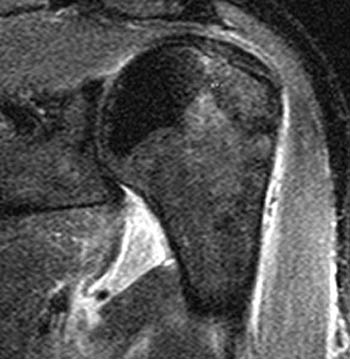
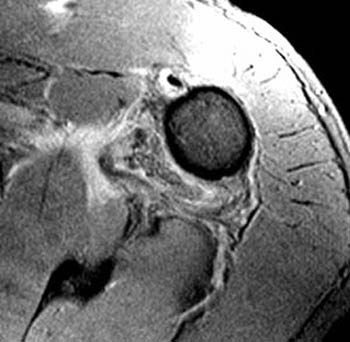
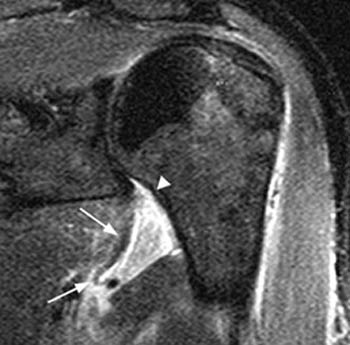
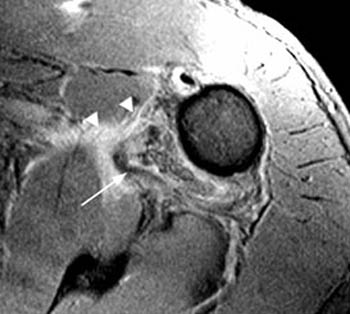
Clinical History: A 28 year-old male sustained a shoulder injury while playing hockey. (1a) Fat-suppressed T2-weighted coronal-oblique and (1b) fat-suppressed proton density-weighted axial images are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Humeral avulsion of the inferior glenohumeral ligament (The HAGL lesion).
Discussion
Recurrent anterior glenohumeral instability is a common clinical problem that can lead to significant disability in all age groups. Shoulder instability may arise from avulsion of the ligament-labral complex at the glenoid (the Bankart lesion), intrasubstance glenohumeral ligament tears, or abnormal laxity of the glenohumeral ligaments.1,2 A lesser known entity, the humeral avulsion of the inferior glenohumeral ligament (HAGL),3,4 has also been identified as being an important contributor to anterior instability.
Anterior dislocations are usually the result of direct or indirect trauma with the arm forced into abduction and external rotation. Anterior dislocations are by far the most frequent type of shoulder dislocation, representing more than 90% of such injuries. When the shoulder is in abduction and external rotation, the most important structure limiting anteroinferior subluxation and dislocation is the inferior glenohumeral ligament (IGL).
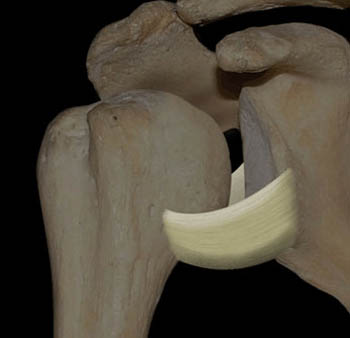
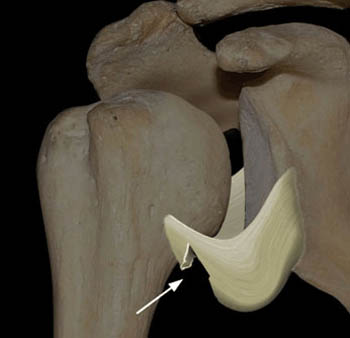
The IGL has a sling-like geometry consisting of an anterior band, a posterior band, and the axillary recess of the capsule between these bands (Figure 4). The anterior band extends from the anteroinferior aspect of the labrum to the surgical neck of the humerus. The posterior band extends from the posteroinferior aspect of the labrum to the surgical neck of the humerus. The anterior band usually is thicker than the posterior band.
Cadaver studies indicate that under tension, the inferior glenohumeral ligament fails at the glenoid 40% of the time, creating the well-known Bankart lesion. The IGL fails at the mid-ligament 35% of the time, and at its humeral attachment 25% of the time,5 the latter resulting in the HAGL lesion. In actual clinical experience, the frequency of HAGL lesions is somewhat lower, having an incidence of 8-10%.
Wolf and colleagues identified HAGL lesions in 9.3% of 64 shoulders preoperatively evaluated by arthroscopy for anterior instability, and 35% of the shoulders were unstable without labral pathology at the level of the glenoid rim.3 Thus, the HAGL lesion may exist in patients with anterior instability, with or without an associated anterior labral tear. Therefore, recurrent shoulder instability thought in the past to result from capsular laxity, may actually be secondary to the pathoanatomy of the HAGL lesion.
HAGL lesions are well-visualized with MRI. MR imaging signs include a thickened, wavy contour and increased signal intensity within the ligament. The IGL is considered abnormal if it is absent, discontinuous, or attenuated. As in this case, a J-shaped appearance to the torn IGL may be found, caused by inferior drooping of the typically U-shaped ligament. In a subset of patients, the IGL injury causes an avulsion fracture at the humeral attachment. This appearance has been termed a BHAGL lesion (bony humeral avulsion of the IGL), and can be recognized on MRI and on plain films due to the irregular ossific fragment that is created by the avulsion injury.
In patients with HAGL lesions, associated injuries to the rotator cuff, humeral head, and labrum are quite common, and should be carefully searched for. In patients with rotator cuff tear, the vast majority of tears, greater than 95%, will involve the subscapularis tendon. Evaluation for associated medial dislocation of the biceps tendon is indicated in such cases.
At arthroscopy, a HAGL lesion may be overlooked if the relevant area is not closely inspected. With open procedures, a medial capsular approach may result in non-visualization of a HAGL lesion. With lateral capsular approaches, careful dissection is required so as not to confuse a HAGL lesion with an iatrogenic capsular breach occurring during division of the subscapularis.7 With proper identification, primary repair of HAGL lesions can be performed via arthroscopic or open technique. Operative repair is thought to considerably reduce the chances of recurrent anterior dislocation.
Conclusion
The HAGL lesion is an important cause of anterior instability at the glenohumeral joint. Because this abnormality may be overlooked in patients undergoing shoulder stabilization procedures, pre-operative diagnosis with MRI is invaluable in the proper management of affected patients.
References
1 Stoller DW, Wolf EM. The Shoulder. N: Stoller DW, ed. Magnetic Resonance Imaging in Orthopaedics and Sports Medicine. Philadelphia: JB Lippincott, 1997: 597-748.
2 Neviaser TJ. The Anterior Labral Ligamentous Periosteal Sleeve Avulsion Lesion: A Cause of Anterior Instability of the Shoulder. Arthroscopy 1993; 9: 17-21.
3 Wolf EM, Chang JC, Dixon K. Humeral Avulsion of Glenohumeral Ligaments as a Cause of Anterior Shoulder Instability. Arthroscopy 1995; 11: 600-607.
4 Tirman PFJ, Steinbach LS, Feller JF, Stauffer AE. Humeral Avulsion of the Anterior Shoulder Stabilizing Structures After Anterior Shoulder Dislocation: Demonstration by MRI and MR Arthrography. Skeletal Radiol 1996; 25:743-748.
5 Bigliani LU, Pawluk, RG, Soslowski LJ, Flatow EL, Pawluk RJ, Mow VC. Tensile Properties of the Inferior Glenohumeral Ligament. J. Orthop Res 1992; 10:187-197.
6 Oberlander NA. The BHAGL Lesion: A New Variant of Anterior Shoulder Instability. Arthroscopy 12:6-7, 1997.
7 Bui-Mansfield LT, Taylor DC, Uhorchak JM, Tenutal JJ. Humeral Avulsions of the Glenohumeral Ligament: Imaging Features and a Review of the Literature. AJR 2002; 179:649-655.