Many referring physicians find themselves juggling extensive patient loads with limited time to interpret critical diagnostic information. Meanwhile, the radiologist (MD)—trained to read imaging exams with pinpoint accuracy—often works in a silo, disconnected from the daily challenges faced by primary care teams, family medicine offices, or the emergency department. This gap can slow diagnoses, create confusion over appropriate imaging, and hinder patient care.
When communication between radiologists and referring clinicians breaks down, the care of patients suffers. Referring clinicians may receive vague or overly technical reports. Referring physicians want clarity, yet they sometimes struggle to gain direct access to radiologists, leading to missed nuances in imaging findings. In many cases, outdated radiology department workflows and cumbersome software integrations pile on extra layers of friction. Radiologists don’t always get the clinical context they need, while referring physicians may feel uncertain about the next step in patient management.
The good news is that improving communication and forging good relationships is entirely possible. In this post, we’ll explore practical strategies for improving relationships between radiologists and referring physicians:. You’ll discover how advanced technology, structured reporting, direct consultation, and a shift toward value-based care are laying the groundwork for better patient outcomes. By the end, you’ll have a clear roadmap for enhancing communication in radiology, ensuring everyone involved—patients and referring physicians alike—receives the highest quality service.
Key Takeaways
- Key Takeaway #1: Upgrading to advanced PACS solutions (like ProtonPACS) and integrating them with EHRs streamlines communication between radiologists and referring physicians, improving overall workflow efficiency.
- Key Takeaway #2: Radiologists collaborate best when they provide direct access and clear, structured radiology report formats; physicians appreciate concise findings and immediate consults for complex cases.
- Key Takeaway #3: Emphasizing value-based care by aligning radiology practice protocols with appropriateness criteria and clinical decision support can yield a significant impact on patient outcomes.
Why Strong Collaboration Matters in Radiology
The Critical Role of Communication in Patient Care
When radiology providers and referring physicians maintain open lines of dialogue, diagnostic radiology becomes a powerful tool for swift and accurate diagnoses. Better communication ensures that each imaging examination is used effectively: the right imaging modality or technique is selected according to the clinical context, and the results are conveyed in a way that referring clinicians can immediately act on. This alignment has a significant impact on the care of patients, often leading to shorter hospital stays and more targeted treatment plans.
By honing the relationship between radiologists and referring physicians, we can improve patient care at every stage. When radiologists collaborate more closely with physicians and radiologists in other specialties—such as interventional radiology or musculoskeletal radiology at Thomas Jefferson—the entire health system benefits. Referring physicians appreciate quick consults, while radiologists must remain readily available to clarify complex imaging findings. This synergy underpins a more seamless patient journey, from initial imaging exams to final treatment decisions.
Challenges in Communication Between Radiologists and Referring Physicians
- Variability in Radiology Report Clarity
Some radiologists rely on long-winded, narrative-style reporting. Although thorough, this can create ambiguity. Meanwhile, referring physicians appreciate concise, clearly structured findings that can inform immediate clinical decisions.
- Lack of Direct Access to Radiologists for Referrers
In many settings, referring physicians do not have a simple channel to reach the radiologist. This lack of access becomes a roadblock to real-time physician collaboration. Referrer frustration can escalate, especially in urgent scenarios such as emergency department admissions or critical abdominal imaging follow-ups.
- Workflow Inefficiencies Due to Outdated PACS Systems and EHR Integrations
The technology used to store and transmit imaging studies can slow or impede the exchange of information if it’s not optimized. Radiologists and referring physicians need integrated solutions that allow for rapid data sharing and immediate feedback loops—a factor crucial for timely, accurate patient-centered radiology.
How Technology Can Improve Communication Between Radiologists and Referring Physicians
The Role of Advanced PACS in Streamlining Radiology Workflows
Modern PACS platforms, such as Radsource’s ProtonPACS, bridge critical communication gaps. With a cloud-based and hybrid approach, ProtonPACS delivers imaging data rapidly to both the radiologist and the referrer. This workflow transformation lets referring physicians see reports and high-resolution images in real time, preventing delays in patients’ treatment plans. Additionally, ProtonPACS integrates seamlessly with EHRs and RIS platforms, ensuring that the preferences of referring physicians for timely updates and clear data are respected.
For instance, if a primary care physician requests imaging follow-up, advanced PACS technology can trigger automated alerts, guaranteeing no crucial imaging volume is overlooked. By offering remote access—whether you’re in a medical center or a private practice—ProtonPACS reduces friction points. In short, these solutions empower radiologists to collaborate with referrers no matter where they are located, promoting g consistent, high-quality care.
AI and Automation: Supporting Decision-Making for Radiologists and Referring Physicians
The rise of AI tools and clinical decision support systems is reshaping communication between radiologists and referring. Automated templates and structured data extraction help reduce errors and standardize results. AI-driven image analysis can highlight areas of suspicion in imaging studies, aiding radiologist accuracy while speeding up the process of generating a final radiology report.
By quickly surfacing key findings through intelligent alerts, AI ensures referring physicians: receive actionable insights as soon as they are available. This reduces the risk of overlooked abnormalities and shortens the imaging examination life cycle. Moreover, automated checks for appropriateness—based on appropriateness criteria—guide referring clinicians toward the most appropriate imaging pathways, conserving resources and focusing on the best patient care possible.
Best Practices for Better Communication Between Radiologists and Referring Physicians
Optimizing Radiology Reports for Referring Physicians
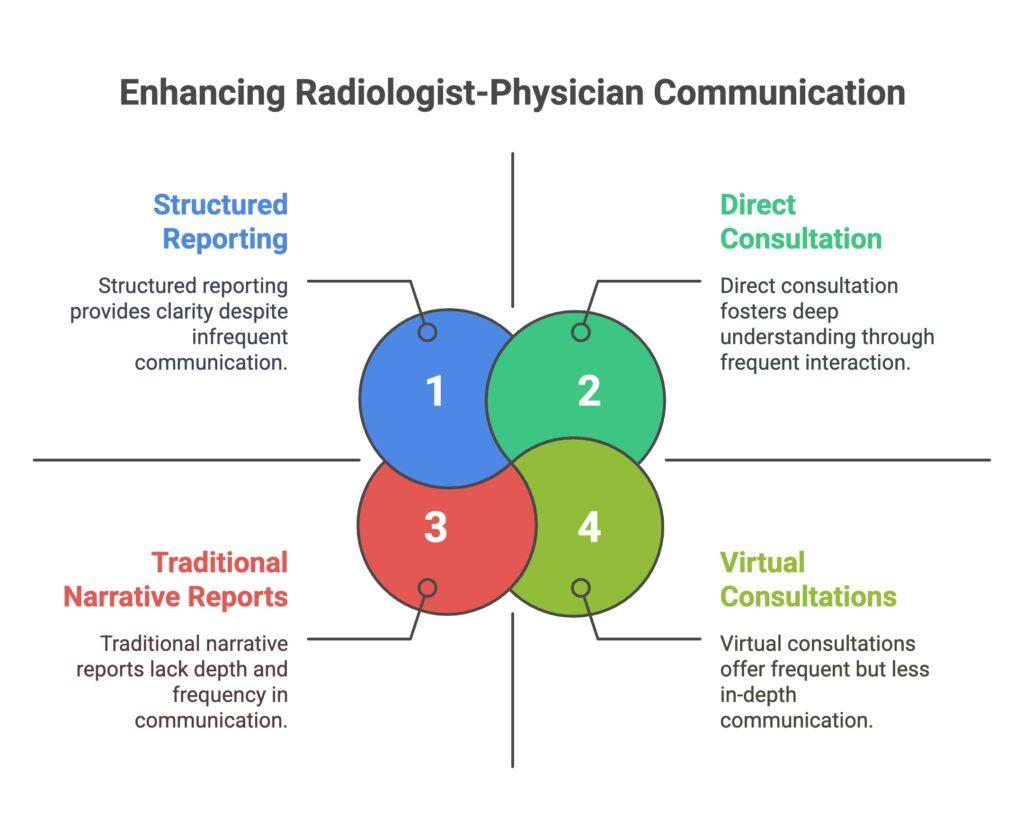
Structured reporting has gained traction, often recommended by the american college of radiology to address variability and enhance clarity. Compared to traditional narrative styles, structured reports highlight the essential points—diagnosis, impression, and recommended follow-up imaging—in a succinct format that referring physicians can scan quickly. The Journal of the American College recently published findings indicating that standardized reporting fosters improving relationships between radiologists and referrers.
Radsource builds on these insights by providing crystal-clear radiology report structures. Borrowing from radiology at Thomas Jefferson University best practices, each report focuses on relevant anatomical details, recommended next steps, and disclaimers about the imaging modality or technique used. This thorough yet concise approach aligns with referring physicians’ need for immediate clarity.
Direct Consultation: Enhancing the Radiologist’s Role as a Clinical Partner
Referring physicians and radiologists function at their best when direct, person-to-person consultations become part of regular clinical practice. Real-time discussions allow each radiologist to better understand the primary care context, guiding more accurate interpretations of imaging findings. Meanwhile, physicians know they can rapidly confirm a suspicion or adjust a patient’s treatment plan based on up-to-the-minute diagnostic insights.
Particularly in complex or subspecialty scenarios—such as interventional radiology or abdominal imaging—immediate feedback can be life-saving. When communication in radiology is prioritized, referring clinicians receive swift clarifications on complicated anomalies, ensuring the physician’s orders align with the most recent evidence. This collaborative ethos has been championed by experts like the assistant professor of radiology at the University of Virginia health system, highlighting the importance of open dialogue.
Radsource invests heavily in ensuring relationships with referring physicians remain strong. By providing phone, video conferencing, and secure messaging channels, radiologists can offer immediate second opinions or confirm preliminary diagnoses. This is especially valuable for high-stakes departments like Thomas Jefferson University Hospital, where quick decision-making can improve patient outcomes.
Virtual consultations and teleradiology: Making expert insights available anytime.
Today’s digital landscape makes it easier than ever for radiologists to offer tele-consults—especially in rural or underserved areas. Communicating with patients directly is still fairly rare among radiologists, but virtual consultation tools let them connect with primary care teams and specialists across various facilities. This model has proven beneficial when scans are conducted at an institutional level with limited on-site expertise.
Timely reporting is an essential factor for referring physicians to appreciate and for patients who want swift answers. With a strong teleradiology setup, radiologists can analyze images promptly, expedite official interpretations, and deliver them to the referrer in minutes or hours rather than days. Radsource, for instance, employs radiology partners who are experts in diagnostic radiology and can handle large volumes of advanced cases without sacrificing accuracy. By leveraging advanced systems and imaging follow-up reminders, they ensure that no detail slips through the cracks.
The Future of Radiology Collaboration: Moving Toward Value-Based Care
From Volume to Value: The Shift in Radiology Practices
As the healthcare industry embraces value-based care, there is a time when value and patient satisfaction are paramount. Moving from volume-driven models to value and patient satisfaction means prioritizing the quality of outcomes over sheer imaging volume. This shift encourages robust communication between radiologists and referring clinicians to choose appropriate imaging based on clinical necessity, not revenue.
For example, the american journal of roentgenology has discussed how imaging studies American clinical benefits can be avoided, freeing up resources for more essential scans. This shift toward value-based care also complements the drive for interoperability—data sharing across health platforms helps coordinate care across multiple specialties. Radiologists must ensure their tools are integrated seamlessly to facilitate quick consultations with primary care physician teams.
Conclusion: A Collaborative Approach to Better Patient Outcomes
Effective collaboration hinges on direct consultations, structured radiology report formats, and integrated technology platforms. Whether in a sprawling medical center or a smaller outpatient clinic, these steps bolster communication in radiology and strengthen the relationship between radiologists and referring physicians.
With cutting-edge PACS technology like ProtonPACS and partnerships forged with industry leaders, Radsource stands out for its commitment to the best patient care. Drawing from institutions such as Thomas Jefferson University Hospital in Philadelphia and insights gleaned during radiology residency programs each radiologist is fully equipped to support referring physicians across multiple specialties—from musculoskeletal radiology at thomas jefferson to family medicine.
In a time when value and patient Thomas Jeffersontter most, investing in robust technology and direct physician-to-radiologist relationships is non-negotiable. If you’re ready to collaborate with a leading innovator in patient-centered radiology, reach out to Radsource today. Let’s forge good relationships that empower and improve patient outcomes, reduce overall costs for your health system, and deliver the clarity and expertise both referring physicians and patients want. By working together, we can elevate radiology practice to new levels of efficiency and excellence—ultimately delivering the highest standard of care for every patient’s journey.