Clinical History:
A 19 year-old male presents with distal femur pain from a running injury 1 week ago. What are the findings? What is your diagnosis?
Findings:
Figure 2:
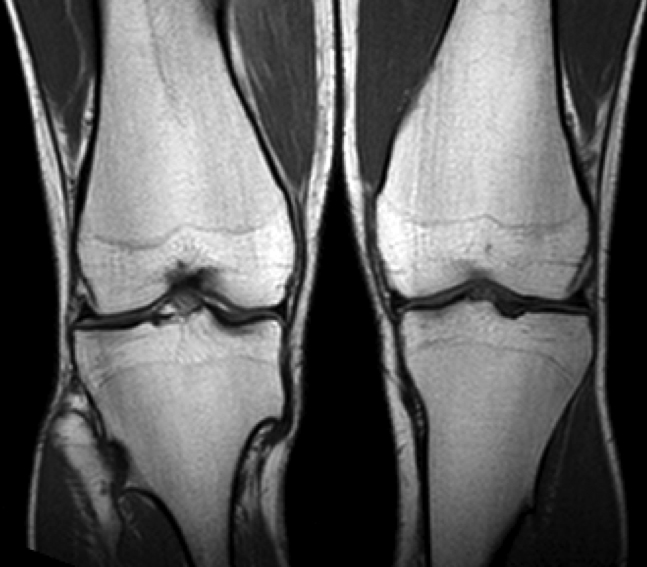
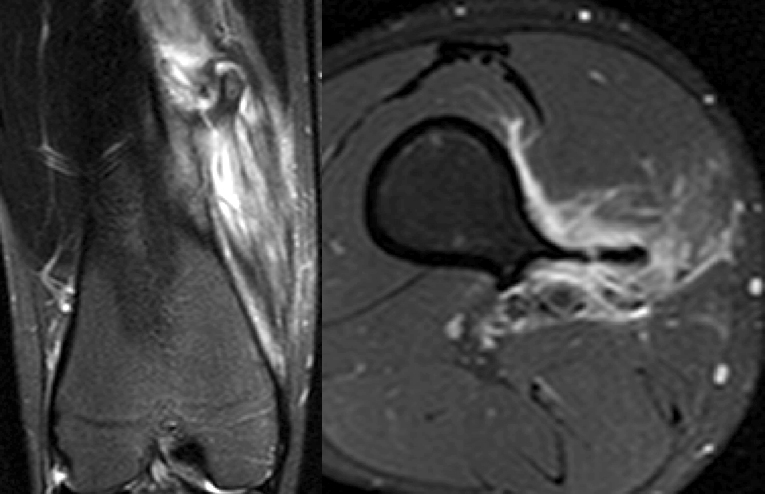
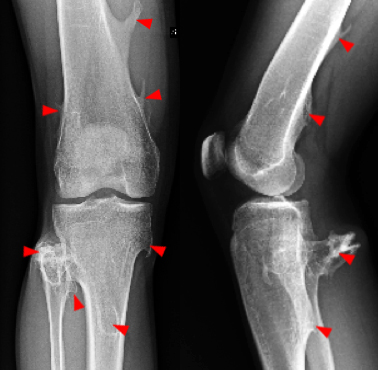
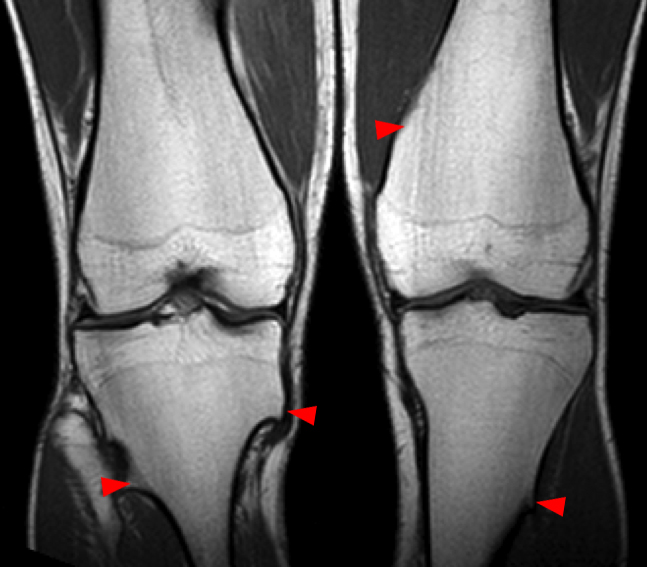
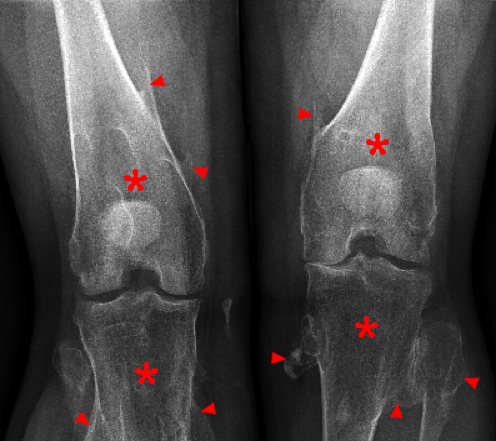
(2a) The AP and lateral radiographs of the knee demonstrate widening of the metaphyses with multiple osteochondromas (arrowheads). (2b) The T1-weighted coronal images demonstrate bilateral osteochondromas (arrowheads). (2c) The STIR coronal (left) and proton density-weighted fat-suppressed axial (right) images reveal a fracture (arrows) at the base of a pedunculated osteochondroma of the femur with adjacent soft tissue edema. The fracture is not visible on the plain films.
Diagnosis
Hereditary multiple exostoses (HME) with fracture.
Introduction
Hereditary multiple exostoses (HME) is an autosomal dominant disorder in which multiple exostoses, or osteochondromas, form. The lesions are caused by separation of a cartilage fragment from the epiphyseal growth plate which herniates through the periosteum surrounding the growth plate. The fragment grows and undergoes enchondral ossification resulting in a subperiosteal bony protuberance with a cartilage cap.1 The disorder was first described in 1786 and a familial occurrence was first recorded in 1814.1,2 Around 60 to 70% of patients have a positive family history.2 HME has also been seen in other animals, including horses, cats, dogs and lizards.2
Most patients are diagnosed between the ages of 5 and 12 and some can be diagnosed at birth.1 Osteochondromas continue to grow until the child reaches skeletal maturity at which point no new lesions will occur.2 Spontaneous regression has been reported in childhood and puberty, particularly following a fracture.1,2,3
Complications and Imaging
Osteochondromas, whether single or multiple, are typically asymptomatic unless complications occur. Most complications are common to both HME and solitary exostoses but are more common in HME, primarily because of the increased number of lesions. Growth retardation and metaphyseal widening, caused by disruption of normal bone tubulation by the lesions, are specific to HME.
HME may result in deformity and remodeling of adjacent bony structures. Neural impingement may result in pain. The spinal cord can be compressed by vertebral or rib exostoses. Muscle weakness and atrophy are additional possible sequelae of nerve impingement.3 Vascular complications include displacement, stenosis, occlusion and pseudoaneurysm formation.1
Figure 4:
Coronal proton density-weighted fat-suppressed (top left) and axial T1-wieghted (top right) images with corresponding CT images (bottom) demonstrate a sessile osteochondroma (asterisks) arising from the lateral distal tibial diaphysis causing marked thinning and remodeling of the fibula (arrowheads).
Formation of an overlying adventitial bursa can occur which may present as an enlarging mass.1 The bursa may be complicated by inflammation, infection, hemorrhage, chondral bodies and synovial chondromatosis.1 The cartilage cap can be prominent in a child and shows high signal intensity on fluid sensitive sequences and differentiation from a bursa can be difficult.
Figure 5:
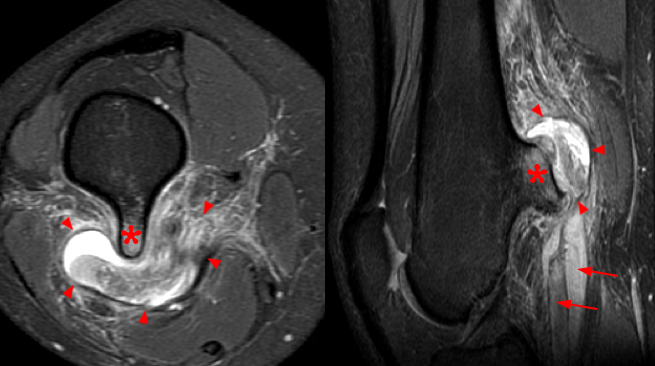
A 25 year-old woman presented with a painful mass. Axial (left) and sagittal (right) proton density-weighted fat-suppressed images show a large osteochondroma (asterisks) projecting from the posterior femur. A large complex adventitial bursa (arrowheads) has formed with adjacent soft tissue inflammation and displacement of the popliteal vessels (arrows).
Figure 7:
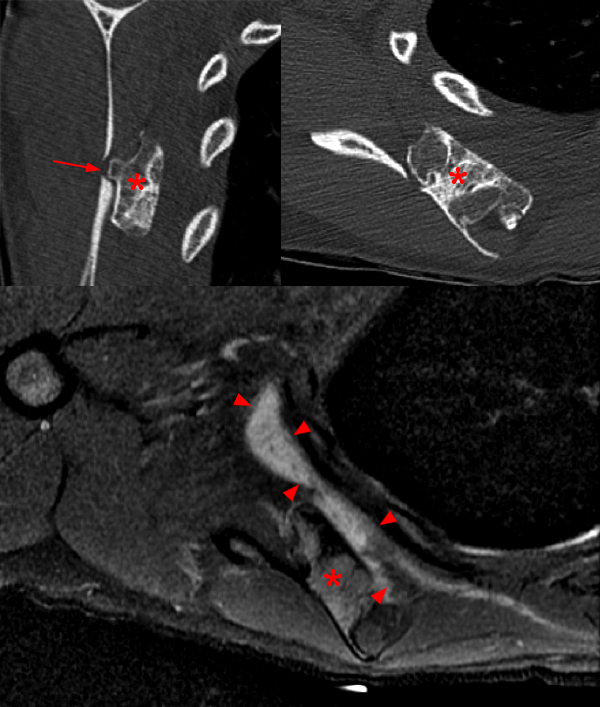
20 year-old female with a shoulder mass. Sagittal (top left) and axial (top right) CT images show a large osteochondroma (asterisks) projecting anteriorly from the scapula. A portion of the osteochondroma has grown posteriorly and has eroded the adjacent scapular body (arrow). An axial proton density-weighted fat-suppressed image (bottom) shows a large adventitial bursa (arrowheads) between the exostosis (asterisk) and ribs. When the fluid collection is this large there is no difficulty distinguishing it from the cartilage cap.
Fractures can result from direct trauma and typically occur at the base of a pedunculated osteochondroma.1 Injury to an adjacent muscle has been described and is felt to be due to repetitive motion of the muscle over the osteochondroma causing pain and swelling, similar to a muscle contusion.3
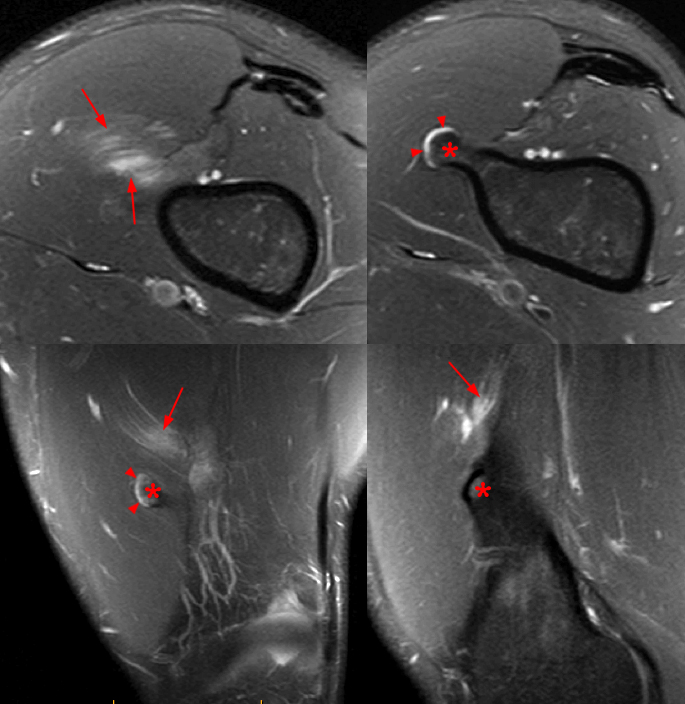
Figure 8:
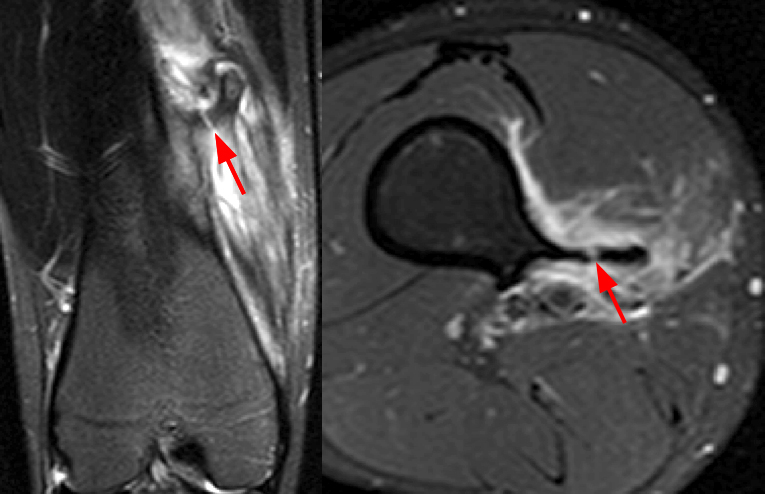
A 24 year-old male with chronic pain, aggravated by a recent injury. Fat-suppressed proton density-weighted axial (top left and right), coronal (bottom left) and sagittal (bottom right) images of the distal femur show a pedunculated osteochondroma (asterisks) with a normal thin cartilage cap (arrowheads). Edema in the vastus medialis muscle (arrows) may be due to muscle impingement.
Malignant degeneration of the cartilage cap is the most serious complication of HME, seen in approximately 3-5% of patients with a mean age of onset of 31.1,2 (Malignant transformation of a solitary osteochondroma occurs in approximately 1% of patients.)3 It rarely occurs before the age of 20 or after the age of 50.1,2 The average age of occurrence in a patient with HME is 25-30 years, younger than that of a solitary osteochondroma in which the average age is 50-55 years.1 By far the most common malignancy is a chondrosarcoma. The tumors are slow growing and metastases (commonly to the lungs) are unusual and occur late.1,2,4 Complete surgical resection is required. Radiation and chemotherapy are not helpful.1,2,4
Radiographic findings suggestive of malignant transformation include growth in a skeletally mature patient, irregularity or indistinctness of the surface, focal areas of radiolucency within the lesion, destruction of adjacent bone, irregular scattered calcifications and a soft tissue mass.1,2 Cartilage cap thickness is used as a primary criterion on MRI. The majority of benign osteochondromas have a cartilage cap less than 1 cm thick and the majority of malignant cases have a cap thickness of greater than 2 cm. A cartilage cap measuring greater than 1.5 cm should be highly suspected of malignant transformation.2 A positive bone scan cannot differentiate between benign and malignant lesions, although a negative scan typically excludes malignant transformation.1,2
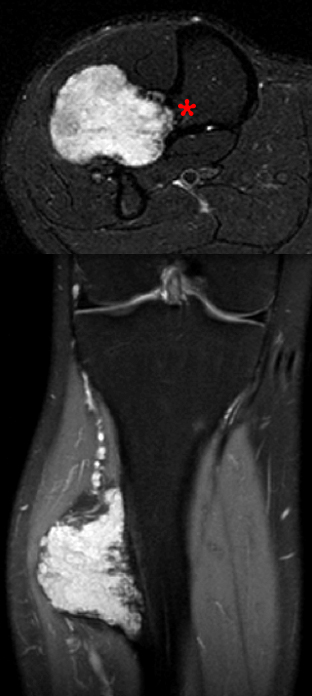
Figure 10:
A 37 year-old male with a palpable mass. STIR axial (top) and proton density-weighted fat-suppressed coronal (bottom) images reveal a large juxtacortical mass with chondroid matrix. The axial image shows continuity of the cortex and medullary space at the base of the mass (asterisk), giving the diagnosis of chondrosarcoma due to malignant degeneration of the cartilage cap of an osteochondroma. The cartilage cap measures 4 cm.
Conclusion
Hereditary multiple exostoses is not a difficult imaging diagnosis to make. The entity is typically asymptomatic unless complications occur. The purpose of imaging is to diagnose and define those complications, including inflammation and impingement of adjacent structures. The ability of MRI to evaluate the thickness of the cartilage cap and other associated findings is critical in detection of the most serious complication, malignant degeneration.
References
- Murphey MD, Choi JJ, Kransdorf MJ, Flemming DJ, Gannon FH. Imaging of osteochondroma: variants and complications with radiologic-pathologic correlation. Radiographics 2000; 20(5). ↩
- Hennekam RCM. Hereditary multiple exostoses. J Med Genet 1991; 28:262-266. ↩
- Uri DS, Dalinka MK, Kneeland JB. Muscle impingement: MR imaging of a painful complication of osteochondromas. Skeletal Radiology 1996; 25:689-692. ↩
- Solomon L. Hereditary multiple exostoses. JBJS (BR); May 1, 1963. ↩