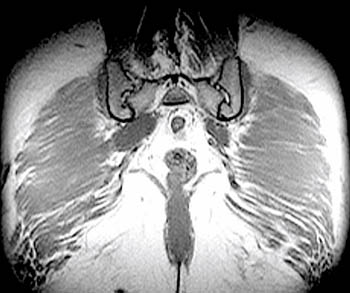
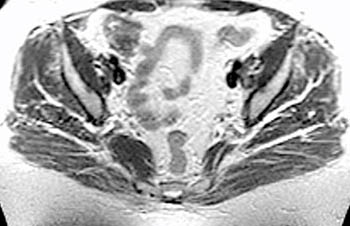
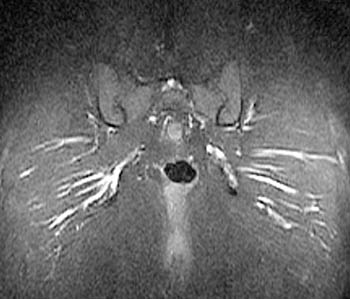
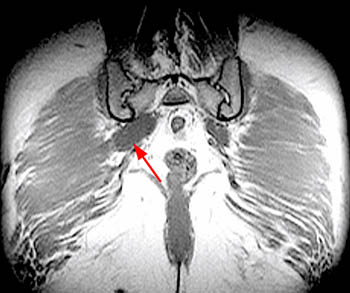
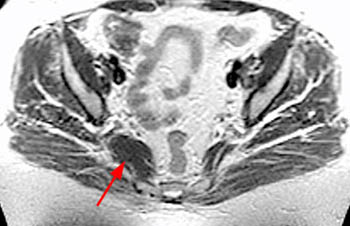
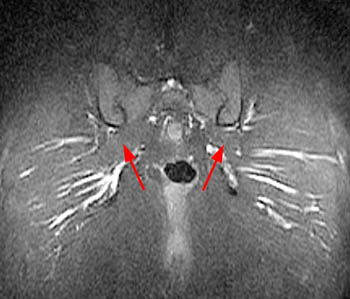
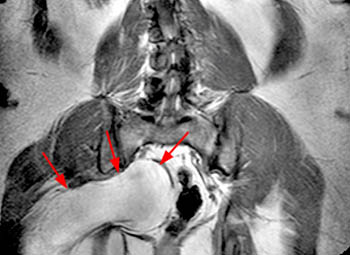
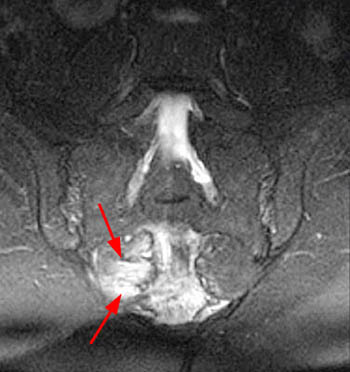
Clinical History: A 48 year-old female presents with chronic right hip and pelvic pain. Coronal T1-weighed (1a), axial T2-weighted (1b) and coronal inversion recovery (1c) images are provided. What are the findings? What is the diagnosis?
Findings
Diagnosis
Piriformis syndrome.
Introduction
Piriformis syndrome is an uncommon cause of buttock and hip pain due to entrapment of the sciatic nerve by the piriformis muscle at the greater sciatic notch. Entrapment of the sciatic nerve by the piriformis muscle was first described in 1928 by Yeoman1. In 1937 Freiberg described such entrapment in great detail, specifying that it can be distinguished from other causes of radicular pain such as disc herniation, extrinsic pressure by tumor or other mass, or intrinsic nerve abnormality2. He also described two tests that recreate the patients pain referable to the piriformis muscle, felt to be diagnostic of entrapment: Lasegue’s sign (pain at sciatic notch with extension of the knee while the hip is flexed to 90 degrees, and tenderness to palpation at the sciatic notch) and Freiberg’s sign (pain with passive internal rotation of the hip). Pace’s sign has also been described (pain and weakness in association with resisted abduction and external rotation of the affected thigh3.
Robinson4 first introduced the term piriformis syndrome in 1947, and enumerated six classic diagnostic findings:
- History of trauma to the sacroiliac and gluteal areas.
- Pain at the sacroiliac joint, greater sciatic notch, and piriformis muscle that radiates down the limb and causes difficulty walking.
- Acute exacerbation of pain by stooping or lifting and moderate relief of pain by traction in a supine position.
- Palpable sausage-shaped tender mass over the piriformis muscle on the painful side.
- Positive Lasegue’s sign.
- Gluteal atrophy, depending upon duration of the affliction.
Despite considerable attention given to piriformis syndrome, it remains a controversial clinical syndrome, in part a diagnosis of exclusion, often an elusive and delayed diagnosis, and its very existence has been called into question5. With its exquisite depiction of soft tissues, MRI aids in the diagnosis of piriformis syndrome by demonstrating normal and abnormal anatomy of the piriformis muscle and sciatic nerve, and helping to exclude other possible causes of external sciatic nerve entrapment at the level of the greater sciatic foramen.
Etiologic factors
Once intraspinal causes of sciatic nerve symptoms have been excluded, many causes of piriformis syndrome may be detected. To clarify, Papadopoulos suggested further classification of piriformis syndrome: primary piriformis syndrome, due to intrinsic pathology of the muscle itself, such as myofascial pain, anatomic variations, and myositis ossificans; secondary piriformis syndrome (pelvic outlet syndrome) – which includes all other etiologies of piriformis syndrome excluding lumbar spinal pathology6. Posttraumatic piriformis syndrome is believed to be due to blunt trauma to the buttock with resultant hematoma formation and scarring between the sciatic nerve and the piriformis muscle7. Inflammation and swelling of the traumatized muscle is posited to cause the nerve to be compressed between the muscle and the osseous pelvis4. Others suggest that an anomalous course of the sciatic nerve through the piriformis muscle may predispose the nerve to injury8,9. However, recent anatomic studies suggest that anatomic variants may not be as important in the pathogenesis of piriformis syndrome as previously suggested10. Post traumatic irritability of the piriformis muscle resulting in a trigger-point syndrome has also been proposed3. Other primary causes of piriformis syndrome due to muscle pathology have been described in case reports of myositis ossificans11 and abscess12 of the piriformis muscle. Hughes et al. have described cases of piriformis syndrome due to a bifid piriformis muscle, a fibrous band on the undersurface of the muscle compressing the nerve, and a traumatic venous aneurysm of a persistent sciatic artery and vena comitantes 9. Pseudoaneurysm of the inferior gluteal artery has also been described6. Finally, an anomalous attachment of accessory fibers of a piriformis muscle has been reported as a cause of piriformis syndrome, diagnosed by MRI and successfully treated operatively13.
Anatomic considerations
The piriformis muscle acts as a lateral rotator of the hip joint and also helps abduct the hip in flexion. It is innervated by L5, S1 and S2. The piriformis muscle arises along the anterior border of the sacrum at the level of the S2 through S4 segments, from the capsule of the sacroiliac joint, from the anterior sacrospinous ligament and from the pelvic portion of the sacrotuberous ligament. It then runs laterally, passing through the greater sciatic foramen, with its distal tendinous insertion onto the greater trochanter of the femur. The sciatic nerve passes though the sciatic foramen along with the piriformis muscle. Also coursing through the foramen and emerging along the inferior border of the piriformis muscle are the inferior gluteal nerve and artery, the posterior cutaneous nerve of the thigh, and the pudendal nerve. The superior gluteal nerve and artery exit the pelvis through the greater sciatic foramen and course above the superior border of the piriformis muscle (Figure 5a). Therefore, although piriformis muscle syndrome primarily involves the sciatic nerve, and is so defined, Papadopoulos notes that the superior and inferior gluteal nerves, pudendal nerve and posterior cutaneous nerve of the thigh may also be involved, and describes a patient with pain and neurologic deficit involving all of these nerves as well as the sciatic nerve6. Given the primary involvement of the sciatic nerve in piriformis syndrome, Beaton performed anatomic investigation upon 216 specimens, and determined the possible anatomic variations in the relation of the sciatic nerve to the piriformis muscle14. In the vast majority (90%) the nerve exits the greater sciatic foramen below the muscle. But in 7.1% the nerve demonstrated anterior and posterior divisions which passed through a divided piriformis muscle. In 2.1% the divided nerve passed above and below an undivided muscle, and in .8% an undivided nerve passed though the 2 heads of a divided muscle. The nerve can also pass undivided along the anterior superior surface of the muscle.
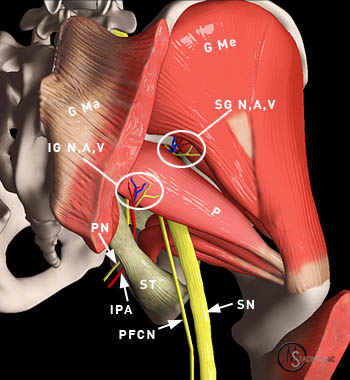
Figure 5:
This 3-D rendering depicts the structures passing through the sciatic foramen, which includes the piriformis muscle (P), the sciatic nerve (SN), the superior gluteal nerve, artery, and vein (SG NAV), the inferior gluteal nerve, artery, and vein (IG NAV), the pudenal nerve (PN), the internal pudendal artery, and the posterior femoral cutaneous nerve (PFCN). The sciatic nerve most commonly exits the sciatic foramen below the inferior margin of the piriformis as depicted. The gluteus medius (G Me) and the partially resected gluteus maximus (G Ma) muscles and the sacrotuberous ligament (ST) are also indicated.
Imaging
Given the multiple etiologies of piriformis syndrome, the findings on imaging studies are variable. The most common finding on MRI or CT is asymmetry of the piriformis muscle, most often hypertrophy, but sometimes atrophy of the muscle on the affected side15,9. Abnormal increased radiotracer uptake by the piriformis muscle on the affected side has been reported on bone scan16. In the case of myositis ossificans, x-ray, bone scan and MRI will all have diagnostic value11. In the case of anatomic variation such as an accessory head of the piriformis muscle, the superior soft tissue detail of MRI will be most useful for diagnosis. Since the symptoms of piriformis syndrome and lumbosacral disc herniation are often difficult to distinguish, and intraspinal etiologies are, after all, far more common, many patients undergo lumbar spine MRI first. Once causes of radicular symptoms have been excluded by MRI or CT myelogram, an MRI of the pelvis is useful in cases where physical exam is suggestive of piriformis syndrome, since asymmetry of the muscles, if found, is highly suggestive of the diagnosis. MRI may also uncover other causes of piriformis syndrome.
Figure 6a demonstrates a large lipoma creating a space occupying lesion in the region of the greater sciatic notch and piriformis muscle. In this case the mass was seen in a scout film of a lumbar spine MRI obtained for a patient with a 2 year history of right sided hip pain. In another patient, an MRI of the pelvis obtained to exclude piriformis syndrome demonstrated edema of both the piriformis muscles, right greater than left, in a patient with right sided symptoms (Fig 7a). In this case the patient also had a history of previous colorectal tumor resection, and on the basis of the subtle signal abnormality on MRI, a diagnosis of recurrent tumor was suggested and subsequently confirmed clinically.
Treatment
Conservative measures such as NSAIDs, physical therapy focusing on stretching the piriformis muscle, and steroid injections are commonly used in the treatment of piriformis syndrome. Recently, injection of botulinum toxin has also been reported as a treatment17. In recalcitrant cases, several studies report disappearance of symptoms following operative release of the piriformis muscle2,7,9. In cases where imaging clearly demonstrates a resectable cause of nerve entrapment or muscle compromise such as tumor, vascular anomaly, myositis ossificans, anomalous piriformis muscle, or pyomyositis, resection has been curative6,9,11,12,13.
Conclusion
Piriformis syndrome remains a controversial topic, and though rare, is an important diagnosis to keep in mind for the patient with chronic buttock and hip pain. Since the pain is often similar to and difficult to distinguish from sciatica due to the more common intraspinal nerve root compression, MRI of the lumbar spine is often performed first. If lumbar spine MRI findings are normal or equivocal, it is important to consider the diagnosis of piriformis syndrome, especially if there has been a history of localized trauma and the patient demonstrates positive findings on physical exam. In such cases, MRI of the pelvis is useful in demonstrating the abnormal appearance of the piriformis muscle, or extrinsic abnormalities such as a mass or vascular anomaly.
References
1 Yeoman, W.: The Relation of Arthritis of the Sacro-Iliac Joint to Sciatica, with an Analysis of 100 cases. Lancet, 2: 1119-1122, 1928.
2 Freiberg, A.H.: Sciatic Pain and its Relief by Operations on Muscle and Fascia. Arch. Surg., 34: 337-350, 1937.
3 Pace, J. B., and Nagle, D.: Piriformis Syndrome. Western J. Med., 124: 435-439, 1976.
4 Robinson, D. R.: Piriformis Syndrome in Relation to Sciatic Pain. Am. J. Surg., 73: 355-358, 1947.
5 Halpin, RJ, Ganju, A: Piriformis Syndrome: A Real Pain in the Buttock? Neurosurgery 2009 Oct; 65 (4Suppl): S197-202.
6 Papadopoulos SM, McGillicuddy JE, Albers JW. Unusual cause of Piriformis Muscle Syndrome’. Arch Neurol. Oct 1990; 47(10):1144-6.
7 Benson, ER, Schutzer SF: Posttraumatic Piriformis Syndrome: Diagnosis and Results of Operative Treatment. The Journal of Bone and Joint Surgery 81:941-9 (1999).
8 Pecina, M.: Contributions to the Etiological Explanation of the Piriformis Syndrome. Acta Anat., 105: 181-187, 1979.
9 Hughes, S. S.; Goldstein, M. N.; Hicks, D. G.; and Pellegrini, V. D., Jr.: Extrapelvic Compression of the Sciatic nerve. An Unusual Cause of Pain About the Hip: Report of Five Cases. J. Bone and Joint Surg., 74-A: 1553-1559, Dec. 1992.
10 Smoll, NR: Variations of the Piriformis and Sciatic Nerve with Clinical Consequence: a Review. Clin Anat 2010 Jan; 23 (1): 8-17.
11Beauchesne RP, Schutzer SF. Myositis Ossificans of the Piriformis Muscle: an Unusual Cause of Piriformis Syndrome-a Case Report. J Bone Joint Surg Am1997; 79:906-910.
12 Chen, W.-S.: Sciatica due to Piriformis Pyomyositis: Report of a Case. J. Bone and Joint Surg., 74-A: 1546-1548, Dec. 1992.
13 Lee, EY, Margherita, AJ, Dierade, DS, Narra VR: MRI of Piriformis Syndrome. AJR 2004; 183:63-64.
14 Beaton, L.E., and Anson, B. J.: The Sciatic Nerve and the Piriformis Muscle: their interrelation a possible cause of coccygodynia. J Bone and Joint Surg., 20: 686-688, July 1938Benzon HT, Katz JA, Benzon HA, Iqbal MS. Piriformis Syndrome: Anatomic Considerations, a New Injection Technique, and a Review of the Literature. Anesthesiology.2003; 98:1442-1448.
15 Jankiewicz JJ, Hennrikus WL, Houkom JA. The Appearance of the Piriformis Muscle Syndrome in Computed Tomography and Magnetic Resonance Imaging: a case report and review of the literature. Clin Orthop 1991;262:205-209.
16 Karl, R. D., Jr.; Yedinak, M. A.; Hartshorne, M. F.; Cawthon, M. A.; Bauman, J. M.; Howard, W. H.; and Bunker, S. R.: Scintigraphic Appearance of the Piriformis Muscle Syndrome. Clin. Nucl. Med., 10: 361-363, 1985.
17 Lang, AM: Botulinum Toxin Type B in Piriformis Syndrome. Am J Phys Med Rehabil. 2004 Mar; 83 (3): 198-202.