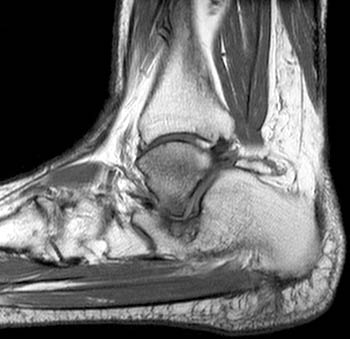
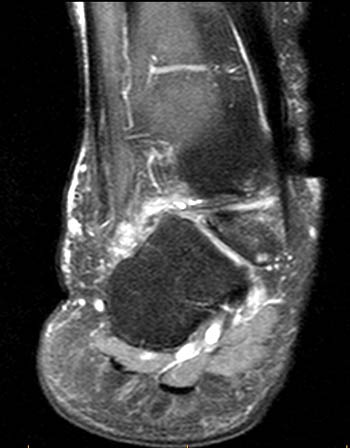
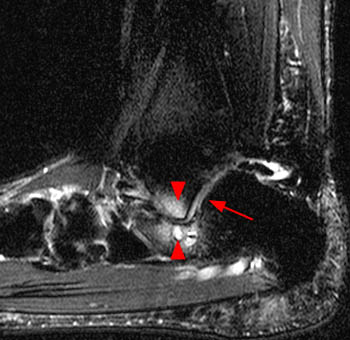
Clinical History: A 52 year-old man presents with history of 10 years of right ankle pain, and clinical suspicion of subtalar arthritis. Sagittal T1- and fat-suppressed T2-weighted (1a,1b), and coronal fat-suppressed proton density-weighted (1c,1d) images are shown below. What are the findings, and what is your diagnosis?
Findings
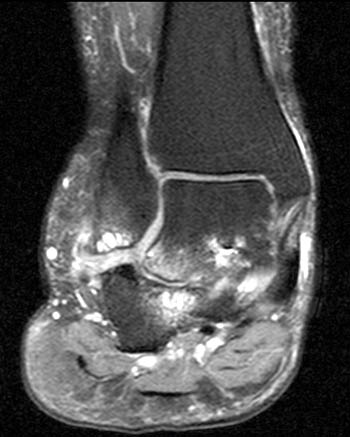
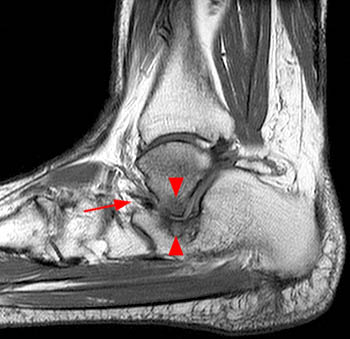
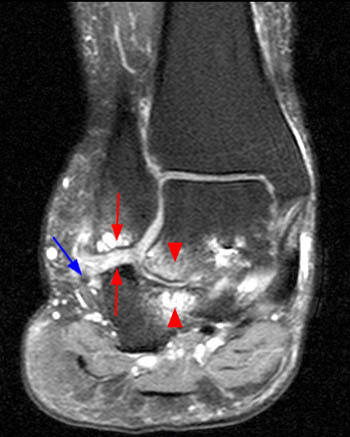
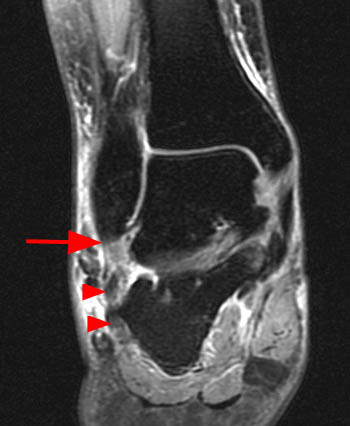
Figure 4:
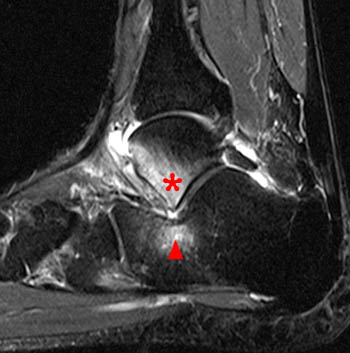
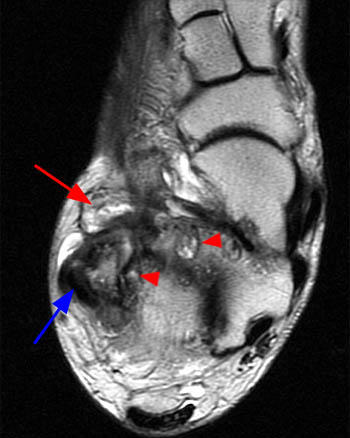
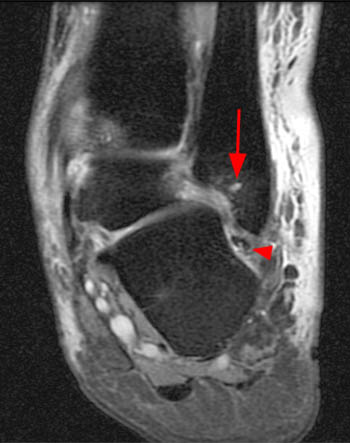
A coronal fat-suppressed proton density-weighted image obtained just anterior to the posterior subtalar joint reveals the extra-articular subcortical bone marrow edema and cystic changes at both the talocalcaneal region (arrowheads), and the calcaneofibular region, with bony remodeling and flat neo-facets at the fibula distally and at the adjacent lateral calcaneus (red arrows). There is peroneal tendinosis (blue arrow), and edema at interposed lateral soft tissues.
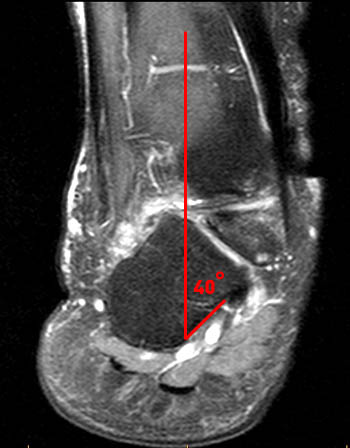
Figure 5:
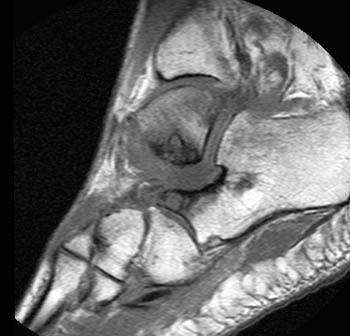
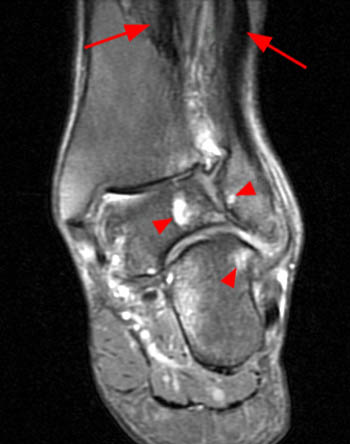
A posterior coronal view demonstrates that severe heel valgus is present, with an abnormal, 40 degree angle between the medial calcaneal cortex and the long axis of the tibia, measured just posterior to the sustentaculum at the level of the posterior talus and tibia. As the MR was not obtained during weight-bearing, the measurement may underestimate the extent of functional malalignment.
Diagnosis
Lateral hindfoot impingement, with extra-articular talocalcaneal impingement and subfibular (calcaneofibular) impingement.
Introduction
Pain localized to the lateral subtalar region is often clinically felt to represent either subtalar joint degeneration or sinus tarsi syndrome. CT and MR imaging of patients with lateral hindfoot symptoms have demonstrated features of extra-articular osseous impingement laterally, involving the talus, calcaneus and fibula. These manifestations have been termed “lateral hindfoot impingement”1,2,3,4. Similar terms such as “sinus tarsi impingement”, “talocalcaneal impingement” and “subtalar impingement” have also been used in the orthopaedic literature.
Lateral hindfoot impingement is characteristically not related to an acute injury, but to chronic hindfoot valgus malalignment. This hindfoot malalignment is often due to posterior tibial tendon insufficiency, as this tendon is crucial in maintaining the longitudinal arch of the foot. The resulting hindfoot valgus malalignment is one of the components of acquired flatfoot deformity (pes planovalgus), and in severe cases a progressive lateral calcaneal subluxation occurs, such that the calcaneus may contact the fibula during weight-bearing.
Clinical Presentation
Posterior hindfoot impingement most commonly occurs in middle-aged and older individuals with a chronic hindfoot valgus deformity. Symptoms often include hindfoot pain on weight-bearing, swelling and tenderness in the region anterior and inferior to the lateral malleolus, and limited subtalar range of motion. These clinical symptoms are not specific and may also be encountered in patients with subtalar degenerative arthritis, sinus tarsi syndrome, and other disorders affecting the hindfoot region.
Posterior tibial tendinopathy is a common cause of hindfoot valgus deformity. The prevalence of lateral hindfoot impingement has been found to increase with higher grades of posterior tibial tendon tear2. Patients with posterior tibial tendon dysfunction experience both pain and disability. The pain is initially located along the medial aspect of the foot, often associated with swelling due to tenosynovitis. With progressive collapse of the longitudinal arch and development of a hindfoot valgus deformity, lateral foot pain develops, found to frequently relate to extra-articular talocalcaneal or calcaneofibular impingement1. The relative frequency of lateral hindfoot impingement, or the severity of hindfoot deformity required before the impingement occurs, are not known1.
Affected patients may also experience subluxation or dislocation of the peroneal tendons, causing a popping sensation at the posterior margin of the lateral malleolus. This instability is not related to the lateral impingement, but rather is caused by severe hindfoot valgus malalignment, and resultant overactivity of the unopposed peroneus brevis in the presence of posterior tibial tendon insufficiency.
Normal Anatomy
Lateral hindfoot impingement involves the anatomic structures at the junction of the posterior subtalar joint and the posterolateral margin of the sinus tarsi, including the lateral malleolus.
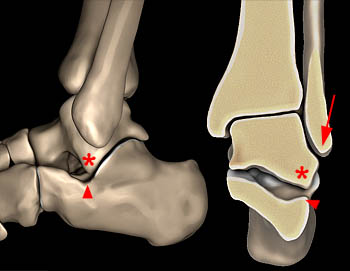
Figure 6:
A 3D representation of the normal appearance of the structures involved with lateral hindfoot impingement. On the left a lateral view of the ankle shows the normal space between the lateral talar process (asterisk) and the calcaneal angle of Gissane (arrowhead). The image on the right depicts the plane just anterior to the posterior subtalar joint demonstrating normal alignment and spacing between the lateral talus (asterisk), the lateral calcaneus (arrowhead), and the lateral malleolus (arrow).
The sinus tarsi is a non-articular cone-shaped passage between the talus and calcaneus, with a larger opening towards its lateral aspect. The sinus tarsi is located immediately anterior to the posterior subtalar joint, and is separated from this joint by the joint capsule and the short but stout talocalcaneal interosseous ligament. Anteriorly, the sinus tarsi extends to the margin of the talocalcaneal (anterior subtalar) joint, and medially it extends to the middle facet of the subtalar joint. The sinus tarsi contains mostly fat, but also small vascular and nerve branches, the cervical ligament, and the 3 roots combining to form the inferior extensor retinaculum, located towards the anterolateral margin of the sinus tarsi. Normally the sinus tarsi extends into a small space between the apex of the lateral process of the talus and the adjacent calcaneus, just anterior to the posterior subtalar joint margin, and the adjacent talar lateral process is normally rounded or slightly pointed, without a flat facet (8a,9a).
The “critical” angle of Gissane was devised on lateral radiographs to evaluate calcaneal fractures, as commonly the talar lateral process is driven downward into the adjacent relatively weak part of the calcaneus5. The angle is measured using a line along the superior calcaneal cortex at the body and anterior calcaneal process, and another line along the posterior articular facet of the calcaneus (8a); normally it measures around 130 degrees. The apex of the angle of Gissane is at the location of chronic talar impact with lateral hindfoot impingement, and this is the center of the bony changes, therefore the angle of Gissane, or “calcaneal angle” can be used as a term to identify the calcaneal location of pathology. The actual angle measurement is not critical and indeed typically remains normal in hindfoot impingement cases.
The fibula normally does not extend distally to near the lateral cortex of the calcaneus in the plane of the lateral process of the talus. With valgus malalignment the calcaneus may sublux and rotate laterally, resulting in direct osseous contact with the fibula.
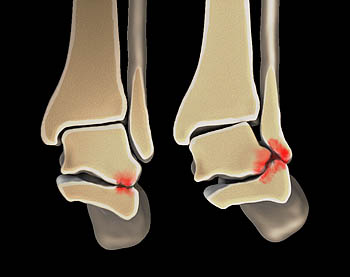
Figure 7:
3D representation in the coronal plane just anterior to the posterior subtalar joint demonstrates changes of lateral hindfoot impingement. On the left the lateral talus impacts the lateral calcaneus. With more severe hindfoot valgus and lateral calcaneal subluxation additional impingement may occur between the lateral malleolus and lateral calcaneus as depicted on the right.
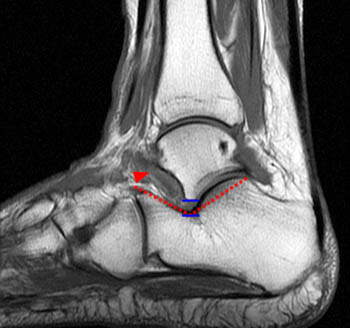
Figure 8:
A sagittal T1-weighted image of the ankle in a 54 year-old woman demonstrates normal talocalcaneal alignment, with a normal small interval between the apex of the lateral talar process and the calcaneus at apex of the angle of Gissane (blue lines). Dotted red lines demonstrate the landmarks for measuring the angle of Gissane. An unremarkable cervical ligament at the sinus tarsi, with adjacent normal fat signal is indicated (arrowhead).
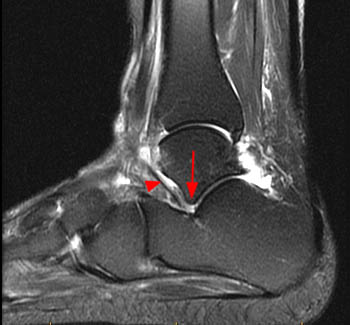
Figure 9:
The corresponding fat-suppressed T2-weighted image demonstrates the normal rounded to slightly pointed apex of the lateral talar process (arrow), and the unremarkable cervical ligament (arrowhead). Normal minimal fluid is present at the posterior subtalar joint, without capsular distension into the sinus tarsi.
Figure 10: A fat-suppressed proton density-weighted image, obtained coronal to the apex of the angle of Gissane in a 54 year-old woman showing normal talocalcaneal alignment, with a normal interval between the lateral malleolar tip and the lateral calcaneus (arrow), and normal position of the peroneal tendons (arrowheads).
Pathophysiology
Subluxation at the talocalcaneal joint has been shown to occur in symptomatic adults with acquired flat foot, involving a lateral translocation of the calcaneus into valgus malalignment, with the subluxation greater at the anterior and middle talocalcaneal articular facets than at the posterior facet, leading to reduction of articular contact surfaces at these joints6. This subluxation causes a change in the overall shape of the foot, with flattening of the longitudinal arch, valgus of the hindfoot, and abduction of the forefoot6. With a significant hindfoot valgus deformity, there will be a lateral shift of the main weightbearing forces at the ankle and hindfoot, from the talar dome towards the lateral talus and also to the fibula7. If excessive, this can result in subtalar pathology including degenerative arthritis, sinus tarsi syndrome, or extra-articular bony contact as with lateral hindfoot impingement.
Regarding the frequent association with posterior tibial tendinopathy, it should be emphasized that an acquired flat foot deformity may develop without a complete tendon tear and distraction, as functional insufficiency may present at earlier stages such as with a grade 1 interstitial tear (11a).
MRI Findings
Osseous findings of lateral hindfoot impingement include extra-articular subcortical bone marrow edema at specific locations at the talus, calcaneus or fibula. Also frequently present are cystic changes at the bone marrow at these same locations, and subcortical sclerosis at bony contact surfaces.
In reported cases, the incidence of calcaneofibular impingement was somewhat lower than talocalcaneal impingement, with calcaneofibular impingement present almost exclusively in individuals who also had talocalcaneal impingement, suggesting that the talocalcaneal osseous changes occur before the calcaneofibular changes.
Subcortical bone marrow edema characteristically involves both opposing aspects of the talus, calcaneus, or fibula (3a). The location of the bone marrow edema is characteristic, at the extra-articular region at the inferior apex of the lateral talar process and at the immediately subjacent aspect of the calcaneus at the apex of the angle of Gissane (12a). The bony changes sometimes are seen to also involve the adjacent subcortical region of the anterosuperior calcaneal process (13a), however if bone marrow edema is present all along the cortex around the margins of the sinus tarsi, this would not be characteristic and would instead suggest a diagnosis of sinus tarsi syndrome.
Figure 13:
A sagittal fat-suppressed T2-weighted image in 70 year-old woman with clinical symptoms of posterior tibial tendon insufficiency and lateral hindfoot pain, shows extra-articular distribution of bone marrow edema at lateral talar process (arrow), with a small flat facet at the distal apex, and with subcortical calcaneal bone marrow edema extending anteriorly (arrowhead).
The subcortical cystic changes are not always present, but are frequent and usually are multiple, small and rounded, and are located at regions of maximal bony impact, histologically representing bony resorption and cystic necrosis. Subcortical sclerosis, representing regions of bone formation replacing marrow fat, is seen as low signal on both T1 and T2-weighted images, located at region of maximal bony impact, often with adjacent bone marrow edema (14a). With more advanced changes, there will be cortical remodeling leading to flattening of the bony contours at the contact site, and “neofacet” formation (15a).
Figure 14:
A T1-weighted sagittal image in a 61 year-old male with lateral hindfoot pain, demonstrating mild sclerosis at the lateral talar process (arrowhead) and adjacent calcaneus. The corresponding T2-weighted images (not shown) demonstrated adjacent mild bone marrow edema and very subtle cystic changes in this region as well.
Figure 15:
A T1-weighted sagittal image in a 65 year-old female with cortical remodeling with bone loss and "neofacet" formation at both the lateral talar process and the calcaneus, as well as subcortical sclerosis. Note the absence of signs of osteoarthritis at the adjacent posterior subtalar joint.
Soft tissue features of lateral hindfoot impingement include soft tissue edema located at the most posterior aspect of the sinus tarsi, interposed at the region of talocalcaneal impingement at the angle of Gissane, often also with edema at soft tissues at the adjacent subfibular region (16a). The calcaneofibular ligament may become entrapped in calcaneofibular impingement, as it courses from the fibula to the calcaneus (17a).
Peroneal tendon subluxation or dislocation has been reported in association with more severe cases of lateral hindfoot impingement2 (16a), leading to tenosynovitis and tendinosis with possible longitudinal split tears or complete tendon tears.
Figure 16:
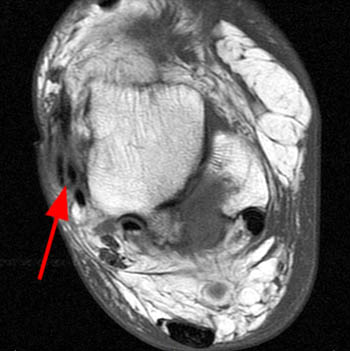
An axial T2-weighted image in 60 year-old male with symptomatic lateral hindfoot impingement including calcaneofibular impingement, also with lateral dislocation of the peroneal tendons which are located lateral to the most distal aspect of the fibula (blue arrow). Bone marrow cystic changes are present at the lateral talar process and the calcaneofibular region (arrowheads), and soft tissue fullness and edema is noted at the lateral soft tissues of the hindfoot (red arrow).
Figure 17:
A fat-suppressed coronal proton density-weighted image in 71 year-old woman with lateral hindfoot impingement related to posterior tibial tendinopathy and hindfoot valgus, demonstrates entrapment of the calcaneofibular ligament (arrowhead). Bone marrow cystic changes are present at the deep aspect of the fibula (arrow).
Hindfoot valgus malalignment is a requisite for lateral hindfoot impingement to develop. The hindfoot valgus angle is likely to be underestimated when measured on MR images obtained with the patient supine, due to the absence of weight bearing forces on the ankle. In addition, there are challenges obtaining measurements at a consistent location due to anatomic variations.
The MRI hindfoot valgus angle measurement suggested in the literature has been adapted from methods using frontal weight-bearing radiographic studies and CT reconstruction exams. It is calculated as the angle between the long axis of the tibia, and the border of the calcaneal medial cortex (D)2. The measurement is performed on the most posterior coronal image that includes both the tibia and calcaneus, taking care not to use an image through the calcaneal sustentaculum tali as that would increase the angle. The medial, rather than the lateral, calcaneal wall is selected for MR measurements because it has less variability and fewer bony protuberances. Hindfoot valgus on MRI has been graded as mild (7-16°), moderate (17-26°), and severe (> 26°), with normal at 0-6 degrees2. This measurement has limitations related to the short segment of tibia included on ankle MRI exams being insufficient for an accurate long axis determination, and the medial wall of the calcaneal tuberosity gradually slopes towards vertical also in cases of severe valgus malalignment, so it is important to perform the measurement between the sustentaculum and the calcaneal tuberosity; available slice selection also somewhat limits reproducibility.
Differential Diagnosis
The main imaging differential diagnosis for lateral hindfoot impingement is sinus tarsi syndrome. It can be difficult to separate findings of sinus tarsi syndrome from those of lateral hindfoot impingement, and some authorities consider these to represent aspects of the same lateral subtalar impingement pathology. The characteristic findings of sinus tarsi syndrome have been described as diffuse edema throughout the sinus tarsi, sometimes with mild bone marrow edema extending along the subcortical region around the sinus tarsi, also with indistinctness compatible with degeneration and scarring at the cervical and interosseous ligaments (18a, 19a)8.
An increased incidence of hindfoot valgus collapse is seen in individuals with inflammatory arthropathy, including rheumatoid arthritis and psoriatic arthropathy, related to a higher risk of tibialis posterior tendon tear related to long-standing inflammation at the tendon sheath and adjacent joints. The marginal erosions of RA may also mimic the bony changes of lateral hindfoot impingement but erosions and synovitis are generally also present elsewhere, clarifying the diagnosis. Rarely a hindfoot deformity with lateral bony impingement may result from prior displaced hindfoot fracture (20a).
Calcaneal intraosseous ganglion formation or prominence of vascular structures may mimic the calcaneal changes of lateral hindfoot impingement, but no osseous abnormalities would be expected at the adjacent lateral talar process (21a)9.
Figure 20:
A fat-suppressed coronal proton density-weighted image in a 53 year-old woman with sequelae of remote displaced fractures (arrows) with a hindfoot valgus fixed deformity and 2 year history of diffuse ankle pain. Talofibular as well as calcaneofibular extra-articular bony impingement with subcortical bone marrow edema (arrowheads) is present.
Treatment
Recommended therapy for lateral hindfoot impingement usually involves surgery, due to the difficulty to stabilize a valgus deformity of the hindfoot with conservative measures such as medial wedge inlays or orthotics. At an earlier stage, physical therapy with Achilles tendon stretching may be warranted in cases of symptomatic flexible flatfoot. With a fixed deformity, or significant malalignment, surgery including calcaneal osteotomy is usually required and may provide hindfoot realignment without the restriction of movement of a fusion. Alternatively, rearfoot fusions such as triple arthrodesis may be required to realign and provide pain-free stability10.
Arthroereisis is a surgical technique which aims to limit motion at a hypermobile joint. The procedure has evolved from early use of a bone block placed into the sinus tarsi for extra-articular arthrodesis, to placement of a metal or plastic implant configured to specifically block the anterior translation of the lateral talar process towards the floor of the sinus tarsi, aiming to limit hindfoot eversion11.
Conclusion
Lateral hindfoot impingement is an extra-articular osseous impingement affecting the talus, calcaneus and distal fibula. Its development relates to hindfoot valgus malalignment, and a lateral shift of the calcaneus which may lead to abnormal bony contact between the talus and calcaneus specifically at the posterior peripheral margin of the sinus tarsi, and sometimes also the development of “neofacets” at the sinus tarsi, as well as at the fibula and adjacent calcaneus. The predominant MR features of this diagnosis are bone marrow edema and bony cystic changes, located at the apex of the lateral talar process and the calcaneus at the apex of the angle of Gissane. Treatment often requires surgery to realign and stabilize the hindfoot. Some overlap with sinus tarsi syndrome MRI features has been suggested, and indeed some orthopaedic ankle authorities use the term “sinus tarsi impingement” for this clinical picture, characteristically associated with chronic symptomatic pes planovalgus, congenital or acquired through posterior tibial tendinopathy.
References
1 Talocalcaneal and subfibular impingement in symptomatic flatfoot in adults. Malicky ES, Crary JL, Houghton MJ et al. Journal of Bone and Joint Surgery (Am) 2002 November 84-A: 2005-2009 http://www.jbjs.org/article.aspx?Volume=84&page=2005 (full text)
2 Extra-articular lateral hindfoot impingement with posterior tibial tendon tear: MRI correlation. Donovan A, Rosenberg ZS. American Journal of Radiology, September 2009, Vol. 193: 672-678 http://www.ajronline.org/content/193/3/672.full (full text)
3 MRI of Ankle and Lateral Hindfoot Impingement Syndromes. Donovan A, Rosenberg ZS. American Journal of Radiology, September 2010, Vol. 195: 595-604 http://www.ajronline.org/content/195/3/595.full (full text)
4 Accessory Anterolateral Talar Facet as an Etiology of Painful Talocalcaneal Impingement in the Rigid Flatfoot: A New Diagnosis. Jeffrey E. Martus, John E. Femino, Michelle S. Caird et al. Iowa Orthop J. 2008; 28: 1-8. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2603342/
5 Fractures of the Calcaneus: A Review with Emphasis on CT. Daftary A, Haims AH, and Baumgaertner MR. Radiographics25, September 2005:1215-1226 http://radiographics.rsna.org/content/25/5/1215.full (full text)
6 Subluxation of the talocalcaneal joint in adults who have symptomatic flatfoot. Ananthakrisnan D, Ching R, Tencer A, Hansen ST Jr, Sangeorzan BJ. J Bone Joint Surg Am. 1999 Aug;81(8):1147-54. http://www.jbjs.org/article.aspx?volume=81&page=1147 (full text)
7 The effects of adult acquired flatfoot deformity on tibiotalar joint contact characteristics. Friedman MA, Draganich LF, Toolan B, Brage ME. Foot Ankle Int. 2001 Mar;22(3):241-6. http://www.ncbi.nlm.nih.gov/pubmed/11310867?dopt=Abstract
8 Tarsal sinus: arthrographic, MR imaging, MR arthrographic and pathologic findings in cadavers and retrospective study data in patients with sinus tarsi syndrome. Lektrakul N, Chung CB, Lai Y et al. Radiology 219, June 201:802-810. http://radiology.rsna.org/content/219/3/802.full
9 Incidence and morphologic characteristics of benign calcaneal cystic lesions on MRI. Elias I, Zoga AC, Raikin SM, et al. Foot Ankle Int. 2007 Jun; 28(6):707-14.
10 Therapeutic management of flexible flatfoot pain. Blitz N, Hanulewicz P. Lower Extremity Review, July 2010
http://www.lowerextremityreview.com/article/therapeutic-management-of-flexible-pes-planovalgus
11 Pediatric and adult flatfoot reconstruction: subtalar arthroereisis versus realignment osteotomy surgical options. Soomekh DJ, Baravarian B. Clin Podiatr Med Surg. 2006 Oct;23(4):695-708 http://www.ncbi.nlm.nih.gov/pubmed/17067888