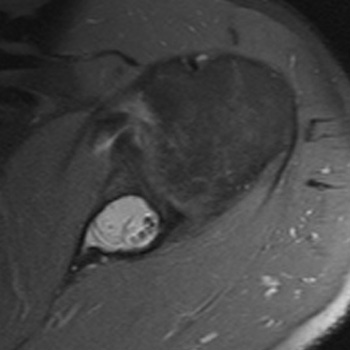
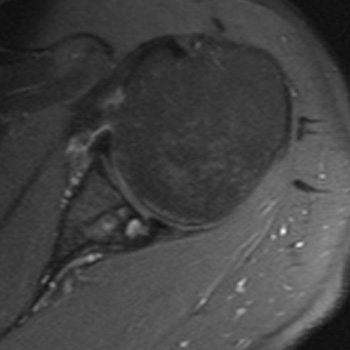
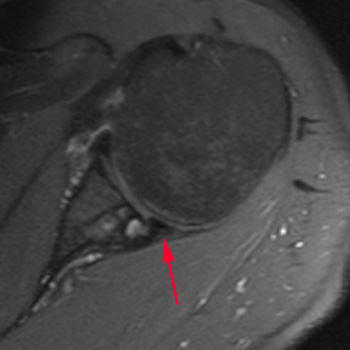
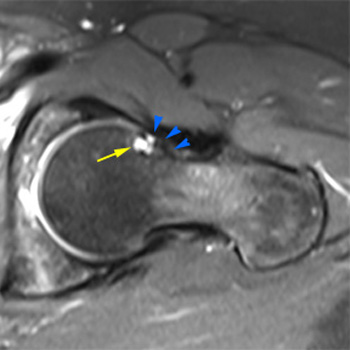
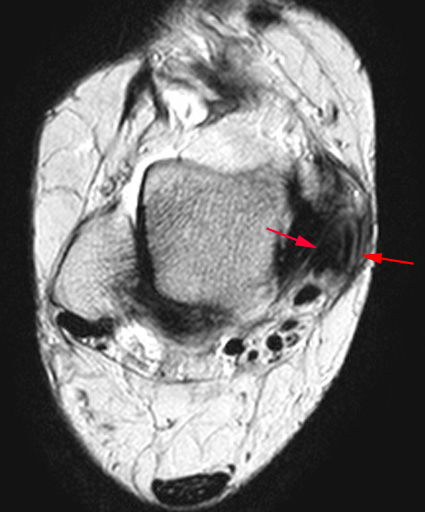
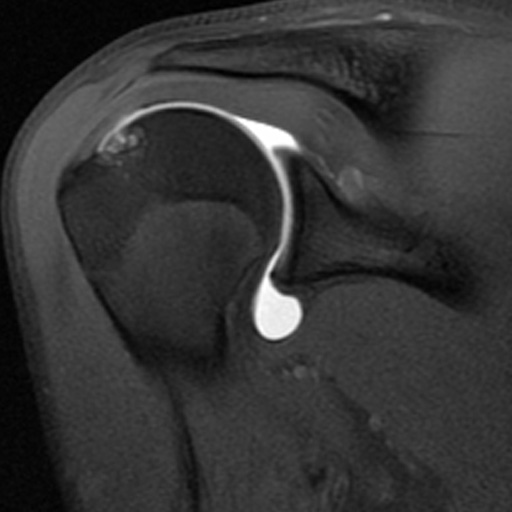
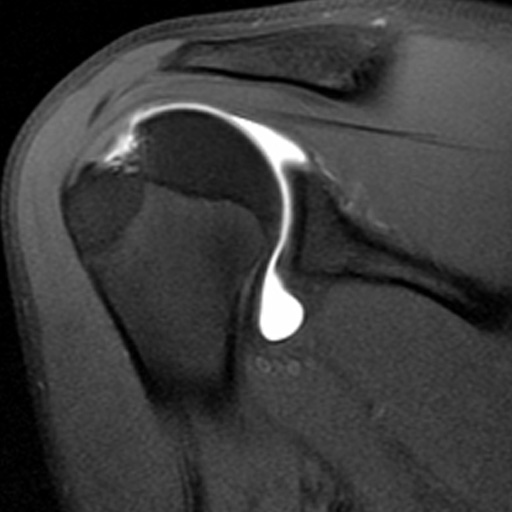
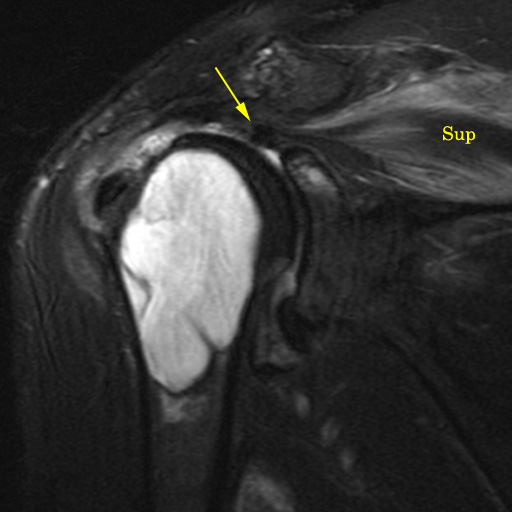
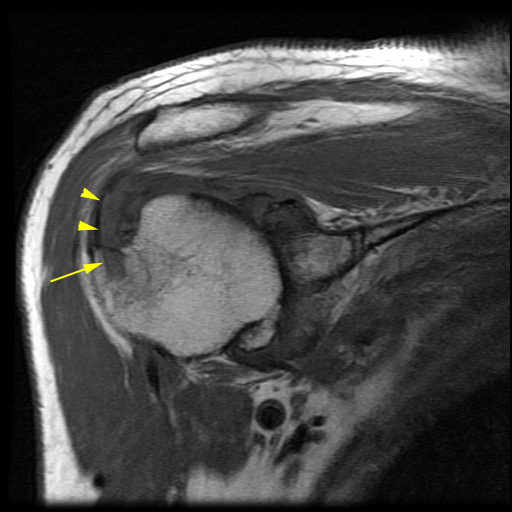
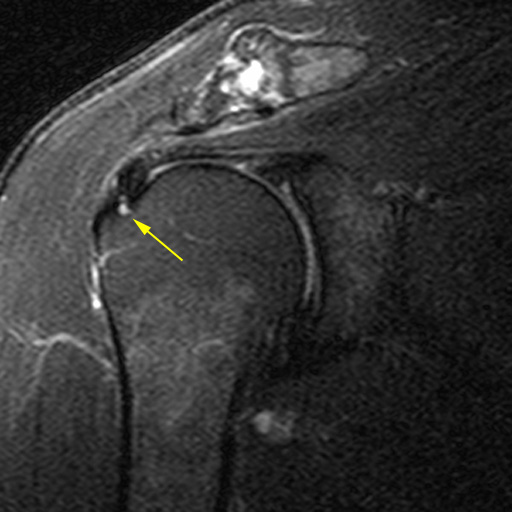
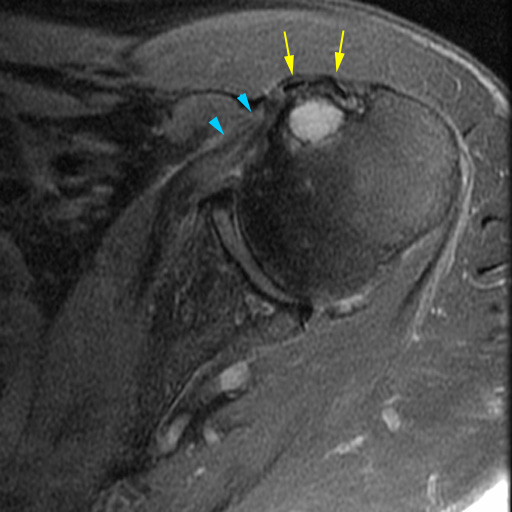
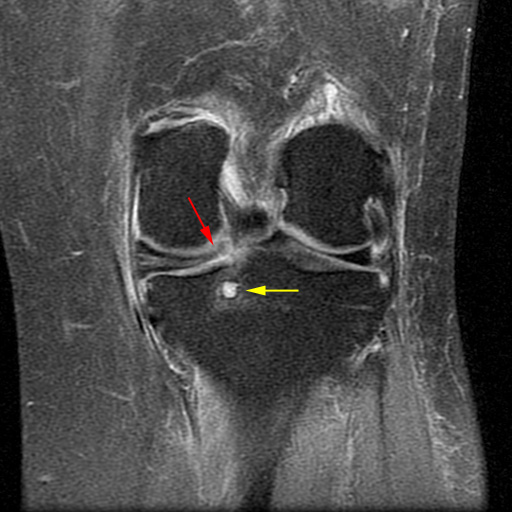
Clinical History: A 61 year-old male presents with posterior left shoulder pain and limited range of motion for six months. No known injury. What are the findings? What is your diagnosis?
Findings
Diagnosis
Intraosseous paralabral cyst arising from a posterior glenoid labral tear.
Introduction
In medicine, an uncommon presentation of a common entity is more likely than a classic presentation of a rare one. In a busy MRI practice, we see intraosseous cysts and cyst-like lesions many times throughout the day. Such lesions are very common, although occasionally they may be atypically large or unusual in some other way. It is important to not mistake benign bone cysts for more aggressive lesions and to understand which are incidental or which may be clues to important underlying abnormalities. This clinic will not be an exhaustive review of all the types of cysts that you may potentially encounter, but rather a discussion of the cysts encountered frequently, with a look at how and why they form, their significance, and some of the unusual and potentially confusing appearances.
Cysts Associated with Lost Cartilage
The most common cysts we encounter are degenerative in nature, associated with areas of chondral loss and other classic findings of osteoarthritis. These are not true cysts, since they lack an epithelial lining, and therefore some prefer to call them pseudocysts or geodes. For brevity, we continue to refer to them as cysts. Two basic theories exist as to their formation — synovial fluid intrusion and bony contusion. Proponents of the intrusion theory argue that joint fluid under pressure causes local bone destruction. Displaced trabeculae and reinforcing new bone create a sclerotic rim around the cyst margins. The cyst may remain open to the joint, but more often is closed by fibrous tissue, fibrocartilage, or new bone. Bone contusion theory proponents explain that subchondral bone that has lost some of the overlying cartilage cushion is more susceptible to injury from repetitive microtrauma. This leads to local osteonecrosis and cyst formation, eventually leading to joint communication. Some argue that the histology supports the contusion theory, since most cysts are noncommunicating and contain necrotic bone fragments with dead denuclearized cells, surrounded by a layer of fibrous connective tissue containing adipocytes and osteoblasts 1. However, cyst contents can also contain small fragments of articular cartilage centrally and foci of metaplastic cartilage in the wall, suggesting that both mechanisms are involved 2.
Figure 3:
Communicating and noncommunicating subchondral cysts. In the intrusion theory of cyst formation, the cyst starts open and later becomes covered. In the bone contusion theory, the cyst develops before opening up to communicate with the joint. Noncommunicating cysts may be covered with fibrous tissue, fibrocartilage, or new bone (arrowhead). A variable layer of surrounding fibrous tissue is present and a surrounding rim of bone.
Cysts Associated with Repetitive Osseous Microtrauma
Osseous injury can cause trabecular microfractures and later cyst formation. This may be secondary to an acute contusion or from chronic repetitive microtrauma from impaction or traction forces. Chronic repetitive force loading on bone can lead to osseous hypertrophy as well as cystic changes. Several sites of classic osseous abutments occur, such as with femoroacetabular impingement, acromial abutment of the humerus in the setting of large rotator cuff tears, or ulnocarpal abutment.
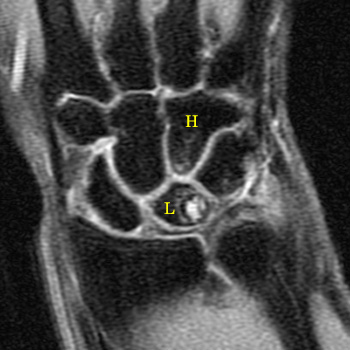
Figure 4:
Cystic change in the lunate from chronic repetitive ulnocarpal abutment is not uncommon. Note that the cystic changes are subchondral at the proximal ulnar portion of the lunate (L). This is not Kienbock's disease, where cystic changes develop more diffusely. Note the more subtle subchondral cyst formation in the proximal margin of the hamate (H), related to chronic repetitive abutment with the lunate (type II lunate morphology with an extra facet which articulates with the hamate).
Figure 5:
Cystic change at the anterosuperior femoral head-neck junction (yellow arrow), associated with a hypertrophic bump (blue arrowheads) in a patient with cam-type femoroacetabular impingement (FAI). An isolated cyst in this area may be an incidental finding. However, in the setting of a bump, diminished femoral head-neck offset, and characteristic clinical findings, FAI is more likely.
Additionally, chronic abutment changes can occur from external forces, such as in the foot. Chronic repetitive pressure (typically from standing in high heeled shoes) can lead to hallux valgus and bunion deformities. These are accompanied by bone hypertrophy at the medial eminence of the head of the first metatarsal.
Intraosseous Paralabral Cysts
Tears of the glenoid labrum in the shoulder and tears of the acetabular labrum of the hip often have associated paralabral cysts in the adjacent soft tissue or bone. These are helpful indicators of adjacent labral pathology as they are often more conspicuous than the underlying labral pathology itself (as in our test case). A paralabral cyst may form when joint fluid pushes outward through a labral defect. This may expand into adjacent soft tissue or enter directly into the adjacent bone. Additionally, labral tears can often lead to failure of the adjacent hyaline cartilage followed by formation of degenerative subchondral cysts.
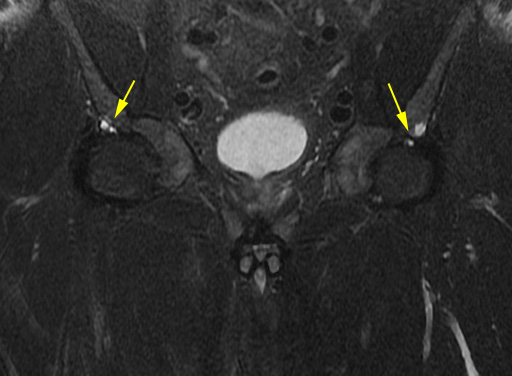
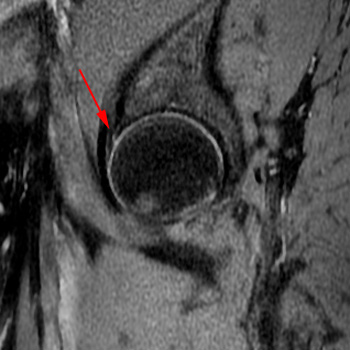
Figure 7:
Paralabral cysts. Left hip exam, including a coronal view of both hips. Intraosseous cysts (yellow arrows) are found in the anterolateral margins of the acetabular roofs bilaterally. A sagittal image of the left hip confirms an anterosuperior acetabular labral tear (red arrow). Although the study did not include high resolution images of the right hip, a labral tear is also highly likely on that side as well. The cysts may be from intrusion of fluid through a defect produced at the labral tear or from associated degeneration of adjacent hyaline cartilage.
Cysts Adjacent to Ligament Attachments
Intraosseous ganglion cysts are gelatinous cyst-like lesions containing fibrous tissue, collagenous fibers similar to flattened histiocytes, partly mucoid-degenerated. Although they have no synovial lining and are generally surrounded by sclerotic bone, they have a fibrous membrane of variable thickness, which accounts for their variable degree of contrast enhancement. Their pathogenesis is not firmly established and there is debate about whether they are distinct from degenerative, insertional, or post-traumatic cysts3. We will presume that insertional cysts are in fact intraosseous ganglion cysts. These may form when tension on the osseous attachment of a ligament insertion creates a local vascular disturbance leading to bone breakdown and eventual fluid production4. Alternatively, it can be an outside-in process. Degeneration and microtears lead to small amounts of mucinous fluid accumulating between collagen fibers. The fluid can then be forced outward into surrounding tissues or into the adjacent bone3. About half have mild surrounding edema on MRI3 and this should not be misinterpreted as a sign of an aggressive process. A small zone of edema is typically visible at a site as a cyst is about to develop.
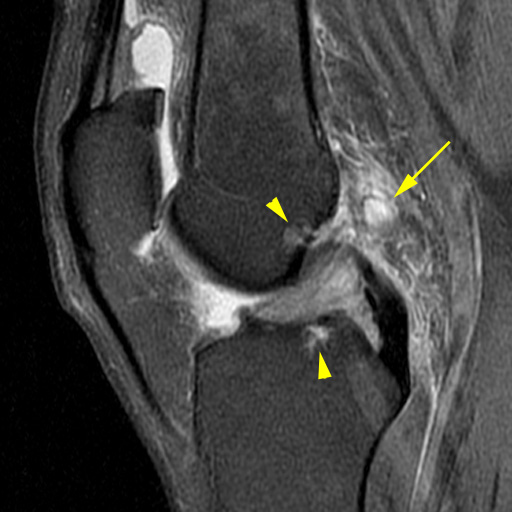
In the knee, ligament degeneration is most commonly found in the ACL. Mucoid degeneration leads to coalescence of fluid and cyst formation. This begins as an elongated cyst within the ligament substance, but then may project into surrounding soft tissues posteriorly from the proximal end of the ligament or anteriorly from the distal end. Intraosseous cyst formation is very common at both the femoral and tibial ACL attachments, manifesting first as a small zone of edema, and finally as frank intraosseous cysts. Cysts at the ACL attachments are almost always associated with mucoid degeneration and ganglion cyst formation in the ligament. The cysts may be more obvious than the associated ligament pathology, and are useful flags.
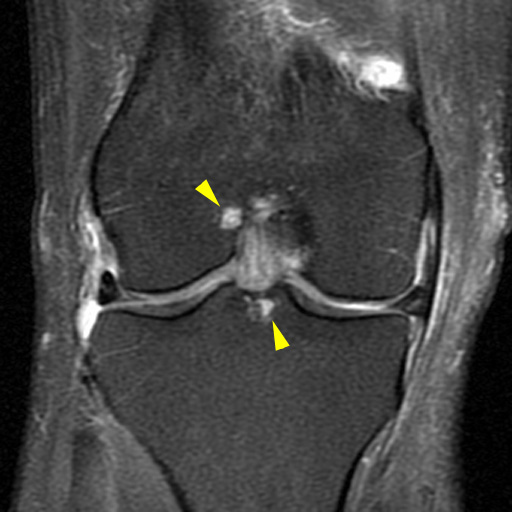
Figure 8:
ACL mucoid degeneration and ganglion cyst formation. The ACL is mildly expanded and increased in T2 signal, with a small cyst projecting into posterior soft tissues (yellow arrow). Small intraosseous cysts (yellow arrowheads) typically form at the anterior margin of the femoral attachment of the ACL and at the posterior margin of the distal attachment.
Intraosseous ganglion cysts are very frequent in the carpal bones, located at the attachments of degenerative ligaments5. The cysts may be the result of mucoid degeneration in the adjacent ligament, or both the degeneration and intraosseous cystic change may individually result from the tensile loads placed on the ligaments. Wrist ganglion cysts most commonly arise from the dorsal component of the scapholunate interosseous ligament, projecting through the dorsal joint capsule. Intraosseous ganglion cysts may also form at this ligament’s bony attachments. They are also frequent incidental findings in the capitate, arising volarly at the attachment of the radioscaphocapitate ligament. Intraosseous ganglion cysts can be occasionally be symptomatic, but a symptomatic ganglion cyst is a diagnosis of exclusion.
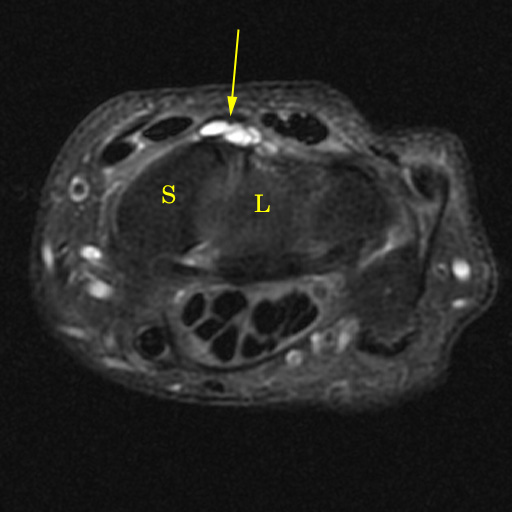
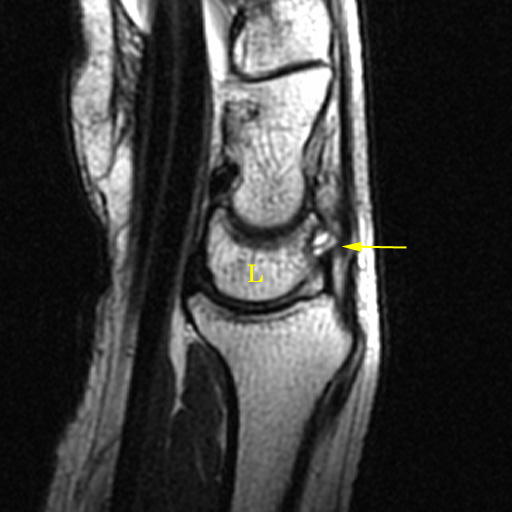
Figure 9:
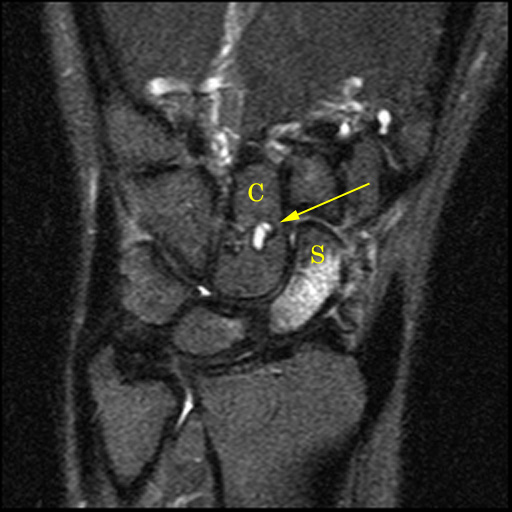
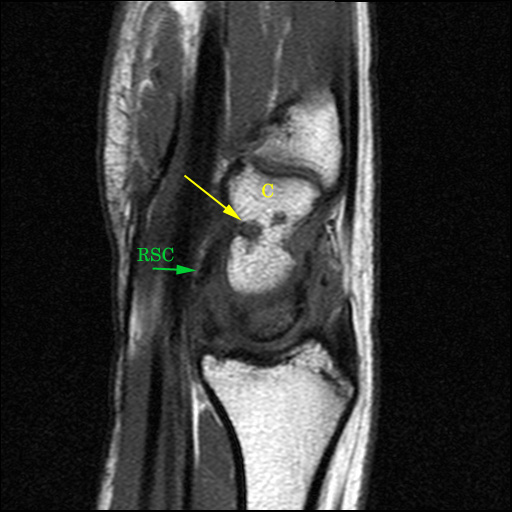
Ganglion cysts arising from the scapholunate ligament. Typical dorsal capsular ganglion cyst (arrow), lobulated and positioned adjacent to the dorsal component of the scapholunate ligament, from which it arises (S=scaphoid, L=lunate). Sagittal image showing a partially intraosseous ganglion cyst at the dorsal margin of the lunate.
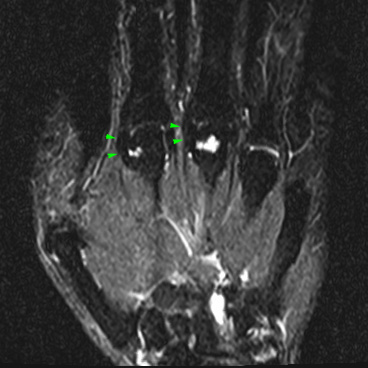
Small cysts are often found incidentally in the metacarpal heads. These are positioned most commonly adjacent to the attachments of the radial collateral ligaments of the index, long, and ring metacarpal heads6, corresponding to sites that undergo the highest stresses during grasping. Interestingly, patients with early rheumatoid arthritis (RA) develop erosions at these same sites, rather than being randomly distributed at any bare area. It is likely that compressive forces (nutcracker-like effect) adjacent to the ligament attachments play a significant underlying role for erosion development and that inflammation in RA exaggerates the inherent tendency for bone damage adjacent to the ligaments6. Incidental cysts at these sites can be identical in appearance to rheumatoid erosions, although the latter tend to be larger, more indistinct, more numerous, and more often associated with marrow edema or obvious synovitis. Each can enhance with intravenous contrast. Associated edema has a specificity of 87.5% for RA erosions, if the lunate is ignored (due to high prevalence of edema from ulnocarpal abutment)7. Juxtaarticular bone cysts can become quite large in RA8.
Another common site of cyst formation is in the mid calcaneus, beneath the angle of Gissane. A prior study determined them to be intraosseous ganglion cysts, suggesting that they may arise at the sites of penetrating microvessels9 and noting that they occasionally communicate with the posterior subtalar joint. However, the attachments of the inferior extensor retinaculum and the interosseous talocalcaneal ligament (the primary soft tissue stabilizer of the subtalar joint) are also at this site. As at other anatomic sites, the ligament attachment may be causally related to cyst development. Ligamentous injury and degeneration have been documented at this site10 and may underlie sinus tarsi syndrome. Soft tissue ganglia arising from this area may develop by fluid leaking from torn ligaments10. Cysts in the lower mid talus are less frequent than in the calcaneus, but are also found adjacent to the ligament attachment.
Figure 13:
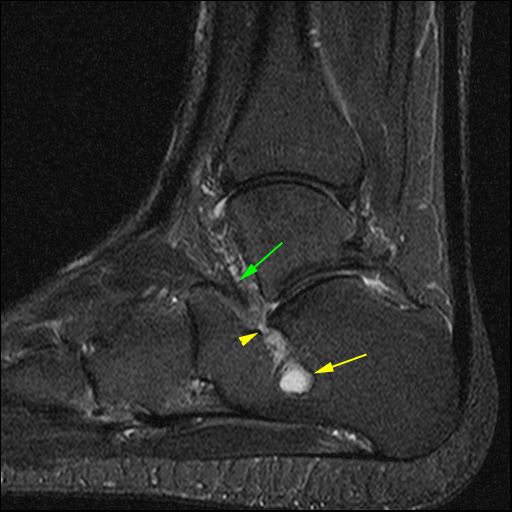
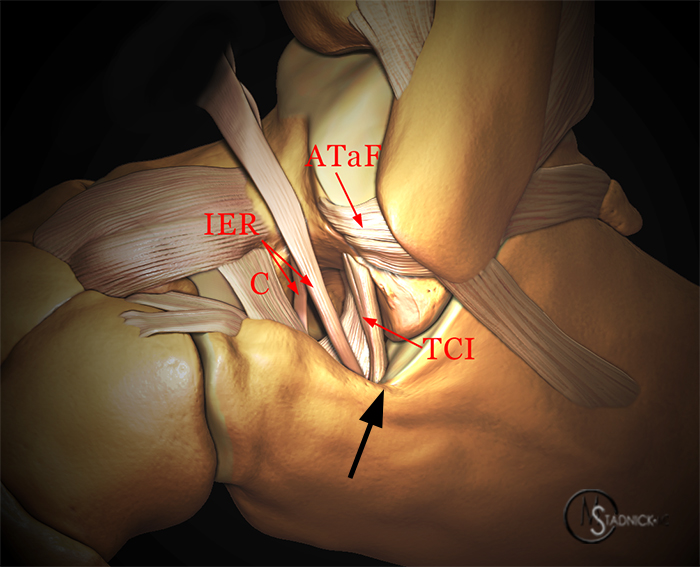
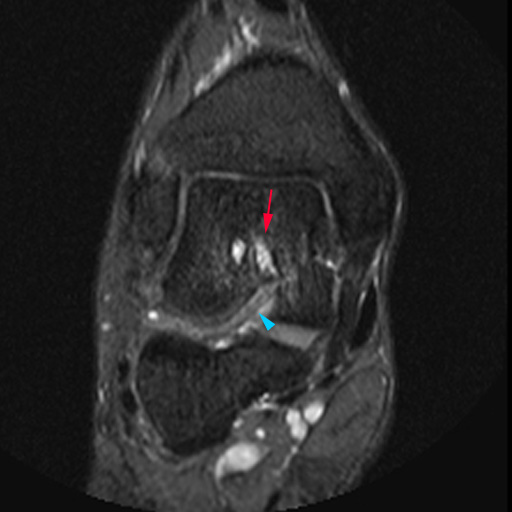
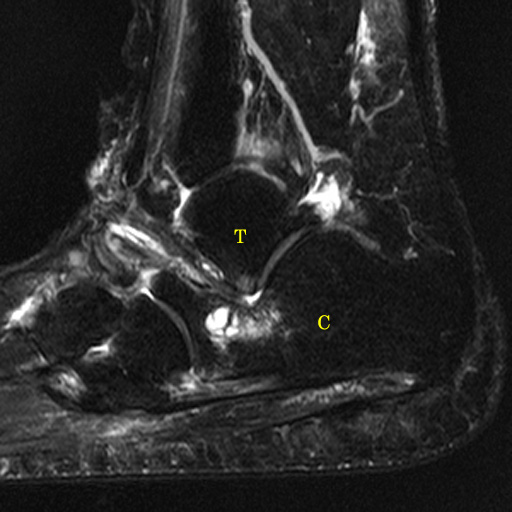
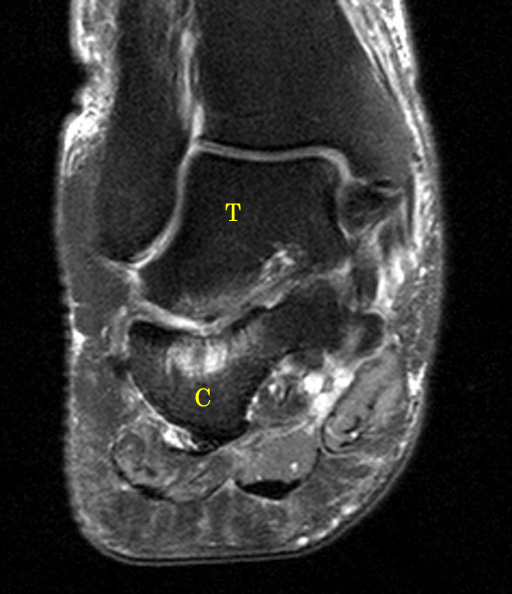
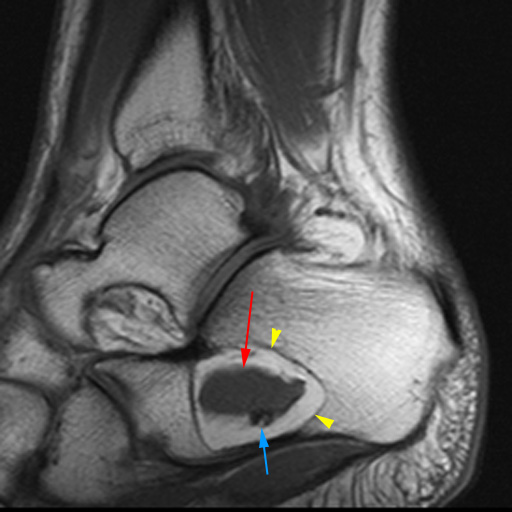
(13a) Intraosseous cysts adjacent to the sinus tarsi. Calcaneal intraosseous cyst (yellow arrow) arising through a narrow cortical defect (yellow arrowhead) at the angle of Gissane near the distal attachment sites of the talocalcaneal interosseous ligament and the roots of the inferior extensor retinaculum (green arrow). (13b) Corresponding anatomical illustration. black arrow=angle of Gissane, TCI=talocalcaneal interosseous ligament, C=cervical ligament, ATaF=anterior talofibular ligament, IER=inferior extensor retinaculum. (13c) Talar cysts (red arrow) adjacent to the attachment of the talocalcaneal interosseous ligament (blue arrowhead).
Cystic changes at the upper margin of the calcaneus resulting from lateral talocalcaneal impingement are important to distinguish from the incidental intraosseous ganglion cysts in this vicinity. Impingement at this site develops secondary to hindfoot valgus, typically as a late consequence of posterior tibial tendinopathy. This is discussed in a separate web clinic. Key differentiating features include a slightly anteriorly subluxed position of lateral process of the talus with a narrowed sinus tarsi, as well as marrow edema on both sides of the abutment area.
Figure 14:
Lateral talocalcaneal impingement secondary to posterior tibial tendinopathy. Calcaneal cystic changes extend further anteriorly than the common incidental cysts and are accompanied by marrow edema. The lateral process of the talus is subluxed anteriorly and the sinus tarsi is narrowed, as a result of hindfoot valgus. During weightbearing they come into contact. Subcortical edema is found in the directly corresponding portion of the talus (T). The axial image demonstrates the underlying posterior tibial tendinopathy (red arrows). The tendon is partially torn and irregular.
Cysts Adjacent to Tendon Attachments
Small cysts are frequently encountered in the shoulder near the rotator cuff tendon attachments. Two distinct types are present, one associated with tendinopathy of the supraspinatus and subscapularis tendons and positioned anteriorly, and one independent of cuff pathology, positioned more posteriorly at the bare area of the humeral neck11.
More posteriorly positioned cysts beneath the superolateral humeral head margin are seven times more common than more anteriorly positioned cysts12, being highly prevalent among both younger and older patients, and occurring independent of rotator cuff status14. The cysts are connected to the joint space and lined with collagen connective tissue, and some suggest that they should be considered normal variants13. While they are typically incidental findings, occasionally they can become large enough to be confused with tumor, or the overlying cortex may collapse to the point that they form a notch-like divot that can be mistaken for a Hill-Sachs deformity. The characteristic location of these cysts and their variability in size, number, and shape need to be kept in mind when considering differential diagnoses at this site.
Figure 15:
Cysts at the posterior superolateral humeral head margin on MR arthrogram, fat-suppressed T1-weighted images. High signal in the cysts indicates communication with the contrast-filled joint. On the slightly further posterior image, the overlying cortex has collapsed or resorbed, simulating a Hill-Sachs deformity. A true Hill-Sachs deformity is typically more elongated and smoothly marginated. Both can be associated with marrow edema.
Figure 17:
Enchondroma. Several cystic-appearing areas are present (yellow arrow) which may alternatively be hyaline cartilage. Multiple calcifications are present centrally (blue arrow). A paralabral cyst is noted adjacent to the glenoid neck (green arrow) arising from a labral tear (not visible on this image).
Cysts located more anteriorly, adjacent to the supraspinatus tendon footprint, are highly associated with adjacent tendinopathy14. Tendon microtearing and degeneration (i.e. tendinosis) are common in this area. Associated mucoid fluid that doesn’t decompress through a bursal or articular surface tear can course longitudinally in the tendon. Medially this may result in cyst accumulation near the myotendinous junction. Laterally fluid may leak beneath the tendon footprint through small cortical infractions that form as the tendon continues to tear. Cysts at this site are particularly frequent with articular side partial tears, presumably since such tears expose the underlying bone to joint fluid, facilitating ingrowth of synovium and granulation tissue.
Figure 18:
An interstitial partial tear of the supraspinatus tendon is filled with fluid, producing an intratendinous cyst (yellow arrowheads). Fat-suppressed T2-weighted image and T1-weighted image. The cyst is beginning to extend into the adjacent bone (yellow arrow), better seen on the T1-weighted image, with surrounding marrow edema.
An additional potential implication for cysts at the tendon attachment is that for patients undergoing rotator cuff repair, cysts may weaken the suture anchor placement site. Bone grafting may be utilized in this situation15.
Cysts located within the lesser tuberosity are indicative of tendinopathy in the superior portion of the subscapularis tendon16. Associated lesions of the pulley system and abnormalities of the tendon of the long head of the biceps are frequent. [A previous web clinic discusses pathology of the long head of the biceps tendon and the pulley system].
Cysts at Meniscal Attachments
The posterior root of the medial meniscus is a common site of degeneration and radial tearing that can be easily overlooked. Edema and cyst formation beneath the osseous attachment often occur concomitant with degeneration at this site. These are therefore helpful flags, suggesting a closer look at the posterior root and a higher degree of suspicion for a radial tear.
Figure 21:
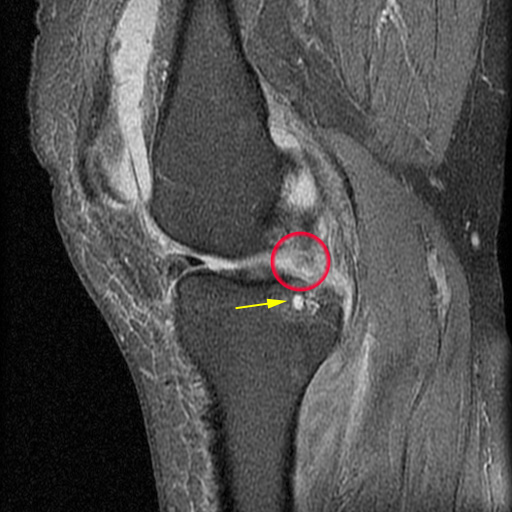
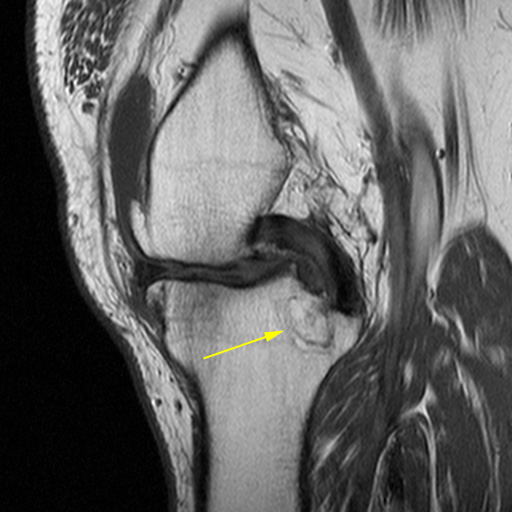
Cysts adjacent to medial meniscus posterior root degeneration and tear. Small cysts (yellow arrows) are present adjacent to the medial meniscus posterior root attachment, with mild adjacent edema. The posterior root of the meniscus is degenerated and radially torn. The tear is visible directly on the coronal view (red arrow) and manifests as a "ghost meniscus" (red circle) on the sagittal images.
Cyst Formation and Healing
As cysts form, there is a balance between breakdown versus repair. Histologically both processes are evident, with necrotic tissue, macrophages, and osteoclasts, as well as reparative tissue, fibroblasts and osteoblasts. Calcification may be present from necrosis. Occasionally hemorrhage may develop in a cyst, followed by healing with fat deposition. Subsequently new bone trabeculae may be formed.
It is interesting to note that although intraosseous lipomas are considered rare lesions, they are relatively frequent in the calcaneus, at the same location as the more commonly found cysts at this site. Lipomas of the calcaneus with central necrosis and cystic change may be indistinguishable from partially healed intraosseous ganglion cysts which have developed fat around the periphery. Some have suggested that lipomas at this site are not really neoplasms, but rather hamartomatous proliferations of fat17,18 and it is plausible that most calcaneal lipomas have actually developed from cysts at this site. The frequency of cysts among children and young adults and the older age range of patients with lipomas supports this idea, and transformation from a calcaneal cyst to a lipoma has been reported9.
Conclusion
This web clinic discusses some of the most commonly encountered bone cysts in daily practice, including how they may form, what they may mean, and how unusual they may look. Most intraosseous cysts encountered are degenerative cysts, intraosseous ganglia, or insertional cysts, although it is probably just semantics to distinguish between these terms. These cysts may form from inside out, outside in, or a combination of both. Often the cysts are associated with adjacent pathology and can be useful flags for these abnormalities.
Key Points
- subchondral cysts
- from synovial fluid intrusion, bone contusion, or both
- can communicate or be sealed off from joint
- contain variable amounts of fibrous tissue
- cysts from bone impingement
- degenerative cysts from repetitive contusion injury
- created at sites of internal impingement (e.g. FAI, ulnocarpal) or external impingement (e.g. bunion)
- can be large and lobulated
- cysts at ligament attachments
- intraosseous ganglion cysts from tension stress, intrusion of fluid from degenerative ligament, or a nutcracker-like phenomenon
- origin of carpal cysts, metacarpal head cysts, cysts at ACL attachments, and possibly calcaneal and talar cysts adjacent to sinus tarsi
- early RA erosions develop at these sites, generally larger size and more indistinct
- cysts near tendon attachments
- tendon insertion type
- anterior superolateral humeral head margin and lesser tuberosity
- from avulsive stress, entry or extension of fluid from a degenerative tendon, or exposure to joint fluid
- anterior greater tuberosity cysts are a useful flag for supraspinatus tendinopathy
- lesser tuberosity cysts are flags for subscapularis and biceps tendon abnormalities
- bare area type
- the majority of cysts at the posterior superolateral humeral head margin
- incidental, found in young and old
- can be very large or extend deeply, and can simulate a Hills-Sachs defect
- tendon insertion type
- cysts at meniscal attachments
- most common at medial meniscus posterior root attachment
- from avulsive injury or fluid intrusion
- flag for degeneration and radial tear at the posterior root
- intraosseous paralabral cysts
- adjacent to glenoid or acetabular labrum
- flag for underlying labral tear
- from fluid extension through the tear or from adjacent articular cartilage damage
- healing cysts
- can fill with fibrovascular tissue
- can fill with fat, starting at periphery
- possible origin of calcaneal lipomas
- Pouders C, De Maeseneer M, Van Roy P, Gielen J, Goossens A, Shahabpour M. Prevalence and MRI-anatomic correlation of bone cysts in osteoarthritic knees. AJR Am J Roentgenol. 2008;190:17–21. http://www.ajronline.org/doi/full/10.2214/AJR.07.2098 ↩
- Resnick D, Niwayama G, and Coutts RD. Subchondral cysts (geodes) in arthritic disorders. Pathologic and radiographic appearance of the hip joint. AJR: Am. J. Roentgenol., 128: 799-806, 1977. http://www.ajronline.org/doi/abs/10.2214/ajr.128.5.799 ↩
- Williams HJ, Davies AM, Allen G, Evans N, Mangham DC. Imaging features of intraosseous ganglia: a report of 45 cases. Eur Radiol. 2004 Oct;14(10):1761-9. Epub 2004 Jun 25. http://www.encyclopediamagnetica.dk/doc/muskuloskeletal/intraosseos%20ganglia.pdf ↩
- Schajowicz F, Clavel Sainz M, Slullitel JA. Juxta-articular bone cysts (intra-osseous ganglia): a clinicopathological study of eighty-eight cases. J Bone Joint Surg Br 1979; 61: 107–116. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3697270/ ↩
- Schrank C, Meirer R, Stabler A, Nerlich A, Reiser M, and Putz R. Morphology and topography of intraosseous ganglion cysts in the carpus: An anatomic, histopathologic, and magnetic resonance imaging correlation study. J Hand Surg 2003;28A:52–61. http://www.jhandsurg.org/article/S0363-5023%2802%2905501-6/abstract ↩
- Tan AL, Tanner SF, Conaghan PG, Radjenovic A, O’Connor P, Brown AK, et al. Role of metacarpophalangeal joint anatomic factors in the distribution of synovitis and bone erosion in early rheumatoid arthritis. Arthritis Rheum 2003;48:1214–22. http://onlinelibrary.wiley.com/doi/10.1002/art.10963/full ↩
- Olech E, Crues JV 3rd., Yocum DE, Merrill JT. Bone marrow edema is the most specific finding for rheumatoid arthritis (RA) on noncontrast magnetic resonance imaging of the hands and wrists: a comparison of patients with RA and healthy controls. J Rheumatol 2010;37:265–74. http://www.jrheum.org/content/37/2/265.full ↩
- Tehranzadeh J, Ashikyan O, Dascalos J, Dennehey C. MRI of large intraosseous lesions in patients with inflammatory arthritis. AJR Am J Roentgenol. 2004 Nov;183(5):1453-63. http://www.ajronline.org/doi/abs/10.2214/ajr.183.5.1831453 ↩
- Elias I, Zoga AC, Raikin SM, Schweitzer ME, Morrison WB. Incidence and morphologic characteristics of benign calcaneal cystic lesions on MRI. Foot Ankle Int. 2007 Jun; 28(6):707-14. http://fai.sagepub.com/content/28/6/707.full ↩
- Lektrakul N, Chung CB, Lai Ym, Theodorou DJ, Yu J, Haghighi P, Trudell D, Resnick D. Tarsal sinus: arthrographic, MR imaging, MR arthrographic, and pathologic findings in cadavers and retrospective study data in patients with sinus tarsi syndrome. Radiology. 2001 Jun;219(3):802-10. http://dx.doi.org/10.1148/radiology.219.3.r01jn31802 ↩
- Sano A, Itoi E, Konno N, Kido T, Urayama M, Sato K. Cystic changes of the humeral head on MR imaging. Relation to age and cuff-tears. Acta Orthop Scand. 1998 Aug;69(4):397-400. http://www.ncbi.nlm.nih.gov/pubmed/9798449 ↩
- Williams M, Lambert RG, Jhangri GS, et al. Humeral head cysts and rotator cuff tears: An MR arthrographic study. Skeletal Radiol. 2006;35: 909–914. http://www.ncbi.nlm.nih.gov/pubmed/16741738 ↩
- Jin W, Ryu KN, Park YK, et al. Cystic lesions in the posterosuperior portion of the humeral head on MR arthrography: correlations with gross and histologic findings in cadavers. AJR Am J Roentgenol. 2005;184:1211–1215. http://www.ajronline.org/doi/full/10.2214/ajr.184.4.01841211 ↩
- Fritz LB, Ouellette HA, O’Hanley TA, Kassarjian A, and Palmer WE. Cystic changes at supraspinatus and infraspinatus tendon insertion sites: association with age and rotator cuff disorders in 238 patients. Radiology. 2007; 244: 239–248. http://dx.doi.org/10.1148/radiol.2441050029 ↩
- Levy DM, Moen TC, and Ahmad CS. Bone grafting of humeral head cystic defects during rotator cuff repair. Am J Orthop. 2012;41(2):92-94. http://www.amjorthopaedics.com/fileadmin/qhi_archive/ArticlePDF/AJO/041020092.pdf ↩
- Wissman RD, Kapur S, Akers J, et al. Cysts within and adjacent to the lesser tuberosity and their association with rotator cuff abnormalities. AJR Am J Roentgenol. 2009;193:1603–1606. http://www.ajronline.org/doi/abs/10.2214/AJR.09.2377 ↩
- Murphey MD, Carroll JF, Flemming DJ, Pope TL, Gannon FH, Kransdorf MJ. From the archives of the AFIP : benign musculoskeletal lipomatous lesions. Radiographics. 2004;24(5):1433–66. http://pubs.rsna.org/doi/full/10.1148/rg.245045120 ↩
- Diard F, Hauger O, Moinard M, Brunot S, Marcet B.: Pseudo-cysts, lipomas, infarcts and simple cysts of the calcaneus: are there different or related lesions? JBR-BTR. 2007 Sep-Oct;90(5):315-24. http://www.rbrs.org/dbfiles/journalarticle_0471.pdf ↩