Clinical history: 36-year-old male presents after being hit by a motor vehicle and thrown several feet, landing on his right arm. The patient presents with neck and right arm pain and right upper extremity weakness.
Findings:
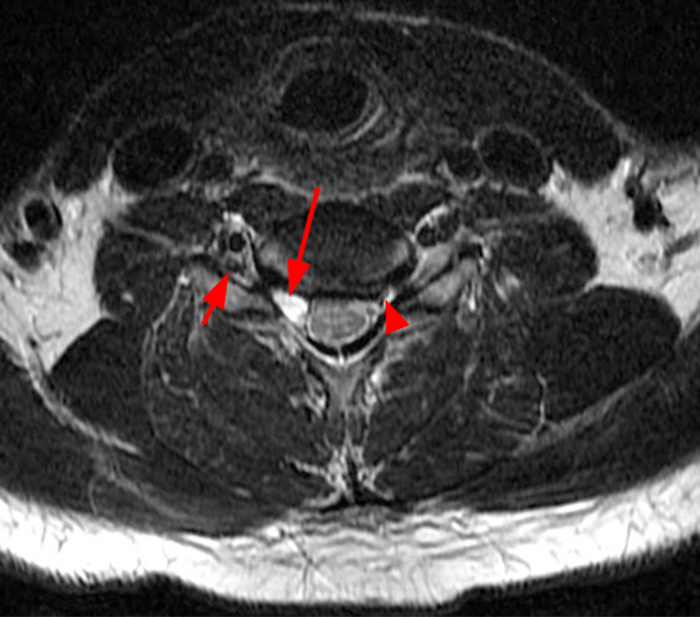
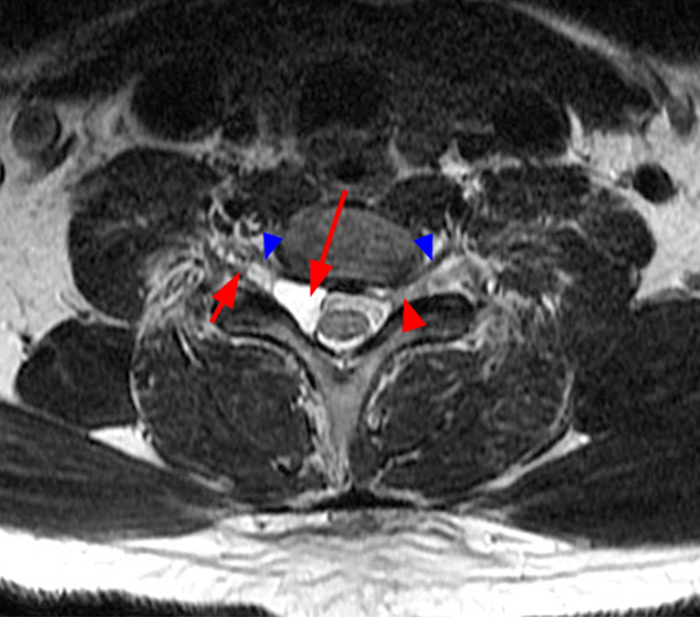
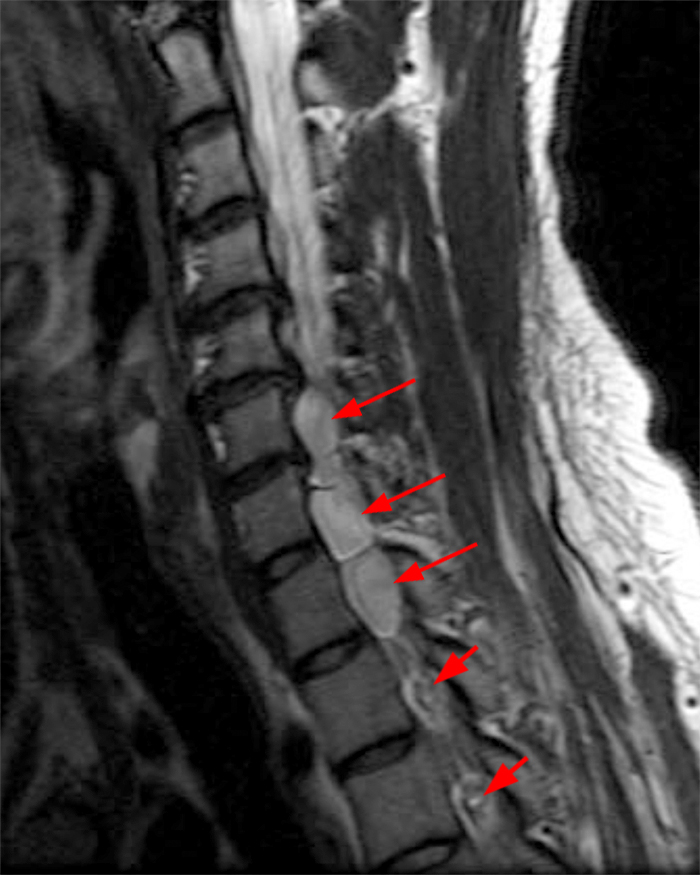
Figure 2:
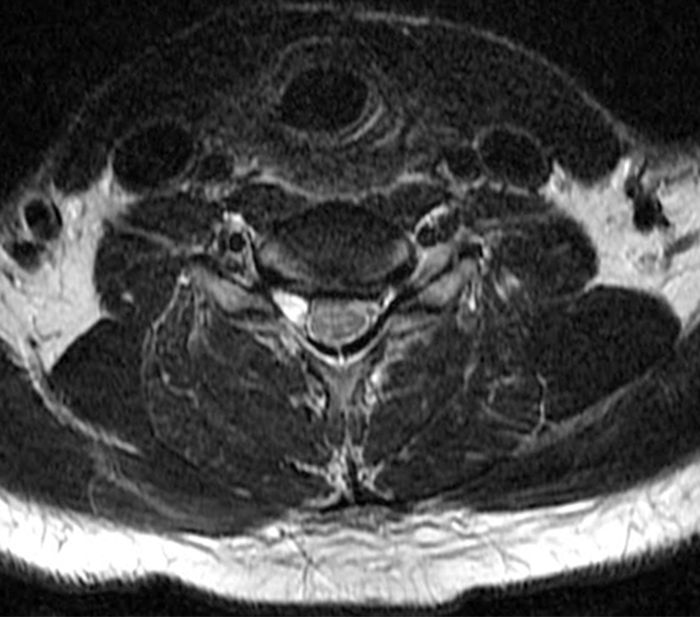
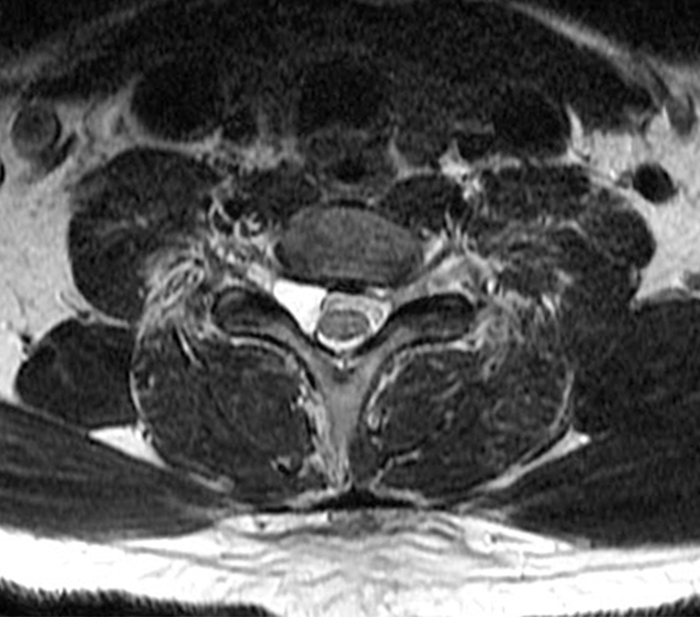
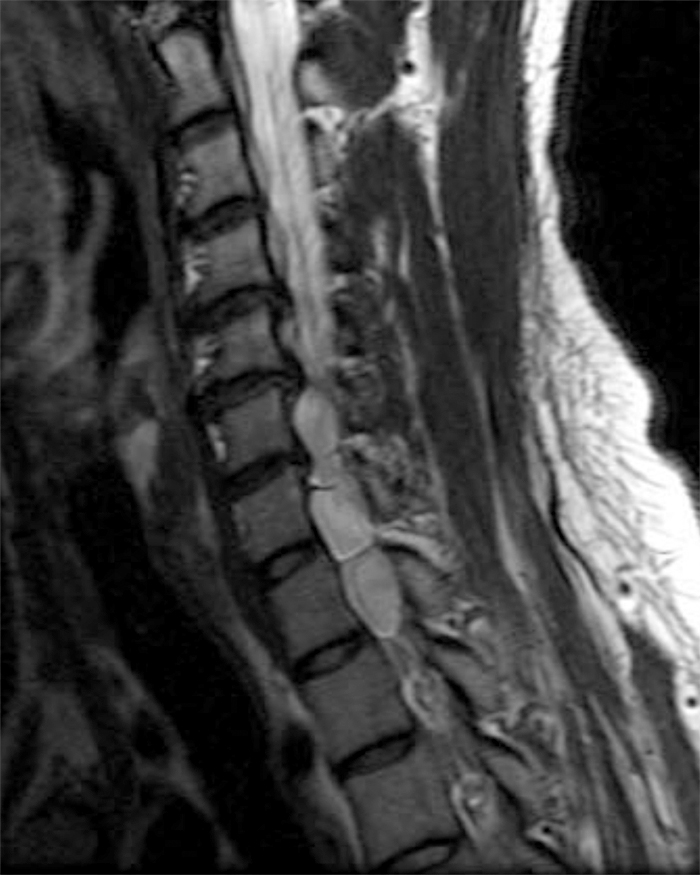
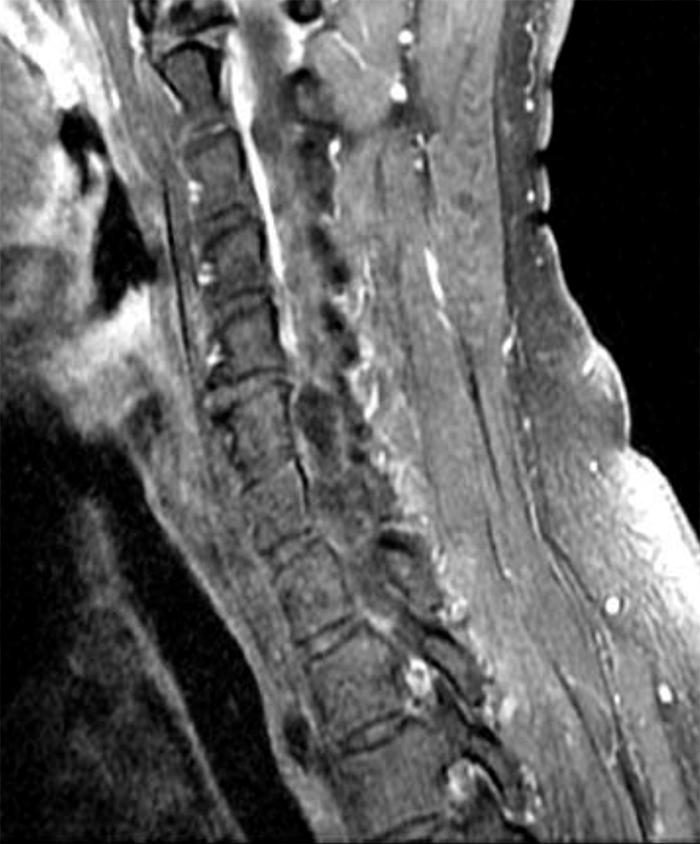
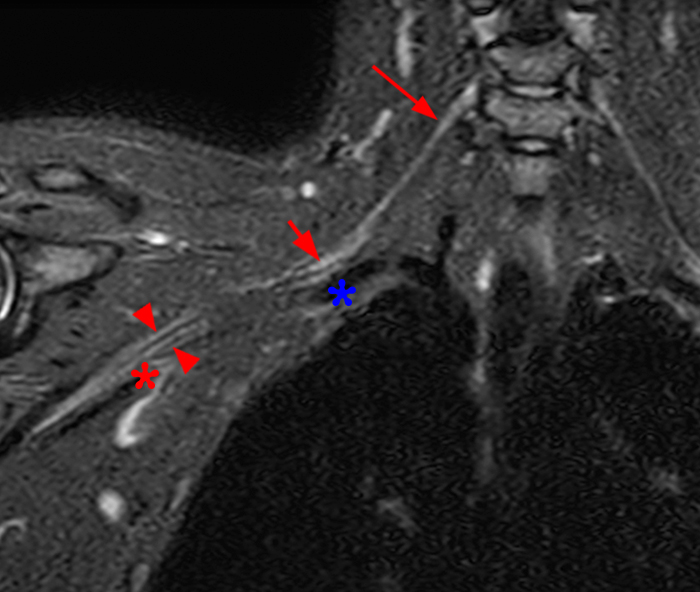
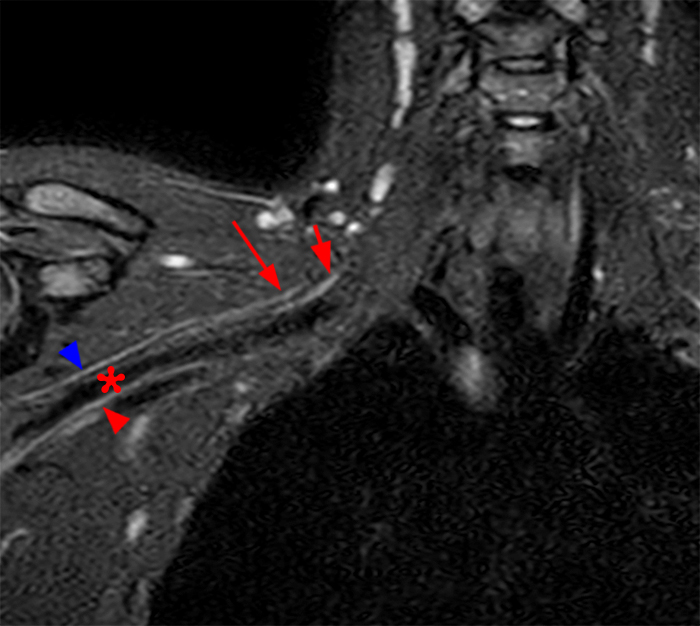
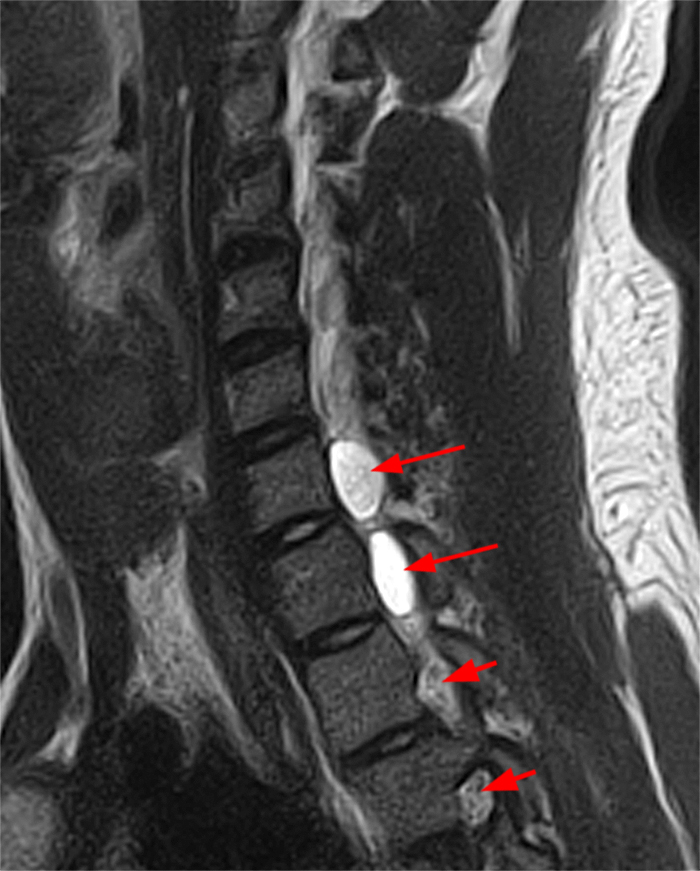
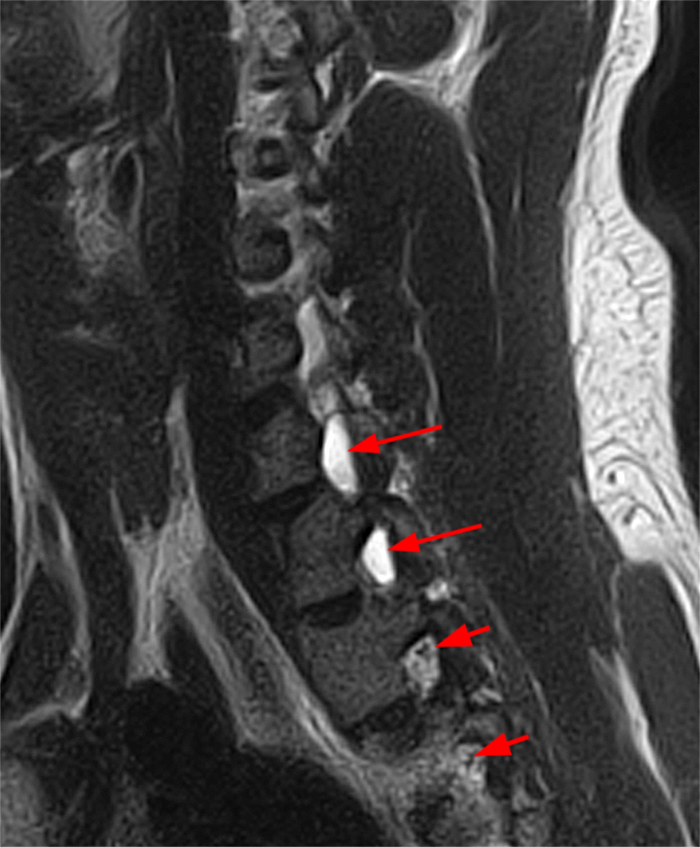
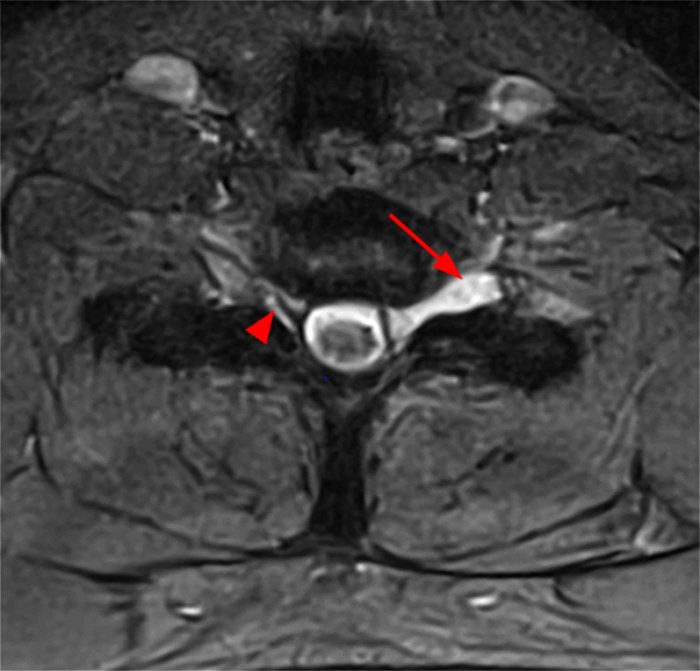
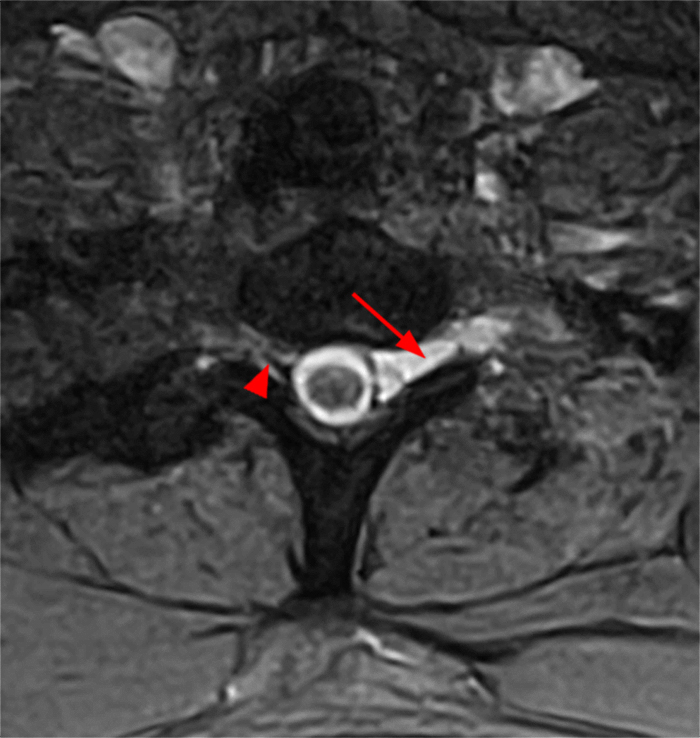
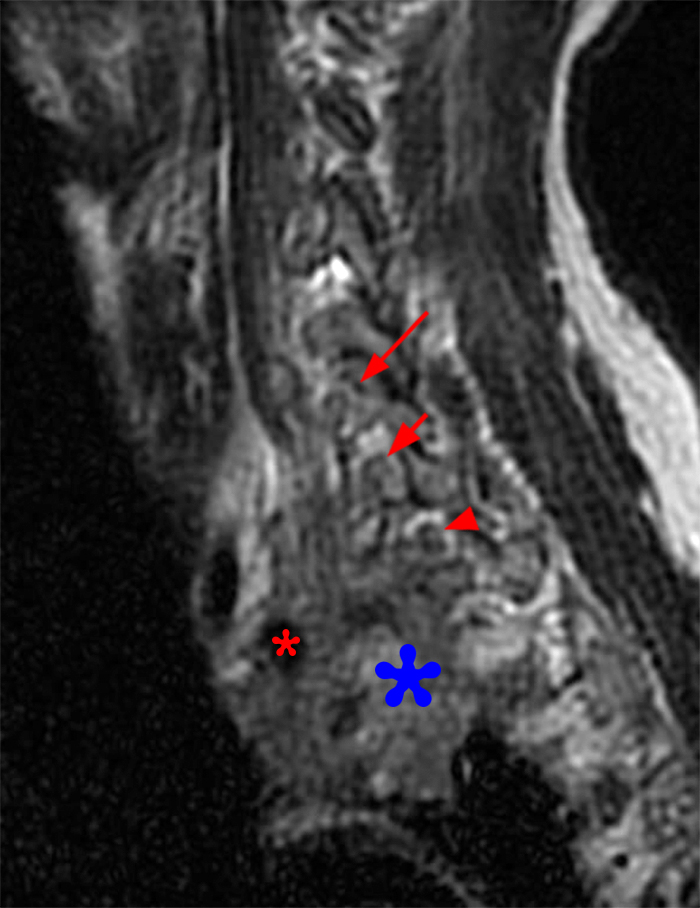
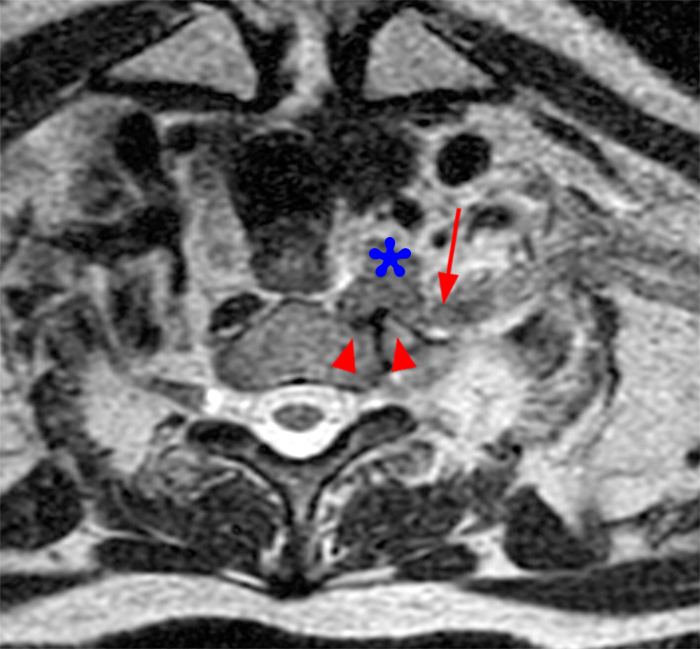
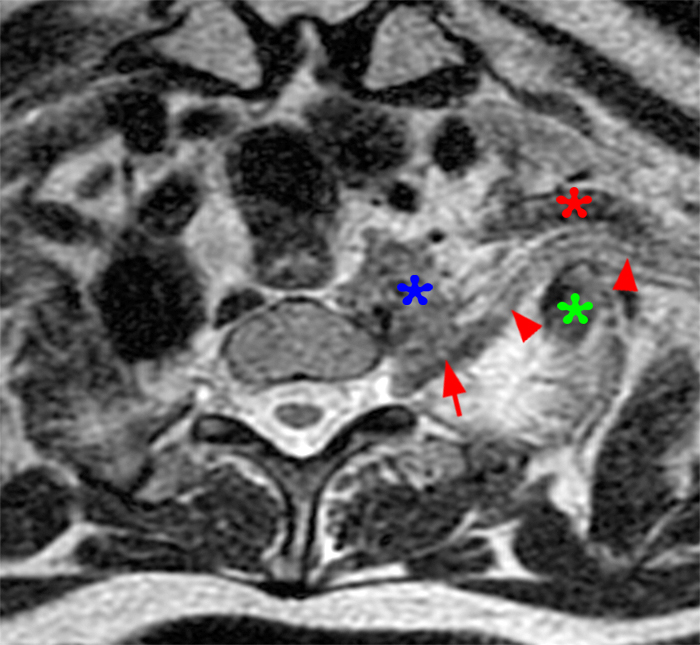
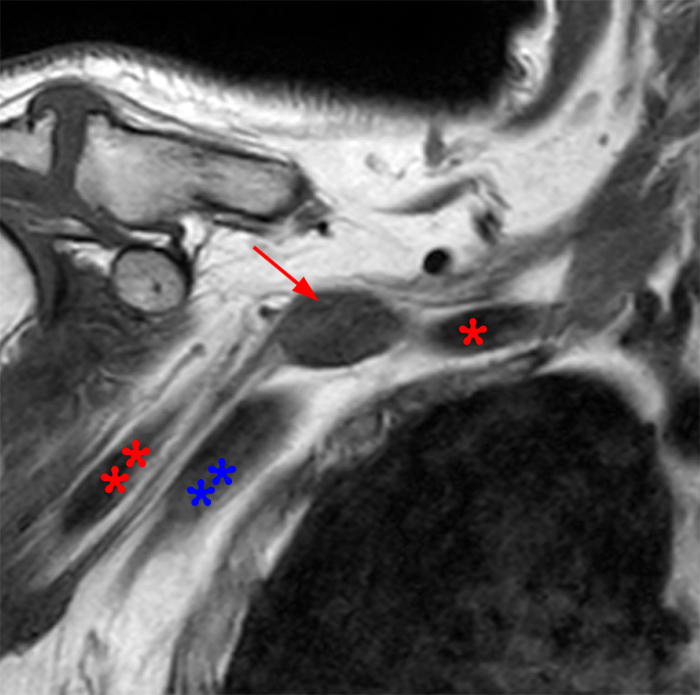
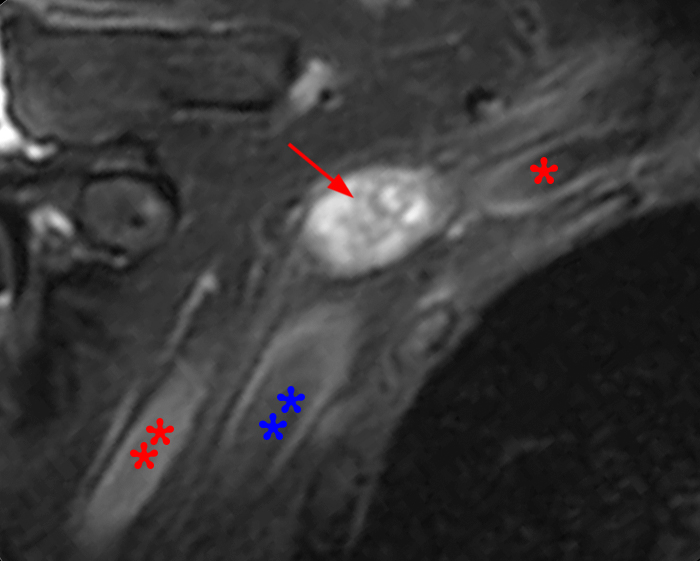
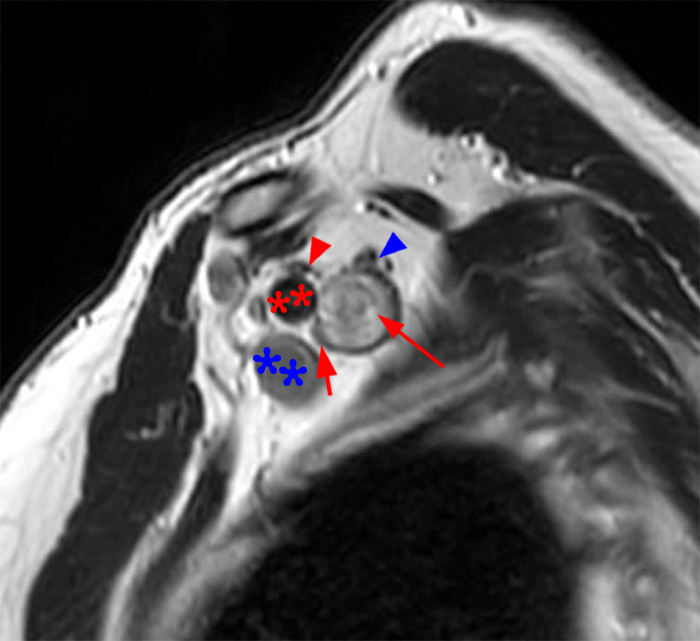
Figure 2: Axial T2-weighted (2a-b) images at the C6-7 (2a) and C7-T1 (2b) levels demonstrate extradural pseudomeningoceles in the right aspect of the spinal canal extending to the medial neural foramina without visualization of the associated pre-ganglionic C7 and C8 nerve roots (arrows). The more laterally located right C7 and C8 dorsal root ganglia are visualized (short arrows). Note the normal left C7 and C8 nerve roots within the neural foramina (red arrowheads). Linear low T2 signal intensity along the bilateral anterolateral C7-T1 foramina in Figure 2b (blue arrowheads) likely represents segmental veins. Sagittal T2-weighted (2c) and T1 fat-suppressed post-contrast (2d) images demonstrate ipsilateral, contiguous pseudomeningoceles at the C6-T2 levels (arrows). The normal, more caudal T2 and T3 nerve roots (short arrows, 6b-d) are seen within the medial neural foramina and surrounding venous plexus enhancement (arrowheads) just medial to the dorsal root ganglia.
Diagnosis
Traumatic avulsions of the right C7,C8, and T1 nerve roots with associated pseudomeningoceles.
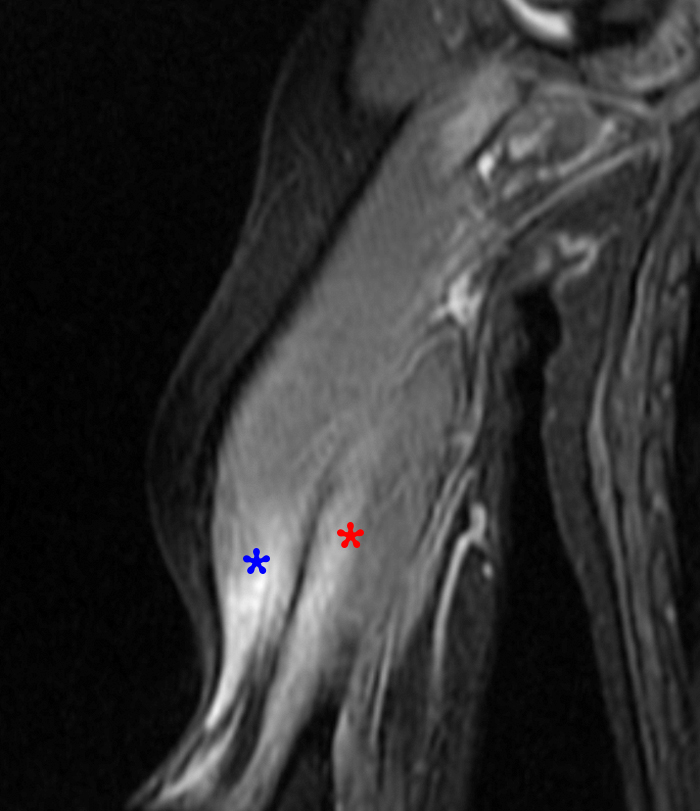
Figure 3:
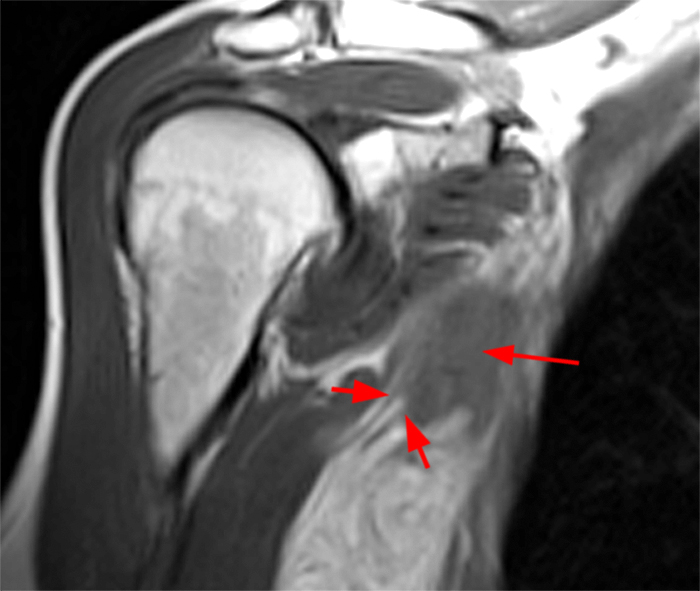
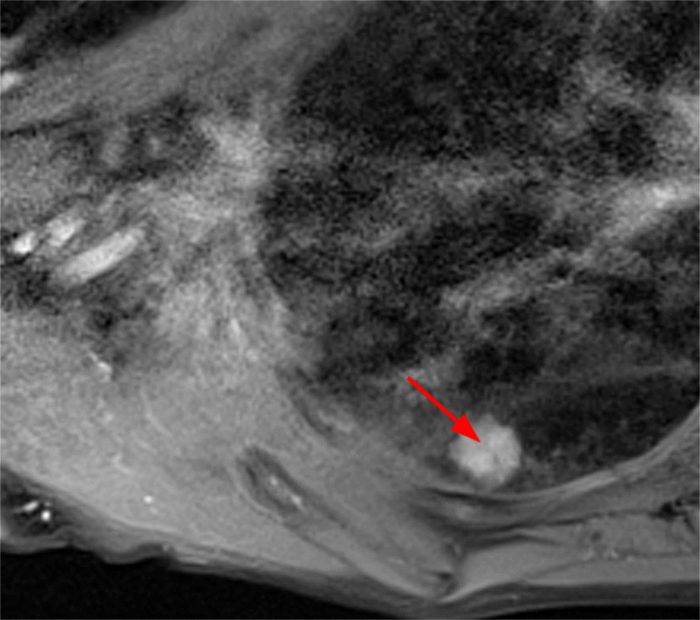
Axial T2-weighted (3a) and corresponding coronal short tau inverison recovery (STIR) images (3b) of the right upper extremity of the patient in the test case demonstrate denervation edema within lateral and long heads of the triceps muscle (blue and red asterisks, respectively) in a radial nerve (predominately C7-C8 nerve root) distribution.
Introduction
Injury to the brachial plexus, or brachial plexopathy, is most frequently due to trauma but can be due to several other etiologies, including radiation therapy, benign or malignant neoplasms, paraneoplastic syndromes, infection and autoimmune reactions.1,2 MRI plays a valuable role in evaluating direct and indirect signs of brachial plexus injuries and complements injury localization with electromyography.
Anatomy
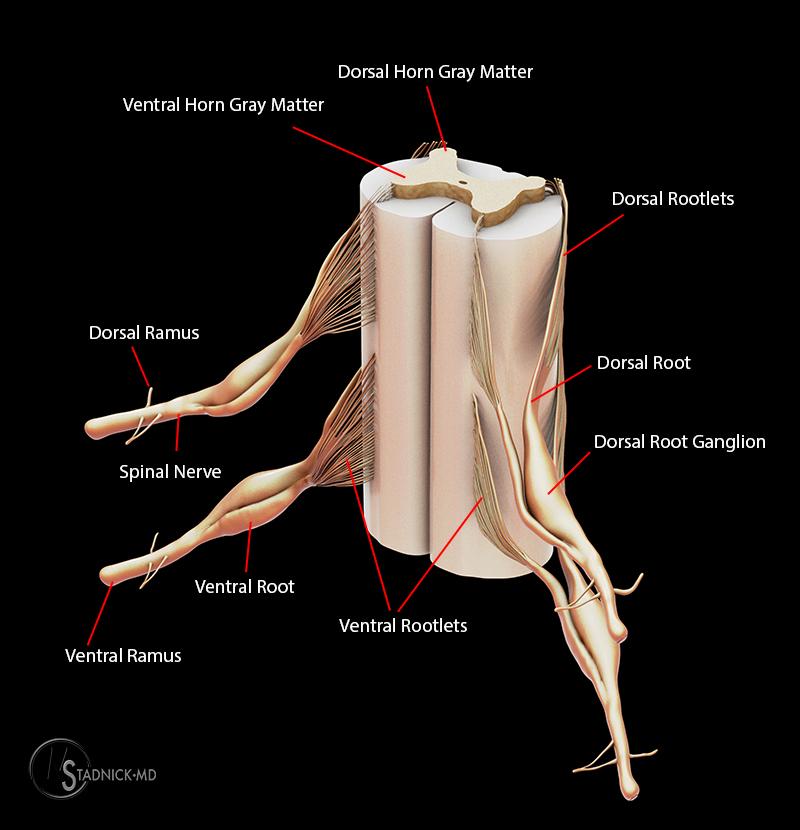
The brachial plexus (BP) provides sensory and motor innervation to the shoulders and upper extremities and is divided into roots, trunks, divisions, cords and terminal branches. The BP is formed by the ventral rami of the C5-8 and T1 nerve roots. Anatomic variations also exist with formation by the ventral roots of the C4-7 nerves (termed a “pre-fixed” brachial plexus) or the ventral roots of C6-T2 (a “post-fixed” brachial plexus).3 Ventral and dorsal rootlets emerge from the spinal cord to form ventral and dorsal nerve roots, respectively, which then join just distal to the dorsal root ganglia. This nerve root then branches into ventral and dorsal rami containing motor and sensory fibers (Figure 4).3
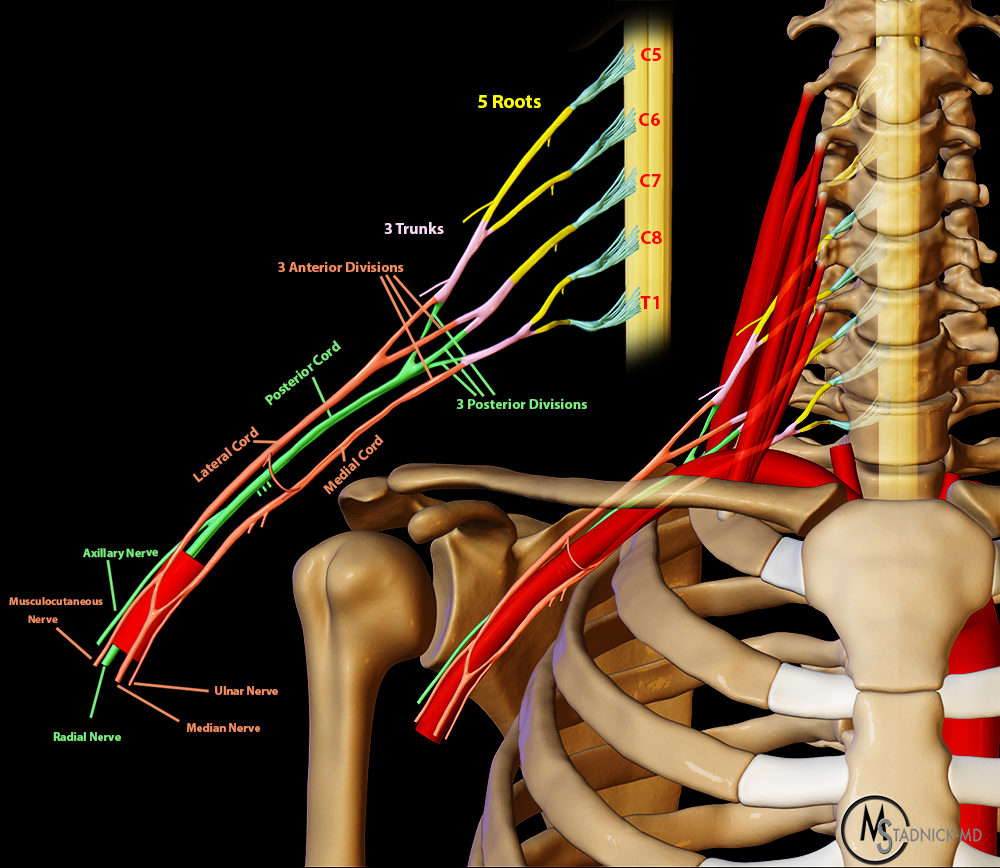
The ventral rami of the nerve roots continue into the interscalene triangle, between the anterior and middle/posterior scalene muscles and superior to the first rib and subclavian artery (Figures 5, 6 and 7). Within the interscalene triangle, the C5 and C6 nerve roots form an upper trunk, the C7 nerve root forms a middle trunk, and the C8 and T1 nerve roots form a lower trunk.4,5,6,7 The trunks travel superior to the subclavian artery and divide into three anterior and three posterior divisions. The divisions then travel in the costoclavicular space, posterior to the subclavius muscle and middle third of the clavicle, and anterior to the first rib and posterior scalene muscle.8 More distally at an infraclavicular location, the divisions form medial, lateral and posterior cords, each cord named relative to the adjacent axillary artery.4,5,9 In relation to the axillary artery, the lateral cord is located anterosuperior, the medial cord posteroinferior and the posterior cord superoposterior to the artery (Figure 8).8 At the distal margin of the pectoralis minor muscle, the cords divide into terminal branches including the axillary, median, radial, ulnar, long thoracic and musculocutaneous nerves with additional smaller terminal branches.4,5,6,7
Normal MRI anatomy of the brachial plexus
Figure 6:
Sequential coronal 3D STIR (6a-b) images from posterior to anterior demonstrate the course of a normal brachial plexus. Figure 6a demonstrates the right C5 nerve root (arrow) and C6 and C7 trunks (short arrow) just superior to the subclavian artery (blue asterisk). The medial and posterior cords (arrowheads) are seen superior and posterior to the axillary artery (red asterisk). The lateral margin of the 1st rib denotes the transition point from the subclavian to the axillary artery. Figure 6b at a slightly more anterior location shows the divisions superior to the subclavian artery (arrow) and medial (red arrowhead) and lateral (blue arrowhead) cords along the axillary artery (red asterisk). The most lateral aspect of the trunks are also also included (short arrow). Small lymph nodes are seen in the lower neck.
Figure 7:
Coronal T1-weighted (7a) and sagittal T2-weighted (7b) images through the lateral interscalene triangle. Figures 7a-b show the root/trunk junctions of the BP (arrows) with surrounding fat as they extend between the anterior (short arrows) and middle scalene muscles (arrowhead in 7b) and superior to the subclavian artery (red asterisk). The first rib (blue asterisk) and subclavian artery constitute the inferior border of the interscalene triangle.
Figure 8:
Axial T1-weighted (8a) and sagittal T2-weighted (8b) images demonstrate cords (arrowheads) posterior to the pectoralis minor muscle (short arrows) and along the margins of the axillary artery (red asterisk). The cords divide into terminal branches (not shown) at the most lateral margin of the pectoralis minor muscle.
Pathology of the brachial plexus
Brachial plexopathy is usually catagorized as supraclavicular, retroclavicular and infraclavicular. The location of pathology along the brachial plexus, particularly in the setting of trauma, has important prognostic and treatment implications.
Supraclavicular lesions involve the roots or trunks and represent the most common location for brachial plexus injuries. Nerve root injuries are most frequently secondary to severe traction due to a motor vehicle or motorcycle accident.1,2,10 When evaluating nerve root injuries, determining whether a lesion is proximal to the dorsal root ganglion (pre-ganglionic) or distal to the dorsal root ganglion (post-ganglionic) has important clinical implications. Pre-ganglionic injuries due to nerve root avulsions are particularly devastating injuries that commonly occur in younger adults with very limited spontaneous recovery or return of motor function.11 In addition to absent nerve roots/rootlets in the spinal canal, post-traumatic pseudomeningoceles are a common secondary finding associated with nerve root avulsions (Figure 9). Frequently seen at more than one ipsilateral contiguous level, traumatic pseudomeningoceles represent extradural fluid collections after a tear in the dura and arachnoid mater, usually with an intraspinal and extraspinal component extending into the neural foramen.12 However, a post-traumatic pseudomeningocele may occur without a nerve root avulsion. Therefore, additional imaging with high-resolution 3D MR neurography or thin section CT myelography is usually indicated to allow direct visualization of the ventral and dorsal nerve roots/rootlets.8
Figure 9:
22-year-old male involved in a recent motor vehicle accident with clinical suspicion for brachial plexus injury. Sagittal T2-weighted (9a-b) images from medial to lateral and axial T2* gradient echo images at the C7-T1 (9c) and T1-2 (9d) levels demonstrate traumatic extradural pseudomeningoceles (arrows) without visualization of the C8 and T1 nerve roots in the spinal canal. Although the C8 and T1 nerve roots are likely completely avulsed, a CT myelogram was recommended for direct nerve root visualization and potential surgical planning. Note the normal, more caudal T1 and T2 nerve roots (short arrows in 9a-b) and normal contralateral right C8 and T1 nerve roots (arrowheads in 9c-d).
Traumatic brachial plexus injuries may occur from traction, compression, direct contusion or less commonly transection.1 In the setting of multisystem trauma, particulary common injuries associated with BP pathology include closed head injuries, cervical spine fractures, scapular and clavicle fractures and subclavian or axillary artery injuries, including pseudoaneurysm formation.13 Apart from motor vehicle accidents, BP trauma is particularly common in contact sports. A “stinger”, usually resulting in temporary pain, burning or paresthesias, is most frequently due to traction of the C5 or C6 nerves, and typically occurs at least once in the career of 50% of American football players.14,15,16,17 Glenohumeral dislocation may also injure the axillary nerve. Prolonged BP compression or traction due to tight backpack straps is referred to as Rucksack Palsy.18 Obstetrical trauma associated with shoulder dystocia or extreme lateral neck flexion during delivery can result in traction or compression of the BP, typically affecting the C5-7 nerve roots (most frequently an Erb’s palsy involving the C5-6 nerve roots).1,2 MRI findings of BP trauma include nerve enlargement, nerve signal hyperintensity on T2-weighted sequences (particularly when compared to the normal contralateral side), deviated course of the nerve, nerve discontinuity and development of a neuroma.8 Indirect findings of nerve injury include edema in the perineural fat, compressive hematomas and muscle denervation changes, including edema in the acute or subacute phases and fatty atrophy in the chronic phase.
Nontraumatic causes of brachial plexopathy
Non-traumatic causes of BP injury that may be seen on MRI include radiation fibrosis, metastatic tumors (predominantly breast and lung carcinoma) and benign tumors (particulary peripheral nerve sheath tumors).19 Radiation fibrosis usually occurs after several months to years following treatment, with a peak incidence of 10-20 months following completion of radiation therapy.19,20,21 MR findings favoring radiation fibrosis over tumor infiltraton include diffuse nerve thickening without focal nodularity, diffuse rather than focal nerve enhancement, ill-defined isointense to low T1 and T2 signal intensity relative to muscle within the surrounding perineural fat and absence of an adjacent mass.19 However, some overlap of imaging features can exist, particulary on post-contrast images.
Breast and lung carcinoma are the two most common malignancies to involve the brachial plexus. Lymphatic drainage of breast carcinoma to axillary lymph nodes in proximity to the cords and branches of the BP predispose them to invasion or compression (Figure 10).2
Figure 10:
A 72-year-old female with a history of breast cancer presents with right periscapular and finger pain. A coronal T1-weighted (10a) image of the right shoulder shows a large metastatic lymph node (arrow) invading the distal cords and proximal branches (short arrows) of the BP. An axial proton-density fat suppressed (10b) image from the same shoulder exam demonstrates a metastatic posterior right lung nodule (arrow).
Superior sulcus tumors, or Pancoast tumors, involve the lung apex and are most commonly due to bronchogenic adenocarcinoma.22 Patients frequently present with severe shoulder pain radiating to the neck and upper extremity and Horner’s syndrome (ipsilateral ptosis, miosis, enopthalmos and anhidrosis) due to involvement of the sympathetic chain and inferior cervical (stellate) ganglion.22 This locally aggressive tumor has a propensity for direct invasion of the brachial plexus, particularly the C8-T2 nerves, in addition to the subclavian vessels, first rib and adjacent vertebrae (Figure 11).22 Superior extension of a Pancoast tumor commonly results in effacement of the interscalene fat between the anterior and middle scalene muscles associated with invasion of the traversing BP roots or trunks.
Figure 11:
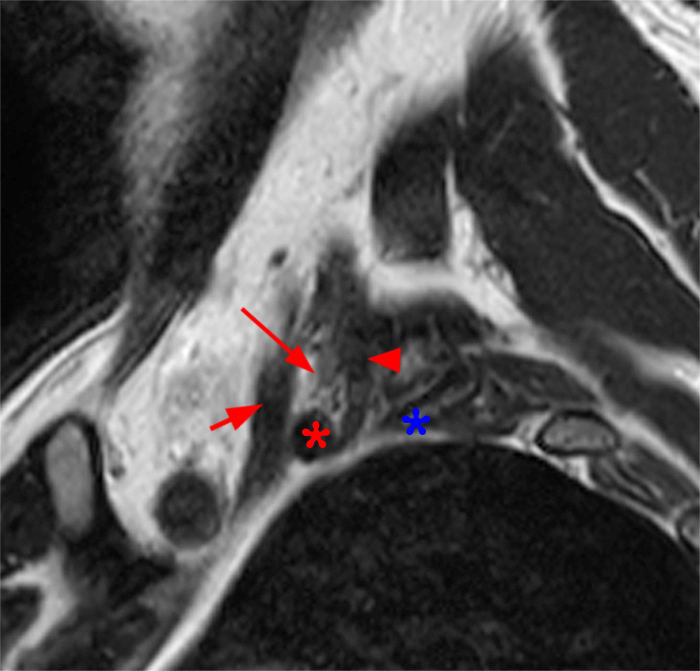
72-year-old male with left arm pain and weakness. Sagittal T2-weighted (11a-b) images of the cervical spine from medial to lateral demonstrate a newly discovered Pancoast tumor (blue asterisk) invading the left C8 (arrows), T1 (short arrows) and T2 (arrowheads) nerve roots. Also note near circumferential encasement of the left subclavian artery (red asterisk). Corresponding consecutive axial T2-weighted (11c,d) images at the T1-2 vertebral level at the superior margin of the tumor (blue asterisk) show invasion of the left C8 nerve root (arrow) and abutting the 1st rib and verterbral body (arrowheads). At the next slice (11d), tumor (blue asterisk) involves the T1 nerve root, which is thickened from invasion, at and lateral to the dorsal root ganglion (short arrow). Note the normal caliber and signal of the more laterally located BP divisions (arrowheads) just posterior to the subclavian artery (red asterisk) and anterolateral to the 1st rib (green asterisk).
Although more infrequent than malignant neoplasms, several benign lesions can also compress or involve the brachial plexus, most commonly peripheral nerve sheath tumors (PNST). Neurofibromas are the most common peripheral nerve sheath tumor to involve the brachial plexus, usually with multifocal or diffuse involvement in patients with neurofibromatosis type 1.19,23 Other PNST include schwannomas, ganglioneuromas or rarely malignant peripheral nerve sheath tumors (which are typically greater than 5 cm in size and demonstrate more rapid growth and heterogeneous signal but can sometimes be difficult to distinguish from benign PNST).8 In additon to following the course of a nerve, PNST are typically fusiform in shape, with neurofibromas located centrally along the nerve and schwannomas more commonly located in an eccentric location relative to the nerve.24 Additional imaging features of PNST include a target sign (central T2 hypointensity with surrounding T2 hyperintensity and central contrast enhancement) usually seen with neurofibromas, a fascicular sign demonstrating ring-like foci of T2 hypointense signal surrounded by T2 signal hyperintensity (Figure 12) and a split-fat sign with well-defined fat margins along the superior and inferior margins of of the PNST due to its intermuscular location (of note, other benign non-neurogenic tumors may also demonstrate a spit-fat sign).24
Figure 12:
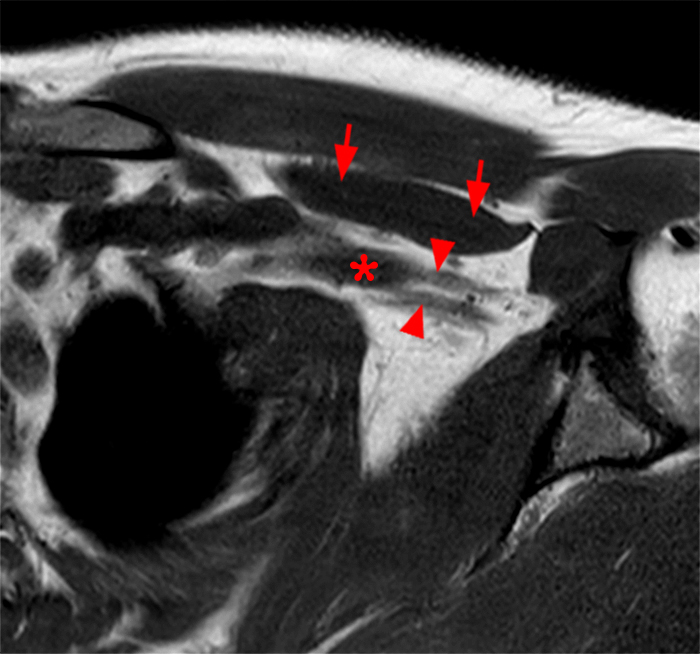
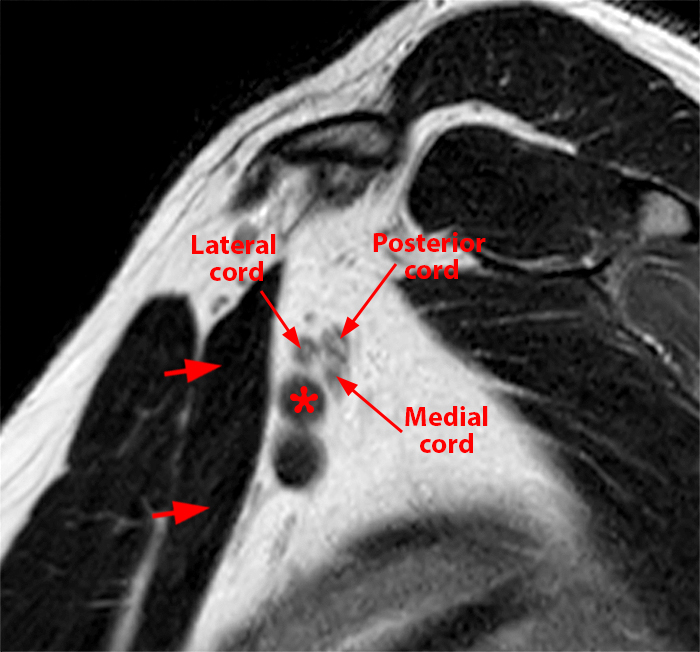
65-year-old male with a stable PNST over the past 2.5 years. A coronal T1-weighted (12a) image and a coronal T2-weighted fat suppressed (12b) image demonstrate a fusiform PNST (arrow) involving the medial cord of the BP. The subclavian artery (red asterisk), axillary artery (double red asterisks) and axillary vein (double blue asterisks) are seen. Corresponding sagittal T2-weighted images from medial to lateral (12a and 12b) demonstrate the PNST (arrows) eccentrically involving the medial cord (short arrows) posterior to the axillary artery (double red asterisks) and axillary vein (double blue asterisks), favoring a schwannoma over a neurofibroma. The uninvolved lateral cord (arrowheads) superior to the axillary artery (double red asterisks) and posterior cord (blue arrowheads) posterosuperior to the axillary artery are also seen. Note the fascicular sign (ring-like foci of T2 hypointense signal surrounded by T2 signal hyperintensity) commonly seen with PNST.
Other benign lesions which can result in compressive brachial plexopathy include lipomas, fibromatosis (extra-abdominal desmoids), low-flow or mixed veno-lymphatic vascular malformations and post-traumatic hematomas or cysts. Diffuse BP involvement may also be seen with hypertrophic polyneuropathies (such as a Charcot-Marie-Tooth disease or chronic inflammatory demyelinating polyneuropathy).25
Neurogenic thoracic outlet syndrome is an infrequent cause of compression of the BP. Reported causes include hypertrophy of the scalene muscles, aberrant intramuscular course of trunks, fibrous bands or a cervical rib.26,27,28,29
Parsonage-Turner Syndrome, also known as brachial neuritis, idiopathic brachial plexopathy or neuralgic amyotrophy is an uncommon cause of shoulder pain, although not infrequently encountered on shoulder MRI.30 Please refer to last month’s Web Clinic – April 2019 for an in depth discussion of Parsonage-Turner Syndrome.
Treatment
Surgical options for pre-ganglionic root avulsions are limited, including nerve transfers or more recently nerve grafts directly implanted into the spinal cord with partial recovery of proximal upper extremity muscle function.31 Post-ganglionic injuries are more amenable to surgical repair with options including nerve grafts, nerve transfers (neurotization), direct end-to-end repair and palliative reconstruction.32 Outcomes are typically better when surgery is performed at least 3-4 months after the initial injury to allow for spontaneous improvement but prior to 20-24 months before permanent denervation changes occur. Pre-ganglionic injuries are commonly surgically treated within 8 weeks.1
Non-surgical treatments for BP trauma include physical and occupational therapy, including avoiding exacerbating repetitive activities, and functional orthotics.1,2,33 Commonly used medications to manage neuropathic pain include gabapentin, amitriptyline, duloxetine and opiods. Pain management with transcutaneous electrical nerve stimulation (TENS), spinal cord or peripheral nerve stimulators and sympathetic blocks are also options.1
Conclusion
Brachial plexopathy can be due to a variety of causes, most commonly trauma. With excellent soft tissue contrast, MRI accurately localizes BP pathology and demonstrates direct and indirect signs of nerve injury which can have important prognostic implications. In addition to evaluating BP trauma, MRI is also invaluable to characterize masses compressing or invading the brachial plexus, particularly in the setting of breast or lung carcinoma or lesions directly involving the BP, as with peripheral nerve sheath tumors. For idiopathic brachial plexopathy, MRI is also useful to exclude other more common causes of shoulder pain such as rotator cuff pathology.
References
- Karandikar, N. S., Zakrasek, E. (2013, September 20, updated 2017, August 16). Brachial Plexopathy: Differential Diagnosis and Treatment. PM&R Knowledge Now. Retrieved from https://now.aapmr.org. ↩
- Ferrante, M.A., Brachial plexopathies: classification, causes, and consequences. Muscle Nerve. 2004. 30(5):547-68. ↩
- Castillo, M. Imaging the Anatomy of the Brachial Plexus: Review and Self-Assessment Module. American Journal of Roentgenology. 2005;185: S196-S204. ↩
- Vijayasarathi A, Chokshi FH. MRI of the brachial plexus: A practical review. Appl Radiol. 2016;45(4):9-18. ↩
- Rehman I, Chokshi FH, Khosa F. MR Imaging of the Brachial Plexus. Clin Neuroradiol. 2014;24(3):207-216. ↩
- Mikityansky I, Zager EL, Yousem DM, et al. MR Imaging of the Brachial Plexus. Magn Reson Imaging Clin N Am. 2012;20(4):791–826. ↩
- Martinoli C, Gandolfo N, Perez MM, et al. Brachial plexus and nerves about the shoulder. Semin Musculoskeletal Radiol. 2010;14(5):523–546. ↩
- Chhabra A, Thawait GK, Soldatos, T, et al. High-Resolution 3T MR Neurography of the Brachial Plexus and Its Branches, with Emphasis on 3D Imaging. AJNR Am J Neuroradiol. 2013;34(3):486–497. ↩
- Van Es HW, Bollen TL, Heesewijk HPM. MRI of the brachial plexus: a pictorial review. Eur J Radiol. 2010;74(2):391–402. ↩
- Sakellariou VI, Badilas NK, Mazis GA, et al. Brachial Plexus Injuries in Adults: Evaluation and Diagnostic Approach. ISRN orthopaedics. 2014;1–9. doi:10.1155/2014/726103. ↩
- Moran SL, Steinmann SP, Shin AY. Adult brachial plexus injuries: mechanism, patterns of injury, and physical diagnosis. Hand Clin. 2005;21(1):13-24. ↩
- Khosla A, Wippold FJ. CT Myelography and MR Imaging of Extramedullary Cysts of the Spinal Canal in Adult and Pediatric Patients. American Journal of Roentgenology. 2002;178(1):201–207. ↩
- Midha R. Epidemiology of brachial plexus injuries in a multitrauma population. Neurosurgery. 1997; 40(6):1182-8; discussion 1188-9. ↩
- Daly CA, Payne SH, Seiler JG. Severe Brachial Plexus Injuries in American Football. orthopaedics. 2016; 39(6):e1188-e1192. ↩
- Castro FP Jr, Ricciardi J, Brunet ME, et al. Stingers, the Torg ratio, and the cervical spine. Am J Sports Med. 1997;25(5):603-608. ↩
- Castro FP Jr. Stingers, cervical cord neurapraxia, and stenosis. Clin Sports Med. 2003; 22(3):483-492. ↩
- Charbonneau RM, McVeigh SA, Thompson K. Brachial neuropraxia in Canadian Atlantic University sport football players: what is the incidence of “stingers”? Clin J Sport Med. 2012;22(6):472-477. ↩
- Nahas S, Yeoh C, Jahnich H. Upper Brachial Plexus Palsy (Rucksack Palsy). J Trauma Treat. 2018;07(1)419. ↩
- Wittenberg KH, Adkins MC. MR Imaging of Nontraumatic Brachial Plexopathies: Frequency and Spectrum of Findings. RadioGraphics. 2000; 20(4)1023–1032. ↩
- Moore NR, Dixon AK, Wheeler TK, et al. Axillary fibrosis or recurrent tumor: an MRI study in breast cancer. Clin Radiol. 1990; 42:42-46. ↩
- Kori SH, Foley KM, Posner K. Brachial plexus lesions in patients with cancer: 100 cases. Neurology. 1989; 39:450-451. ↩
- Marulli G, Battistella L, Mammana M, et al. Superior sulcus tumors (Pancoast tumors). Ann Transl Med. 2016;4(12):239. ↩
- Mukherji SK, Castillo M, Wagle AG. The brachial plexus. Semin Ultrasound CT MR. 1996; 17:519-538. ↩
- Kakkar C, Shetty CM, Koteshwara P, Bajpai S. Telltale signs of peripheral neurogenic tumors on magnetic resonance imaging. Indian J Radiol Imaging. 2015;25(4):453-8. ↩
- Thawait SK, Chaudhry V, Thawait GK, et al. High-resolution MRN of diffuse peripheral nerve lesions. AJNR Am J Neuroradiol. 2011;32:1365–72. ↩
- Chhabra A, Lee PP, Bizzell C, et al. 3 Tesla MR neurography: technique, interpretation, and pitfalls. Skeletal Radiol. 2011;40:1249–60. ↩
- Demondion X, Herbinet P, Van Sint Jan S, et al. Imaging assessment of thoracic outlet syndrome. Radiographics. 2006;26:1735–50. ↩
- Aralasmak A, Karaali K, Cevikol C, et al. MR imaging findings in brachial plexopathy with thoracic outlet syndrome. AJNR Am J Neuroradiol. 2010;31(3):410–17. ↩
- Parker EE, Glastonbury CM.MR imaging of the thoracic inlet. Magn Reson Imaging Clin N Am. 2008;16:341–53. ↩
- van Alfen N, Clinical and pathophysiological concepts of neuralgic amyotrophy. Nat Rev Neurol. 2011; 7(6):315-22. ↩
- Bertelli JA, Ghizoni MF. Brachial plexus avulsion injury repairs with nerve transfers and nerve grafts directly implanted into the spinal cord yield partial recovery of shoulder and elbow movements. Neurosurgery. 2003;52:1385-1389. ↩
- Bertelli JA, Ghizoni MF. Results and current approach for Brachial Plexus reconstruction. J Brachial Plex Peripher Nerve Inj. 2011;6(1):2. ↩
- Cooper J. Occupational therapy intervention with radiation-induced brachial plexopathy. Eur J Cancer Care (Engl). 1998;7(2):88-92. ↩