Clinical History: A 52 year-old male presents to his orthopaedic surgeon complaining of chronic bilateral hand numbness and tingling. He denies significant trauma in the past, ‘ictal’ episodes, or vasculitis. His motor and sensory exams and reflexes are normal although he does exhibit mild finger clonus. The patient was referred for an MRI of the cervical spine. What are the findings? What is the name of the imaging sign demonstrated by this case?
Findings
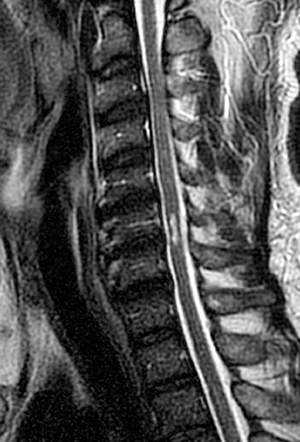
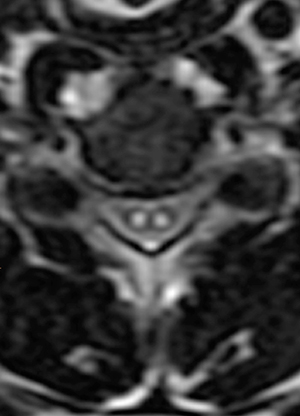
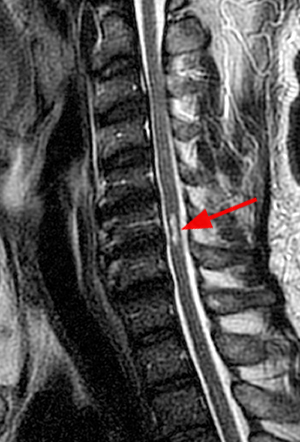
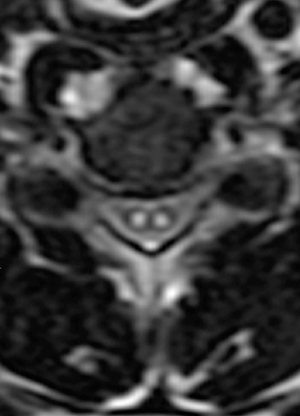
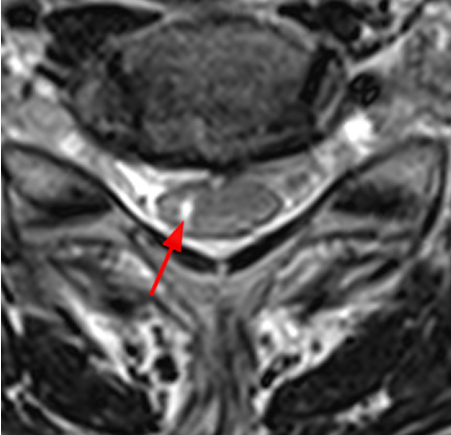
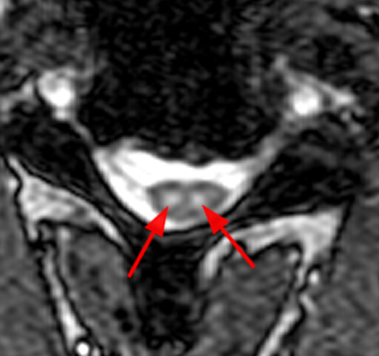
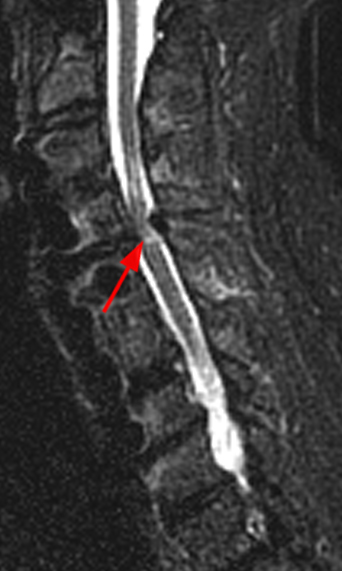
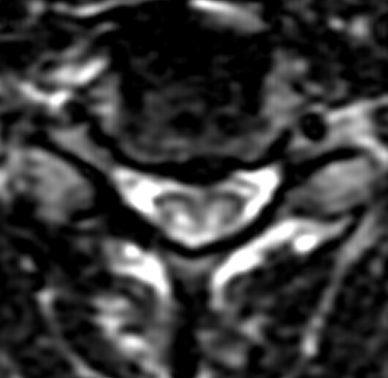
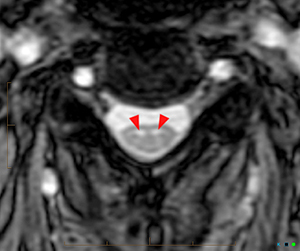
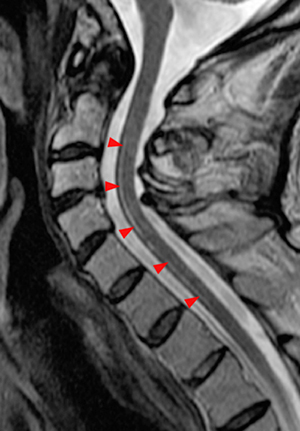
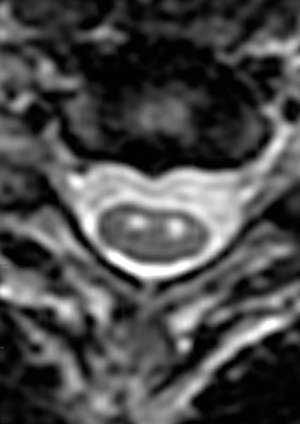
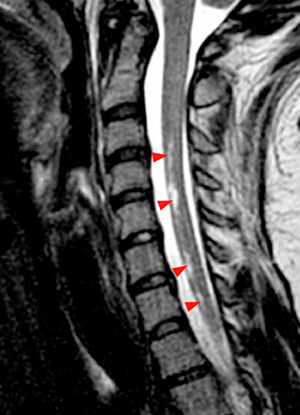
Figure 2:
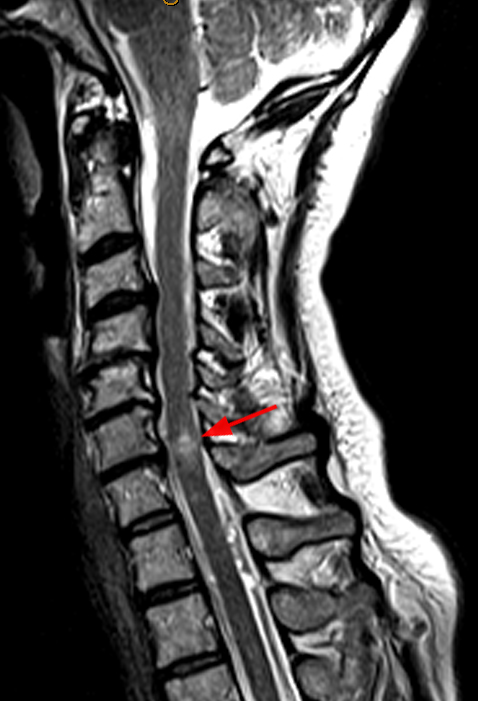
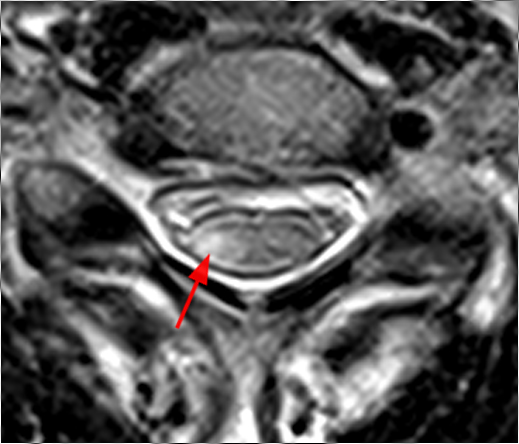
(2a) The T2-weighted sagittal midline image demonstrates elevated signal within the cord at the C6-7 level (arrow). The loss of cord volume and sharp circumscription suggest chronic gliosis rather than acute edema. The subarachnoid space of the mid cervical canal is subjectively relatively small compatible with developmental canal stenosis. (2b) The T2-weighted axial image at the level of C6 demonstrates bilaterally symmetric well- circumscribed circular shaped foci of increased signal intensity (arrowheads) compatible with intramedullary gliosis. The appearance approximates the shape of an owl's face with bright eyes 'staring' at the reader. The cord is not enlarged.
Answer
The Owl’s Eyes Sign.
Introduction
The Owl’s Eyes Sign has been used as a descriptive term in several reports since the advent of MR imaging and is most often thought of as a sign of cord infarction following occlusion of the anterior spinal arteries. The term Owl’s Eyes was perhaps first used by Mawad1 in 1990 but the “sign” was clearly demonstrated on MR in a case reported by Kulkarni in 19872. In fact it is a non-specific sign and not pathognomonic of infarction but can occur with a number of insults to the spinal cord including remote cord contusion, chronic compressive myelopathy, infection and inflammation. To understand why this pattern can develop in these conditions and more specifically why the Owl’s Eyes Sign is not more common requires an understanding of the cord’s vascular anatomy.
Vascular anatomy of the cervical cord
The majority of the blood supply to the spinal cord is from medullary branches of radicular arteries (sometimes called the radiculomedullary arteries) with lesser supply from the single anterior spinal artery and dual posterior spinal arteries. Although embryologically there are 31 pairs of radicular arteries to match the 31 pairs of spinal roots, in the adult neither symmetry, size or the number of radicular arteries is consistent, creating tremendous variability in identifiable “feeders” to the cord. Usually there are 7-8, often 6-10 and rarely only 2 medullary branches arising from the radicular arteries. There are usually 2 but sometimes no radicular arteries contributing to the cervical cord supply at each vertebral level. The radicular arteries arise as spinal branches from the posterior inferior cerebellar, vertebral, deep cervical, intercostal and lumbar arteries and enter the spinal canal through the neural foramina. By definition radicular arteries follow the nerve roots ventrally and dorsally and give rise to the medullary arteries which form a circumferential pial plexus indirectly connecting the anterior and posterior spinal arteries.
The anterior spinal artery is formed as a confluence of branches of the intracranial vertebral arteries and descends along the length of the cord near or in the anterior median fissure (or sulcus). Much of the blood supplied in its distribution is from the anastomotic circumferential plexus, particularly caudal to the fourth cervical segment. The anterior spinal artery gives rise to a central (or sulcal) artery at variable levels and those central arteries pass to the left or the right alternately within the cord. These supply much of the anterior 2/3 of the cord including the anterior horns and the commissure (intermediate gray matter). The peripheral white matter is referred to as the anterior, lateral and posterior funiculi. Pial branches of the circumferential pial plexus contribute substantially to the blood supply of the peripheral white matter of the cord, especially laterally and posteriorly.
The paired posterior spinal arteries originate either as branches of the vertebral arteries or the posterior inferior cerebellar arteries along the dorsal aspect of the caudal brainstem. The posterior spinal arteries descend along the cord in the posterolateral sulci. These dual vessels are variable in size and form frequent anastomoses with the medullary arteries via the pial plexus. The posterior spinal arteries supply the posterior one third of the cord, particularly the posterior horns of gray matter, providing collateral circulation to the dorsal and lateral funiculi and the intermediate gray matter3.
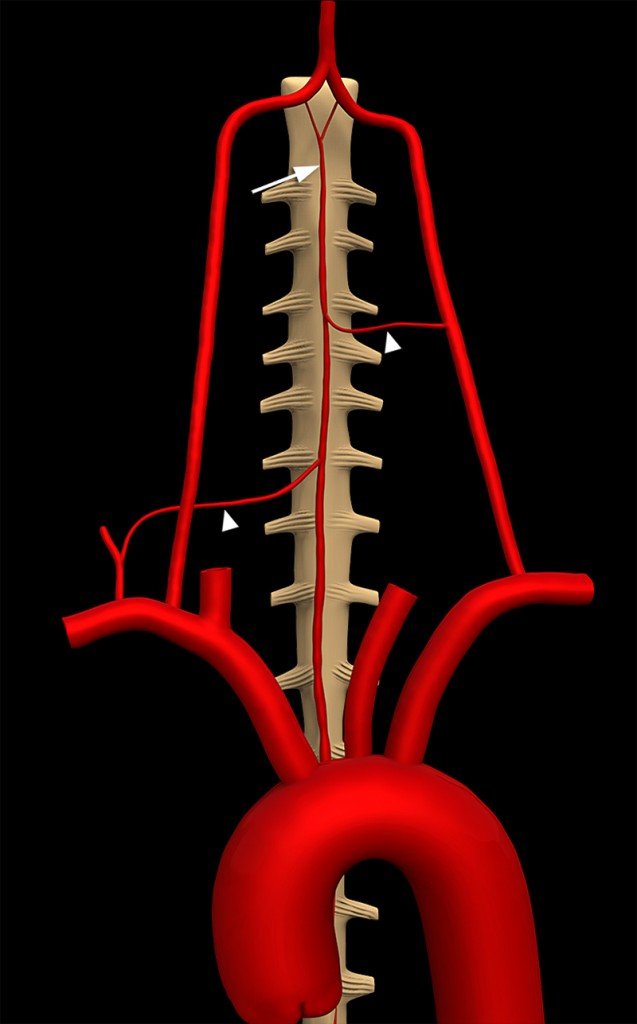
Figure 3:
The anterior spinal artery (arrow) forms as a confluence of branches from the intracranial vertebral arteries and descends on the ventral surface of the spinal cord in the anterior median sulcus. A variable number of radicular arteries (arrowheads) contribute to arterial supply entering the spinal canal through the neural foramina.
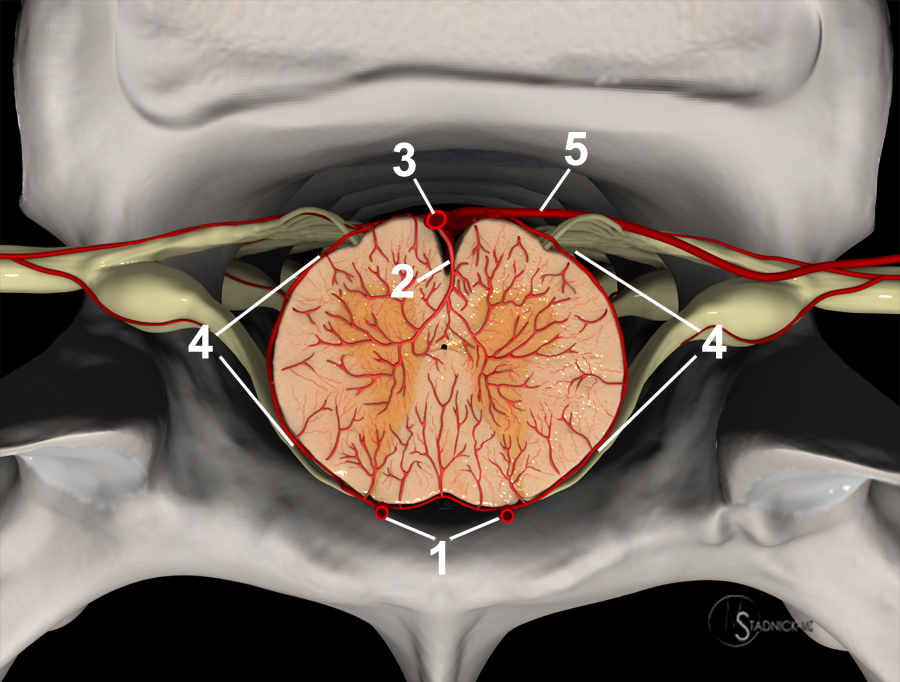
Figure 5:
Cross sectional view of the spinal cord demonstrates arterial supply from paired posterior spinal arteries (1) supplying a small portion of the gray matter, the central sulcal artery (2) arising from the anterior spinal artery (3) and supplying the majority of the gray matter, and the circumferential pial plexus (4). At some levels a radicular artery contributes (5).
Differential diagnosis of the Owl’s Eye Sign
Cord infarction
There are two major types of spinal cord infarction. The first is related to sudden interruption of blood flow through one of the major feeding arteries such as a radicular, anterior spinal or posterior spinal artery. The second is caused by hypoperfusion. Since gray matter has a higher metabolic rate than white matter it is more prone to injury from hypoperfusion. Risks include embolism related to atherosclerosis, discal fibrocartilaginous embolism, aortic or vertebral artery dissection, spinal or aortic surgery, vasculitis, cocaine abuse, acute trauma including acute disc herniation, vasospasm related to transforaminal pain management (Figure 6) and systemic hypotension. Spinal cord infarction represents only about 1% of central nervous system strokes. Unlike brain infarctions, most spinal cord infarctions are accompanied by acute pain. Only about 40% of spinal cord infarctions demonstrate bilaterally symmetric injury to the cord in the expected distribution of the anterior spinal artery. Infarctions may be unilateral anterior or unilateral posterior, affecting the patient’s clinical presentation in many ways. The development of signs and symptoms occurs over minutes to hours and motor signs tend to predominate456789. Given the extensive collateral vessels that are present, the rarity of a spinal cord infarction as well as the rarity of the Owl’s Eyes appearance as a sign of infarction is easily understood.
Figure 6:
(6a) A 53 year-old female presented with acute pain, numbness, and weakness following a transforaminal epidural steroid injection one week earlier. Abnormal T2-hyperintensity is seen within the cord at C6-7 (arrow), compatible with a spinal cord infarct. (6b) A corresponding T2-weighted axial image reveals that the region of cord edema is unilateral on the right (arrow). Presumably this infarct occurred secondary to injury and/or vasospasm involving the right sided radicular artery. (6c) A follow up study performed 1.5 years later reveals well defined residual gliosis (arrow) at the site of the previous infarct. This case illustrates that spinal cord infarcts may not result in the Owl’s Eyes Sign when due to unilateral injury of a radicular artery.
Epidural cord compression
Acute cord compression from a disc herniation, epidural hematoma, abscess or displaced bone fragment from a spinal fracture may injure the cord from contusion, venous ischemia or arterial injury. Chronic cord compression as might be seen with degenerative spinal stenosis can cause chronic hypoperfusion subsequently leading to gliosis clinically presenting as a slowly developing compressive myelopathy (Figures 7-10). The etiology of findings in our initial test case was presumably attributable to hypoperfusion occurring as the result of a now contracted bulging or herniated disc compressing the cord in the setting of a developmentally small spinal canal.
Figure 7:
A T2-weighted sagittal image from a 60 year-old male with a history of spinal stenosis and spinal decompression reveals abnormal central T2-hyperintensity within the cord (arrowheads) at C3 and C4, where canal stenosis was previously present. Spinal stenosis is now present at C4-5 (arrow), though the cord maintains normal signal at this level.
Inflammation and infection
Infection or inflammation of the anterior horns of the gray matter of the cord due to viral myelitis in the acute phase will exhibit edema and swelling whereas later gliosis develops as illustrated in Figure 11. Such a pattern is most closely associated with poliomyelitis10 or enterovirus infections1112
Figure 11:
(11a) A T2*-weighted gradient-echo axial image from the mid cervical spine in a 72 year old man with a remote history of polio. Small symmetrical foci of gliosis are demonstrated in the anterior horns of the gray matter of the cord (arrowheads). (11b) A corresponding midline T2-weighted sagittal image in the same patient illustrates extensive but subtle gliosis in the anterior aspect of the cord (arrowheads).
It should be noted, however, that the Owl’s Eye pattern of intramedullary inflammation/demyelination has also been described in transverse myelitis which may be primarily related to infection or vaccination, or secondary due to vasculitis13. (Figure 12)
Figure 12:
(12a) A T2-weighted axial image at the mid cervical level demonstrating a classic "Owl's Eyes Sign" of gliosis in the anterior horns. This is a 14 year-old female with persistent left arm paralysis following an event clinically regarded as transverse myelitis. (12b) A T2-weighted sagittal image in the same patient months after the inciting event, demonstrating a lengthy region of involvement (arrowheads).
The lengthy involvement of the cord and the Owl’s Eyes Sign can also be found in neuromyelitis optica (NMO), a rare demyelinating condition defined as simultaneous or concurrent optic neuritis and transverse myelitis. It tends to involve the anterior aspect of the cord over multiple segments. When lesions occur in the brain they are found in areas which are not typical for multiple sclerosis including the diencephalon.
Another potential cause of the Owl’s Eye Sign is Hopkins Syndrome, a rare poorly understood neurologic disorder manifested as a polio-like illness with flaccid paralysis during an acute exacerbation of asthma. Signal disturbance in the anterior horns similar to polio have been described14 although an infectious etiology has not been established in this disorder.
Conclusion
Although the Owl’s Eyes Sign can be a striking intramedullary finding on MR, initially thought indicative of occlusion of the anterior spinal arteries, it is a non-specific imaging sign and can result from a variety of pathologies including cord infarction, cord contusion, compressive myelopathy, and various infectious or inflammatory conditions. MR is the most sensitive imaging technique for these cord lesions, and often provides information that suggests the underlying etiology.
References
- Mawad ME, et al, Spinal Cord Ischemia After Resection of Thoracoabdominal Aortic Aneurysms. AJNR Am J Neuroradiol. 1990;11: 987-991. ↩
- Kulkarni M, et al. Acute Spinal Cord Injury: MR Imaging at 1.5T Radiology. 1987; 164:837-843. ↩
- Clark R. Anatomy of the Mammalian Cord. Chapter 1 in Volumes 2 and 3 of “Handbook of the Spinal Cord.” Robert Davidoff, ed. Marcel Dekker, Inc. 1987. ↩
- Duprez T, et al. Fibrocartilaginous Embolization to the Spinal Cord: Serial MR Imaging Monitoring and pathologic Study. AJNR Am J Neuroradiol 2005; 26:496-501. ↩
- Ludwig MA and Burns SP. Spinal Cord Infarction Following Cervical Transforaminal Epidural Injection: A Case Report. Spine. 2005; 30(10): E266-E268. ↩
- Novy J, et al. Spinal Cord Ischemia: Clinical and Imaging Patterns, Pathogenesis and Outcomes in 27 Patients. Arch Neurol. 2006; 63:1113-1120. ↩
- Suzuki K, et al. Anterior Spinal Artery Syndrome Associated with Severe Stenosis of the Vertebral Artery. Am J Neuroradiol 1998; 19: 1353-1355. ↩
- Weidauer S, et al. Spinal Cord Infarction: MR Imaging and Clinical features in 16 Patients. Neuroradiology 2002; 44: (10) 851-857. ↩
- Yuh WTC, et al. MR Imaging of Spinal Cord and Vertebral Body Infarction AJNR Am J Neuroradiol 1992;13:145-154. ↩
- Malzberg MS, et al. Poliomyelitis: Hyperintensity of the Anterior Horn Cells on MR Images of the Spinal Cord. AJR Am J Roentgenol. 1993;161(4): 863-865. ↩
- Chen CY, et al. Acute Flaccid Paralysis in Infants and Young Children with Enterovirus 71 Infection: MR Imaging Findings and Clinical Correlates. AJNR Am J Neuroradiol. 2001; 22:200-205. ↩
- Maloney JA, et al. MR Findings in Children with Acute Flaccid Paralysis and Cranial Nerve Dysfunction Occurring During the 2014 Enterovirus D68 Outbreak. AJNR Am J Neuroradiol. 2015; Published Online Before Print November 20, 2014 as 10.3174/ajnr.A4188. ↩
- Thomas T and Branson HM. Childhood Transverse Myelitis and its Mimics. Neuroimag Clin NA 2013; 23:267-278. ↩
- Arita J, et al. Hopkins Syndrome: T2-Weighted High Intensity of Anterior Horn on Spinal Imaging. Pediatr Neurol. 1995; 13(3): 263-265. ↩