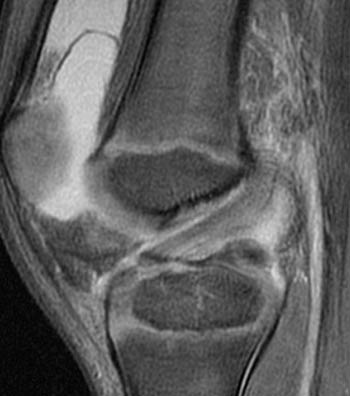
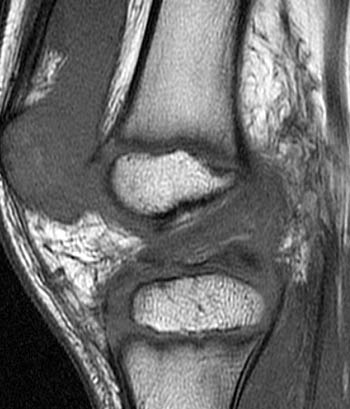
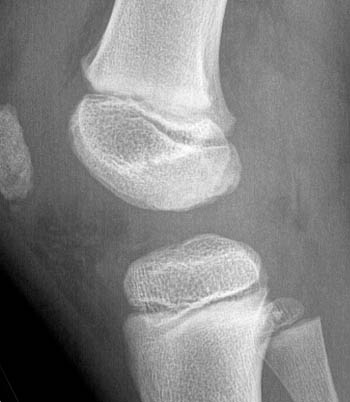
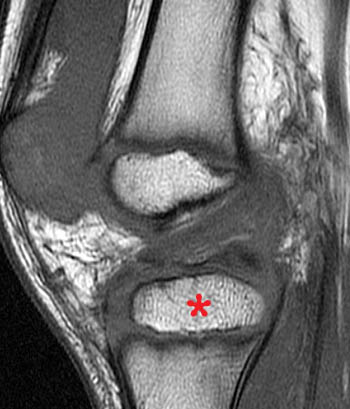
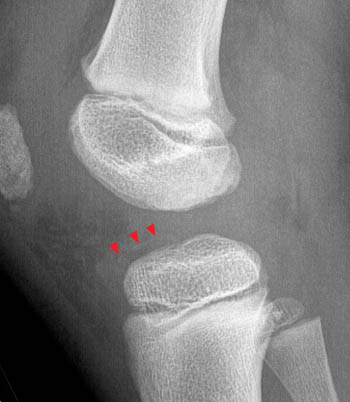
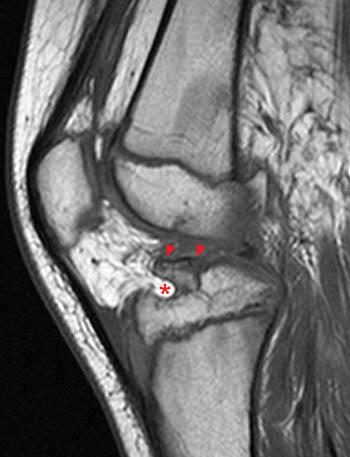
Clinical history: A 7 year-old boy was tackled two day ago. He twisted the knee and felt a pop. Evaluate for anterior cruciate ligament (ACL) tear. (1a) Fat-suppressed proton density and (1b) T1-weighted sagittal images and a (1c) lateral radiograph of the knee are provided. What are the findings? What is your diagnosis?
Findings
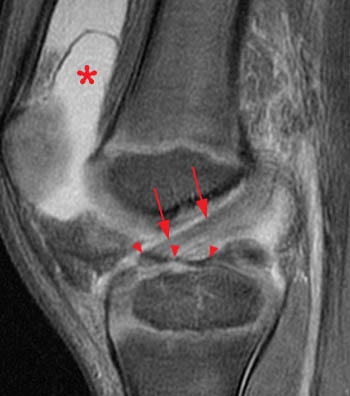
Figure 2:
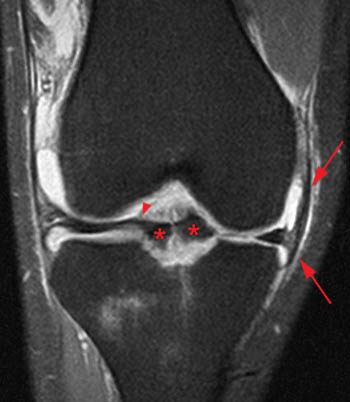
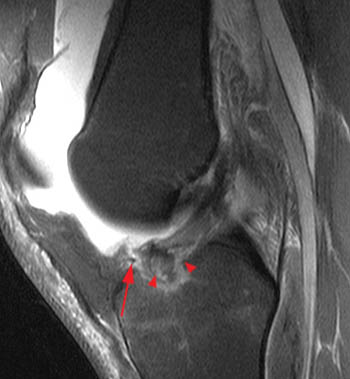
A low signal intensity line representing an avulsed cortical fragment (arrowheads) is demonstrated at the tibial eminence. A small portion of the adjacent non-ossified cartilage is also avulsed and is outlined by fluid. Intact ACL fibers (arrows) are inserting onto the fragment. The anterior margin of the fragment is mildly elevated, while the posterior portion of the fragment is nondisplaced, consistent with a hinged type fracture. Note that bone marrow edema at the fracture is minimal. A large joint effusion (asterisk) is present.
Diagnosis
Intercondylar tibial eminence fracture.
Introduction
The intercondylar tibial eminence fracture is one of the most common knee fractures in children1 and is usually seen between the ages of 8 and 14 years2. It is typically caused by forceful hyperextension or a direct blow upon the distal femur with the knee in flexion. The increased tension on the ACL will typically result in stretching or partial tearing of the ACL before the tibial eminence fractures1,4. The fracture could be nondisplaced or displaced, comminuted or non-comminuted5, and occasionally involves the posterior portion of the intercondylar eminence, especially in adults. There is a high incidence of injury to other structures of the knee joint such as the menisci, capsule, collateral ligaments, or articular cartilage in adults6.
Anatomy and biomechanics of tibial intercondylar eminence fractures
The tibial eminence is located between the articular surfaces of the medial and lateral tibial plateaus and includes the footprint for the ACL. In skeletally immature individuals, the collagen fibers of the ACL blend from ligament to perichondrium to epiphyseal cartilage, as opposed to adults where the ACL inserts directly into bone by Sharpey’s fibers7. This difference is thought to result in failure of the incompletely ossified tibial eminence in children and adolescents with knee injuries.
An isolated tear of the substance of the ACL and a tibial eminence fracture are different responses to similar types of abnormal joint forces, and the patterns of injury could be related to width of the femoral intercondylar notch. In a comparison study of age-and sex matched patients, those with a tear of the substance of the ACL had a significantly narrower notch index (the ratio of the notch width to the width of the distal femur) than those with tibial spine fractures8.
Intimate with the ACL footprint is the anterior root of the lateral meniscus. Structures located anterior to the ACL foot print include the transverse intermeniscal ligament and the anterior root of the medial meniscus. Structures located posterior to the ACL foot print include, in order from front to back, the posterior root of the lateral meniscus, the posterior root of the medial meniscus, and the posterior cruciate ligament (PCL) footprint9.
With a displaced tibial eminence fracture it is not uncommon to see entrapment of adjacent structures underneath the fragment. In one study intraoperative findings included entrapment of the anterior horn of the medial meniscus, transverse intermeniscal ligament, or anterior horn of the lateral meniscus in 26% of type II fractures and 65% of type III fractures10.
Classification
A classification system for tibial eminence fractures aimed at guiding treatment was initially proposed by Meyers and McKeever in 1959, and included three groups11. Type I is a nondisplaced fracture. Type II is a hinged fracture with the posterior cortex intact. Type III is a completely displaced fracture. This classification system was later expanded and included a type IV fracture which is displaced and comminuted12.
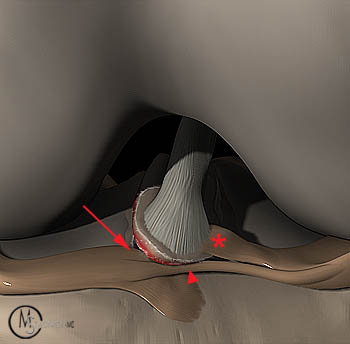
Figure 7:
This 3D graphic representation of a type III avulsion fracture highlights some of the structures that may become entrapped anteriorly or may hinder reduction of the fracture fragment: medial meniscus (arrow), transverse meniscal ligament (arrowhead), and anterior root of the lateral meniscus attachment to the avulsed fragment (asterisk).
Imaging
After initial staging of the fracture based on radiographs, cross-sectional imaging may be required for preoperative planning. CT is frequently used to enhance the understanding of the shape, size and orientation of the displaced fragment13. In the setting of a comminuted and displaced fracture, CT with 3 D reconstruction may be particularly helpful.
MRI enables the surgeon to plan not only the fixation of the tibial eminence fracture but also the repair of concomitant meniscal and ligament tears, as well as osteochondral lesions6,14. MRI aids in the detection of entrapment of soft tissue structures underneath the fragment, a situation which could prevent closed reduction.
The following cases of tibial eminence fractures show a spectrum of important findings on MR imaging.
Figure 9:
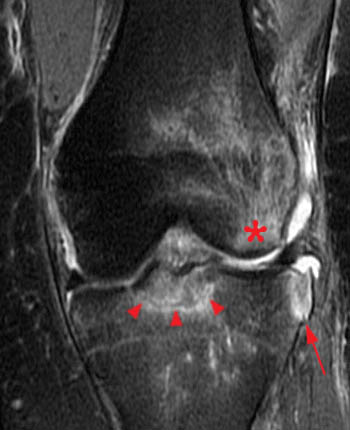
A comminuted, displaced tibial eminence fracture consistent with a type IV injury in an adult shown on a coronal T2-weighted image. The fragments (asterisks) are elevated and are no longer in contact with the underlying bone. Note that the anterior root of the lateral meniscus inserts onto one of the fragments (arrowhead), which could make fracture reduction more difficult. Concomitant injury includes a medial collateral ligament sprain (arrows).
Figure 10:
A proximally displaced and rotated tibial eminence fracture (type III) (arrowheads) in an adult on a fat-suppressed proton density-weighted sagittal view. The transverse meniscal ligament (arrow) is at the anterior margin of the fragment but is not entrapped. The ACL fibers are intact.
Figure 11:
A nondisplaced tibial eminence fracture (type I) (arrowheads) in an adult on a coronal fat-suppressed T2-weighted image. Other injuries include a Segond fracture (arrow), osteochondral injury of the lateral femoral condyle (asterisk), and a vertical longitudinal tear of the medial meniscus (not shown).
Figure 12:
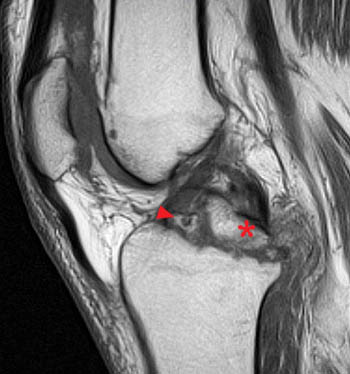
A T1-weighted sagittal image from an adult patient shows a large comminuted tibial eminence fracture with posterior extension. The tibial attachment sites of the anterior cruciate ligament(arrowhead), the posterior cruciate ligament (asterisk), the posterior roots of both menisci (not shown), and the anterior root of the lateral meniscus (not shown) are involved.
Management
Nondisplaced fractures (type I) of the tibial eminence in skeletally immature patients are treated nonsurgically. Immobilization of the knee in a cast or knee immobilizer for four to six weeks with the knee extended or in 20 degree of flexion is recommended5. Healing occurs within 6 to 12 week and should be followed by weight bearing and range-of-motion exercises4.
Successful closed reduction and anatomic healing in type II fracture can often be achieved by extending the knee and keeping the knee extended during immobilization15. If closed reduction fails, entrapment of a portion of the meniscus or the transverse intermeniscal ligament should be considered.
Displaced fractures were routinely treated with open reduction and internal fixation in the past but are now usually amenable to arthroscopic reduction and internal fixation with screws or sutures. Surgical pitfalls include inadvertent placement of hardware across an open physis followed by growth arrest. Screws may later become prominent and rub on the articular surface of the femoral condyle. Utilization of suture at arthroscopy is technically challenging but could be used across the physis if absorbable suture material is chosen2.
In type III fractures it is frequently found that the avulsed osseous fragment involves the insertion sites of both the ACL and the anterior horn of the lateral meniscus, with the meniscus displaced along with the fragment. This can prevent closed reduction because the fragment is pulled in two different directions. Successful reduction of type III injuries can only be performed arthroscopically by performing special manipulation and traction to the fragment via sutures placed around the anterior horn of the lateral meniscus16.
Because of the high incidence of concomitant injury to other structures of the joint it is essential to search for additional pathology at the time of arthroscopic surgery, and this search is aided by preoperative MRI6,14.
Postoperative complications of tibial eminence fractures include nonunion and malunion, which could lead to stiffness and flexion deformity of the knee, and which may require reoperation17. Laxity related to partial tear of the ACL at the time of injury is common, especially in patients with type II and type III fractures, but rarely requires ACL reconstruction18,19,20.
Conclusion
Tibial intercondylar eminence fractures are most common in children and teenagers but do also occur In adults. Staging and initial management are based on the modified version of the Meyers and McKeever classification using radiographs. MRI is extremely useful in the workup and management of these fractures because of the high incidence of concomitant injuries to the menisci, ligaments and cartilage. MRI can depict features that will prevent closed reduction, such as soft tissue entrapment underneath the fracture fragment, and involvement of the insertion site of the anterior horn of the lateral meniscus.
References
1 Mubarak SJ, Kim JR, Edmonds EW, Pring ME, Bastrom TP. Classification of proximal tibial fractures in children. J Child Orthop. 2009; 3(3): 191-197.
2 LaFrance RM, Giordano B, Goldblatt J, Voloshin I, Maloney M. Pediatric tibial eminence fractures: Evaluation and management. J Am Acad Orthop Surg 2010;18:395-405.
3 Kendall NS, Hsu SY, Chan KM. Fracture of the tibial spine in adults and children. A review of 31 cases. J Bone Joint Surg Br.1992; 74(6)848-852.
4 Accousti WK, Willis RB.Tibial eminence fractures. Orthop Clin North Am 2003;34(3):365-375.
5 Meyers MH, McKeever FM. Fracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am.1970; 52:1677-1684.
6 Monto RR, Cameron-Donaldson ML, Close MA, Ho CP, Hawkins RJ. Magnetic resonance imaging in the evaluation of tibial eminence fractures in adults. J Knee Surg, 2006; 19(3): 187-190.
7 Matz SO, Jackson DW. Anterior cruciate ligament injury in children. Am J Knee Surg 1988;1:59.
8 Kocher MS, Mandiga R, Klingele K, Bley L, Micheli LJ. Anterior cruciate ligament injury versus tibial spine fracture in the skeletally immature knee: a comparison of skeletal maturation and notch width index. J Pediatr Orthop 2004; 24 2):185-188.
9 Brody JM, Hulstyn MJ, Fleming BC, Tung GA. Pictorial essay: The meniscal roots: Gross anatomic correlation with 3-T MRI findings. AJR 2007;188:W446-W450.
10 Kocher MS, Micheli LJ, Gerbino P, Hresko TM. Tibial eminence fractures in children: prevalence of meniscal entrapment. Am J Sports Med 2003:31(3) 404-407.
11 Meyers MH, McKeever FM. Fracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am. 1959;41(2):209-222.
12 Zaricznyj B. Avulsion fracture of the tibial eminence: Treatment by open reduction and pinning. J Bone Joint Surg Am 1977; 59( 8):1111-1114.
13 Griffith JF, Antonio GE, Tong CW, Ming CK: Cruciate ligament avulsion fractures. Arthroscopy 2004; 20 (8 ):803-812.
14 Ishibashi Y, Tsuda E, Sasaki T, Toh S. Magnetic resonance imaging aids in detecting concomitant injuries in patients with tibial spine fractures. Clin Orthop Relat Res 2005; 434:207-212.
15 Wilfinger C, Castellani C, Raith J, Pilhatsch A, H?llwarth ME, Weinberg AM. Nonoperative treatment of tibial spine fractures in children-38 patients with a minimum follow-up of 1 year. J Orthop Trauma. 2009 Aug;23 (7):519-524.
16 Lowe J, Chaimsky G, Freedman A, Zion I, Howard C. The anatomy of tibial eminence fractures: arthroscopic observations following failed closed reduction. J Bone Joint Surg Am. 2002; 84-A(11):1933-1938.
17 Aderinto J, WalmsleyP, Keating JF: Fractures of the tibial spine: Epidemiology and outcome. Knee 2008;15 (3):164-167.
18 Perugia D, Basiglini L, Vadalà A, Ferretti A. Clinical and radiological results of arthroscopically treated tibial spine fractures in childhood. Int Orthop. 2009 Feb;33(1):243-8. Epub 2008 Nov 29.
19 Kocher MS, Foreman ES, Micheli LJ. Laxity and functional outcome after arthroscopic reduction and internal fixation of displaced tibial spine fractures in children. Arthroscopy. 2003 Dec;19(10):1085-90.
20 Willis RB, Blokker C, Stoll TM, et al. Long-term follow-up of anterior tibial eminence fractures. J Pediatr Orthop. 1993;13:361-364.