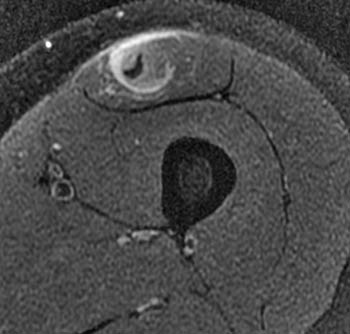
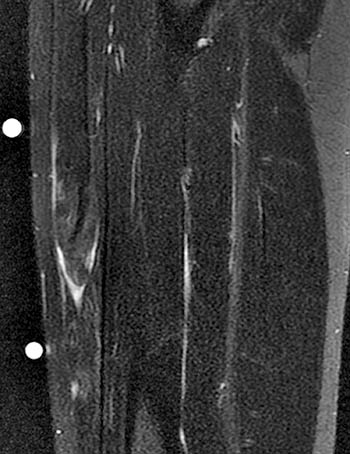
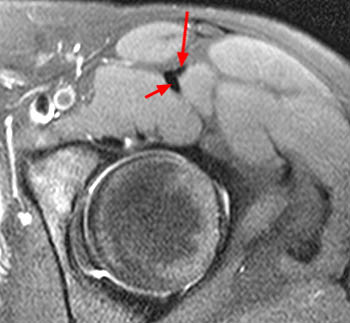
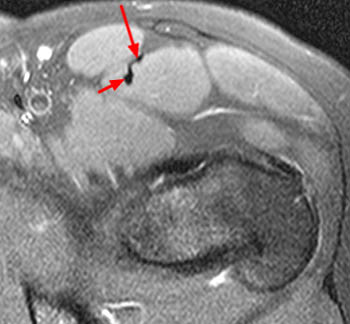
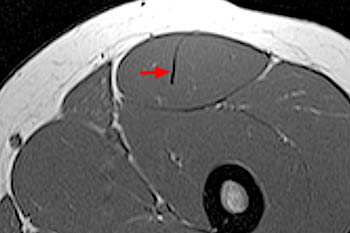
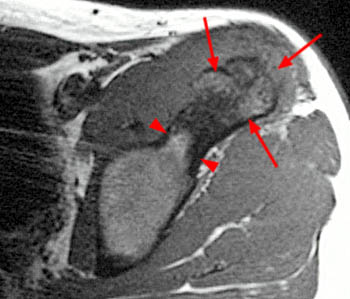
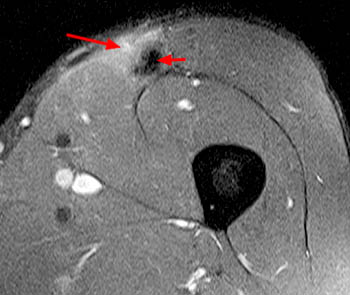
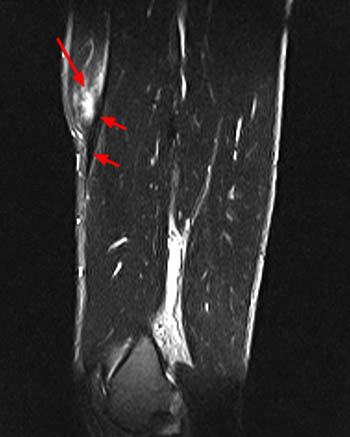
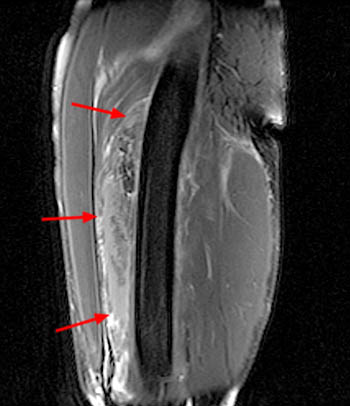
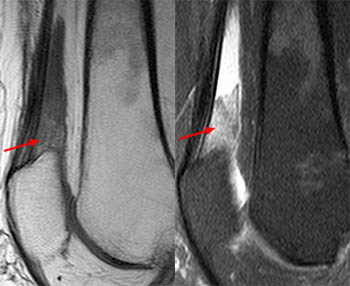
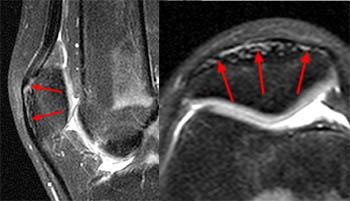
Clinical History: A 16 year-old female track athlete presents with a 6 week history of a thigh mass and pain. Axial proton density fat-suppressed (1a) and sagittal T2-weighted fat-suppressed (1b) images are provided. What are the findings? What is your diagnosis?
Findings
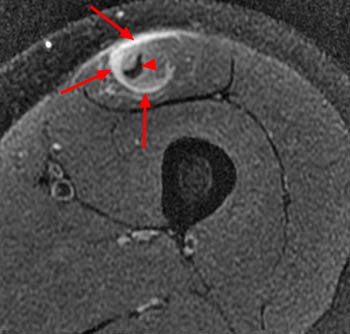
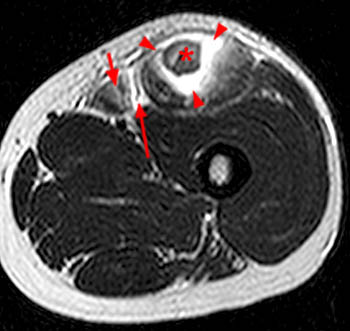
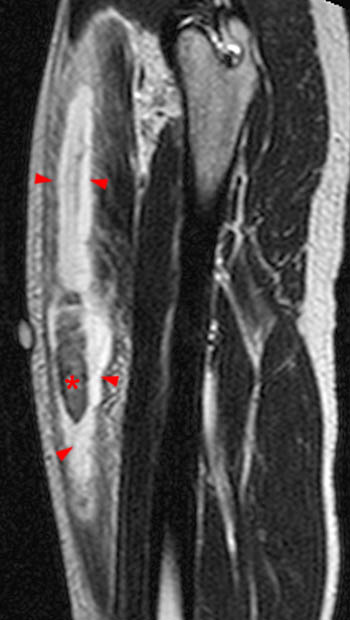
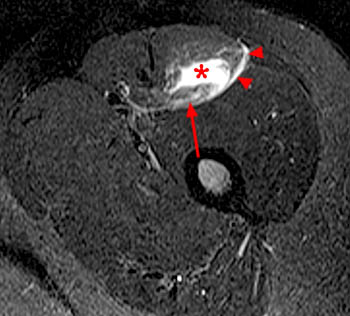
Figure 2:
The axial proton density fat-suppressed image through the mid-thigh demonstrates edema within the inner bipennate component of the rectus femoris muscle, surrounding the indirect tendon (arrowhead), and a band of fluid (arrows) separating this muscle and the outer unipennate muscle of the rectus femoris.
Diagnosis
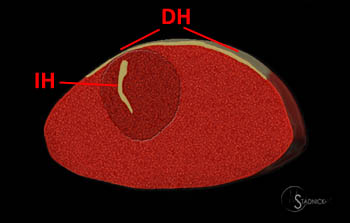
Intramuscular degloving injury of the rectus femoris muscle.
MRI of Rectus Femoris / Quadriceps Injury
Introduction
The quadriceps muscle group is vital for athletes who participate in sports that require running, jumping and kicking. Of the four muscles that comprise this group, the rectus femoris is the most commonly strained and also has the most complex anatomy. This MRI web clinic will describe MR imaging of quadriceps injuries, with emphasis on the rectus femoris (RF), and will review the prognostic significance of MRI findings as they relate to the time required for recovery and return to athletic activity.
Anatomy
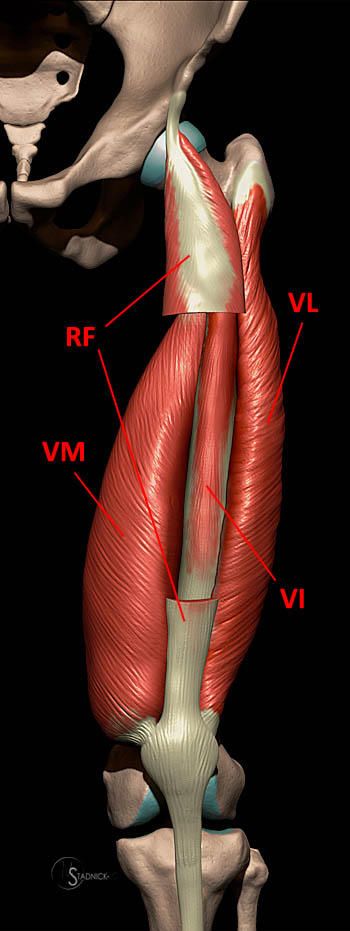
The rectus femoris muscle is the most anterior and superficial of the quadriceps muscle group. The other components of the quadriceps mechanism are the vastus medialis (with its distal, oblique component), vastus intermedius and vastus lateralis. At the distal thigh, the tendons of these muscles merge to form the quadriceps tendon. The rectus femoris acts to extend the lower leg at the knee and flex the thigh at the hip. It is a direct antagonist to the hamstrings and it is innervated by the posterior division of the femoral nerve (L2, L3, L4).
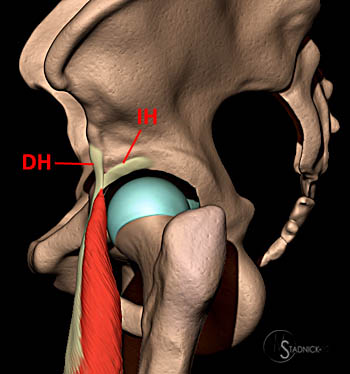
The rectus femoris musculotendinous anatomy is unique and was not fully elucidated until 1995.1 It has two tendinous origins: the direct or straight head, which arises from the anterior inferior iliac spine (AIIS), and the indirect or reflected head, which arises from the superior acetabular ridge and the posterolateral aspect of the hip joint capsule (6a). The two heads form a conjoined tendon about 2 cm distal to their origin, however, as first described by Hasselman et al1, each tendon nearly retains a separate identity, with 10-20% intermingling of fibers, as they extend distally (Figures 7, 8).
Figure 6:
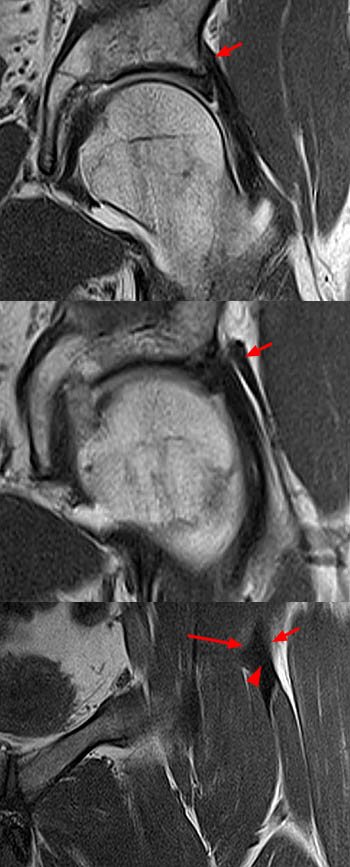
Coronal MR-arthrogram T1-weighted images, from posterior(superior) to anterior(inferior), demonstrate the origin of the indirect head (short arrow) from the acetabulum and joint capsule (superior and middle images). Anteriorly (inferior image) the indirect head (short arrow) and the direct head (long arrow) arising from the anterior inferior iliac spine converge (arrowhead).
Figure 7:
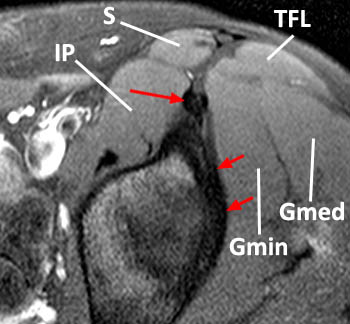
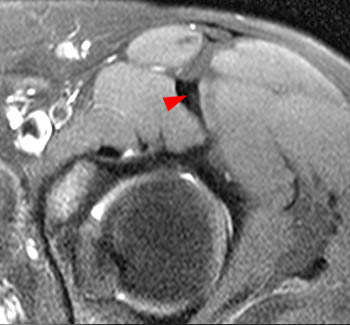
Normal proximal rectus femoris anatomy on axial STIR images. (7a) Direct head (long arrow) and indirect head (short arrows) at their origin. IP = iliopsoas muscle, S = sartorius muscle, TFL = tensor fascia lata muscle, Gmin = gluteus minimus muscle, Gmed = gluteus medius muscle. (7b) More distally, the two heads converge to form the conjoined tendon (arrowhead). (7c) At the level of the femoral head, the tendon begins to diverge into the direct head (long arrow) and the indirect head (short arrow). (7d) At the level of the greater trochanter, the direct head (long arrow) is at the anterior muscle surface and the indirect head (short arrow) has entered the muscle substance.
The direct head forms primarily the superficial anterior tendon that covers the proximal third of the muscle. This gives rise to a unipennate muscle and blends with the anterior fascia. The indirect head primarily contributes to the deep, central intramuscular tendon. At its proximal aspect, this tendon is rounded and located within the medial aspect of the muscle. As it progresses through the proximal two-thirds of the muscle, it becomes flattened, with its long axis parallel to the sagittal plane and located within the anterior, central to medial aspect of the muscle. It gives rise to a bipennate muscle which is surrounded by the unipennate muscle (Figures 10,11).
Figure 9:
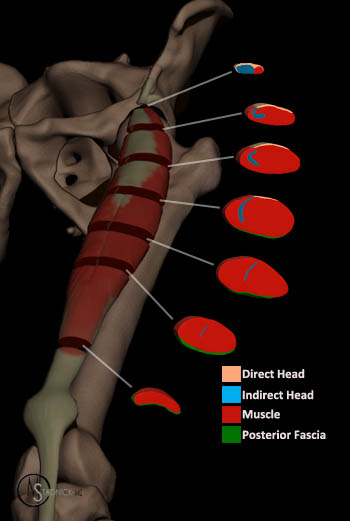
3D cross-sectional illustration of the rectus femoris tendinous anatomy. The direct head extends along the proximal 1/3, the indirect head courses through the proximal 2/3 and the distal, posterior tendon arises from the aponeurosis at the posterior muscle surface. A bipennate muscle arises from the indirect head and is surrounded by a unipennate muscle arising from the direct head.
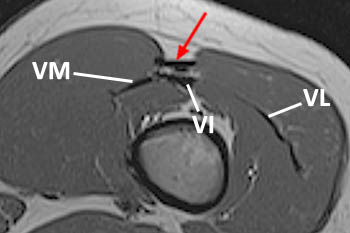
Figure 11:
Normal anatomy of the mid-to-distal rectus femoris on axial T1-weighted images. (11a) Proximal-to-mid-shaft level. The indirect head is more centrally located within the muscle (arrow). (11b) Mid-to-distal shaft level. The terminating indirect head is barely visible (arrow). (11c) Distal shaft level. Distal rectus femoris musculotendinous junction (arrow). (11d) Distal shaft level. Distal rectus femoris tendon (arrow). VI = vastus intermedius tendon, VM = vastus medialis tendon, VL = vastus lateralis tendon.
This unusual tendinous and muscle within a muscle architecture result in patterns of muscle tearing that differ from what is typically encountered. The distal tendon arises as a broad aponeurosis on the posterior surface of the distal two-thirds of the muscle. At its proximal aspect, the posterior aponeurosis may extend into the posterolateral muscle substance. The distal tendon has a flat configuration and merges with the vastus tendons to form the quadriceps tendon. As the most anterior component of this tendon, it inserts on the superior and anterior surface of the patella. The distal rectus femoris musculotendinous junction is located at this posterior tendon, not at the distal end of the deep, central tendon, which is a common misconception.
Significant variations to this anatomy have been reported. For example, a third head, arising from the iliofemoral ligament and gluteus minimus tendon, was seen in a majority of cadavers2 and, in another study, 60% of cadavers had an oblique head of the vastus lateralis muscle with no oblique head of the vastus medialis muscle observed3.
Overview of Rectus Femoris Injury
Injury to the rectus femoris muscle is common in athletes, second only to the hamstrings among lower extremity injuries. It is the most common lower extremity muscle injury among soccer players4. The rectus femoris is vulnerable to injury because it crosses two joints, has a high proportion of type II, fast twitch muscle fibers and because, in an athletic kicking motion (soccer, football, martial arts), it undergoes forceful eccentric contraction while passively stretched at the onset of the forward swing phase5. The most significant of the other risk factors for muscle strain is recent or remote injury to the muscle. Re-injury often occurs at a different location within the muscle or, if in the same region previously affected, is seen at the margin of a region of scarring4. The rectus femoris is also prone to injury if there has been recent hamstring injury. Other proposed risk factors include low muscle strength, muscle imbalance, limited flexibility, muscle fatigue, inadequate warm-up and improper technique6,7,8.
The most proximal rectus femoris tendons may be injured at or just distal to their origin. The same mechanism of injury in a skeletally immature athlete results in avulsion fracture of the AIIS, at the origin of the direct head, owing to the vulnerability of the open apophysis. Rectus femoris muscle injury usually consists of a myotendinous strain centered on the indirect or direct head or, less commonly, myofascial junction injury, at the periphery of the muscle. The majority of rectus femoris injuries occur about the deep intramuscular musculotendinous junction9. Other injuries to the quadriceps mechanism include muscle contusion, vastus muscle strain, distal rectus femoris musculotendinous junction strain and quadriceps tendon tear.
Anterior Inferior Iliac Spine Avulsion
Pelvic avulsion injuries usually involve skeletally immature patients and most often occur between the ages of 14 and 25 years. Injury typically occurs through the cartilaginous growth plate of the apophysis and is due to application of a tensile force by a violent, forceful contraction. Often, the fracture occurs through an apophysis that has been weakened by chronic repetitive trauma. Patients complain of localized pain and swelling and limited range of motion. The diagnosis can usually be established with radiographs. Anterior inferior iliac spine (AIIS) avulsion fracture is usually best seen on an oblique, rather than AP, radiograph of the pelvis10. Comparison radiographs of the contralateral hip may aid in distinction between an open apophysis and an avulsion fracture. Some pelvic avulsion fractures, such as those occurring at the ischium, anterior superior iliac spine and lesser trochanter, exhibit moderate displacement due to a lack of adjacent soft tissue attachments. It has been proposed that distal displacement of the AIIS fracture fragment may be limited if the adjacent indirect head of the rectus femoris is intact11. MRI may be useful for identifying minimally displaced or non-displaced avulsions, purely tendinous avulsions and avulsions or apophysitis that occur prior to apophyseal ossification (Figure 12). MRI may miss a small bone fragment but, if the injury is acute, it will show edema at the apophysis, often extending along the tendon origin. Most patients heal with conservative management but recovery may take up to 4 months10.
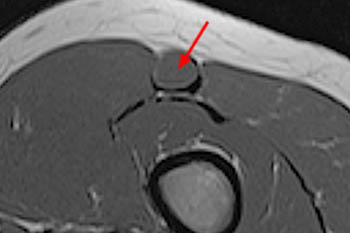
Figure 12:
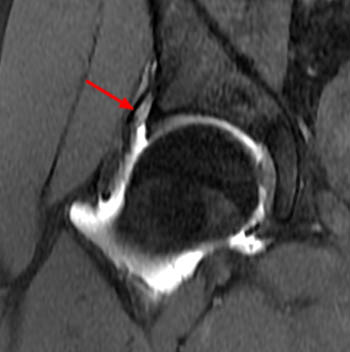
Anterior iliac spine avulsion fracture. 13 year-old female with hip pain, who felt a pop while running two days ago. Axial proton density fat-suppressed image (left): fluid signal intensity at the fracture (arrow) and edema within the origin of the indirect head (short arrow) and the intermuscular fascial planes. Sagittal proton density fat-suppressed image (right): high signal intensity at the minimally displaced avulsion fracture (arrow) and edema within the iliacus (asterisk) and iliopsoas (arrowheads) muscles.
When patients with AIIS avulsion present in the subacute or chronic phase, radiographs may demonstrate an area of heterotopic ossification at the site of injury that may be misinterpreted as osteosarcoma or other bone-forming neoplasm11,12. MRI of this ossified mass usually shows low signal intensity bone admixed with areas of non-specific high signal intensity on fluid-sensitive sequences (Figure 13).
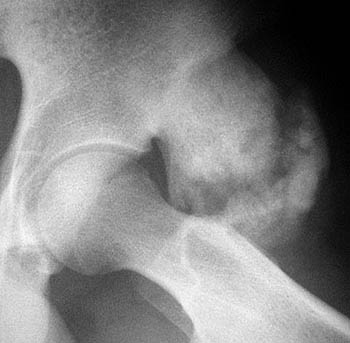
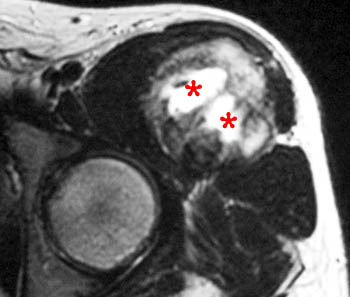
Figure 13:
Post-traumatic periostitis ossificans. A 15 year-old male soccer player presents with a hip mass and a history of "popping" injuries 3 and 6 months prior. The frog view radiograph (13a) reveals a densely ossified mass, with radiolucent zones, continuous with the anterior inferior iliac spine. An axial T1-weighted image (13b) reveals a low signal intensity ossified mass (arrows), continuous with the anterior inferior iliac spine (arrowheads). An axial T2-weighted image (13c) reveals a large area of high signal intensity (asterisks) within the mass. Biopsy of this region revealed reparative fibrovascular tissue, blood clot, bone and cartilage.
CT demonstrates mature and/or immature bone depending upon the age of the injury. Continuity of the mass with the AIIS is a clue to the correct diagnosis. If the central portion of the mass is biopsied, it frequently demonstrates histologic features suggestive of a reactive or aggressive process and an inexperienced pathologist may mistake it for osteosarcoma. Therefore, it is important for the radiologist to be aware of this potential pitfall. A history of acute or chronic, repetitive trauma strongly suggests a non-neoplastic origin of the mass. It should also be kept in mind that juxtacortical osteosarcoma is unusual adjacent to the AIIS.
Rectus Femoris Origin Injuries
Injuries of the origin of the direct and indirect heads of the rectus femoris have been infrequently reported. These injuries are generally not visible on radiographs except when chronic and accompanied by heterotopic bone formation. MRI is useful for diagnosis of subtle tears (Figure 14) and to determine the extent of retraction of complete tears (Figure 15).
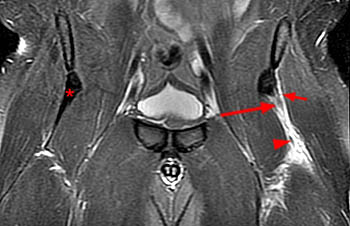
Figure 15:
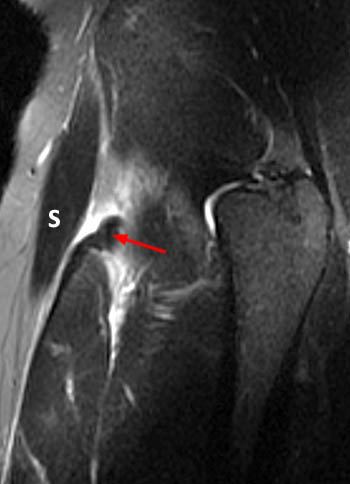
A 20 year-old male with hip pain, injured while playing baseball one week prior to imaging. Axial proton density fat-suppressed image (15a): complete avulsion of the indirect head, replaced by fluid (short arrows). Coronal T2-weighted fat-suppressed image (15b): complete avulsion of the indirect (short arrow) and direct heads (arrow) with distal retraction (arrowhead), replaced by fluid. Compare to intact conjoined tendon on the right (asterisk). Sagittal T2-weighted fat-suppressed image (15c): distally retracted rectus femoris tendon (arrow), draped over the proximal muscle, with adjacent perifascial fluid. S = sartorius muscle.
In prior studies utilizing radiography and CT, all proximal RF avulsions involved the AIIS, the site of attachment of the direct head, with no cases of avulsion of the superior acetabular ridge by the indirect head. Therefore, it was assumed that injury to the direct head origin was more common than to the indirect head13,14. This was not borne out in a report of MR imaging of rectus femoris origin injuries in 17 patients by Oullette et al15. They studied 9 patients with acute symptoms and 8 patients with chronic symptoms with rectus femoris origin injuries. Eight of nine patients with acute symptoms and all patients with chronic symptoms had evidence of indirect head injury on MRI +/- injury to the direct head or conjoined tendon. The exception was a 14 year old patient with acute symptoms who had an AIIS avulsion fracture, partial tear of the direct head and no tear of the indirect head. They hypothesized a progression of injury that begins with the indirect head and, with increasing severity, progresses to the direct head and then the conjoined tendon. This sequence of injury does not apply to AIIS avulsion, as demonstrated by their above-noted 14 year old patient and other reports of AIIS avulsion. Furthermore, isolated, complete avulsion of the direct head has been reported in two National Football League kickers without indirect head injury, and with 3.5 cm and 1.0 cm distal tendon retraction, respectively. Perhaps differences in joint position, magnitude and vector of force exertion and degree of leg excursion determine whether injury primarily involves the indirect head or the direct head / apophysis16. In two patients reported by Oullette et al, a partial tear of the indirect head was seen on MR-arthrography, suggesting an associated tear of the superior joint capsule (Figure 16).
Proximal RF Musculotendinous Junction Strains
The “proximal rectus femoris musculotendinous junction” is distal to the conjoined tendon and refers to the anteriorly located direct head and its unipennate muscle and the indirect head (also referred to as the deep or central tendon) and its bipennate muscle, the latter of which extends to the junction of the middle and distal 2/3 of the RF muscle. A strain may occur at the junction of the conjoined tendon and the muscle belly, but this is uncommon. Tear of the deep musculotendinous junction of the indirect head was first described by Hughes et al in 1995 and is probably the most common tear of the RF tendon17.
Deep musculotendinous junction injuries of the proximal RF are difficult to diagnose clinically, partly because of the deep location of the injury and due to relatively nonspecific and variable symptoms and physical findings. With an acute strain, some patients report sudden onset of thigh pain whereas others describe an insidious onset of mild discomfort at the anterior thigh4,18. This depends, in part, on the extent and severity of the injury. Patients that are mildly symptomatic often continue playing, which interferes with healing and leads to more extensive tearing. Muscle edema and mild spasm and contraction cause thigh enlargement and discomfort and, clinically, may be mistaken for a soft tissue neoplasm. RF hematoma is unusual unless there has been direct impact to the anterior thigh4.
On MRI, because the deep tendon is so long, the craniocaudal extent of this injury is usually large, measuring 10 to 20 cm in length. In a grade 1 strain, no tendon or muscle fibers are disrupted. Intramuscular edema signal intensity surrounds the deep tendon on fluid-sensitive axial images (due to the bipennate muscle attachment) and feathery muscle edema is seen on corresponding coronal and sagittal images. Muscle and tendon may appear normal on T1-weighted images19. A grade 2 strain is defined as a partial tear of the musculotendinous junction with discontinuity of some muscle fibers and variable tearing/thinning of tendon. On MRI, edema and hemorrhage are more prominent. Hematoma at the musculotendinous junction is characteristic of a grade 2 strain and, by definition, is not seen in a grade 1 strain. In other muscles with conventional anatomy, epimysial tear and perifascial fluid usually occur with a grade 2 strain but this is less common with injury to the deep RF musculotendinous junction. The pattern of edema surrounding the deep tendon has been compared to a bull’s eye17 (Figure 17) and a similar pattern may be seen if gadolinium-enhanced images are obtained, due to enhancement of post-injury vascular and inflammatory tissue.
Figure 17:
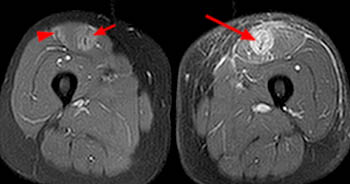
Bull's eye sign. 35 year-old male with bilateral thigh pain. Axial proton density fat-suppressed image (17a): on the left, partial tear of the deep, central tendon with edema throughout the inner muscle (long arrow). On the right, mild edema of the inner muscle, surrounding the central tendon (short arrow) and a mild posterolateral myofascial strain (arrowhead). Coronal T2-weighted fat-suppressed images (17b): grade 3 strain/tear of the left central musculotendinous junction (long arrows) with large proximal hematoma (asterisks) and mild proximal tendon retraction. Mild grade 1 strain of right central musculotendinous junction (short arrows) and grade 1 myofascial strain (arrowheads).
A grade 3 “strain” is defined as a complete tear of the musculotendinous junction and, on MRI, is characterized by discontinuity of all fibers, with or without muscle retraction. The tendon gap is filled with fluid and blood and, as time passes, this is replaced by granulation and scar tissue and degenerating and regenerating muscle20. For the rectus femoris, a complete tear may occur proximally, at the junction of the conjoined tendon and the proximal muscle or at the junction of the distal, posterior tendon and the distal muscle, however, each is uncommon. Because the rectus femoris consists of two muscles, a complete tear of the deep musculotendinous junction is really a grade 3 strain/tear of only the inner muscle.
Recently, a new pattern of tear of the RF muscle has been recognized, termed the “intramuscular degloving injury of the RF”21. In this injury, a circumferential tear occurs through the peripheral fibers of the inner bipennate muscle, separating it from the overlying unipennate muscle.
This dissociation between the inner and outer muscle components has measured between 4 and 18 cm in length. The average proximal retraction of the inner muscle was 1.2 cm, ranging from 0 to 3.5 cm. This injury pattern accounted for only 9% of rectus femoris injuries. It is best demonstrated on fluid-sensitive sagittal MR images which show the inner muscle, usually proximally retracted, with fluid interposed between it and the outer muscle (Figure 19).
Figure 19:
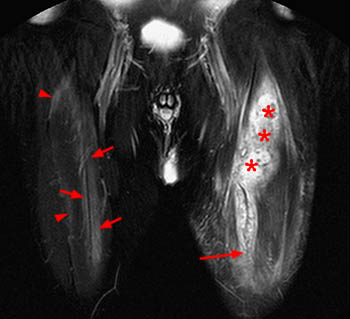
36 year old male with history of injury 4 days ago. Intramuscular degloving injury of the rectus femoris muscle. Axial T2-weighted image (19a): a large amount of fluid (arrowheads) separates the inner (asterisk) and outer rectus femoris muscles with intramuscular edema. Grade 1 strain of sartorius muscle (short arrow) and intermuscular perifascial fluid (arrow). A sagittal T2-weighted fat-suppressed image (19b) reveals proximally retracted inner muscle and the central tendon (asterisk) with a large amount of surrounding fluid ( arrowheads) that extends 20 cm cephalocaudal. An axial T2-weighted image (19c), distal to the retracted muscle, reveals centrally located fluid/hematoma (arrowheads) surrounded by edematous outer muscle. Absence of the central tendon is due to its intramuscular termination proximal to the level of the tear.
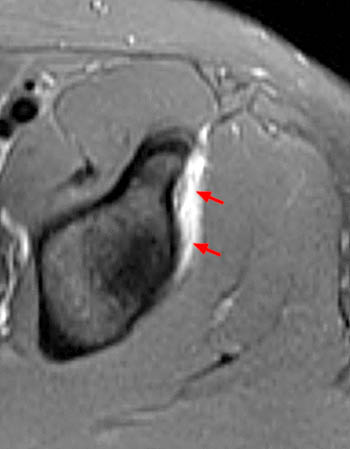
Mild, incomplete lesions appear as a band of edema along the interface between these two muscles (Figure 20).
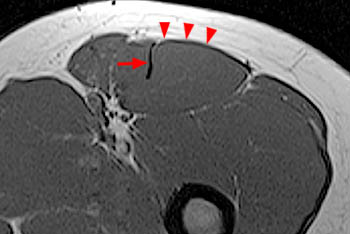
Figure 20:
20 year-old female with recurrent thigh strains and pain over the past 2 months. Axial proton density fat-suppressed image: mild edema within the interface between the inner and outer rectus femoris muscles (arrowheads). Precursor to degloving injury? Minimal posterolateral myofascial strain (arrows).
One study found the return to play interval for soccer players with this type injury ranged from 28 to 58 days21. It has been proposed that this injury is distinct from the typical myotendinous injury and is primarily an intermuscular dissociation, rather than tearing along the longitudinally-oriented musculotendinous junction. The proximally retracted muscle is accompanied by the deep central tendon. These tears have a strong tendency to occur distal to the termination of the central tendon, such that this tendon is not seen distal to the usually proximally retracted inner muscle. The mechanism by which the muscles dissociate from one another and whether there is a histologically visible interface between these muscles in normal individuals has not been elucidated.
Musculotendinous strain of the direct head of the RF is thought to be less common than injury to the indirect head4. On MRI, this injury presents as anterior muscle edema and edema and fluid between the anterior fascia and the muscle belly. Fluid may track several cm distally along the deep surface of the anterior fascia. Because the tendon of the direct head blends with the anterior fascia of the proximal third of the muscle, it may be difficult to distinguish a musculotendinous strain from an anterior myofascial injury. It has not been determined if, for the same grade of injury, recovery times are different for myotendinous versus myofascial injury. It has been suggested that if the site of injury and swelling is compressed by the overlying sartorius muscle, healing may be delayed4,22,23.
Myofascial RF injury is uncommon and not centered on a musculotendinous junction. This tear involves muscle fibers and extends up to or through the investing epimysium and the overlying fascia. It has no relation to myofascial pain syndrome. In one study, myofascial injuries accounted for 15% of all RF injuries in professional soccer players22. This injury usually involves the posterolateral aspect of the muscle and favors the proximal and middle thirds4. On MRI, intramuscular fluid and edema extend to the muscle periphery. If the fascia is intact, fluid dissects between the muscle and fascia and if the fascia is disrupted, fluid will also dissect along the adjacent fascial planes (Figure 21). Anterior RF myofascial injuries are difficult to diagnose with ultrasound and deep posterolateral injuries have a tendency to be re-injured and form seromas when players return to activity4.
Distal RF Musclotendinous Junction Injury
As noted earlier, the distal, posterior rectus femoris tendon forms from the aponeurosis on the posterior muscle surface. The muscle terminates into the tendon and the solitary tendon continues distally for 1-2 cm and then merges with the other tendons that comprise the quadriceps tendon. Injury to this distal musculotendinous junction is rarely reported in the medical literature24. Changes from acute or chronic injury are well demonstrated with MRI (Figure 22).
Vastus Muscle Injury
The vastus medialis, lateralis and intermedius muscles comprise the remainder of the quadriceps muscle group. The vastus medialis originates from the intertrochanteric line of the femur and the medial aspect of the linea aspera. The vastus intermedius originates at the anterolateral aspect of the femoral shaft. The vastus lateralis originates at the greater trochanter, the lateral lip of the linea aspera and the lateral intermuscular septum. The vastus medialis oblique (VMO) muscle is a distal component of the vastus medialis whose fibers have a more oblique course, blending distally with the medial patellofemoral ligament, in order to stabilize patellar tracking. The vastus muscles may be subject to strain or contusion. MRI may be useful for determination of the extent of musculotendinous strain. Except for recent investigation of the role of the VMO muscle in patellar stability, injury to these muscles has not been intensively studied.
Quadriceps Muscle Contusion
A muscle contusion occurs due to direct impact, usually with a blunt object, or by a fall to the ground. It causes intramuscular hemorrhage and edema and varying degrees of pain, tenderness, swelling and skin discoloration. Limitation of motion and difficulty weight-bearing is seen with moderate or large contusions. In athletics, contusion most often involves the quadriceps, and the vastus intermedius is the most commonly affected muscle8. This is due to the muscle being caught between the compressive force of injury and the unyielding, hard surface of the underlying femur.
Quadriceps contusion is a common, disabling injury in those sports wherein the participants have no padding for the thigh and upper leg, such as soccer and rugby. Clinical diagnosis is usually straightforward and MRI is most often used in patients with subacute or chronic thigh pain and an unknown mechanism of injury. On MRI, muscle contusion may have an appearance similar to a muscle strain, although a contusion is not centered on a musculotendinous junction, may cross fascial planes and may enlarge the muscle. Intramuscular hematoma is more common with contusion and causes pain and loss of range of motion (Figure 23). Intramuscular, lower extremity contusions tend to have a shorter recovery time than strains (13-21 days in one study25 and 19 +/- 9 days for contusions vs. 26 +/- 22 days for strains in another26) but recovery is prolonged if a significant hematoma develops.
Treatment of an acute quadriceps contusion differs from that applied to a strain in one important way. Several military studies have shown a shorter rehabilitation time, especially for moderate and severe contusions, if the injured leg is placed in a position of flexion for the first 24 hours after injury to limit hematoma formation. Ice and compression are also applied at this time25.
On MRI, an acute hematoma, up to 2-3 days old, is isointense to muscle on T1 images and hypointense on T2 images. Subacute (several days to 3 months old) and chronic (greater than 3 months old) hematoma demonstrate increased T1 and T2 signal intensity and develop a low signal intensity peripheral rim due to hemosiderin deposition that increases in thickness with time. Actually, most hematomas deviate from these basic guidelines and are heterogeneous in signal intensity due to blood clot, muscle detritus and hemoglobin breakdown products of varying age. The appearance often simulates that of a hemorrhagic neoplasm. A gadolinium-enhanced MRI may be useful to confirm a hematoma if the mass shows rim enhancement without any enhancing, solid components. If the mass does at least partially enhance, this may be due to neoplasm or reparative fibrovascular tissue within a hematoma.
Prognostic Features of MR Imaging Findings
MRI is generally accurate for determining the location, extent and severity of muscle injury. In the elite or professional athlete, the goal is for MRI to provide information to guide rehabilitation and predict the time interval required for recovery and return to play or training. For team sports, this information may be used to guide roster decisions. Currently, the decision of when an athlete can return to full activity is based on clinical assessment. Studies of athletes with hamstring or rectus femoris injury have shown imaging features with prognostic significance and, as experience accumulates, it is likely that findings on MRI will be incorporated into this decision-making process.
In a study of 25 quadriceps muscle strains in professional Australian soccer players, a significant difference in recovery time was found depending on whether the injury occurred about the deep central tendon (indirect head) or in the periphery (myofascial junction or tendon of the direct head)20. Deep, central musculotendinous strains required 27 days for recovery, versus 9 days for peripheral strains. For central tendon injuries, a statistically significant longer rehabilitation time was associated with location in the middle, rather than proximal, third of the muscle (34 days vs. 19 days), length of injury of at least 13 cm (32 days vs. 14 days) and % cross-sectional area of involvement of greater than 15% (30 days vs. 14 days). Vastus muscle strains recovered in only 4.4 days and patients with negative MRI studies needed 5.7 days to return to play. It has been suggested that the vastus muscles are less often affected by significant strain injury since they form a large muscle mass that acts synergistically, they only cross one joint and they are primarily composed of type I muscle fibers20. Patients with signs and symptoms of quadriceps or hamstring injury may have negative MRI examinations (3 of 25 in this study)20,27 This may be due to injury of insufficient size or severity to result in imaging findings, MRI performed before edema/inflammatory response developed or spine or trunk injury with referred pain. Interestingly, in the study summarized here, the site of maximal tenderness was often 3 cm or more from the site of maximal muscle strain injury on MRI. Residual edema signal intensity may persist in athletes that are clinically rehabilitated. It was concluded that in the elite amateur or professional athlete, MRI is indicated to evaluate acute injury to the thigh, as an adjunct to clinical examination, in order to determine presence, extent and prognosis of injury20.
A study of 40 elite soccer players found four factors associated with a poor prognosis for RF myotendinous and myofascial injuries. These were: proximal injury, perifascial fluid, changes seen on T1-weighted images and involvement of more than 50% of the cross-sectional area of the muscle. Perifascial fluid and abnormality seen on T1-weighted images were each statistically associated with longer recovery time. When 3 of these 4 factors were present, a longer recovery interval (37.7 vs. 27.2 days) had even greater statistical significance. The length of injury did not correlate with a longer recovery interval in this study22.
Quadriceps Tendon Injury
The quadriceps tendon is a multi-layered structure formed by the quadriceps muscle group. The most superficial layer arises from the RF and the deepest layer from the vastus intermedius. It is typically described as a trilaminar structure, with the vastus medialis and lateralis converging to form a middle layer. Other arrangements are also observed, such as, a two-layered or four-layered structure or, rarely, as a single band of tendon, depending on separation or convergence of the tendons28. An oblique head of the vastus medialis or of the vastus lateralis, respectively, may or may not be present3.
Quadriceps tendinosis is an overuse injury in athletes who perform intense and repeated jumping, as in volleyball, basketball, high jumping and long jumping. Microtears at the bone-tendon junction heal with fibrous scarring and patients report pain and focal tenderness. MRI reveals intratendinous increased signal intensity on fluid-sensitive images and variable tendon enlargement. As much as 25% of cases of jumper’s knee (see MRI web clinic, March, 2014) may be due to quadriceps tendinosis29. Patients usually respond to conservative measures and tendon debridement/excision is performed for recalcitrant cases. Some patients with anterior knee pain present with enlargement and edema or fluid signal intensity of the quadriceps fat pad and no other findings (Figure 24)30. This is thought to be a sign of a fat pad impingement syndrome and, in the appropriate clinical setting, such a patient may be a candidate for physical therapy.
The quadriceps tendon is most often injured within a hypovascular zone, 1-2 cm superior to the patella. Rupture usually occurs in patients older than 40 with a peak incidence in the 5th through 7th decades. A common mechanism of injury is maximal quadriceps contraction with the knee flexed as occurs when climbing stairs or standing from a seated position. In young, athletic patients, partial or complete tears may occur with strong deceleration while running31. Several systemic diseases and use of certain medications may increase the risk of quadriceps tendon rupture due to tendon degeneration. These include renal disease, diabetes, hyperparathyroidism, collagen vascular disease, rheumatoid arthritis and gout and the use of steroids or fluoroquinolone antibiotics. One of these factors is almost always present in patients with bilateral quadriceps ruptures.
MRI is useful in demonstrating the extent of partial tears and the report should indicate which individual tendon units are affected. Partial tears tend to involve either the rectus femoris or vastus intermedius tendon insertion (Figure 25).
Figure 25:
58 year-old male with recent tennis injury. Sagittal proton density fat suppressed image: complete tear of the rectus femoris portion of the quadriceps tendon with 1.5 cm proximal retraction (arrow). A partial tear of the other components of the quadriceps tendon was seen on other sagittal and axial images.
Isolated tears of the vastus medialis and lateralis are less common. Moderate and severe partial tears are often complex and it may be difficult to sort out the extent of tearing of each tendon. Both axial and sagittal fluid- sensitive sequences should be obtained for accurate assessment of tear extent. Partial tears are usually successfully treated conservatively with the knee immobilized in extension for 4-6 weeks and complete tears require open repair or reconstruction32.
Prepatellar Quadriceps Continuation
Most of the quadriceps tendon inserts on the anterosuperior surface of the patella. Continuity of the quadriceps and patellar tendons is accomplished by distal extension of fibers of the rectus femoris tendon to insert into the bone at the anterior surface of the patella. This is a chondroapophyseal type of attachment (an enthesis) in which tendon fibers transform into fibrocartilage at the insertion. This layer of fibrocartilage is thickest at the quadriceps tendon insertion on the anterosuperior patellar surface (0.136 mm), thinner at the patellar tendon attachment (0.023 mm) and thinnest at the prepatellar quadriceps continuation attachment to the anterior patellar surface (0.004 mm)33. It has been postulated that this layer of fibrocartilage is so thin because its function is to diminish friction between the patella and overlying tendinous fibers rather than to anchor the tendon to the patella33. Separation of the prepatellar quadriceps continuation from the anterior patellar surface has been observed on MRI in patients with anterior knee pain (Figure 26). This appears as a thin layer of fluid anterior to the patella with normal quadriceps and patellar tendons. Whether this is due to injury or degeneration and the clinical significance have not been established
Figure 26:
19 year old volleyball player reports knee pain with flexion. Sagittal (left) and axial (right) proton density fat suppressed images: edema/fluid signal intensity is present deep to the prepatellar quadriceps continuation (arrows), consistent with partial separation from the patella. This region was normal on MR images obtained 15 months earlier.
Sequelae/Complications of RF/Quadriceps Injury
Patients with chronic, deep RF musculotendinous junction tears may present clinically with a soft tissue mass of the anterior thigh with variable pain and weakness. In one study, surgery was performed on three patients and revealed intramuscular fibrous scar, 1-3 cm wide and 15-23 cm long34. Scar may also encase the deep tendon. In another study, 6 patients who presented with an anterior thigh mass could not remember a traumatic event. Because of this lack of correlation with history, MRI was performed, and, in retrospect, showed typical findings of musculotendinous junction strain with perimuscular edema. The pseudotumor was due to muscle edema and, in 5 patients, muscle retraction35. Pseudotumor may also be due to formation of a hematoma or seroma/pseudocyst. Focal or diffuse muscle atrophy, with fatty replacement, may occur due to disuse or denervation.
As was described previously, avulsion fracture of the AIIS may heal with extensive heterotopic ossification, extending laterally and distally from the avulsion site, and this may be confused with an osteoblastic tumor. Myositis ossificans is a significant risk with severe quadriceps contusions, with a reported incidence of 9-20%25. It should be suspected if, after 2-3 weeks, symptoms worsen with loss of knee flexion and persistent swelling. Diagnosis is best achieved with CT which demonstrates the characteristic peripheral rim of ossification, beginning 1-2 months after onset of symptoms. In the first several weeks, radiographs and CT are inconclusive as only non-specific mineralization is present.
Conclusion
Injury to the quadriceps muscle group and, especially the rectus femoris muscle and tendons, is an important source of impaired function in active individuals and elite and professional athletes. Patients may present with acute or chronic symptoms and, often, the location, type and extent of injury are not readily determined by clinical assessment. This information is needed in order to determine prognosis, to formulate an appropriate plan for rehabilitation and, in some cases, for planning surgery. As experience with MRI builds, it is being integrated into this decision-making process. MRI is useful for delineating the presence, severity and extent of acute and chronic injury and for demonstrating confounding factors, such as hematoma and scarring. For the rectus femoris in particular, MRI has revealed myotendinous anatomy and patterns of injury that are unique. By correlating findings on MRI with clinical data, MRI contributes to treatment planning and can be used to predict the recovery interval. For patients with an inadequate response to therapy or chronic symptoms, MRI may demonstrate complications such as scarring, hematoma and heterotopic ossification. It is also useful in patients who present with an apparent mass that is, in fact, related to injury, such as contusion or hematoma, rather than neoplasia. In summary, it is likely that MRI will have a significant and expanding role in evaluation and treatment of many patients with acute or chronic rectus femoris/quadriceps injury.
References
1 Hasselman CT, Best TM, Hughes C, Martinez S, Garrett WE Jr. An explanation for various rectus femoris strain injuries using previously undescribed muscle architecture. Am J Sports Med 1995;23:493-499.
2 Tubbs RS, Stetler W Jr, Savage AJ, Shoja MM, Shakeri AB, Loukas M et al. Does a third head of the rectus femoris muscle exist? Folia Morphol (Warsz) 2006;65:377-380.
3 Waligora AC, Johanson NA, Hirsch BE. Clinical anatomy of the quadriceps femoris and extensor apparatus of the knee. Clin Orthop Relat Res 2009;467:3297-3306.
4 Kassarjian A, Rodrigo RM, Santisteban JM. Current concepts in MRI of rectus femoris musculotendinous (myotendinous) and myofascial injuries in elite athletes. Eur J Radiol 2012;81:3763-3771.
5 Gainor BJ, Piotrowski G, Puhl JJ, Allen WC. The kick: biomechanics and collision injury. Am J Sports Med 1978;6:185-193.
6 Orchard JW. Intrinsic and extrinsic risk factors for muscle strains in Australian football. Am J Sports Med 2001;29:300-303.
7 Jarvinen TAH, Jarvinen TLN, Kaariainen M, Kalimo H, Jarvinen M. Muscle injuries. Biology and treatment. Am J Sports Med 2005;33:745-764.
8 Boutin RD. Muscle. A radiologic prespective: magnetic resonance imaging of muscle. In: Pedowitz RA, Chung CC, Resnick DR: Magnetic Resonance Imaging in Orthopaedic Sports Medicine, Springer, 2008, p. 1-20.
9 Bordalo-Rodrigues M, Rosenberg ZS. MR imaging of the proximal rectus femoris musculotendinous unit. Magn Reson Imaging Clin N Am 2005;13:717-725.
10 Sanders TG, Zlatkin MB. Avulsion injuries of the pelvis. Semin Musculoskel Radiol 2008;12:42-53.
11 Metzmaker JN, Pappas AM. Avulsion fractures of the pelvis. Am J Sports Med 1985;13:349-358.
12 Resnick JM, Carrasco CH, Edeiken, Yasko AW, Ro JY, Ayala AG. Avulsion fracture of the anterior inferior iliac spine with abundant reactive ossification in the soft tissue. Skeletal Radiol 1996;25:580-584.
13 Deehan DJ, Beattie TF, Knight D, Jongschaap H. Avulsion fracture of the straight and reflected heads of rectus femoris. Arch Emerg Med 1992;9:310-313.
14 Nanka O, Havranek P, Pesl T, Dutka J. Avulsion fracture of the pelvis: separation of the secondary ossification center in the superior margin of the acetabulum. Clin Anat 2003;16:458-460.
15 Ouellette H, Thomas BJ, Nelson E, Torriani M. MR imaging of rectus femoris origin injuries. Skeletal Radiol 2006;35:665-672.
16 Hsu JC, Fischer DA, Wright RW. Proximal rectus femoris avulsions in National Football League kickers. Am J Sports Med 2005;33:1085-1087.
17 Hughes C, Hasselman CT, Best, Martinez S, Garrett WE Jr. Incomplete, intrasubstance strain injuries of the rectus femoris muscle. Am J Sports Med 1995;23:500-506.
18 Gyftopoulos S, Rosenberg ZS, Schweitzer ME, Bordalo-Rodrigues M. Normal anatomy and strains of the deep musculotendinous junction of the proximal rectus femoris: MRI features. AJR 2008;190:W182-W186.
19 Palmer WE, Kuong SJ, Elmadbouh HM. MR imaging of myotendinous strain. AJR 1999;173:703-709.
20 Cross TM, Gibbs N, Houang MT, Cameron M. Acute quadriceps muscle strains. Magnetic resonance imaging features and prognosis. Am J Sports Med 2004;32:710-719.
21 Kassarjian A, Rodrigo RM, Santisteban JM. Intramuscular degloving injuries to the rectus femoris: findings at MRI. AJR 2014;202:W1-W6.
22 Rodrigo RM, Santisteban JM, Ortega R, Angulo F, Rodriguez M, Ereno MJ. Predictive value of MRI in rectus femoris strain injuries. Scientific presentation SSA 14-08. RSNA annual meeting, Chicago, IL, 2009.
23 Balius R, Maestro A, Pedret C et al: Central aponeurosis tears of the rectus femoris: practical sonographic prognosis. Br J Sports Med 2009;43:818-824.
24 Jansen JA, Cormier S, Patel JV. Acute rectus femoris rupture at the distal musculotendinous junction in a football player: a case report and surgical technique. Curr Orthop Practice 2012;23:390-392.
25 Ryan JB, Wheeler JH, Hopkinson WJ, Arciero RA, Kolakowski KR. Quadriceps contusions. West Point update. Am J Sports Med 1991;19:299-304.
26 Thorsson O, Lilja B, Nilsson P et al: Immediate external compression in the management of an acute muscle injury. Scand J Med Sci Sports 1997;7:182-190.
27 Verrall GM, Slavotinek JP, Barnes PG et al: Clinical risk factors for hamstring muscle strain injury: a prospective study with correlation of injury by magnetic resonance imaging. Br J Sports Med 2001;35:435-440.
28 Zeiss J, Saddemi SR, Ebraheim NA. MR imaging of the quadriceps tendon: normal layered configuration and its importance in cases of tendon rupture. AJR 1992;159:1031-1034.
29 Ferretti A. Epidemiology of jumper’s knee. Sports Med 1986;3:288-295.
30 Roth C, Jacobson J, Jamadar D, Caoili E, Morag Y, Housner J. Quadriceps fat pad signal intensity and enlargement on MRI: prevalence and associated findings. AJR 2004;182:1383-1387.
31 Nance EP, Kaye JJ. Injuries of the quadriceps mechanism. Radiology 1982;142:301-307.
32 Hak DJ, Sanchez A, Trobisch P. Quadriceps tendon injuries. orthopaedics 2010;33:40-46.
33 Wangwinyuvirat M, Dirim B, Pastore et al: Prepatellar quadriceps continuation: MRI of cadavers with gross anatomic and histologic correlation. AJR 2009;192:W111-W116.
34 Rask MR, Lattig GJ. Traumatic fibrosis of the rectus femoris muscle. JAMA 1972;221:268-269.
35 Temple HT, Kuklo TR, Sweet DE, Gibbons CLMH, Murphey MD. Rectus femoris muscle tear appearing as a pseudotumor. Am J Sports Med 1998;26:544-548.