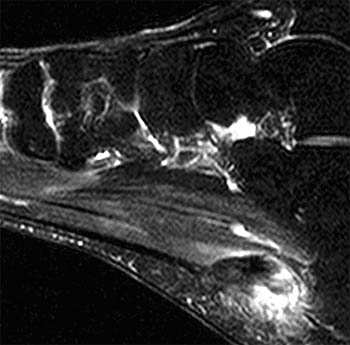
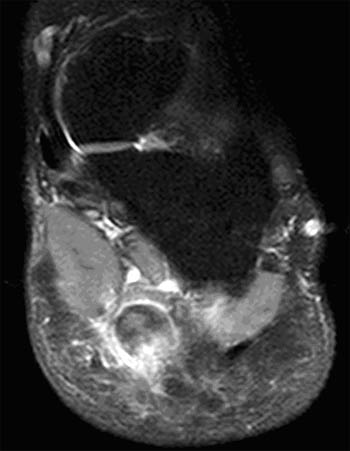
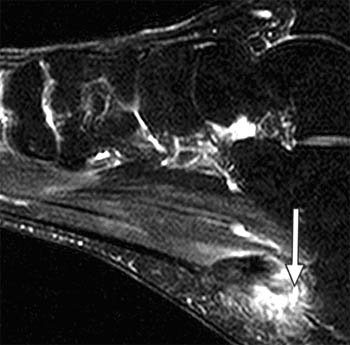
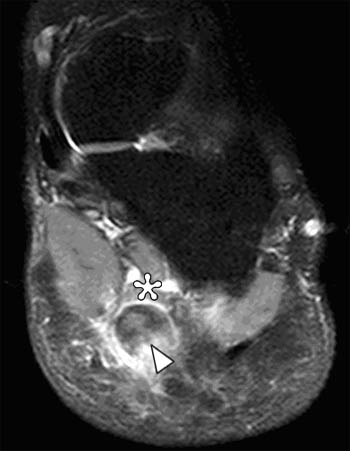
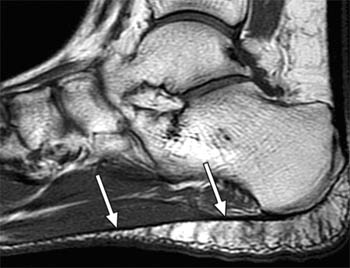
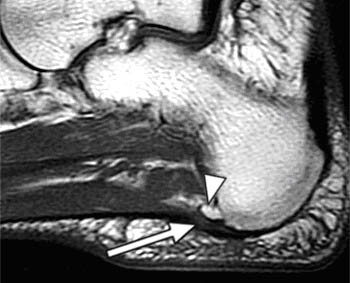
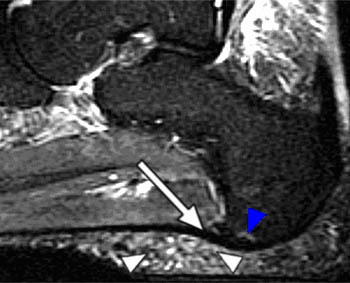
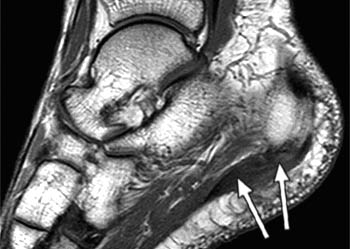
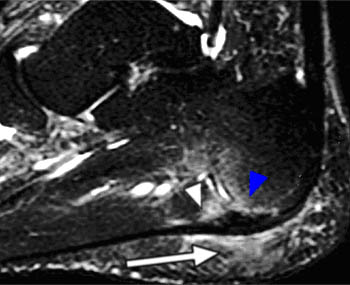
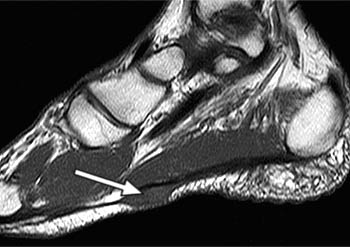
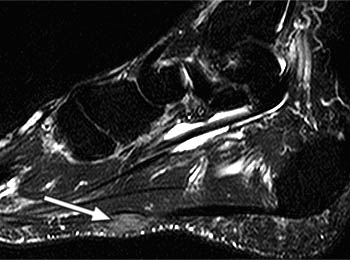
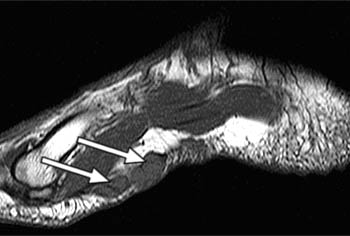
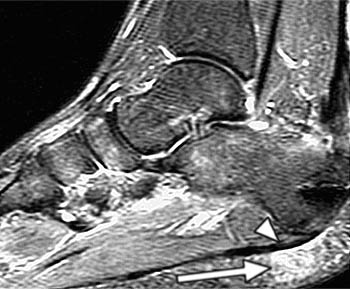
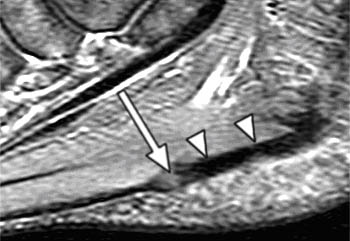
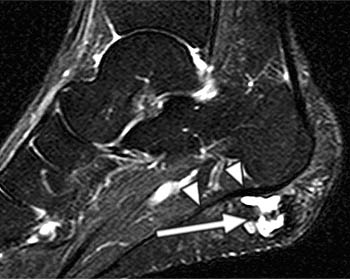
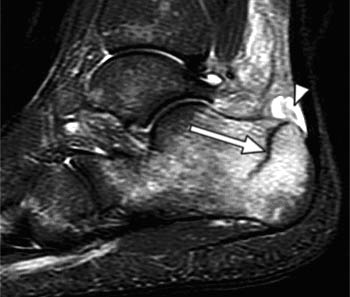
Clinical History: A 47 year-old male presents with a history of acute onset of heel pain while running, with an audible pop. Sagittal (1a) T1-weighted and (1b) fat-suppressed T2-weighted and (1c) coronal fat-suppressed proton density weighted images are provided. What are the findings? What is the diagnosis?
Findings
Diagnosis
Severe plantar fasciitis with acute rupture of the plantar fascia at the calcaneal attachment.
Discussion
Acute rupture of the plantar fascia is relatively rare, even given the widespread incidence of chronic plantar fasciitis. Acute rupture of the plantar fascia is most commonly seen in athletes during an acceleration type injury causing forced plantar flexion, or with jumping.1 Pre-existing plantar fasciitis is commonly present in cases of traumatic rupture, and the thickening of the plantar fascia anterior to the rupture in our case suggests chronic plantar fasciitis. Patients with chronic planter fasciitis treated with serial corticosteroid injections may be at greater risk for rupture.2
Plantar fasciitis is a low grade inflammatory process where repetitive microtrauma induces microtears which elicit an inflammatory reaction. This stress-related type of plantar fasciitis can be seen in athletes, obese patients, or patients with chronic standing or walking work-related activity. Plantar fasciitis can also be seen as an enthesopathy in association with seronegative spondyloarthropathies such as ankylosing spondylitis, Reiter?s syndrome, and psoriatic arthritis.3
The plantar fascia is a fibrous aponeurosis arising from the medial calcaneal tuberosity, and plays a significant role in longitudinal arch support. Distal to the calcaneus, it continues anteriorly, dividing into central, medial and lateral components. The large central component adheres to the underlying flexor digitorum brevis muscle, and divides at the level of the mid sole into five bands at the mid-metatarsal level. These divide into deep and superficial components and course distally toward the toes, along with the medial and lateral marginal superficial tracts, with insertions onto each of the five proximal phalanges.3,4 Coronal images clearly reveal the central portion overlying the flexor digitorum brevis muscle, the medial portion beneath the abductor hallucis muscle, and the lateral component overlying the abductor digiti minimi muscle (5a).
Figure 5:
A proton density-weighted coronal image in a normal patient reveals the largest, central component of the plantar aponeurosis (red), plantar to the flexor digitorum brevis muscle. The medial (blue) component is found beneath the abductor hallucis muscle and the lateral (green) component is found plantar to the abductor digiti minimi muscle.
Many studies have reported the spectrum of MRI findings in plantar fasciitis. Several have reported the most common findings in order of prevalence to be as follows: 1) edema of the soft tissues plantar to the plantar fascia, 2) edema of the tissues deep to the aponeurosis, 3) edema of the aponeurosis itself, 4) marrow edema of the overlying calcaneus, and 4) thickening of the plantar fascia.5,7 Plantar calcaneal spurs may be present, but have also been observed to be present in as many as 25% of asymptomatic patients, so these may not be clinically predictive.6 It has been suggested that inflammatory changes visible on MRI begin at the calcaneal attachment and progress distally with chronicity7 (F-I). Though significantly less common than plantar fasciitis, some patients may present with acute onset of pain following trauma. Such cases of acute plantar fascial strain have imaging findings that may be identical to those seen in mild to moderate plantar fasciitis.
Other disorders of the plantar fascia include plantar fibromatosis, xanthoma, rheumatoid nodule, and clear cell sarcoma. Heel pain can also be caused by chronic weight bearing changes of the heel fat pad, tarsal tunnel syndrome, and occult fracture. In the case of tarsal tunnel syndrome, isolated heel pain is rare, since it is usually accompanied by pain elsewhere in the sole of the foot. Xanthomas are usually bilateral and symmetric, often painless, and exhibit diffuse fusiform thickening and sometimes a speckled appearance on T1 weighted images.3
Plantar fibromatosis is a benign fibrotic proliferative process analogous to Dupuytren contracture in the hand (and may occur concomitantly).8 Although it is a benign neoplasm, it is non-encapsulated, can be locally aggressive and demonstrates a high recurrence rate. For that reason it is treated with wide resection, sometimes with adjuvant radiation and/or Methotrexate therapy.8,9 Plantar fibromatosis is often painless, multifocal and bilateral, with palpable nodules, which allows clinical differentiation from plantar fasciitis. However, when lesions invade adjacent muscles or neurovascular structures, they become symptomatic. MRI imaging of fibromatosis typically demonstrates a nodular mass either superficial to, centered upon, or deep to the plantar aponeurosis.9 Masses are typically isointense to minimally hyperintense to muscle on both T1 and T2-weighted pulse sequences. They tend to be located at the mid to distal plantar fascia rather than at the medial calcaneal tuberosity, and the well defined nodular configuration is also an aid in differentiating them from plantar fasciitis (11a,12a,13a). The rare cases of clear cell sarcoma are very similar in appearance to locally invasive plantar fibromatosis; but both are treated with wide excision and a combination of adjuvant radiation and Methotrexate.9
A potentially difficult differential diagnosis is that between plantar fibroma and chronic partial tear of the plantar fascia, as in the case seen in figures 14a,15a. Scarring in cases of chronic partial tears of the plantar fascia can lead to a nodular appearance mimicking plantar fibromatosis. In this case, there was evidence of plantar fasciitis at the medial calcaneal tuberosity as well.
Figure 15:
A magnified view medial to (13a) demonstrates slightly nodular thickening of the plantar fascia, but this image suggests a partial tear (arrow) of the plantar fascia within the lesion, as well as thickening of the proximal plantar fascia (arrowheads), supporting chronic plantar fasciitis as the most likely etiology.
Subcutaneous rheumatoid nodules are seen in 20% of patients who test positive for blood rheumatoid factor, and they are commonly encountered over osseous protuberances subject to microtrauma, such as the medial calcaneal tuberosity or the olecranon.3 Centered within the heel fat pad rather than the plantar fascia, they demonstrate intermediate to high signal intensity on T2 weighted images, with variable contrast enhancement, and often contain areas of central necrosis (16a). Similar findings can also be seen in patients with rheumatic fever, ankylosing spondylitis, SLE and agammaglobulinemia.1
Figure 16:
A fat-suppressed T2-weighted sagittal image depicts a typical rheumatoid nodule within the heel fat pad (arrow), with central necrosis; no involvement of the plantar fascia (arrowheads). Rheumatoid nodules are typically heterogeneous in appearance on T1 and T2-weighted images, with the central very high signal intensity regions on T2 indicating necrosis. This patient had bilateral heel pad nodules.
Painful heel fat pad is often clinically confused with plantar fasciitis, although pain is slightly more posterior to that of plantar fasciitis. In these cases edema and fibrosis of the heel fat pad can be seen in the absence of plantar fascial changes (17a).
A not uncommon cause of persistent heel pain is the calcaneal stress fracture (18a). Patients with calcaneal stress fractures may have a similar history as patients with plantar fasciitis, as both abnormalities are related to overuse and are exacerbated by weight bearing activities. MRI is highly sensitive for calcaneal stress fractures and is able to make the definitive diagnosis in such cases.
Conclusion
MRI can clearly demonstrate plantar fascia rupture as well as varying degrees of severity and chronicity of plantar fasciitis. Because of the wide clinical differential diagnosis of heel pain, MRI is useful in distinguishing plantar fasciitis from other causes, and treatment recommendations often vary markedly based on the MR findings.
References
1 D. J. Theodorou, S. J. Theodorou, S. Farooki, Y. Kakitsubata, and D. Resnick Disorders of the Plantar Aponeurosis: A Spectrum of MR Imaging Findings Am. J. Roentgenol., January 1, 2001; 176(1): 97 – 104
2 Leach R, Jones R, Silva T. Rupture of the plantar fascia in athletes. J Bone Joint Surg Am 1978; 60:537-539.
3 J. A. Narvaez, J. Narvaez, R. Ortega, C. Aguilera, A. Sanchez, and E. Andia Painful Heel: MR Imaging Findings RadioGraphics, March 1, 2000; 20(2): 333 – 352
4 Theodorou DJ, Theodorou SJ, Kakitsubata Y, et al. Plantar fasciitis and fascial rupture: MR imaging findings in 26 patients supplemented with anatomic data in cadavers. RadioGraphics 2000; 20(special issue):S181-S197.
5 Grasel RP, Schweitzer ME, Kovalovich AM, et al. MR imaging of plantar fasciitis: edema, tears, and occult marrow abnormalities correlated with outcome. AJR Am J Roentgenol 1999; 173:699-701
6 S. Rosenberg, J. Beltran, and J. T. Bencardino MR Imaging of the Ankle and Foot. adioGraphics, October 1, 2000; 20(90001): 153S – 179
7 Berkowitz JF, Kier R, Rudicel S. Plantar fasciitis: MR imaging. Radiology 1991; 179:665-667.
8 Lee TH, Wapner KL, Hecht PJ. Plantar fibromatosis. J Bone Joint Surg Am 1993; 75:1080-1084.
9 Morrison WB, Schweitzer ME, Wapner KL, Lackman RD. Plantar fibromatosis: a benign aggressive neoplasm with a characteristic appearance on MR images. Radiology 1994; 193:841-845.