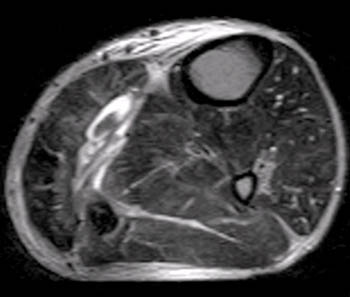
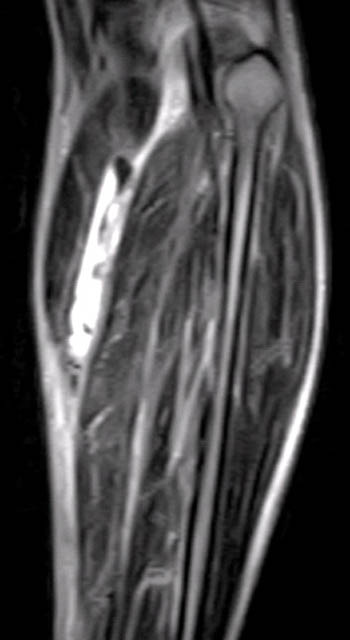
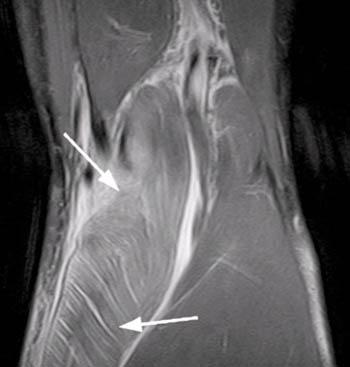
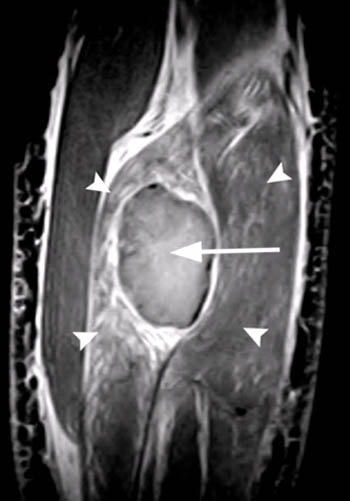
Clinical History: A 44 year-old male presents with calf pain after being injured while pushing a vehicle, at which time he heard a “pop” in his calf. (1a) Axial and (1b) coronal T2-weighted images are provided. What are the findings” What is your diagnosis?
Findings
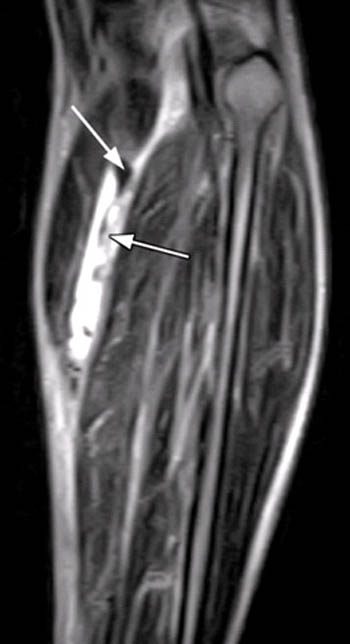
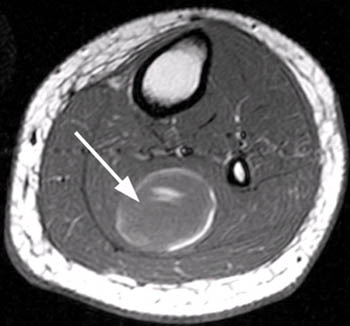
Figure 2:
(2a) The T2-weighted axial image demonstrates fluid between the soleus muscle (white arrow) and the medial head of the gastrocnemius muscle (white arrowhead). Irregular low signal intensity within the fluid collection (black arrow) represents the remnant of the ruptured plantaris tendon.
Diagnosis
Plantaris tendon rupture.
Discussion
The plantaris muscle is of questionable physiological importance. It is thought to be a vestigial structure and is absent in 7% to 10% of the population. Despite these facts, injuries to the plantaris are a not uncommon cause of patient pain, and can present with a confusing clinical picture, thus making an understanding of plantaris anatomy and related pathology important to those who utilize and interpret MRI.
The plantaris arises from the lateral supracondylar line of the distal femur, just superior and medial to the lateral head of the gastrocnemius muscle, and from the oblique popliteal ligament. The plantaris muscle belly lies deep to the lateral head of the gastrocnemius muscle, but the long thin plantaris tendon courses obliquely and medially, lying between the soleus muscle and the medial head of the gastrocnemius muscle. Distally, the tendon lies near the medial border of the Achilles tendon, and inserts on the calcaneus just anteromedial to the Achilles tendon (4a). The plantaris is a component of the triceps surae muscle group, which includes the soleus and gastrocnemius muscles in the superficial posterior compartment of the calf. Like the gastrocnemius muscles, the plantaris muscle traverses two joints, which may make it more vulnerable to injury.1
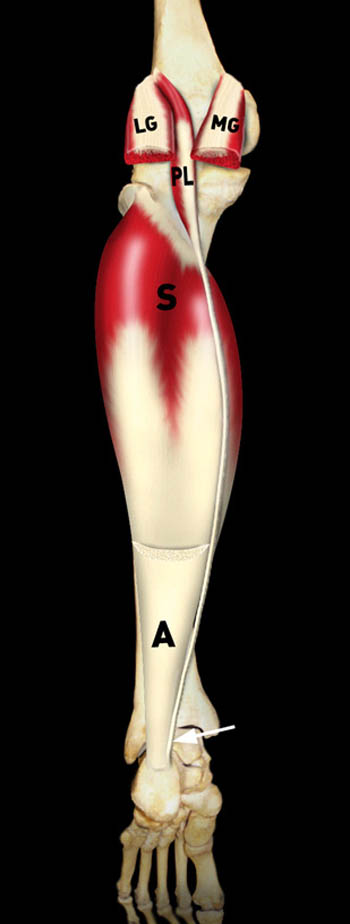
Figure 4:
(4a) This graphic representation of the posterior calf with the medial gastrocnemius (MG) and lateral gastrocnemius (LG) muscle bellies removed demonstrates the plantaris muscle (PL), which originates from the inferior aspect of the lateral supracondylar line of the distal femur adjacent to the origin of the lateral gastrocnemius (LG). The plantaris tendon passes obliquely between the gastrocnemius and the soleus (S) muscles. Distally, the plantaris tendon (arrow) can be seen blending with the medial aspect of the distal Achilles tendon (A) and inserting upon the middle third of the posterior surface of the calcaneus.
Rupture of the plantaris tendon typically occurs in middle-aged patients, often with the mechanism of injury involving forced dorsiflexion of the ankle with the knee in extension (as in our car-pushing patient). The injury may be accompanied by an audible “pop” in the calf, with subsequent pain and swelling, and frequently with a palpable mass caused by hematoma. Injury to the popliteus muscle belly can also occur, but this is more often associated with other injuries, such as ACL tears and posterolateral corner injuries.2,3
An isolated injury to the plantaris tendon or myotendinous junction has been described as “tennis leg.” Powell first described this clinical entity in 1883.4 While there has been controversy in the orthopaedic literature as to whether the clinical entity of plantaris tendon rupture really exists,5 surgically confirmed cases of plantaris tendon rupture have been well documented.6 Tennis leg may be seen in young athletes or in sedentary older individuals. A tearing sensation or pop is often reported, with pain increasing over one to two days and with tenderness and swelling found at the calf.
Though tennis leg is classically caused by rupture of the plantaris muscle, the term is also used more generally and may refer to a strain of the medial head of the gastrocnemius muscle or the soleus muscle (5a,6a). A recent study using ultrasound imaging of patients with a diagnosis of tennis leg found injuries to the medial head of the gastrocnemius muscle more common than plantaris tendon rupture.1 The distinction between plantaris tendon rupture and other calf muscle injuries is important, since the gastrocnemius or soleus injuries are generally more severe and require longer to heal. Such injuries may necessitate splinting with the ankle in dorsiflexion, and may call for dedicated rehabilitation. While these varying muscle injuries are often impossible to differentiate clinically, MRI can accurately distinguish between the entities.
Plantaris tendon rupture and medial head of the gastrocnemius muscle rupture may also occur together, in which case MRI would demonstrate edema of the medial head of the gastrocnemius muscle, fluid between the soleus and medial gastrocnemius muscles, and a visible torn plantaris tendon. Visualization of the torn plantaris tendon is important, since fluid between the soleus muscle and medial gastrocnemius muscle is non-specific, and can be seen with plantaris tendon rupture, medial gastrocnemius muscle injury, or a ruptured popliteal cyst.
The differential diagnosis of calf pain includes the more serious clinical entities of deep venous thrombosis (DVT) and compartment syndrome, as well as Achilles tendon rupture. In the proper clinical situation, calf pain with an otherwise negative MRI raises suspicion for DVT. In such cases, calf MRI may not reliably demonstrate DVT, but Doppler ultrasonography or MR venography can accurately demonstrate a venous occlusion. An Achilles tendon rupture is easily differentiated from plantaris tendon rupture on MRI. Compartment syndrome can also be distinguished from plantaris or gastrocnemius muscle injury, since it demonstrates a more diffuse muscle edema pattern. Compartment syndrome, however, may be seen in conjunction with calf muscle injuries, as a result of hematoma and swelling (7a,8a).
Conclusion
The causes of calf pain are multiple, and often difficult to diagnose clinically. In the diagnosis of tennis leg, MRI can clearly distinguish the more clinically severe medial gastrocnemius or soleus muscle tears from isolated plantaris tendon ruptures. MRI is also useful in differentiating between other serious causes of calf pain such as DVT, compartment syndrome, or Achilles tendon rupture.
References
1 Delgado GJ, Chung CB, Lektrakul N, Azocar P, Botte MJ, Coria D, Bosch E, Resnick D. Tennis Leg: Clinical US Study of 141 Patients and Anatomic Investigation of Four Cadavers with MR Imaging and US. Radiology 2002; 224:112-119.
2 Helms CA, Fritz RC, Garvin GJ. Plantaris muscle injury: evaluation with MR imaging. Radiology 1995; 195:201-203.
3 Bencardino JT, Rosenberg ZS, Brown RR, Hassankhani A, Lustrin ES, Beltran J. Traumatic musculotendinous injuries of the knee: diagnosis with MR imaging. RadioGraphics 2000; 20:103-120.
4 Powell RW. Lawn tennis leg. Lancet 1883; 2:44.
5 Severance HJ, Bassett FH III. Rupture of the Plantaris: does it exist” JBone Joint Surg [Am] 1982: 64:1387-1388.
6 Hamilton W, Klostermeier T, Lim E, Moulton JS. Surgically documented rupture of the plantaris muscle: a case report and literature review. Foot Ankle Int 1977; 18:522-523.
7 Guillodo Y, Botton E, Saraux A, Le Goff P. Effusion between the aponeuroses (letter). J Ultrasound Med 1999; 18:860-861.