Clinical History: A 59 year-old female with no history of prior surgery presents with medial knee pain for 1 month.
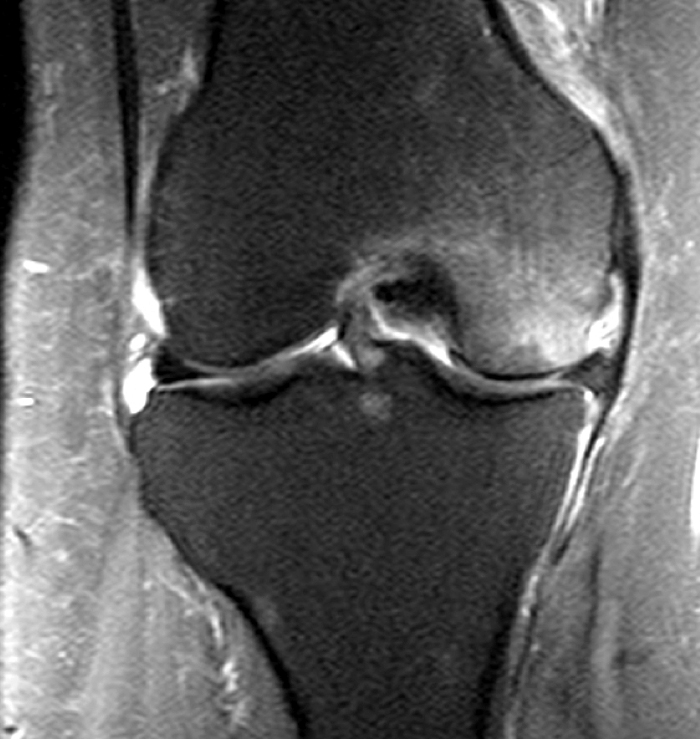
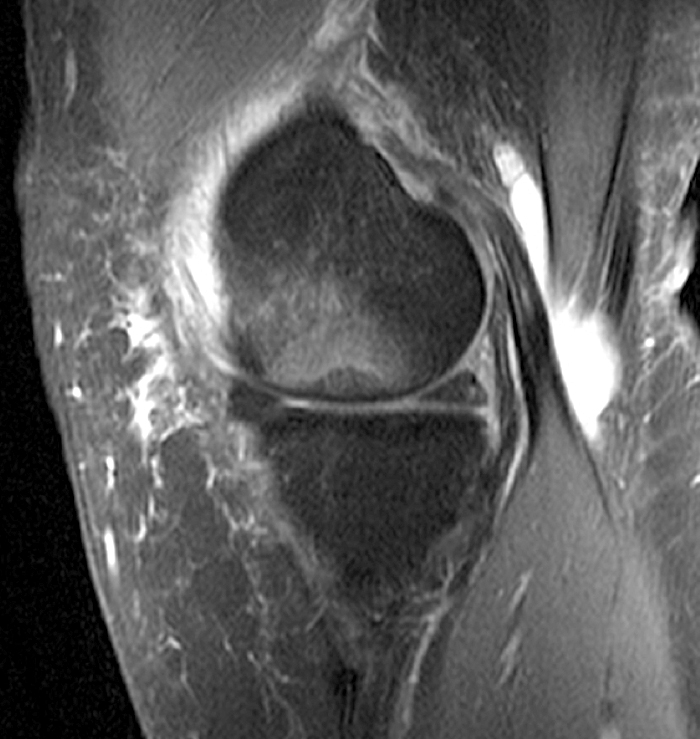
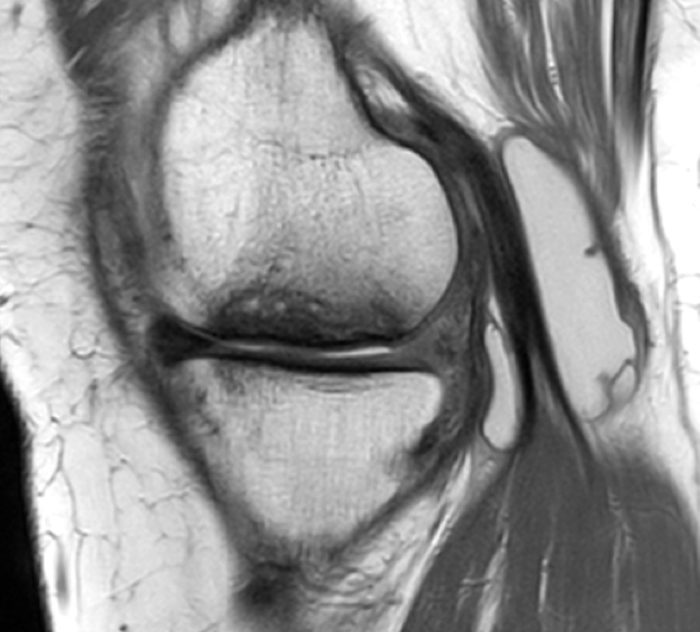
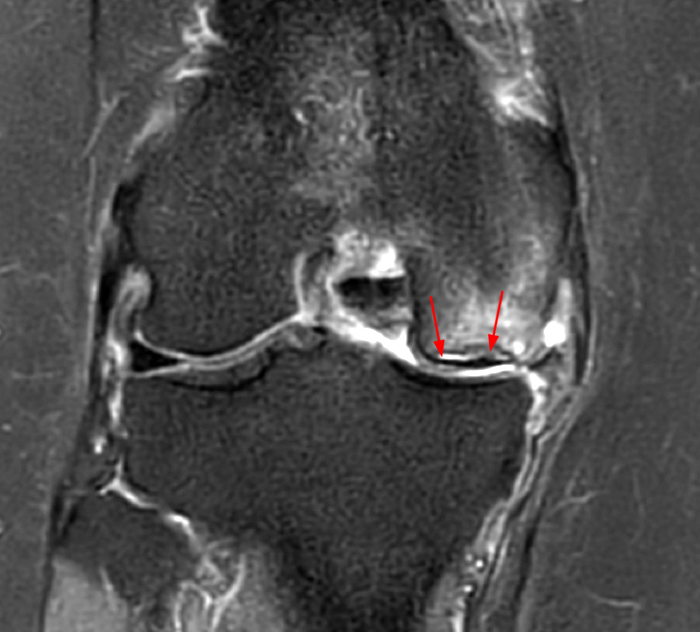
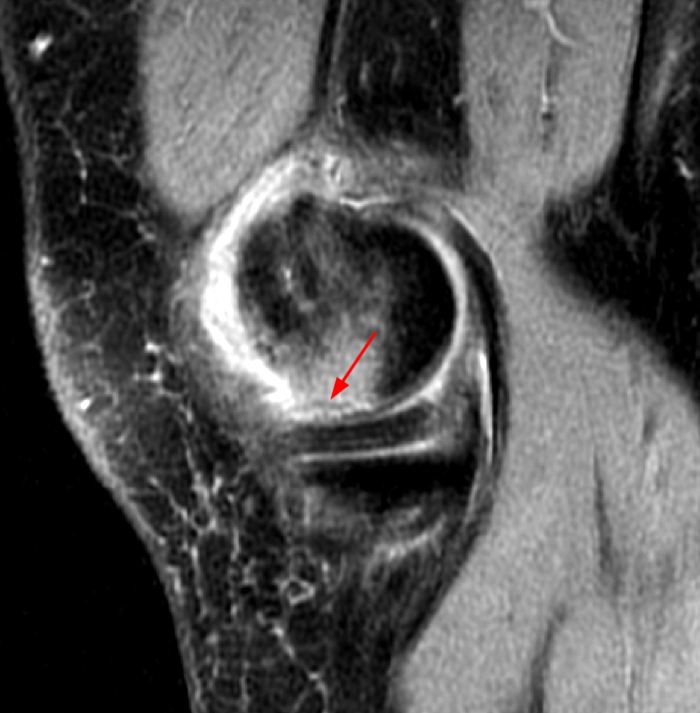
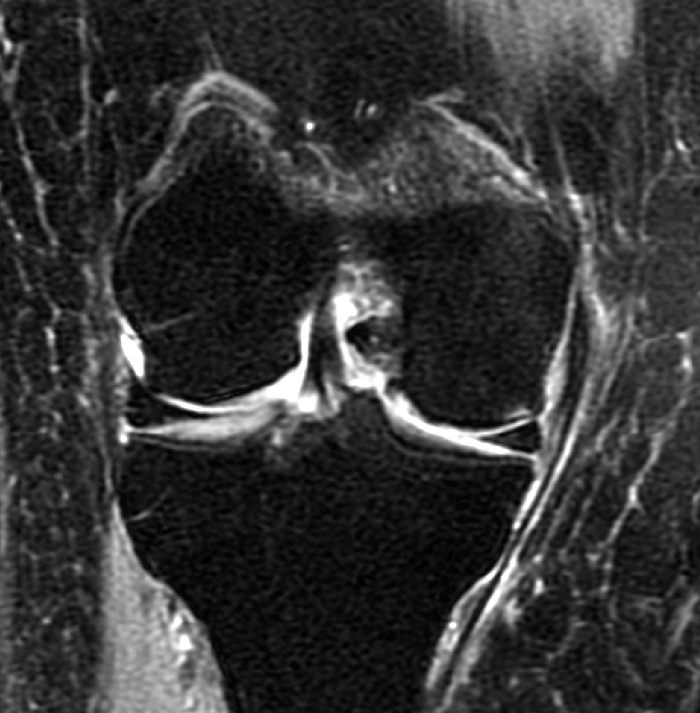
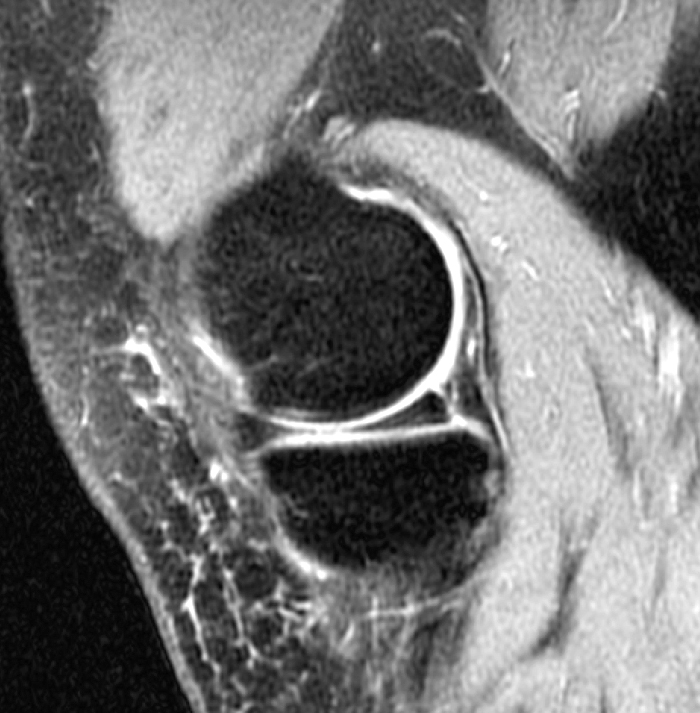
(1a,c) Coronal and (1b) sagittal fat suppressed proton density weighted MR images are submitted for review.
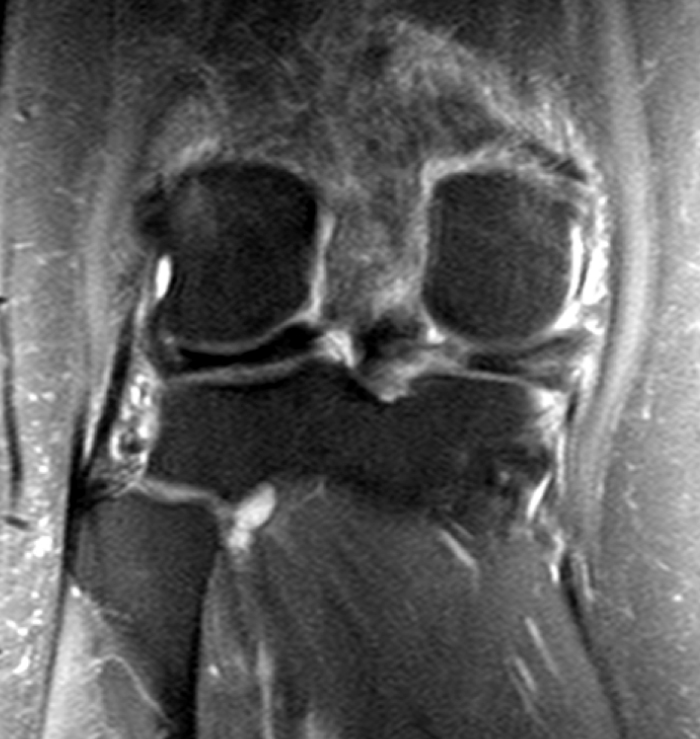
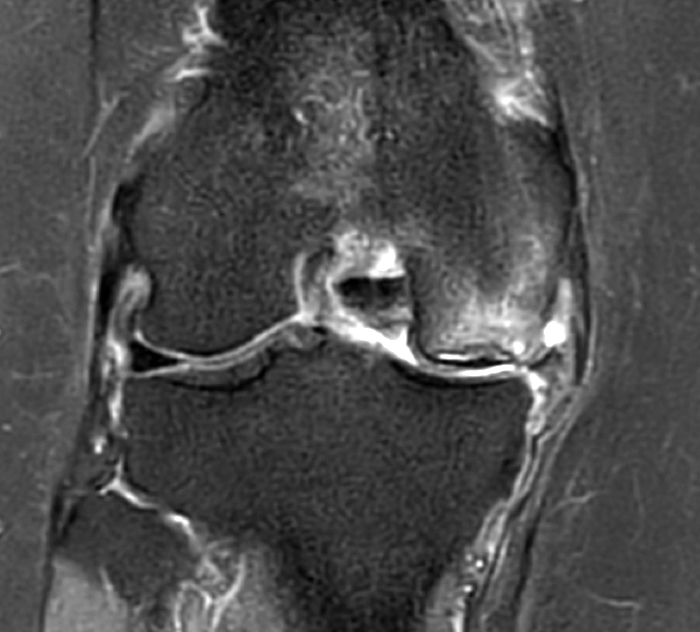
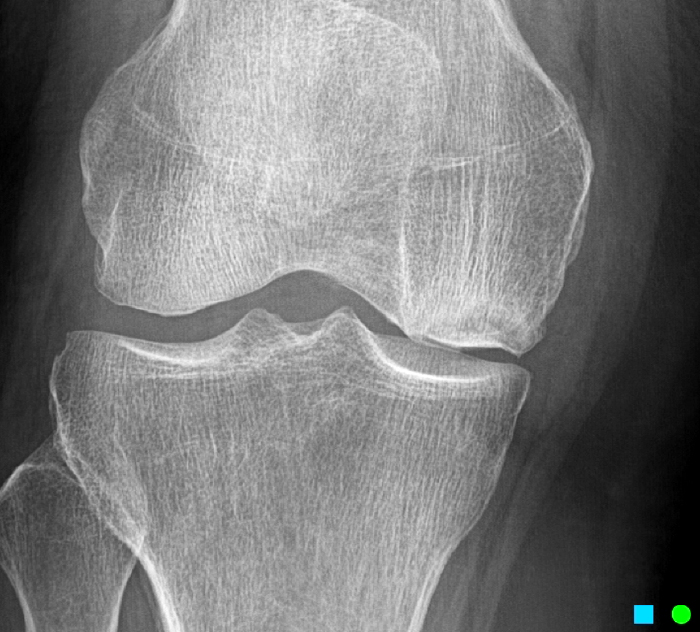
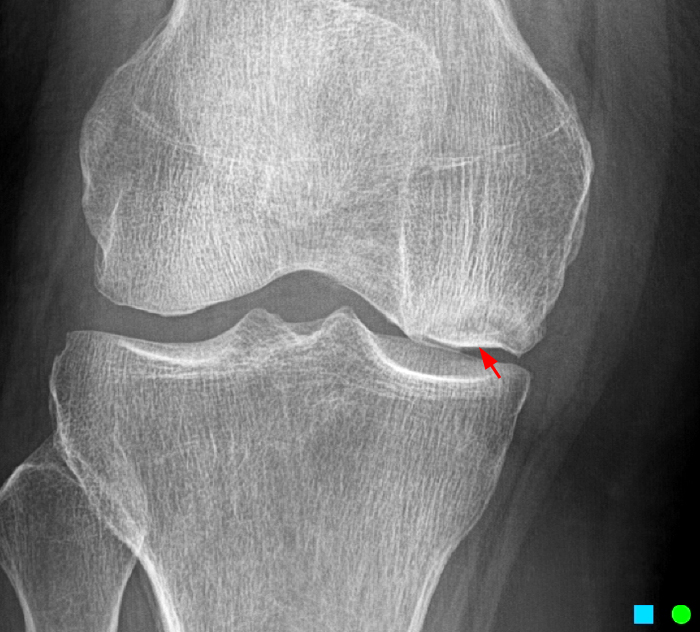
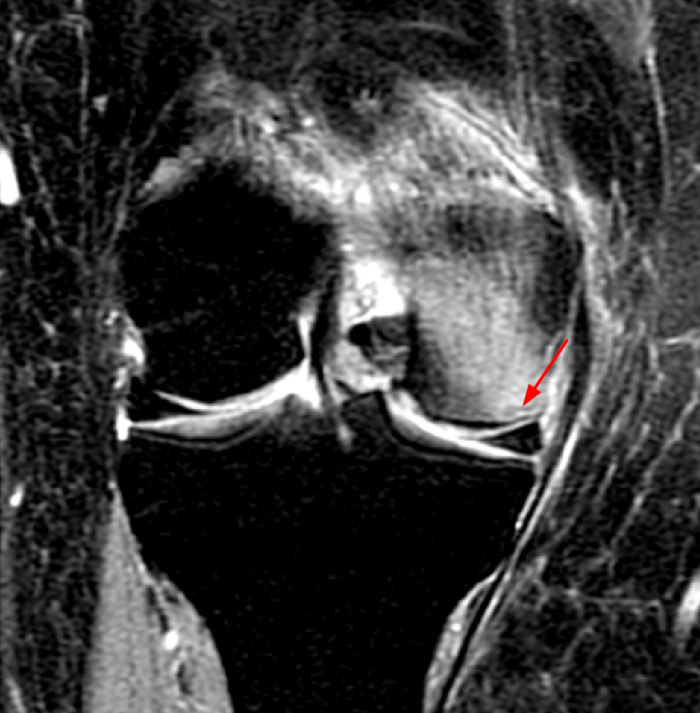
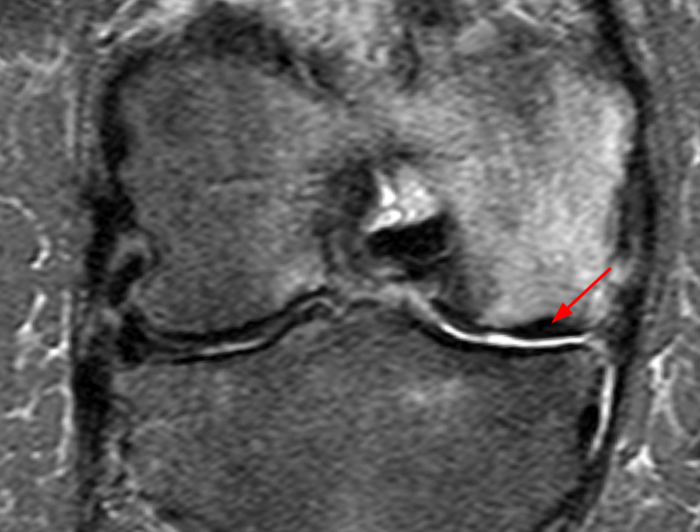
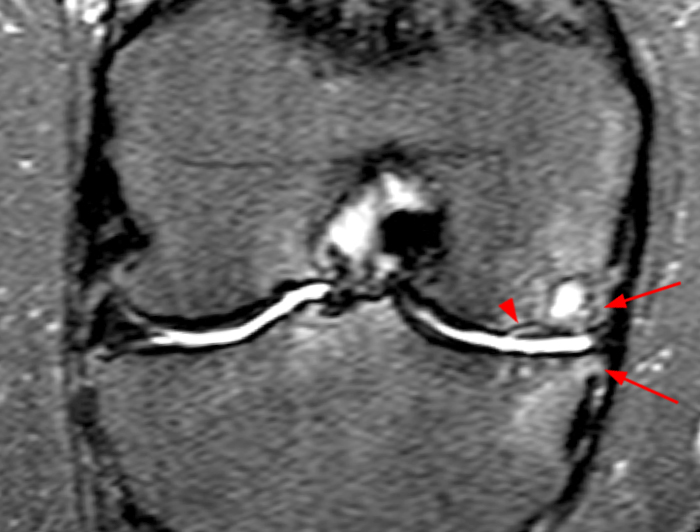
The patient had a follow up MR 4 months later, having had interval meniscal surgery. (1d) Coronal fat suppressed and (1e) sagittal non-fat suppressed proton density-weighted images are presented for review, along with an (1f) AP radiograph.
What are the findings? What is the diagnosis?
Findings
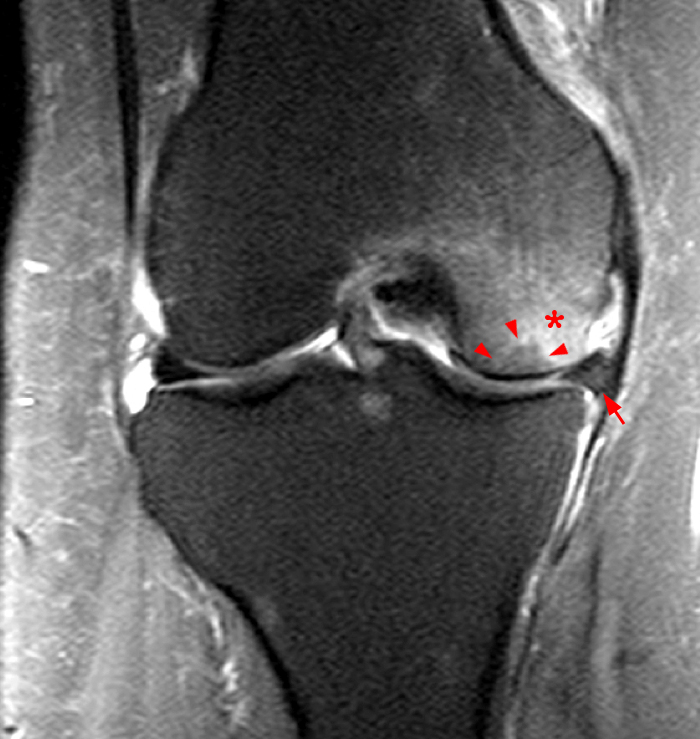
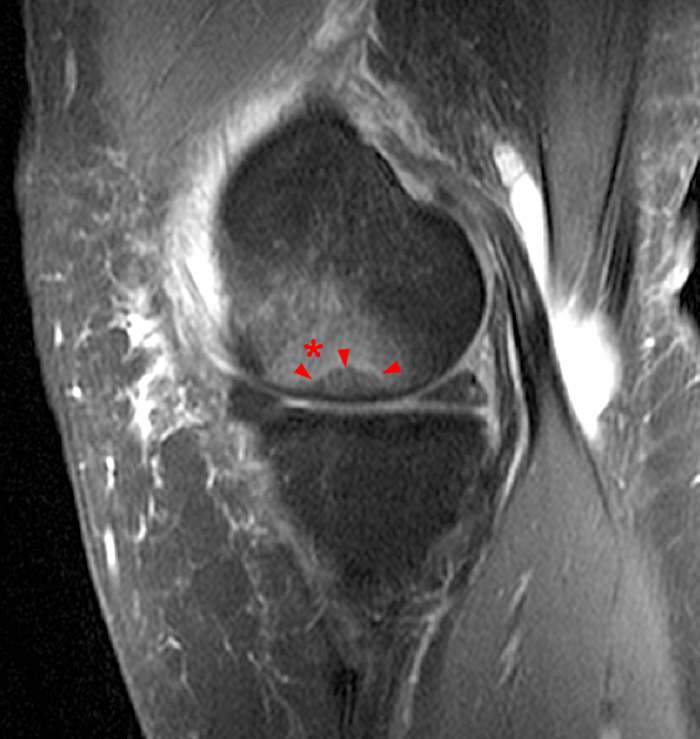
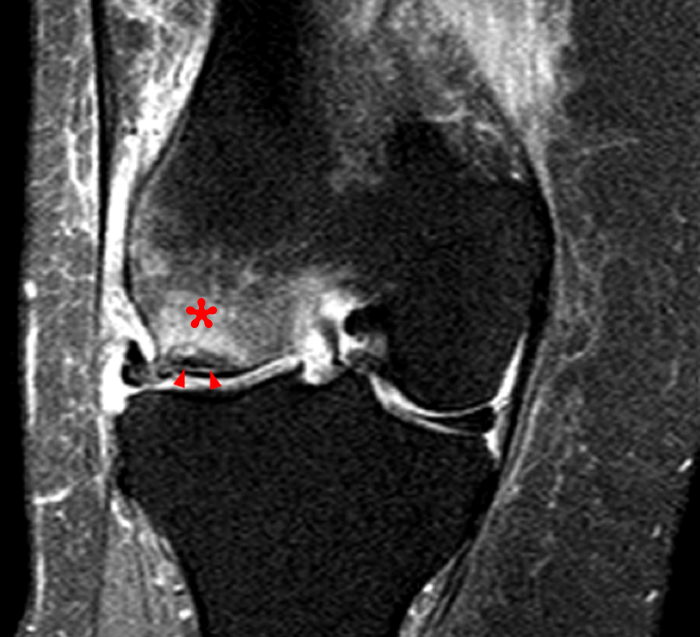
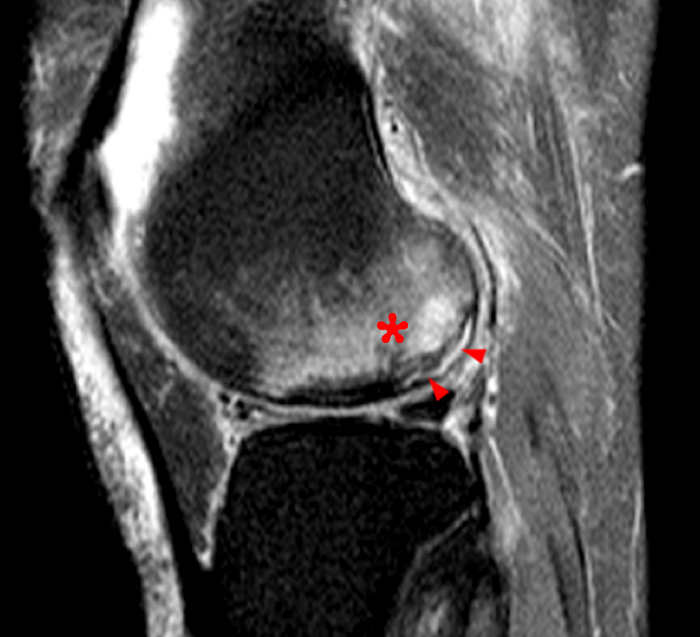
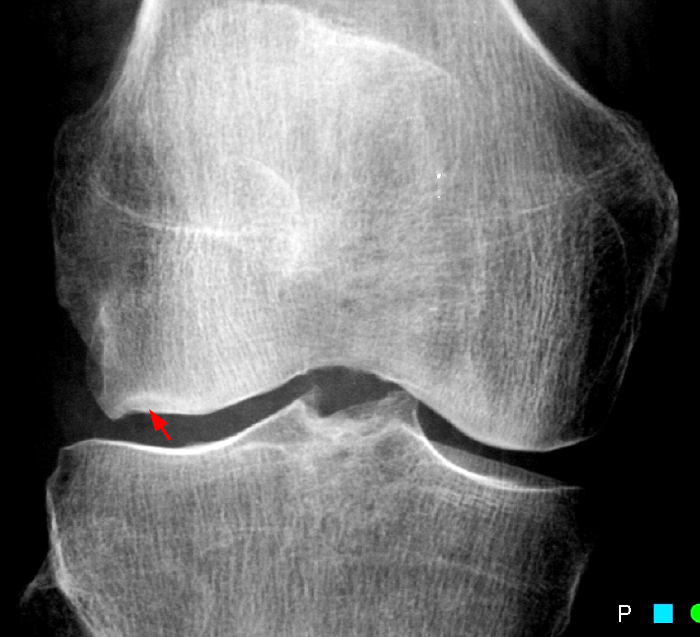
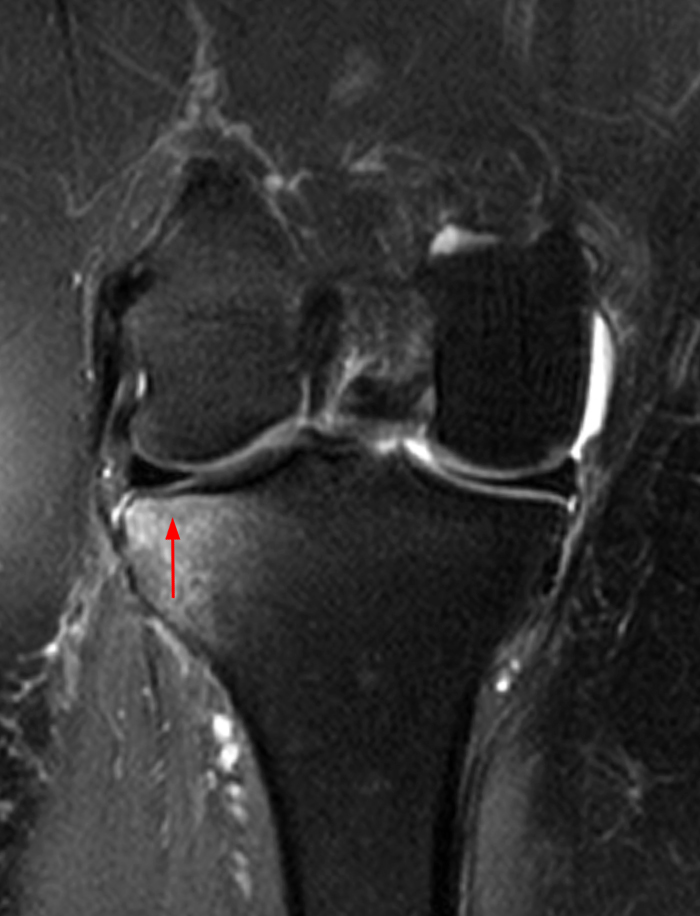
Figure 2:
The initial study (2a-c) demonstrates a crescentic subchondral fracture (arrowheads), inseparable from the subchondral bone plate, surrounded by marrow edema (asterisks), with medial extrusion of the meniscal body (short arrow). There is also a radial tear of the posterior root of the medial meniscus (arrow). The follow up MR 2 months later (2 d-f) demonstrates a fluid filled subchondral fracture (arrows 2d), and a serpentine subcortical ”double line sign” (arrowheads 2e), subcortical cysts, and cortical collapse, demonstrated on both MRI and the radiograph (short arrows).
Diagnosis
Subchondral fracture with progression to osteonecrosis.
Introduction
The index cases demonstrate a subchondral fracture, which progresses to osteonecrosis and cortical collapse. With widespread use of MR it is now not uncommon in clinical practice to observe this progression of findings. As a result, the diagnosis of “spontaneous osteonecrosis of the knee” has been abandoned and is now recognized as osteonecrosis developing following a subchondral fracture (see Web clinic February 2004). This is an important distinction, because a subchondral fracture may completely resolve and never be associated with osteonecrosis. Certain MRI findings have been linked to more favorable or unfavorable outcomes following the initial fracture, so MRI can be used to assist in guiding treatment plans which range from joint sparing conservative treatment to total joint arthroplasty.
Terminology, anatomy and pathology
Literature on osteonecrosis of the femoral condyles is often confusing due to terminology and attempts to classify etiology. What was previously referred to as spontaneous osteonecrosis of the knee (SONK) has been demonstrated to represent a subchondral fracture, with the future development of osteonecrosis being uncertain.1,2
A subchondral fracture refers to a fracture subjacent to the cortex and the subchondral bone plate, without cortical contour abnormality or disruption. An osteochondral fracture involves cartilage and the subchondral bone plate, and may demonstrate cortical disruption, cortical depression, fragmentation or a combination of these findings. Subcortical or osteochondral fractures may occur in the setting of acute trauma, often in a young athletic patient, with recognizable injury patterns, such as injury to the terminal sulcus of the lateral femoral condyle associated with ACL tears. A subchondral fracture may also be due to chronic low intensity stress. Stress fractures can further be categorized as a fatigue fracture or an insufficiency fracture. A fatigue fracture is due to abnormal stress placed on normal bone, such as training for a marathon. An insufficiency fracture refers to normal physiologic stress applied to bone with compromised ability to withstand stress, such as underlying osteoporosis. Although the literature describing osteonecrosis of the knee and femoral head commonly refers to the initial fractures as subchondral insufficiency fractures, osteoporosis is not generally a diagnosis reliably made with MRI, so these injuries are referred to as subchondral fractures in this discussion.
Osteonecrosis is a broad descriptive term which can be applied to any region of bone compromised by partial or complete loss of blood supply. Traditionally, the term avascular or ischemic necrosis has been applied to osteonecrosis occurring in epiphyseal or subchondral locations, while bone infarct has been used for metadiaphyseal locations. Etiologies of osteonecrosis are multiple, including idiopathic, post traumatic, steroids, alcoholism and collagen vascular disease. It can also be seen following meniscal surgery.3 Following an ischemic insult an area of hypervascularized granulation tissue develops in an attempt to wall off and repair the osteonecrotic segment; this hypervascularized zone is called the zone of creeping substitution. At the interface of the zone of creeping substitution with viable vascularized bone, osseous reinforcement occurs, which eventually progresses to a rim of sclerosis which is frequently serpentine in morphology. When the process occurs in the epiphysis of a weight bearing bone such as the femoral condyle, impaction forces on the reactive hypervascularized zone may cause cleavage from overlying cortex and cartilage, resulting in a subchondral fracture plane, which heralds articular collapse and irreversible injury.4
The skeleton is composed of compact cortical bone which is less porous and elastic than the underlying loose trabecular architecture of cancellous bone. Cortical bone is able to withstand more stress, especially axial loading at the end of a long bone, while cancellous bone is more able to deform in response to stress. With age, porosity of cortical bone increases, lessening its capacity to tolerate stress. Simultaneously, complex alterations in mineralization, crystal structure and bone architecture in aging/osteoporotic bone lead to decreased strength and elasticity of cancellous bone.5
Articular cartilage contains four layers: superficial, transitional, deep and calcified. The calcified layer is the transition zone, the point where cartilage adheres to bone. Just deep to the calcified cartilage zone is a layer of compact bone, the subchondral bone plate, which separates cartilage from the underlying trabeculae. It has been suggested that the subchondral bone plate and the immediately underlying trabeculae absorb most of the mechanical stresses across a joint.5
MRI findings
On MRI a subchondral fracture is best seen on T1-weighted images as linear subcortical low signal intensity. It may not be well seen on T2-weighted images unless there is trabecular impaction, which causes a low signal intensity line on both T1 and T2-weighted images. The “double line sign” on T2-weighted images is considered diagnostic of osteonecrosis. The inner increased signal intensity line represents vascularized granulation tissue and the outer low signal intensity line is due to sclerotic appositional new bone.6 The double line sign can be visible in epiphyseal or metadiaphyseal lesions and has no predictive value in and of itself for eventual outcome in cases of pre-existing osteonecrosis, which can either resolve, stabilize, or progress to cortical collapse. However, the development of the double line sign in follow up imaging of a previously uncomplicated subchondral fracture may herald the progression to irreversible damage. It is only in the relatively more recent literature of osteonecrosis of the femoral head and femoral condyles that a subchondral fracture has been recognized as a separate entity which may spontaneously resolve or progress to osteonecrosis. A fluid filled fracture line beneath the subchondral bone plate is predictive of eventual cortical collapse and is analogous to the crescent sign on radiographs.
The index case is a classic presentation of subchondral fracture of the knee, previously referred to as SONK. The typical patient is in at least the 6th decade, and typically presents with the sudden onset of unrelenting pain, with little or no antecedent trauma. It occurs more frequently in females, and the medial femoral condyle is the most common location, due to a more limited intraosseous blood supply, with watershed areas, as opposed to the lateral femoral condyle.7 Subchondral fractures also occur in the lateral femoral condyle or tibial plateau. On MRI a subchondral fracture appears as linear low signal intensity in the subchondral region representing subchondral fracture callus and granulation tissue, surrounded by extensive marrow edema.6 The fracture may appear as linear, thin and often discontinuous within the medullary cavity, curvilinear or paralleling the articular surface, representing fracture callus and granulation tissue. Alternatively, it may be thick and crescentic, in continuity with the articular surface, causing apparent “thickening” of the low signal intensity subchondral bone plate, felt to be callus and granulation tissue with secondary osteonecrosis between the fracture line and the articular surface.6 Differences in morphology and thickness of the fracture line have been linked to the likelihood of resolution or progression of the initial fracture to osteonecrosis. Similarly, literature on osteonecrosis of the femoral head also describes the shape of the subchondral low signal intensity line as a useful tool to differentiate subchondral fracture from osteonecrosis. A linear discontinuous line paralleling or convex to the femoral head articular surface is considered indicative of fracture, while a concave line circumscribing a crescentic necrotic segment is indicative of osteonecrosis.8 Therefore, the amount of viable bone remaining between the low signal intensity line and the cortex seems to be a critical factor in whether a lesion will resolve or progress. One study suggested that subchondral fracture lines greater than 4mm in depth transverse and over 14mm AP were associated with a poor prognosis.9 Other investigators demonstrated that lesions greater than 50% of the transverse width of the femoral condyle are associated with poor outcomes.10 More recently it has been demonstrated that the most important finding of a fracture likely to progress to irreversible osteonecrosis is a measurement of the fracture line greater than 26mm combined AP, transverse and depth, with individual measurements of AP>16.5mm and transverse >10.5mm.7 While the extent of marrow edema was not found to be significant in an earlier study,8 marrow edema involving 75-100% of the medial femoral condyle was associated with poor outcomes in another study.7
Subchondral fractures are correlated with meniscus tears, especially radial tears6 and tears of the posterior root of the medial meniscus, since such tears diminish the ability of the meniscus to withstand hoop stress, resulting in increased axial loading across the articular surfaces.7 Full thickness chondral loss in the compartment with the fracture, and degree of medial extrusion of the medial meniscal body (>5mm measured from the medial tibial cortex to the mid central portion of the medial meniscal body), are both associated with subchondral fractures not likely to resolve.7 The presence of a fluid -filled subchondral fracture or development of a double line sign with cystic changes or cortical collapse were all indicative of irreversible or high grade lesions.6,7 One staging system for subchondral fractures was proposed based on the modified Ficat and Arlet system for avascular necrosis of the hip, but it was based on x-ray which is not sensitive to early stage disease.11 A recent study has offered a grading system for subchondral fractures based on MR, with grade 1 and 2 as low grade lesions, reversible with conservative treatment, while grade 3 and 4 are high grade requiring surgery.7 Grade I is somewhat controversial, since it is described as marrow edema alone. Grade 2 is marrow edema with a low signal intensity subchondral fracture line, Grade 3 findings include fluid filled subchondral fracture lines and cystic changes, and Grade 4 refers to subchondral collapse with cortical step off.7
The index case has several findings associated with progression to osteonecrosis. The lesion measures 10mm transverse x 15mm AP x 5mm in depth, totaling 30, greater than the maximal cut off of 26mm. There is also significant chondral loss, a posterior root medial meniscus tear, and medial extrusion of the meniscal body >5mm. The follow up MR demonstrated progression to a Grade 4 lesion, with a fluid filled subchondral fracture and cortical collapse.
Figure 3 demonstrates a low grade subchondral fracture of the medial femoral condyle. The fracture line measures 6mm transverse by 10mm AP by 1mm in thickness, well below the 26mm combined measurement suggestive of irreversible injury. Although extensive marrow edema is present, there is only mild to moderate chondromalacia at the medial femoral condyle, and no meniscal tear. The patient returned 9 weeks later with only a tiny residual signal abnormality at the site of the previous fracture.
Figure 3:
(3a,b) A thin subcortical low signal intensity fracture line surrounded by extensive marrow edema (arrows) is seen subjacent to mild-moderate thinning and fissuring of cartilage at the medial femoral condyle on fat-suppressed proton density-weighted coronal (3a) and sagittal (3b) images.
(3c,d) At follow up 9 weeks later, only a thin line of subchondral marrow edema remains in the area of the original fracture.
The patient in figure 4 is a 69 year-old female with a subchondral fracture measuring 11mm transverse by 18mm AP by 3mm in depth (4a,b). She also has full thickness chondral loss and complex degenerative tearing of the posterior horn and body of the medial meniscus, with truncation of the free edge of the meniscus, a radial tear of the posterior root of the medial meniscus (not shown), and medial extrusion of the meniscal body. Although this is technically a grade 2 lesion, its size is predictive of poor outcome, as is the type of meniscal tear and extent of chondromalacia. The patient underwent partial meniscectomy and 2 years later presented with a grade 3 lesion (4c), demonstrating subcortical cysts, and a fluid filled subchondral fracture line, along with extensive degenerative changes of the apposing surface of the tibia.
Figure 4:
Figure 4a,b: Coronal (4a) and sagittal (4b) STIR images at initial presentation with thick subchondral fracture (arrow), extensive marrow edema, full thickness chondral loss, and medial extrusion of the medial meniscal body.
Figure 4c: A two year follow up demonstrates a fluid filled subchondral fracture (arrowhead), subcortical cysts and new degenerative bony changes at the medial tibial plateau (arrows).
The patient in figure 5 is a 66 year-old female who presented with pain, r/o meniscus tear 3 weeks following a fall.
Figure 5:
Figure 5: Subchondral fracture (arrowheads a,b) with double line sign and marrow edema (asterisk a,b). Coronal (5a) and sagittal (5b) fat-suppressed proton density weighted images demonstrate a large subchondral fracture of the lateral femoral condyle (arrowheads) with a double line sign indicating osteonecrosis, and cortical depression (short arrow) most easily appreciated on x-ray (5c). This constellation of findings is consistent with a grade 4 lesion.
Treatment
For low grade fractures, without evidence for osteonecrosis, a fluid filled fracture line or cortical collapse, conservative treatment is recommended, consisting of NSAIDs and restricted weight bearing (toe touch weight bearing only). Additional medical therapy can also include administration of prostaglandin I-1 and biphosphonates. Biphosphonates bind to bone which is internalized by osteoclasts, whereupon the drug interferes with cellular metabolism of the osteoclasts, and so diminishes bone resorption.11 Traditionally, conservative therapy is continued for 3 months, but it has been demonstrated that in reversible cases of subchondral fracture, bone marrow edema required an average of 5 months to resolve,7 so a longer period of conservative treatment and observation may be preferable.
Joint preserving surgical procedures include core decompression, drilling, microfracture, or osteochondral grafting. High tibial osteotomy has also been utilized to decrease load upon the affected femoral condyle, with favorable outcomes.12 Subchondroplasty is a technique indicated for treatment of early subchondral fractures or stress related marrow edema associated with osteoarthritis and involves the injection of synthetic calcium phosphate into the trabecular space, providing mechanical support.13 Figure 6 demonstrates pre and post-operative images of a subchondral fracture of the lateral tibial plateau treated with subchondroplasty.
High grade lesions, which demonstrate cortical collapse and/or fluid filled fracture lines will eventually require arthroplasty. Depending upon the degree of osteoarthritis, unicompartmental or total knee arthroplasty are indicated.
Conclusion
Subchondral fractures are commonly encountered on MR studies. It has now been accepted that the previous diagnosis of “spontaneous osteonecrosis of the knee” (SONK) was a misnomer, and that, in fact, the clinical presentation of sudden onset of unrelenting pain in an older patient with underlying osteoporosis or osteoarthritis is typically a subchondral fracture. Such fractures present with varying grades of severity and may or may not progress to osteonecrosis. Previous attempts to stage subchondral fractures with radiographs were of limited utility, since they were not sensitive to early stage disease. MRI is able to detect and characterize low grade lesions, as well as evaluate co-existing meniscal tears and chondromalacia, which also have a bearing on prognosis. Although MRI cannot always predict outcomes, it is important for the MR radiologist to recognize and report findings which have been proven to be associated with reversible or irreversible injury.
The most reliable finding for predicting progression of an early stage subchondral fracture to irreversible osteonecrosis and cortical collapse is the size of the lesion (total AP, transverse and depth measuring >26mm). Radial tears and posterior root medial meniscal tears are highly associated with subchondral fractures, and the combination of these tears with advanced chondromalacia is often associated with a poor outcome. MR can identify early stage lesions which have a good chance of resolving with restricted weight bearing and medical therapy. Once fluid filled fracture lines or frank cortical collapse are evident, surgical treatment is indicated. MR can be used to guide the surgical approach, ranging from joint preserving techniques to total knee arthroplasty.
References
- Kidwai AS, Hemphill SD, Griffiths HJ. Radiologic case study spontaneous osteonecrosis of the knee reclassified as insufficiency fracture. orthopaedics 2005 Mar,28(3):236, 333-6. ↩
- YamamotoT, Bullough PG.Spontaneous osteonecrosis of the knee: the result of subchondral insufficiency fracture. J Bone Joint Surg Am. 2000;82(6):858–66. ↩
- Brahme SK, Fox JM, Ferkel RD, Friedman MJ, Flannigan BD, Resnick DL. Osteonecrosis of the knee after arthroscopic surgery: diagnosis with MR imaging. Radiology 1991;178(3):851–853. 27. ↩
- Murphey MD, Foreman KL, Klassen-Fischer MK, Fox MG, Chung EM, Kransdorf MJ. Imaging of osteonecrosis: radiologic-pathologic correlation. RadioGraphics2014;34(4):1003–1028. ↩
- Pathria MN, Chung CB, Resnick DL. Acute and stress-related injuries of bone and cartilage: pertinent anatomy, basic biomechanics, and imaging perspective. Radiology. 2016;280(1):21–38. ↩
- Gorbachova T, Melenevsky Y, Cohen M, Cerniglia BW. Osteochondral lesions of the knee: differentiating the most common entities at MRI. Radiographics. 2018;38(5):1478–95. ↩
- Sayyid, S., Younan, Y., Sharma, G. et al. Subchondral insufficiency fracture of the knee: grading, risk factors, and outcome. Skeletal Radiol (2019). https://doi.org/10.1007/s00256-019-03245-6. ↩
- Ikemura S, Yamamoto T, Motomura G, et al. MRI Evaluation of Collapsed Femoral Heads in Patients 60 Years Old or Older: Differentiation of Subchondral Insufficiency Fracture From Osteonecrosis of the Femoral Head. American Journal of Roentgenology 2010 195: 1,W63-W68. ↩
- Lecouvet FE, van de Berg BC, Maldague BE et al. Early irreversible osteonecrosis versus transient lesions of the femoral condyles: prognostic value of subchondral bone and marrow changes on MR imaging. AJR Am J Roentgenol 1998;170(1):71–77. ↩
- Norman A, Baker ND. Spontaneous osteonecrosis of the knee and medial meniscal tears. Radiology. 1978;129:653–6. https://doi.org/ 10.1148/129.3.653. ↩
- Mont MA, Marker DR, Zywiel MG, Carrino JA (2011) Osteonecrosis of the knee and related conditions. J Am Acad Orthop Surg 19: 482-494. 37. ↩
- Karim AR, Cherian JJ, Jauregui JJ, Pierce T, Mont MA. Osteonecrosis of the knee: review. Ann Transl Med 2015;3(1):6. Doi 10.3978/j.issn.2305-5839.2014.11.13. ↩
- Christoph A. Agten, Daniel J. Kaplan, Laith M. Jazrawi, and Christopher J. Burke. Subchondroplasty: What the Radiologist Needs to Know. American Journal of Roentgenology 2016 207:6, 1257-1262 ↩