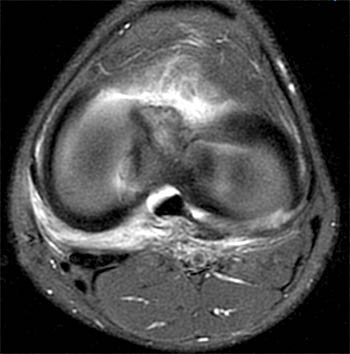
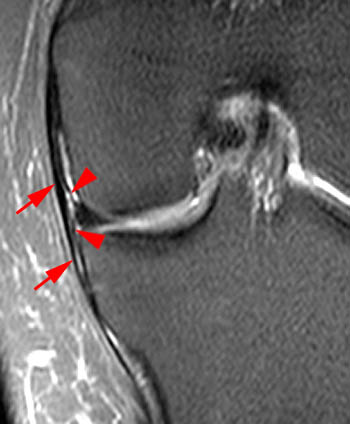
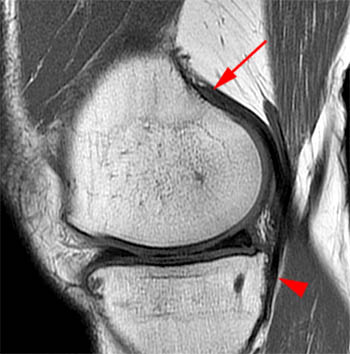
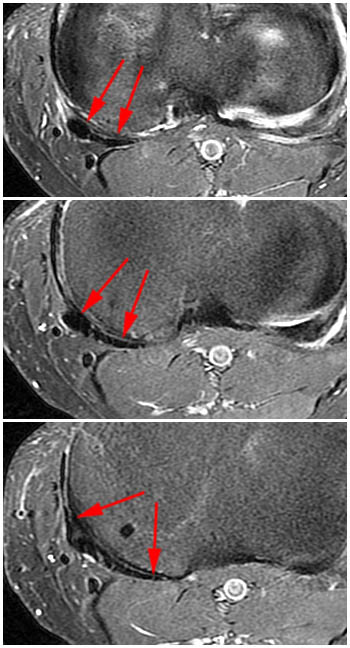
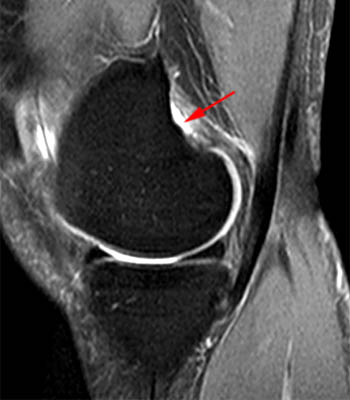
Clinical History: A 13 year-old male twisted his knee playing basketball 2 weeks ago. The MR demonstrates an ACL tear (not shown). Fat-suppressed proton density axial (1a) and coronal (1b) images from the study are provided. What additional findings can be seen? What is the diagnosis?
Findings
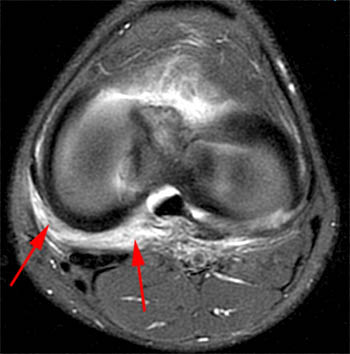
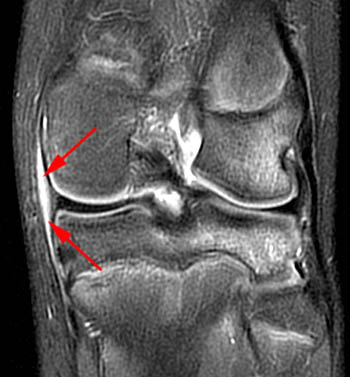
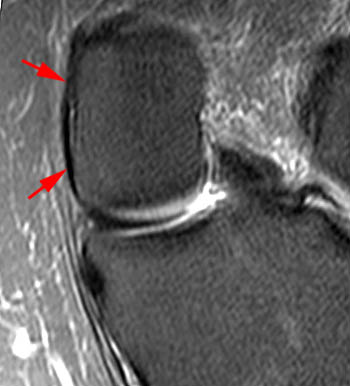
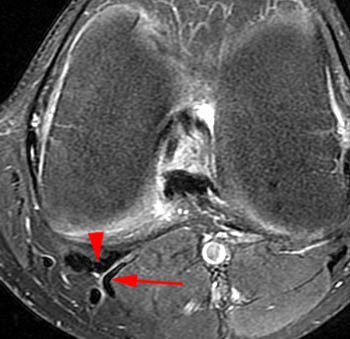
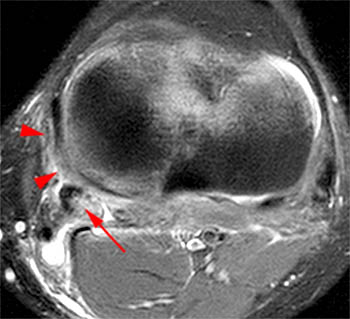
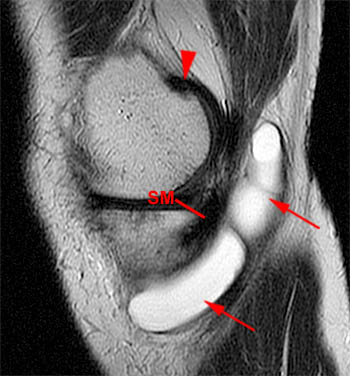
Figure 2:
(2a)The axial image demonstrates edema along the joint line in the posteromedial and posterior central knee (arrows). This edema is in the expected location of the posterior oblique and oblique popliteal ligaments and the posterior joint capsule. (2b) The coronal image also shows posteromedial edema, posterior to the MCL (arrows).
Diagnosis
Posteromedial corner injury of the knee.
Introduction
The posteromedial corner of the knee (PMC) is comprised of the structures between the posterior border of the superficial medial collateral ligament (SMCL) and the medial border of the posterior cruciate ligament (PCL). This includes the posterior oblique ligament (POL), semimembranosus tendon (SM), the oblique popliteal ligament (OPL) and the posterior horn of the medial meniscus (PHMM).1,2,3 The medial head of the gastrocnemius also provides support.4 These structures are important for knee stability but have received much less attention in the radiology literature than the posterolateral corner. It is important to identify injuries of the PMC as, unlike isolated MCL injuries, they do not tend to heal without surgery and can lead to instability of the knee which can cause chronic pain and lead to late failure of cruciate ligament reconstructions.2
Anatomy and Function
The POL originates from the adductor tubercle of the medial femur, just posterior and proximal to the MCL and anterior and inferior to the medial head of the gastrocnemius. The POL has three distal arms. The central or tibial component is the most prominent and attaches strongly to the PHMM near the posterior tibial articular surface. The superior or capsular arm is most posterior and is continuous with the posterior joint capsule and the OPL, lying deep to the medial head of the gastrocnemius. The distal or superficial arm is the most anterior and is associated with the SM tendon, attaching to the tendon sheath and inserting on the tibia just distally to the SM.1,2,3,4
The semimembranosus tendon fans out distally with 5 insertions, attaching to bone, capsule, ligaments and the medial meniscus. The SM flexes and internally rotates the knee and pulls the PHMM out of the joint during flexion, preventing impingement of the meniscus by apposing surfaces of the tibia and femur. It provides dynamic stability to the knee during flexion, causing increased tension in the joint capsule and POL, which increases medial stability, and in the OPL, which assists with lateral capsular stability.1,3 The OPL connects the posterior medial and lateral knee, attaching medially to the capsular arm of the POL and the SM and coursing superolaterally along the posterior joint capsule to the arcuate ligament and lateral head of the gastrocnemius.3 These structures of the PMC are biomechanically and structurally separate from the SMCL. The PMC is a primary stabilizer of the extended knee, the load-bearing position of the knee in gait. The SMCL becomes the stabilizer in flexion as the PMC slackens. The POL is the primary stabilizer for internal rotation at all flexion angles and helps prevent posterior translation in extension. The POL, with the SMCL, stabilizes valgus stress, internal and external rotation and anterior and posterior tibial motion. The PMC also mitigates posterior translation in the PCL deficient knee.2
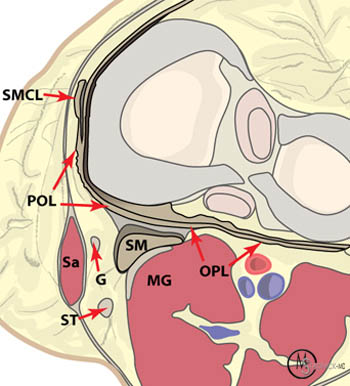
Figure 3:
An axial plane illustration of the knee at the level of the menisci demonstrates the components of the posteromedial corner. At this level the semimembranosus (SM) can be seen contributing fibers to the oblique popliteal ligament (OPL) and to the posterior capsule. The posterior oblique ligament (POL) is found between the superficial medial collateral ligament (SMCL) and the semimembranosus tendon on this view. The medial head of the gastrocnemius muscle (MG), sartorius muscle (SA), gracilis tendon (G) and semitendinosus tendon (ST) are also indicated.
MR Imaging
Many of the normal individual components of the PMC are difficult to see on MRI because of their complex anatomy, thinness and close association with other structures.4 The POL can be identified by location, as it forms the capsular layer posterior to the SMCL (Figures 4-7). The medial gastrocnemius tendon and the semimembranosus can typically be directly visualized on either sagittal or axial images. The OPL is not typically directly visualized on routine MR images.
Many injuries of the PMC can be identified by recognizing edema and soft-tissue thickening at the posteromedial knee, posterior to the MCL, in the expected location of the POL. Following trauma, injuries to the POL may be accompanied by marrow edema due to avulsive forces related to the strong proximal attachment of the POL at the adductor tubercle (Figures 8 and 9). As the medial gastrocnemius tendon and SM tendon3,4 can be directly visualized, injuries to these structures can be specifically diagnosed by recognizing the intrinsic abnormalities of the affected regions (Figures 10 and 11). Of course, not all causes of posteromedial edema or fluid are related to the PMC. Other causes of posteromedial edema include a ruptured popliteal cyst, parameniscal cyst and pes anserine bursitis (Figure 12).
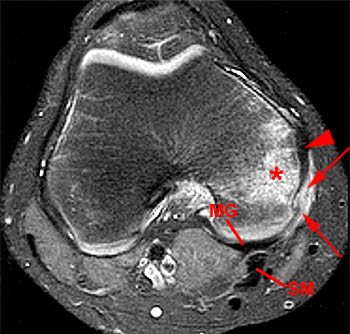
Figure 8:
An axial fat-suppressed proton density-weighted image in a 13 year old following a fall with twisting reveals soft tissue thickening and edema throughout the region of the POL (arrows). The low signal intensity SMCL (arrowhead) is visible anterior to the region of the POL. Marrow edema (asterisk) is visible within the medial femoral condyle as well. The medial gastrocnemius tendon (MG) and the semimembranosus tendon (SM) are unaffected.
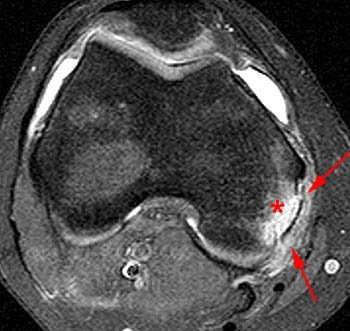
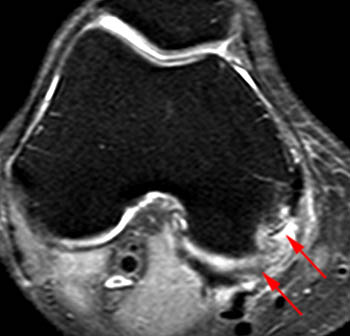
Figure 9:
Axial and coronal fat-suppressed proton density images in a 15 year-old with medial pain demonstrate avulsive marrow edema within the medial epicondyle (asterisks), at the expected attachment site of the POL. There is edema and soft tissue thickening in the region of the POL (arrows).
Clinical Evaluation and Treatment
Clinical evaluation for PMC injuries includes testing for medial opening of the knee with valgus stress with the knee in full extension and in 30 degrees of flexion. With isolated SMCL injuries, the knee will be unstable in flexion. If instability is demonstrated in extension, the capsule and/or POL are injured.2 Another pattern of instability that can occur is termed anteromedial rotatory instability (AMRI). This refers to anterior subluxation and external rotation of the medial tibial plateau with respect to the femur. Patients with symptomatic AMRI almost always have an injury of the POL.2 Isolated MCL injuries are treated conservatively as chronic instability is rare.2 Acute MCL and PMC injuries are repaired only in the context of multi-ligament injury. In these cases the cruciate tear is repaired first, then the medial structures are repaired or reconstructed, from deepest to most superficial. The meniscus and meniscocapsular area are treated, followed by the SMCL. If a repair is performed, the POL and postermedial capsule are then sutured to the MCL and the lax SM attachments are retensioned to the POL or MCL.2 Reconstruction is frequently performed using the semitendinosus tendon which is released, leaving the pes anserinus insertion intact. The graft is secured at the femoral insertion of the SMCL with the free end recreating the POL.2,5 There is controversy as to whether early or late repair should be performed, if at all.5 Complications of MCL and PMC surgery are rare, the most common being knee stiffness which is treated with manipulation. Saphenous nerve injury can also occur.2
Conclusion
Injuries of the posteromedial corner of the knee are easily overlooked but functionally significant. Knowledge of the anatomy of this area is crucial as the imaging findings may consist of edema without clear visualization of the individual structures. Proper identification of PMC injuries may lead to alterations in the treatment pathway, particularly in the setting of coexistent cruciate ligament disruption.
References
1 Sims WF, Jacobson KE. The posteromedial corner of the knee, medial-sided injury patterns revisited. Am J Sports Med, Mar 2004; 32(2):337-345.
2 Tibor LM, Marchant Jr MH, Taylor DC, Hardaker WT, Garrett WE, Sekiya JK. Management of medial-sided knee injuries, Part 2, posteromedial corner. Am J Sports Med, Dec 20, 2010.
3 Resnick D, Kang HS, Pretterklieber ML. Internal Derangement of Joints 2nd edition. Saunders Elsevier.
4 Loredo R, Hodler J, Pedowitz R, Yeh LR, Trudell D, Resnick, D. Posteromedial corner of the knee: MR imaging with gross anatomic correlation. Skeletal Radiology; 28(6): 305-311.
5 Lind M, Jakobsen BW, Lund B, Hansen MS, Abdallah O, Christiansen SE. Anatomical reconstruction of the medial collateral ligament and posteromedial corner of the knee in patients with chronic medial collateral ligament instability. Am J Sports Med, June 2009; 37(6): 1116-1122.