In the rapidly evolving field of medical technology, understanding the protocols that govern data exchange and storage is crucial. This article delves into DICOM (Digital Imaging and Communications in Medicine) and HL7 (Health Level 7). These two cornerstone standards facilitate the seamless operation of medical imaging and health information systems.
What is DICOM?
DICOM stands for Digital Imaging and Communications in Medicine. It is the international standard for storing and transmitting medical images and related information. DICOM enables the integration of scanners, servers, workstations, printers, and network hardware from multiple manufacturers into a picture archiving and communication system (PACS). It supports a range of imaging formats including, but not limited to, X-ray, ultrasound, CT, and MRI.
What is HL7?
Health Level 7 (HL7) refers to a set of international standards for the transfer of clinical and administrative data between software applications used by various healthcare providers. HL7 focuses on the language and structure of that data to ensure interoperability between systems. Unlike DICOM, HL7 is not limited to imaging data, encompassing a broad spectrum of in-patient and outpatient services data.
DICOM vs. HL7: Understanding the Differences
In the world of healthcare information technology, understanding the distinctions between DICOM and HL7 is crucial for professionals tasked with managing patient data and medical imaging. These standards serve different, though sometimes overlapping, functions within healthcare settings.
Core Functions
DICOM (Digital Imaging and Communications in Medicine) is specifically designed for handling, storing, printing, and transmitting information in medical imaging. It includes a file format definition and a network communications protocol that uses TCP/IP to communicate between systems.
HL7 (Health Level 7) focuses on the exchange, integration, sharing, and retrieval of electronic health information. It supports clinical practice and the management, delivery, and evaluation of health services, which is broader than the imaging-specific focus of DICOM.
Usage in Healthcare
DICOM is predominantly utilized in medical imaging departments such as radiology, cardiology, and dental imaging. It is essential for daily operations where imaging is critical for diagnosis and treatment planning. Radiology PACS, Cardiology PACS, and Dental Imaging PACS systems are the backbone for linking patient care data to the imaging center of the operations.
HL7 is used throughout the entire healthcare environment. It facilitates a broader scope of communications for hospital systems, including laboratory, pharmacy, billing, and other administrative and clinical data exchanges.
Key Differences
Here are the fundamental differences between DICOM and HL7 summarized in a table format:
| Feature | DICOM | HL7 |
|---|---|---|
| Primary Use | Management of imaging data | Exchange of clinical and administrative data |
| Scope | Specific to imaging processes | Broad, covering all aspects of healthcare information |
| Data Format | Standardized image formats and files | Structured data conforming to a wide range of messaging standards |
| Network Protocol | Built on TCP/IP for image transfer | Uses a variety of protocols, often tailored per implementation |
| Integration | Integrates with imaging equipment and PACS | Integrates with EHRs, lab systems, and other health information systems |
| Functionality | Focuses on image capture, storage, and retrieval | Facilitates a wide range of hospital communications, patient records, and more |
| Standards Versions | Relatively stable and specific | Frequently updated, with multiple versions in use (e.g., v2.x, v3, FHIR) |
Enhancing Efficiency Through Understanding
By comprehending these differences, healthcare IT professionals can better tailor their systems and workflows to meet the specific needs of their medical facilities. For instance, a hospital might prioritize upgrading its PACS and ensuring DICOM compliance in its radiology department, while also deploying an HL7-compliant EHR system that integrates seamlessly with all other departments. This comprehensive approach ensures that both imaging and non-imaging patient data are managed effectively, enhancing overall operational efficiency and patient care.
Integrating DICOM with HL7
The seamless integration of DICOM with HL7 protocols is essential for modern healthcare facilities to effectively manage both imaging and non-imaging patient data. This integration ensures that all aspects of patient care—from medical imaging to clinical history—are accessible within a unified system, facilitating better patient outcomes and streamlined operations.
Understanding the Integration
DICOM and HL7 serve complementary functions in a healthcare setting. DICOM primarily handles the storage, retrieval, and management of medical images. In contrast, HL7 deals with the exchange of clinical and administrative data between systems. Integrating these two standards allows healthcare providers to have a holistic view of a patient’s medical record. For example, when a patient undergoes an MRI, the DICOM protocol ensures that the images are correctly stored in the PACS and are readily accessible. Simultaneously, HL7 protocols ensure that relevant patient information from the hospital information system (HIS) or electronic health record (EHR), such as patient demographics, medical history, and current medications, is available to the radiologist.
Real-World Application
Consider a scenario in a large hospital where a patient is admitted with severe headaches. The patient undergoes several diagnostic tests, including an MRI. Here’s how DICOM and HL7 work together:
DICOM: The MRI machine uses DICOM standards to capture the images and sends them to the PACS where they are stored with unique identifiers and can be retrieved for viewing on any DICOM-compliant system within the network.
HL7: Simultaneously, the patient’s symptoms, history of present illness, and preliminary tests are documented in the EHR. HL7 standards are used to push this information from the EHR to other clinical systems, including the PACS, where it can be viewed alongside the DICOM images.
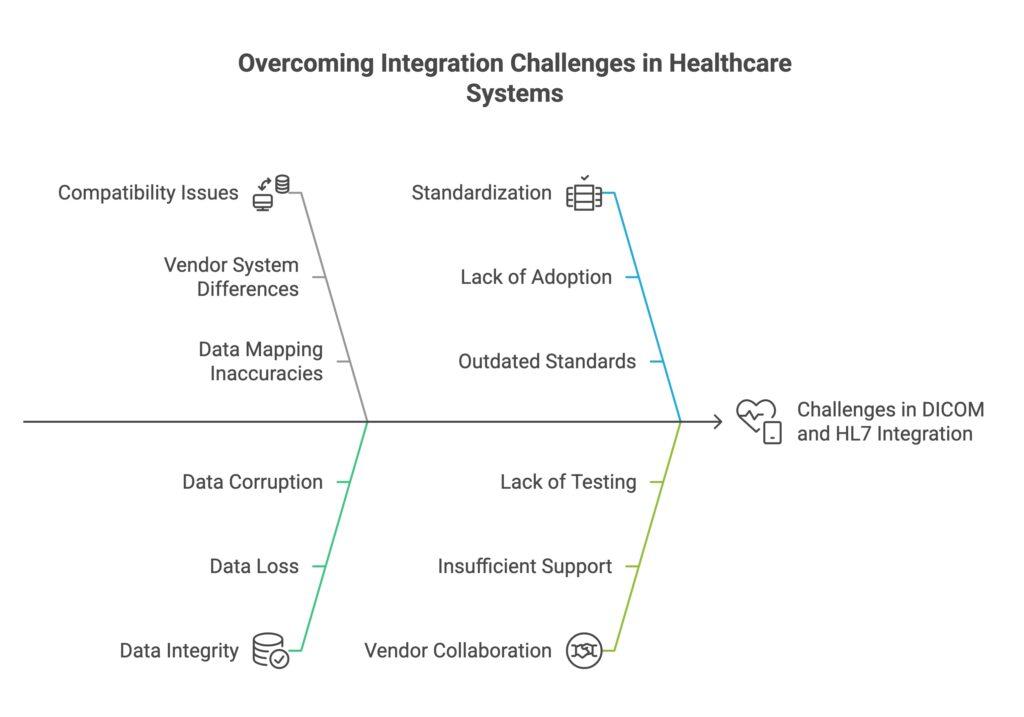
Challenges and Solutions in Integration
Integrating DICOM with HL7 is not without challenges. The primary issue often lies in the compatibility between different vendors’ systems and the need for precise data mapping between systems to maintain data integrity. Solutions include:
Middleware: Implementing middleware solutions that can translate and route data between DICOM and HL7 systems, ensuring that data flows seamlessly across different platforms and applications.
Standardization Efforts: Encouraging the adoption of newer and more integrated versions of these standards, such as HL7 FHIR, which is designed to simplify implementation and increase interoperability.
Vendor Collaboration: Working closely with vendors to ensure that both DICOM and HL7 protocols are well-supported and that their integration is tested and certified.
Future Trends and Standards
The future of healthcare IT is being shaped by developments in artificial intelligence, machine learning, and cloud computing. These technologies promise to enhance the capabilities of both DICOM and HL7 by offering more sophisticated data analysis tools and scalable storage solutions. It’s important for professionals to stay informed about these trends as they develop.
Practical Tips for Radiologists
Practical advice for radiologists may include tips on choosing DICOM and HL7-compliant software, insights into the training necessary to effectively use these standards, and strategies for keeping up with ongoing changes and updates in the field.