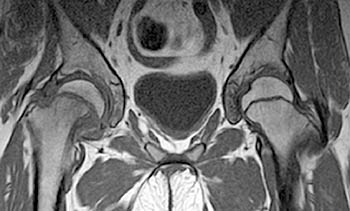
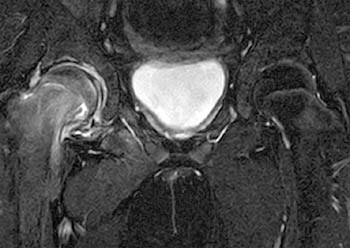
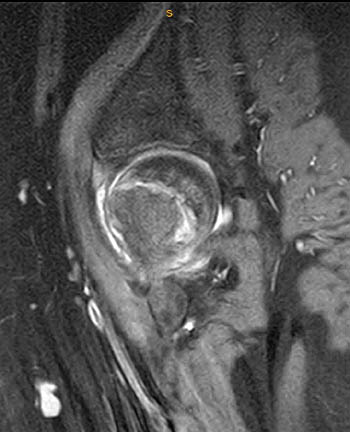
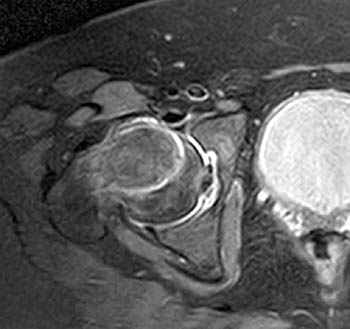
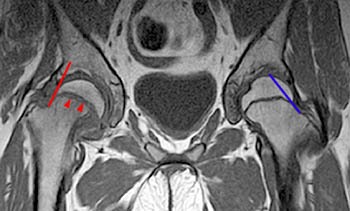
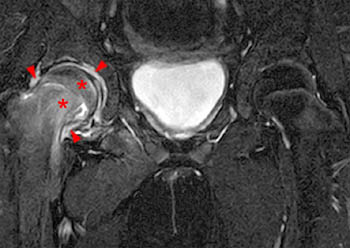
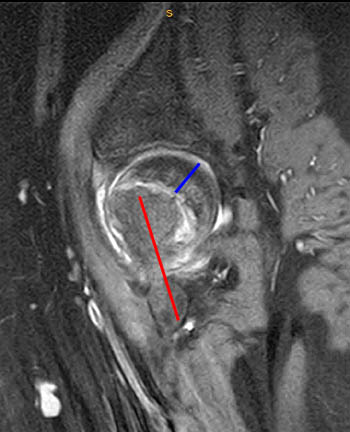
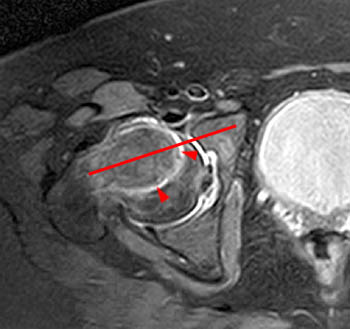
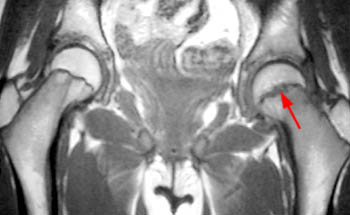
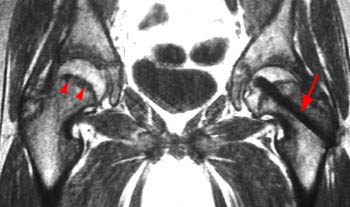
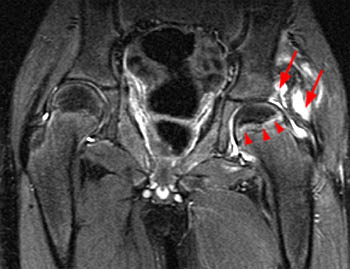
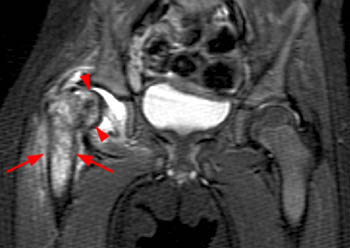
Clinical History: A 10 year-old girl presents with a limp and pain in the right thigh and knee after a fall onto the right knee five months ago. MR imaging of the right knee was normal. MRI of the right hip was obtained and coronal T1 (1a), coronal fat-suppressed T2 (1b), sagittal fat-suppressed proton density (1c) and axial fat-suppressed T2 (1d) weighted images are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Slipped capital femoral epiphysis.
Introduction
Slipped capital femoral epiphysis (SCFE) is a Salter-Harris type1 fracture through the proximal femoral physis and is the most common adolescent hip disorder. SCFE is a misleading term because it is actually the femoral neck metaphysis that displaces with respect to the capital femoral epiphysis 1. In most cases the femoral head will reside posterior to the femoral neck. The overall incidence of SCFE is 10.8 cases per 100,000 children, and is higher in African-American and Hispanic children as compared to Caucasian children 2. Within the United States there is a higher incidence in the northeast and west than the midwest and the southern regions. The incidence in male children is 13.35 cases per 100,000 children, and the incidence in female children in 8.07 cases per 100,000 children. The average age of onset is 12.1 ± 1.8 years 3.
Etiologic Factors
The exact etiology of SCFE is unclear. Only in a small number of cases (<10%) is there a specific traumatic event, such as a fall. In addition to trauma, suggested causes have included mechanical factors, inflammation, endocrine and renal disorders, nutritional deficiencies, and radiation therapy. The combination of abnormal shear forces on the growth plate during rapid growth at the time of adolescence has been implicated 4,5. Most children with SCFE are obese with at least half weighing in the 95th percentile of children in their age group.
Clinical Presentation
Symptoms include pain in any or all of the following regions: groin, medial thigh, hip and knee, with or without a limp 6. The physician may be misled by the presence of pain in the knee, not realizing that the pain is referred from the hip. Indeed, the patient that is presented above underwent MRI of the knee two months before SCFE was diagnosed.
There are three presentations of SCFE based on duration of symptoms 7. The most common presentation is chronic and is characterized by a gradual onset and progression of symptoms for more than 3 weeks. Another presentation is the acute slip which has a sudden onset of symptoms, with a less than 3 week duration. Finally, in an acute-on-chronic presentation there is a sudden exacerbation of symptoms due to acute displacement of the physis, superimposed on a chronic slip.
In chronic SCFE the patient walks with a limp and the affected extremity is externally rotated. There is a lack of full internal rotation, and flexion and abduction ability is limited. With acute slips the patients often cannot walk. A preferred clinical classification system 3,4,5 uses only two designations: stable (child can bear weight with or without crutches) and unstable (severe pain makes weight bearing impossible even with crutches).
The prevalence of bilateral SCFE has reportedly ranged from 21-80%, and bilateral involvement is not typically simultaneous and symmetric. Almost all patients who develop SCFE in the contralateral hip do so within 18 months of diagnosis of the first slip 8 and should be followed accordingly.
Imaging
Anteroposterior and “frog-leg” lateral radiographs are the most important imaging studies for diagnosis. Both hips should be included on the radiographs because of the high incidence of bilateral slip 9. The earliest radiographic finding on the AP view is widening and irregularity of the femoral capital physis. Klein’s line can be drawn on the AP view along the superior aspect of the femoral neck. The line does not intersect the femoral head in SCFE. Subtle slipping is more obvious on the “frog-leg” lateral view 9,10.
There are two radiographic classification systems; the Wilson classification which is based on the relative displacement of the epiphysis on the metaphysis, and the Southwick method which is based on the epiphyseal-shaft angle. The term “pre-slip” has been used in radiographically occult cases, in which physeal and metaphyseal abnormalities may be seen on MR images or CT 11. The earliest evidence of SCFE on MRI is diffuse or globular physeal widening (6a,7a)12. Hyperintense signal of the marrow along the physis on T2-weighted images indicates stress and edema 13. Axial and sagittal MR images are important for identification of any retroversion at the epiphyseal-metaphyseal junction. Both hips should be included on MRI because of the high prevalence of bilateral SCFE.
Figure 7:
A coronal T1 weighted in another patient image shows previous pinning of the left femoral head (arrow). The patient started having pain in the right hip a few months after the surgery. The physis is widened and mildly irregular (arrowheads), consistent with early SCFE. There is a normal postoperative appearance of the left femoral head without avascular necrosis.
Differential Diagnosis
Hip pain in the child and adolescent has many causes (8a,9a) and includes fracture, AVN, Legg-Calve-Perthes disease, septic arthritis, osteomyelitis, muscle injury, apophyseal avulsion and femoroacetabular impingement. In the setting of negative or inconclusive radiographs, MRI of the entire pelvis with fluid sensitive sequences has a unique advantage because of its ability to image ossified and non-ossified structures.
Figure 8:
Coronal STIR image in a 10-year-old child with a recent posterior hip dislocation and extensive capsulolabral injury (arrows). There is hyperintense signal of the left femoral head along the physis (arrowheads), which was thought to be related to ischemia. He later developed AVN with collapse of the femoral head.
Treatment and Prognosis
The goal of treatment is stabilization of the slipping process and to achieve premature closure of the physis. For stable slips, a percutaneous in situ single-screw fixation under fluoroscopic control is performed 14. The treatment of unstable SCFE is more complicated and requires immediate hospitalization in order to protect the tenuous blood supply to the capital epiphysis. Early preoperative traction and manipulative reduction followed by internal fixation is the most commonly used treatment, but open reduction is also being performed at some institutions by experienced surgeons 15, and may carry a lower risk of avascular necrosis.
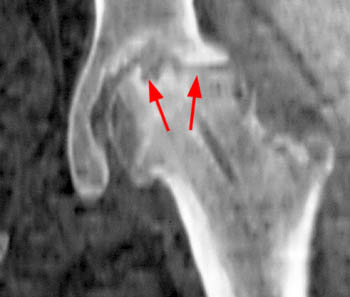
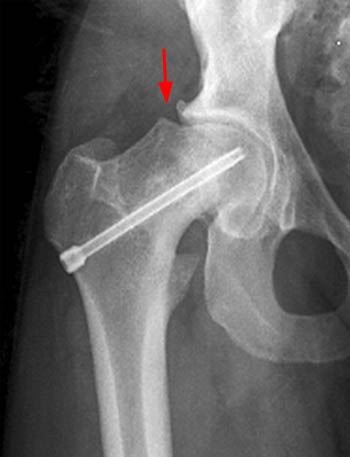
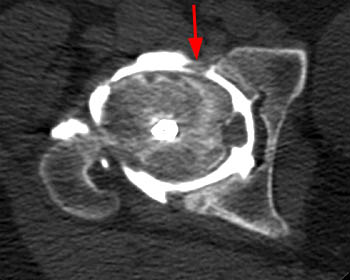
The most serious complication after treatment of SCFE is avascular necrosis (I), which is relatively infrequent after in situ fixation of stable slips 16, but is not uncommon in unstable slips 15. Chondrolysis is a rare complication and represents acute dissolution of the articular cartilage which can occur before or after treatment 17. A chronic deformity of the femoral head and neck after healing of SCFE could result in femoroacetabular impingement with difficulty sitting and with other activities involving hip flexion (J,K) 18,19. MRI may be of limited use for the assessment of complications in SCFE due to severe magnetic susceptibility artifact from hardware, however, with the use of cannulated titanium screws better quality MRI can be achieved, as only minor susceptibility artifact results 20.
Conclusion
SCFE is characterized by a Salter-Harris type 1 fracture through the proximal femoral physis. The typical patient with SCFE is an older obese male child or adolescent with a limp and pain in the hip, groin, thigh, or knee. Radiographs often provide adequate information for correct diagnosis and treatment, but in patients with atypical presentation or inconclusive radiographs in pre-slip cases, MRI may provide a more accurate depiction. For the evaluation of complications of SCFE which include avascular necrosis, chondrolysis and femoroacetabular impingement, MRI plays an important role, even in the presence of a femoral head screw.
References
1 Loder RT, Aronsson DD, Dobbs MB, Weinstein SL. Slipped capital femoral epiphysis. Instr Course Lect 2001; 50:555-570.
2 Lehman CL, Arons RR, Loder RT, Vitale MG. The epidemiology of slipped capital femoral epiphysis: an update. J Pediatr Orthop 2006; 26:286-290.
3 Loder RT, Starnes T, Dikos G, Aronsson DD. Demographic predictors of severity of stable slipped capital femoral epiphysis. J Bone Joint Surg Am 2006; 88:97-105.
4 Gelberman R. The association of femoral retroversion with slipped capital femoral epiphysis. J Bone Joint Surg Am 1986;68:1000-1007.
5 Pritchett J. Mechanical factors in slipped capital femoral epiphysis. J Pediatric Orthop 1988;8:385-388.
6 Matava MJ, Patton CM, Luhman S, et al. Knee pain as the initial symptom of slipped capital femoral epiphysis: An analysis of initial presentation and treatment. J Pediatr Orthop 1999; 19:455-460.
7 Morrissy RT. Slipped capital femoral epiphysis. In: Lovell and Winter’s Pediatric orthopaedics, 3rd edition, Philadelphia: J.B. Lippincott Company, p. 885-904.
8 Jerre R, Billing L, Hansson G, et al. The contralateral hip in patients primarily treated for unilateral slipped upper femoral epiphysis: long-term follow-up of sixty-one hips. J Bone and Joint Surg 76 B:563-567, 1994.
9 Causey AL, Smith ER, Donaldson JJ, et al. Missed slipped capital femoral epiphysis: illustrative cases and a review. J Emerg Med 1995; 13: 175-189.
10 Frick SL. Evaluation of the child who has hip pain. Orthop Clin North Am 2006; 37:133-140.
11 Dillon JE, Connolly SA, Connolly LP, Young-Jo K, Jaramillo D. MR Imaging of Congenital/Developmental and Acquired Disorders of the Pediatric Hip and Pelvis. Magnetic Resonance Imaging Clinics of North America, vol 13, no 4, 2005.
12 Umans H, Liebling MS, Moy L, et al. Slipped capital femoral epiphysis: a physeal lesion diagnosed by MRI, with radiographic and CT correlation. Skeletal Radiol 1998; 27:139-44.
13 Dwek J. The hip: MR Imaging of Uniquely Pediatric Disorders. Magnetic Resonance Imaging Clinics of North America. Vol 17, No 3, 2009.
14 Loder RT. Controversies in slipped capital femoral epiphysis. Orthop Clin North AM 2006; 37: 211-221;vii.
15 Peterson MD, Weiner DS, Green NE, Terry CL. Acute slipped capital femoral epiphysis: the value and safety of urgent manipulative reduction. J Pediatr Orthop 1997;17:648-654.
16 Loder RT, Richards BS, Shapiro PS, et al. Acute slipped capital femoral epiphysis: the importance of physeal stability. J Bone Joint Surg AM 1993;75:1134-1140.
17 Purushottam AG, Cameron D, Millis M. Slipped capital femoral epiphysis update. Current Opinion in Pediatrics, 2009, 21:39-45.
18 Leunig M, Casillas M, Hamlet M, et al. Slipped capital femoral epiphysis: early mechanical damage to the acetabular cartilage by a prominent femoral metaphysis. Acta orthop Scand 2000; 71: 370-375.
19 Dodds MK, McCormack D, Mulhall KJ. Femoroacetabular Impingement after slipped capital femoral epiphysis: does slip severity predict clinical symptoms? J Pediatr Orthop 2009; 29:535-539.
20 Staatz G, Honnef D, Kochs A, Hohl C, et al. Evaluation of femoral head vascularization in slipped capital femoral epiphysis before and after cannulated screw fixation with use of contrast-enhanced MRI: initial results. Europ Radiol 2007; 17: 163-168.