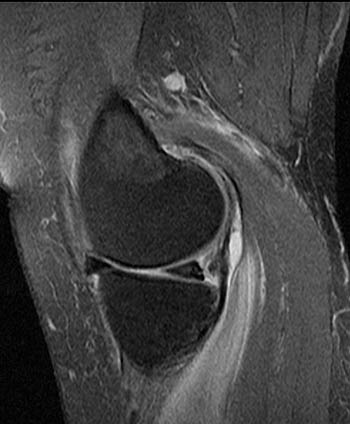
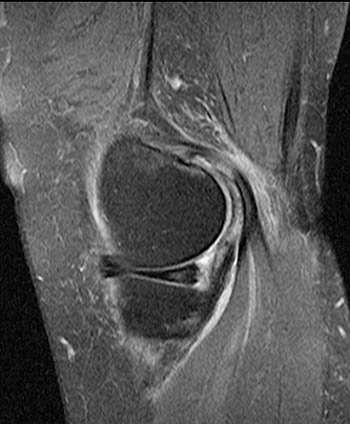
Clinical history: A 58 year old woman presents for MRI with right knee and leg pain and swelling medially for 3 weeks, without a specific injury. Sagittal proton density images with fat saturation at the medial aspect of the knee (1a,1b) are provided. What are the findings? What is the diagnosis?
Findings
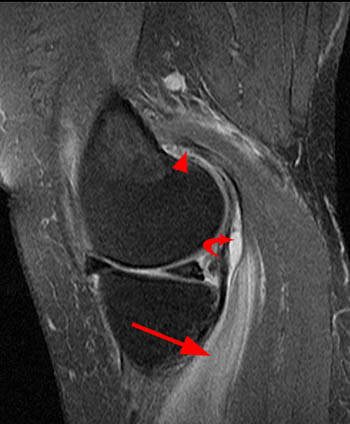
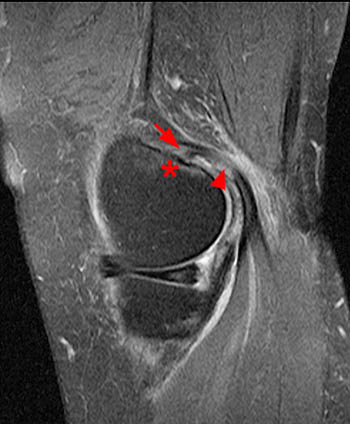
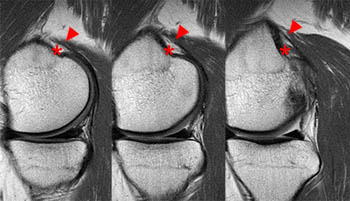
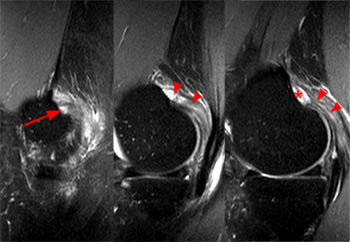
Figure 2:
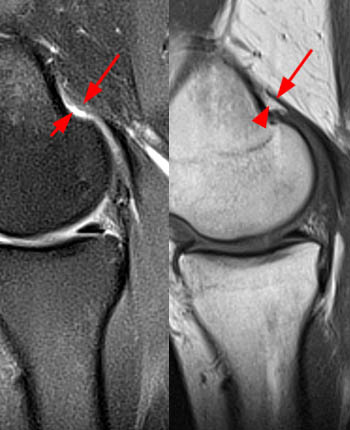
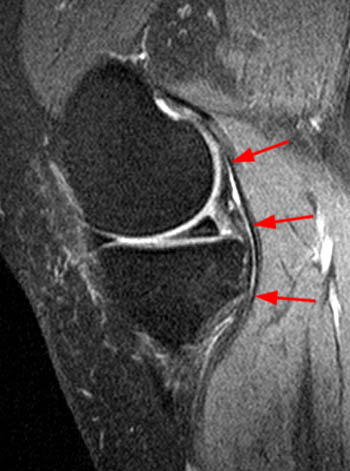
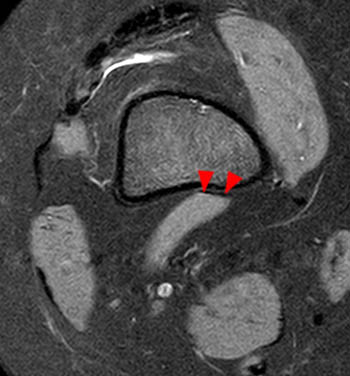
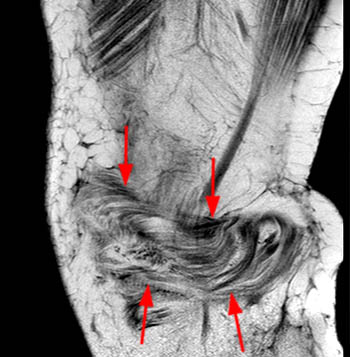
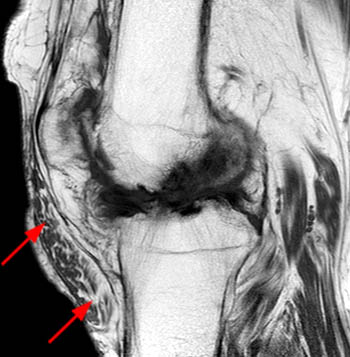
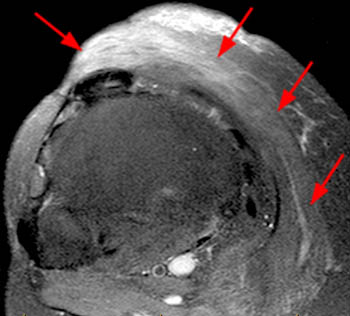
The sagittal proton density-weighted fat-suppressed MRI images through the medial aspect of the knee demonstrate intramuscular edema at the anteromedial aspect of the medial gastrocnemius (arrow), without intramuscular tear or hematoma. In addition, there is abnormality of the medial gastrocnemius tendon, with intratendinous high signal (short arrow, 2b), and focal surface fraying and contour abnormality (arrowheads). There is also femoral bone marrow edema deep to the tendon insertion (asterisk). Fluid is present in the gastrocnemius bursa (curved arrow, 2a), located anterior to the myotendinous region.
Diagnosis
1: Acute medial gastrocnemius muscle strain.
2: Chronic degenerative medial gastrocnemius tendinosis, with partial tearing of medial tendon fibers, and with femoral bone marrow edema.
3: Joint effusion, with fluid within the gastrocnemius-semimembranosus bursa.
Introduction
Abnormalities involving the medial and lateral gastrocnemius tendons are often not considered among the many possible causes of knee pain. The medial gastrocnemius is rarely affected in traumatic injuries to the knee, and symptomatic chronic degenerative changes are also relatively uncommon. However, case reports in the literature1,2, describe gastrocnemius tendon degenerative interstitial, longitudinal or partial-thickness tearing, and note that such abnormalities may cause clinical symptoms mimicking symptoms from more common lesions such as meniscal tears or collateral ligament strains. The medial and lateral gastrocnemius tendons proximal myotendinous regions are included in the field-of-view of knee MRI exams. Familiarity with the normal gastrocnemius tendon MRI features, as well as the spectrum of MRI findings with different types of pathology that may involve these structures is relevant for accurate interpretation of knee MRI.
Anatomy and Function
The medial and lateral gastrocnemius tendons together with the soleus muscle form the calf. The gastrocnemius muscles extend half-way down the lower leg, distally contributing to the Achilles tendon. The gastrocnemius muscles but not the soleus cross the knee joint, and they all distally cross the tibiotalar joint (and the subtalar joint as well). Innervation is by the tibial nerve. Vascular supply to the gastrocnemius muscles is by stout short branches from the adjacent popliteal artery and vein; detailed studies of the venous vascular configuration has demonstrated 4 main patterns, with 2 to 12 branches per muscle head3. The proximal tendons of the gastrocnemius muscles originate at the medial and lateral femoral epicondylar regions; the medial tendon is thicker along its medial margin and closer to midline contain small amounts of interspersed fat.
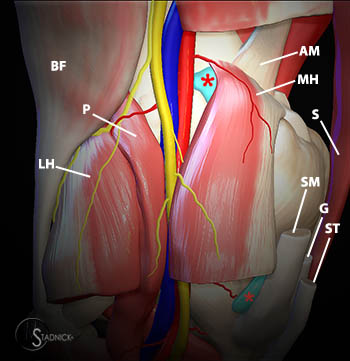
Figure 3:
A 3D representation of the popliteal fossa with partial resection of the semimembranosus (SM), gracilis (G), and semitendinosus (ST) musculotendinous junctions demonstrates the origin of the medial head of the gastrocnemius muscle (MH) with medial tendinous and muscular lateral portions, arising just posterior to the adductor magnus tendon (AM) insertion. The plantaris (P), lateral head of the gastrocnemius muscle (LH), and biceps femoris (BF), and sartorius (S) muscles are also labeled. The medial gastrocnemius bursa and semimembranosus bursa are indicated by asterisks.
The gastrocnemius bursa is located deep to the tendon in the proximal myotendinous region, and usually communicates with the semimembranosus bursa. Fluid in the bursa is frequent when there is gastrocnemius tendinopathy, but is non-specific as it also occurs with internal derangement of the knee joint and multiple other pathologies. When the gastrocnemius-semimembranosus bursa is distended, this is termed a Baker’s cyst, frequently communicating with the knee joint through a 15-20 mm slit between the two, thought to occur at a region of frequent capsular insufficiency, and sometimes with a one-way valve function leading to continuous filling of the cyst4.
The main gastrocnemius muscle function is plantar flexion of the foot, but it also provides flexion of the non-weight-bearing knee, and acts as an agonist for the PCL. The gastrocnemius muscles have a higher proportion of fast twitch fibers than the soleus, reflecting their function in jumping and running, while the soleus, with a higher proportion of slow twitch fibers, mainly functions in walking and postural control. In addition, all the calf muscles have a role as a venous pump for the lower limb (the “calf muscle pump” function)5.
Of interest, the gastrocnemius muscle bellies are known by bodybuilders to be quite difficult to hypertrophy. This has been attributed to the already high repetitive use of these muscles during daily activities.
Mechanism of Injury and Clinical Findings
Gastrocnemius tendon degeneration may result from prior gastrocnemius injury, chronic overuse, or underlying posteromedial or posterolateral knee joint instability. Gastrocnemius tendinosis may progress to an interstitial tear, longitudinal split tear, partial tear, or very rarely a complete tear. Clinical symptoms usually develop gradually and may include local pain and tenderness, as well as swelling at the posteromedial or posterolateral knee and proximal lower leg, weakness, and limited range of motion.
MRI evaluation
Normal MRI anatomy
The proximal tendons of the gastrocnemius muscles are flat, and originate at the medial and lateral femoral epicondylar regions in a linear fashion towards midline, slightly proximal to the condylar articular margin. At the medial gastrocnemius tendon origin, there are 2 features of importance for MRI evaluation: (1) the origin extends from the epicondyle (about 1 cm distal to the adductor magnus tendon insertion) and runs obliquely so that it is more proximal near the femoral posterior midline, and (2) the tendon is thicker and more defined medially, and more attenuated closer to femoral midline (4a,4b).
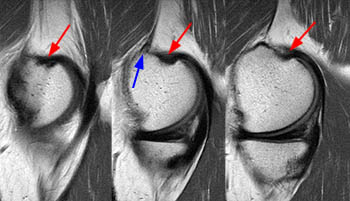
Figure 4:
Normal medial gastrocnemius tendon and myotendinous region in 21 year-old male. Six consecutive T1 weighted sagittal images demonstrate the thicker low-signal medial aspect of the tendon (arrows) inserting just posterior to the adductor magnus insertion and adductor tubercle (blue arrow, 4a), and the more attenuated tendon fibers towards the intercondylar region (arrowheads, 4b). Note the normal fat tissue deep to the tendon attachment (asterisks, 4b), present only at the lateral aspect of the origin.
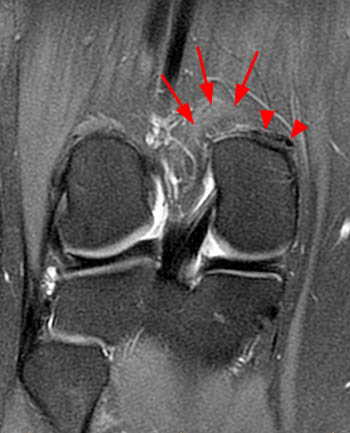
Figure 5:
A coronal proton density-weighted image with fat saturation obtained at the origin of the medial head of the gastrocnemius tendon demonstrates that the medial thicker tendinous portion has a linear low signal intensity configuration (arrowheads), while the lateral part of the medial head of the gastrocnemius origin is muscular (arrows).
A small amount of fat tissue is normally present deep to the tendon fibers towards the midline, and often a small amount of fluid is present normally at the adjacent recess at the posterior capsular femoral insertion (6a).
Figure 6:
Sagittal fat-suppressed proton density-weighted and T1-weighted images at the medial gastrocnemius tendon origin in a 41 year-old female without symptoms from the gastrocnemius tendon region, demonstrating a normal minimal amount of joint fluid (short arrow) at the posterior recess, and normal adjacent fat tissue (arrowhead) located next to the joint capsule and deep to the tendon fibers at the origin (long arrow).
On cross-sectional images, the low-signal tendon is seen at the medial to central aspects of the medial gastrocnemius, while closer to midline there is muscle to near the bony origin, with attenuated tendinous fascicles. The tendon remains well defined for only 1-2 cm distal to the medial joint line (7a).
A common finding at the medial gastrocnemius involves the muscle adjacent to the origin extending partly into the most proximal aspect of the intercondylar notch (8a). This is not known to be related to symptomatology.
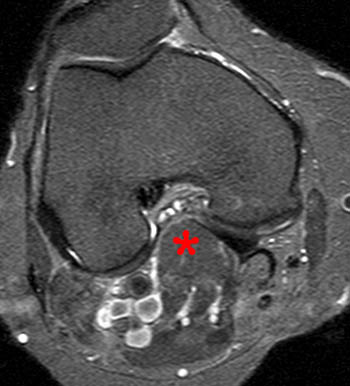
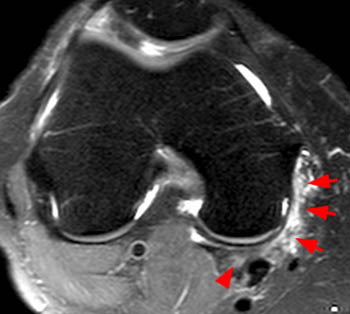
Figure 8:
An axial STIR image in a 55 year-old female with locking episodes at the right knee and an MRI exam demonstrating a radial tear at the medial meniscus (not shown). No posterior symptoms were reported. The medial gastrocnemius muscle belly (asterisk) is noted to extend slightly into proximal aspect of the intercondylar notch.
Abnormalities of the Gastrocnemius Tendon on MR images
It has been noted that symptomatic abnormalities at the proximal gastrocnemius tendon and myotendinous junction are rare. This is in contrast to the well-described more distal gastrocnemius muscle injury (“tennis leg”). The clinical significance of proximal tendon injury has also been questioned6. It is therefore not surprising that the MRI features of proximal gastrocnemius tendon injuries have rarely been reported in the literature1,2,7. The MRI findings associated with abnormalities of the proximal medial gastrocnemius tendon have been described to include high signal within the tendon on proton density and T2-weighted images, poorly defined tendon margins, and sometimes a contour defect usually involving the most medial tendon fibers, at or near the femoral origin (9a).
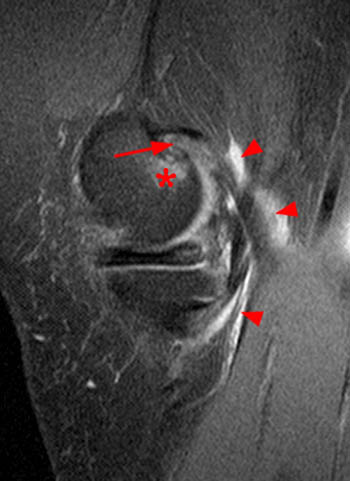
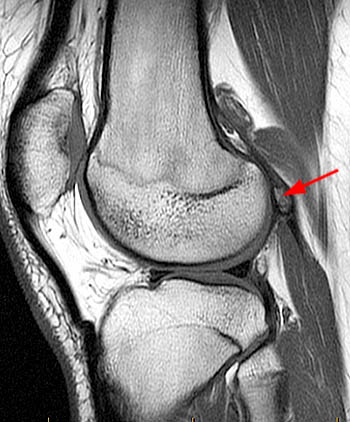
Figure 9:
A sagittal fat-suppressed proton density-weighted image in a 56-year old female with posteromedial knee pain demonstrates a partial avulsion at the medial margin of the medial gastrocnemius tendon (arrow), tendinosis, and femoral bone marrow edema deep to the region of avulsion (asterisk). There is fluid at the gastrocnemius-semimembranosus bursa (arrowheads).
Tendon thickening which can be focal or diffuse (10a,10b), or tendon attenuation may also be present. Intratendinous interstitial longitudinal tearing has also been reported2. Usually there is no associated proximal myotendinous muscle edema.
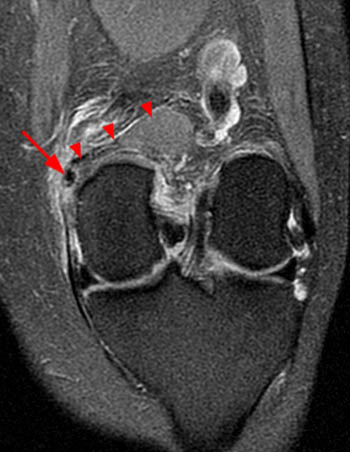
Figure 10:
A series of sagittal proton density-weighted images with fat saturation proceeding from medial to lateral and an axial proton density-weighted image with fat suppression (10a) demonstrate a partial insertional tear of the medial gastrocnemius tendon (arrows), with a longitudinal interstitial tendon tear seen as increased signal within the diffusely thickened tendon (arrowheads). Edema within fat deep to the attenuated fibers towards the midline (asterisk) is apparent. Associated medial pericapsular edema is also seen (short arrows, 10b).
A complete gastrocnemius tendon tear is quite rare in the setting of chronic tendinosis, and is also rare in cases of acute knee trauma. Fluid in the gastrocnemius bursa, located deep to the proximal tendon and immediately superficial to the posteromedial joint capsule, is associated with medial gastrocnemius tendon pathology but is non-specific as it is commonly found with many types of knee joint pathology.
It is important to consider the “magic angle” MRI artifact as a common cause of intratendinous intermediate signal within especially the medial gastrocnemius tendon. This artifact can be seen on short TE images (such as T1s) in regions where a tendon is oriented at 55 degrees to the main magnetic field, such as the medial gastrocnemius tendon about 2 cm distal to the femoral origin; correlation with T2 weighted images will help to exclude focal pathology (11a).
Figure 11:
Sagittal T1-weighted (TE=20 ms) and a corresponding STIR image in a 49 year-old male demonstrates focal intermediate signal on the T1-weighted image at a location in the medial gastrocnemius tendon making this suspicious for magic angle artifact; no abnormality is seen on the STIR image.
Differential Diagnoses
Focal symptoms from the proximal gastrocnemius tendon at its femoral origin may also be caused by HADD, the rarely reported acute gastrocnemius avulsion fracture8, or fabellar fracture with or without a related tendon tear9,10. Symptoms from the adjacent proximal myotendinous region may relate to retracted longitudinal partial tendon tears2, rare intramuscular dissecting Baker’s cysts11,12, or venous thrombosis limited to the calf muscle veins13.
Hydroxyapatite deposition disease (HADD) is a rare but well-described cause of acute knee pain14. The medial margin of the medial gastrocnemius tendon is characteristically involved (12a), with a low signal center and surrounding soft tissue edema. There is often adjacent mild reactive bone marrow edema and synovitis at adjacent joint or bursa. Correlation with radiographic exams is often useful, and resolution of the calcific deposit can be followed radiographically after therapy.
Figure 12:
An oblique fat-suppressed proton density-weighted image demonstrates a calcific deposit (arrow) at the medial margin of the medial gastrocnemius tendon in a 49 year-old woman with HADD. The remainder of the medial gastrocnemius is unremarkable (arrowheads). Soft tissue edema is present adjacent to the calcific deposit.
In calcium pyrophosphate crystal deposition disease (CPPD), in addition to chondrocalcinosis there is often calcification involving tendons. Around the knee, calcification of the medial gastrocnemius tendon has been reported15. Acute gastrocnemius avulsion fracture has rarely been described in the literature, and would result from an acute injury; if there is significant displacement, surgery may be indicated.
The fabella is a small sesamoid located within the lateral gastrocnemius at the level of the lateral femoral condyle. It is present in 10-20% of the population, and is usually ossified with a small facet of hyaline cartilage towards the joint, or may be fully cartilaginous (13a). It might show participation in osteoarthritis of the knee joint, with cartilage loss, subarticular marrow edema, and marginal osteophytes causing overall enlargement of the fabella which occasionally leads to localized pain related to impingement during knee flexion. Fabellar fracture9 or displacement10 are rare causes of acute posterolateral knee pain, while localized discomfort labeled “fabellar syndrome” has been described as a cause of insidious chronic symptoms, accessible to manual fabellar mobilization therapy16.
A dissecting Baker’s cyst11 may present with tender fullness at the posteromedial aspect of the knee just below the joint; these lesions represent rare instances where a Baker’s cyst enters through the muscle fascia and is present often both outside and within a muscle compartment. Normally a Baker’s cyst enlarges in the direction of least resistance, most commonly along the medial gastrocnemius muscle belly distally. If a focal fascial defect occurs, or at a pre-existing weak region, the Baker’s cyst can enter the muscle compartment. As with other Baker’s cysts, treatment of the underlying cause of the joint effusion is indicated, as the cysts are manifestations of fluid decompressing out of the joint due to higher intra-articular pressure.
Venous thrombosis of the lower leg most commonly involves the deep vessels and often also the calf muscle veins, and is often thought to originate at these muscle veins. A small percentage of cases demonstrate thrombosis limited to the calf muscle veins; these cases may present with symptoms similar to post-exertion calf muscle pain, and may be clinically mistaken for a muscle strain13.
Other abnormalities involving the gastrocnemius tendons or proximal myotendinous region include an accessory gastrocnemius muscle belly, post-surgical changes related to the use of the gastrocnemius for a vascular flap at a soft tissue defect around the knee, the rare use of a gastrocnemius silicone implant for cosmetic procedures, and soft tissue masses such as a lipoma.
Accessory gastrocnemius muscle bellies (“third head of the gastrocnemius”) have been associated with vascular claudication due to extrinsic vascular functional compression or entrapment17, though the majority of these congenital lesions are asymptomatic (Figure 14). MR angiography has proven useful for evaluation of suspected popliteal artery entrapment syndrome18.
Figure 14:
Fat-suppressed proton density-weighted axial (14a,14b) and sagittal images (14c) demonstrate an accessory medial gastrocnemius muscle belly in a 17 year-old asymptomatic patient. The accessory belly has a femoral midline origin at the femur (arrowheads) well proximal to the origin of the medial and lateral heads, with the two medial heads (asterisks) surrounding the popliteal artery (A) and vein (V) and the tibial nerve (N).
Unusual distribution of muscle tissue around the knee (Figure 15) may be related to prior reconstructive surgical procedures. It has been stated that the medial gastrocnemius muscle flap is the workhorse of all muscle flaps around the knee19, due to the proximal entry of the main arterial and venous (sural) branches and the tibial nerve supply, the considerable size and length of the muscle belly, and that its transfer does not significantly impair knee joint function.
Figure 15:
Sagittal T1-weighted (15a,15b) and axial proton density-weighted fat suppressed (15c) images demonstrate muscle with partial fatty replacement at the medial aspect of the knee in a 74 year-old male with a history of myocutaneous rotational flap surgery, using the medial gastrocnemius muscle belly (arrows) to cover a prior soft tissue defect of the anteromedial knee. The distally detached muscle region is present anterior to the patellar tendon.
Surgical release procedures with tenotomy or myofascial recession have been developed for the gastrocnemius tendons in cases of resistant contracture, or spasticity related to cerebral palsy. Another surgical procedure involving the proximal gastrocnemius region involves muscle augmentation using silicone gastrocnemius implants placed in the submuscular plane between the gastrocnemius and the soleus20.
Soft tissue masses including intermuscular lipoma (16a,16b) and intramuscular lipoma may involve the proximal gastrocnemius tendon and muscle, and may be asymptomatic or present as a non-tender mass.
Figure 16:
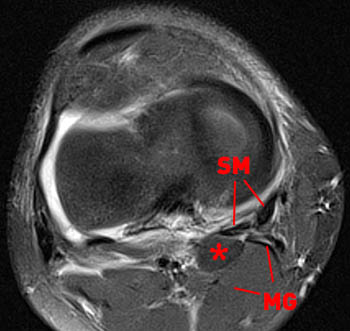
Sagittal T1-weighted (16a) and axial proton density-weighted fat-suppressed (16b) images demonstrate an asymptomatic posteromedial intermuscular lipoma (asterisk) ventral to the medial gastrocnemius muscle and tendon (MG) in a 25 year-old male runner who underwent MR imaging after a running injury. The semimembranosus tendon (SM) is also indicated.
Treatment
The treatment for symptomatic medial or lateral gastrocnemius proximal tendinosis is usually conservative, including rest from strenuous activities. Physical therapy may be indicated, aiming to reduce inflammation and improve range of motion. Rarely, surgical repair has been described in cases of retracted acute tendon tears.
Conclusion
Degenerative proximal tendinosis at the medial or lateral gastrocnemius may develop into interstitial or partial-thickness tendon tearing. These abnormalities may co-exist with the more common causes of knee pain such as meniscal tear or osteoarthritis, or may be the only abnormality demonstrated on an MRI examination of the knee. Gastrocnemius tendons may demonstrate MRI signal changes attributed to magic angle artifact, but when there is high T2 signal within the tendon, contour change or defect, and associated edema at bone marrow and soft tissues, gastrocnemius tendinopathy can be diagnosed on knee MRI exams, and may well be contributing to the patient’s clinical symptoms.
References
1 Watura C, Ward A, Harries W. Isolated partial tear and partial avulsion of the medial head of the gastrocnemius tendon presenting as posterior medial knee pain. BMJ Case Reports 2010; 10:1136
2 Watura C, Harries W. Isolated tear of the tendon to the head of gastrocnemius presenting as a painless lump in the calf. BMJ Case Reports 2009: 1468
3 Aragao JA, Reis FP, Pitta GBB et al. Anatomical study of the gastrocnemius venous network and proposal for a classification of the veins. Eur J vasc endovasc surg 2006;31:439-442
4 Rauschning W. Popliteal cysts and their relation to the gastrocnemius-semimembranosus bursa: studies on the surgical and functional anatomy. Acta orthopaedica Scandinavica 1979:179:1-43
5 Stick C, Grau H, Witzleb E. On the edema-preventing effect of the calf muscle pump. European Journal of Applied Physiol Occup Physiol 1989:59:39-47
6 Armfield DR, Kim DH-M, Towers JD et al. Sports-related muscle injury in the lower extremity. Clin Sport Med 2006:25:803-842
7 Bencardino JT, Rosenberg ZS, Brown RR, Hassankhani A, Lustrin ES, Beltran J. Traumatic Musculotendinous Injuries of the Knee: Diagnosis with MR Imaging. RadioGraphics October 2000, 20:103-120
8 Maehara H, Sakaguchi Y. Avulsion fracture of the medial head of the gastrocnemius muscle. A case report. J Bone Joint Surg Am 2004:86-A:373-375
9 Bareto ARF, Chagas-Neto FA, Crema MD et al: Fracture of the Fabella: a rare injury in knee trauma. Case Reports in Radiology 2012: ID 390150, 3 p (www.hindawi.com/crim/radiology/2012/390150)
10 Frey C, Bjorkengren A, Sartoris D, Resnick D. Knee dysfunction secondary to dislocation of the fabella. Clin Orthop 1987:222:223-227
11 Nicholson LT, Freedman Hl. Intramuscular dissection of a large ganglion cyst into the gastrocnemius muscle. orthopaedics July 2012:35(7):1122-1124
12 Fang CSJ, McCarthy CL, McNally EG. Intramuscular dissection of Baker’s cysts: report on three cases. Skeletal Radiology 2004:33:367-371
13 Krunes U, Teubner K, Knipp H et al. Thrombosis of the muscular calf veins – reference to a syndrome which receives little attention. Journal of Vascular Diseases August 1998:172-175
14 Quinn SF. Hydroxyapatite Deposition Disease. Radsource Web Clinic, March 2009 (www.radsource.us/clinic/0903)
15 Foldes K, Lenchik L, Suphaneewan J et al. Association of gastrocnemius tendon calcification with chondrocalcinosis of the knee. Skeletal Radiology 1996:25:621-624
16 Zipple JT, Hammer RL, Loubert PV. Treatment of Fabellar Syndrome with manual therapy: a case report. J Orthop Sports Ther 2003:33: 1-7
17 Koplas MC, Grooff P, Piraino D, Recht M. Third head of the gastrocnemius: an MR imaging study based on 1,039 consecutive knee examinations. Skeletal Radiology 2009:38:349-354
18 Sookur PA, Naraghi AM, Bleakney RR et al. Accessory muscles: anatomy, symptoms, and radiologic evaluation. RadioGraphics March 2008:481-499
19 Quader AR, Shaxawan S. The gastrocnemius muscle flap used as cover for exposed upper tibia. Duhok Medical Journal 2010, 4:60-66
20 Kalixto MA, Vegara R: Submuscular calf implants. Aesth. Plast. Surg. 2003:27:135-138