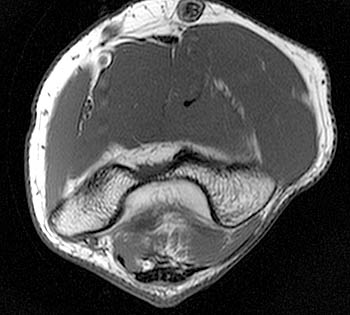
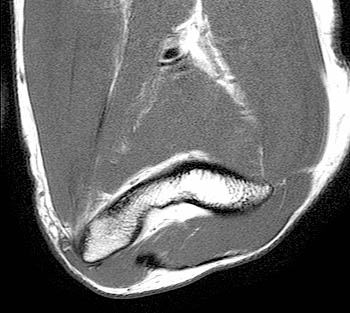
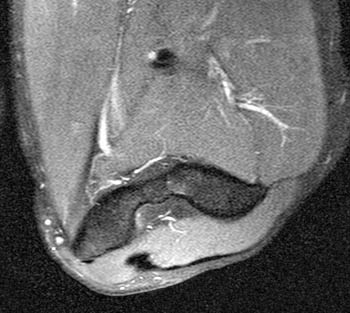
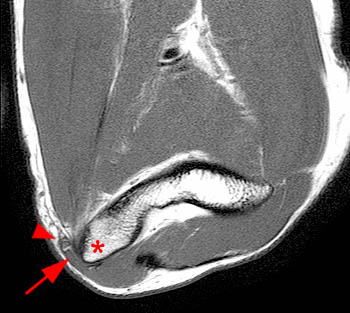
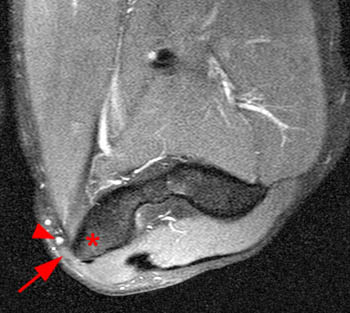
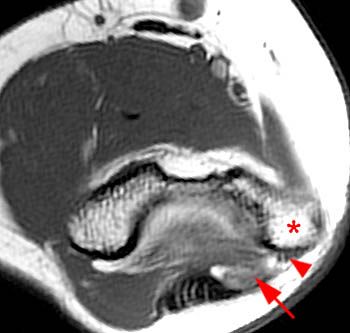
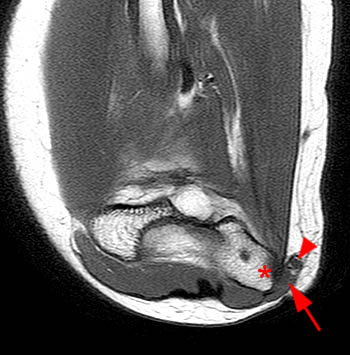
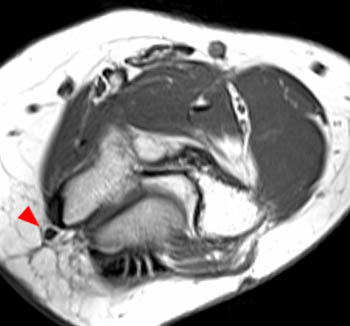
Clinical History: A 19 year-old male presents with numbness and tingling in the ring and small fingers, tenderness to palpation over the cubital tunnel, subluxation of the ulnar nerve with elbow flexion, and medial elbow snapping. (1a) Axial T1-weighted magnetic resonance (MR) image in elbow extension, (1b) axial T1-weighted MR image in elbow flexion, and (1c) axial fat-suppressed proton density-weighted MR image in elbow flexion are provided. What are the findings? What is your diagnosis?
Findings
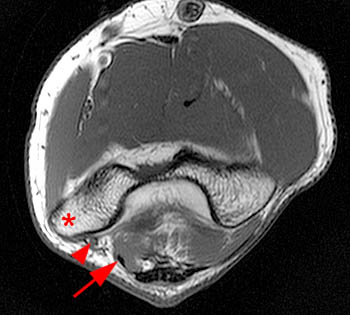
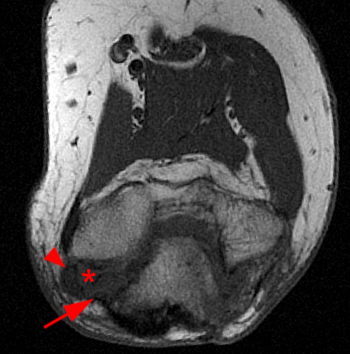
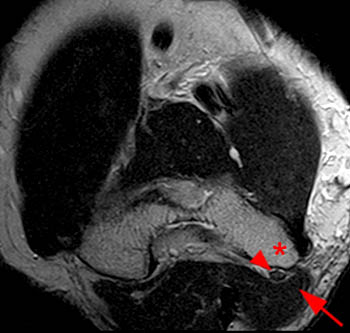
Figure 3:
(3a) Axial T1 and (3b) axial fat-suppressed proton density-weighted MR images with the elbow fully flexed show the ulnar nerve (arrowhead) and the medial triceps (arrow) anterior to the medial epicondyle (*). Note increased signal within the ulnar nerve on the fat- suppressed proton density view, consistent with neuropathy.
Diagnosis
Ulnar neuropathy related to ulnar nerve dislocation and snapping triceps.
Introduction
Ulnar neuropathy refers to the motor or sensory abnormalities that occur in the ulnar nerve distribution. Symptoms include pain, parasthesias, numbness, and motor weakness. Ulnar nerve subluxation occurs in approximately 16% of healthy individuals, has no age or sex predilection, can be unilateral or bilateral, painful or painless, and can have associated ulnar neuropathy.1
Snapping at the elbow is most frequently caused by ulnar nerve dislocation over the medial epicondyle of the humerus in elbow flexion or as the elbow is extended from a flexed position. Due to the clinical frequency of ulnar nerve dislocation, some physicians erroneously attribute all medial elbow snapping to the ulnar nerve. However, a portion of the medial head of the triceps muscle or an accessory triceps tendon can also dislocate, causing one or more additional snaps.
Medial head triceps dislocation can occur in combination with ulnar nerve dislocation, with or without pain, and with or without ulnar neuropathy. In some patients, the medial head triceps dislocates without snapping. Failure to appreciate concomitant ulnar nerve and triceps dislocation has resulted in misdiagnoses, and many patients have required secondary surgeries for persistent snapping after otherwise successful ulnar nerve transpositions.2,3,4
Standard MR imaging with the elbow extended often misses the dynamic abnormalities that occur with ulnar nerve and triceps dislocations. Flexed and extended MR Imaging is therefore indicated in patients who have ulnar nerve dislocation, snapping, or in patients who have undergone prior ulnar nerve transpositions and have persistent symptoms. (Figures 4-6, video).
Figure 6:
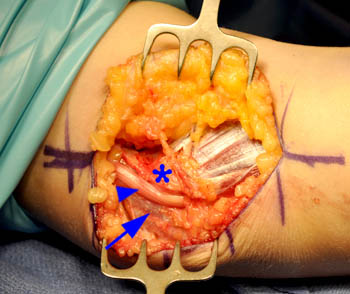
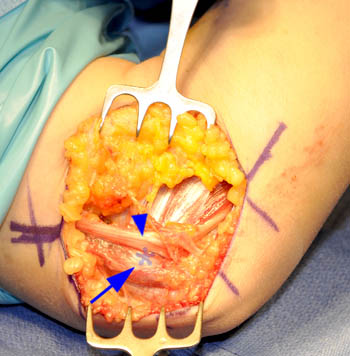
Intra-operative photographs of the same patient, with the elbow in (6a) extension showing the show the ulnar nerve (arrowhead) and the medial triceps (arrow) posterior to the medial epicondyle (*), and in (6b) flexion showing the ulnar nerve (arrowhead) and the medial triceps (arrow) dislocated anterior to and covering the medial epicondyle.
Intraoperative video of the same patient showing the ulnar nerve and medial head of the triceps muscle posterior to the medial epicondyle while in extension. As the surgeon passively flexes the elbow the ulnar nerve and medial head triceps dislocate anteriorly and medially, covering the medial epicondyle. The surgeon then returns the elbow to the fully extended position, and the triceps returns to its normal location posterior to the medial epicondyle. The surgeon uses forceps to return the ulnar nerve to its normal location. Intraoperative images and video courtesy of Thomas T. Dovan, M.D., Elite Sports Medicine and Orthopaedic Center, Nashville, TN.
Clinical Evaluation
Ulnar nerve dislocation is most often isolated, can be asymptomatic, associated with snapping, pain, or ulnar neuropathy. Chronic compression of the ulnar nerve can lead to loss of grip and claw deformities of the fourth and fifth fingers.5,6,7 The medial head triceps can dislocate with the ulnar nerve and can be symptomatic or asymptomatic. Patients with triceps dislocation can experience painless snapping, pain and snapping, snapping and ulnar neuropathy, or isolated ulnar neuropathy.
On physical exam the ulnar nerve can be palpated in the cubital tunnel with the elbow extended. While passively flexing the elbow the examiner palpates for anterior dislocation of the nerve, the medial head of the triceps muscle, or an accessory triceps tendon. Snapping of the medial edge of the triceps over the medial humeral epicondyle is often subtle, but can be detected with careful palpation, and occasionally it can be seen or heard.
When the ulnar nerve and triceps both dislocate, the first snap is typically related to dislocation of the ulnar nerve and the second snap is related to dislocation of the medial head of the triceps muscle. Occasionally there can be more than two snaps. Spinner and Goldner described a 12 year old male patient with three snaps.2 The first snap was related to ulnar nerve dislocation at 90 degrees of elbow flexion. The second snap was related to subluxation of the edge of the medial head triceps muscle along the medial epicondyle at 105 degrees of elbow flexion. The final snap was related to subluxation of a tendinous triceps band at 120 degrees of elbow flexion.
Anatomy
The ulnar nerve is a terminal branch of the brachial plexus arising from the medial cord and inferior trunk, containing C8, T1, and occasionally C7 nerve root fibers. The nerve courses along the brachial and axillary artery medially in the anterior compartment of the proximal arm. It enters the posterior compartment at the mid-arm after passing through the medial intermuscular septum. It descends along the medial head of the triceps muscle, and enters the cubital tunnel.
The term cubital tunnel was first used in 1958 by Feindel and Stratford, at which time they described ulnar nerve compression related to the local anatomy. The cubital tunnel is located along the posterior medial elbow. The floor of the cubital tunnel is formed by the elbow joint capsule and the posterior and transverse portions of the ulnar collateral ligament. The walls are formed by the medial epicondyle and olecranon, and the roof is formed by the cubital tunnel retinaculum, also called the arcuate ligament or the ligament of Osborne.
After exiting the cubital tunnel, the ulnar nerve enters the medial forearm between the superficial and deep heads of the flexor carpi ulnaris muscle. It then courses distally between the flexor carpi ulnaris and flexor digitorum profundus muscles, and then through Guyon’s canal at the volar wrist. Distal to Guyon’s canal it subdivides into deep and superficial motor branches.
No muscles are innervated by the ulnar nerve at the upper arm. At the elbow, the ulnar nerve supplies motor branches to the flexor carpi ulnaris and ulnar portion of the flexor digitorum profundus muscles. In the distal forearm, the nerve supplies a dorsal sensory branch that innervates the ulnar aspect of the dorsal hand. In the palm, the superficial branch supplies the palmaris brevis muscle, the skin of the ulnar aspect of the palm and the ring and little fingers. The deep motor branch supplies the opponens digiti minimi, flexor digiti minimi, abductor digiti minimi, deep head of the flexor pollicis brevis, adductor pollicis, dorsal and palmar interosseous muscles, and the third and fourth lumbrical muscles.
Discussion
The ulnar nerve can be compressed at several locations along its course: at the intermuscular septum due to the arcade of Struthers, at the medial epicondyle entrance to the cubital tunnel, within the cubital tunnel, at the flexor/pronator aponeurosis between the heads of the flexor carpi ulnaris, and at Guyon’s canal.5,11,12
Most commonly, ulnar nerve compression occurs at the elbow. Cubital tunnel syndrome is the second most common compressive neuropathy after carpal tunnel syndrome. Causes of cubital tunnel syndrome include subluxation of the ulnar nerve over the medial epicondyle, bone spurs, underlying synovitis, intraarticular bodies, cubitus valgus, constricting fascial bands, tumors, ganglia, and direct compression (Figure 8).
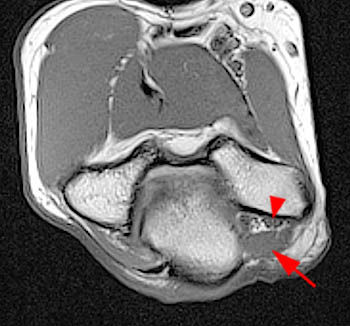
Figure 8:
(8a) Axial T1 and (8b) axial proton density-weighted MR images from a 66 year old male patient with pain, stiffness, and inability to flex or extend the arm. (The patient has a history of four prior surgeries related to an old motor vehicle accident). Note medial subluxation of the ulnar nerve (arrowhead) related to an olecranon bone spur (arrow), underlying joint effusion with synovitis and an intraarticular body (*).
When the elbow is flexed, increased stress is placed on the ulnar collateral ligament and retinaculum. The shape of the cubital tunnel changes and decreases in size causing increased intraneural pressure. These changes are most pronounced when there is concurrent elbow flexion, wrist extension, and shoulder abduction, such as in throwing athletes. These compressive forces can be symptomatic or asymptomatic. Cubital tunnel syndrome occurs more frequently in males and is associated with overuse. It affects people in a variety of occupations, such as laborers, truck drivers, and radiologists.8,9
In normal patients, when the elbow is fully flexed, there is mild medial displacement of the ulnar nerve and triceps, but both remain posterior to the medial epicondyle (Figure 9).
Causes of ulnar nerve dislocation include absence or laxity of the cubital tunnel retinaculum, cubitus valgus, cubitus varus, hypertrophied triceps muscle, anomalous triceps tendon, loose anchorage of the nerve, and osseous anomalies of the medial epicondyle. Dislocation of the ulnar nerve can be asymptomatic, but it can leave the nerve open for direct trauma or cause a friction neuritis over time related to excessive motion of the nerve against the medial epicondyle. On MR imaging, increased T2 signal, increased STIR signal, and increased caliber of the nerve are suggestive of neuritis.5,10 (Figure 10)
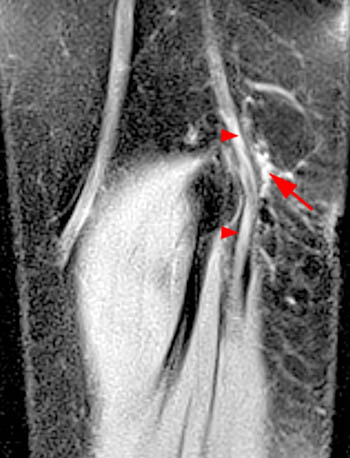
Figure 10:
(10a) Axial T1 and (10b) sagittal fat suppressed proton density-weighted MR images of the elbow in a 54 year old female who presented with ulnar sided pain and numbness for one year, demonstrates medial subluxation of the ulnar nerve, and increased intrinsic signal within the nerve (arrowheads) and adjacent soft tissue edema (arrow), consistent with neuropathy.
The most common abnormality of the cubital tunnel that causes compressive symptoms is the accessory anconeus epitrochlearis muscle.5,11 The anconeus epitrochlearis muscle extends from the medial olecranon to the inferior surface of the medial epicondyle, following the normal course of the cubital tunnel retinaculum. In this location, it extends superficial to the ulnar nerve in the cubital tunnel where it can be associated with compressive neuropathy (Figure 11).
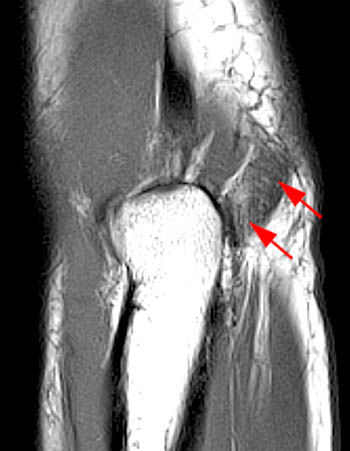
Figure 11:
Accessory anconeus epitrochlearis muscle. (11a) Axial and (11b) coronal T1-weighted MR images of the elbow in a 38 year old female who presented with elbow pain. The anconeus epitrochlearis muscle (arrows) courses from the medial cortex of the olecranon to the inferior surface of the medial epicondyle, along the normal expected course of the cubital tunnel retinaculum, where it courses superficial to the ulnar nerve (arrowhead).
Conclusion
Ulnar neuropathy can be caused by static structures or dynamic factors. High spatial resolution, excellent image contrast and multiplanar capabilities make MR an excellent tool in the evaluation of abnormalities of the ulnar nerve. Bone spurs, synovitis, cubitus valgus, constricting fascial bands, tumors, ganglia, and direct compression are well delineated on standard MR imaging. However, standard MR imaging in elbow extension often misses the dynamic type abnormalities that occur with ulnar nerve and triceps dislocations.
Snapping at the elbow is most frequently caused by ulnar nerve dislocation over the medial epicondyle. Some patients also have snapping related to dislocation of a portion of the medial head triceps muscle or an accessory triceps tendon. Failure to appreciate concomitant ulnar nerve and triceps dislocation has resulted in misdiagnoses, and many patients have required secondary surgeries for persistent snapping after otherwise successful ulnar nerve transpositions. Therefore, MRI with flexed and extended images is indicated in patients who have ulnar nerve dislocation, snapping on clinical exam, or patients who have undergone prior ulnar nerve transpositions but continue to have symptoms.
References
1 Childress HM. Recurrent ulnar-nerve dislocation at the elbow. J Bone Joint Surg Am 1956:38-A:978-984.
2 Spinner RJ, Goldner RO. Snapping of the medial head of the triceps and recurrent dislocation of the ulner nerve. J Bone Joint Surg Am 1998; 80:239-247.
3 Spinner RJ, Hayden FR, Hipps CT, Goldner RD. Imaging the Snapping Triceps. AJR 1996;167:1550-1551.
4 Haws M, Brown RE. Bilateral snapping triceps tendon after bilateral ulnar nerve transposition for ulnar nerve subluxation. Ann Past Surg 1995;34:551-551.
5 Miller TT, Reinus WR. Nerve Entrapment Syndromes of the Elbow, Forearm, and Wrist. AJR 2010;195:585-594.
6 Andreisek G, Crook DW, Burg D, Marincek B, Weishaupt D. Peripheral Neuropathies of the Median, Radial, and Ulnar Nerves: MR Imaging Features. Radiographics 2006; 26:1267-1287.
7 Darowish M, Lawton JN, Evans PJQ. What is cell phone elbow, and what should we tell our patients? Clev Clin J Med 2009;76:306-308.
8 Ruess L, O’Connor SC, Cho KH, Hussain FH, Howard WJ, Slaughter RC, Hedge A. Carpal Tunnel Syndrome and Cubital Tunnel Syndrome: Work-Related Musculoskeletal Disorders in Four Symptomatic Radiologists. AJR 2003;181:37-42.
9 Jensen A, Kaerlev L, Tuchsen F, et al. Locomotor diseases among male long-haul truck drivers and other professional drivers. Int Arch Occup Environ Health 2008; 81:821-827.
10 Baumer P, Dombert T, Staub F, Kaestel T, Bartsch AJ, Heiland S, Bendszus M, Pham M. Ulnar Neuropathy at the Elbow: MR Neurography-Nerve T2 Signal Increase and Caliber. Radiology 2011;260:199-206.
11 Sookur PA, Naraghi AM, Bleakney RR, Jalan R, Chan O, White LM. Accessory Muscles: Anatomy, Symptoms, and Radiologic Evaluation. RadioGraphics 2008; 28:481-499.
12 Spiess AM, Gursel E. Entrapment of the ulnar nerve at Guyon’s canal by an accessory abductor digiti minimi muscle. Plast Reconstr Surg 2006;117:1060-1061.
13 Madsen M, Marx RG, Millett PJ, Rodeo SA, Sperling JW, Warren RF. Surgical Anatomy of the Triceps Brachii Tendon Anatomical Study and Clinical Correlation. The American journal of Sports Medicine 2006;34:1839-1843.
14 Jacobson JA, Jebson PJ, Jeffers AW, Fessell DP, Hayes CW. Ulnar Nerve Dislocation and Snapping Triceps Syndrome: Diagnosis with Dynamic Sonography-Report of Three Cases. Radiology 2001; 220:601-605.
15 Rosenberg ZS, Beltran J, Cheung Y, Broker M. MR Imaging of the Elbow: Normal Variant and Potential Diagnostic Pitfalls of the Trochlear Groove and Cubital Tunnel. AJR 1995;164:415-418.