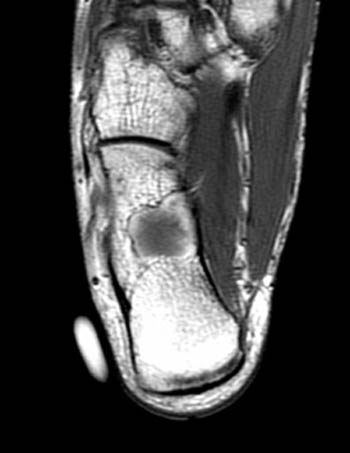
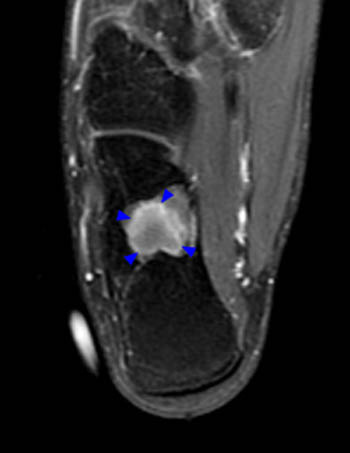
Clinical History: A 16 year old male complains of intermittent right heel pain for 7 years, with a recent increase after sports activities. Plain radiographs suggest a “bone cyst”. (1a,1b) Sagittal and axial T1-weighted and (1c,1d) STIR images were obtained. What are the findings? What is the diagnosis?
Findings
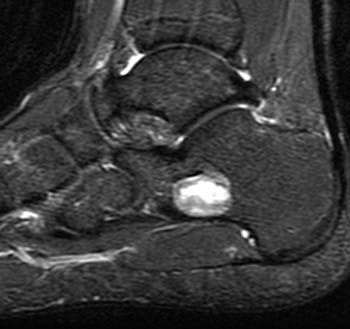
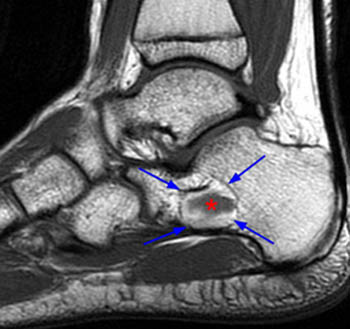
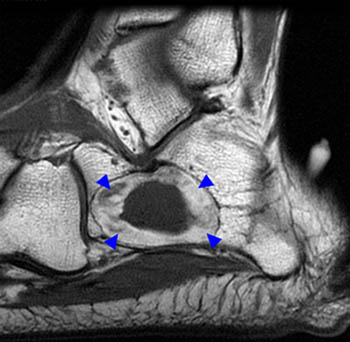
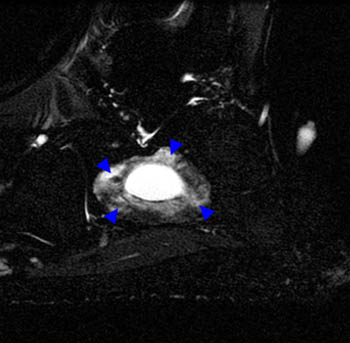
Figure 2:
The (2a) sagittal and (2b) axial T1-weighted images demonstrate a geographic, peripherally sclerotic lesion (arrows) with a hyperintense outer layer suggestive of fat. Central low signal intensity (asterisks) is suggestive of fluid. The corresponding inversion recovery (2c) sagittal and (2d) axial views confirm the presence of fat due to the suppression of the outer rim (arrowheads). The presumed central fluid (asterisks) demonstrates expected high signal intensity.
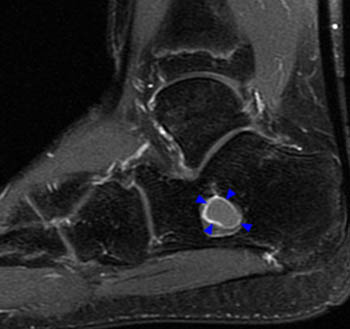
Figure 3:
Post-contrast images were also obtained. The post-contrast fat-suppressed T1-weighted (3a) sagittal and (3b) axial images demonstrate enhancement at the interface (arrowheads) between the outer fatty and inner fluid components. No other internal or extra-lesional calcaneal enhancement is noted. Overall, the well defined appearance and differentiation of various layers of tissues, in concert with the absence of subjacent reactive marrow edema, cortical breakthrough, or soft tissue mass, strongly indicates a benign etiology.
Diagnosis
Calcaneal Intraosseous Lipoma.
Introduction
The intraosseous lipoma is the most common lipogenous lesion of bone. Intraosseous lipoma is found most frequently in the intertrochanteric region of the proximal femur (34%), with the calcaneal intraosseous lipoma being the next most prevalent, found in 8-15% of cases.1,4 The high incidence of proximal femoral and calcaneal sites is considered to be a function of the relative paucity of trabecular bone in both of these locations, a characteristic that is also responsible for the “pseudolesion” appearance seen on radiographs at these sites. The sparse trabecular bone at the anteroinferior calcaneus has led to the supposition that intraosseous lipomas represent an “overshoot” phenomenon that develops during the transition of hematopoietic to fatty marrow, and therefore that intraosseous lipomas in these sites might more correctly be considered hamartomas rather than neoplasms.2,3 Many of these lesions are found incidentally in the calcaneus on routine radiographs, however a significant percentage of these lesions present due to pain, which is reported up to 66% of the time.4 The symptoms may result from remodeling of bone due to expansion, or due to intralesional ischemia, noted to be a common pathogenetic consequence of a long-standing calcaneal intraosseous lipoma.
Pathology and Staging
On gross examination, intraosseous calcaneal lipomas are pale or bright yellow and may possess a thin surrounding capsule.2,4 There may be thin septa, or complete resorption of intralesional bone. The lesions are composed of mature adult fat and may contain combinations of solid, liquefied and/or necrotic fat. A central nidus may be evident, with or without the presence of calcification or woven bone, fibrovascular tissue and/or recent and remote hemorrhage (4a).5,6 Milgram devised a staging system in 1988, reflecting three clinical patterns: Stage 1- absence of necrosis; Stage 2- partial necrosis and dystrophic calcification; Stage 3- near complete/complete necrosis, cysts, calcification, and reactive new bone.
Imaging Considerations
The radiologic appearance of intraosseous lipoma depends on the histologic composition of the lesion. Intraosseous lipomas can contain varying amounts of fat, bone, fibrous tissue, and cystic degeneration, resulting in a range of radiographic manifestations. Intraosseous lipomas composed solely of fat (Milgram stage 1 lesions) are radiolucent, well-circumscribed lesions that frequently are associated with mild, focal, expansile remodeling.1 On MRI, the lesion is geographic, rounded, without cortical interruption, with a peripheral rim of high signal intensity on T1- weighted images (1a,1b). Homogeneous fat suppression should occur on fat-suppressed T2-weighted or inversion recovery-weighted images (1c,1d). In Milgram stage 2 or 3 lesions, the ossifications and calcifications may produce a distinctive radiographic appearance (5a).
Milgram 2 and 3 lesions on T1-weighted MR images may show a central zone of intermediate signal intensity with a surrounding rim of hyperintense tissue (2a,2b). Variations on the much reported theme of peripheral fatty and central cystic signal characteristics of this lesion should not dissuade the radiologist or orthopaedic surgeon from making the diagnosis of calcaneal intraosseous lipoma. In some cases, the peripheral rim of fatty tissue may be quite thick, show heterogeneous T1 hyperintensity, and demonstrate an irregular edema pattern within the fatty rim on inversion recovery-weighted images (6a,7a). It is acceptable for the fibrovascular fatty rim to demonstrate enhancement after gadolinium administration (3a,3b).
Figure 7:
On (7a), the corresponding inversion recovery sagittal image, incomplete suppression of fat signal intensity is evident within the fatty rim (arrowheads), and edema like changes are present. Although such an appearance would raise concern in soft tissue lipomas, it is well recognized and acceptable in patients with calcaneal intraosseous lipomas. The variable fat suppression and edema-like appearance is explained by the presence of fibrous elements and may also in part be related to ongoing ischemia/necrosis. Images 6a and 7a courtesy of Tudor Hughes, M.D.
Discussion
Calcaneal intraosseous lipoma is an uncommon benign bone tumor which, as it slowly expands and remodels adjacent osseous structures, acquires a typical appearance that should be readily diagnostic on plain radiographs and MRI. Calcaneal intraosseous lipomas may present with bone pain up to 66% of the time from chronic expansion, or with acute symptoms related to pathologic (insufficiency) fracture.1,3 Although there exists a differential diagnosis, including bone infarct, unicameral bone cyst, aneursymal bone cyst, chondromyxoid fibroma, osteoblastoma and giant cell tumor, the presence of patently obvious fat signal intensity on T1-weighted MR images should allow a near 100% sensitivity and specificity in the diagnosis of calcaneal intraosseous lipoma. Bone infarcts can occasionally be a source of diagnostic confusion, as infarcts contain fat and often have a low signal intensity rim. However, it should be emphasized that calcaneal intraosseous lipoma is an expansile lesion that remodels cancellous and cortical bone, which is never a feature of bone infarction.3
It has been noted that a simple bone cyst treated with percutaneous alcohol ablation subsequently replaced the central cystic fluid with fatty tissue as it underwent reparative involution.9 The author suggests there may be a relationship, and possible maturational continuum, between an involuting simple bone cyst and an intraosseous lipoma. Conversely, intraosseous lipomas that completely involute may acquire a purely cystic appearance, leading some to speculate that unicameral bone cysts simply represent a completely involuted intraosseous lipoma.
Solitary lipomas are known to commonly have rearrangements with translocations involving chromosome 12, not seen in multiple lipomas and spindle cell/allomorphic varieties.10 Type IV hyperlipidemia has been reported in association with multiple lipomas.8 Rare reports of dedifferentiation into a malignant lesion are of interest.1,2 In one study,7 3 of the 4 lesions undergoing dedifferentiation were fatal, despite treatment with amputation.
If a calcaneal intraosseous lipoma is discovered incidentally, it is typically simply monitored, as malignant transformation is exceedingly rare. Large lesions at risk of pathologic fracture, however, may be prophylactically resected. Symptomatic lesions or those that have already resulted in pathologic fracture are generally treated with surgical curettage and packing of the defect with bone graft.
Conclusion
Calcaneal intraosseous lipoma is a benign lesion that may present a diagnostic challenge to those uninitiated in its appearance. In some instances it may mimic a more biologically aggressive, osteolytic process in a patient who presents with foot pain. It is therefore important to be aware of the MR imaging features that allow it to be discriminated from lesions of similar appearance and location, such as the identification of fat, necrosis, hemorrhage and characteristic internal calcification. The unequivocal diagnosis of an incidentally discovered calcaneal intraosseous lipoma prevents the unnecessary workup, biopsy and treatment of affected patients.
References
1 Mark D. Murphey, John F. Carroll, Donald J. Flemming, Thomas L. Pope, Francis H. Gannon, and Mark J. Kransdorf. From the Archives of the AFIP: Benign Musculoskeletal Lipomatous Lesions. RadioGraphics 2004 24: 1433-1466
2 Milgram JW. Intraosseous lipomas: a clinicopathologic study of 66 cases. Clin Orthop 1988; 231:277-302.
3 Milgram JW. Intraosseous lipomas: radiologic and pathologic manifestations. Radiology 1988; 167:155-160.
4 Resnick D. Tumor and tumor-like diseases. In: Resnick D, eds. Diagnosis of bone and joint disorders. 4th ed. Philadelphia, Pa: Saunders, 1995; 3745-4128.
5 MR Findings of Calcaneal Intraosseous Lipoma with Hemorrhage. Hyo-Sung Kwak, Kwang-Bok Lee, Sang-Yong Lee and Young-Min Han. AJR 2005; 185:1378-1379
6 Barcelo M, Pathria MN, Abdul-Karim FW. Intraosseous lipoma: a clinicopathologic study of four cases. Arch Pathol Lab Med 1992; 116:947 -950
7 Milgram JW. Malignant transformation in bone lipomas. Skeletal Radiol. 1990;19(5):347-52.
8 Freiberg RA, Air GW, Glueck CJ, Ishikawa T, Abrams NR. Multiple intraosseous lipomas with type-IV hyperlipoproteinemia: a case report. J Bone Joint Surg Am 1974; 56:1729-1732
9 Deposition of intraosseous fat in a degenerating simple bone cyst. R Wada, R G,
10 W Lambert. Skeletal Radiol. 2005 Jul ;34:415-8
11 Weiss SW. Lipomatous tumors. Monogr Pathol. 1996;38:207-39.