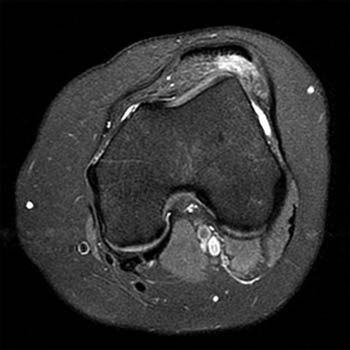
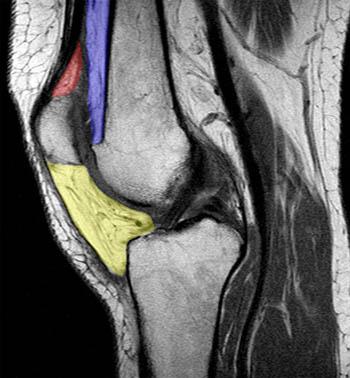
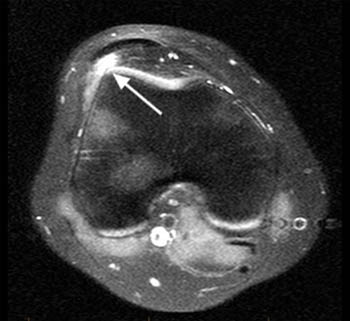
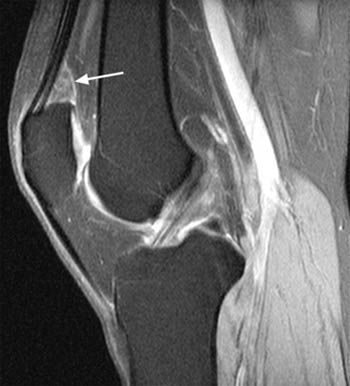
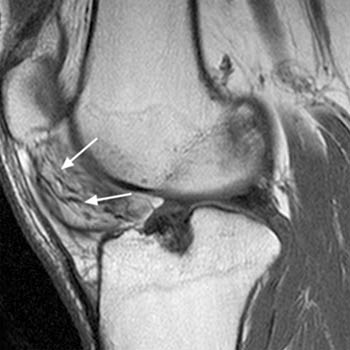
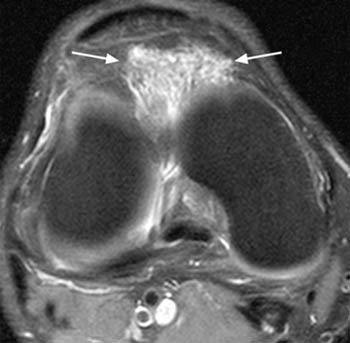
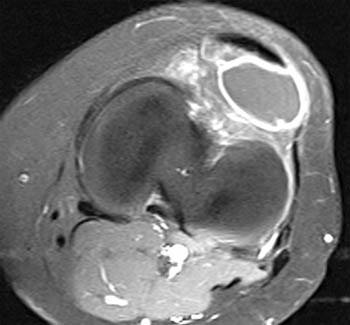
Clinical History: 25 year old female presents with a history of chronic lateral knee pain and instability. (1a) Axial and (1b) sagittal fat-suppressed proton density weighted images of the left knee are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Patellar Tendon-Lateral Femoral Condyle Friction Syndrome (PT-LFCFS).
Introduction
Knee pain is a very common clinical complaint, especially among active individuals. Numerous traumatic and non-traumatic processes may be encountered, many occurring relative to the anterior compartment, including impingement or friction syndromes. The most common friction syndrome of the knee is the iliotibial band friction syndrome. However, despite the lack of extensive literature on PT-LFCFS, it appears to be a well-recognized process among primary care physicians, who may refer to it as fat pad impingement syndrome.1,2
Normal Anatomy
The infrapatellar fat pad is bordered by the inferior pole of the patella superiorly, the joint capsule and patellar tendon anteriorly, the proximal tibia and deep infrapatellar bursa inferiorly, and the synovium-lined joint cavity posteriorly. Thus, it is intracapsular but extrasynovial. It is tethered to the intercondylar notch superiorly by the infrapatellar synovial fold or infrapatellar plica. It also is attached directly to the anterior horns of the menisci inferiorly and to the periosteum of the tibia.3,6
Biomechanics
The biomechanics of PT-LFCFS are not well understood, with it being described as an impingement from an anterverted patella and as an overuse injury. Overuse injury is the favored mechanism, with the patellar tendon chronically rubbing against the lateral femoral condyle or compressing the lateral aspect of Hoffa’s fat pad between itself and the lateral femoral condyle. It is probably related to patellar maltracking or malalignment, because most patients with this abnormality have patella alta and/or lateral subluxation of the patella.7
MRI Findings
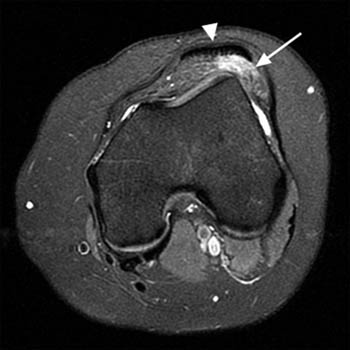
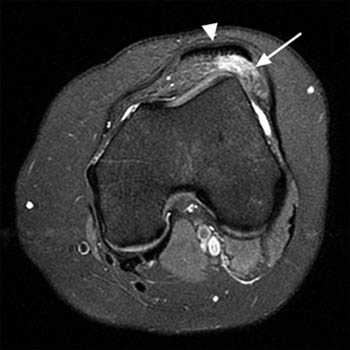
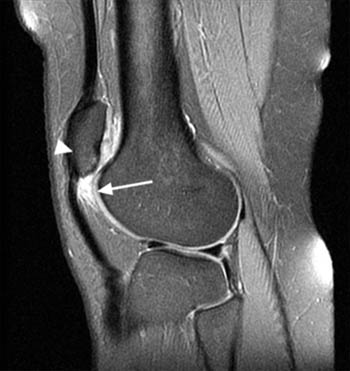
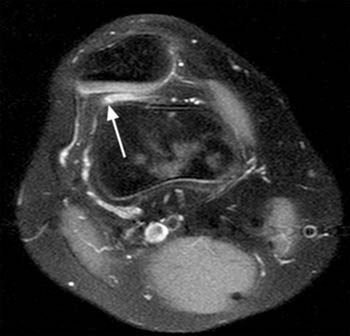
On MRI, a focal area of high signal or edema on STIR or T2 weighted sequences is present at the inferolateral aspect of the patellofemoral joint, specifically the lateral portion of the infrapatellar fat pad (5a,5b). Specifically, this is just below the inferior margin of the patella and anterior to the lateral trochlear ridge. A focal lobulated mass with signal characteristics of fluid or cystic change can sometimes be present in the lateral soft tissues of the knee between the lateral femoral condyle and the lateral retinaculum. Associated findings of lateral patellar subluxation (6a) and/or patella alta are frequently present.
Discussion
Patellar pain and anterior knee pain are common presenting problems encountered in primary care and orthopaedic clinics. Patients with PT-LFCFS typically present with knee pain exacerbated by hyperextension, accompanied by focal point tenderness at the inferior pole of the patella. The fat pad may even be thickened resulting in difficulty palpating the patella on the affected side.
PT-LFCFS usually occurs in young adults but has a reported age range of 13 to 56 years.7 Most people affected do not participate in routine athletic activities and the pain may result from both acute trauma and from chronic repetitive stress.7
PT-LFCFS is likely related to the clinical entity of fat pad impingement and has previously been called Hoffa’s Fat Pad Impingement.2 Although this entity is recognized by some clinicians on the basis of clinical presentation, it receives little attention in the orthopaedic, rheumatology, and radiology literature.7 Patients are often misdiagnosed as having patellar tendonitis.
This entity is associated with patella alta and patellar tracking abnormalities as well as partial tears of the patellar tendon. In the retrospective study by Chung, et. al.7 alignment abnormalities were noted in 38 of 42 patients. In 33 of 42 patient, patella alta was present. Lateral patellar subluxation was seen in four of 42 patients, and evidence of patellar dislocation was demonstrated in a single patient.
Treatment
Treatment is usually conservative. Treatment of PT-LFCFS is not difficult, although it can take a long time to fully recover.8,9 The superior pole of the patella may be taped or bandaged, so that the inferior patella imposes less mass effect on the underlying intra-articular fat. The success rate has been touted to be high.7
Modifying activities that increase pain is important. Stretching the quadriceps and hip flexor muscles may help to lessen some of the downward pressure the patella applies to the fat pad.8,9 Anti-inflammatory medicines are also frequently used. Much less often, injections of corticosteroids to reduce inflammation or surgery to trim the fat pad are required.8,9
Related Entities
Several other entities that involve the peripatellar fat may be encountered when evaluating MR of the knee. Of these, one of the most common is quadriceps/suprapatellar fat pad impingement syndrome. A study by Roth, et al.10 demonstrates mass effect from the quadriceps fat pad on the suprapatellar recess (defined as a posterior convex border) in 12% of 92 consecutive knee MRI examinations. The quadriceps fat pad was of intermediate or fluid signal intensity in 54%. They found that the finding of quadriceps fat pad mass effect on the suprapatellar recess was significantly associated with anterior knee pain at physical examination. However, none of the patients in the study by Roth had a history of direct trauma or overuse. The abnormality thus may have a developmental cause related to the anatomy of the extensor mechanism, or may be related to abnormal mechanics.
Another not uncommon patellar fat pad region abnormality is Hoffa disease (8a,8b). Hoffa disease is a syndrome of infrapatellar fat pad impingement, due to single or repetitive traumatic episodes, with hyperextension and rotational forces resulting in hemorrhage. The inflamed fat pad then becomes hypertrophied with predisposition to impingement between the tibia and femur, and thus to further injury.6 On MR images, acute findings indicate the presence of fluid and chronic findings resemble those of scarring after knee arthroscopy.
On sagittal T2-weighted images, the affected region of the fat pad may have diffuse high signal intensity edema or a heterogeneous appearance due to hemorrhage. The patellar tendon may be bowed anteriorly by the swollen pat pad. Chronically, areas of low signal intensity within the fat pad may represent foci of hemosiderin, fibrosis, or ossified fibrocartilaginous tissue.3,6
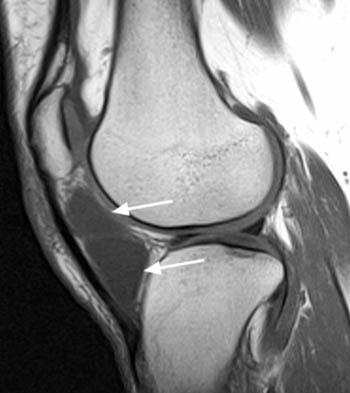
Figure 8:
Focal soft tissue thickening and edema (arrows) are seen within the infrapatellar fat pad in a patient following acute trauma on (8a) sagittal T1-weighted and (8b) axial fat-suppressed proton density-weighted images. In acute cases of Hoffa disease such as this, the abnormality may also be described as a fat pad shearing injury.
Infrapatellar fat pad ganglia may resemble Hoffa disease on MR images, but this entity is typically more homogeneous and well defined in nature (9a,9b,10a). Originally thought to be rare, the advent of MRI has revealed that the infrapatellar fat pad is one of the most common locations for a ganglion cyst at the knee. Although often simply an incidental finding, at times large infrapatellar ganglia may cause mechanical symptoms that warrant surgical excision.
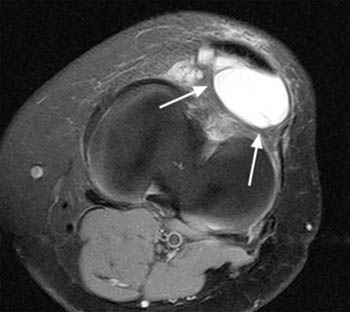
Figure 9:
(9a) T1-weighted sagittal and (9b) proton density-weighted axial images demonstrate a large, fluid signal intensity mass (arrows) which fills the infrapatellar fat pad in this patient who presented with palpable anterior knee swelling. The well-defined, homogeneous appearance of the lesion is typical for a benign ganglion, but in light of lesion size, intravenous contrast was administered.
Conclusion
Patellar tendon lateral femoral condyle friction syndrome is one of several entities that result in anterior knee pain and in which abnormalities of the patellar fat pads are found on MR imaging. Though the entities are related based on location of disease, their imaging appearances are varied and distinctive, allowing the astute interpreter of MR to identify the abnormalities, thereby enabling the clinician to provide necessary and appropriate care based on the correct diagnosis.
References
1 Walsh WM. Patellar tracking problems in athletes. Prim Care 1992;19:303-330.
2 Bergman AG, Fredericson M. MR imaging of stress reactions, muscle injuries, and other overuse injuries in runners. MRI Clin North Am 1999;7:151-174.
3 Jacobson JA, Lenchik L, Ruhoy MK, Schweitzer ME, Resnick D. MR imaging of the infrapatellar fat pad of Hoffa. Radiographics 1997;17:675-691.
4 Staeubli HU, Bollmann C, Kreutz R, Becker W, Raushning W. Quantification of intact quadriceps tendon, quadriceps tendon insertion, and suprapatellar fat pad: MR arthrography, anatomy, and cryosections in the sagittal plane. AJR 1999; 173:691-698.
5 Schweitzer ME, Falk A, Pathria M, Brahme S, Hodler J, Resnick D. MR imaging of the knee: can changes in the intracapsular fat pads be used as a sign of synovial proliferation in the presence of an effusion” AJR 1993;160:823-826.
6 Saddik D, McNally EG, Richardson M. MRI of Hoffa’s fat pad. Skeletal Radiol. 2004;33:433-444.
7 Chung CB, Skaf A, Roger B, Campos J, Stump X, Resnick D. Patellar tendon-lateral femoral condyle friction syndrome: MR imaging in 42 patients. Skeletal Radiol. 2001;30:694?697.
8 www.clinicalsportsmedicine.com (Chapter 24)
9 Radiol Med (Torino). 1998 Apr;95(4):278-85
10 Roth C, Jacobson J, Jamadar D, Caoili E, Morag Y, Housner J. Quadriceps fat pad signal intensity and enlargement on MRI: Prevalence and associated findings. AJR. 2004;182:1383-1387.
11 Resnick et al. Internal derangements of joints. 2nd edition. Saunders Elsevier. 2007.