force of the quadriceps mechanism across the knee joint. The vertical position of the patella relative to the femoral trochlea is recognized as an important element of normal knee function. In relaxed extension the inferior pole of the patella is located within the superior margin of the femoral trochlear groove but not fully engaged with the trochlea and with no compressive force acting across the patellofemoral joint. As flexion begins initial contact occurs between the distal, lateral edge of the patellar articular surface and with increasing flexion the area of contact between the patella and femur increases in area and moves superiorly and medially so that at full flexion (1200) the medial facet contacts the lateral margin of the medial femoral trochlea. Normally the patella is fully engaged with the trochlea by 200 of flexion. In patella alta, the patella is abnormally elevated relative to the femoral trochlea and engagement occurs later in flexion with the contact area between the patella and trochlea diminished. This predisposes to tracking abnormalities and instability. In patella alta, the patellofemoral contact area has been suggested to be on average 19% less than normal17. Elevation of the patella by 8mm can result in as much as a 25% increase in magnitude of contact force across the patellofemoral articulation18. This increase in compressive force with diminished contact area across the articulation results in abnormal stress on the articular cartilage, predisposing to chondromalacia and patellofemoral osteoarthrosis. Patella alta has been associated with a number of disorders of the knee, with patellofemoral instability and recurrent patellofemoral dislocation among the strongest associations2,3,5,6,7,8. The association between patella alta and chondromalacia patella has been subject to debate with most investigators demonstrating a positive association2,3,6,8,9,10 though others have been unable to document a positive correlation11,12,19,20. Patella alta has also been linked with other entities, including neuromuscular disease such as poliomyelitis, Osgood Schlatter disease, Sinding Larsen Johanssen disease and patellar tendon-lateral femoral condyle friction syndrome1,2,8,13.
Patella baja (patella infera) refers to an abnormal inferior location of the patella relative to the femoral trochlea with the patella remaining engaged within the trochlear groove in full knee extension1,2,3,4. Patella baja occasionally is seen in otherwise normal individuals and is common in achondroplasia1. In most instances patella baja is not associated with functional abnormality. Patella baja has been described in association with Osgood Schlatter disease but it is unclear whether the association is cause or effect2,9. Secondary patella baja is an occasional surgical complication occurring in tibial tubercle transfers in young patients1, in patients with total knee arthroplasty16, and in association with scarring and contracture of the anterior soft tissues and patellar tendon entrapment14,15. Treatment, in most instances, is not directed primarily at patella alta or patella baja, but rather at associated abnormalities such as chondromalacia or instability. Surgical tibial tubercle transfers, in addition to shifting the patellar tendon insertion to correct the Q angle may also correct patella alta and baja by shifting the point of insertion proximally or distally3,14,15. Arthroscopic debridement with our without osteotomy has been recommended for infrapatellar contracture symdrome14,15.
A number of radiographic techniques have been developed for the evaluation of patellar height. These include the Insall-Salvatti Index21, the Modified Insall-Salvatti Index22,23, the morphology index23, Boon-Itt’s formula26, Blumensaat’s Method27, Blackburn-Peel Ratio24, de Carvahlo’s Index28, Caton-Deschamps Index25, Vertical height of Norman29, Linclau Measurement30, Patellotrochlear ratio31, Patellophyseal31 ratio, and patellar articular surface physeal height ratio32. These methods vary in complexity from a complex geometric formula using nomograms (Boon-Itt) to a simple line extended from the roof of the intercondylar notch on a lateral radiograph of the knee in 30 degrees of flexion (Blumensaat). The Insall-Salvatti, Modified Insall-Salvatti, Blackburn-Peel and Caton-Deschamps have been the most commonly used radiographic techniques (Fig 3a-3d) for evaluation of patellar height (Table 1). All are measured on lateral radiographs of the knee obtained in 30° of flexion.
Figure 3:
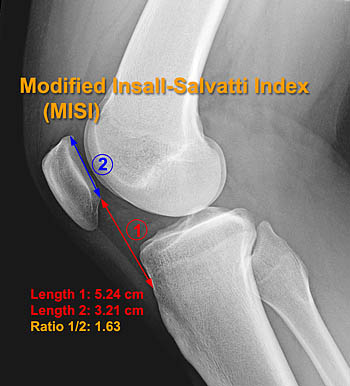
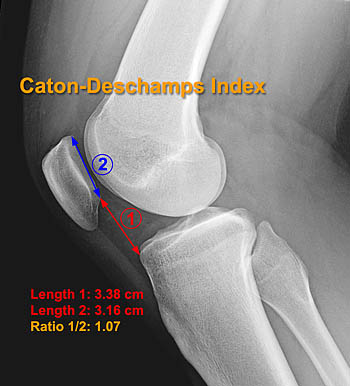
Radiographic Evaluation of Patella Alta and Baja. Lateral radiographs of the knee in 30° of flexion demonstrate the measurements for the Insall-Salvatti Index (A), Modified Insall-Salvatti Index (B), Caton-Deschamps Index (C) and Blackburn-Peel Index (D) Normal values for these measurements are listed in Table 1.
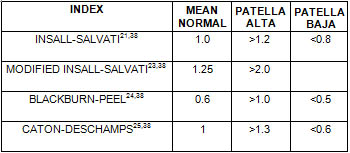
TABLE 1
RADIOGRAPHIC EVALUATION OF PATELLAR HEIGHT*
*All obtained on lateral knee radiograph in 30° flexion.
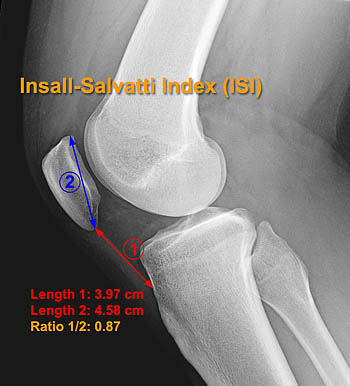
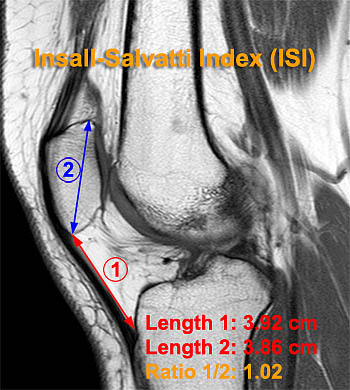
The most widely accepted and utilized method of evaluating patellar height has been the Insall-Salvatti Index (ISI)21 (Fig 3a). This method involves a simple ratio between the length of the patellar tendon (TL) and the maximum vertical length of the patella (PL). Evaluation is performed on a lateral radiograph of the knee in 30° of flexion. TL is obtained by measuring the length of the inner border of the patellar tendon from the lower pole of the patella to the notch in the tibial cortex at the superior border of the tibial tubercle. PL is measured as an oblique line connecting the inner margin of the upper pole of the patella with the most inferior point of the lower pole. In the ISI normal is defined as 1.0 +/-20%. Thus Patella baja is defined as an ISI value of <0.8, patella alta as> 1.2 and the normal range is between .8 and 1.2. Other authors, including Miller31, Kannus6, Schlenzka and Schwesinger, and Grelsamer22 have substantiated these values.
Using a formula based on the Morphology Index (Vertical length of the patella/length of the patellar articular surface) Gelsamer et al22,23 identified three variations involving the length of the articular surface of the patella and the shape of the lower pole of the patella which introduce error in the Insall-Salvatti Index (Fig 4a-4c) . Type I (85%) (Fig 4a) has an articular surface of normal length with typical rounded lower pole and yields accurate ISI measurements. Type II (11%)(Fig 4b) has an abbreviated articular surface length and an elongated lower pole (Cyrano Nose) understates patella alta while overstating patella baja in ISI measurements. Type III (4%) (Fig 4c) has a normal length articular surface with a flattened lower pole with patella alta overstated and patella baja understated in ISI measurements. These authors suggested the Modified Insall-Salvatti Index (MISI) to be used in conjunction with the ISI in patients with unusual patellar shapes or old fractures or Sinding Larsen Johansson disease where the lower pole of the patella is abnormal or difficult to evaluate.
Figure 4:
The shape of the lower pole of the patella and length of the patellar articular facets should be considered in evaluating patella alta and baja. The three types described by Gelsamer24 are Type I (4a) with the typical rounded lower pole (red arrow) and normal length patellar facets (blue arrow), Type II with an elongated patellar nose (Cyrano nose) (red arrow) and variable abbreviation of the length of the articular facet (blue arrow) (4b), and Type III with a flattened and truncated lower pole (red arrow) and a normal length articular facet (blue arrow) (4c).
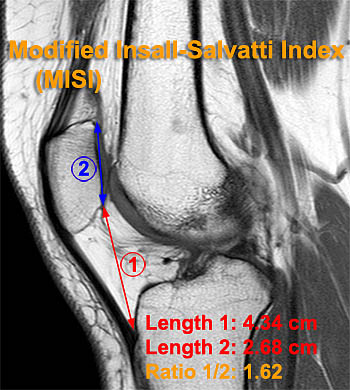
The Modified Insall-Salvatti Index (MISI) (Fig 3b) utilizes the Length of the patellar tendon TL divided by the length of the articular surface of the patella (PC) in order to avoid inaccuracies associated with the variability in shape of the lower pole of the patella. A MISI value of >2 being indicative of patella baja. The authors recommended that the MISI be used in conjunction with the ISI and that its primary value is in identifying cases of patella alta in which the ISI is in question. With either method there can be a problem in patients with Osgood Schlatter disease in which it is difficult to identify the patellar tendon insertion. In these instances the Blackburn-Peel ratio (Fig 3d), Caton-Deschamps index (Fig 3c), and de Carvalho’s index have been recommended as alternatives for radiographic evaluation. The Blackburn-Peel ratio measures the ratio of a measurement of the shortest distance between the inferior margin of the patellar articular surface and a line extended parallel to the proximal tibial articular surface (TA) and the length of the patellar articular surface (PC). The mean normal Blackburne-Peel ratio (TA/PC) is 0.8 with patella alta defined as > 1.0. The Caton-Deschamps Index uses the length between the inferior articular surface of the patella and the anterior lip of the tibial plateau while de Carvalho’s index is similar to the Caton-Deschamps index but replaces the denominator with the shortest length between the inferior margin of the patellar articular cartilage and the closest point on the anterior margin of the tibial plateau. These methods share the advantage of being independent of the shape of the lower pole of the patella and the vagaries of identification the patellar tendon insertion but are all easily obscured by arthritic or post-traumatic change of the patella and femorotibial articulation. Caton-Deschamps and de Carvalho’s indices can be applied easily to MRI but the Blackburn-Peel ratio is difficult, requiring measurements across different sections. As with the ISI and MISI they share the measuring of patellar height relative to the tibia rather than the femoral trochlea, which is the site of actual abnormality in patella alta.
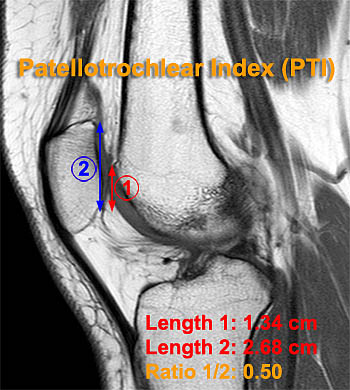
MRI (Fig 5a-5d) provides a new way to more precisely evaluate abnormalities of patellar height since most of the existing methods can be duplicated and direct visualization of patellar and trochlear cartilage is provided. Miller32, Shabshin34, and Ali31 have evaluated patellar height by MRI. Miller found a mean ISI of 1.1 with SD = 0.1 and defined Patella alta as > 1.3 and patella baja as > 0.9 and noted a good correlation with the radiographic ISI. Miller also measured the patellar articular surface physeal height ratio in which the height of the patellar articular cartilage was compared to the length of the patellar cartilage below the anterior margin of the physeal scar and found only fair correlation with the ISI. Shabshin34 found mean ISI to be 1.05 with a range of 0.56 to 1.71 and SD of 0.18 but noted a prominent skew in the histogram of distribution of TL/PT ratios toward higher ratios. They concluded that patella alta would be over called and patella baja under called if the typical ISI rule was used (>1.41 and <.69) and instead included 95% of the values in the normal range with the outer 2.5% defining patella alta (>1.5) and patella baja (<.74). They postulated the discrepancies between the MRI and radiographic ISI related to obliquity of the true long axis of the patella which slightly decrease the value in single sagittal MRI images and indirect measurement of the patellar tendon on radiographs which may introduce error into the measurement. Ali et al. measured the ISI, MISI and patellotrochlear and patellophyseal ratios on 103 consecutive patients with exclusion of patients with previous surgery, bipartite patella and prior patellar fractures. The patellotrochlear index (Fig 5c) was calculated as the ratio between the length of the patellar articular cartilage (PC) and the length of the overlap of trochlear and patellar cartilage (TC). The patellophyseal index (Fig 5d) used the reverse of the measurement used by Miller32 comparing PC to the length of the patellar cartilage above the level of the physeal scar (PHY). The mean values for each of these ratios was identified and patella alta and patella baja assigned to values +/- 2 SD above and below the mean. Values for ISI, MISI, PTI and PPI are summarized in Table 2.
Figure 5:
MRI methods for evaluation of patella alta and baja. The Insall-Salvatti Index (5a) and Modified Insall-Salvatti Index (5b) are measured the same way on MRI studies as on plain radiographs. Two additional methods providing more direct correlation between the patellar articular facet and femoral trochlea are the patellotrochlear Index (5c) and the patellophyseal Index. Normal values for these measurements are provided in Table 2.
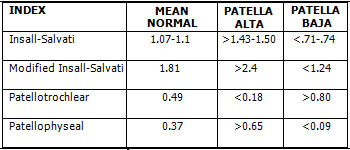
Table 2
MRI Values of Patellar Height Indices*
* from Shabshin31 and Ali34
Other studies have used MRI in patella alta. Stefanik et. al35 and Kalichman et.al36 demonstrated correlation between chondromalacia and osteophytosis in the patellofemoral compartments and increasing ISI. The correlation was much more pronounced in the lateral patellofemoral compartment than in the medial compartment. Escala et.al.37 evaluated 46 patients with clinically proven Objective Patellar Instability (OPI) which was defined as documented prior patellar dislocations or convincing clinical history with appropriate mechanism for dislocation.. Multiple parameters were evaluated and found to be associated with OPI, including shallow trochlear groove (<5mm), larger Insall-Salvatti Index (>1.2), Shorter patellar nose (<9mm), smaller morphology ratio (<1.2), and larger patellar tilt (>110). Greater sensitivity was noted with lateral patellar tilt, trochlear groove depth and the Insall-Salvatti Index while greater specificity was identified with the morphology ratio, patellar nose length, and patellar tendon length.
The Insall-Salvatti index is the most widely accepted technique and is easily performed on radiographs and MRI examinations. Shabshin’s values seem to be reasonable for MRI examinations with patella alta >1.5 (Fig 6a & 6b) and patella baja 31 and Ali34. Evidence or history of patellofemoral instability or the presence of chondromalacia patella lend importance to the presence of patella alta. Abnormalities at the origin or insertion of the patellar tendon may diminish the value of the ISI and indicate the need for use of another method. Observation of the patellofemoral relationship is important as it is difficult to imagine patella alta in the presence of normal overlap between the patellar and trochlear articular visualized directly on a MRI. In addition to patellar trochlear overlap other observations including patellar shape, length of the patellar articular surface, the origin and insertion of the patellar tendon, and the presence of edema or scarring in the infrapatellar fat pad, chondromalacia patella and patellar subluxation represent important findings.
Figure 7:
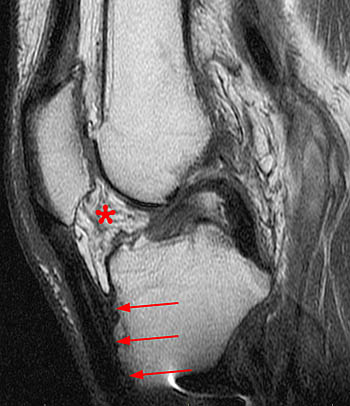
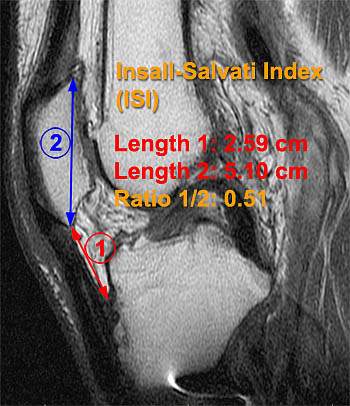
Patella Baja. Demonstration of an abnormal MRI Insall-Salvatti Index measurement on a patient with patella baja (7a). The patient in 7b and 7c is post operative tibial tubercle transfer and demonstrates thickening of the patellar tendon insertion (arrows) and scarring in the infrapatellar fat pad (asterisk) (7b) and an abnormal MRI Insall-Salvatti Index of 0.51 (7c) which is diagnostic of patella baja.
Patella baja (infera) is not typically of clinical significance and in many instances is factitious in patients with elongated patella “noses” (Fig 4b). Observation of a short patellar tendon in association with postoperative scarring in the infrapatellar fat pad may be a very important finding (Fig 7b & c).
Conclusion
In everyday practice the height of the patella is typically an “eyeball” observation and measurement of patellar height indices are not routinely obtained. If a more objective measurement is required, in most cases the Insall-Salvatti Index (ISI) is sufficient. There are instances in which the values produced by the ISI may be misleading such as with an elongated patellar “nose” or a flattened patellar lower pole. In others patients, old trauma, post-operative changes, or changes relating to Osgood Schlatter disease or Sinding-Larsen-Johansson disease may make the measurement difficult. In these instances, as well as anytime an abnormal ISI is encountered, observation of the overlap between the inferior aspect of the patella and upper femoral trochlea is useful, especially in suspected patella alta. If the patella appears well seated in the upper trochlea, patella alta is extremely unlikely and this may be confirmed with patellotrochlear or patellophyseal measurements. Likewise, if the inferior margin of the patellar facets project superior to the superior margin of the trochlea, patella alta is quite likely. The height of the patella is an observation, rather than a diagnosis, and may or may not be associated with other significant patellofemoral abnormalities. No single method of evaluation is diagnostic in every instance and the knowledge of common sources of measurement error as well as alternative measurement methods is useful when evaluation beyond the “eyeball” method is indicated.
References
1 Fulkerson JP, Hungerford DS. Disorders of the Patellofemoral Joint. 2nd ed. Baltimore: Williams & Wilkins. 1990
2 Stoller DW, Li LE, Anderson LJ, Cannon WD. The Knee in Stoller DS et al, eds. Magnetic Resonance Imaging in orthopaedics and Sports Medicine 3rd ed. Baltimore: Lippincott, Williams & Wilkins. 2007
3 Colvin AC, West RV. Patellar Instability. J Bone Joint Surg Am. 2008;90:2751-2762
4 Ward SR, Terk MR, Powers CM. Patella Alta: Association with patellofemoral alignment and changes in contact during weight-bearing. J Bone Joint Surg Am. 2007;89:1749-1755
5 Insall J, Goldberg V, Salvati E. Recurrent dislocation and the high-ridings patella. Clin Orthop Relat Res. 1972;88:67-69
6 Kannus PA. Long patellar tendon: radiographic sign of patellofemoral pain syndrome a prospective study. Radiology. 1992;185:859-863
7 Simmons E, Cameron JC. Patella alta and recurrent dislocation of the patella. Clin Orthop Relat Res. 1992;274:265-269
8 Resnick D. Degenerative Disease of Extraspinal Locations in Resnick D ed. Diagnosis of Bone and Joint Disorders. 4th ed. Philadelphia: W.B. Saunders. 2002
9 Lancourt JE, Cristini JA. Patella alta and patella infera: Their etiological role in patellar dislocation, chondromalacia and apophysitis of the tibial tubercle. J Bone Joint Surg Am. 1975;57:1112-1115
10 Stefanik JJ, Zhu Y, Zumwalt AC, Gross KD, et al. The association between patella alta and the prevalence and worsening of structural features of patellofemoral joint osteoarthritis: The multicenter osteoarthritis study. Arthritis Care and Research. 2010;999(999A);online
11 Endo Y, Schweitzer ME, Bordalo-Rodrigues M, Rokito AS, Babb JS. MRI quantitative morphologic analysis of patellofemoral region: Lack of correlation with chondromalacia patellae at surgery. AJR. 2007;189:1165-1168
12 Marks KE, Bentley G. Patella alta and chondromalacia. J Bone Joint Surg Br. 1978;60-B: 71-73
13 Chung CB, Skaf A, Roger B, Campos J, Stump X, Resnick D. Patellar tendon-lateral femoral condyle friction syndrome: MR imaging in 42 patients. Skeletal Radiol. 2001;30:694-697
14 Paulos LE, Rosenberg TD, Drawbert J, Manning J, Abbott P. Infrapatellar contracture syndrome. an unrecognized cause of knee stiffness with patella entrapment and patella infera. Am J Sports Med. 1987;15(4):331-341
15 Paulos LE, Wnorowski DE, Greenwald AE. Infrapatellar Contracture Syndrome: diagnosis, Treatment, and long-term follow-up. Am J Sports Med. 1994;22:440-449
16 Chonko DJ, Lombardi AV Jr, Berend KR. Patella baja and total knee arthroplasty (TKA): etiology, diagnosis, and management. Surg Technol Int. 2004;12:231-238
17 Ward SR, Terk MR, Powers CM. Patella alta: association with patellofemoral alignment and changes in contact area during weight-bearing. J Bone Joint Surg Am 2007;89:1749-1755
18 Singerman R, Davy DT, Goldberg VM. Effects of patella alta and infera on patellofemoral contact forces. J Biomech. 1989;27:1059-1065
19 Dowd GS, Bentley G. Radiographic assessment in patellar instability and chondromalacia patellae. J Bone Joint Surg Br. 1986;68:297-300
20 Marks KE, Bentley G. Patella alta and chondromalacia. J bone Joint Surg Br. 1978;60:71-73
21 Insall J, Salvati E. Patella position in the normal knee joint. Radiology 1971;101:101-104
22 Grelsamer RP, Proctor CS, Bazos AN. Evaluation of patellar shape in the sagittal plane: a clinical analysis. Am J Sports Med. 1994;22:61-66
23 Grelsamer RP, Meadows S. The modified Insall-Salvati ratio for assessment of patellar height. Clin Orthop. 1992;282:170-176
24 Blackburne JS, Peel TE. A new method of measuring patellar height. J Bone Joint Surg Br. 1977;59-B(2): 241-242
25 Caton J, Deschamps G. et. al. Les rotules basses: a propos de 128 observations. Rev Chir Orthop Reparatice Appar Mot. 1982;68:317-325
26 Boon-Itt SB. The Normal Position of the Patella. Radiology. 1930;24:389-394
27 Blumensaat C. Die Lagaebweichungen und Verrenkungen der kniescheibe. Ergebn Chir Ortho 1938;31:149-223
28 de Carvahlo A, Anderson AH, Topp S, Jurick AG. a Method for Assessing the height of the Patella. Int Orthop. 1985;9:195-197
29 Norman O, Egund N, Ekelund L, Runow A. The Vertical Position of the Normal Patella. Acta Orthop Scand 1983;54:908-913
30 Linclau L. Measurement of Patellar Height. Acta Orthop Belg. 1984;50:70-74
31 Ali S, Heimer R, Terk MR. Patella Alta: Lack of Correlation between patellotrochlear cartilage congruence and commonly used patellar height ratios. AJR 2009;193:1361-1366
32 Miller TT, Staron RB, Feldman F. Patellar height on sagittal MR Imaging of the knee. AJR. 1996;167:339-341
33 Schlenzka D, Swesinger G. The height of the patella: and anatomical study. Eur J Radiol. 1990;11:19-21
34 Shabshin N, Schweitzer ME, Morrison WB, Parker L. MRI criteria for patella alta and baja. skeletal Radiol 2004;33:445-450
35 Stefanik JJ, Zhu Y, Gross KD, Clancy M, Lynch JA, Frey Law LA, Lewis CE, Roemer FW, Powers CM, Guermazi A, Felson DT. The association between patella alta and the prevalence and worsening of structural features of patellofemoral joint osteoarthritis: The multicenter osteoarthritis study. Arthritis Care adn Research 2010;9999(999A)Online
36 Kalichman L, Zhang Y, Niu J, Goggins J, Gale D, Zhu Y, Felson DT, Hunter DJ. The association between patellar alignment on magnetic resonance imaging and radiographic manifestations of knee osteoarthritis. Arthritis Research & Therapy 2007;9(2)online
37 Escala JS, Mellado JM, Olona M, Gine J, Sauri A, Neyret P. Objective patellar instability: MR-based assessment of potentially associated anatomical features. Knee Surg Sports Traumatol Arthrosc. 2006;14(3):264-272
38 Berg EE, Mason SL, Lucas MJ. Patellar Height Ratios. A comparison of four measurement methods. Am J Sports Med. 1996;24(2):218-221