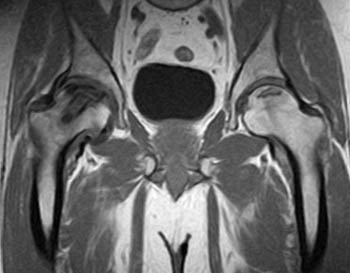
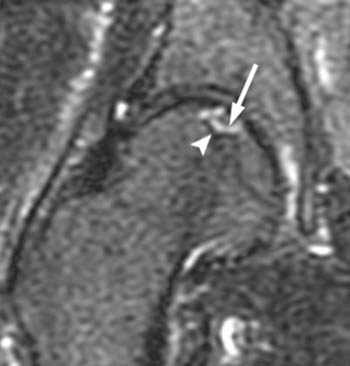
Clinical History: A 62 year-old male with a history of right sciatica and previous right femoral head core decompression for avascular necrosis (AVN) presents with recurrent pain. A coronal T1-weighted image (1a) is shown. What is the unexpected finding and what is the diagnosis?
Findings
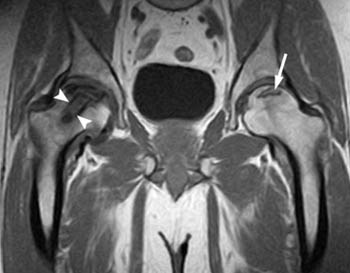
(2a) Right hip AVN was diagnosed one year prior in this patient, and stigmata of core decompression are seen at the right femoral head (arrowheads) on this T1-weighted image. Signal changes compatible with occult left hip AVN (arrow) are noted on the asymptomatic contralateral side.
Diagnosis
Clinically occult left femoral head avascular necrosis (AVN).
Introduction
The femoral head is the most common location for avascular necrosis (AVN). AVN of the hip is a significant cause of morbidity in the United States, and can affect patients both young and old. With disease progression, articular surface collapse and secondary osteoarthritis develop, and the end result in many patients is total hip replacement.
Pathophysiology
The exact pathophysiology of AVN remains somewhat controversial, but most agree that the cell death found in AVN is related to some type of interruption in the normal blood supply. The potential causes of interruption are numerous, and include trauma, corticosteroid use, sickle cell disease, alcoholism, radiation, and Caisson’s disease. While trauma, steroids, and alcoholism predominate in the United States, in Africa, HIV infection and hemoglobinopathies are a significant source of AVN. In the Mediterranean and in Southeast Asia, the highly prevalent thallassemias are a major cause.
Many authors feel that AVN results from an acute interruption of blood supply, as is seen with trauma, thrombosis, or embolization. Others feel that the cause is vasculopathic in nature, with damage to arterial or venous walls resulting in structural damage, constriction, or release of vasoactive substances. Quite likely, the cause is multifactorial, as many factors influence the eventual development of osteonecrosis.
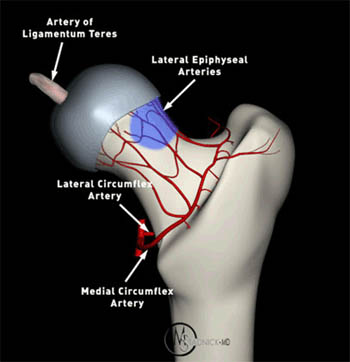
The femoral head is the most vulnerable site for development of AVN. The site of necrosis is usually immediately below the weightbearing articular surface of the bone, most commonly at the anterolateral aspect of the femoral head. The anterolateral head is the site of the greatest mechanical stress, directly affecting the lateral epiphyseal arteries (3a). However, no region of the femoral head is protected from AVN.
Once AVN develops, repair begins at the interface between viable and necrotic bone, with lymphocyte infiltration occurring early in the disease process. Dead bone is ineffectively removed, and thus reactive and reparative bone is formed over regions of necrosis. Hyperemia, inflammation, and fibrosis are found to varying degrees, and this variability in part accounts for the changing appearance of hip AVN on MR images.
Clinical
AVN may be acutely painful, but as seen in the case above, it can also be asymptomatic. Huang et al noted that presence of bone marrow edema on MRI correlated with a much greater likelihood of a symptomatic lesion. Similarly, joint effusions, often present with AVN, also increase the likelihood of a symptomatic lesion, particularly when paired with marrow edema.
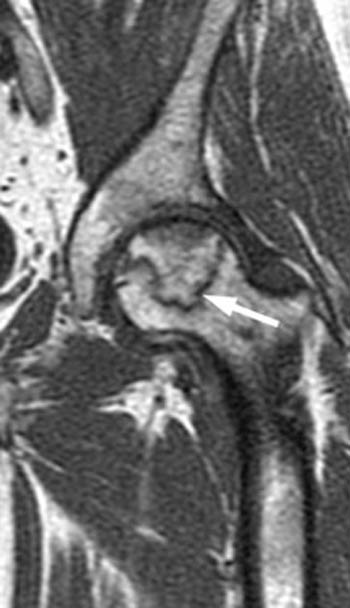
The treatment of choice for early AVN remains core decompression, which is thought to decrease vascular engorgement and inflammation, thereby treating the “compartment syndrome” within the hip and its resultant increased intramedullary pressure. Recombinant human bone morphogenetic protein (rhBMP) has been used as an adjuvant therapy to core decompression. This substance enhances bone formation and decreases bone resorption, and thus assists in maintaining the structural integrity of the femoral head to limit the development of femoral head collapse. Rotational osteotomy and bone grafting have yielded limited success in select cases. Complications of AVN included development of stress fractures, which can propagate distally into the femoral neck region (4a), femoral head collapse, joint space narrowing, and severe osteoarthritis.
MR of AVN
Early detection of hip AVN is critical, as all treatments geared towards preservation of the femoral head are more successful early in the course of the disease. Of all imaging tests, MRI is the most sensitive means to diagnose AVN. At high magnetic field strength, MRI is more sensitive than CT scanning or nuclear scintigraphy, and is much more sensitive than plain film radiography for detecting AVN. Numerous studies have demonstrated that MRI is highly sensitive, specific, and accurate in the detection of AVN.
T1-weighted images: AVN most often presents with a crescentic, ring-like or well defined band of low signal within the superior portion of the subchondral femoral head bone marrow (5a). This band is thought to represent the reactive interface between the necrotic and reparative zones, and typically extends to the subchondral plate.
T2 weighted images: The subchondral lesion shows a high signal intensity inner border with a low signal intensity peripheral rim. This is termed the “double-line” sign, which may add to the specificity in the diagnosis of AVN.
The MRI staging classification of Mitchell et al. (see Table 1) describes four classes of AVN based on the signal characteristics within the center of the lesion on T1 and T2-weighted images. This classification may be useful in grading lesion acuity, as infarcted bone will tend to progress through the classes of signal intensity over time. However, this progression is not always consistent, and more than one class of signal abnormality may be found in a single lesion.
| Table 1: MRI staging of AVN 8 | |||
| Class | T1 | T2 | Definition |
| A | bright | intermediate | “fat” signal |
| B | bright | bright | “blood” signal |
| C | intermediate | bright | “fluid” or “edema” signal |
| D | dark | dark | “fibrosis” signal |
Currently, the prognostic value of MRI is thought to be more dependent upon the size and location of lesions noted on the examination. Small lesions confined to the medial anterosuperior portion of the femoral head tend not to collapse, and thus may be amenable to conservative therapy. AVN that does not contact the subchondral margins tends to have a good prognosis regardless of lesion size. Larger lesions with articular surface involvement are more likely to collapse and thus may warrant core decompression. Shimizu et al. found a 74% rate of femoral head collapse if the region of AVN on MRI involved more than two-thirds of the weightbearing surface area.
Conclusion
MRI is indispensable for the detection and accurate staging of AVN because it is able to clearly depict the size of the lesion, and estimates of the stage of disease can be made. MRI allows sequential evaluation of asymptomatic lesions that are undetectable on plain radiographs. MRI facilitates better responses to treatment since AVN can be diagnosed at an earlier stage, and therapeutic measures are more successful the earlier they are initiated.
References
1 Bluemke DA: Avascular necrosis of the hip: MR evaluation. Contemp Diagn Radiol 1996; 19: 23.
2 Huang G-S, Chan WP, Chang Y-C, et al: MR imaging of bone marrow edema and joint effusions in patients with osteonecrosis of the femoral head: relationship to pain. AJR 2003 Aug; 181: 545-549.
3 Bluemke DA, Zerhouni EA: MRI of avascular necrosis of bone. Top Magn Reson Imaging 1996 Aug; 8(4): 231-46 [Medline].
4 Lafforgue P, Dahan E, Chagnaud C, et al: Early-stage avascular necrosis of the femoral head: MR imaging for prognosis in 31 cases with at least 2 years of follow-up. Radiology 1993 Apr; 187(1): 199-204[Medline].
5 Mitchell DG, Rao VM, Dalinka MK, et al: Femoral head avascular necrosis: correlation of MR imaging, radiographic staging, radionuclide imaging, and clinical findings. Radiology 1987 Mar; 162(3): 709-15.
6 Shimizu K, Moriya H, Akita T: Prediction of collapsed with magnetic resonance imaging of avascular necrosis of the femoral head. JBJS (AM) 1994; 76: 215-233.