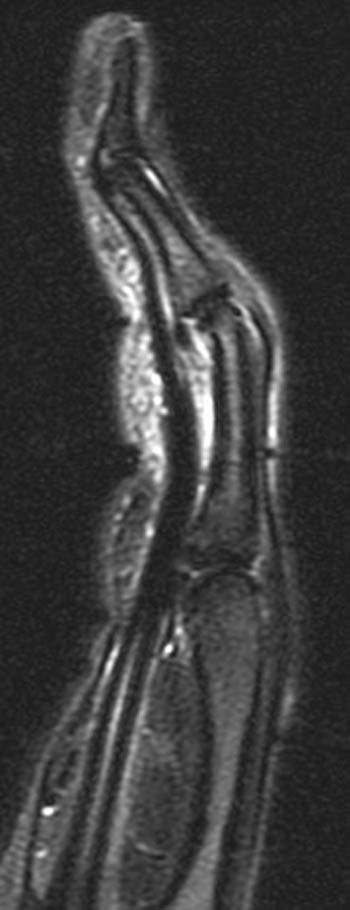
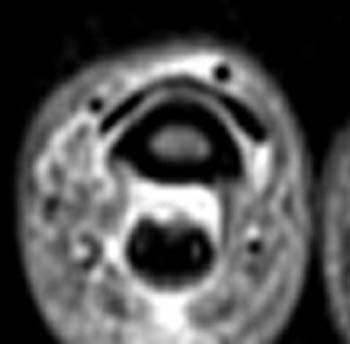
Clinical History: A 28 year-old rock climber presents with persistent pain and swelling at the index finger. (1a) A T2-weighted sagittal image with fat-suppression and (1b) a proton density-weighted fat-suppressed axial image are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Rupture of the A2 pulley of the finger (Climber’s Finger).
Discussion
The annular and cruciate pulleys are areas of focal thickening of the flexor tendon sheath that are of critical importance to the normal biomechanical function of the finger. The pulleys are appropriately named, as they have a pulley-like function that allows the flexor muscle and tendon units to efficiently exert their force upon their respective fingers. In so doing, the pulleys assure proper movement and apposition of the flexor tendons relative to the adjacent osseous structures.
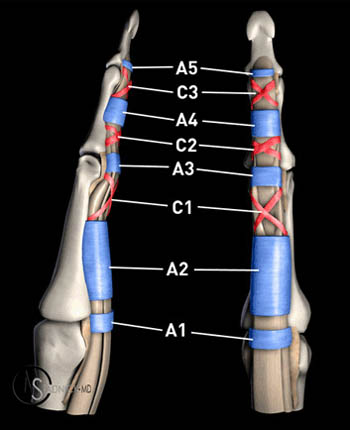
Eight functional pulleys are found at each finger, extending from the volar plate of the metacarpal-phalangeal joint to the base of the distal phalanx.1 The five annular pulleys (A1-A5) are the stronger and more functionally important pulleys, whereas the cruciate pulleys (C1-C3) are important to the intrinsic strength of the flexor tendon sheath (Figure 4a). Of all the pulleys, the most important in proper finger function are the A2 pulley, found at the proximal aspect of the proximal phalanx, and the A4 pulley, found at the level of the mid middle phalanx. The A2 pulley is the strongest, but also the most frequently injured pulley, and the pulley most frequently identified as abnormal on MR images. Increasingly severe pulley injuries follow a predictable pattern, with A2 ruptures progressing from partial to complete, and with more severe injuries then involving the A3 pulley and subsequently the A4 pulley. The A1 and A5 pulleys are rarely injured.
Closed pulley ruptures in the finger first became apparent in the mid 1980s, coinciding with the development of the sport of rock climbing. Pulley injuries are an overuse phenomenon, occurring in rock climbers because of the repetitive, excessive forces placed upon the fingers during the activity, with competitive climbers often placing the stress of their entire body weight upon one or two flexed fingers. A study by Schoffl et al. in 20032 of over 600 injured rock climbers found pulley lesions to be the single most common injury in these athletes.
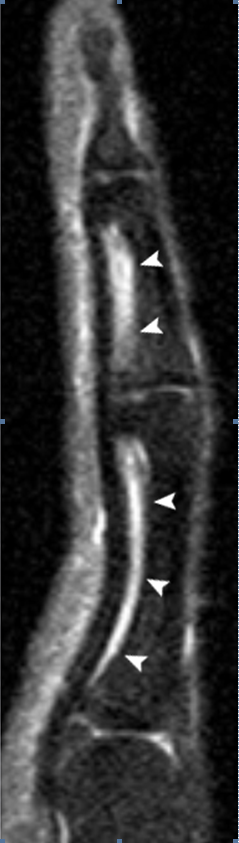
The pulley system of the finger is often difficult to visualize on routine sagittal MR images. Normal pulleys can be visualized by utilizing MR tenography, but this invasive technique is rarely performed. In patients with tenosynovitis, the fluid within the tendon sheath provides a physiologic tenogram, and outlines the pulleys, particularly the larger A2 and A4 pulleys, making them visible (5a).
Of course, one cannot routinely rely on tenography or the presence of tenosynovitis for the accurate visualization of the pulley system, and thus pulley injuries are often first suggested by indirect signs. In acute mild pulley injuries or partial tears, edema is seen along the course of the involved pulleys in the sagittal plane (6a), and pulley edema or irregularity may be directly visualized on axial views (7a).
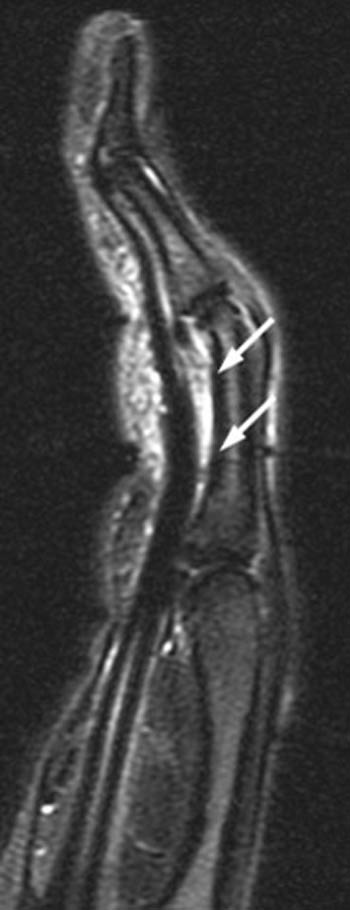
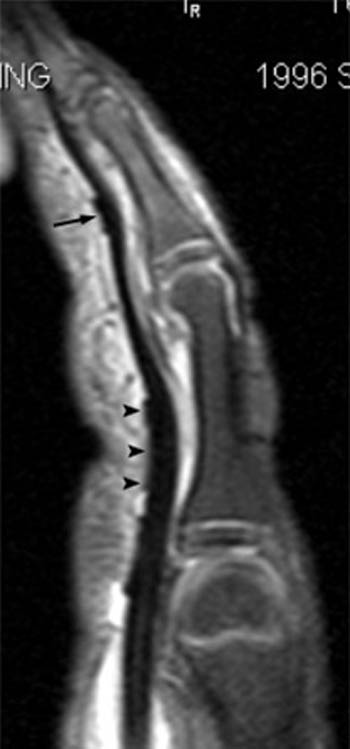
Figure 6:
Edema is present between the flexor tendons and the adjacent phalanxes in the region of the A2 through A4 pulleys (arrowheads) in this fat-suppressed T2-weighted sagittal view of the index finger from an elite rock climber with finger pain. No significant abnormal separation of the tendons from the phalanxes is noted.
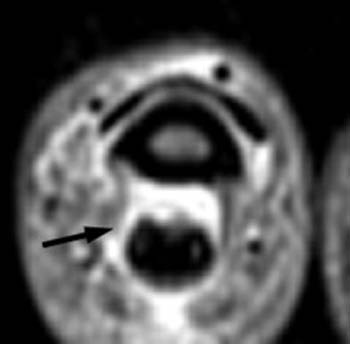
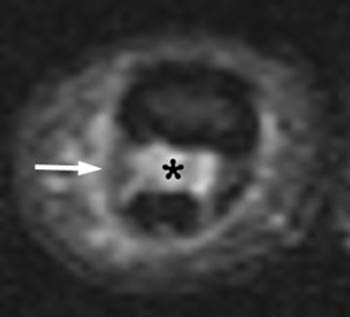
Figure 7:
(7a) At the level of the A4 pulley, a fat-suppressed proton density-weighted axial image reveals edema and irregularity along the radial side of the pulley (arrow), and edema between the flexor digitorum profundus and the middle phalanx is redemonstrated (asterisk). The appearance in this patient is compatible with partial tears.
With worsening injuries that involve complete pulley tears, as demonstrated in our first case, an abnormal gap referred to as “bowstringing” may be visualized between the flexor tendons and the adjacent phalanxes.3 This gap can be exaggerated if the patient is scanned in forced flexion, which is accomplished by having the patient flex the finger while pushing the tip of the finger against a firm surface. Unfortunately, forced flexion also increases patient discomfort and resultant motion artifact on MRI. One alternative is the use of dynamic ultrasound,4 which has been found to be sensitive for both A2 and A4 pulley ruptures. With ultrasound the distance between the flexor tendon and the phalanx can be measured in forced flexion, with abnormal separation of greater than 1mm being seen in pulley injuries. With complete A2 pulley ruptures, separation of greater than 3mm is often present. However, ultrasound lacks the soft-tissue contrast and resolution of MR, is more operator dependent, and lacks sensitivity for associated osseous or intrinsic tendon injuries that may be found in this patient group. In clinical practice, with careful, high-resolution technique, MR is frequently able to directly visualize pulley ruptures in the axial plane, eliminating the need for forced flexion techniques.
Patients with pulley injuries may report a sudden onset of pain coinciding with a slip or forceful maneuver, and an audible pop may be heard. However, the diagnosis of a pulley lesion may be challenging, as pain, swelling, and limited range of motion makes the physical examination difficult. MR allows accurate diagnosis in such patients, and provides valuable guidance in the operative approach. Most orthopaedic surgeons agree that strains and partial tears of the pulley system can be treated conservatively, with immobilization and pulley-protective physical therapy. Complete ruptures, however, often require operative repair to avoid future functional disability.
Conclusion
Climber’s Finger is a relatively new entity that is found in rock climbers who injure the pulley system at the finger. As the sport of rock climbing continues to expand, radiologists and orthopaedic surgeons will encounter this entity with increasing frequency. MRI allows accurate diagnosis in these patients, and importantly, is able to provide a simultaneous evaluation for occult osseous, ligamentous, or intrinsic tendon injuries.
References
1 Hauger O, Chung CB, Lektrakul N, et al. Pulley System in the Fingers: Normal Anatomy and Simulated Lesions in Cadavers at MR Imaging, CT, and US with and without Contrast Material Distention of the Tendon Sheath. Radiology 2000; 217:201-212.
2 Schoffl V, Hochholzer T, Winkelmann HP, Strecker W. Pulley Injuries in Rock Climbers. Wilderness and Environmental Medicine 2003; 14(2):94-100.
3 Gabl M, Rangger C, Lutz M, et al. Disruption of the Finger Flexor Pulley System in Elite Rock Climbers. The American Journal of Sports Medicine 1998; 26:651-655.
4 Klauser A, Frauscher F, Bodner G, et al. Finger Pulley Injuries in Extreme Rock Climbers: Depiction with Dynamic US. Radiology 2002; 222:755-761.