Clinical History: A 13 year-old boy presents with constant dull ache in the anterior aspect of the knee. He has a history of basketball and football injuries. A marker was placed over a palpable nodule at the time of the MR imaging. T1-weighted and fat-suppressed proton density-weighted sagittal images are provided. What are the findings? What is your diagnosis?
Findings
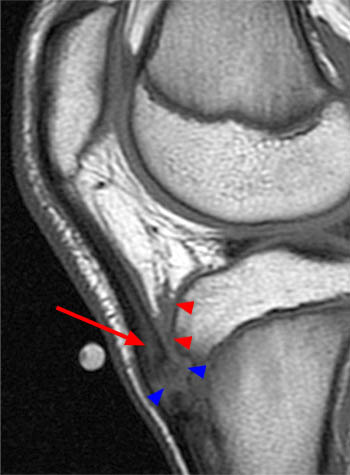
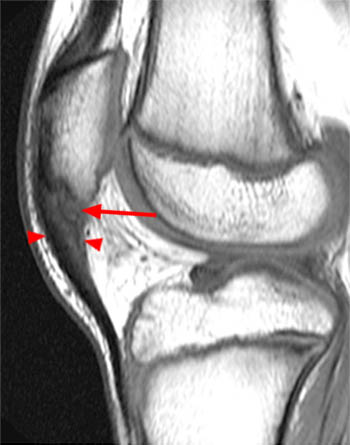
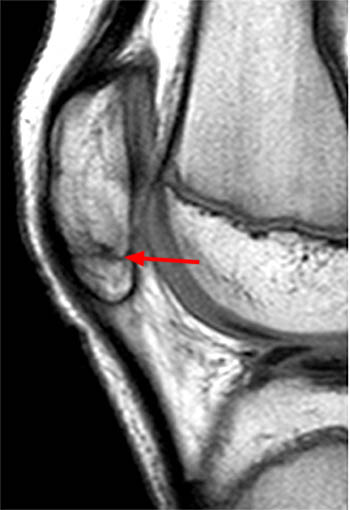
Figure 2:
The sagittal T1-weighted image of the knee demonstrates a marker which has been placed at the skin surface in the region of concern. The distal patellar tendon (arrow) and the deep infrapatellar bursa (red arrowheads) are mildly thickened at this level consistent with early Osgood-Schlatter disease. A large portion of the ossification center of the tibial tuberosity is not ossified (blue arrowheads), which can be expected at this age.
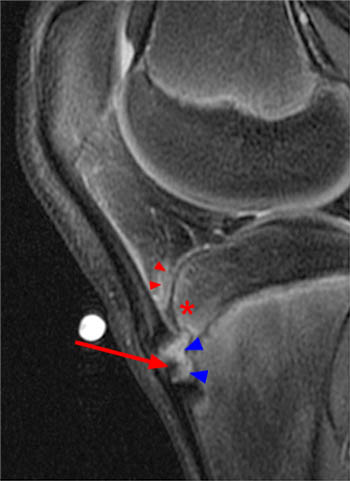
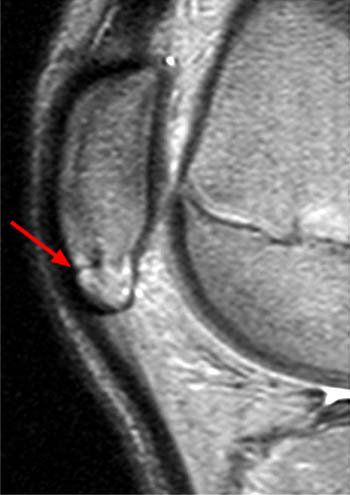
Figure 3:
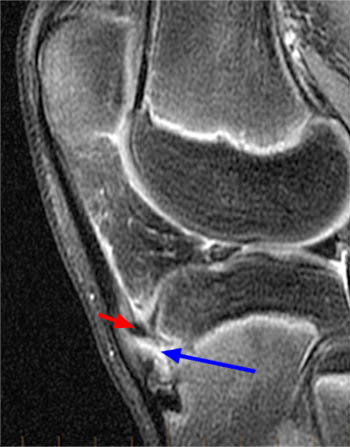
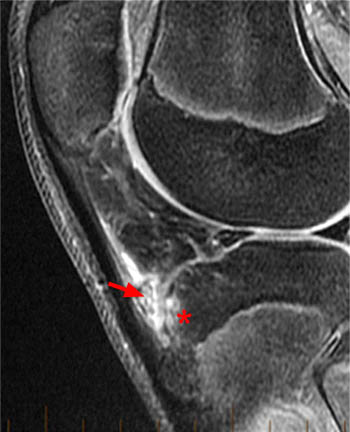
The sagittal fat-suppressed proton density-weighted image demonstrates marrow edema of the anterior aspect of the proximal tibial epiphysis (asterisk). There is edema but no apparent disruption of the ossification center at the patellar tendon insertion (blue arrowheads). A small focus of hypointense signal in the distal portion of the tibial tuberosity (arrow) suggests early ossification which is a normal finding. The deep infrapatellar bursa (red arrowheads) is thickened and Hoffa's fat pad is mildly edematous consistent with early Osgood-Schlatter disease.
Diagnosis
Osgood-Schlatter disease.
Introduction
The extensor apparatus of the knee consists of several structures working together, and if chronically stressed by strong traction forces, this apparatus may fail at different levels, including the patella, patellar tendon and tibial tuberosity. Although patients typically present with chronic anterior knee pain, it should be noted that chronic avulsion injury of the extensor mechanism of the knee sometimes is an incidental finding when a patient is being imaged for other reasons. The imaging appearance of these injuries varies depending on the age of the patient and the duration and force of stress. The focus of this web clinic is on Osgood-Schlatter disease. Sinding-Larsen-Johansson disease, patellar stress fracture and Jumper’s knee are also discussed with an emphasis on the MR imaging findings.
Osgood-Schlatter Disease
Osgood-Schlatter disease is a traction “apophysitis” which involves the insertion of the patellar tendon at the tibial tuberosity. This disease is typically seen in active adolescent males with cyclic pain during sports activity and with tenderness and swelling over the tibial tuberosity1. An associated tibial tuberosity deformity sometimes raises concern of a bone tumor. Knowledge of the normal development of the tibial tuberosity is essential for understanding of the pathogenesis of Osgood-Schlatter disease2,4. The normal ossification of the tibial tuberosity occurs from two centers, one distal and one proximal. Ossification begins distally between the ages of seven and nine years. The proximal center has a physis and is a cartilaginous extension of the tibial epiphysis which expands distally. The physis is transformed from fibrocartilage, to columnar cartilage and finally to bone during its normal maturation process, and fuses with the parent bone in a proximal to distal direction during the teenage years, earlier in girls (aged 13-15) than boys (aged 15-19). A portion of epiphyseal cartilage which remains between the ossification centers of the tuberosity is relatively weak and especially susceptible to tensile forces at the patellar tendon insertion3,4.
Bilateral knee involvement has been observed in up to 50% of cases of Osgood-Schlatter disease. There is an association with knee malalignment, such as patella alta5. The course of the disorder is benign and self-limiting, with resolution expected at the time of skeletal maturity6. The abnormalities found on imaging depend on the age of the child, and the duration and the recurring nature of the disease. Radiographs are helpful to confirm the clinical diagnosis, and typically show soft tissue swelling and edema over the tibial tuberosity and one or more small foci of ossification at the tibial tuberosity. Avulsed fragments are not apparent on radiographs early in the disease process when the tibial tuberosity is completely cartilaginous. The fractures may heal and the tibial tuberosity may have a completely normal appearance or be enlarged and irregular7. Residual tibial tuberosity deformity with adjacent ununited fragments may cause symptoms in adults8.
MRI has a high sensitivity in the evaluation of the soft tissue changes and patellar tendon abnormalities associated with Osgood-Schlatter disease. Findings include diffuse edema within the subcutaneous fat and Hoffa’s fat pad, thickening and effusion of the deep infrapatellar bursa, and thickening of the distal patellar tendon. Displaced and nondisplaced osseous and cartilaginous fragments with varying degrees of marrow edema at the tibial tuberosity can be documented with MRI9. Sonography can be used in the diagnosis and monitoring of the course of the disease, but is operator dependent10.
Nonoperative treatment, specifically anti-inflammatory medication, quadriceps flexibility exercises and activity modification, is usually successful. Symptoms resolve within 12-18 months in most cases. Surgical excision of ossicles and tubercleplasty are considered in patients who fail conservative treatment and should be performed after physeal closure11.
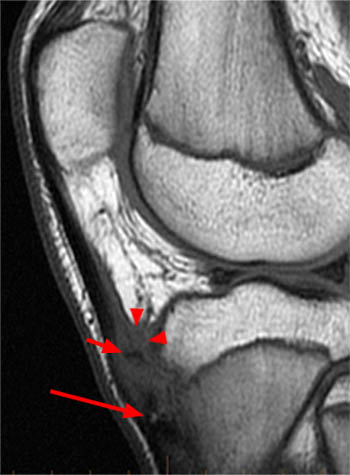
Figure 4:
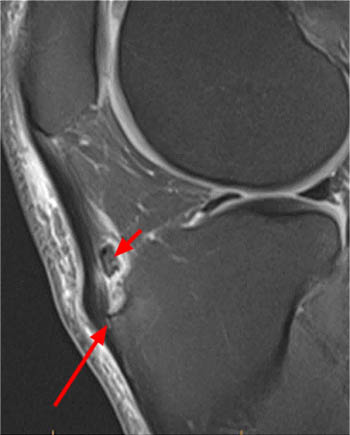
Follow up MRI (a sagittal T1-weighted image) of the knee nine months later in the same patient as the test case shows persistent thickening of the deep infrapatellar bursa (red arrowheads). Ongoing ossification of the distal portion of the tibial tuberosity is now demonstrated (long arrow). A small low-signal bony fragment is demonstrated superior to the tibial tuberosity (short arrow).
Figure 5:
The corresponding sagittal proton-density weighted image nine months after the initial MRI. A tear (blue arrow) of the cartilaginous ossification center of the tibial tuberosity with an adjacent small fragment (short arrow) pulled proximally by the patellar tendon is better seen. The distal patellar tendon remains mildly thickened.
Figure 6:
A sagittal T1-weighted image 22 months later in the same patient reveals persistent thickening of the deep infrapatellar bursa (red arrowheads). Again noted is the small fragment (short arrow) pulled proximally by the patellar tendon. Further ossification of the distal portion of the tibial tuberosity is evident (long arrow).
Figure 8:
Chronic changes related to Osgood-Schlatter disease in a 69 year-old male. The sagittal proton-density weighted image demonstrates a deformity of the tibial tuberosity (long arrow) and an ununited separated bone fragment (short arrow). Mild patellar tendinosis and infrapatellar bursitis are also shown.
Sinding-Larsen-Johansson Disease
In Sinding-Larsen-Johansson disease there is chronic osseous avulsion injury at the inferior pole of the patella caused by repetitive microtrauma to the knee in children between the ages of 10 and 14 years. Symptoms include limited knee motion, and swelling and tenderness over the lower patella. There is an association with patella alta. Healing with osseous incorporation of the fragments into the patella may occur12.
On radiographs, one or more foci of ossification can be seen at the inferior pole of the patella. MRI shows abnormal signal in the inferior patella with irregular cortical margins and osseous fragmentation. Thickening of the patellar tendon at the patellar attachment and diffuse edema of Hoffa’s fat pad are common findings13. A potential but rarely seen imaging pitfall is accessory ossification centers at the inferior patella. Fragmentation in this location can also occur in patients with spastic lower extremities.
The treatment of Sinding-Larsen-Johansson disease is similar to Osgood-Schlatter disease. If symptoms persist, surgical excision of ununited ossicles is an option.
Figure 10:
Sinding-Larsen-Johansson in the same patient as in Figure 9. A gradient echo sagittal image provides better definition of the avulsed fragment at the inferior pole of the patella (arrow) and the thickened and edematous proximal patellar tendon (arrowheads). Marrow edema was present in the patella on T2-weighted images (not included).
Patellar stress fracture
A patellar stress fracture is an unusual injury in active children and adults, and can result in a complete fracture with a sudden contraction of the quadriceps muscle while the knee is in flexion14,15,16. A variety of sports have been associated with this injury. The patients have anterior knee pain, intensified by knee flexion. Tension forces at the anterior surface of the patella and compression forces at the articular surface of the patella during knee flexion result in a transversely oriented fracture, usually in the inferior pole17. Transverse patellar stress fractures have been reported in pediatric patients with spastic cerebral palsy. Nondisplaced fractures may be missed on radiographs. MRI demonstrates a transverse fracture, typically in the inferior anterior aspect of the patella. A bipartite patella or an accessory ossification center should not be mistaken for a patellar stress fracture.
Figure 12:
An incomplete stress fracture (arrow) of the inferior pole of the patella with marrow edema in a 12 year-old boy who plays basketball and has pain with knee extension. The sagittal proton density-weighted image shows that the fracture extends only to the anterior cortex which is a result of the tension forces at the anterior surface of patella and the compression forces at the articular surface of patella during flexion. Note chronic elongation of the inferior pole of the patella consistent with chronic stress on the extensor apparatus during growth.
Jumper’s Knee
When the patella is fully ossified, overuse and chronic repetitive traction forces related to various sports activities, especially jumping, tend to result in patellar tendon thickening rather than osseous avulsion injury18. The clinical manifestations do not differ significantly from those observed in Sinding-Larsen-Johansson disease, and are related to mucoid degeneration, fibrinoid necrosis and fiber failure of the patellar tendon19. Jumper’s knee is associated with patellar tracking abnormalities. Rarely, the patellar tendon may rupture. When used, radiography may demonstrate soft tissue swelling and patellar tendon thickening. MRI shows an increased AP dimension of the tendon with increased signal of the tendon on T1- and T2-weighted images. Marrow edema can be present in the adjacent patella. Partial tendon tears are located within regions of patellar tendinosis and have hyperintense signal on T2-weighted images20,21. A pitfall in the MRI interpretation is related to the normally occurring regions of increased signal within the patellar tendon, most prominent on gradient-echo sequences. Another factor related to a false positive diagnosis is that the normal patellar tendon is not always uniform in thickness. A mild increase in the tendon caliber can be expected both proximally and distally as a normal variation. Ultrasound can be utilized for diagnosis and disease monitoring, and shows tendon enlargement and hypoechoic regions within the tendon22. Symptoms related to Jumper’s knee are usually treated successfully with conservative methods; however, in a small number of patients, surgical tendon debridement is necessary23.
Conclusion
Subacute and chronic avulsion injuries of the extensor mechanism of the knee are commonly encountered abnormalities on MR imaging in children and adult patients participating in sports related activities. Although the prognosis is usually good, prompt and accurate diagnosis is still essential for initiation of proper treatment and prevention of more serious injury. Radiographic findings may be subtle or may be misinterpreted, especially in the skeletally immature patient. MRI allows evaluation of the full extent of osseous and tendon abnormalities. Chronic avulsion injuries of the extensor mechanism are sometimes incidental findings when patients are being imaged for internal derangement of the knee, and knowledge of the correct terminology and the variable appearances of these injures will assist in clinical management.
References
1 Gholve PA, Scher DM, Khakharia S, Widman RF, Green DW. Osgood Schlatter syndrome. Curr Opin Pediatr 2007; 19(1): 44-50.
2 Ogden JA, Hempton RJ, Southwick WO. Development of the tibial tuberosity. Anat Rec. 1975; 182(4): 431-445.
3 Ogden, JA, WO Southwick. Osgood-Schlatter’s disease and tibial tuberosity development. Clin Orthop Relat Res. 1976; 116:180-189.
4 Ehrenborg G, Engfeldt B. Histologic changes in Osgood Schlatter lesion. Acta Chir Scand. 1961; 121:328-337.
5 Aparicio G, Abril JC, Calvo E, Alvarez L. Radiologic study of patellar height in Osgood Schlatter disease. J Pediatr Orthop. 1997; 17(1):63-66.
6 Krause BL, Williams PR, Catterall A. Natural history of Osgood-Schlatter disease. J Pediatr Orthop. 1990; 10(1):65-68.
7 Ozonoff MB. Pediatric orthopaedic radiology, 2nd edition, Philadelphia, WB Saunders, 1992: 365-368
8 Mital MA., Matza RA., Cohen J. The so-called unresolved Osgood-Schlatter lesion: a concept based on fifteen surgically treated lesions. J Bone Joint Surg. Am.1980; 62(5):732-739.
9 Hirano A, Fukubayashi T, Ishii T, Ochiai N. Magnetic resonance imaging of Osgood-Schlatter disease: the course of the disease. Skeletal Radiol. 2002; 31(6):334-342.
10 De Flaviis L, Nessi R, Scaglione P, Balconi G, Albisetti W, Derchi LE.Ultrasonic diagnosis of Osgood-Schlatter and Sinding-Larsen-Johansson diseases of the knee. Skeletal Radiol 1989;18(3) (1989):193-197.
11 Flowers MJ, Bhadreshwar DR. Tibial tuberosity excision for symptomatic Osgood-Schlatter disease. 1995; J Pediatr Orthop.(15)3: 292-297.
12 Medlar RC, Lyne ED. Sinding-Larsen-Johansson disease. Its etiology and natural history.J Bone Joint Surg Am. 1978; 60(8):1113-1116.
13 Dwek JR, Chung CB. The patellar extensor apparatus of the knee. Pediatr Radiol, 2008;38(9):925-935.
14 Teitz, CC.Harrington RM. Patellar stress fracture. Am J Sports Med. 1992; 20(6):761-765
15 Brogle PJ, Eswar S, Denton JR. Propagation of a patellar stress fracture in a basketball player. Am J Orthop. 1997; 26(11):782-784.
16 Orava S, Taimela S, Kvist M, Karpakka J, Hulkko A, Kujala U. Diagnosis and treatment of stress fracture of the patella in athletes. Knee Surg, Sports Traumatol Arthroscopy 1996; 4:206-211.
17 Garcia Mata S, Hidalgo Ovejero A, Martinez Grande M. Transverse stress fracture of the patella in a child. J Pediatr Orthop B. 1999; 8(3):208-211.
18 Ferretti A. Epidemiology of jumper’s knee. Sports Med. 1986; 3(4):289-295.
19 Khan, KM, Bonar F, Desmond PM, Cook JL, Young DA, Visenti PJ, et al. Patellar tendinosis (jumper’s knee): findings at histopathologic examination, US, and MR imaging. Radiology, 1996; 200(3):821-827.
20 Davies SG, Baudouin CJ, King JB, Perry JD. Ultrasound, computed tomography and magnetic resonance imaging in patellar tendinitis. Clin Radiol.1991; 43(1):52-56.
21 Shalaby M, Almekinders LC. Patellar tendinitis: the significance of magnetic resonance imaging findings. Am J Sports Med. 1999; 27(3):345-349.
22 Carr JC, Hanley S, Griffin J, Gibney R. Sonography of the patellar tendon and adjacent structures in pediatric and adult patients. Am J Roentgenol. 2001; 176(6):1535-1539.
23 Romeo AA, Larson RV. Arthroscopic treatment of infrapatellar tendonitis. Arthroscopy 1999; 15(3):341-345.