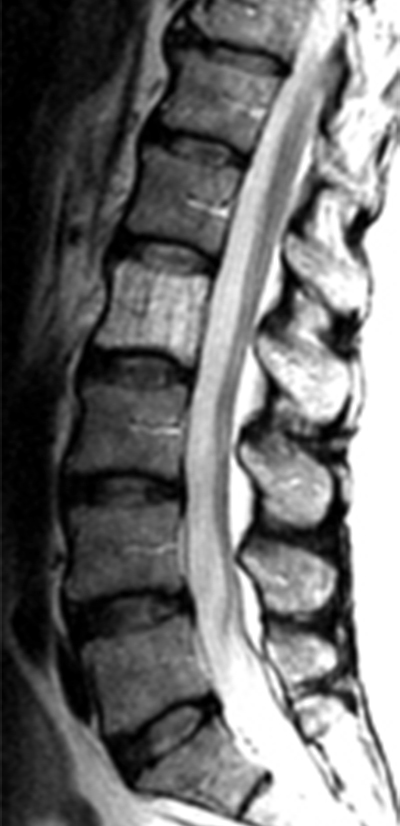
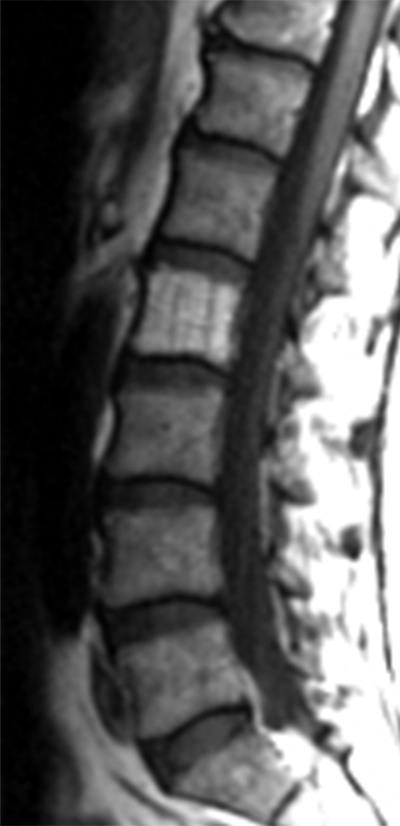
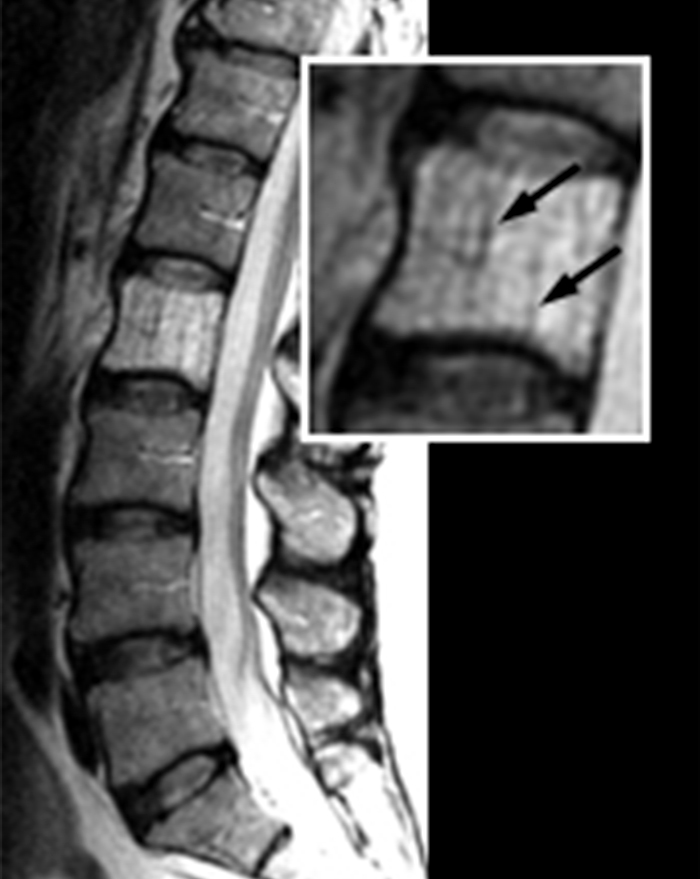
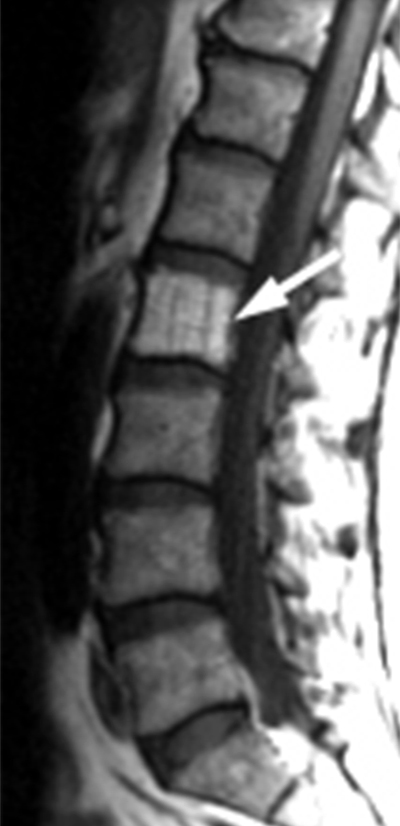
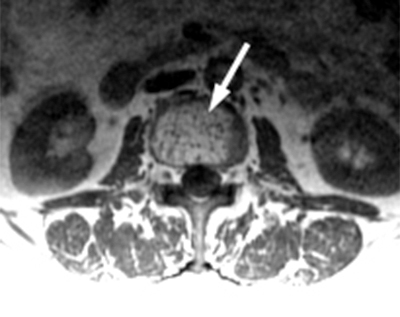
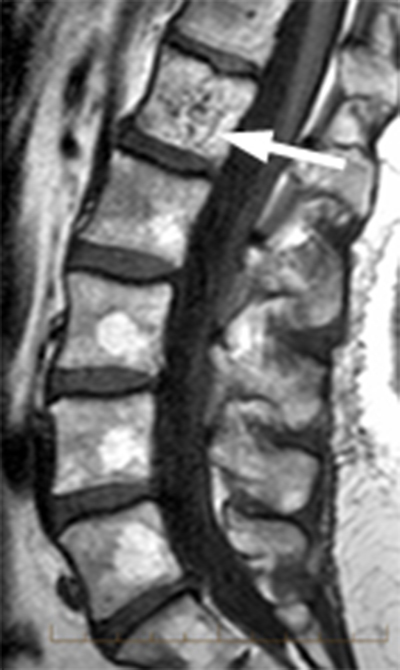
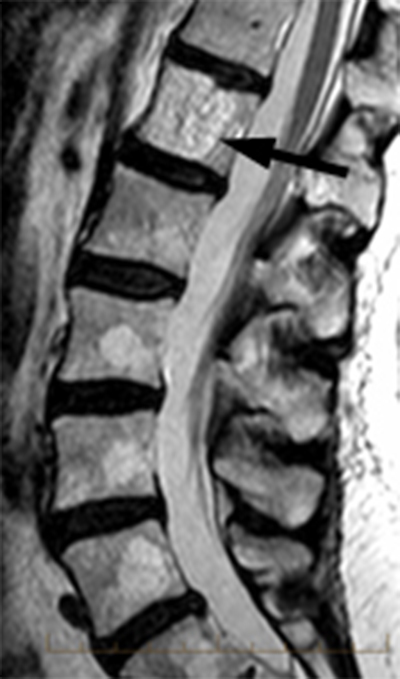
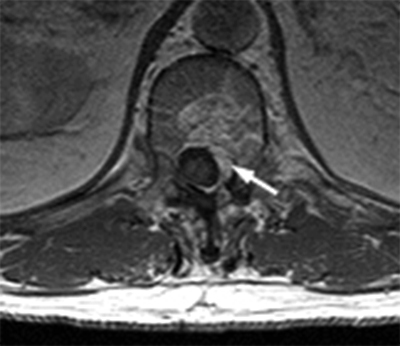
Clinical History: A 46 year-old female with a history of breast cancer presents with low back pain. (1a) Sagittal T2-weighted, (1b) sagittal T1-weighted and (1c) axial T1-weighted images are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Vertebral Hemangioma
Discussion
Hemangiomas of the vertebral bodies are common benign vascular tumors. Vertebral body hemangiomas are the most common tumor of the spinal axis and occur in approximately 10-20% of adults.1 Most of the lesions occur in the thoracolumbar spine. The majority of the hemangiomas seen with imaging studies are asymptomatic and incidental findings. Some authors report a 2:1 female/male predominance, but others report an equal incidence in males and females, and that only the symptomatic lesions are more common in females.1,2 Approximately 20-30% of hemangiomas are multiple, particularly in the thoracic spine. The lesions are usually rounded with discrete margins, unless a pathologic fracture has occurred. They can vary from being subcentimeter in size to replacing the entire vertebral body. The lesions are most commonly limited to the vertebral body, but 10-15% extend into the posterior elements. Hemangiomas seldom arise primarily from the posterior elements. The majority of vertebral body hemangiomas have no associated abnormalities, but rarely they are associated with an autosomal dominant syndrome that includes cerebral cavernous malformations.1
Osseous hemangiomas are slow growing hamartomas. Histopathologically they consist of thin-walled blood vessels and sinuses lined by endothelium and interspersed among sparse longitudinally oriented trabeculae of bones. The dilated vascular channels are set in a stroma of fat. More aggressive hemangiomas contain less fat and more vascular stroma, and may look similar to a metastatic lesion on imaging studies.3
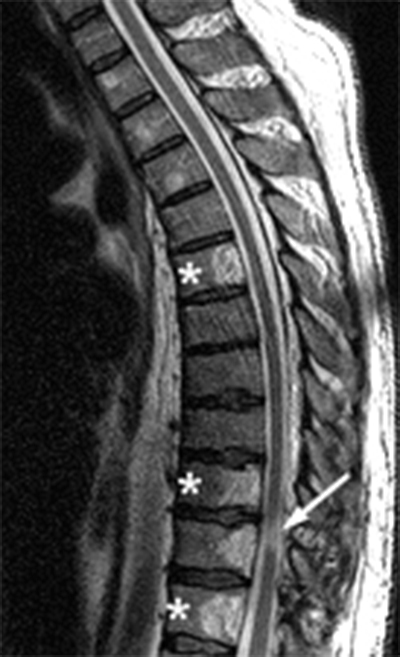
Hemangiomas have typical appearances with routine radiography, CT and MR. On plain radiographs, hemangiomas often have a vertically striated appearance due to thickening of bony trabeculae. This appearance has been described as “corduroy cloth” or “jail bar” and the overall density of the vertebral body is decreased due to the presence of fatty marrow.2 With CT, vertebral body hemangiomas have low attenuation interspersed with thickened bony trabeculae, causing a characteristic “salt and pepper” or “polka dot” appearance on axial images.1 With MR imaging, the intralesional fat of the hemangioma causes increased signal intensity on T1 weighted MR images.4 On T2-weighted images, the signal intensity of the hemangiomas also increases because of high water content,4 and the T2-hyperintensity is typically greater than that of fat, thereby differentiating hemangiomas from focal fat deposition. These signal characteristics also differ from those of metastatic lesions, which have decreased signal intensity on T1 weighted images and increased signal intensity on T2 weighted images. As with CT, the thickened bony trabeculae on MR axial images results in a “salt and pepper” or “polka dot” pattern. The signal intensities of atypical hemangiomas can be indeterminate, but the morphology of the lesion, including the presence of coarse trabeculae, can be used to make the diagnosis (5a, 6a). For more difficult indeterminate cases, CT can be used to problem solve, as CTs are more sensitive to the characteristic osseous remodeling of hemangiomas than MR imaging.5 If necessary, follow-up examinations can be performed to ensure stability. Only in rare cases is a core biopsy necessary to make the diagnosis.
Aggressive hemangiomas typically occur between T-3 and T-9 and commonly involve the entire vertebral body with extension into the neural arch. Aggressive hemangiomas generally have an expanded and indistinct cortex, an irregular honeycombing pattern, and a soft tissue mass.6 Aggressive vertebral hemangiomas can become symptomatic with growth, which often occurs during pregnancy. Symptomatic pathologic fractures can occur with hemangiomas and compression fractures can lead to myelopathy from cord compression.7 Symptomatic hemangiomas are usually treated non-surgically with embolization, sclerotherapy8 or vertebroplasty.9 Surgery is reserved for cases with cord compression, and radiation therapy may be used following subtotal resection.10
Conclusion
Vertebral body hemangiomas are the most common tumors of the spinal axis and in most circumstances are incidental findings. Most hemangiomas are diagnosed based on their characteristic imaging findings, though the diagnosis can be challenging in cases of atypical or aggressive hemangiomas. In such cases, the recognition of vertically oriented coarse bony trabeculae surrounded by fatty stroma, resulting in the “salt and pepper” appearance on axial images and a striated appearance on coronal or sagittal images, is the key to the correct diagnosis. Though rare, aggressive hemangiomas can be symptomatic and pathologic fractures can lead to myelopathy and cord compression. In such patients, MR accurately displays the extraosseous extension of the hemangioma and its effect upon the spinal canal and cord.
References
1 Ross JS. Hemangioma. In:Spine. First edition ed. Salt Lake City, UT: Amirsys, 2004; IV 1 14-16.
2 Grossman RI, Yousem DY. Nondegenerative diseases of the spine. In:Neuroradiology. Philadelphia: Mosby, 2003; 827-828.
3 Laredo JD, Assouline E, Gelbert F, Wybier M, Merland JJ, Tubiana JM. Vertebral hemangiomas: fat content as a sign of aggressiveness. Radiology 1990; 177:467-472.
4 Ross JS, Masaryk TJ, Modic MT, Carter JR, Mapstone T, Dengel FH. Vertebral hemangiomas: MR imaging. Radiology 1987; 165:165-169.
5 Cross JJ, Antoun NM, Laing RJ, Xuereb J. Imaging of compressive vertebral haemangiomas. Eur Radiol 2000; 10:997-1002.
6 Laredo JD, Reizine D, Bard M, Merland JJ. Vertebral hemangiomas: radiologic evaluation. Radiology 1986; 161:183-189.
7 Dickerman RD, Bennett MT. Acute spinal cord compression caused by vertebral hemangioma. Spine J 2005; 5:582-584; author reply 584.
8 Doppman JL, Oldfield EH, Heiss JD. Symptomatic vertebral hemangiomas: treatment by means of direct intralesional injection of ethanol. Radiology 2000; 214:341-348.
9 Galibert P, Deramond H. [Percutaneous acrylic vertebroplasty as a treatment of vertebral angioma as well as painful and debilitating diseases]. Chirurgie 1990; 116:326-334; discussion 335.
10 Fox MW, Onofrio BM. The natural history and management of symptomatic and asymptomatic vertebral hemangiomas. J Neurosurg 1993; 78:36-45.