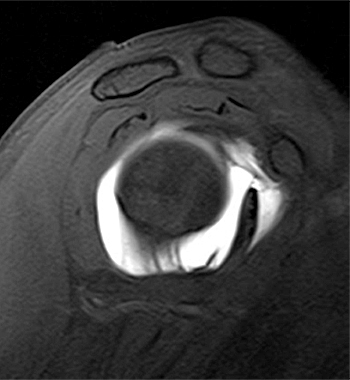
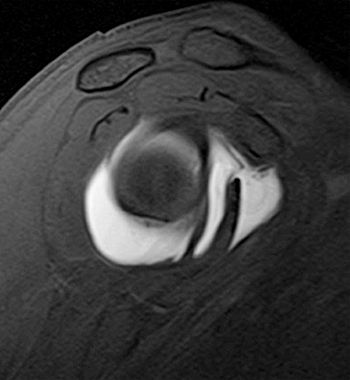
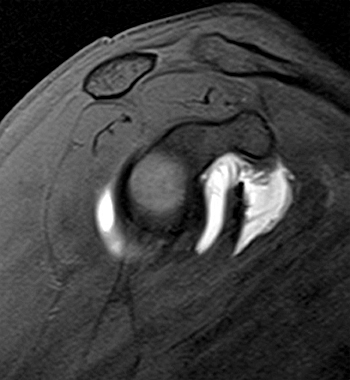
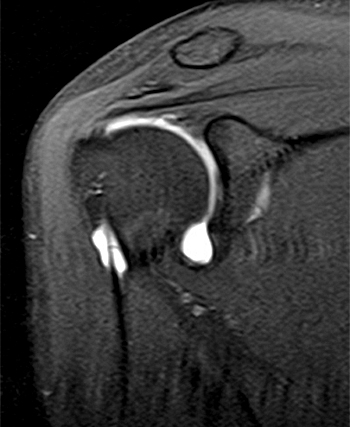
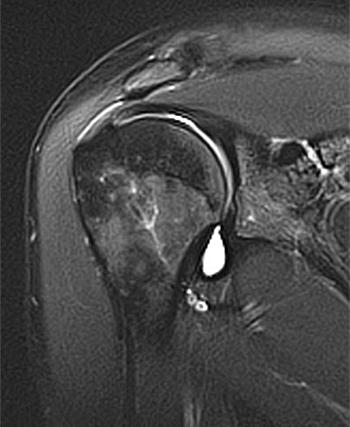
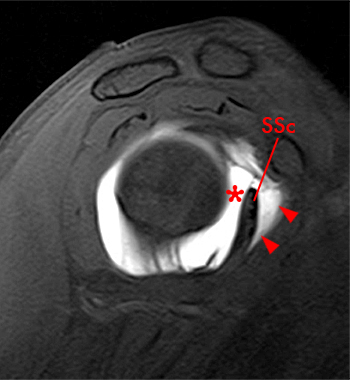
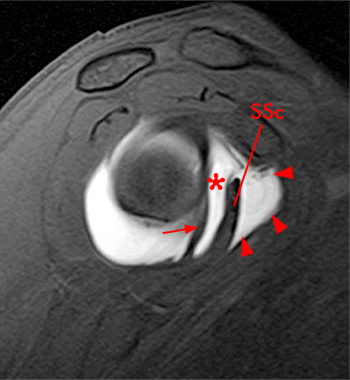
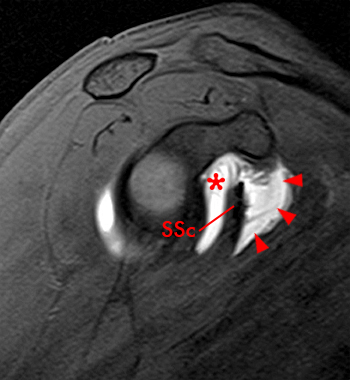
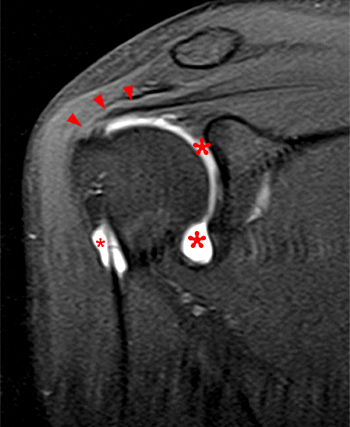
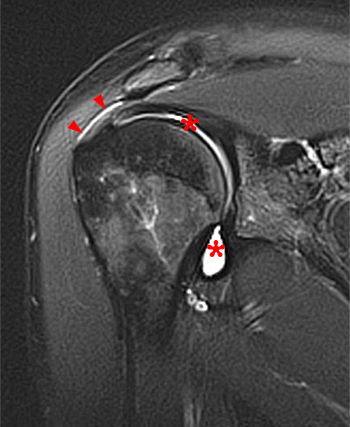
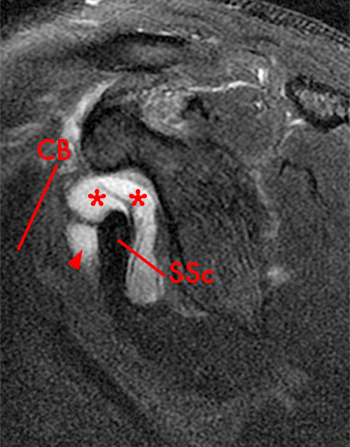
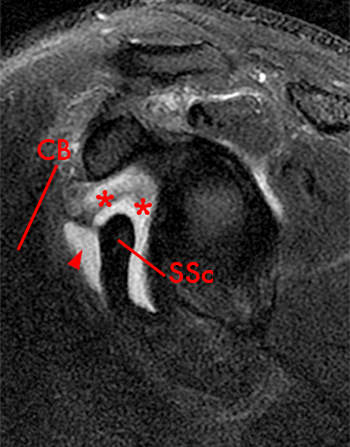
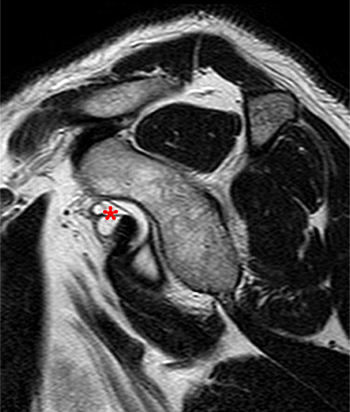
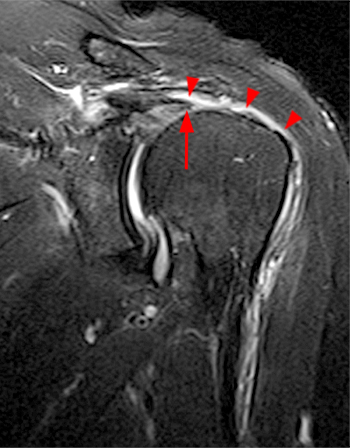
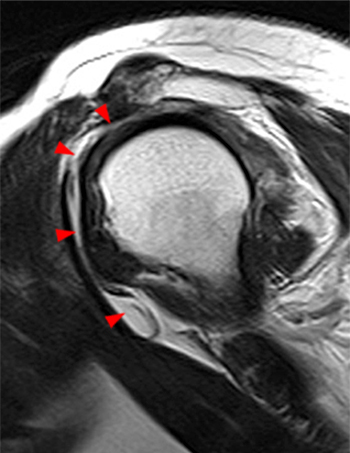
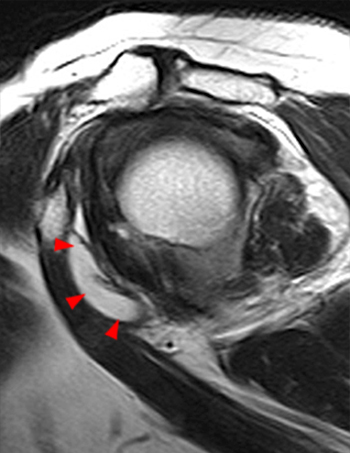
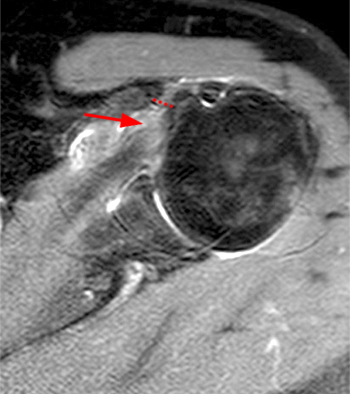
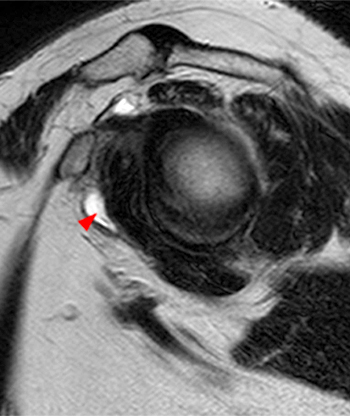
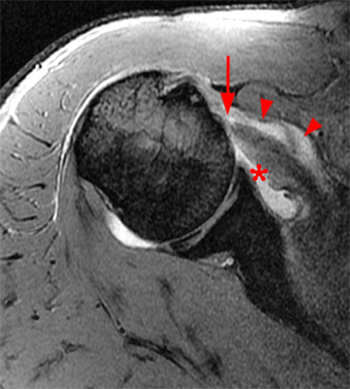
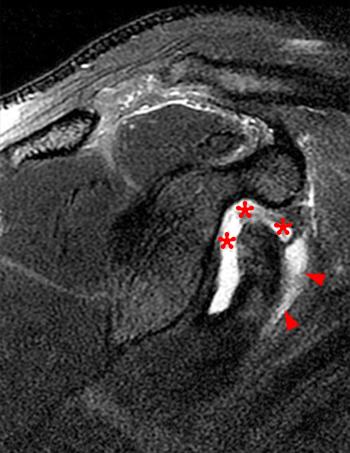
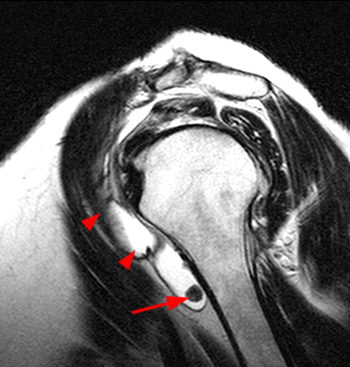
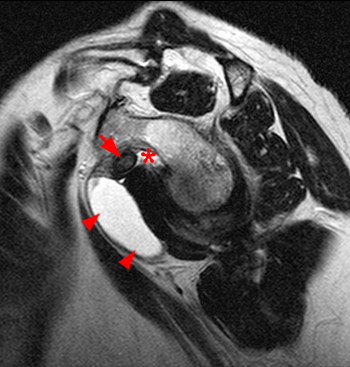
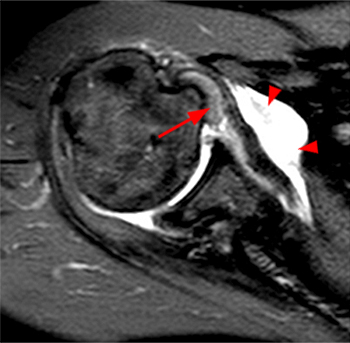
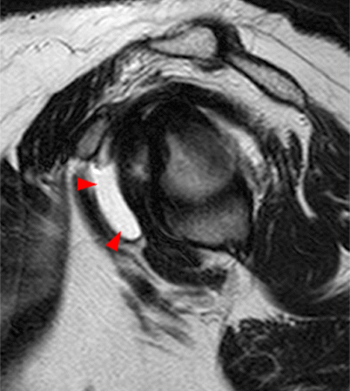
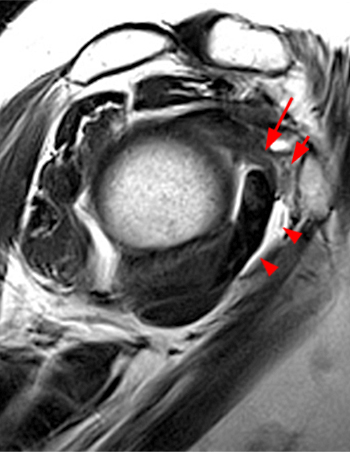
Clinical History: A 35 year-old female presents with shoulder pain after injuring her shoulder lifting a gate. Images from an MR arthrogram are presented. Three sagittal fat-suppressed T1-weighted images extending lateral to medial (1a, 1b, 1c), a coronal fat suppressed T1-weighted image (2a), and a coronal fat suppressed T2-weighted image (2b) are provided. What are the findings? What is the diagnosis?
Findings
Diagnosis
Intact rotator cuff, mild subacromial bursitis, inadvertent injection of subcoracoid bursa during anterior injection of joint. No communication between subcoracoid and subacromial bursae.
Introduction
The subcoracoid bursa is one of 5 bursae about the shoulder: the subacromial/subdeltoid bursa, the subscapularis recess/bursa, the subcoracoid bursa, the coracoclavicular bursa, and the supra-acromial bursa (figure 8). A bursa is a synovial lined potential space which reduces friction at tendon-tendon and tendon-bone interfaces. In pathologic situations such as trauma, arthritides or infection, a bursa becomes distended and fluid filled, and wall thickening may be observed in chronic cases. A communicating bursa is one that normally communicates with the joint 1; in the shoulder only the subscapularis bursa communicates with the joint. Indeed this bursa is actually a recess of the joint, alternatively referred to as the subscapularis recess. The only other such structure communicating normally with the joint is the biceps tendon sheath. The subacromial bursa and the subcoracoid bursa do not communicate with the joint under normal circumstances. The supra-acromial and coracoclavicular bursae have been described as locations of calcific tendonitis 2, but are not as frequently identified as sources of pathology on MRI as the other bursae, which are more intimately related to the rotator cuff. Distension of the subcoracoid bursa can be an isolated finding, but more frequently it is a marker of significant pathology elsewhere in the shoulder. Correctly identifying the subcoracoid bursa and its relationship to other bursae in the shoulder should prompt the MRI radiologist to search for specific associated abnormalities.
Anatomy of the subcoracoid bursa
The subcoracoid bursa lies deep to the conjoined tendons of the coracobrachialis and short biceps tendons, and superficial to the subscapularis tendon. An early anatomic study identified the subcoracoid bursa in nearly 90% of gross specimens, and in 11% of those, there was a normal communication between the subcoracoid bursa and the subacromial/subdeltoid bursa 3. Neither the subacromial nor the subcoracoid bursa should communicate with the joint under normal circumstances. The subacromial bursa and the subscapularis recess are in close proximity; both track anterior to the subscapularis muscle and deep to the coracoid process, separated only by a thin fibrous band. It is not uncommon for radiologists to confuse a distended subscapularis recess with the subcoracoid bursa. Proper distinction between the two spaces can be made on sagittal images by identifying the typical “saddle bag” appearance of the subscapularis recess as it drapes over the superior margin of the subscapularis tendon, its normal communication with the joint, and the septum between the subscapularis recess and the subcoracoid bursa (figures 9-10).
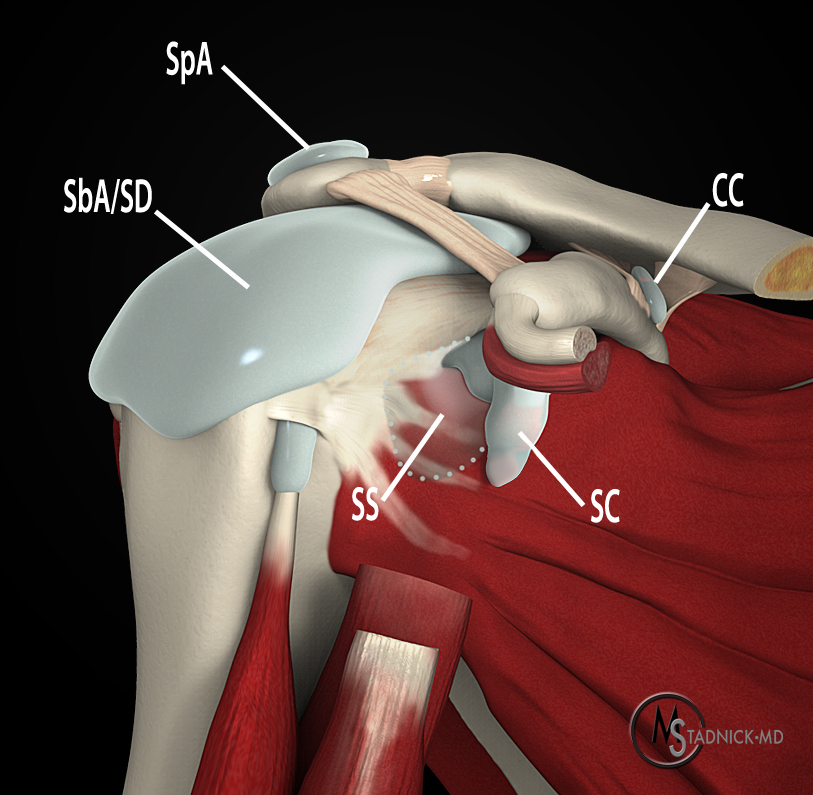
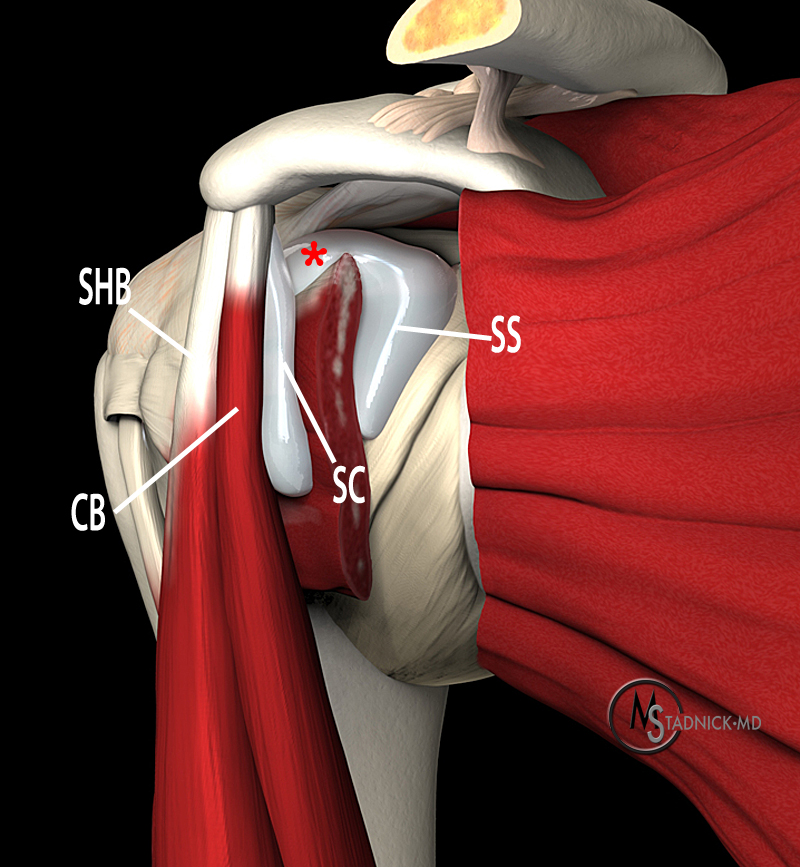
Figure 9:
With the subscapularis muscle partially removed, this anterior oblique 3D representation depicts the subscapularis bursa (SS) deep to the subscapularis muscle and tendon protruding anterosuperiorly (asterisk) over the superior edge of the subscapularis tendon. The subcoracoid bursa (SC) is separate and lies anterior to the subscapularis muscle and deep to the origins of the short head of the biceps tendon (SHB) and coracobrachialis (CB) muscles. Illustration by Dr. Michael Stadnick.
Figure 10:
Two sequential medial to lateral sagittal fat-suppressed T2 weighted images demonstrate the saddlebag appearance of the subscapularis recess (asterisks), draping over the subscapularis tendon (SSc) and communicating with the joint. The separate subcoracoid bursa (arrowheads) has an elongated configuration tracking inferior to the subscapularis recess, along the anterior inferior margin of the subscapularis tendon and deep to the coracobrachialis muscle and tendon (CB).
The subscapularis recess can be loculated, and when markedly distended it can drape even further inferiorly along the anterior border of the subscapularis tendon (figure 11), but should not be confused with the subcoracoid bursa which extends significantly more caudally along the anterior border of the subscapularis tendon.
Pathology associated with the subcoracoid bursa
The clinical significance of fluid within the subcoracoid bursa is variable, but multiple studies have demonstrated its association with significant pathology, indicating that it is not to be considered a normal finding. The most frequently reported and well-established pathology associated with a distended subcoracoid bursa is a full thickness tear of the rotator cuff, specifically the anterior rotator cuff, or supraspinatus tendon 4, 5. Fluid within the subacromial bursa is a well-established sign of a full thickness rotator cuff tear, so in cases where a communication between the subacromial and subcoracoid bursae exists, a full thickness supraspinatus tendon tear would result in fluid within both bursae. Figure 12 demonstrates a full thickness supraspinatus tendon tear in a patient with communicating subacromial and subdeltoid bursae. The amount of fluid within the subcoracoid bursa has not been directly correlated with degree of patients’ symptoms, but it has been suggested that larger amounts of fluid within the bursa correlate with the presence of a full thickness rotator cuff tear4. This could be explained in cases with communication with the subacromial bursa, which would allow for the ongoing decompression of glenohumeral joint fluid through the tear into the subacromial bursa and the subcoracoid bursa.
Figure 12:
(12a) A fat-suppressed T2-weighted coronal image reveals a full thickness supraspinatus tendon tear, with fluid tracking from the joint into the subacromial bursa (arrowheads). The medially retracted supraspinatus tendon is evident (arrow). (12b) Communicating fluid is seen to extend from the subacromial bursa into the subcoracoid bursa (arrowheads) on the corresponding T2-weighted sagittal view. (12c) A more lateral sagittal image demonstrates the distended subcoracoid bursa (arrowheads).
This communication between the subacromial and subcoracoid bursae is a well known pitfall in the diagnosis of rotator cuff tears based on arthrography alone. Although in our test case the injection into the subcoracoid bursa was recognized and the needle was advanced further into the joint, inadvertent injection of contrast into the subcoracoid bursa can lead to a false positive diagnosis of rotator cuff tear. In shoulders where a normal communication between the subacromial and subcoracoid bursa exists, the resultant filling of the subacromial bursa may lead the radiologist to assume that contrast is extending from the joint though a full thickness rotator cuff tear into the subacromial bursa . Since most arthrograms these days are performed in conjunction with MRI, this is not usually a significant problem, as MRI will reveal the status of the rotator cuff. But in those few patients who may be unable to undergo MRI, the shoulder arthrogram alone is still a useful tool for assessing the status of the rotator cuff. In such cases it is useful to note that one study has demonstrated that even an inadvertent subcoracoid bursagram can be used to demonstrate a full thickness rotator cuff tear, since delayed post exercise imaging can reveal retrograde filling of the joint through the rotator cuff tear 6.
Varying incidence of communication between the subcoracoid and subacromial bursae on the basis of MRI findings have been reported as 23% 5 and 55% 4, much higher than the 11% based on an early anatomic study3. A 10.7% incidence of bursal communication was identified in a study using subacromial bursography6. The discrepancy between these numbers has not been explained, but it has been speculated that significant bursal distension may disrupt normal barriers between the bursae5. It is worth noting that bursal communication is much easier to confidently identify in cases with largely distended bursae, suggesting that MRI sensitivity for detecting bursal communication may be directly correlated with the degree of bursal distention.
In cases where there is no communication between the subcoracoid bursa and the subacromial bursa, fluid within the subcoracoid bursa cannot be explained simply by the presence of a supraspinatus tendon tear. One possibility is that the rotator cuff tear has altered the joint space, resulting in new patterns of impingement. Subcoracoid impingement has also been suggested as a cause of subcoracoid bursal distention5,7. A normal coracohumeral distance measures 8-11mm, with an average value of 5.5mm in symptomatic individuals 8,9. Figure 13 demonstrates a distended subcoracoid bursa, narrowing of the coracohumeral distance to 3mm, and a partial thickness subscapularis tendon tear.
Figure 13:
(13a) A fat-suppressed proton density-weighted axial image demonstrates a partial thickness subscapularis tendon tear (arrow), and a narrowed coracohumeral distance (dotted line, measuring 3mm). (13b) A fat-suppressed proton density-weighted axial image demonstrates a partial thickness subscapularis tendon tear (arrow), and a narrowed coracohumeral distance (dotted line, measuring 3mm).
Although relatively rare, an isolated full thickness subscapularis tendon tear also results in fluid within the subcoracoid bursa, allowing fluid to freely decompress from the subscapularis recess into the subcoracoid bursa (figure 14).
Figure 14:
(14a) A gradient-echo axial image reveals a retracted subscapularis tendon (arrow) due to a full thickness tear. Fluid is present within the subscapularis (asterisk) and the subcoracoid (arrowheads) bursae. (14b) A sagittal fat-suppressed image confirms the fluid in the subscapularis recess (asterisk) decompressing out into the subcoracoid bursa (arrowheads).
Some authors have suggested that distention of the subcoracoid bursa alone may produce symptoms4,10, characterized clinically by anterior shoulder pain inferior to the coracoid process 11. However, given the wide range of pathology with which a distended subcoracoid bursa may be associated, isolated subcoracoid bursitis is best considered a diagnosis of exclusion, after all other associated pathology has been ruled out. Involvement of the subacromial bursa with calcific bursitis or synovial chondromatosis has also been described2,9,12. Involvement of the various spaces of the shoulder with synovitis or loose bodies will also follow known normal anatomic patterns, and any departure from this should prompt a search for further pathology. Figures 15 and 16 demonstrate loose bodies within the subscapularis recess and biceps tendon sheath, which communicate with the shoulder joint normally. There is a notable absence of loose bodies in a distended non-communicating subcoracoid bursa (figure 16b).
Figure 15:
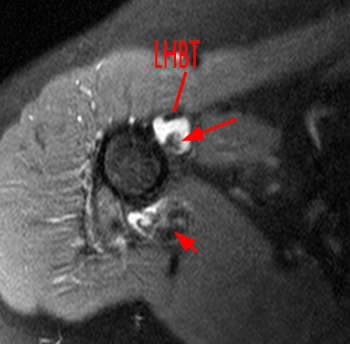
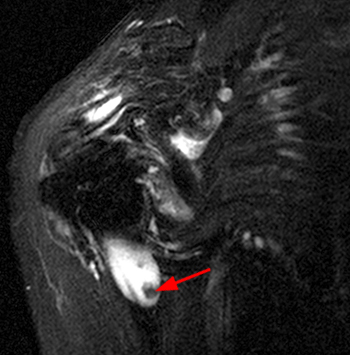
(15a) An axial fat suppressed proton density-weighted image reveals loose bodies within the axillary recess (short arrow) and within the biceps tendon sheath (long arrow). The biceps tendon is indicated (LHBT). (15b) A coronal fat suppressed T2-weighted image redemonstrates the loose body (arrow) within the distended biceps tendon sheath.
Figure 16:
(16a) The sagittal T2-weighted image confirms the same loose body (arrow) within the distended biceps tendon sheath. The adjacent distended subcoracoid bursa (arrowheads) is apparent. (16b) A more medial sagittal T2-weighted image demonstrates a loose body within the subscapularis recess (arrow) and the distended subcoracoid bursa (arrowheads) with a notable absence of loose bodies in the latter. A small amount of fluid within the subscapularis recess is indicated (asterisk).
Distention of the subcoracoid bursa in the absence of rotator cuff tear or communication with the subcoracoid bursa is less frequently seen, and more difficult to explain. Direct MR visualization of rotator interval tears is acknowledged to be difficult5 and published illustrations are rare 13,14, but subcoracoid effusions have been reported in association with rotator interval tears5. Even in the absence of directly visualized rotator interval tears, effusions of the subcoracoid bursa can be seen in association with pathology of the rotator interval. Given the location of the subcoracoid bursa just caudal to the rotator interval, it is possible that bursal distention could be due to localized trauma, chronic inflammation, or altered biomechanics resulting in increased local friction. Figure 17 demonstrates a lesion of the biceps pulley with medial dislocation of the biceps tendon (see Radsource web clinic February 2014), and an associated subcoracoid bursal effusion.
Figure 17:
(17a) A fat-suppressed proton density-weighted axial image reveals a degenerated and medially dislocated long biceps tendon (arrow), providing presumptive evidence of a rotator interval injury. Fluid is evident within a distended subcoracoid bursa (arrowheads). (17b) The distended subcoracoid bursa (arrowheads) is confirmed on the T2-weighted sagittal view.
Another common pathology of the rotator interval is adhesive capsulitis. Subcoracoid effusions are not infrequently seen in association with thickening of the rotator interval capsule and coracohumeral ligament, and infiltration of the subcoracoid fat triangle, all findings described in the MRI diagnosis of adhesive capsulitis14. The presence of contrast filling the subcoracoid bursa has been described as an indirect sign of adhesive capsulitis on MR arthrography 15. Figure 18 demonstrates findings commonly associated with adhesive capsulitis, together with a distended subcoracoid bursa. There was no rotator cuff tear, and although very mild subacromial bursitis was present, there was no visible communication between the subacromial bursa and the subcoracoid bursa.
Figure 18:
(18a) A sagittal T2-weighted image demonstrates a thickened coracohumeral ligament (arrow), infiltration of the subcoracoid fat triangle (short arrow), and a distended subcoracoid bursa (arrowheads). (18b) The coronal fat suppressed T2-weighted image demonstrates thickening and edema of the inferior glenohumeral ligament typical for adhesive capsulitis. The small subacromial fluid collection (arrowheads) did not communicate with the subcoracoid bursa, and there was no full thickness rotator cuff tear.
Conclusion
Radiologists often mistake a distended subscapularis recess for a distended subcoracoid bursa. It is essential to properly distinguish these two potential spaces about the shoulder, since fluid within the subcoracoid bursa is considered pathologic, while the fluid in the subscapularis recess is due to a normal communication with the glenohumeral joint. Isolated subacromial bursitis should be considered a diagnosis of exclusion after all other associated pathology has been ruled out. Neither the subcoracoid bursa nor the subacromial bursa should communicate with the glenohumeral joint when the rotator cuff is intact, but they may communicate with one another. When this interbursal communication exists, subcoracoid bursal distention can be a sign of a full thickness rotator cuff tear. Distention of the subcoracoid bursa has also been recognized in subcoracoid impingement and rotator interval tears, and may be associated with other pathology of the rotator interval such as adhesive capsulitis. Identification of a fluid-filled subcoracoid bursa should thus prompt a diligent search for associated pathology of the shoulder.
References
- Hirji Z, Junjun JS, Choudur HN. Imaging of the Bursae. J Clin Imaging Sci 2011: 1:22 ↩
- Bureau N, Dussault R, Keats T. Imaging of bursae around the shoulder joint. Skeletal Radiol.1996;25:513–7 ↩
- Horwitz T, Tocantins LM. An anatomical study of the role of the long thoracic nerve and related scapular bursae in the pathogenesis of local paralysis of the serratus anterior muscle. Anat Rec. 1938; 71:375-386 ↩
- Schraner AB, Major NM. MR imaging of the subcoracoid bursa. AJR Am J Roentgenol 1999;172(6): 1567–1571 ↩
- Grainger AJ, Tirman PF, Elliott JM, Kingzett-Taylor A, Steinbach LS, Genant HK. MR anatomy of the subcoracoid bursa and the association of subcoracoid effusion with tears of the anterior rotator cuff and the rotator interval. AJR Am J Roentgenol 2000;174(5):1377–1380 ↩
- Mikasa M. Subacromial bursography. Nippon Seikeigeka Gakkai Zasshi 1979; 53:225-231 ↩
- Yi-Hsuan Lee, Ginger H.F. Shu, Ching-Juei Yang, Wen-Sheng Tzeng, Clement Kuen-Huang Chen. Subcoracoid Bursa: Imaging Diagnosis and Significance. J Radiol Sci 2013; 38: 111-118 ↩
- Clark, JM, Harryman DT. Tendons, ligaments, and capsule of the rotator cuff: gross and microscopic anatom. J Bone Joint Surg [Am} 1992, 74: 713-725. ↩
- Friedman RJ, Bonutti PM, Genez B. Cine magnetic resonance imaging of the subcoracoid region. orthopaedics 1998;21(5): 545–548 ↩
- Jonathan TF, Jeffrey MT, Mark C, Diane D. Subcoracoid bursitis as an unusual cause of painful anterior shoulder snapping in a weight lifter. Am J Sports Med 2010; 38: 1687-1692 ↩
- Meraj S, Bencardino JT, Steinbach L. Imaging of Cysts and Bursae about the Shoulder. Semin Musculoskelet Radiol 2014;18:436–447 ↩
- Demirhan M, Eralp L, Atalar AC. Synovial chondromatosis of the subcoracoid bursa. Int Orthop. 1999;23:358-360 ↩
- Morag Y, Jacombson A, Shields G et al. MR Arthrography of Rotator Interval, Long head of the biceps brachii and biceps pulley of the shoulder. Radiology 2005; 235: 1 ↩
- Petchprapal CN, Beltran LS, Lath M, et al.. The Rotator Interval: A Review of Anatomy, Function, and Normal and Abnormal MRI Appearance. American Journal of Roentgenology 2010;195: 567-576 ↩
- Kim HJ, Han TI, Lee KW, et al. Adhesive capsulitis of the shoulder: MR arthrography. J Korean Radiol Soc 2001; 45(1):55-59 ↩