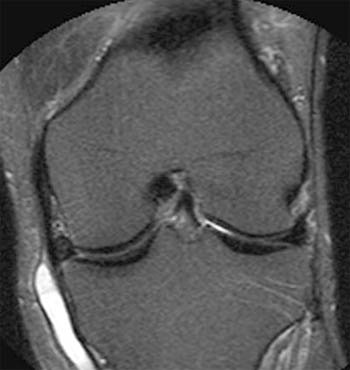
Clinical History: A 67 year old male presents with medial knee pain and swelling for 1.5 years, no known injury. (1a) Coronal fast spin-echo inversion recovery and (1b) axial fast spin-echo proton density images are presented. What are the findings” What is your diagnosis?
Findings
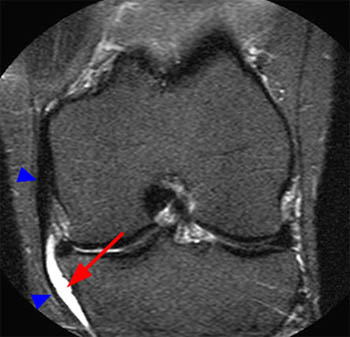
Figure 2:
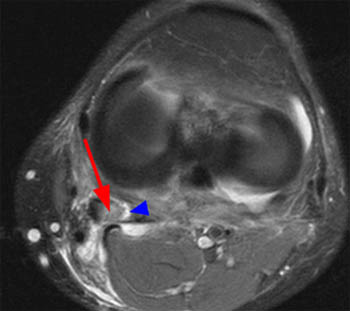
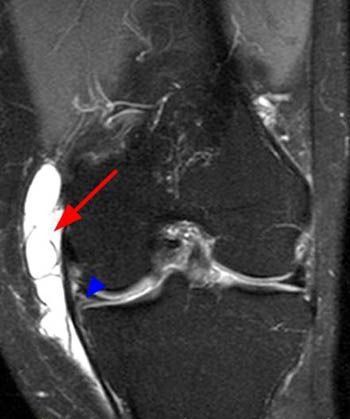
(2a) The coronal inversion recovery image demonstrates a fluid collection (arrow) distal to the joint line and superficial to the medial collateral ligament. (2b) The axial proton density-weighted image demonstrates that the fluid collection (arrow) is deep to the sartorius, gracilis, and semitendinosus tendons (arrowheads).
Diagnosis
Pes Anserine Bursitis.
Introduction
The pes anserinus (Latin for “goose’s foot?) refers to the webbed foot appearance of the conjoined tendons of the sartorius, gracilis and semitendinosus at their insertion onto the proximal medial tibia. The tendons course superficial to the medial collateral ligament, and the bursa lies just deep to the pes tendons. The pes anserine bursa is distal and anterior to the medial collateral ligament bursa.
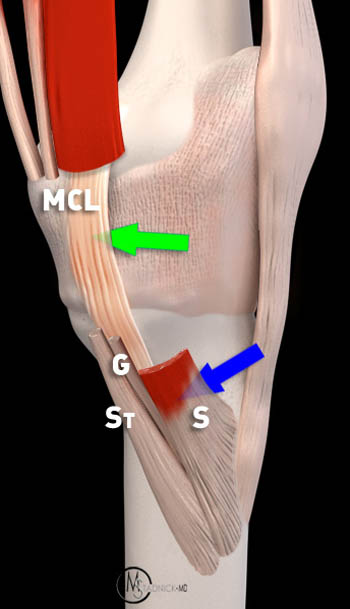
Figure 3:
The pes anserinus is formed from the fusion of the sartorius (S), the gracilis (G), and the semitendinosus (St). In this graphic representation the pes tendons have been removed to reveal the medial collateral ligament (MCL). The blue arrow indicates the location of the pes anserine bursa, which is located deep to the pes anserinus. The green arrow indicates the location of the tibial collateral bursa, which is found deep to the medial collateral ligament.
Pes anserine bursitis was initially described by Moshcowitz in the 1930’s as an affliction of older adults with arthritis1, but it can also be seen in the young, athletic population, especially runners.2 The bursa becomes inflamed and distended with repetitive microtrauma. Etiologic factors include valgus stress and tendon tightness, as well as irritation from underlying osteophytes or exostoses. A high association with diabetes and obesity has also been reported.3 Patients typically present with medial joint line tenderness and swelling, or more diffuse medial pain, often more prominent while ascending or descending stairs.
MR Differential Diagnosis
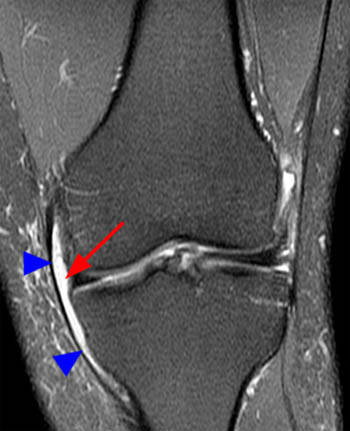
Medial pain and swelling can also be seen with inflammation of a variety of other medial bursae about the knee. The tibial collateral ligament bursa4 lies deep to the medial collateral ligament, extends both proximal and distal to the joint line (4a), and is readily distinguishable from the more superficial and distal pes anserine bursa.
Another bursa that may cause a posteromedial knee fluid collection is the semimembranosus/tibial collateral ligament bursa. This bursa, when filled with fluid, displays a characteristic horseshoe configuration as it courses around the semimembranosus tendon and deep to the MCL, distal to the joint line5(5a,6a). Semimembranosus tendinosis or partial thickness tears with tenosynovitis are also included in the differential diagnosis (7a).
Even more important is the distinction between bursitis and more serious injuries to the knee. Meniscal tears with parameniscal cysts may present with medial joint line pain and palpable swelling, and generally require arthroscopic treatment for adequate relief. The meniscal cyst may remain intracapsular, but may also track between the layers of the capsule, into the extracapsular soft tissues or the subcutaneous fat. As such it may mimic bursitis, but careful examination will reveal a meniscal tear, and in many cases a communication between the cyst and the meniscal tear will be evident (8a). Another important differential is a tear of the medial collateral ligament. Lastly, proximal tibial stress fractures are a not uncommon diagnosis which is very important to distinguish from the clinically similar presentation of pes anserine bursitis. MR allows accurate characterization of the relevant pathology in such cases.
Treatment
Typical treatment for pes anserine bursitis includes rest, NSAIDs, cryotherapy and physical therapy, the latter focusing on stretching and strengthening of the adductor and quadriceps musculotendinous units. A second line of treatment includes injection of the bursa with local anesthetics and/or corticosteroids. MRI can clearly depict the exact location of the bursitis to guide such injections. Rarely, with prolonged disability, and particularly when a mechanical irritant such as an exostosis is present, surgical intervention may be warranted, in which case the bursa and any offending anatomical anomaly is resected.
Conclusion
Pes anserine bursitis is a not uncommon cause of medial knee pain, particularly in the running athlete, the obese, or diabetics. The posteromedial pain of pes anserine bursitis is often confused clinically with more common entities such as osteoarthritis, meniscal tears, and medial collateral ligament sprains. In such patients, treatments vary markedly, and MR allows pes anserine bursitis to be clearly distinguished from these other entities. In cases of medial bursitis of the knee, MRI differentiates between the types of bursitis, and is useful in directing therapeutic injection, should it be required.
References
1 Moschowitz E. Bursitis of the Sartorius bursa: an undescribed malady simulating chronic arthritis. JAMA 1937; 109:1362.
2 Forbes RJ, Celms CA, Janzen DL. Acute Pes Anserine Bursitis: MR Imaging. Radiology 1995; 194:525-527.
3 Glencross PM, Little JP. Pes anserine bursitis. E-medicine March 28, 2006.
4 Lee JK, Yao L. Tibial collateral ligament bursa: MR imaging. Radiology 1991; 198: 855-857.
5 Rothstein CP, Laorr A, Helms CA, Tirman PF. Semimembranosus-tibial collateral ligament bursitis: MR imaging findings. AJR 1996 Apr; 166 (4): 875-7.