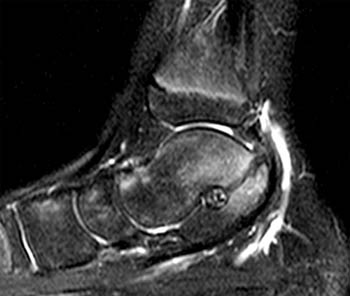
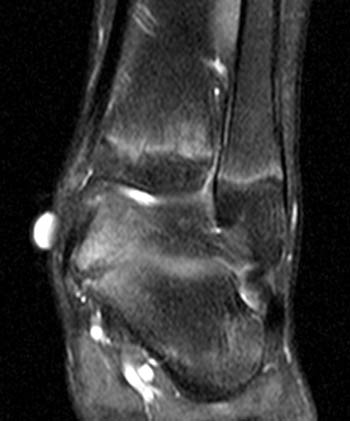
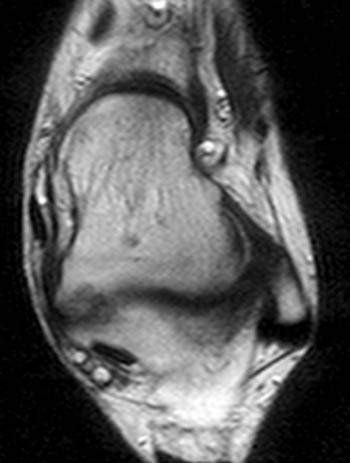
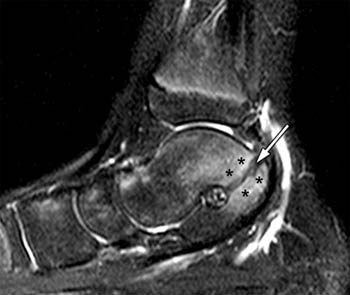
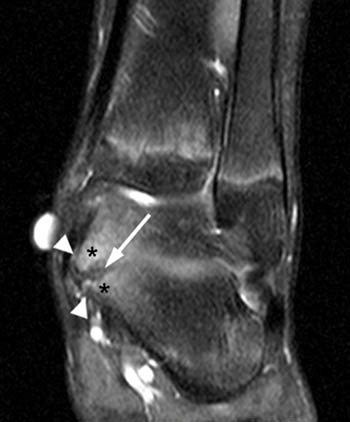
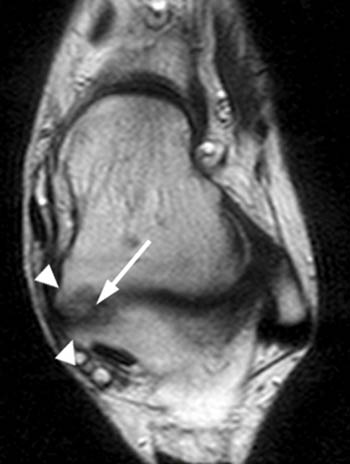
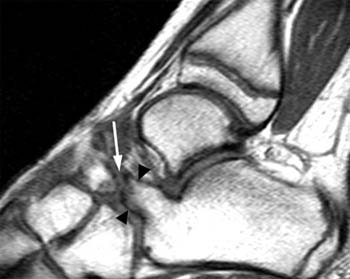
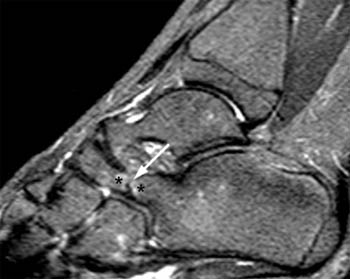
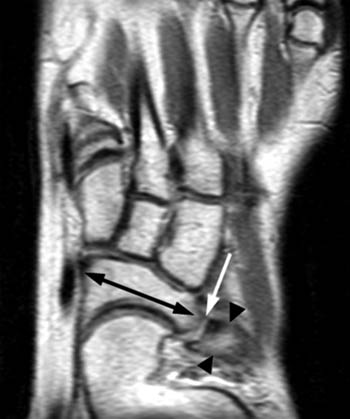
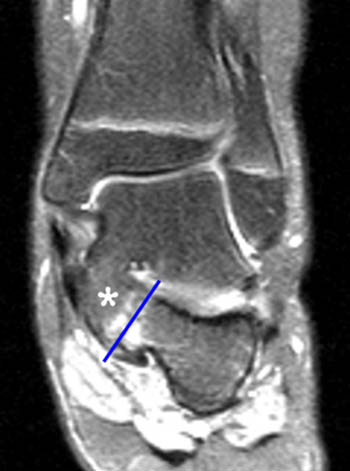
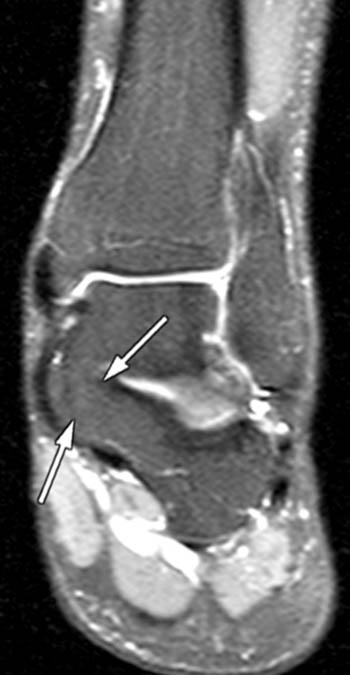
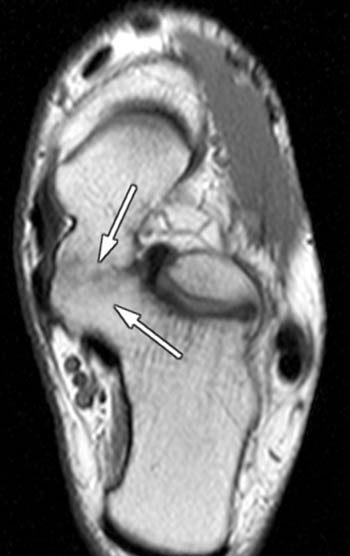
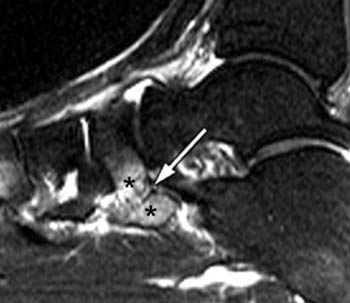
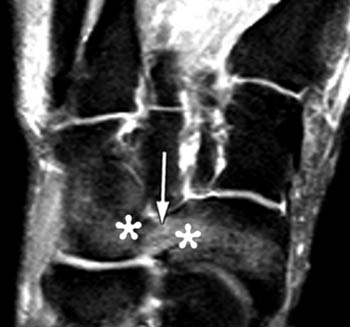
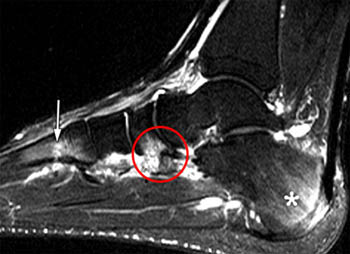
Clinical History: A 12 yo female presents with a history of medial pain and clinician’s note to “evaluate posterior tibial tendon.” (1a) Fat-suppressed T2-weighted sagittal, (1b) fat-suppressed proton density-weighted coronal, and (1c) T2-weighted axial images of the ankle are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Talocalcaneal fibrous coalition, posterior facet
Introduction
Tarsal coalition is defined as the abnormal union of one or more bones of the hindfoot or midfoot, felt to be the result of failure of segmentation of primitive mesenchyme.1 These unions can be osseous (synostosis), cartilaginous (synchondrosis), or fibrous (syndesmosis). Although these distinctions have implications for imaging and treatment, tarsal coalition is best thought of as a continuum, progressing from fibrous to osseous as the patient ages, often demonstrating different coexistent histologic stages.2 The incidence is 1% or less in the general population, with evidence for autosomal dominant inheritance with variable penetration; it is bilateral in close to 50% of cases.4,5 Approximately 90% of all tarsal coalitions are talocalcaneal or calcaneonavicular, although cases of cubonavicular, calcaneocuboid, and navicular-first cuneiform coalitions have been reported.2,3,6,7 The presentation of tarsal coalition is insidious, non-specific, and variable, depending upon progressive ossification, which typically occurs between 8-12 years in calcaneonavicular coalition and 12-16 years in talocalcaneal coalition.8 However, some patients present in adulthood, or may even be asymptomatic. Common clinical presentations include tarsal pain or stiffness, ankle sprains, rigid flatfoot, or peroneal spastic flatfoot (more correctly referred to as peroneal spasm/shortening secondary to heel valgus).2 Given the variable presentation of tarsal coalition, it is a difficult diagnosis to make clinically, and is frequently discovered on MRI imaging for non-specific foot and ankle pain. MRI is an excellent tool for diagnosis of tarsal coalition and other associated abnormalities, as well as for surgical planning.
Imaging of Tarsal Coalitions
Plain film diagnosis of tarsal coalition presents varying degrees of difficulty and accuracy. Osseous coalitions with clear bony bridging are more easily diagnosed than fibrous or cartilaginous coalitions, which demonstrate varying degrees of joint space narrowing, cortical irregularity and sclerosis. Calcaneonavicular coalitions are typically fairly easily visualized on oblique 45 degree radiographs, but talocalcaneal coalitions require the axial (Harris-Beath) view and are more difficult to visualize. Although CT and MRI have been shown to clearly demonstrate the full extent and detail of tarsal coalitions, many useful radiographic signs for tarsal coalition have been described, and several articles have been published recently revisiting the use of plain film diagnosis for tarsal coalitions.9-12 Scintigraphy is of limited use in the skeletally immature patient, due to increased radiotracer uptake in normal epiphyses.3 Given the subtlety of findings, even on multiplanar imaging, a thorough knowledge of both plain film and MRI findings of tarsal coalition are required for accurate diagnosis. Some plain film findings are also visible on MRI, and can aid in diagnosis in difficult cases.
Calcaneonavicular coalitions demonstrate varying degrees of osseous and fibrous/cartilaginous bridging between the anterior process of the calcaneus and the lateral aspect of the navicular. Lateral plain films13 and sagittal MRI images often demonstrate the “anteater’s nose,” elongation and broadening of the anterior process of the calcaneus. MRI images clearly demonstrate surrounding marrow edema. Axial images demonstrate widening of the mediolateral dimension of the navicular, with lateral tapering. (Figures 5a,6a,7a)
The subtalar joint consists of posterior, middle and anterior articulating facets. Fusion at the middle articular facet is by far the most common. While the normal medial facet of the talocalcaneal joint demonstrates an upward or horizontal orientation, a middle facet coalition has a typical downward medial sloping seen on coronal MRI (Figure 8a) and CT images. A hypoplastic or aplastic sustentaculum tali may also be present.2 The most common associated plain film findings is the talar beak, a dorsal excrescence at the site of the calcaneonavicular ligament insertion arising from excessive traction due to abnormal motion of the subtalar joint.9 The c-sign is a plain film finding only, due to overlapping bone shadows, and dependent upon proper positioning of the foot and proper incidence of the x-ray beam.9,10,11
An osseous coalition demonstrates a solid anomalous osseous bridge between bones, easily detectible on both MRI and CT scans (Figures 9a,9b). Although CT and MRI both provide detailed information for diagnosing and determining the extent of tarsal coalitions, MRI can be more accurate in subtle cases of fibrous coalition, where osseous changes may not be as conspicuous.14
The rare cubonavicular coalition presents a diagnostic challenge, and findings are subtle, even with the aid of multiplanar imaging. MRI has the added advantage of demonstrating marrow edema surrounding the anomalous articulation, which itself may only be seen on one or two images, due to the relatively small size of the tarsal articular surfaces (Figure 10a,11a). Importantly, MRI will often detect concomitant pathology, some of which may be secondary to the underlying coalition, such as stress fracture or stress reaction due to altered biomechanics, or ankle sprains (Figure 12a).15,16
Treatment
Treatment of tarsal coalition begins with conservative therapy, including orthotics, non-steroidal anti-inflammatory medications, or steroid injection. Calcaneonavicular coalitions requiring surgery are commonly treated with excision and interposition of the extensor digitorum brevis tendon. Talocalcaneal coalitions are treated surgically with resection of the middle facet bony bridge and fat interposition. In either case, the existence of concomitant degenerative joint disease may mandate triple arthrodesis rather than resection.2
Conclusion
Given the insidious onset and non-specific symptoms of tarsal coalition, the diagnosis may not be obvious clinically. Routine plain films may not be adequate to make the diagnosis, especially in the case of a fibrous talocalcaneal coalition or with rare types of tarsal coalition. MRI provides the most detailed and accurate diagnosis of all types of tarsal coalition, many of which are found on MRIs ordered for other clinical indications. MRI provides the added benefit of depicting concurrent injuries such as stress fractures or sprains. It is also invaluable for surgical planning, depicting the full extent of involvement, evaluating the tendon that may be destined for surgical interposition, and allowing detection of associated osteoarthritis.
References
1 Jack FA. Bone anomalies of the tarsus in relation to “peroneal spastic flat foot”. J Bone Joint Surg Br. 1954; 36:530-542.
2 Newman JS, Newberg AH. Congenital tarsal coalition: multimodality evaluation with emphasis on CT and MR imaging. Radiographics. Mar-Apr 2000;20(2):321-32.
3 Pachuda NM, Lasday SD, Jay RM. Tarsal coalition: etiology, diagnosis, and treatment. J Foot Surg 1990; 29:474-488.
4 Leonard MA. The inheritance of tarsal coalition and its relationship to spastic flat foot. J Bone Joint Surg Br. Aug 1974;56B(3):520-6.
5 Stormont DM, Peterson HA. The relative incidence of tarsal coalition. Clin Orthop. Dec 1983;(181):28-36.
6 Kumai T, Tanaka Y, Takakura Y, Tamai S. Isolated first naviculocuneiform joint coalition. Foot Ankle Int 1996; 17:635-640.
7 Palladino SJ, Schiller L, Johnson JD. Cubonavicular coalition. J Am Podiatr Assoc 1991; 81:262-266.
8 Cowell HR, Elener V. Rigid painful flatfoot secondary to tarsal coalition. Clin Orthop 1983; 177:54-60.
9 Resnick D. Talar ridges, osteophytes, and beaks: a radiologic commentary. Radiology. May 1984;151(2):329-32
10 Lateur LM, Van Hoe LR, Van Ghillewe KV, et al. Subtalar coalition: diagnosis with the C sign on lateral radiographs of the ankle. Radiology. Dec 1994;193(3):847-51.
11 Taniguchi A, Tanaka Y, Kadono K, Takakura Y, Kurumatani N. C sign for diagnosis of talocalcaneal coalition. Radiology. Aug 2003;228(2):501-5.
12 Crim JR, Kjeldsberg KM. Radiographic diagnosis of tarsal coalition. AJR Am J Roentgenol. Feb 2004;182(2):323-8.
13 Chapman VM. The anteater nose sign. Radiology, November 1, 2007; 245(2): 604 ” 605.
14 Wechsler RJ, Schweitzer ME, Deely DM, Horn BD, Pizzutillo PD. Tarsal coalition: depiction and characterization with CT and MR imaging. Radiology1994; 193:447 “452.
15 Moe DC, Choi JJ, Davis KW. Posterior subtalar facet coalition with calcaneal stress fracture Am. J. Roentgenol. January 1, 2006; 186(1): 259 – 264.
16 Schweitzer ME, White LM. Does altered biomechanics cause marrow edema” Radiology 1996;198 : 851-853.