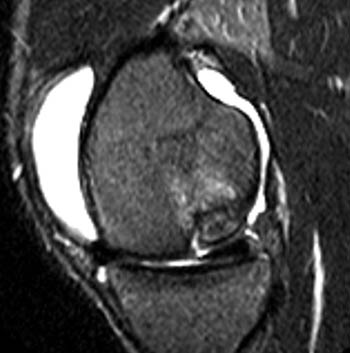
Clinical History: A nineteen year-old male presents with knee pain for several years. A (1a) STIR sagittal image is provided. What are the findings? What is your diagnosis?
Findings
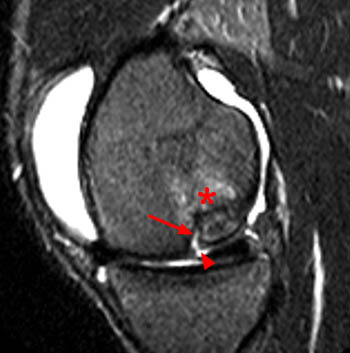
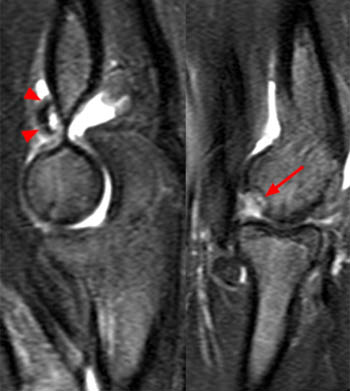
Figure 2:
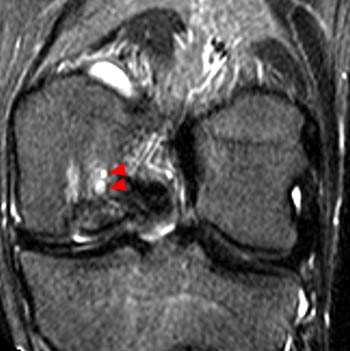
An osteochondral lesion is seen at the posterior weightbearing surface of the medial femoral condyle. A fluid-filled break in the articular surface (arrowhead) is present, and there is fluid at the anterior interface of the fragment (arrow). Edema is present in the bed of the defect (asterisk).
Diagnosis
Unstable osteochondritis dissecans of the medial femoral condyle.
Introduction
Osteochondritis dissecans (OCD) is an acquired disorder of bone in which there is fragmentation of the articular surface with varying degrees of cartilage involvement. The etiology is felt to be related to indirect trauma in most cases but familial factors, avascular necrosis, enchondral ossification abnormalities and fat emboli have been implicated as possible causes as well.1,2,3,4,5,6 In the elbow, the tenuous blood supply to the capitellum likely contributes.7,8 The most common locations for OCD are the femoral condyles, talar dome and capitellum. OCD of the talar dome is frequently related to an acute traumatic incident. Capitellar lesions are also strongly associated with elbow trauma or overuse in sports such as baseball pitching and gymnastics. In contrast, there is only a 40-50% association of OCD of the knee with knee trauma.6,7,8
Treatment of OCD can be conservative or surgical, depending on how likely the lesion is to heal on its own. Factors that affect this are age of presentation, lesion size and stability. Lesions that present before skeletal maturity (juvenile) frequently heal without surgical treatment and are generally treated conservatively. OCD presenting in adults has a worse prognosis due to decreased vascularity and development of interposed fibrous tissue, and almost always requires surgical intervention.1,3,6,9,10
MR evaluation
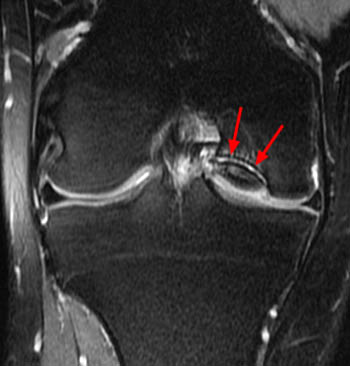
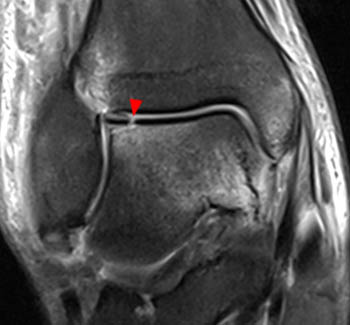
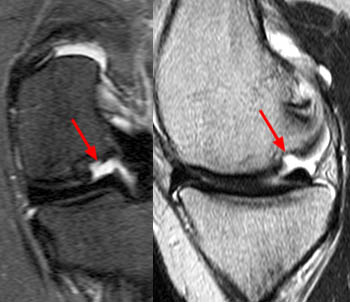
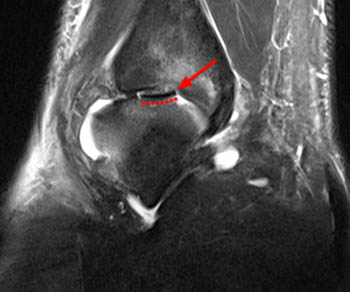
The most important thing to be evaluated for and reported on in MR of OCD cases is lesion stability/instability. This is best evaluated on fluid sensitive sequences. MR criteria for lesion instability include a high signal-intensity line indicating granulation tissue or fluid in the base of the lesion (3a), fluid extending to the articular surface (4a), a discrete cyst beneath the lesion (5a), or a focal articular defect (6a). Normal or low signal intensity beneath the lesion indicates stability.5,6
While the evaluation of OCD is similar for all anatomic locations, there are subtle differences which will be discussed below.
Knee
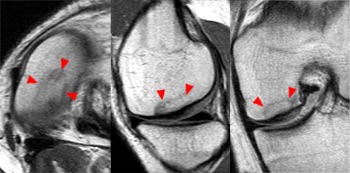
The MR criteria for lesion instability in OCD of the knee differ between juvenile and adult cases as the lesions in juveniles frequently heal with conservative treatment. As a result, healed osteochondral lesions are a not uncommon incidental finding in adult patients (7a). In adults, the MR imaging criteria of a high-signal-intensity rim surrounding an OCD lesion on T2-weighted images, cysts surrounding an OCD lesion, a high T2 signal intensity fracture line extending through the articular cartilage overlying an OCD lesion, and a fluid-filled osteochondral defect have high sensitivity and specificity for instability. In juveniles, the most useful findings of instability are a rim of fluid signal intensity, multiple breaks in the subchondral bone plate and a second outer rim of low T2 signal intensity. When used together, these three findings are highly sensitive and specific. While the presence of cysts in juvenile OCD is nonspecific, the presence of multiple cysts or a single cyst larger than 5mm is highly specific but not highly sensitive for instability.10 The high signal intensity rim must be as bright as fluid and the cysts in the base of the lesion must be multiple and larger than 5mm.3
OCD in juveniles must also be distinguished from normal ossification variants. The variants will have normal overlying cartilage and no associated marrow edema and are commonly located in the posterior lateral femoral condyle.3,4,13
Talar Dome
Most OCD of the talar dome (8a) treated non-operatively improve or show no change on MRI at an average of 13.7 months, and marrow edema and subchondral cysts are not reliable indicators of progression. Current guidelines suggest operative treatment for nondisplaced chronic lesions after a failed 3-6 month trial of conservative management. Larger lesions (greater than 15mm in diameter) are less likely to have good surgical outcomes.11
Capitellum
Capitellar OCD is frequently found in young teenagers. Nonoperative treatment is favored in young patients with small stable lesions. There is high stress on the elbow in overhead athletes, predisposing to lesion instability.12,8 Baseball pitchers and gymnasts are most susceptible due to severe compressive and shearing forces across the radiocapitellar joint. OCD usually occurs in the anterolateral portion and must be distinguished from the normal pseudodefect in the posterior capitellum.7,8 Surgical intervention is indicated for unstable lesions or lesions that have failed conservative measures. Surgery may be debridement, drilling or microfracutre or internal stabilization (for a single large fragment). OCD of the capitellum is easiest to identify on the T1 weighted images, especially if the lesion is stable. A stable lesion can still have chondral injury and it is important to look carefully for loose bodies (9a).8
Surgical options
The goal of surgery is decreased pain, increased function and prevention of lesion enlargement.11 Surgical treatment options for OCD include primary fixation of the fragment, arthroscopic debridement, curettage and microfracture, autogenous or allogenic osteochondral grafting (OATS), excision with or without curettage and drilling and autologous chondrocyte implantation (ACI).11
Microfracture has an advantage in that it can be performed arthroscopically and the disadvantage of prolonged period of non-weightbearing postoperatively and the fact that the articular surface will be fibrocartilage, which is less durable than hyaline cartilage.
Return to athletic activity is one criterion of a successful outcome following surgery. OATS is a good surgical option for treatment of OCD in the knee in an active patient because it is the only procedure that provides immediate structural integrity to the joint and restores the articular surface. Return to full athletic activity is more likely in patients under 25 years of age with less than 12 months of symptoms.14
OATS advantages include rapid incorporation of bone and immediate restoration of a hyaline cartilage surface. The disadvantages are donor site problems and fibrocartilage filling in between the plugs. The technique is also limited by defect size.
ACI is durable but invasive and requires a long time for the defect to fill. An osteotomy is frequently required for optimal results. To address these drawbacks, an arthroscopic technique is being developed and more aggressive, sports-specific rehabilitation is being used.14 ACI is useful in adult knee lesions with previous failed non-ACI treatment.9
Bioabsorbable fixation of lesions in the knee in adults has a high failure and complication rate.1
Conclusion
Osteochondritis dissecans is a not uncommon abnormality that may be found in several characteristic locations in the musculoskeletal system. In cases of OCD, MR is able to reliably detect the abnormality and provide important diagnostic information. Treatment options are often dependent upon factors such as lesion instability, the presence of loose bodies, and skeletal age; all of these factors can be accurately evaluated through proper MR technique and interpretation.
References
1 Millington K, Shah J, Dahm D, Levy B, Stuart M. Bioabsorbable Fixation of Unstable Osteochondritis Dissecans Lesions. Am J Sports Med; 2010; 38: 2065-2070.
2 Resnick D, Kang HS, Pretterklieber, ML. Internal Derangement of Joints, 2nd ed. 2007. Saunders
3 Thapas M, Chaturvedi A, Darling S, Khanna P, Ishak G, Chew F. MRI of Pediatric Patients: Part 2, Normal Variants and Abnormalities of the Knee. AJR; 2012; 198: W456-W465.
4 Pail D, Strouse P. MRI of the Pediatric Knee. AJR; 2011; 196: 1019-1027.
5 Osteochondritis Dissecans of the knee: Value of MR Imaging in Determining Lesion Stability and the Presence of Articular Cartilage Defects. AJR; 1990; 155:549-553.
6 De Smet A. Radiology of Osteochondritis Dissecans. Radiology; 1998;5: Reprint.
7 Iyer R, Thapa M, Khanna P, Chew F. Pediatric Bone Imaging: Imaging Elbow Trauma in Children-A Review of Acute and Chronic Injuries. AJR; 2012; 198: 1053-1068.
8 Kijowski R, De Smet A. MRI Findings of Osteochondritis Dissecans of the Capitellum with Surgical Correlation. AJR; 2005; 185:1453-1459.
9 Cole B, DeBerardino T, Brewster R, Farr J, Levine D, Nissen C, Roaf P, Zaslav K. Outcomes of Autologous Chondrocyte Implantation in Study of the Treatment of Articular Repair (STAR) Patients With Osteochondritis Dissecans. Am J Sports Med; 2012; Published online before print July 19, 2012.
10 Kijowski R, Blankenbaker D, Shinki K, Fine J, Graf B, De Smet, A. Juvenile versus Adult Osteochondritis Dissecans of the Knee: Appropriate MR Imaging Criteria for Instability. Radiology; 2008; 248: 571-578.
11 Hunt K, Lee A, Lindsey D, Slikker W, Chou L. Osteochondral Lesions of the Talus: Effect of Defect Size and Plantar flexion Angle on Ankle Joint Stresses. Am J Sports Med; 2012; 40: 895-901.
12 Iwasaki N, Kamishima T, Kato H, Funakoshi T, Minami A. A Retrospective Evaluation of Magnetic Resonance Imaging Effectiveness on Capitellar Osteochondritis Dissecans Among Overhead Athletes. Am J Sports Med; 2012; 40: 624-630.
13 Kjellin, Ingrid. Radsource Web Clinic: October, 2009.
14 Krych A, Robertson C, Williams R, Carthage Study Group. Am J Sports Med; 2012; 40: 1053-1059.